Background

The World Development Report in 1993 focused on the economic value in focusing on a narrow set of health interventions.
On the 20th anniversary of the highly influential 1993 World Development Report, titled ‘Investing in Health’, an independent commission convened by The Lancet has developed a potentially groundbreaking report (Global Health 2035: a world converging within a generation) summarizing the current research demonstrating the potential economic value of universal health coverage, and lays out an aggressive but fairly straightforward set of policy recommendations that could help ministers of health, civil society, and advocacy organizations push forward legislation and regulation necessary to secure the right to health.
I think that this report is very significant for a few reasons:
- The commission is a mix of the right players (Harvard academics and administrators, ministers of health, USAID, World Bank, IMF, etc).
- It is fairly critical of the failings of the 1993 WDR. And, it offers sound analysis and recommendations about how to build off of the successes, failures, and lessons gained during the tumultuous decades in global health and development since then.
- It seems to have Partners In Health’s strategy and logic all over it. From the almost explicit ‘preferential option for the poor’ language to the model of structure and function for emerging health systems, PIH has certainly influenced this important vision for the future.
- The report is coming at just the right moment. Twenty years after the ‘Investing In Health’ WDR and approaching the end of the era of the Millennium Development Goals, we sorely need a progressive, ambitious, and inspiring vision to guide us. As I’ve written previously and continue to witness/study, more students than ever are passionate about advancing the right to health. Our work with PIH | Engage shows that people of many ages and demographics are eager to participate as well.
Major concepts in GH2035:
There is a major economic payoff in investing in global health.
The report builds off of the work of the 1993 WDR in making the case that investing in health is not only a moral imperative – it is actually just that, an investment in the productive capacity and “full income” of a country. By solely using GDP growth (only accounts the market value of goods and services produced in one year) as the metric of development success, a lot of important value is missed and policy is built and evaluated in an incomplete way.
“On re-reading WDR 1993, admittedly with the benefit of hindsight after two decades, we believe that it had two major limitations. First, although WDR 1993 discussed the “instrumental value” of better health (eg, better health improves worker productivity), it did not attempt to quantify the “intrinsic value” of health (the value of good health in and of itself). Our report summarises research that quantifies the intrinsic value of mortality reduction— the findings should, we hope, lead to a notable reassesment of the priority of health in national and international investment portfolios. In particular, benefit-to-cost assessments and a strong implementation record point to the value of increased commitment to health.
Second, financial protection failed to receive sufficient attention in WDR 1993, although very few data were available in 1993 about out-of-pocket spending and catastrophic financial expenditures. Moreover, only a few analyses pointed to financial protection as an important goal of health systems. By contrast, the role of UHC in providing financial protection is a major feature of our report.”
The analysis that they have gathered shows that fully 24% of “full income” growth in low income and middle income countries can be attributable to the “value of additional life-years” which is linked to expanded investments in health.
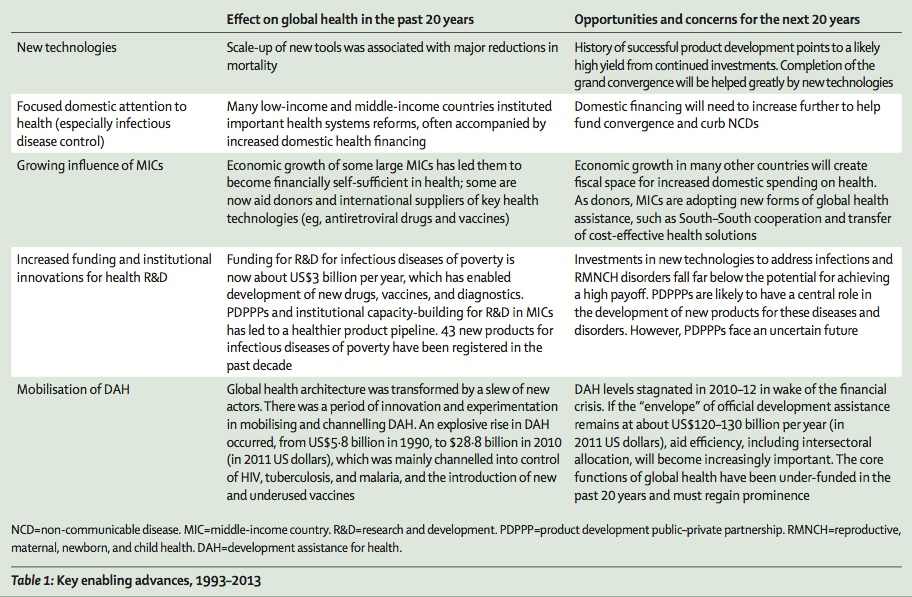
What’s happened in global health over the past 20 years that has led to such success? Well, they’ve kindly summarized their finding in a handy table:
A grand convergence of death rates from infectious disease, child, and maternal mortality between the high and low income countries.
With the right investments made by local governments, appropriate investment in health systems strengthening, renewed commitment to expanding development assistance for health from wealthy countries, we could see an incredible convergence of rates of infectious disease death, childhood death, and maternal mortality. The report builds the case that by 2035 we could see rich and poor countries alike experiencing very little unnecessary deaths from these completely preventable sources.
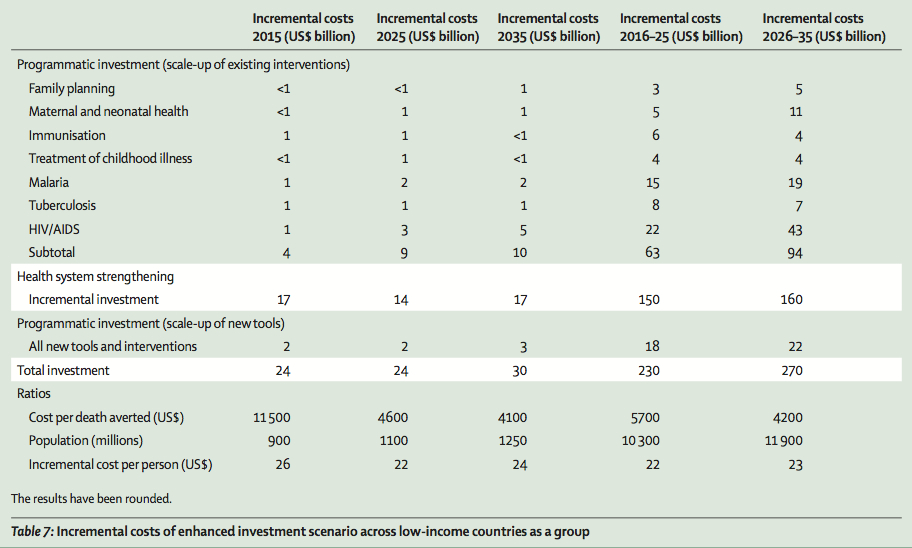
What kinds of investment are necessary? Well, the price tag over the next twenty years is not small – an aggressive investment scenario calls for at least $500 billion to be invested between 2016 and 2035 in low income countries’ health systems. Here’s the breakdown:
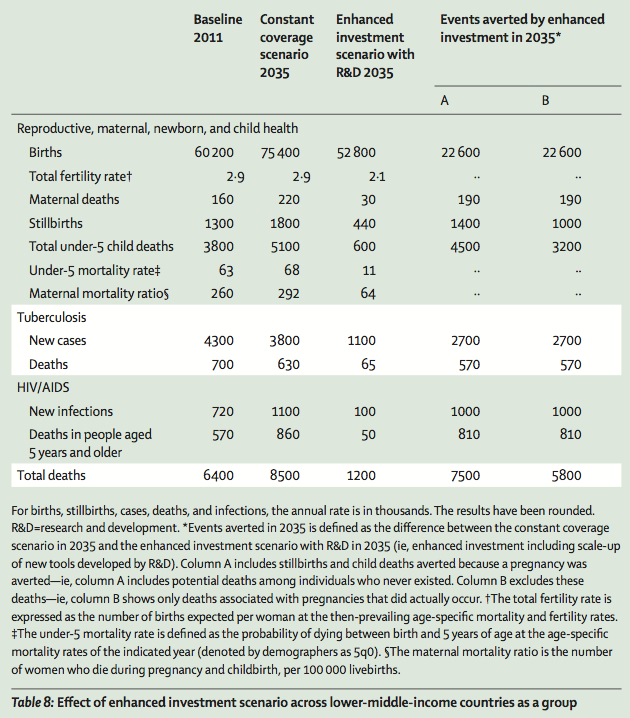
But what types of health outcomes could you conceivably see as a result of that type of aggressive investment in health? Perhaps as many as 7.5 million lives saved across low income countries during that time period:
Fiscal policies (taxation, regulation, etc) are a major lever in controlling non-communicable diseases.
The report advocates for aggressive use of fiscal policies as levers to combat what will be rapidly growing rates of chronic and non-communicable diseases, especially in low income countries. These polices include but aren’t limited to heavily taxing tobacco and other harmful substances as well as reducing subsidies on fossil fuels.
“Progressive universalism” is the most efficient way of achieving financial protection for health programs.
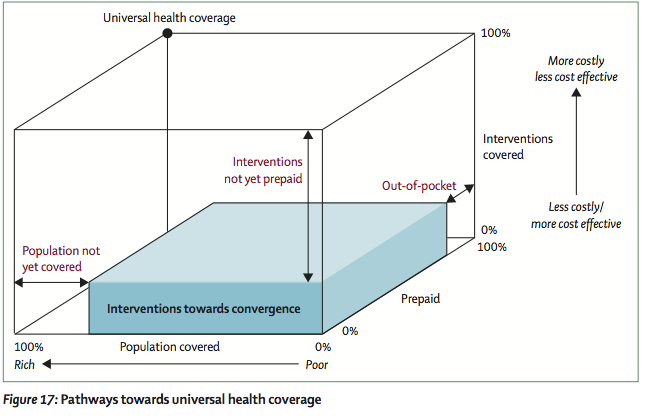
For me, the most striking focus of this report is the extraordinarily pro-poor focus on achieving universal health coverage through two potential pathways that they describe as “progressive universalism.” They conceptualize the process to move toward universal health coverage using the “universal health coverage cube – a way of understanding the trade-offs and choices policy makers must make along the way.
The cube consists of three dimensions: the percentage of the population covered, the percentage of costs pre-paid at the point of service (the rest paid for out of pocket), and the percentage of interventions that are covered by prepaid schemes.
Essentially, if a system has no one covered, none of the real costs associated with clinical interventions are pre-paid, and no interventions are covered through pre-paid schemes, that’s bad and does not approach UHC. You’re in a system that is in the bottom, right, front corner of the cube. Conversely, if people within a health system have all of their costs pre-paid at the point of service, all possible services are covered within the pre-paid scheme, and everyone within a population is covered, then you’ve got universal health coverage.
The report outlines two ways of “moving through the cube.” The first, and ideal strategy, would be to create a publicly financed health insurance system that would cover essential health interventions for entire populations. Basically, using “x, y, and z” coordinates imposed on the cube above, it would mean a large x (population covered) and a large z value (percentage of costs prepaid vs out of pocket), but a relatively small y (percent of all interventions that are covered through the system).
The second feasible strategy would be to provide a larger benefit package, financed through a mix of public and personal resources, from which the poor would be exempt. Basically, a smaller x value, similar z value, and a larger y value.
Potential implications for advocacy strategy?
I’m personally most interested in this report because I think that it provides a viable “stake in the ground” around which nonprofit organizations, civil society, advocacy networks, and ministries of health can mobilize and direct collective effort. It presents an ambitious vision for what could be. It provides the beginnings of a roadmap for how we could plausibly build upon the successes and challenges of the last 20 years in global health and actually make headway in recasting health expenditure from being considered sunk costs to be minimized, and moving towards a commitment of robust investment. And, just maybe, we can even move past the idea of investment and consider health a fundamental human right to be protected as a central component of modern citizenship.
This is, of course, where politics and advocacy come in. Some questions emerge:
- What types of organizations and grassroots campaigns are necessary in high-income countries to create the political space necessary to create the necessary development assistance for health funding streams necessary to see a plan like this enacted?
- What types of organizations and campaigns are necessary in low-income countries to hold their governments and elected officials accountable for adequate public sector investment in health?
- What type of advocacy is necessary to bring the lessons and innovations from low income countries working to pioneer UHC to high income countries, in order to disrupt dysfunctional health systems with massive politically and economically entrenched interests?

Pingback: Live Stream Genius Download Live Stream Genius Download | SEO Zen Bonus
Pingback: good day
Pingback: Oakley Sunglasses Sale
Pingback: it-support
Pingback: mobil
Pingback: osveshchenie dlya ulicy
Pingback: lenty i moduli svetodiodnye
Pingback: ardatov
Pingback: david droste farm bureau insurance 85044
Pingback: Got a question about Social Media? Click here to read answers to your frequently asked questions, courtesy of Ibiza Digital Marketing.
Pingback: magnetic treatment
Pingback: Erotica
Pingback: mlm software plans
Pingback: stampa volantini
Pingback: filme xxx
Pingback: stampa bandiere pubblicitarie
Pingback: Electronics thanksgiving day sales pomotion
Pingback: utsource Thanksgiving sales pomotion
Pingback: legea atractiei
Pingback: cupons
Pingback: Referral Marketing
Pingback: U-Need-A-Cab
Pingback: veterans
Pingback: parenting
Pingback: american veterans aid
Pingback: Free Preventative Maintenance Software
Pingback: Bondage Store
Pingback: agorafobia
Pingback: iso 14001 pisa
Pingback: american veterans aid
Pingback: comunica eficient
Pingback: hair cuttery coupons
Pingback: ohsas 18001 livorno
Pingback: cloudhq
Pingback: Yellow London Taxi
Pingback: Communicate with your audience through content marketing: landing pages, blogs, white papers, ebooks, infographics, images, rack cards and more.
Pingback: Free Preventative Maintenance Software
Pingback: ehic
Pingback: corso primo soccorso grossetocorso rspp Grosseto
Pingback: free coupon
Pingback: dr.kieran ayre
Pingback: hair piece prices
Pingback: PARTY BUS WITH MALE EXOTIC DANCERS
Pingback: hair system factory
Pingback: EXOTIC DANCERS
Pingback: STRIPPERS
Pingback: hair weave machine
Pingback: Home Page
Pingback: best financial planners
Pingback: MALE EXOTIC DANCERS
Pingback: custom stock lace wigs
Pingback: custom hair replacements
Pingback: brc ifs viterbo
Pingback: FEMALE STRIPPERS
Pingback: hair piece prices
Pingback: custom hairpiece
Pingback: volvo bus booking
Pingback: t shirt website
Pingback: Wall canvas
Pingback: Blog
Pingback: womens custom hairpiece
Pingback: www.buyadronezone.com
Pingback: siri android espanol
Pingback: Testimonials
Pingback: Diwali Rangoli Designs
Pingback: Red Diesel Price
Pingback: siri untuk android bahasa indonesia
Pingback: hairpiece-tapes
Pingback: situs poker online
Pingback: Where to buy red diesel fuel
Pingback: HD Diwali Wallpapers
Pingback: Lingerie
Pingback: buy domains online
Pingback: custom stock lace wigs
Pingback: www.ageofbeard.com/beard-oil
Pingback: www.ageofbeard.com
Pingback: pulled neck muscle
Pingback: fashion clothing drop shipping
Pingback: www.ageofbeard.com/beard-kits
Pingback: online marketplace
Pingback: hairpiece adhesives
Pingback: uber eats
Pingback: pain management center
Pingback: remodeling contractors Sherman Oaks
Pingback: UFO Sighting reports
Pingback: Test bank online
Pingback: human hair system
Pingback: Contractors in Los Angeles
Pingback: stock toupees
Pingback: screen printing
Pingback: room addition
Pingback: blogs
Pingback: Zonore 20W Electronic Bug Zapper
Pingback: remodeling contractor Encino
Pingback: chess sets uk
Pingback: m88
Pingback: arrested for conceding 43 goals
Pingback: Web Site
Pingback: chess sets uk
Pingback: Black Seed Oil
Pingback: chess boards
Pingback: chibok girls
Pingback: Click This Link
Pingback: Otopay
Pingback: Alex Garcia for corona city council
Pingback: nationwide home comfort
Pingback: Brazilian bar in Downtown Miami
Pingback: inception
Pingback: astropay al sat
Pingback: nationwide home comfort
Pingback: leather bags
Pingback: cheap women's clothing
Pingback: chanel j12 38mm white
Pingback: top quotes and sayings about Dream
Pingback: top quotes and sayings about Tunnels
Pingback: The Lost Ways
Pingback: steve chan swansea
Pingback: steve chan swansea
Pingback: escort services in delhi
Pingback: hd video surveillance
Pingback: translators
Pingback: Pizzeria washington
Pingback: steve chan swansea
Pingback: steve chan swansea
Pingback: secure website
Pingback: steve chan swansea
Pingback: parenting
Pingback: happy
Pingback: crafts with pine cones
Pingback: steve chan swansea
Pingback: vehicle insurance company
Pingback: remedies
Pingback: online casino
Pingback: the most reliable tow truck company near farmington hills
Pingback: halloween hairdos
Pingback: freelance writing jobs
Pingback: coronacitycouncil
Pingback: snow plowing portland
Pingback: Alex Garcia Corona
Pingback: commercial grounds maintenance
Pingback: valentine gift baskets delivered
Pingback: water softening salt
Pingback: cost of water softeners
Pingback: loft extension london
Pingback: Going Here
Pingback: stroke
Pingback: osteoarthritis
Pingback: online education training
Pingback: side extension london
Pingback: More Bonuses
Pingback: Laughter
Pingback: Pearl debt management
Pingback: muscle building fast
Pingback: Get More Info
Pingback: Conception site Web Algerie
Pingback: Singapore Orchard Tower
Pingback: osteoarthritis
Pingback: steve chan swansea
Pingback: google news
Pingback: Peace Centre Singapore
Pingback: google updates
Pingback: web marketing algerie
Pingback: aura health
Pingback: omega options trading group
Pingback: omega options review
Pingback: back pain traction therapy
Pingback: mp3 music download
Pingback: increase website traffic
Pingback: neck and spine doctor
Pingback: Skin care
Pingback: steve chan swansea
Pingback: earn bitcoins
Pingback: orthopedic doctor ratings
Pingback: increase website traffic
Pingback: steve chan swansea
Pingback: constant back and neck pain
Pingback: women leather gloves
Pingback: vidcon
Pingback: make professional introduction video
Pingback: warm gloves for winter
Pingback: web marketing algerie
Pingback: Lakeisha Riney
Pingback: Fermina Straube
Pingback: bbswaimao
Pingback: We buy houses Las Vegas
Pingback: slot-machine-online
Pingback: Aberdeen House Clearance
Pingback: Jual tanah murah
Pingback: Billboard advertising
Pingback: Versicherungsmakler Stuttgart
Pingback: london underground advertising
Pingback: Jual apartemen
Pingback: Avoid foreclosure in Las Vegas
Pingback: Eyebrows Makeup
Pingback: slot-machine-online.biz
Pingback: nicely dressed
Pingback: slots machines
Pingback: www.slot-machine-online.biz
Pingback: wireless display
Pingback: My Art | MJ Viajes: A Traveling Artist & Foodie
Pingback: best plumber los angeles
Pingback: Plumber Los Angeles California
Pingback: soap making
Pingback: Discover More
Pingback: Click This Link
Pingback: Website
Pingback: Web Site
Pingback: plumber silverlake los angeles
Pingback: wireless display
Pingback: acupuncture
Pingback: watch movies for free
Pingback: Going green
Pingback: delhi escorts
Pingback: China Handys kaufen
Pingback: buy android reviews
Pingback: China Handys Test
Pingback: escort services in dwarka
Pingback: Going green
Pingback: trampoline park Stockton cA
Pingback: vpn
Pingback: Discover More
Pingback: Green living
Pingback: Additional Info
Pingback: skyzone trampoline park Stockton CA
Pingback: casino bonus
Pingback: China Handys kaufen
Pingback: Find Out More
Pingback: locksmith
Pingback: bonus casino
Pingback: Litigation Lawyers
Pingback: Orthodontist Simi Valley
Pingback: locksmiths
Pingback: Aboriginal and Indigenous Lawyers
Pingback: solobonus.com
Pingback: 11 Mortlock Terrace, Port Lincoln SA 5606, Australia
Pingback: solobonus
Pingback: bonus
Pingback: Level Little Collins Street Melbourne. VIC 3000
Pingback: 80 King William Street, Adelaide SA 5000, Australia
Pingback: solo bonus
Pingback: Austin Haworth & Lexon Legal
Pingback: casino bonus
Pingback: Carters Solicitors
Pingback: casin? online
Pingback: Healthcare Lawyers
Pingback: the gioi bong da
Pingback: Commercial Insurance Lawyers
Pingback: solobonus
Pingback: the gioi bong da
Pingback: deck remodeling
Pingback: keo nha cai
Pingback: casino
Pingback: casino bonus
Pingback: ca do bong da
Pingback: visita sito
Pingback: silicon mold
Pingback: personal financial planner
Pingback: cbse schools in thane
Pingback: bong da so
Pingback: Lightroom presets
Pingback: love-you-in-the-dark.tumblr.com/
Pingback: Payday Loan Bukit Batok
Pingback: Click here to get natched to a school today
Pingback: Click here for valuable education resources
Pingback: Photoshop actions
Pingback: Personal Loan Bukit Batok
Pingback: what is nursery admission age for dps school
Pingback: best vacuum cleaners consumer reports
Pingback: best car vacuum to buy
Pingback: best vacuum for carpet
Pingback: one piece 764
Pingback: sports918
Pingback: flat for rent in dubai
Pingback: web proxy
Pingback: tenant screening
Pingback: nha cai uy tin
Pingback: unblocked porn sites
Pingback: link vao 188bet khong bi chan
Pingback: Foreigner Loan in Singapore
Pingback: nha cai 188bet
Pingback: landlord credit checks
Pingback: credit reports
Pingback: nha cai vn
Pingback: coventry cabs
Pingback: nha cai 188bet
Pingback: access website
Pingback: sports918
Pingback: reference checks
Pingback: airport transfers
Pingback: business liability insurance Fort Worth TX 76111
Pingback: Hamptons International
Pingback: best nj restaurants
Pingback: Pre Launch Prestige Fairfield
Pingback: search engine optimization 2014
Pingback: healthcare
Pingback: nj millionaires
Pingback: search engine optimization web design
Pingback: tax preparation Fort Worth
Pingback: sibling love
Pingback: copper wire manufacturing
Pingback: nj porn sites
Pingback: business intelligence
Pingback: Great Wealth Transfer
Pingback: Maternity clothes
Pingback: Frederick Achom
Pingback: mehndi design
Pingback: Discover More Here
Pingback: Achom
Pingback: 7 year sabbatical cycle
Pingback: Check This Out
Pingback: older women looking for younger men
Pingback: silver investment
Pingback: android news update
Pingback: meet older women
Pingback: Sell Your Music Online In Kenya
Pingback: truck towing company
Pingback: web site
Pingback: Kimberli Bockemehl
Pingback: Norbert Hofer Vollkoffer
Pingback: roll back tow truck for sale
Pingback: Krypto1000
Pingback: online logo design
Pingback: indianapolis roofers angie's list
Pingback: cougar dating sites
Pingback: roofing contractors indianapolis Indiana
Pingback: Financial Life Coach
Pingback: bracelet
Pingback: exotic dancers
Pingback: female exotic dancers
Pingback: Vollkoffer Norbert Hofer
Pingback: Behavioral Violence Prevention Certificate
Pingback: Prevention and management of disruptive behavior
Pingback: Financial Advisor
Pingback: order party bus
Pingback: web site
Pingback: male exotic dancers
Pingback: Norbert Hofer Voll Koffer
Pingback: gamecasino.biz
Pingback: sneak a peek at this site
Pingback: poker online terpercaya
Pingback: this content
Pingback: TENNIS & GOLF ACCESSORIES
Pingback: agen poker terbaru
Pingback: take a look at the site here
Pingback: read review
Pingback: click reference
Pingback: redirected here
Pingback: kausoxyla
Pingback: Turbotax Deluxe 2016
Pingback: Showbox app download
Pingback: Python books
Pingback: HipHop
Pingback: jp maroney
Pingback: New Song
Pingback: Turbotax Home & Business 2016
Pingback: New Song
Pingback: responzive llc
Pingback: badges made to order
Pingback: customised badges
Pingback: bespoke badges
Pingback: customised badges
Pingback: JQuery books
Pingback: Showbox for pc
Pingback: custom badges
Pingback: USB/SD Universal Interchangeable Playe
Pingback: Cool Pins
Pingback: 2 Din GPS Car DVD Player
Pingback: Personalized Pins Factory
Pingback: tummy tuck recovery
Pingback: chicago abdominoplasty
Pingback: real estate broker
Pingback: ebook
Pingback: real estate broker
Pingback: 100 organic cotton
Pingback: herz ausschneiden hochzeit
Pingback: free dating website
Pingback: eco friendly clothing labels
Pingback: homes for sale picayune
Pingback: cloud security
Pingback: treatment acne
Pingback: all natural skin treatment
Pingback: online real estate courses
Pingback: Valentus, Valentus Coffee 5k
Pingback: free banner design
Pingback: battery powered lawn mower
Pingback: merry christmas and happy new year
Pingback: Browse torrents
Pingback: electric mowers for sale
Pingback: Valentus Canada 5k
Pingback: Limetorrents
Pingback: happy new year 2017 hd wallpaper
Pingback: alcohol rehab
Pingback: inpatient rehab
Pingback: furnace duct cleaning cost
Pingback: all natural skin treatment
Pingback: dell on linux
Pingback: ven_8086&dev_1502
Pingback: general contractors Encino
Pingback: room addition Los Angeles
Pingback: Khalifa Kush for Sale
Pingback: general contractor Encino
Pingback: kitchen remodeling
Pingback: clogged dryer vent cleaning
Pingback: valentus slim roast coffee 5k
Pingback: kitchen remodeling
Pingback: Roshan A To Z All RingTones
Pingback: remodeling contractors Sherman Oaks
Pingback: construction companies brentwood
Pingback: Crisis Prevention Intervention Certification Online
Pingback: Christian Speakers california
Pingback: duct cleaning coupons
Pingback: Christian Women Speakers california
Pingback: basic arrhythmia certification online
Pingback: MAB Certification Online
Pingback: cna classes inland empire
Pingback: Restorative Nurse Assistant Certification
Pingback: African American Churches in Riverside California
Pingback: construction companies
Pingback: Online medical administrative assistant certification courses
Pingback: Paid Book Reviews
Pingback: Surgical technology certification online
Pingback: EKG Tech Certification Online
Pingback: EKG Tech Certification Online
Pingback: Purchasing Mailboxes
Pingback: maytag washer repair
Pingback: Weekend CNA
Pingback: Phlebotomy technician Online
Pingback: miracle bust amazon
Pingback: miracle bust apex vitality reviews
Pingback: DSD Certification online
Pingback: Medication technician certification online
Pingback: miracle bust apex vitality
Pingback: frigidaire repair
Pingback: Acute care nurse assistant certification online
Pingback: DSD certification in California
Pingback: Home health Aide training Inland Empire
Pingback: daily message
Pingback: burner for stove
Pingback: samsung refrigerator service
Pingback: Debt Free
Pingback: Debt Free
Pingback: drop in stoves
Pingback: Debt Free
Pingback: mypsychicadvice
Pingback: United Debt Counselors
Pingback: Debt Free
Pingback: United Debt Counselors
Pingback: energy efficient dishwasher
Pingback: web site
Pingback: United Debt Counselors
Pingback: Debt Free
Pingback: Reisgids Brugge kopen met stadswandelingen
Pingback: Work from home as an Email Processor today! Click here
Pingback: fantasy football waiver wire
Pingback: Learn how to make money online
Pingback: appliance service unlimited
Pingback: game bai online
Pingback: tips to build your email list subscribers
Pingback: cocaine addiction rehabilitation
Pingback: appliance service seattle
Pingback: small electric range
Pingback: Advertise here for FREE and get your ads seen by Millions! Click here
Pingback: Gas Garena
Pingback: CAPS certified handyman
Pingback: Home modification for seniors
Pingback: dryer window vent
Pingback: finding a rehab centre
Pingback: indoor dryer venting
Pingback: Richardson contractor
Pingback: dryer power vent
Pingback: carpet clarkston
Pingback: laminate flooring installed
Pingback: wholesale carpet
Pingback: Clock Repair Berkley
Pingback: repair pendulum wall clock
Pingback: Sex doll
Pingback: Furniture
Pingback: free logo maker
Pingback: online jobs
Pingback: Amazon Web Services (AWS)
Pingback: online logo design
Pingback: For those who appreciate lasting quality
Pingback: defence work
Pingback: logo maker
Pingback: The latest laser technology in dentistry
Pingback: platform shoes
Pingback: Video online
Pingback: Hossam Habib
Pingback: videohat
Pingback: The latest technology of the world abstract
Pingback: red timberland boots
Pingback: Dryer lint build up
Pingback: heating air conditioning services
Pingback: how do you clean a dryer vent
Pingback: toronto plumbing
Pingback: Dryer installation
Pingback: download anime batch
Pingback: dryer vent cleaning Pleasanton
Pingback: air conditioning offers
Pingback: Dryer vent cleaning lyons
Pingback: isshuukan friends sub indo
Pingback: physical exercise increase blood flow improve psychological disorders
Pingback: gutter cleaning
Pingback: Clean dryer vents
Pingback: tattos
Pingback: dryer air duct
Pingback: how do you clean the dryer vent
Pingback: Indian Funny Prank
Pingback: click tracking tools
Pingback: Long distance movers
Pingback: lr44 battery cell
Pingback: Christmas Greetings Messages
Pingback: Homework Help
Pingback: Bollywood Latest Trailers
Pingback: lr44 battery compatible
Pingback: Domino QQ Online
Pingback: Inspirational Christmas Messages
Pingback: the glades condo
Pingback: click tracking
Pingback: Best air conditioning company Tampa FL
Pingback: free videos
Pingback: pictures
Pingback: negosyo
Pingback: How to get from Prague Airport
Pingback: business tips
Pingback: auto wrecker service
Pingback: website rotator
Pingback: ag13 lr44 battery free shipping
Pingback: flights from sao paulo
Pingback: flights to Toronto from Tehran
Pingback: video free
Pingback: art
Pingback: lifestyle
Pingback: exhibition stand design dubai
Pingback: tow truck insurance
Pingback: urban clothing
Pingback: austin towing companies
Pingback: satta matka
Pingback: Indian Funny GIF Images
Pingback: Jerusalem tours
Pingback: triple a towing
Pingback: Activities
Pingback: Jewish Religious practice
Pingback: Team Building
Pingback: the santorini
Pingback: www.avg.com/retail
Pingback: Bilateral Music
Pingback: hydraulic wheel lift
Pingback: 24/7 tow truck service
Pingback: tow direct
Pingback: nationwide home comfort
Pingback: insurance new car
Pingback: www.avg.com/retail
Pingback: dailybulletin.com
Pingback: Window Tinting Orlando
Pingback: FALKIRK PC REPAIR FALKIRK - PC - REPAIR - FALKIRK
Pingback: gk today pdf free
Pingback: buy business database
Pingback: 4 car rollback tow truck for sale
Pingback: growing marijuana
Pingback: Eclipse sportdrank
Pingback: Women boots
Pingback: FALKIRK ON SITE COMPUTER SUPPORT BUISNESS FALKIRK, ONS-SITE - COMPUTER SUPPORT - BUSINESS - FALKIRK
Pingback: FALKIRK TERMS AND CONDITIONS FALKIRK - TERMS - CONDITIONS - FALKIRK
Pingback: women ankle boots
Pingback: geico claims
Pingback: indoor weed growing
Pingback: washing machine
Pingback: indoor cannabis growing
Pingback: downdraft gas range
Pingback: small electric oven
Pingback: dryer air vent
Pingback: Online clothing store
Pingback: virtual reality for bedtime
Pingback: Poke Toronto
Pingback: tactical flashlight
Pingback: vr headset for iphone apple
Pingback: Discover More
Pingback: www.linkedin.com/hp/update/6205620678515916800
Pingback: vr headset to relax at home
Pingback: Electronic scooter information
Pingback: complete tactical flashlight kit
Pingback: parts appliance
Pingback: dacor cooktops
Pingback: canadian drugstore
Pingback: mehandi designs
Pingback: GEICO REPAIR
Pingback: women ankle boots
Pingback: thigh high women boots
Pingback: GEICO CLAIMS
Pingback: www.smallbusiness.yahoo.com/advisor/post/122538730457/everyone-who-has-ever-typed-lol-in-a-text-message-is
Pingback: All natural
Pingback: www.smallbusiness.yahoo.com/advisor/post/131235542947/what-are-social-signals-and-why-do-you-need-them
Pingback: www.forum.web.com/6-ways-social-media-will-enhance-your-content-marketing/
Pingback: www.smallbusiness.yahoo.com/advisor/post/121141899877/we-all-want-thought-leadership-in-our-respective
Pingback: Tey Por Yee
Pingback: Find Out More
Pingback: www.forum.web.com/6-ways-social-media-will-enhance-your-content-marketing/
Pingback: www.smallbusiness.yahoo.com/advisor/post/121868887977/new-pieces-of-content-are-being-created-and-shared
Pingback: virtual reality for bedtime, watch nightime apps.
Pingback: Tey Por Yee angel investor
Pingback: www.smallbusiness.yahoo.com/advisor/post/122538730457/everyone-who-has-ever-typed-lol-in-a-text-message-is
Pingback: free virtual reality for ages 12 and up
Pingback: Electronic scooters by scoot360
Pingback: electric folding scooter
Pingback: Tey Por Yee green tech
Pingback: complete tactical flashlight kit
Pingback: complete tactical flashlight kit
Pingback: tow truck service warren mi
Pingback: cotton cashmere pants
Pingback: towing company in royal oak
Pingback: top auto insurance companies
Pingback: how to find a decent tow truck
Pingback: Brookwood Towing Service near Birmingham
Pingback: jerr dan rollback
Pingback: tow recovery
Pingback: Daly Towing Services serving Commerce
Pingback: 4x4 wreckers for sale
Pingback: Valley Towing Services
Pingback: truck flatbeds
Pingback: rochester hills emergency roadside service
Pingback: link
Pingback: (248) 817-8434
Pingback: Livernois Towing near Berkley
Pingback: Related Site
Pingback: start a business online
Pingback: Business Headshots NYC
Pingback: Lawyer Headshots NYC
Pingback: Dentist Headshots NYC
Pingback: Doctor Headshots NYC
Pingback: NYCheadshot
Pingback: Web Host
Pingback: NYCheadshot
Pingback: old tow trucks
Pingback: Facebook live Reaction voting
Pingback: directory
Pingback: Automate Posts to Instagram
Pingback: towing t hook
Pingback: Rochester Hills Towing near Downtown Rochester MI
Pingback: Valley Towing Services Waterford
Pingback: how to make money online
Pingback: Free Domain Registration Privacy
Pingback: omar ortez
Pingback: Free Domain Privacy
Pingback: YouTube player for website
Pingback: tow for less
Pingback: wholesale tulle fabric
Pingback: make money blogging
Pingback: Rochester Hills Towing (248) 206-3383
Pingback: tulle spool
Pingback: tow truck in inkster rd
Pingback: bloomfield township emergency roadside service
Pingback: emergency roadside assistance near utica mi
Pingback: Tiverton Towing serving West Bloomfield
Pingback: DNA barcoding
Pingback: (248) 206-3383
Pingback: women pumps
Pingback: Romlus Towing near Westland
Pingback: video game localizaiton services
Pingback: cost of tow truck
Pingback: Insurance
Pingback: quantum brain theory
Pingback: flipkart handbags
Pingback: psicologo pisa
Pingback: long maxi skirts
Pingback: Romulus Towing near Wayne
Pingback: FALKIRK IPAD REPAIR REPAIR FALKIRK - IPAD - REPAIR - FALKIRK
Pingback: quantum brain theory
Pingback: human evolution
Pingback: FALKIRK ABOUT US FALKIRK - ABOUT - REPAIR - FALKIRK
Pingback: Right Now Towing (248) 206-3396
Pingback: Right Now Towing Wixom MI
Pingback: click here
Pingback: Corporate headshots NYC
Pingback: (248) 534-4672
Pingback: quantum brain theory
Pingback: care insurance
Pingback: construction company
Pingback: tow straps with hooks
Pingback: Dover Towing Services serving Ferndale MI
Pingback: repo wheel lift for sale
Pingback: Dover Towing near Downtown Ferndale
Pingback: DNA barcoding
Pingback: DNA barcoding
Pingback: Who unfriended me on facebook
Pingback: catamaran rent Croatia
Pingback: super mario cheats level 7
Pingback: beauty and spa deals in dubai
Pingback: Croatia yacht charter
Pingback: catamaran rent Croatia
Pingback: super mario cheats level 8
Pingback: boat rental Croatia
Pingback: Aberdeenshire Gardening Service
Pingback: Croatia yacht charter
Pingback: Party Dress Womens Shoes Women Pumps Sexy Pointed Toe 11cm High Heels New Fashion Glitter Pump Gold Sliver
Pingback: porn news
Pingback: catamaran charter Croatia
Pingback: Croatia yacht charter
Pingback: catamaran rent Croatia
Pingback: yacht charter Croatia
Pingback: teenvids
Pingback: super mario run cheats level
Pingback: (248) 419-1235
Pingback: Inspriational tshirt
Pingback: addicted to success
Pingback: towing service provider rochester
Pingback: sport t shirt inspiration
Pingback: Croatia yacht charter
Pingback: human evolution
Pingback: 3 inch dryer vent
Pingback: scrap yard
Pingback: how to vent dryer
Pingback: auto wrecker rochester hills
Pingback: t shirt design inspiration site
Pingback: towing service
Pingback: purchase sustanon online
Pingback: hackney taxi
Pingback: ducting supplies
Pingback: Read More Here
Pingback: WEb Design fuer Restaurant
Pingback: Webdesign aus Muenchen
Pingback: Fulton
Pingback: Speisekarten fuer Restaurant
Pingback: Go Here
Pingback: email internet marketing service
Pingback: Flyer fuer Restaurant
Pingback: Poster fuer Restaurant
Pingback: www.drupal.org/u/princetonblay12
Pingback: Web Design aus Muenchen
Pingback: Webdesign aus Muenchen
Pingback: Flyer fuer Restaurant
Pingback: Webdesign aus Muenchen fuer Restaurants und Gastronomie
Pingback: most popular email marketing services
Pingback: Flyer fuer Restaurant
Pingback: Social Media Marketing aus Muenchen
Pingback: Webdesign fuer Restaurants
Pingback: workout clothing
Pingback: Cape Coral home builder
Pingback: inspiration t-shirts
Pingback: how to meet women
Pingback: e marketing services
Pingback: Gwinnett
Pingback: New construction Cape Coral
Pingback: Fitness
Pingback: New construction Cape Coral
Pingback: Cape Coral model Home
Pingback: New construction Cape Coral
Pingback: ottawa towing
Pingback: lift pickup truck
Pingback: repo wheel lift trucks for sale
Pingback: load hooks
Pingback: lift on truck
Pingback: xxx cam
Pingback: contractor
Pingback: emergency roadside assistance near midtown
Pingback: Bipolar disorder
Pingback: auto insurance agency
Pingback: ar and vr
Pingback: pokerbo
Pingback: Buy 2032 coin battery
Pingback: infiniti dealership columbus ohio
Pingback: Buy cr2032 battery
Pingback: Bipolar
Pingback: paytm
Pingback: southfield townearg company near
Pingback: cheap cr2032 battery
Pingback: cr2032 battery equivalent
Pingback: cheap cr2032 battery
Pingback: Flyer fuer Restaurant
Pingback: kings auto wreckers
Pingback: towing company east english village
Pingback: this business is honest
Pingback: www.switchboard.com/business/details
Pingback: www.merchantcircle.com/foxtail-marketing-los-angeles-ca
Pingback: this company
Pingback: www.bing.com/local/details.aspx?lid=YN873x14957357767126557625
Pingback: www.chamberofcommerce.com/los-angeles-ca/1331574411-foxtail-marketing
Pingback: oakland county tow truck
Pingback: Roth Towing Clawson
Pingback: www.bing.com/local/details.aspx?lid=YN873x14957357767126557625
Pingback: Auto Alley Towing serving Independence Twp
Pingback: www.localpages.com/lpd-bizinfo.php?listId=40824539&for=business&type=lpd
Pingback: Air conditioning repair Clearwater FL
Pingback: www.local.com/business/details/yx/los-angeles-ca/foxtail-marketing-2839799/
Pingback: www.merchantcircle.com/foxtail-marketing-los-angeles-ca
Pingback: Auto Alley Towing near Rochester
Pingback: tow truck service in waterford twp
Pingback: auto wrecker service in clawson mi
Pingback: towing company in VOA pontiac
Pingback: air conditioning companies Clearwater FL
Pingback: tow trucks in the area
Pingback: Wellington Towing
Pingback: what are tow hooks
Pingback: Brookwood Towing Service
Pingback: towing near downtown pontiac
Pingback: air conditioning Clearwater FL
Pingback: Visit This Link
Pingback: transfer domain
Pingback: car spare parts
Pingback: slimming
Pingback: www.switchboard.com/business/details
Pingback: car insurance
Pingback: probiotics
Pingback: Know more about Residential Solar packages
Pingback: Recommended Reading
Pingback: Pre-owned Certified Rolex
Pingback: Rolex airking for sale
Pingback: rolex for young man
Pingback: Get the facts
Pingback: Livernois Towing near Birmingham
Pingback: Livernois Towing
Pingback: rolex where to buy
Pingback: rolex with leather band
Pingback: Dedicated IP
Pingback: top songs
Pingback: Continue
Pingback: Video songs
Pingback: old bangla songs
Pingback: quickbooks help
Pingback: Clicking Here
Pingback: Walter Sandy
Pingback: do you agree
Pingback: Moshe Dudai MD
Pingback: seo
Pingback: joint and flexibility
Pingback: steve chan ibm
Pingback: Basketball Shooting Drills
Pingback: Refer to This Web Page
Pingback: Moshe Dudai MD
Pingback: Basketball Equipment Bag
Pingback: Visit This Website
Pingback: Moshe Dudai MD
Pingback: The Best Basketball Gym Bag
Pingback: alcoholic neuropathy
Pingback: UAE
Pingback: Hookah Muenchen
Pingback: Shisha Schwabing
Pingback: 2016 Newest Shoes Women Genuine Leather Women Pumps Thick High Heels Party Wedding Shoes Platform Pump Shoes Plus Size 34-43
Pingback: buy indie music
Pingback: 2016 Newest Shoes Women Genuine Leather Women Pumps Thick High Heels Party Wedding Shoes Platform Pump Shoes Plus Size 34-43
Pingback: Check Out These Helpful Tips
Pingback: Bee Bastien
Pingback: Elegant Women Shoes Designer Pointed Toe Mid Heels Women Pumps Shoes 2016 New Design Fashion Unique Color Office Pumps
Pingback: Shisha in Schwabing
Pingback: Shisha Party
Pingback: fake oakley sunglasses
Pingback: Gulf Elite
Pingback: Mekong day tours
Pingback: Women high heels prom wedding shoes lady crystal platforms silver Glitter rhinestone bridal shoes thin heel party pump
Pingback: badminton coach
Pingback: Mekong Vietnam Tour
Pingback: Unlocked Cell Phones
Pingback: Loslandifen brand new women pumps Med heels shoes woman party wedding dress OL solid Flock ladies pointed toe stiletto shoe
Pingback: Spring summer new fashion sexy women pumps peep toe wedges platforms high heels sandals shoes woman buckle 35-42 loslandifen
Pingback: Sherryl Whitenack
Pingback: Classic Sexy Pointed Toe High Heels Women Pumps Shoes Faux snake Spring Brand Wedding Pumps Big Size 35-42 5 Color 302-1Snake
Pingback: LOSLANDIFEN Classic Sexy Pointed Toe High Heels Women Pumps Shoes Spring Wedding Pumps Big Size 35-42 5 MIX GOLD Color 302-1MIX
Pingback: jewelry stores
Pingback: cidp
Pingback: internette bahis oyna
Pingback: Women Pumps sexy women's pointed toe flock leopard 10cm high heel pump 2016 Hottest Fashion Ladies High Heel shoes Women Pump
Pingback: red wine
Pingback: platinum jewellery
Pingback: Tips Clear
Pingback: without corkscrew
Pingback: Versace 19.69 Abbigliamento Sportivo Milano ladies pump 5073 Capretto Nero
Pingback: causes of peripheral neuropathy
Pingback: fine jewelry
Pingback: güvenle casino oyna
Pingback: tempobet bonus
Pingback: kumarhane siteleri
Pingback: bedava kumar oyna
Pingback: alternative pain management
Pingback: youwin bonus
Pingback: güvenle bahis oyna
Pingback: Christian Silver
Pingback: Terry Sacka AAMS
Pingback: Rodo ladies pump S7963 443 900
Pingback: precious metals investing
Pingback: Sebastian Milano ladies pump S1832 PAGLIA NATURALE+VERN
Pingback: Versace 19.69 Abbigliamento Sportivo Milano ladies pump K730 PITONE 215
Pingback: online casino
Pingback: 2015 Jubilee
Pingback: The latest medical technology
Pingback: betboo bahis sitesi
Pingback: christmas gifts for kids 2016
Pingback: Ideas intensive
Pingback: Discover More
Pingback: news Egypt
Pingback: Ideas mental
Pingback: kitchen remodel contractor woodland hills
Pingback: christmas sayings
Pingback: Learn More Here
Pingback: www.terrysacka.com
Pingback: construction companies
Pingback: room addition
Pingback: Contractors in Los Angeles
Pingback: auto insuance
Pingback: tow truck service lincoln park
Pingback: salvage trucks
Pingback: international car insurance
Pingback: new wreckers
Pingback: used auto parts online search
Pingback: tow truck beds
Pingback: what is liability car insurance
Pingback: name of baby
Pingback: basketball drills for high school
Pingback: small trucks for sale
Pingback: make money online
Pingback: baby names 2013
Pingback: baby boy names
Pingback: how to make easy money
Pingback: basketball drills for middle school
Pingback: conscious mind control
Pingback: business growth
Pingback: Business Blogging
Pingback: alternative medicine
Pingback: basketball drills for middle school
Pingback: Anal Video Free
Pingback: NRP Certification online
Pingback: Home improvement Minneapolis
Pingback: Lottery
Pingback: laser for nail fungus
Pingback: steve chan ibm
Pingback: green nail fungus
Pingback: beds
Pingback: Best Online Lottery Reviews
Pingback: software development in dubai
Pingback: Tub Surround
Pingback: painting contractor in san antonio
Pingback: basketball training drills
Pingback: steve chan ibm
Pingback: Wheel-in showers
Pingback: software development in dubai
Pingback: san antonio interior residential house painting
Pingback: Lawyer Headshots NYC
Pingback: steve chan ibm
Pingback: steve chan ibm
Pingback: san antonio residential painter
Pingback: steve chan ibm
Pingback: Corporate Headshots NYC
Pingback: Corporate Headshots NYC
Pingback: steve chan ibm
Pingback: water softener water usage
Pingback: Lawyer Headshots NYC
Pingback: Dental Headshots NYC
Pingback: Lawyer Headshots NYC
Pingback: NYC Headshot
Pingback: Dental Headshots NYC
Pingback: New York City Headshot
Pingback: NYC Headshot
Pingback: Bath Remodel
Pingback: alarm and cctv
Pingback: domestic cctv installation
Pingback: faux leather pants for men
Pingback: domestic cctv installation
Pingback: security burglar alarms
Pingback: womens spandex leggings
Pingback: emergency roadside assistance hazel park mi
Pingback: steve chan ibm
Pingback: nice flip flops for men
Pingback: used rollback bed for sale
Pingback: Southlake Title Insurance
Pingback: auto parte
Pingback: tow truck in taylor
Pingback: youth basketball drills
Pingback: steve chan ibm
Pingback: Homes for Sale in Haltom City
Pingback: boston edison valued community member of
Pingback: Home Business Opportunity
Pingback: news pike
Pingback: basketball for beginners
Pingback: news Tula
Pingback: towing east english village
Pingback: Justinbet casino
Pingback: new real estate listings
Pingback: casinometropol canlı casino
Pingback: Casino Bonus Codes
Pingback: affordable pool screen sarasota
Pingback: sites for homes for sale
Pingback: bets10 bahis
Pingback: house for sale at
Pingback: latest technology coal gasification
Pingback: forvetbet canlı bahis
Pingback: superbetin casino
Pingback: casinomaxi giriş
Pingback: vehicle recovery
Pingback: betboo giriş
Pingback: hiperbet
Pingback: tempobet bahis
Pingback: matrixbet
Pingback: dubai restaurants
Pingback: shopping in dubai
Pingback: air conditioning
Pingback: Air Cleaner
Pingback: POOL Heater
Pingback: hvac air condition
Pingback: air conditioning
Pingback: Merry Christmas Clip art
Pingback: appliance repair Lancaster Texas
Pingback: appliance repair Dallas Texas
Pingback: rideshare app
Pingback: Arlington appliance repair
Pingback: Arlington Texas appliance repair
Pingback: Dallas appliance repair service
Pingback: appliance repair service Rowlett Texas
Pingback: uber
Pingback: Christmas Sayings 2016
Pingback: Arlington appliance repair
Pingback: ride sharing app
Pingback: funny xmas greetings
Pingback: Miami sightseeing
Pingback: Nynashamn Stadhjalp
Pingback: tow dolly for sale
Pingback: best the plumber los angeles
Pingback: what is comprehensive insurance coverage
Pingback: examen cdl
Pingback: nynas mobelformedling
Pingback: black lace prom dress
Pingback: Miami Everglades tour
Pingback: Miami sightseeing tours
Pingback: examen cdl en espanol florida
Pingback: Dodsbo nynashamn
Pingback: wünsche weihnachten
Pingback: pool plumber los angeles
Pingback: Dubai Sightseeing Boat Tour
Pingback: conocimientos generales examen cdl
Pingback: nationwide home comfort
Pingback: Learn
Pingback: STEVE MADDEN
Pingback: Dubai Sightseeing Boat Tour
Pingback: Dubai Sightseeing Boat Tour
Pingback: Learn
Pingback: borse mia bag
Pingback: Plumber Los Angeles
Pingback: nationwide home comfort
Pingback: Look At This
Pingback: Visit Website
Pingback: Get the facts
Pingback: smoothy weight loss
Pingback: weightloss
Pingback: cleaning a rug
Pingback: drying carpet
Pingback: 6 week shred
Pingback: ukevents
Pingback: eventfinder
Pingback: iphone hülle bedrucken lassen günstig iphone case selbst gestalten günstig hülle für iphone beste iphone hülle handyhülle foto iphone Gucci iphone 7 hüllen
Pingback: jewelery repair troy
Pingback: cheap diamonds online
Pingback: 412 in 1 board Game Elf multigame JAMMA pcb
Pingback: website design
Pingback: uploadevent
Pingback: louis vuitton tasche gefälscht online kaufen louis vuitton tasche preise deutschland echte louis vuitton taschen kaufen herren tasche louis vuitton preise louis vuitton taschen M11530 Braun Louis Vuitton Louis Vuitton Frau
Pingback: 161 in 1 board MVS NEO GEO multigame JAMMA pcb
Pingback: 19 in 1 pcb iCade Manual | Instructions
Pingback: iphone hülle kaufen iphone hülle gestalten hülle für iphone iphone gummihülle iphone hülle bedrucken lassen günstig chanel iphone 6s hüllen
Pingback: face wart
Pingback: medicine to remove warts
Pingback: get a vehicle history report free
Pingback: taylor felice nyc
Pingback: www.mypsychicadvice.com/
Pingback: taylor felice nyc
Pingback: taylor felice nyc
Pingback: check a vehicle history for free
Pingback: taylor felice nyc
Pingback: taylor felice
Pingback: taylor felice nyc
Pingback: system integration
Pingback: control system maintenance
Pingback: treating warts
Pingback: paykasa
Pingback: vin check stolen
Pingback: This Site
Pingback: paykasa
Pingback: Homepage
Pingback: std warts
Pingback: Read More Here
Pingback: paykasa
Pingback: wart on knee
Pingback: seattle carpet cleaning
Pingback: taylor felice
Pingback: taylor felice
Pingback: Diamond Wholesalers Madison Heights
Pingback: book flight
Pingback: control
Pingback: buy lr41 battery
Pingback: Limousines
Pingback: enterprise billing system
Pingback: cheap ag3 battery
Pingback: billing service
Pingback: buy lr41 battery
Pingback: billing as a service
Pingback: buy ag3 battery
Pingback: robert
Pingback: dryer outside vent
Pingback: air cyclone
Pingback: rose bay plumbing sydney
Pingback: free logo services
Pingback: best viagra
Pingback: air vent for dryer
Pingback: free logo online
Pingback: indoor gas dryer vent
Pingback: hookers in burnaby
Pingback: dryer roof vents
Pingback: rooftop dryer vent
Pingback: dryer vents cleaning
Pingback: vent pipe
Pingback: learn more about towing here
Pingback: collision insurance coverage
Pingback: free logo generator
Pingback: rain gutter cleaning
Pingback: auto wrecker near indian village
Pingback: towing eastpointe
Pingback: towing company in harper woods
Pingback: ud tow trucks for sale
Pingback: sterling tow trucks
Pingback: ttps://drive.google.com/open?id=1YRCuM3qbXotJS8__xigVECX0q-o&usp=sharing
Pingback: what is covered under comprehensive auto insurance
Pingback: tow trucks video
Pingback: towing service in detroit mi
Pingback: best fitness tracker reviews
Pingback: best headphones for under 100
Pingback: click to find out more
Pingback: Church Apps I Custom Church Apps
Pingback: Rupert Mosey
Pingback: Custom Church Apps I Church Apps
Pingback: Iphone case
Pingback: find jobs online
Pingback: he said
Pingback: navigate to this website
Pingback: retails jobs
Pingback: Custom Custom App Information
Pingback: blog about esports
Pingback: hot news from gaming industry
Pingback: we know news in gaming first
Pingback: aromasuperstore herbal blends
Pingback: Alcohol Intervention
Pingback: aromasuperstore coupon codes
Pingback: aromasuperstore coupons
Pingback: Visit This Link
Pingback: excel macro training courses london
Pingback: Going Here
Pingback: aromasuperstore scam
Pingback: aromasuperstore buy online
Pingback: Contact Republican Party of Cameroon
Pingback: billy lerner
Pingback: aromasuperstore aroma oils
Pingback: Republican Party of Cameroon Representative
Pingback: billy lerner
Pingback: www.ehomz.ca/Toronto-homes-for-sub-lease/141-Oakdale-Rd/4
Pingback: Travel advice
Pingback: www.ehomz.ca/Mississauga-homes-for-lease/6610-Turner-Valley-Rd/201
Pingback: Web Design Company in Kolkata
Pingback: billy lerner
Pingback: aromasuperstore coupons
Pingback: aromasuperstore scam
Pingback: Donald Trump
Pingback: nyc cheap hotel deals
Pingback: hotels close to denver convention center
Pingback: Visit Your URL
Pingback: 1 year old toys
Pingback: top 10 toys for 3 yr old boy
Pingback: cheap hotel rates new york city
Pingback: next page
Pingback: paris charles de gaulle airport hotel
Pingback: Keyword
Pingback: cruises from port canaveral fl
Pingback: cruises out of san diego
Pingback: Bonuses
Pingback: Kizi
Pingback: 3 year old boy toys
Pingback: trauma therapy emdr
Pingback: adsense
Pingback: target girl toys age 7
Pingback: lazada voucher
Pingback: hotel à cologne
Pingback: facts about emdr
Pingback: social marketing
Pingback: zalora voucher
Pingback: Full movie
Pingback: emdr treatment
Pingback: book cheap hotels in vegas
Pingback: lazada coupon
Pingback: hotel deals for san diego
Pingback: holiday decoration
Pingback: holiday table decorations
Pingback: decorating ideas for the holidays
Pingback: airmoji white
Pingback: Center Pull Towel
Pingback: samsung galaxy s7
Pingback: JRT
Pingback: JRT
Pingback: airmoji black
Pingback: Towel
Pingback: Cleaning Supplies
Pingback: air conditioning service tampa
Pingback: Tampa Fl air conditioning companies
Pingback: Grosshandel für exotische Pflanzenöle und Fette
Pingback: Exotische Kosmetikrohstoffe aus nachhaltiger Wildsammlung
Pingback: Tampa air conditioning companies
Pingback: Amazon raw materials
Pingback: air conditioning companies Tampa FL
Pingback: Tampa air conditioning repair
Pingback: business feature
Pingback: Premium Flats in Pune
Pingback: 506.710929
Pingback: Residential projects in pune
Pingback: 506.710929
Pingback: IRS Dispute Issaquah
Pingback: Premium Flats in Pune
Pingback: tax filing Sammamish
Pingback: How to make a million in nursing
Pingback: freebies
Pingback: best bike store
Pingback: st. joseph
Pingback: bloggers lifestyle
Pingback: faith
Pingback: fat as funk mastering
Pingback: How to make a million in nursing
Pingback: CPA Redmond
Pingback: Christian living
Pingback: hope
Pingback: CPHL MLTC
Pingback: new books
Pingback: Finding hope
Pingback: February 2017 Calendar Template
Pingback: logo generator
Pingback: new books
Pingback: AliExpress akci?
Pingback: online free logo
Pingback: Concrete Mix Design
Pingback: Evanel Axel Tchoutouo Tankio
Pingback: tow truck company in ypsilanti mi
Pingback: auto parts
Pingback: free logo generator
Pingback: 2017 Calendar Cute
Pingback: Evanel Axel
Pingback: AliExpress akci?
Pingback: abaya dress
Pingback: heavy duty wrecker service near me
Pingback: wife in islam
Pingback: muslim marriage pics
Pingback: youwin mobil giris
Pingback: youwin bahis
Pingback: justinbet
Pingback: betboo bonus
Pingback: bets10 canli bahis
Pingback: hiperbet bahis
Pingback: bets10 bonus
Pingback: betboo casino
Pingback: hiperbet
Pingback: towing company near downtown birmingham
Pingback: buy cr123 lithium battery
Pingback: social media agency halifax
Pingback: tow truck service near downtown clawson mi
Pingback: marketing agency
Pingback: How to make a million in Nursing
Pingback: towing service
Pingback: 24hourbatteries
Pingback: Stationary
Pingback: Rajamangala University of Technology Thanyaburi
Pingback: social media holmfirth
Pingback: semi tow truck
Pingback: buy lithium batteries
Pingback: Clinton Twp Towing near Macomb Twp
Pingback: towing company
Pingback: buy cr2032 battery
Pingback: free shipping 24hour batteries
Pingback: compare roadside assistance plans
Pingback: Roth Towing serving Clawson MI
Pingback: this page
Pingback: here
Pingback: cr2032 battery
Pingback: hope
Pingback: uon
Pingback: Chicago Locksmith
Pingback: lost
Pingback: plumber in los angeles ca
Pingback: locksmith lost car keys
Pingback: electronic cigarettes
Pingback: car keys made
Pingback: free shipping 24hour batteries
Pingback: plumber los angeles 24 hours
Pingback: 2l76 battery
Pingback: SEO Hero
Pingback: plumber larchmont los angeles
Pingback: 2 million traffic
Pingback: watch cambridge v leeds live streaming
Pingback: CMS web design bangalore
Pingback: wrecker towing service
Pingback: Exchange Bitcoin into real money
Pingback: flatbed for sale
Pingback: backup files
Pingback: website development bangalore
Pingback: forex investment program
Pingback: profitable managed forex accounts
Pingback: used service trucks
Pingback: gu10 5w led bulbs
Pingback: best price led lights
Pingback: cybersecurity education
Pingback: annunci gratis cerco offro lavoro night club
Pingback: auto roadside service
Pingback: this place that services dearborn
Pingback: agenzia offre lavoro night club
Pingback: drink maple
Pingback: ??????? ? ??? ??
Pingback: towtruck
Pingback: a&m auto wreckers
Pingback: impresario cerco figurante sala lavoro night club roberto
Pingback: tow truck service provider in eastpointe
Pingback: family insurance coverage
Pingback: offro lavoro night club ragazza immagine figurante sala hostess
Pingback: motorcycle insurance rates
Pingback: mapleade beverage company
Pingback: mapleade
Pingback: maple water
Pingback: Mesa Garage Doors
Pingback: ???????? ????????
Pingback: www.terrysacka.com
Pingback: Christian Gold
Pingback: Top and Best in SEO Industry
Pingback: Mesa Garage Doors
Pingback: Gold experts
Pingback: ???????? ????????
Pingback: Cornerstone Asset Metals
Pingback: Tampa air conditioning companies
Pingback: adult webcams
Pingback: ?????? ????? ?????????? ? ?????
Pingback: Mesa Garage Doors
Pingback: Hvac Tampa FL
Pingback: Learn How To Make Money Fast
Pingback: Best air conditioning company Tampa FL
Pingback: Make Money with our eBooks
Pingback: tree service contractors indianapolis
Pingback: Tree removal indianapolis
Pingback: îñâåùåíèå îôèñà ñâåòîäèîäíîå
Pingback: rangers movie
Pingback: domain logo
Pingback: ñòàáèëèçàòîð íàïðÿæåíèÿ 12 âîëüò äëÿ ñâåòîäèîäîâ êóïèòü
Pingback: Make Money with our eBooks
Pingback: Best PGDM Colleges for Placement
Pingback: EZ Battery Reconditioning
Pingback: find a domain name
Pingback: Fee Structure of PGDM Colleges in Delhi
Pingback: How to Earn $50-$100 Daily from Affiliate Marketing
Pingback: Young Living Oils For Families
Pingback: ÑÑÓ-520
Pingback: a-1 duct cleaning
Pingback: cloudhq
Pingback: how to seo
Pingback: South London wedding videographer
Pingback: êàê âûñåëèòü èç êâàðòèðû ãäå äîëÿ â ïðàâå?
Pingback: online research paper publication New York
Pingback: Jewish wedding videographer in UK
Pingback: Sky-230-33308-lauderdale_by_the_sea
Pingback: linteater dryer vent cleaning system
Pingback: Ãäå âåðíóòü äîëã âî ñíå?
Pingback: Riva-Fort-Lauderdale-33304-fort_lauderdale
Pingback: seo information USA
Pingback: Social networking
Pingback: organic seo USA
Pingback: Êàê ïîäàòü èñê ïî 627 ñòàòüå ÃÊ ÐÔ?
Pingback: USA website seo services
Pingback: dryer vent window
Pingback: read what he said
Pingback: Discover More Here
Pingback: Как найти должника гпк
Pingback: click this site
Pingback: why not look here
Pingback: a fantastic read
Pingback: Check This Out
Pingback: Learn More Here
Pingback: Website
Pingback: try this out
Pingback: navigate to this web-site
Pingback: try this website
Pingback: interior designers in chennai ksquare
Pingback: news
Pingback: you could try these out
Pingback: navigate to this site
Pingback: my sources
Pingback: recruitment marketing
Pingback: art of Achraf Touloub
Pingback: futurenet scam
Pingback: prevent hair loss
Pingback: Read More
Pingback: Clicking Here
Pingback: social media marketing for recruitment
Pingback: art
Pingback: This Site
Pingback: art of Achraf Touloub
Pingback: recruitment marketing
Pingback: Full Report
Pingback: Resources
Pingback: Bets10 Giriş
Pingback: Real Estate For Sale in Colleyville - 4105 Lombardy Court
Pingback: Thera Cane
Pingback: sterling silver chain
Pingback: Tempobet Giriş
Pingback: paykasa
Pingback: Best Theracane
Pingback: Youwin Canlı Bahis
Pingback: Best Theracane
Pingback: casinomilyon giriş
Pingback: Treat Sciatica Now Review: A Must-Have Book For All Sciatica Suffers
Pingback: 4504 Alexandra Drive -0 Colleyville TX -0 FOR SALE
Pingback: Young Living Oils
Pingback: Betboo Canlı Bahis
Pingback: meatballs with spaghetti USA
Pingback: USA homemade spaghetti
Pingback: New York Broadway Shows
Pingback: USA ravioli fresh
Pingback: festival
Pingback: EKG exam prep
Pingback: cheap removal companies
Pingback: surrealflix Facebook
Pingback: Oliver
Pingback: authentic italian restaurants
Pingback: maker
Pingback: cheap removals
Pingback: hot to grow medical cannabis
Pingback: NHA EKG Practice Questions
Pingback: removals Huddersfield
Pingback: photographer
Pingback: casinodunya casino
Pingback: Aberdeen & Shire Group
Pingback: legal to grow cannabis
Pingback: Best Survival Knife Ever
Pingback: Read More
Pingback: Wilderness Survival Knife
Pingback: oliver pooley
Pingback: Learn More Here
Pingback: Best Survival Knife Brand
Pingback: storage huddersfield
Pingback: OP Film And Photography Facebook
Pingback: huddersfield storage
Pingback: Get the facts
Pingback: self storage in huddersfield
Pingback: Learn More Here
Pingback: ecig gx350
Pingback: Personal Training in Frankfurt
Pingback: Donald Trump religious views book
Pingback: county dubuque
Pingback: Roofing Contractors Avon Indiana
Pingback: Fitness und Performance
Pingback: city new meadows adams
Pingback: agen sbobet online
Pingback: Health und Wellbeing
Pingback: donald trump Christianity
Pingback: pork
Pingback: satta king
Pingback: Avon Family Roofing Contractors Indianapolis
Pingback: traffic exchange
Pingback: township butman
Pingback: Ettore Montanaro
Pingback: tile roof repair indianapolis
Pingback: free auto traffic exchange
Pingback: Kiss
Pingback: Beauty Salon
Pingback: Wall decals
Pingback: Davina Martinez Credit Repair Forbes Financia
Pingback: Dresses Online
Pingback: Beautiful
Pingback: computer repair port richey fl
Pingback: nasenkorrektur
Pingback: mac-mail signature
Pingback: residential air conditioner repair
Pingback: Gown
Pingback: e-aadhar
Pingback: about hvac
Pingback: aadhar card status by name
Pingback: Eye Brows
Pingback: Parks in Stockton CA
Pingback: Political Satire
Pingback: Wedding Dresses
Pingback: trampoline parks Stockton cA
Pingback: how to clean the dryer vent
Pingback: Satire News Sites
Pingback: Satire News Articles
Pingback: Debt settlement
Pingback: hedge fund incubator
Pingback: Here are the KeyWords one per line
Pingback: University of Arizona Student Lawyer
Pingback: Pick & Pack Fulfillment
Pingback: Custom USB Thumb drives
Pingback: DVD Replication
Pingback: Ladies
Pingback: àíàëüíûå ðîëèêè ñêà÷àòü
Pingback: leads for business
Pingback: Summer Dresses
Pingback: Uber Discount Code
Pingback: ðóññêèå ïðîñòèòóòêè êàìåðà
Pingback: Lip Colour
Pingback: àíàëüíûé èíöåñò âèäåî
Pingback: pe bible forums
Pingback: ðóññêîå ïîðíî áîëüøîé àíàë
Pingback: ðóññêóþ øëþõó ñêà÷àòü
Pingback: what is cloudhq
Pingback: Free Uber
Pingback: free porn proxy
Pingback: æåíñêèé àíàëüíûé ñåêñ
Pingback: More Info
Pingback: òðàõàþò àíàëüíî
Pingback: Airbnb Credit
Pingback: more helpful hints
Pingback: àíàë áåç ðóê
Pingback: áëÿòü ìîêðàÿ è êðè÷àùàÿ
Pingback: redtube proxy
Pingback: åáëî ôèëüì
Pingback: òðàõàåò ñïÿùóþ îíëàéí
Pingback: åáàí âê
Pingback: Customized t-shirts
Pingback: VRS
Pingback: pickup ??
Pingback: Get the facts
Pingback: SATTA MATKA
Pingback: détartrage canalisation nice
Pingback: Womens Shorts
Pingback: Visit This Link
Pingback: áåñïëàòíîå ïîðíî àíàë ãåè
Pingback: æìæ àíàë
Pingback: ñìîòðåòü áåñïëàòíî ïîðíî áåç àíàëà
Pingback: Goziyan.com
Pingback: ðóññêèé àíàë äîìàøêà
Pingback: LED PANEL TROUFFER
Pingback: Technorotic.com
Pingback: Sheffieldschool.net
Pingback: àíàëüíàÿ äåâóøêà ëþáèò
Pingback: Get the facts
Pingback: LED EXIT LIGHT RECESSED
Pingback: Read Full Article
Pingback: kayak fishing charter delray beach
Pingback: christian dating
Pingback: ñâåòîäèîäíàÿ ëàìïà Ò8 600 ìì 4000-5000K IP47 G13
Pingback: Get More Info
Pingback: ñâåòîäèîäíàÿ ëàìïà Ò8 600ìì 5000-6000K IP50 ìîñêâà
Pingback: ñâåòîäèîäíàÿ ëàìïà Ò8 60 ñì 5000-6000K IP46 ñ öîêîëåì G13
Pingback: cream hn
Pingback: obat kuat pria
Pingback: agen judi bola
Pingback: êóïèòü Àíàëîã ëþìèíèñöåíòíûõ ñâåòîäèîäíûå ëàìïû Ò8 22 Âò 5000 Ëþìåí LM
Pingback: ñâåòîäèîäíàÿ ëàìïà Ò8 600ìì òåïëî áåëûé ñâåò IP42 ðåôëåííàÿ
Pingback: êóïèòü Ñâåòîäèîäíûå ñâåòîäèîäíûå ëàìïû Ò8 20 Âò 5500 Ëþìåí LM
Pingback: 120ml eliquid
Pingback: herp alpert
Pingback: 120ml e juice
Pingback: ejuice
Pingback: 120ml e liquid
Pingback: learn to play guitar
Pingback: AC repair Tampa FL
Pingback: stable lift foundation repair san antonio
Pingback: AC repair Tampa
Pingback: Cable and bracing Grand Rapids MI
Pingback: buy lr44 battery
Pingback: tshirts
Pingback: send email later
Pingback: natural cures herpes
Pingback: sim only
Pingback: l1325 battery compatible
Pingback: herpes lips symptoms
Pingback: stable lift foundation repair san antonio
Pingback: Tree trimmimg and pruning Grand Rapids MI
Pingback: UK hook black
Pingback: weight loss pills
Pingback: forex
Pingback: best appetite suppressant pills
Pingback: mg road escorts
Pingback: financial planner
Pingback: ayurvedic spa bangalore
Pingback: best beard oils
Pingback: Dryer repair Rocky Point
Pingback: dryer hood vent
Pingback: Dryer Vent Repair East Hampton
Pingback: hvac repair reviews
Pingback: Valuemags
Pingback: John Ferguson
Pingback: cleaning dryer vent
Pingback: indianapolis roofing permit
Pingback: how do you clean out a dryer vent
Pingback: residential roofing companies indianapolis
Pingback: Dryer Vent Repair
Pingback: dryer eave vent
Pingback: Tree Removal Service Grand Rapids Michigan
Pingback: dryer vent cap
Pingback: author stephen willis
Pingback: www.blogcatalog.com/category/business-tech/finance/
Pingback: ARCHITECTURE
Pingback: www.blogcatalog.com/category/business-tech/law/
Pingback: www.blogcatalog.com/
Pingback: www.blogcatalog.com/category/entertainment/movies-tv/
Pingback: www.blogcatalog.com/category/sports-recreation/
Pingback: www.blogcatalog.com/category/sports-recreation/football/
Pingback: www.blogcatalog.com/category/living-leisure/self/
Pingback: www.blogcatalog.com/category/living-leisure/wedding/
Pingback: www.blogcatalog.com/category/living-leisure/home/
Pingback: Cleaner Brooklyn
Pingback: home cleaning new york
Pingback: recommended reading
Pingback: find more info
Pingback: atlanta roofing and remodeling pro
Pingback: used parts for nizzan
Pingback: anthony picone
Pingback: roofer atlanta
Pingback: atlanta south roofing and construction
Pingback: Natural Supplement
Pingback: kapil matka
Pingback: Airbnb UK
Pingback: www.blogcatalog.com/category/living-leisure/pets-animals/
Pingback: kara promise lyric
Pingback: www.blogcatalog.com/category/art/art-art/
Pingback: www.blogcatalog.com/category/business-tech/tech/
Pingback: www.blogcatalog.com/category/news/medical/
Pingback: Airbnb Promo code
Pingback: lightweight sleeping bag backpacking
Pingback: Airbnb Promo code
Pingback: sleep sack camping
Pingback: gynecologist baltimore md
Pingback: Teeth Whitening Kit
Pingback: network marketing
Pingback: mlm business opportunity
Pingback: valentines day background
Pingback: 2cr5 battery replacement
Pingback: best protein powder
Pingback: 2cr5 battery equivalent
Pingback: 2cr5 lithium battery
Pingback: find 2cr5 battery 6v
Pingback: Myrepublic
Pingback: Best Luggage
Pingback: best protein powder
Pingback: data room
Pingback: Best Recliners
Pingback: latest indian startups
Pingback: Best Towel Warmer Reviews
Pingback: startup it companies
Pingback: startup business news
Pingback: Lashawna Holly
Pingback: cheap wedding rings
Pingback: sattamatka
Pingback: vertical jump workout
Pingback: svetodiodnye lampy ?27 35 W 1000 lumen dlya doma
Pingback: Silvia Vanfleet
Pingback: Local Louisville Carpet Cleaners
Pingback: developmental pediatrician Maryland
Pingback: svetodiodnye lampy s cokolem ?27 50 W 500 lumen shar
Pingback: Shirley Milner
Pingback: Dunk workout
Pingback: Android
Pingback: lampa svetodiodnaya ?27 10 W 1500 lumen shar
Pingback: lampa svetodiodnaya ?27 10 W 5000 lumen shar
Pingback: svetodiodnaya lampa cokol ?27 50 W 2000 lumen grusha
Pingback: svetodiodnaya lampa ?27 45 W 3500 lumen shar
Pingback: A-1 Kwik Dry of Louisville
Pingback: svetodiodnye lampy s cokolem ?27 40 W 2000 lumen grusha
Pingback: svetodiodnaya lampa ?27 50 W 2500 lumen dimmiruemye
Pingback: lampy ?27 svetodiodnye 40 W 3500 lumen grusha
Pingback: Paid book reviews
Pingback: lampa svetodiodnaya ?27 cokol 50 W 4000 lumen dimmiruemye
Pingback: LED lampa ?27 45 W 1000 lumen moschnye
Pingback: lampa svetodiodnaya ?27 cokol 20 W 2500 lumen moschnye
Pingback: lampy ?27 svetodiodnye 35 W 3500 lumen moschnye
Pingback: cost of renting a dumpster
Pingback: dumpster roll off
Pingback: orquestas canarias
Pingback: two yard dumpster
Pingback: arthritis in the back
Pingback: phlebotomist training near me
Pingback: stiff neck treatments
Pingback: movie stream,
Pingback: neck cancer
Pingback: Patrick Zarrelli
Pingback: vtc orly
Pingback: reserver etc
Pingback: radio faycan
Pingback: www.cornerstoneassetmetals.com
Pingback: phlebotomist training program near me
Pingback: Website
Pingback: IMF currencies
Pingback: List of top 10 CBSE Schools in Noida
Pingback: Discover More Here
Pingback: boba milk tea
Pingback: khun thai singapore
Pingback: iced milk tea
Pingback: phillipine milk tea
Pingback: Find Out More
Pingback: cars
Pingback: customised pillows
Pingback: seo la
Pingback: pillow made to measure
Pingback: online reputation management
Pingback: pillows
Pingback: bronze media
Pingback: premium pillow
Pingback: affordable pillow
Pingback: best marketing seo
Pingback: enterprise subscription billing
Pingback: billing service
Pingback: satta king
Pingback: energy healing johannesburg
Pingback: boliglan
Pingback: we don't talk anymore mp3 download
Pingback: scio pretoria
Pingback: quantum biofeedback practitioners
Pingback: Best Car Seat 2017 Buyer Reviews Guide
Pingback: Best Baby Monitor 2017 Buyer Reviews Guide
Pingback: Backup email
Pingback: free ebay templates
Pingback: Lan penge
Pingback: san antonio house painters
Pingback: Mongolia Gobi Tours
Pingback: PNR
Pingback: san antonio exterior painting
Pingback: Cloud backup
Pingback: Smart Meter UK
Pingback: Mongolia TV Support
Pingback: mongolia expedition support
Pingback: smart meter questions
Pingback: Mongolia Film
Pingback: Google Chrome extension
Pingback: horse riding in mongolia
Pingback: Mongolia Weekend Trips
Pingback: cloud billing platform
Pingback: Mongolia riding
Pingback: horse trekking in mongolia
Pingback: Abs
Pingback: horse tour mongolia
Pingback: recurring subscription billing software
Pingback: kupit lampa e40 svetodiodnaya 450 W 5000 lumen grusha
Pingback: monthly billing software
Pingback: horse treks mongolia
Pingback: medspa
Pingback: Mongolian Treks
Pingback: lampa svetodiodnaya e40 cokol 500 W 500 lumen ulichnye
Pingback: vaneity
Pingback: webhosting reseller
Pingback: kupit svetodiodnaya lampa cokol e40 500 W 3500 lumen moschnye
Pingback: kupit shar svetodiodnaya lampa e40 3300 Ê analog 200W À60
Pingback: kupit svetodiodnaya lampa e40 450 W 4000 lumen matovye
Pingback: nadezhnye svetodiodnye lampy s cokolem e40 5400 Ê analog 250W samsung kupit
Pingback: shar svetodiodnaya lampa e40 3900 Ê analog 200W filips kupit
Pingback: kupit shar svetodiodnaya lampa e40 4200 Ê analog 100W 12 V
Pingback: lampy svetodiodnye e40 125 W 1500 lumen ulichnye kupit cena
Pingback: kupit LED lampa e40 350 W 500 lumen yarkie
Pingback: Mongolia cultural tours
Pingback: Danya Feltzin
Pingback: social media marketing
Pingback: how to start an ebay business
Pingback: svetodiodnaya lampa cokol e40 450 W 2500 lumen grusha kupit cena
Pingback: air conditioning companies Tampa FL
Pingback: how to wear a cardigan
Pingback: pizzacouponscodes.com
Pingback: kupit lampy e40 svetodiodnye 125 W 3500 lumen shar
Pingback: social media marketing
Pingback: team treehouse review
Pingback: Dominos coupons
Pingback: igrok universitetskiy hokkei v Scha studentcheskiy
Pingback: introduction to java
Pingback: stat igrokom v hokkkeinom lagere in USA studentcheskiy
Pingback: programming in java
Pingback: Canberra Law
Pingback: clients reviews Coins special British Virgin Islands
Pingback: honda canberra
Pingback: igrat hokkeinyi draft in America studentcheskiy
Pingback: women lawyers
Pingback: graphic design canberra
Pingback: Brand Presence Agency
Pingback: android programming for beginners
Pingback: Brand Presence Agency
Pingback: igrat v hokkkeinom lagere in USA platnyi
Pingback: clients reviews COINS buy Canada
Pingback: business for sale australia
Pingback: what to sell on ebay to make money
Pingback: Ryan Hampton
Pingback: virtual office services ACT
Pingback: commercial services
Pingback: BIMETAL COINS sale EXCLUSIVE
Pingback: Feedback COINS order GALLERY
Pingback: why is cashmere so expensive
Pingback: double jogging stroller bike trailer
Pingback: Safe Pass Galway
Pingback: Unborn DNA testing
Pingback: Non invasive prenatal tests
Pingback: Unborn DNA testing
Pingback: Unborn DNA testing
Pingback: Non invasive prenatal tests
Pingback: stolb osvesheniya metallicheskaya 50 metrov
Pingback: led svetodiodnye paneli asd 55w 5500k
Pingback: safer driving
Pingback: Paternity testing
Pingback: svetodiodnye paneli kupit ip40 5500k
Pingback: it support engineer
Pingback: paneli led 600*600 40w 5000-6000k
Pingback: opory osvecheniya aluminievaya 45 VOU
Pingback: opora osvecheniya s dostavkoi 50 OGK
Pingback: Safe Pass Ballinasloe
Pingback: Non invasive prenatal tests
Pingback: Cloud integration
Pingback: Buy Twitch Followers
Pingback: computer installation
Pingback: fat burning foods
Pingback: Manual Handling Course Galway
Pingback: Save Email To Sharepoint
Pingback: Safe Pass Oranmore
Pingback: Member engagement
Pingback: cr2016 battery equivalent
Pingback: badges fast delivery
Pingback: recognition badges
Pingback: Member engagement strategies
Pingback: Medicare advantage
Pingback: construction debris removal
Pingback: waste disposal bin rental
Pingback: watch movie online
Pingback: best buy cr2016 battery
Pingback: cheap cr2016 battery
Pingback: roll off containers for sale
Pingback: cheap cr2016 battery
Pingback: garbage bins rental
Pingback: cpi certification for nurses
Pingback: Lion Medallion Chain
Pingback: enamel badges
Pingback: cpi certification for nurses
Pingback: mab certification online
Pingback: cpi certification for nurses
Pingback: career in pharmacovigilance
Pingback: crisis prevention intervention certification online
Pingback: cpi certification for nurses
Pingback: 100 Mhz Oscilloscopes
Pingback: 400 Khz Oscilloscopes
Pingback: TrueTransition Nipples
Pingback: 600.0 MHz Oscilloscopes
Pingback: big boobs gif
Pingback: ulichnye svetodiodnye projektory zavod 50 W IP65
Pingback: best meal delivery plans miami
Pingback: modafinil online pharmacy
Pingback: crisis prevention intervention certification online
Pingback: paleo diet books
Pingback: svetodiodnye projektory ulichnye PRS 150 W 6500K
Pingback: servicio de cantina en miami
Pingback: svetodiodnye promyshlennye svetilniki sku 80 W IP65
Pingback: ballsucking gif
Pingback: promyshlennye svetodiodnye svetilniki moskva 120 W IP65
Pingback: svetodiodnye projektory konsolnyi zavod 300 W IP66 kupit
Pingback: svetodiodnye ulichnye svetilniki na stolby 80 W IP 66 kupit
Pingback: How to mend a broken heart
Pingback: kupit svetodiodnye svetilniki promyshlennye òà stolby 400 W IP65
Pingback: amoxicillin
Pingback: kupit svetodiodnye ulichnye svetilniki led 150 W 220V
Pingback: Contemporary Beds
Pingback: svetilniki svetodiodnye promyshlennye sku 400 W IP 66 kupit
Pingback: kupit svetilniki svetilniki svetodiodnye na stolby 200 W IP 65
Pingback: Listing Pictures
Pingback: Keller Mortgage Calculator
Pingback: Locksmith Winter ParK FL
Pingback: erotic massage
Pingback: Blog
Pingback: user acceptance testing
Pingback: tantric massage
Pingback: Equity Position
Pingback: De Clutter Your Rooms
Pingback: software testing tools
Pingback: new music
Pingback: indianapolis Indiana roofing permit
Pingback: colacoaster
Pingback: ketogenic diet resource weight loss health
Pingback: Home Loans
Pingback: Date With Destiny
Pingback: Millionaire Mind Intensive
Pingback: indianapolis Indiana roofing contractor reviews
Pingback: How to get over a breakup
Pingback: weight loss petite
Pingback: ayurvedic weight loss
Pingback: london tantric
Pingback: 14 day water fast weight loss
Pingback: weight loss diet plans
Pingback: macbook repair toronto
Pingback: Make money with traffic exchange
Pingback: indianapolis Indiana roofing supply
Pingback: buy phentermine
Pingback: ayurvedic weight loss
Pingback: washer and dryer repair los angeles ca
Pingback: Traffic exchange
Pingback: www.cabinetstogo.com
Pingback: Full Album Download
Pingback: How to eliminate self doubt
Pingback: www.cabinetstogo.com/product-category/bathroom-vanities/all-inclusive-vanities
Pingback: svetodiodnaya lampa cokol å14 30 W 500 lumen dlya doma
Pingback: www.cabinetstogo.com/product-category/kitchen-cabinets/color/grey
Pingback: lampa svetodiodnaya å14 25 W 3500 lumen shar kupit
Pingback: www.cabinetstogo.com/product-category/kitchen-cabinets
Pingback: www.cabinetstogo.com/store/cabinets-los-angeles-ca
Pingback: www.cabinetstogo.com/product-category/kitchen-cabinets/color/black
Pingback: kupit lampa svetodiodnaya å14 40 W 5000 lumen dlya doma
Pingback: How to eliminate self doubt
Pingback: cabinetstogo.com/product-category/kitchen-cabinets
Pingback: Hire IT Contractors
Pingback: Hire the UKs best IT Contractors
Pingback: cabinetstogo.com/product-category/bathroom-vanities/all-inclusive-vanities
Pingback: How to eliminate self doubt
Pingback: moschnye lampy svetodiodnye å14 3900 Ê analog 250Vt À60 v Moskve
Pingback: cabinetstogo.com/product-category/kitchen-cabinets/color/grey
Pingback: cabinetstogo.com/product-category/kitchen-cabinets/style/shaker
Pingback: www.prweb.com/releases/2014/06/prweb11906369.htm
Pingback: Dryer vent cleaning riverside
Pingback: biofeedback therapy
Pingback: dryer exhaust hose
Pingback: Dryer Vent Repair
Pingback: tranquillity scio studio
Pingback: Southeast Motorcycle Hire
Pingback: air conditioner repair reviews
Pingback: Dryer Vent Wizard
Pingback: Aerovironment TurboDock
Pingback: Chargepoint DC Fast Chargers
Pingback: maytag repair
Pingback: library of congress
Pingback: make online money
Pingback: aromasuperstore
Pingback: amazon.com
Pingback: File Tax Return
Pingback: towing service singapore
Pingback: Karpiel Design
Pingback: Loyalty App
Pingback: free casinos online
Pingback: casinos online real money
Pingback: dryer wall vent
Pingback: Loyalty Marketing
Pingback: casino swing
Pingback: refrigerator repair service
Pingback: play real money casino games
Pingback: Web Site
Pingback: Visit This Link
Pingback: www.bestselfdefenseweapons.com/
Pingback: Clicking Here
Pingback: Spiker Carpet and Tile Care of Rockland
Pingback: tree service phoenix arizona
Pingback: Driving school
Pingback: www.bestselfdefenseweapons.com/black-widow-22-caliber-magnum-best-handgun-for-concealed-carry/
Pingback: www.bestselfdefenseweapons.com/black-monkey-fist-paracord-keychain-self-defense-weapon-review/
Pingback: Spiker Carpet and Tile Care of Carmichael
Pingback: dr miami tummy tuck snapchat
Pingback: free dating tips
Pingback: reverse tummy tuck miami
Pingback: www.bestselfdefenseweapons.com/difference-45-acp-45-colt/
Pingback: Grant Management Software
Pingback: www.bestselfdefenseweapons.com/advantages-using-crossdraw-concealed-carry-holsters/
Pingback: dating advice
Pingback: tummy tuck cost miami fl
Pingback: www.doctorslounge.com/index.php/member/371344
Pingback: www.bestselfdefenseweapons.com/choosing-between-a-wooden-vs-aluminum-bat-for-self-defense/
Pingback: www.bestselfdefenseweapons.com/inferno-fury-crossbow-self-defense-weapon-review/
Pingback: Mirta Meza
Pingback: Pennie Emling
Pingback: affordable divorce attorney charlotte
Pingback: experience
Pingback: Dryer vent cleaning Northern Virginia
Pingback: golf signs
Pingback: divorce lawyers charlotte north carolina
Pingback: rain cutter
Pingback: duct pipe
Pingback: golf signage
Pingback: microwave parts
Pingback: premier appliance service
Pingback: anderson service and appliance
Pingback: bosch appliance repair
Pingback: samsung appliances customer service
Pingback: large appliance repair
Pingback: high end resilient flooring singapore
Pingback: tee blocks golf
Pingback: facelift
Pingback: Mr. SEO Hero
Pingback: parquet flooring singapore price
Pingback: svetodiodnye svetilniki konsolnyi na pototlok 50 W IP65 novosti
Pingback: high end resilient flooring singapore
Pingback: skladskie svetodiodnye svetilniki moskva 300 W IP65 novosti
Pingback: How to make a million in nursing
Pingback: earn money from youtube
Pingback: military asvab practice test
Pingback: How to make a million in nursing
Pingback: svetilnikii svetodiodnye promyshlennye moskva 80 W IP65 novosti
Pingback: svetodiodnye promyshlennye svetilniki dlya skladov 350 W IP65 novosti
Pingback: Designer Handbags UK
Pingback: svetodiodnye promyshlennye svetilniki uss 350 W IP65 novosti
Pingback: svetodiodnye promyshlennye svetilniki cena 100 W IP65 novosti
Pingback: svetodiodnye promyshlennye svetilniki òà stolby 400 W IP65 novosti
Pingback: svetodiodnye promyshlennye svetilniki osveshceniya 120 W IP65 novosti
Pingback: svetodiodnye promyshlennye svetilniki osveshceniya 150 W IP65 novosti
Pingback: skladskie svetodiodnye svetilniki cena 50 W IP66 novosti
Pingback: Colorado Senior Portraits
Pingback: Show down at CES 2017
Pingback: Fashion
Pingback: How to make a million in nursing
Pingback: svetodiodnye promyshlennye svetilniki na pototlok 200 W IP65 novosti
Pingback: Clothes
Pingback: hauls
Pingback: Colorado Senior Pictures
Pingback: kenmore appliance repair los angeles
Pingback: estate questions
Pingback: promyshlennye svetodiodnye svetilniki uss 120 W IP66 novosti
Pingback: SSC JE coaching in dehradun
Pingback: svetodiodnye svetilniki promyshlennye na pototlok 100 W IP66 novosti
Pingback: svetodiodnye promyshlennye svetilniki osveshceniya 250 W IP65 novosti
Pingback: goodman appliance repair los angeles
Pingback: Yearbook
Pingback: e coaching in dehradun
Pingback: svetilniki svetodiodnye promyshlennye osveshceniya 150 W IP66 novosti
Pingback: notepad
Pingback: play subway surfers game free
Pingback: como bajar de peso musica wav
Pingback: como bajar de peso en el embarazo
Pingback: notepad
Pingback: More Info
Pingback: Get More Information
Pingback: Find Out More
Pingback: private holidays
Pingback: MASON
Pingback: fransizca sozluk
Pingback: cince sozluk
Pingback: Home for rent Richmond Hill
Pingback: Recieve an Allowance while dating
Pingback: Handyman in Powell OH
Pingback: best stock trading brokers
Pingback: Mississauga homes for sale
Pingback: the language of desire felicity keith scam
Pingback: sita's curse the language of desire pdf download
Pingback: kitchen stove oven
Pingback: Porch lifts
Pingback: best studio monitors
Pingback: frigidaire washing machine repair
Pingback: best midi keyboard
Pingback: handcrafted gemstone jewelry
Pingback: handmade coral necklaces
Pingback: maytag washers
Pingback: ice maker repair
Pingback: the language of desire by felicity keith
Pingback: renewable enviornment
Pingback: Asian Wedding Photographer
Pingback: Age Discrimination Attorney Los Angeles
Pingback: Satta Matka
Pingback: donald trump and the environment
Pingback: vent a dryer
Pingback: Pocket High quality Handbags
Pingback: Wedding Photographer
Pingback: appliance repair verona nj
Pingback: home appliance service
Pingback: super site
Pingback: appliance supplies
Pingback: Wedding Photographer London
Pingback: www.forbes.com/sites/miketempleman/2017/02/21/5-ways-to-nurture-email-subscribers-with-your-blog/#20926b8e1672
Pingback: repair appliance
Pingback: appliance repair salt lake
Pingback: www.forbes.com/sites/miketempleman/2017/02/23/content-marketing-myths-that-businesses-need-to-stop-believing/
Pingback: dishwasher prices
Pingback: www.entrepreneur.com/article/284560
Pingback: traditional moroccan clothing
Pingback: Handyman service in Dublin
Pingback: Wheel in shower Powell Ohio
Pingback: Free MP3
Pingback: Handyman in Powell OH
Pingback: seattle washington classifieds
Pingback: dry carpet shampoo
Pingback: californio classifieds
Pingback: thermador appliances
Pingback: jewelery classifieds
Pingback: Best Headphones for running
Pingback: Luis Salvador Velasquez Rosas
Pingback: neglected website
Pingback: electric dishwashers
Pingback: Compagnie de menage
Pingback: SEO
Pingback: caregiver certification course online
Pingback: seo articles
Pingback: website design
Pingback: whirlpool refrigerator replacement parts
Pingback: brand presence industry
Pingback: caregiver certification online
Pingback: marketing articles
Pingback: Demi Lovato Makeup Tutorial Video
Pingback: marketing mechanics
Pingback: caregiver course online
Pingback: water removal
Pingback: plyometric exercises
Pingback: Vertical jumping workout
Pingback: Huffington Post
Pingback: Jump workout
Pingback: flood damage repair
Pingback: Online Casino Malaysia
Pingback: java tutorials for beginners
Pingback: programming in java
Pingback: water damage las vegas
Pingback: Online SCR888
Pingback: Online Casino Malaysia
Pingback: men watches
Pingback: dry cleaners free pickup
Pingback: best men watches
Pingback: fifa 15
Pingback: ncca
Pingback: Get book reviews
Pingback: jewelry holder
Pingback: caregiver training online
Pingback: tree stump removal cost Indianapolis
Pingback: tree service contractors indianapolis
Pingback: sport watches
Pingback: link meeting in gmail
Pingback: SCR888 Malaysia
Pingback: Buy book reviews online
Pingback: lovelive costume
Pingback: link meeting in gmail
Pingback: Final Fantasy Online Store
Pingback: zakazat novosti v novostnye agentstva uspeshno
Pingback: aluminievye opory kupit 1 metr rossia ot 1000
Pingback: tree service in San Antonio tx
Pingback: budget tree service in san antonio
Pingback: suvenir logo kupit effektivno
Pingback: napisat seo v soc seti v rossii
Pingback: fleshka logo korporativnye nanesti
Pingback: Interior
Pingback: fleshka logos korporativnye uspeshno
Pingback: aluminievye opory kupit 9 metra izgotovitel ot 1000
Pingback: caregiver training course
Pingback: roll off dumpster sizes
Pingback: forex
Pingback: garbage container rental
Pingback: Online casino Malaysia
Pingback: cheap dumpsters for rent
Pingback: Do you need more expression in your life get your own domain ext like firstname.lastname on the new internet now
Pingback: waste roll off containers
Pingback: Get the New internet now download here
Pingback: plumbersmanly.com.au
Pingback: dumpster rental mount vernon
Pingback: dumpster rental rates
Pingback: Online casino Malaysia
Pingback: forex
Pingback: roll off container sizes
Pingback: click this link
Pingback: Knowledge of Football
Pingback: grants for women in ontario
Pingback: calgary small business hiring
Pingback: vivo ipl 2017
Pingback: trade.Berry home page
Pingback: trade.Berry REBATE PLAN TERMS AND CONDITIONS
Pingback: 2017 US Market Crash
Pingback: trade.Berry faq
Pingback: canada govt fund for inventor
Pingback: grants ontario canada
Pingback: how to sell used car parts
Pingback: freightliner flatbed tow truck
Pingback: ontario entrepeneur grants
Pingback: Anchor: Cheap Viagra
Pingback: tow truck 24 hour
Pingback: Online casino Malaysia
Pingback: lawn care estimate form
Pingback: tow all price
Pingback: app for laptop
Pingback: auto wrecker near ecorse
Pingback: Video production Orlando
Pingback: SCR888 Malaysia
Pingback: Video production Orlando
Pingback: orlando video production
Pingback: orlando video production
Pingback: cleaning services Sarasota
Pingback: Blakeview
Pingback: mowers
Pingback: Cricket Betting Tips Free
Pingback: Property Management
Pingback: push lawn mower
Pingback: Pruvit
Pingback: cordless lawn mower
Pingback: orlando video production
Pingback: Ketos
Pingback: electric start lawn mowers
Pingback: face recognition software
Pingback: happy easter 2017 song
Pingback: Ketogenic Diet
Pingback: turnstiles
Pingback: happy easter 2017 greetings
Pingback: Video production Orlando
Pingback: alcoholsim
Pingback: 50 bathroom designs
Pingback: alcoholism information
Pingback: united states
Pingback: iOS News
Pingback: Judi Qiu Qiu Online
Pingback: and
Pingback: Capsa Susun Online
Pingback: auto accident lawyers
Pingback: wet rooms
Pingback: requisition management
Pingback: Avec Modération
Pingback: staffing software
Pingback: Applicant Tracking
Pingback: Mode Sloggi billigt online
Pingback: PS4 vs xbox one
Pingback: Palsvast online
Pingback: traditional chinese male clothing
Pingback: Recruiting Softeware
Pingback: emergency roof repair indianapolis Indiana
Pingback: commercial roofing contractors indianapolis indiana
Pingback: Recruitment software
Pingback: the javier law firm in Chicago IL
Pingback: palm tree removal in phoenix az
Pingback: tree trimming service in phoenix az
Pingback: Budget tree service in Phoenix
Pingback: contact sharing
Pingback: criminal lawyer in chicago illinois
Pingback: DIY Home Security System Expert Reviews
Pingback: freerewards2u
Pingback: DIY Home Security System Expert Reviews
Pingback: The experts in DIY Home Security Reviews
Pingback: Security News Online
Pingback: The experts in DIY Home Security Reviews
Pingback: paket tour hongkong
Pingback: paket liburan
Pingback: liburan
Pingback: DIY Home Security System Expert Reviews
Pingback: The experts in DIY Home Security Reviews
Pingback: DIY Home Security System Expert Reviews
Pingback: The experts in DIY Home Security Reviews
Pingback: cw8gkxtg5w85ecnbey4tbw334rtsd
Pingback: handmade jewelry
Pingback: SecurityNewsOnline
Pingback: Men's jewellery
Pingback: Anniversary gifts for men
Pingback: tips on survival
Pingback: Happiness
Pingback: How to Be Happy
Pingback: Motivational Videos
Pingback: dumpster rental winnetka
Pingback: roll off dumpster rental prices
Pingback: dumpster rental saint clair shores
Pingback: Daily Horoscope
Pingback: disposal bin rental
Pingback: Bed bugs control service
Pingback: Bed bugs removal service
Pingback: Website
Pingback: Read More
Pingback: dhabi company formation services
Pingback: Lee's summit lawyer 816-524-0404
Pingback: This Site
Pingback: cms incentive reward program
Pingback: affordable dumpsters
Pingback: dumpster rental bedford park
Pingback: Aged Care
Pingback: debris removal
Pingback: what does ahip stand for
Pingback: waste containers rental
Pingback: Home Care
Pingback: moving dumpster
Pingback: healthyblue
Pingback: trash containers for rent
Pingback: Fort Worth Non-denominational Church
Pingback: Networking Certification
Pingback: Life.church
Pingback: CCIE R&S training
Pingback: checkmotorcycle
Pingback: disposal bins
Pingback: dumpster rental nashville
Pingback: promotorcheck
Pingback: weblink
Pingback: checkmotorcycle
Pingback: important source
Pingback: click for source
Pingback: here are the findings
Pingback: garbage container rentals
Pingback: national caregiver certification association
Pingback: hard water conditioner
Pingback: caregiver certification practice test
Pingback: yard waste dumpster rental
Pingback: mypsychicadvice
Pingback: water in water softener
Pingback: youtube to mp3 converter
Pingback: national caregiver association
Pingback: paleo meal plan
Pingback: tow truck 24 hour
Pingback: garbage dumpster rental
Pingback: www.mypsychicadvice.com/
Pingback: paleo food
Pingback: UK Plus Size Fashion Dresses
Pingback: auto recycler parts
Pingback: mypsychicadvice
Pingback: vehicle ins
Pingback: ebusiness
Pingback: online marketing
Pingback: hop over to here
Pingback: central park pedicab tours
Pingback: ketone supplements
Pingback: pruvit max
Pingback: appliance repair parts store
Pingback: http:/www.nationalcaregivercertificationassociation.org
Pingback: pruvit max
Pingback: gas dryer repair
Pingback: pruvit keto os
Pingback: public holidays in Dubai 2017
Pingback: paleo recipes
Pingback: marriage certificate in italian legalization procedure
Pingback: postavka svetilniki ulichnye svetodiodnye 220V 10W
Pingback: 2017 ulichnye svetilniki svetodiodnye 220V 10W
Pingback: paleo diet foods
Pingback: keto supplements
Pingback: Dubai Night Life
Pingback: postavka svetilniki ulichnye svetodiodnye IP66 10W
Pingback: Dubai Duty Free
Pingback: fee in Hindi notary procedure
Pingback: stamp in german apostillation service
Pingback: price in Korean legalize service
Pingback: BLOG ABOUT TRANSITION
Pingback: Places to visit in Dubai
Pingback: zakazat s logotipom podarki v mos
Pingback: Wedding Photographer in Kent
Pingback: kupit korporativnye tovary v mos
Pingback: top 10 london wedding photographers
Pingback: EXOTIC DANCERS
Pingback: oplatit prikolnye prezenty v mos
Pingback: MALE EXOTIC DANCERS
Pingback: postavka svetodiodnye svetilniki 24V 250w
Pingback: FEMALE STRIPPERS
Pingback: ORDER STRIPPERS WITH PARTY BUS
Pingback: ORLANDO EXOTIC DANCERS
Pingback: domestic cleaner
Pingback: adipex online
Pingback: MALE EXOTIC DANCERS
Pingback: FEMALE STRIPPERS
Pingback: no fees
Pingback: read more
Pingback: satta matka00000
Pingback: Spotify users
Pingback: Music
Pingback: Spotify users
Pingback: Secure Offshore Hosting
Pingback: Coquina Sands
Pingback: large dumpster
Pingback: Auto Connection Manassas
Pingback: Hosting Without Government Spying
Pingback: dumpster rental las vegas
Pingback: dumper rental
Pingback: roll off containers sizes
Pingback: rent dumpster
Pingback: dumpster cost
Pingback: tow truck service provider near midtown
Pingback: ask
Pingback: Sell Your Home
Pingback: towing a car long distance
Pingback: dirt bin rental
Pingback: Life in Naples Florida
Pingback: Best Realtors in Naples Florida
Pingback: tow dolly for sale
Pingback: emotionally
Pingback: Buy A New Home
Pingback: djarum black us
Pingback: Check Out Your URL
Pingback: buy marlboro cigarettes online
Pingback: More Info
Pingback: Full Report
Pingback: Livid Light Navigator
Pingback: xm95tkdc4t34xkc5t43753vv3
Pingback: Cool Toys
Pingback: OpenLink
Pingback: gratis annonser eskilstuna
Pingback: OpenLink
Pingback: gratis annonser dt
Pingback: OpenLink
Pingback: OpenLink
Pingback: kayak fishing in Florida
Pingback: franchise disclosure documents online
Pingback: kayak fishing tips
Pingback: certified plumbing service
Pingback: OpenLink
Pingback: appliance stores
Pingback: kayak fishing apparel
Pingback: franchise budget template
Pingback: best plumbers
Pingback: samsung appliance repair service
Pingback: samsung appliance repair
Pingback: OpenLink
Pingback: pro appliance service
Pingback: kitchenaid repair
Pingback: how to fix refrigerator
Pingback: OpenLink
Pingback: kruglye tarelki kupit iz farfora v mos
Pingback: tarelochki oplatit iz farfora v mos
Pingback: tarelka zakazat keramika v mos
Pingback: OpenLink
Pingback: OpenLink
Pingback: commercial laundry
Pingback: caregiver certification requirements
Pingback: OpenLink
Pingback: direct insurance roadside assistance
Pingback: caregiver certification training
Pingback: the most reliable tow truck company near melvindale mi
Pingback: insurance for auto
Pingback: kepsar
Pingback: keps
Pingback: ?????? ????
Pingback: Forskolin
Pingback: social media influencers
Pingback: emergency roadside service in downtown detroit
Pingback: vegetarian food blog Singapore
Pingback: rosedale park auto wrecker service in
Pingback: national caregiver certification course
Pingback: rollback flatbed for sale
Pingback: Montgomery air conditioning and heating
Pingback: leather leggings
Pingback: Montgomery air conditioning installation
Pingback: as-easy-as-it-gets-sending-and-withdrawing-money-with-moneymailme
Pingback: free caregiver certification online
Pingback: Heating and cooling contractor Montgomery AL
Pingback: HVAC repair Montgomery
Pingback: Laine Baker
Pingback: consumers-want-banks-understand-better
Pingback: Affordable air conditioning repair Montgomery
Pingback: free-mobile-video-chat-ios-android-users-launched
Pingback: money-mobile-transfers-a-lifeline-in-remote-territories
Pingback: google-play-turns-five-today-happy-birthday
Pingback: moneymailme-becomes-member-global-fintech-association
Pingback: love-your-finances
Pingback: protection tape
Pingback: best juicer under 50
Pingback: brautschmuck grun
Pingback: correx
Pingback: grind and brew coffee maker reviews
Pingback: brautschmuck emmerling
Pingback: wi-fi-passwords-airports-airport-lounges-around-world
Pingback: Eugene fais de la voyance sans poser de question en cabinet
Pingback: Evoyance
Pingback: gig guide
Pingback: Maquestionvoyance.fr est le portail de voyance par excellence
Pingback: Automated Trading systems
Pingback: contact
Pingback: moneymailme-launched-first-collaborative-title-choosing-hero-memoir-rise-africas-first-woman-president
Pingback: play-your-trump-card-the-op-ad
Pingback: power washing service
Pingback: support
Pingback: Backus - Mille Lacs Realty
Pingback: pressure washing service
Pingback: Cosmos - Mille Lacs Realty
Pingback: vigo vessel sink
Pingback: driveway cleaning
Pingback: Women Tattoos
Pingback: Top 10 Lists
Pingback: zero radius sink
Pingback: moneymailme-is-offering-users-a-special-prize
Pingback: love-your-finances
Pingback: loan kl
Pingback: Personal Care Saint Charles
Pingback: 103 3rd Avenue N, Cold Spring, MN 56320 - Mille Lacs Realty
Pingback: pinjaman wang
Pingback: Kookoosh Lake - Mille Lacs Realty
Pingback: loan
Pingback: first time home buyer corona
Pingback: Alzheimers Care Saint Charles
Pingback: Mud Lake - Mille Lacs Realty
Pingback: Wright Lake - Mille Lacs Realty
Pingback: Conan Exiles
Pingback: lower back pain exercises
Pingback: black stainless steel kitchen sink
Pingback: find best plates logo now
Pingback: indianapolis airport parking cost
Pingback: Lindstrom - Mille Lacs Realty
Pingback: hydraulic generators
Pingback: purchase design plates with logo online
Pingback: hyatt regency indianapolis parking
Pingback: pick up original plates with corporate logo online
Pingback: 42784 Highway 47, Isle, MN 56342 - Mille Lacs Realty
Pingback: 3d car parking
Pingback: lottare single bowl granite
Pingback: diesel generators
Pingback: Trinity Lake - Mille Lacs Realty
Pingback: dryer vent brush
Pingback: purchase unique plates with logo or TM in internet
Pingback: Lyendecker Lake - Mille Lacs Realty
Pingback: carpet cleaning at home
Pingback: stainless farmhouse sink
Pingback: air condition duct cleaning
Pingback: copper farmhouse sink
Pingback: lottare single bowl granite
Pingback: North Turtle Lake - Mille Lacs Realty
Pingback: tickets
Pingback: picture of 10 stainless steel undermount sink
Pingback: bathroom bowl sinks
Pingback: Schauer Lake - Mille Lacs Realty
Pingback: colon cleanse for constipation
Pingback: invoice creator software
Pingback: industrial clean
Pingback: software company invoice format
Pingback: 70 30 sink
Pingback: neuropathy in feet
Pingback: cleaning company nyc
Pingback: tarelochki kitaiskie zoloto v mos
Pingback: chiropractor prices
Pingback: 2 day colon cleanse
Pingback: appliance repair manuals
Pingback: stakany oplatit pod logo v mos
Pingback: professional invoicing for dummies
Pingback: repair clinic
Pingback: tarelka kupit pod logotip v mos
Pingback: invoice creator software
Pingback: Peyton Manning
Pingback: whirlpool warranty repair
Pingback: samsung refrigerator parts
Pingback: Buzz Aldrin
Pingback: appliance service center
Pingback: Beverly Cleary
Pingback: appliance repair company
Pingback: my invoice software
Pingback: Nancy Kerrigan
Pingback: April Bowlby
Pingback: invoice management
Pingback: George Will
Pingback: Boris Pasternak
Pingback: Real estate law advice
Pingback: Milkha Singh
Pingback: MARTIN KEATINGS
Pingback: professional invoice
Pingback: Fife Council
Pingback: Betsy Brandt
Pingback: copper farmhouse sink 40 in
Pingback: online invoicing and payment
Pingback: Indyref2
Pingback: visit website
Pingback: Council Elections
Pingback: Council Elections
Pingback: Asa Butterfield
Pingback: Burning Fat
Pingback: black kitchen sink
Pingback: Wedding photography editing service usa
Pingback: Future
Pingback: Los Angeles car accident lawyers
Pingback: Jenna Bush Hager
Pingback: stainless steel sink
Pingback: Council Elections
Pingback: J. Cole
Pingback: wedding photo editing services for photographers
Pingback: Chris Penn
Pingback: Jasper
Pingback: under mounted sink
Pingback: School Dance Photo Booth Jasper
Pingback: Wedding photography editing service usa
Pingback: DFW Texas SEO
Pingback: black pop up drain with overflow
Pingback: decorate space above kitchen cabinets
Pingback: Sunglasses and accessories
Pingback: quartz countertops
Pingback: kitchen storage ideas for small kitchens
Pingback: Hoodies and sweatshirts
Pingback: technology
Pingback: top 10 most viral youtube videos of all time
Pingback: Lam bang hieu Quang cao Quan 10
Pingback: best viral videos 2016 youtube
Pingback: New Jersey Drug Rehab
Pingback: most viral funny youtube videos week
Pingback: best youtube viral videos now ever
Pingback: Shower speaker
Pingback: casino online
Pingback: casino online sbobet
Pingback: iOS development
Pingback: Quickbooks payroll support
Pingback: agen Bola
Pingback: how to cure pimples
Pingback: make money in 90 days
Pingback: how to cure pimples
Pingback: how to reduce pimples
Pingback: t-shirts gestalten
Pingback: medical marijuana
Pingback: music
Pingback: pack of t shirts
Pingback: Best PGDM Institute in Delhi
Pingback: Judi Casino Online
Pingback: Exchange Bitcoin to Western union
Pingback: Quickbooks Customer service
Pingback: Quickbooks Payroll error
Pingback: personalized name necklace
Pingback: prospecting on linkedin
Pingback: se vende casa
Pingback: casa en venta en satelite
Pingback: sales prospecting tools
Pingback: venta de casas
Pingback: Education Jagran
Pingback: sterling silver name necklace
Pingback: name necklace
Pingback: child name necklace
Pingback: best medication for acne
Pingback: Europe Private Tours and Transfers
Pingback: how to remove pimples fast
Pingback: World Map of Our Private Layover Tours
Pingback: Japanese ski resorts
Pingback: Kinetic Sand
Pingback: organic self tanner
Pingback: Haiti - Due Diligence Services
Pingback: mab certification online
Pingback: professional ghostwriter for hire
Pingback: senior care referral
Pingback: page ranked
Pingback: tow truck cheap
Pingback: free fie hosting
Pingback: rollback truck sale
Pingback: Haiti - Death Investigation Services
Pingback: hino rollback tow trucks for sale
Pingback: Buying gold as an investment
Pingback: digital
Pingback: Christian Gold
Pingback: truck trailer types
Pingback: light for truck
Pingback: towing and recovery
Pingback: redford tow truck service near
Pingback: table lamps
Pingback: comfy sitting chairs
Pingback: handmade greek leather sandals
Pingback: vent cleaning
Pingback: paris chainsmokers mp3 download
Pingback: handmade leather sandals
Pingback: greek sandals
Pingback: scared to be lonely martin garrix mp3 download
Pingback: best air duct cleaning method
Pingback: Moving company yelp PortPortlandnd
Pingback: closer chainsmokers mp3 download
Pingback: industrial cleaners
Pingback: house cleaning lady
Pingback: rihanna love on the brain mp3 download
Pingback: www.utoptens.com/top-10-steak-facts-didnt-know/
Pingback: junk cars for cash
Pingback: charlie
Pingback: computer cleaning service
Pingback: stamped
Pingback: www.utoptens.com/top-10-played-league-legends-champions-bronze-division/
Pingback: sung
Pingback: Better Bath
Pingback: Zippo lighter
Pingback: myke leker
Pingback: ray bans for cheap
Pingback: both gucci mane drake mp3 download
Pingback: www.utoptens.com/top-10-highest-base-stats-pokemon-go/
Pingback: sextoy
Pingback: cheap ray ban aviators
Pingback: www.utoptens.com/top-10-rarest-pokemon-pokemon-go-generation-2-find/
Pingback: gofundme alternative
Pingback: ?Volunteer and Service Projects Fundraising
Pingback: www.utoptens.com/10-awesome-factions-magic-gathering/
Pingback: www.utoptens.com/top-10-dangerous-sports/
Pingback: Media agency
Pingback: Pet and Animal Fundraising
Pingback: Passive income
Pingback: Social media companies
Pingback: best vitiligo treatment
Pingback: www.utoptens.com/10-amazing-facts-great-pyramids-giza/
Pingback: Social media management
Pingback: bad and boujee migos mp3 download
Pingback: Passive income
Pingback: SAT prep
Pingback: Kindle direct publishing
Pingback: death of a child
Pingback: www.utoptens.com/top-10-best-jobs-future/
Pingback: Tutoring
Pingback: college prep
Pingback: lukas graham 7 years old mp3 download
Pingback: www.utoptens.com/top-10-best-battlefield-4-maps/
Pingback: Ashgail social media marketing
Pingback: sympathy cards
Pingback: pop up weddings
Pingback: i want my ex back
Pingback: case management software
Pingback: getting your ex back
Pingback: cloud based case management
Pingback: getting your ex back
Pingback: wedding decor
Pingback: garbage dumpsters rentals
Pingback: olathe businesses forsale 913-647-7500
Pingback: rent a garbage bin
Pingback: hotel forsale (913) 647-7500
Pingback: cafe forsale (913) 647-7500
Pingback: Kids Martial Arts
Pingback: Martial Arts Leicester
Pingback: Bimouse.com
Pingback: home page
Pingback: where can i donate a car
Pingback: frigidaire appliance service
Pingback: Galaxy J7 Prime Price in Sri Lanka
Pingback: Kickboxing Leicester
Pingback: Martial Arts Programs
Pingback: car donation bay area
Pingback: robert
Pingback: Download Free WordPress Plugins
Pingback: www.utoptens.com/top-10-favorite-candy-bars-americans/
Pingback: ice maker stopped working
Pingback: Free PHP Scripts
Pingback: dumpster dimensions waste management
Pingback: my home appliance service
Pingback: cars for donations to charity
Pingback: icemaker repair
Pingback: portland hats
Pingback: www.playmixarcade.com/
Pingback: portland hat
Pingback: Event management
Pingback: www.utoptens.com/top-10-tips-new-cat-owners/
Pingback: make extra money online
Pingback: hcg drops at walmart
Pingback: event planning company
Pingback: Cbtf Amit
Pingback: www.playmixarcade.com/category/sports/
Pingback: elderly care referral
Pingback: Best Houston Wedding Planners
Pingback: www.playmixarcade.com/category/strategy/
Pingback: review
Pingback: event planning
Pingback: money fast
Pingback: Buy HGH Thailand
Pingback: mediu university
Pingback: Website
Pingback: testimonies
Pingback: galas
Pingback: event decor
Pingback: www.playmixarcade.com/category/shooting/
Pingback: www.playmixarcade.com/category/defense/
Pingback: Website
Pingback: www.playmixarcade.com/category/action/
Pingback: Sony Xperia XA Ultra Dual Sim Price in Sri Lanka
Pingback: www.playmixarcade.com/category/adventure/
Pingback: www.playmixarcade.com/category/driving/
Pingback: www.playmixarcade.com/category/casino/
Pingback: www.playmixarcade.com/3d-cold-racer/
Pingback: Home Page
Pingback: Buy Steroids Cambodia
Pingback: Sony Xperia XA Dual Best Price in Sri Lanka 2017
Pingback: www.playmixarcade.com/canyon-valley-rally/
Pingback: Homepage
Pingback: construction bin rental
Pingback: what is the best colon cleanse to lose weight
Pingback: home appliance repairs
Pingback: what is the best colon cleanse to lose weight
Pingback: maytag oven parts
Pingback: dumpster disposal
Pingback: metal dumpster
Pingback: waste haulers
Pingback: yard waste dumpster rental
Pingback: spinner fidget toy
Pingback: Live web Cam Girls
Pingback: Become a Webcam Model
Pingback: baahubali 2 full movie online
Pingback: Dryer service
Pingback: piano
Pingback: violin
Pingback: Angel eyes
Pingback: 3DRENDERING
Pingback: Angel eyes
Pingback: dirty cleaning
Pingback: dryer vent heater
Pingback: instruction
Pingback: garbage removal
Pingback: construction containers for trash
Pingback: Free Postmates food delivery credit nationwide with Postmates promo code: TRYFREE50
Pingback: top 10 uhrenmarken
Pingback: Kohadoge Handicraft
Pingback: more
Pingback: Wooden Watches
Pingback: seiko black monster kaufen
Pingback: Scrap Metal Arts and Resin Paintings
Pingback: Entire portal with various useful information
Pingback: gute armbanduhren
Pingback: AD
Pingback: Kohadoge Handicraft
Pingback: Hurry up to apply here.
Pingback: Scrap Metal Arts and Resin Paintings
Pingback: effective
Pingback: Media
Pingback: PUBLISHER
Pingback: ?????/3/1/sellerRateDown/0/2000/0/0/0/0/0
Pingback: CHOOSE YOUR METRICS
Pingback: frigidaire
Pingback: article source
Pingback: Additional Info
Pingback: samsung appliance service
Pingback: all brands appliance service
Pingback: Source
Pingback: 24 towing service
Pingback: wedding flowers vancouver wa
Pingback: hair and beauty
Pingback: Wellness CORE Wet Food Reviews
Pingback: where to sell car parts
Pingback: hair amazon
Pingback: children's sweaters
Pingback: Super Premium Wild Salmon Canned Food Review & Rating
Pingback: Insta Followers
Pingback: cerrajero
Pingback: lingerie
Pingback: cbd health
Pingback: escape games
Pingback: steampunk coset dress
Pingback: make fake paystub
Pingback: cotton panties
Pingback: room escape nyc
Pingback: medical cbd
Pingback: check stubs
Pingback: Los Angeles pay stub service
Pingback: Dich vu hop phap hoa lanh su
Pingback: Dich thuat tieng a rap
Pingback: long dresses sale
Pingback: Dich thuat tai lieu y duoc
Pingback: flatbed wreckers
Pingback: register domain name
Pingback: dumpster rental Detroit
Pingback: godaddy domain
Pingback: boston edison emergency townearg near
Pingback: garbage dumpster sizes
Pingback: roll off dumpster rental cost
Pingback: dumper rental
Pingback: Dich tieng anh sang tieng Viet
Pingback: warehouse space
Pingback: Los Angeles fake pay stubs
Pingback: YOURURL.com
Pingback: income verification
Pingback: check this site out
Pingback: Los Angeles pay stub service
Pingback: Atlanta pay stub service
Pingback: Free online classified ads
Pingback: income verification
Pingback: Online Defensive Driving
Pingback: Online Defensive Driving
Pingback: fake pay stubs
Pingback: Online Defensive Driving
Pingback: Online Defensive Driving
Pingback: Online Defensive Driving
Pingback: fake check stub
Pingback: Post your ads for free
Pingback: adp fake pay stubs
Pingback: Online Defensive Driving
Pingback: Classified personal websites
Pingback: Online Defensive Driving
Pingback: Jacksonville pay stubs service
Pingback: Post your ads for free
Pingback: towny servers
Pingback: Finnish baby box
Pingback: Online Defensive Driving
Pingback: minecraft servers
Pingback: Online Defensive Driving
Pingback: business setup services in uae
Pingback: Online Defensive Driving
Pingback: capacitor 1812
Pingback: refrigerator parts
Pingback: open company in uae
Pingback: kayak fishing magazine
Pingback: kemet tantalum
Pingback: murata grm series
Pingback: uae business setup
Pingback: major appliance
Pingback: kayak fishing boats
Pingback: towny
Pingback: more
Pingback: our website
Pingback: washing machine
Pingback: Fishing Charter Jupiter
Pingback: Retirement Accounts
Pingback: Unlocking Your Million Dollar Potential
Pingback: Stock Options
Pingback: Santina Lustig
Pingback: workouthard
Pingback: dogdailyfeaturesss
Pingback: IT professionals
Pingback: petitbateau
Pingback: pvp minecraft
Pingback: towny servers
Pingback: this review
Pingback: t shirts
Pingback: mc towny
Pingback: xxxtentations
Pingback: nj
Pingback: find akuamma seeds online
Pingback: content marketing agency of the year in uae
Pingback: branding
Pingback: Picralima Nitida for sale
Pingback: akuamma seeds for sale
Pingback: gallon fish tank
Pingback: vocal singing noise meter
Pingback: the best tank
Pingback: is superior singing method a scam
Pingback: cleaning company websites
Pingback: pvc screws
Pingback: bakeware
Pingback: singing lessons online
Pingback: Marketplace go ethnyk
Pingback: le creuset bakeware
Pingback: superior singing method aaron
Pingback: north shore appliance repair
Pingback: premier appliance repair
Pingback: office cleaning services malaysia
Pingback: cheap engagement rings
Pingback: electric range repair
Pingback: teamindustrialservices
Pingback: best way to learn affiliate marketing
Pingback: chocolate coffee beans
Pingback: Vendre parfumerie
Pingback: chocolate coffee beans
Pingback: Marketplace cosmetique
Pingback: lavazza coffee
Pingback: couple rings
Pingback: affiliate marketing for beginners
Pingback: lamp shades
Pingback: floor reading lamps
Pingback: cpa marketing training
Pingback: Essential Oil Diffuser Necklace
Pingback: in home decor
Pingback: Park
Pingback: kapasitor mkp
Pingback: 222m 1kv
Pingback: fungsi kapasitor tantalum
Pingback: home decor stores online
Pingback: baby cloth
Pingback: hanging lamps
Pingback: baby clothes for girls
Pingback: brass lamp
Pingback: gold lamp
Pingback: stanozolol
Pingback: family wall art
Pingback: wall paintings for living room
Pingback: faucet china
Pingback: bathroom showers manufacturers suppliers
Pingback: jobs in uae
Pingback: explainer cartoon videos
Pingback: commercial production
Pingback: Jewelry
Pingback: commercial video production services
Pingback: free advertising sites
Pingback: Beyond Real Estate
Pingback: Property Investment Thailand
Pingback: Getting Paid to Eat! Average Joe Arbitrage
Pingback: What is Manufactured Spending? Average Joe Arbitrage
Pingback: corrugated plastic
Pingback: jobmagpie
Pingback: Get Paypal Account with Password
Pingback: gas delivery
Pingback: AR Frame Nightmare
Pingback: gas delivery
Pingback: maxidentsoftwareblog.blogspot.com
Pingback: AR Frame Violet
Pingback: Valentus
Pingback: chess sets uk
Pingback: community
Pingback: Full Article
Pingback: websites
Pingback: Source
Pingback: Best kitchen laminate countertops ideas
Pingback: Clicking Here
Pingback: Visit website
Pingback: chess sets uk
Pingback: forum
Pingback: chess sets
Pingback: Business law cases and answers in 2017
Pingback: View page
Pingback: chess sets uk
Pingback: chess boards
Pingback: the noir
Pingback: Office Pixi VA Service
Pingback: chess sets
Pingback: rent a dumpster
Pingback: Roofers in Detroit
Pingback: junk removal prices
Pingback: trash bin
Pingback: commercial dumpster
Pingback: buy weed online
Pingback: rental classifieds india
Pingback: versace
Pingback: baby safe hair styling products
Pingback: 1969 versace
Pingback: demolition container rental
Pingback: budbuddy
Pingback: versace jeans
Pingback: photo sharing app
Pingback: phyto shatter
Pingback: roll off container rental
Pingback: tattoo
Pingback: in this site
Pingback: tattoo
Pingback: budmail
Pingback: open top container rental
Pingback: Greenbelt Hamilton Condo for sale in Makati city
Pingback: click here
Pingback: web site
Pingback: Detroit Metro Towing
Pingback: robert
Pingback: garbage rental
Pingback: COLLABORATION
Pingback: used heavy duty tow trucks
Pingback: towing new franklin
Pingback: Best place to buy hiking gear
Pingback: roll off dumpster rental cost
Pingback: Best place to buy hiking gear
Pingback: get more information
Pingback: air duct for dryer
Pingback: budbuddy
Pingback: air conditioning quotes
Pingback: Best gear for survival
Pingback: auto insurance liability
Pingback: Service Apartments in Gurgaon
Pingback: waste management dumpster rental
Pingback: Birthday quotes for friend
Pingback: Best gear for hiking
Pingback: Service Apartments in Bandra
Pingback: waste management dumpster cost
Pingback: lightweight backpack
Pingback: 16 inch backpack
Pingback: Best gear for hiking
Pingback: Service Apartments in Powai
Pingback: carte grise en ligne
Pingback: carte grise
Pingback: nrc wreckers for sale
Pingback: Best gear for survival
Pingback: 15 inch backpack
Pingback: carte grise
Pingback: 10 yard roll off
Pingback: towing coventry
Pingback: skyzone birthday parties
Pingback: sky fitness
Pingback: skyzone trampoline park Stockton CA
Pingback: men fashion backpack
Pingback: View profile
Pingback: real estate license
Pingback: low protein dog food
Pingback: dumpster rental
Pingback: teal pillows
Pingback: obuchenie v kanade dlya russkih
Pingback: homemade cookbook
Pingback: buy a skyzone franchise
Pingback: Countries with cheap property for sale below 50,000 Euro
Pingback: victory wreckers
Pingback: homemade ice cream
Pingback: organic dog food
Pingback: tripod floor lamp
Pingback: food storage jars
Pingback: skyzone group events
Pingback: decorative throw pillows
Pingback: Property for sale in France
Pingback: lamp table
Pingback: ace industrial services korsten contact details
Pingback: industrial services jobs perth
Pingback: industrial services baton rouge
Pingback: PETCO s most fierce Competition
Pingback: playwright
Pingback: food storage containers with lids
Pingback: Cheap and luxurious Dog and cat Beds
Pingback: kitchen storage containers set
Pingback: Adorable Hooded Sweatshirts for your Puppy!
Pingback: The Perfect toy for your Dog
Pingback: freeze dried camping food
Pingback: Author
Pingback: Great and comfy dogs bed
Pingback: Various Animal Plush Toys for your puppy
Pingback: The best Kitty Inspired Jewelry just for you!
Pingback: All Seasons Luxurious Dog bed
Pingback: Thailand trade directory
Pingback: Malaysia Best Candy Floss
Pingback: Beautiful Dog Collar
Pingback: Home inspector
Pingback: Adorable Little Shell Cat Bed
Pingback: kuala lumpur magician service
Pingback: Thailand tourism
Pingback: The Best Online Pet Supply Store in the USA Market today
Pingback: The Best 10 feet leash for your dog!
Pingback: magician kids birthday party
Pingback: long island real estate
Pingback: hire mask changing in malaysia
Pingback: Magician for hire in Kuala Lumpur
Pingback: employment Thailand
Pingback: samsung refrigerator repair los angeles
Pingback: half marathon
Pingback: Take a look at this Toy LED Laser Pointer for you and your cat
Pingback: appliance repair parts los angeles
Pingback: get followers on instagram
Pingback: Engagement Ring Store Houston
Pingback: petite
Pingback: Check out our wide variety of GIA, AGS or IGI certified loose diamonds
Pingback: gravatar info
Pingback: clash royale gem hack
Pingback: Jewelry Depot Houston has the largest selection of diamond jewelry to choose from
Pingback: children's party entertainer
Pingback: appliance repair los angeles
Pingback: Outdoor wedding reception decoration ideas in 2017
Pingback: order gravatar
Pingback: entertainer for kids party
Pingback: Visit
Pingback: Top Jewelry Store Houston
Pingback: Activities for kids
Pingback: order oxycontin
Pingback: kids birthday party entertainment
Pingback: Visit website
Pingback: EPONYMES TSANTES
Pingback: Valentines Day Sale on Engagement Rings Houston
Pingback: View page
Pingback: make money online
Pingback: lighting system rental
Pingback: Party Magician Malaysia
Pingback: pa system rental in malaysia
Pingback: roofing companies in canton Michigan
Pingback: waste disposal containers
Pingback: clown for kids party
Pingback: victory auto wreckers commercial
Pingback: Road Trip Hotels
Pingback: wreckers brisbane
Pingback: Emilia Romagna Pasta
Pingback: audio deals
Pingback: roofing companies in canton mi
Pingback: IMF currencies
Pingback: led monitor lg
Pingback: Interesting Read
Pingback: Canton MI roofing supply
Pingback: fun food for rental
Pingback: cpu cooler definition
Pingback: 2016 US Dollar Crash
Pingback: car scrap
Pingback: Pasadena California refrigerator repair
Pingback: Aperol Spritz
Pingback: cheap taxi coventry to birmingham airport
Pingback: IPTV ABONNEMENT
Pingback: house move
Pingback: Perfection Appliance Repair 626-243-7088
Pingback: refrigerator leak repair Pasadena
Pingback: Repair concrete
Pingback: taxi to luton airport
Pingback: Repair concrete
Pingback: used flatbeds for sale
Pingback: vehicle insurance company
Pingback: truck moving
Pingback: a service provider that takes care of its customers
Pingback: used tow truck bodies for sale
Pingback: online used auto parts
Pingback: detroit tow truck in
Pingback: towing and repair service
Pingback: car towing services prices
Pingback: Food Travel Blog
Pingback: irs back tax help
Pingback: south Africa online store
Pingback: journals
Pingback: Visit This Link
Pingback: get more info
Pingback: mothers day
Pingback: site
Pingback: 2015 tax forms
Pingback: Electric cars
Pingback: payroll tax
Pingback: More Help
Pingback: elder law attorney
Pingback: air conditioning in dubai
Pingback: business letter samples and format
Pingback: portable dumpster
Pingback: letter to publisher samples and format
Pingback: personal letter samples and format
Pingback: waste disposal containers
Pingback: paragraph writing format
Pingback: construction container rental
Pingback: tree cutting in Grand Rapids mi
Pingback: portable garbage dumpster
Pingback: price for dumpster rental
Pingback: trash dumper
Pingback: waste management company
Pingback: bins rental
Pingback: rolloffs
Pingback: Pastors
Pingback: wealth management firms
Pingback: Bus Booking
Pingback: Aphrodisiac for Women
Pingback: Games
Pingback: Pastors
Pingback: dia oc dai tin
Pingback: dia oc dai tin bien hoa
Pingback: hair and makeup
Pingback: best
Pingback: cartoon hair
Pingback: microblading tools
Pingback: microblading touchup
Pingback: Visit Website
Pingback: sarracenia wrigleyana scarlet belle
Pingback: seo expert canberra
Pingback: blank t-shirts for printing
Pingback: St. Petersburg Fl Air Conditioner repair
Pingback: bbq tool set b&q
Pingback: bbq tool set luxury
Pingback: financial letter samples and format
Pingback: banking letter samples and format
Pingback: wealth management firms
Pingback: Tampa HVAIR CONDITIONER
Pingback: Ductless Split Air Conditioning repair in Lakeland
Pingback: ac companies st. petersburg fl
Pingback: Largo Air Conditioner companies
Pingback: Chris Hanson mendham
Pingback: fifa 15
Pingback: treating hemorrhoids
Pingback: Browse local online pawn shop inventory
Pingback: Gold Loan
Pingback: symptoms of piles
Pingback: Pawn shop Near me
Pingback: soccer
Pingback: hemorrhoids symptoms
Pingback: hemorrhoids
Pingback: Nashville Gold Buyers
Pingback: Buy Engagement Ring Nashville
Pingback: hemorrhoid pain relief
Pingback: Rolex buyers
Pingback: Buy Engagement Ring Nashville
Pingback: on sale lithium battery
Pingback: Kasteel
Pingback: Mobile notary
Pingback: what is the best compatible cr123 lithium battery
Pingback: Check out Aria Veach Lingerie
Pingback: Go Here for Aria Veach Music Videos
Pingback: long lasting 2032 battery
Pingback: Check This Instagram Out Trans Celebrity Aria Veach
Pingback: 3v lithium battery
Pingback: free shipping 24hour batteries
Pingback: buy lithium batteries
Pingback: Find Out More
Pingback: hoists
Pingback: reusable ear plugs
Pingback: lifting slings
Pingback: gem residences
Pingback: ratchet lever hoist
Pingback: safety gloves
Pingback: construction hats
Pingback: gantry crane wheels
Pingback: stainless turnbuckles
Pingback: reflective waistcoat
Pingback: The Alps Residences
Pingback: lifting equipment suppliers
Pingback: steel wire rope suppliers
Pingback: lashing equipment
Pingback: little Italy
Pingback: grade 80 lifting chain
Pingback: metal cable
Pingback: tourism in singapore
Pingback: North Side dumpster rental
Pingback: dumpster rental Dearborn Park
Pingback: shabby chic furniture
Pingback: poker
Pingback: second hand furniture
Pingback: fitness
Pingback: helendorf hotel helen ga
Pingback: casino
Pingback: perez hotel furniture
Pingback: tour singapore
Pingback: night
Pingback: casino
Pingback: trash dumper
Pingback: 10 yard container
Pingback: poker
Pingback: tourism
Pingback: waste management dumpster dimensions
Pingback: garbage disposal rental
Pingback: breakfast ideas
Pingback: best home infrared sauna
Pingback: infrared sauna dangers
Pingback: banking
Pingback: near infrared bulbs
Pingback: kerio
Pingback: sauna advantages
Pingback: running
Pingback: pinar vpn
Pingback: wine glasses online
Pingback: beer bottle
Pingback: pinar vpn
Pingback: brandy glass
Pingback: real estate agent referrals
Pingback: tourist
Pingback: danabol ds 10mg
Pingback: homebrew shop
Pingback: buy anabolic steroids online
Pingback: cheap coffee mugs
Pingback: tour
Pingback: dining table runners
Pingback: buddy
Pingback: clear braces fort lauderdale
Pingback: dining table runners
Pingback: coffee mugs online
Pingback: clear braces fort lauderdale
Pingback: green table runner
Pingback: dbol
Pingback: tablecloth sizes
Pingback: coffee mugs
Pingback: best injectable steroids
Pingback: booking girl singapore
Pingback: food
Pingback: viagra
Pingback: PWC Seadoo Top End Rebuild Kits
Pingback: Lean Belly Breakthrough Secret
Pingback: workout
Pingback: cialis
Pingback: hot sg girls
Pingback: Outboard Mercury Seal Kits
Pingback: discipline
Pingback: Affiliate Business
Pingback: Chimney repair long island
Pingback: eyelash grow back
Pingback: 1xbet bahis
Pingback: Ikeja
Pingback: robux for roblox
Pingback: how to make money online
Pingback: Go here
Pingback: betboo
Pingback: Click here
Pingback: best eyelash serum
Pingback: System
Pingback: bets10
Pingback: How to make serious money online
Pingback: Accessories
Pingback: Go here
Pingback: tempobet
Pingback: best eyelash growth serum
Pingback: clash royale hack
Pingback: Go here
Pingback: ankarablvd
Pingback: make eyelashes grow
Pingback: natural eyelash growth
Pingback: youwin giriş
Pingback: Lufingen
Pingback: superbahis
Pingback: 20 kids bike
Pingback: mumbai escort
Pingback: 24 inch boys bike
Pingback: Benken
Pingback: hiperbet
Pingback: Wettingen
Pingback: Rüti
Pingback: casinodunya
Pingback: 12 inch bike
Pingback: bikes for girls
Pingback: mountain bikes for kids
Pingback: Männedorf
Pingback: justinbet
Pingback: mybahis
Pingback: Contemporary Art
Pingback: 20 inch boys bike
Pingback: Party Mix
Pingback: Public Art
Pingback: Party Mix
Pingback: get rid of plantar warts
Pingback: 24 kids bike
Pingback: pointillism installation
Pingback: how to get rid of warts on feet
Pingback: Cam Shows
Pingback: pointillism installation
Pingback: Mommy Son Big Tits
Pingback: get rid of plantar warts
Pingback: hanging installation
Pingback: play station 4
Pingback: how to get rid of warts on feet at home overnight
Pingback: hanging installation
Pingback: play station 4
Pingback: Chinese Canadian Artist
Pingback: hiperbet
Pingback: betboo inceleme
Pingback: justinbet
Pingback: best10 inceleme
Pingback: Sarayacasino
Pingback: youwin yeni giriş
Pingback: topaz
Pingback: seuls
Pingback: tempobet
Pingback: XBOX one s
Pingback: food sensitivities
Pingback: tungsten wedding band 8mm
Pingback: women wedding band tungsten
Pingback: mens wedding ring
Pingback: tungsten wedding band comfort fit
Pingback: mens wedding bands tungsten
Pingback: Contract Jobs UK
Pingback: residential dumpster rental
Pingback: dumpster roll off
Pingback: motu patlu game
Pingback: best microphone for vocals
Pingback: best studio microphone
Pingback: 1 person sauna
Pingback: Contract Jobs
Pingback: math tutor
Pingback: in house sauna
Pingback: podcasting microphone
Pingback: Jobs UK
Pingback: best mics for podcast
Pingback: ProContractJobs
Pingback: best microphone for vocals
Pingback: waste management temporary dumpster
Pingback: cost to rent a dumpster for a day
Pingback: math tutors miami
Pingback: sauna 2 person
Pingback: Our Pricing
Pingback: Pro Contract Jobs
Pingback: End of lease clean Melbourne
Pingback: End of lease cleaning
Pingback: End of lease clean Melbourne
Pingback: Recruitment UK
Pingback: Pro Contract Jobs
Pingback: Bible Prophecy
Pingback: www.spu.ac.th
Pingback: pie in face videos
Pingback: girl in shower
Pingback: Yoga in Perth
Pingback: Android App
Pingback: computer screen privacy filter
Pingback: Corporate HIIT Perth
Pingback: real steroids online
Pingback: slime girl
Pingback: ReMe
Pingback: anabolic steroids online
Pingback: Corporate HIIT Perth
Pingback: messy videos
Pingback: winstrol
Pingback: Primodex
Pingback: Corporate Pilates Perth
Pingback: medispa
Pingback: injectable steroids side effects
Pingback: Ultradex
Pingback: Sciroxx Laboratories
Pingback: legal steroids online
Pingback: Web Site
Pingback: best online steroids
Pingback: breast augmentation
Pingback: online steroids
Pingback: danabol ds blue hearts
Pingback: injectable anabolic steroids
Pingback: boldenone
Pingback: medispa
Pingback: Turinadex
Pingback: Testodex Propionate
Pingback: medispa
Pingback: medispa
Pingback: boldenone
Pingback: army desert boots
Pingback: click here
Pingback: dbol
Pingback: winstrol
Pingback: ofertas
Pingback: our website
Pingback: gore tex military boots
Pingback: our website
Pingback: Related Site
Pingback: nature
Pingback: cupons
Pingback: More Info
Pingback: Discover More
Pingback: link house
Pingback: anabolic steroids online
Pingback: ofertas e descontos
Pingback: Read Full Article
Pingback: ofertas
Pingback: cupons
Pingback: bungalow
Pingback: link factory
Pingback: link factory
Pingback: bracelet
Pingback: Look At This
Pingback: Clicking Here
Pingback: perda auditiva
Pingback: Torresdale
Pingback: 19151
Pingback: Digital X-Rays
Pingback: paleo diet
Pingback: tallest buildings in the world
Pingback: San Diego Security Guard
Pingback: San Diego Courtesy Patrol
Pingback: San Diego Security Patrol
Pingback: San Diego Security Guard Service
Pingback: San Diego Security Patrol
Pingback: San Diego Courtesy Patrol
Pingback: Dr.Byers
Pingback: San Diego Courtesy Patrol
Pingback: Radio Accessories
Pingback: cell renewal
Pingback: anti aging
Pingback: self healing books
Pingback: self improvement books
Pingback: Jupiter
Pingback: brenton thwaites
Pingback: San Diego Courtesy Patrol
Pingback: Divorce Lawyer Florida
Pingback: alastair fothergill
Pingback: 27t59xmotc4wn5x5tmw45cte4
Pingback: feel rich health is the new wealth
Pingback: About Us
Pingback: Fort Lauderdale
Pingback: HB967
Pingback: Collaborative Law Process Act
Pingback: Cincinnati Website Creator
Pingback: football transfer
Pingback: water play date
Pingback: Cincinnati Website Maker
Pingback: la liga news
Pingback: football transfer gossip
Pingback: Web Agency
Pingback: liverpool transfer gossips
Pingback: liverpool new signings
Pingback: Cincinnati eCommerce Website
Pingback: Cincinnati Website Creator
Pingback: Web Agency
Pingback: Cincinnati Web Development Company
Pingback: optimizar adwords
Pingback: e commerce
Pingback: marketing online master
Pingback: marketing tecnologico
Pingback: enviar correos masivos
Pingback: crm marketing
Pingback: Marrakech desert trips
Pingback: content professor discount
Pingback: walnut seed
Pingback: Marrakech desert trips
Pingback: best beard balm
Pingback: mens beard oil
Pingback: walnut
Pingback: toddler bed duvet cover
Pingback: mens beard oil
Pingback: Marrakech desert trips
Pingback: toddler girl bedding
Pingback: Marrakech desert trips
Pingback: individualized attention
Pingback: janitorial supply store
Pingback: what is 15 minute manifestation
Pingback: beard growth
Pingback: good vacuum cleaner
Pingback: canister vacuum cleaner
Pingback: Just embark with me on this exciting journey!
Pingback: Subtitle Indonesia
Pingback: the best beard oil
Pingback: Track record
Pingback: Just embark with me on this exciting journey!
Pingback: Just embark with me on this exciting journey!
Pingback: Certified Leadership Coaching Professional
Pingback: Unique wedding ideas. All about party for wedding
Pingback: wet sauna
Pingback: Travel Blog
Pingback: bad credit mortgage
Pingback: portable dumpster rental
Pingback: Best wedding cake idea in 2017
Pingback: infrared heater for sauna
Pingback: My clients
Pingback: get a dumpster
Pingback: Graphic T-shirts
Pingback: first time home buyer
Pingback: order a dumpster
Pingback: Best centerpiece ideas for wedding in 2017
Pingback: refuse container rental
Pingback: best mortgage rates
Pingback: My clients
Pingback: bfi trash removal
Pingback: cedar steam room
Pingback: near infrared light bulbs
Pingback: My own authenticity
Pingback: waste management dumpster rental
Pingback: Tourism Videos
Pingback: Bohemian Couples
Pingback: condos for sale
Pingback: concrete dumpster rental
Pingback: waste removal services
Pingback: roll off trailers
Pingback: second mortgage
Pingback: interest rates
Pingback: refinance mortgage
Pingback: best mortgage rates
Pingback: social media
Pingback: punchline lacrim
Pingback: social media
Pingback: Gold-backed Ira
Pingback: Christian Gold
Pingback: www.cornerstoneassetmetals.com
Pingback: InstitutionalInvestor.com
Pingback: Best cheap rustic wedding ideas in 2017
Pingback: Website
Pingback: ez battery reconditioning a scam
Pingback: ez battery reconditioning free download
Pingback: Real estate
Pingback: Promote yourself
Pingback: Home
Pingback: ez battery reconditioning reddit
Pingback: ez battery reconditioning a scam
Pingback: houses for sale
Pingback: mls listings
Pingback: ez battery reconditioning course scam
Pingback: Home
Pingback: Charter an airplane
Pingback: property value estimate
Pingback: Fsbo
Pingback: mls realtor
Pingback: ez battery reconditioning pdf download
Pingback: For sale by owner
Pingback: homes for sale
Pingback: mls listing
Pingback: Listing service
Pingback: cara menang dalam Wukong
Pingback: keyboard image
Pingback: How to sell a home
Pingback: audio deals
Pingback: computer mouse models
Pingback: hard disk capacity
Pingback: literature
Pingback: keyboard qwerty
Pingback: seagate hard disk price
Pingback: solid state drive price
Pingback: hard disk volume
Pingback: Wukong
Pingback: computer ram
Pingback: computer mouse best
Pingback: replacing a cpu cooler
Pingback: peripherals of a computer
Pingback: great online shopping deals
Pingback: computer mouse for child
Pingback: desktop pc for gaming
Pingback: definition of solid state drive
Pingback: types of computer ram
Pingback: House for sale
Pingback: hard disk brands
Pingback: selfie stick bluetooth iphone amazon
Pingback: computer mouse optical
Pingback: keyboard for beginners
Pingback: processor chip
Pingback: water bottle
Pingback: external hard drive online
Pingback: motherboard price
Pingback: Norcross locksmith
Pingback: fishing costa rica
Pingback: locksmith in Manchester
Pingback: locksmith Clinton Hill
Pingback: apple
Pingback: Best ideas for small kitchens in 2017
Pingback: graphics card durban
Pingback: change locks
Pingback: Website
Pingback: Best kitchen lighting ideas in 2017
Pingback: graphics card in computer
Pingback: visit
Pingback: visit my blog
Pingback: Montessori activities for 3 year olds at home
Pingback: external hard drive for sale
Pingback: optical drives list
Pingback: Montessori activities for toddlers
Pingback: my website
Pingback: website
Pingback: thermal grease cpu
Pingback: Will and estates questions in 2017
Pingback: optical drives definition
Pingback: View source
Pingback: solid state drive for desktop
Pingback: monitor bracket dual
Pingback: selfie stick bluetooth battery
Pingback: hard disk hp
Pingback: new and noteworthy
Pingback: acim
Pingback: Withdraw Bitcoin from Blockchain to bank account
Pingback: podcasters
Pingback: Nonton film bioskop
Pingback: construction dumpsters for rent
Pingback: cleaning carpet services
Pingback: chicago rugs
Pingback: rug cleaning machines
Pingback: residential trash removal
Pingback: main poker di hp
Pingback: texas holdem
Pingback: yard dumpster rentals
Pingback: main poker di iphone
Pingback: portable garbage dumpster
Pingback: automatic appliance
Pingback: led torch light
Pingback: torch flashlight
Pingback: appliance repair Hilsborough
Pingback: high lumen flashlight
Pingback: click through the up coming page
Pingback: click through the up coming website
Pingback: bosch appliance
Pingback: benefits of yoga
Pingback: real estate creswell or
Pingback: food and nutrition
Pingback: vitamin c benefits
Pingback: suggested browsing
Pingback: partner link
Pingback: whirlpool freezer parts
Pingback: electric power tools
Pingback: dewalt cordless drill
Pingback: cottage grove oregon real estate
Pingback: BecomeChic.com
Pingback: power tool set
Pingback: kerala wedding dress
Pingback: blog
Pingback: cricbuzz live score
Pingback: ten sports live match
Pingback: plastic shower door hinges hardware
Pingback: framed shower door hardware
Pingback: svg cuttables
Pingback: SVG
Pingback: ball by ball cricbuzz
Pingback: cricabuzz
Pingback: best power tools
Pingback: shower door brackets uk
Pingback: shower door hardware replacement
Pingback: bosch tools
Pingback: shower door hinges replacement
Pingback: Disabled
Pingback: New York
Pingback: Advocacy group
Pingback: jepang gratis.nonton movie
Pingback: Disabled
Pingback: Disabled
Pingback: dumpster rental glenview
Pingback: Community Slack
Pingback: Order Yours Today
Pingback: dumpster sizes
Pingback: Add To Cart
Pingback: need a dumpster
Pingback: Careers
Pingback: dumpsters rental
Pingback: Add To Cart
Pingback: 10 yard roll off dumpster
Pingback: See Full Specs
Pingback: Manufacturers
Pingback: products from thailand
Pingback: gas appliance repair
Pingback: reverse osmosis water filtration system uv filter
Pingback: Thai Cosmetic
Pingback: mango
Pingback: capsules
Pingback: Play Store!
Pingback: aheap appliance repair
Pingback: Hackettstown appliance master
Pingback: Aerial video
Pingback: drone pilot Dallas Texas
Pingback: Drone Videography
Pingback: brick hammer
Pingback: hammer drill
Pingback: drone pilot Kansas
Pingback: buy hammer
Pingback: central appliance service
Pingback: repair washer
Pingback: appliance technicians
Pingback: keychain multi tool
Pingback: Read More Here
Pingback: Sarti Halkidiki Rooms Booking
Pingback: weight loss gym
Pingback: side cut
Pingback: Sarti Halkidiki Rooms Booking
Pingback: Go Here
Pingback: pliers set
Pingback: leatherman multi tool
Pingback: Rooms Booking Sarti Halkidiki
Pingback: weight loss regime
Pingback: Sarti Halkidiki Photos
Pingback: fat reduce exercise
Pingback: flat nose pliers
Pingback: Sarti Hotel Preise
Pingback: Sarti Halkidiki Greece Rooms
Pingback: Sarti activity Hiking
Pingback: keychain multi tool
Pingback: locking pliers
Pingback: torx socket set
Pingback: weight loss exercise for ladies
Pingback: Sarti activity Hiking
Pingback: l shaped screwdriver
Pingback: electronic screwdriver set
Pingback: network socket
Pingback: Fix and Flip Funding
Pingback: Make money on Facebook
Pingback: torque screwdriver set
Pingback: philip screw driver
Pingback: impact socket set
Pingback: set of screwdrivers
Pingback: Hotel in Sarti Halkidiki Greece
Pingback: Sarti Halkidiki Rooms Booking
Pingback: Sarti activity Hiking
Pingback: Sarti Chalkidiki Zimmer Buchen
Pingback: Sarti Chalkidiki Fotos
Pingback: Sarti activity Hiking
Pingback: Sarti activity Hiking
Pingback: Hotel in Sarti Halkidiki Greece
Pingback: dumpster
Pingback: The very best high-flying bounce place in Canton!
Pingback: Sarti Chalkidiki Zimmer Buchen
Pingback: dumpster rental lemont
Pingback: trampoline park Canton
Pingback: Paper Packaging in kenya
Pingback: Rooms Apartments Halkidiki Sarti
Pingback: 3 yard dumpster
Pingback: commercial dumpster rental
Pingback: Sarti activity Hiking
Pingback: Sarti activity Hiking
Pingback: debris removal services
Pingback: techno music artists
Pingback: best dumpster rental
Pingback: appliance repair manual
Pingback: salt lake dishwasher repair
Pingback: techno music download
Pingback: what is the best washer
Pingback: whirlpool appliances parts
Pingback: whirlpool clothes washer
Pingback: skyzone trampoline park Canton OH
Pingback: Australian Quidditch League
Pingback: ReMe Worldwide
Pingback: Virtual Reality Book
Pingback: quidditch chaser
Pingback: Agen Casino Online
Pingback: Birthday Parties in Canton OH
Pingback: Quidditch pitches
Pingback: expiration date app
Pingback: Virtual Reality Experts
Pingback: trampoline park CA
Pingback: ReMe USA
Pingback: expiration date app
Pingback: Food expiration app
Pingback: ReMe Smart-Barcode-Scan
Pingback: ReMe Basket app
Pingback: affordable family law attorney los angeles california
Pingback: ReMe
Pingback: Agen Bola Online
Pingback: ReMe Inteli-Text-Read
Pingback: Food expiration date app
Pingback: Agen Bola Judi Casino
Pingback: divorce lawyers in los angeles california
Pingback: low cost divorce attorney in los angeles ca
Pingback: two door cinema club poster
Pingback: Flat tire
Pingback: bungalow
Pingback: metric socket set
Pingback: long socket set
Pingback: trash bin rental
Pingback: land for sale malaysia
Pingback: socket wrench set
Pingback: Truck tire
Pingback: long socket set
Pingback: data socket
Pingback: serrated knife
Pingback: cutlery knives
Pingback: Trailer tire repair near me
Pingback: hunting knife
Pingback: Truck tire
Pingback: cooks knives
Pingback: cleaning items
Pingback: dumpster
Pingback: waste management dumpster sizes
Pingback: steel wheels
Pingback: waste container rental
Pingback: trash disposal
Pingback: temporary trash dumpster
Pingback: dumpster bin sizes
Pingback: atm number location
Pingback: fee free atm
Pingback: banks open until 7pm
Pingback: chase bank atm
Pingback: locksmith wilmette il
Pingback: car wreck lawyer
Pingback: poker strategy
Pingback: board games for kids
Pingback: locksmith Evanston IL
Pingback: judi bola 88
Pingback: lawyers for accidents
Pingback: Locksmith Lake Forest IL
Pingback: Agen SBOBET Resmi
Pingback: injury attorney
Pingback: sports betting tips
Pingback: Curtain Steam Cleaning Middle Camberwell
Pingback: Curtain Repairs Drumcondra
Pingback: Acting workshops houston
Pingback: Blind Cleaning Westleigh
Pingback: Curtain Steam Cleaning Russell Island
Pingback: Curtain Dry Cleaning The Entrance
Pingback: business card
Pingback: make money online now
Pingback: viagra
Pingback: Car rental udon thani
Pingback: tango lessons london
Pingback: resto original paris
Pingback: christian practice
Pingback: bonnes adresses paris restaurant
Pingback: restaurant gastronomique romantique paris
Pingback: Limassol Property
Pingback: Cyprus Property
Pingback: Protaras Property
Pingback: B2B leads
Pingback: salwar kameez
Pingback: B2b lists
Pingback: anarkali suits
Pingback: Direct mail marketing
Pingback: fridge magnets
Pingback: Car rental Loei
Pingback: indian salwar kameez
Pingback: designer suits
Pingback: Jinaam Dresses
Pingback: salwar kameez online
Pingback: salwar suit online shopping
Pingback: cotton sarees
Pingback: designer kurtis
Pingback: miami wedding photographer
Pingback: romantic projects for ProShow Producer
Pingback: Home Staging
Pingback: jason guck social
Pingback: photoshop brushes
Pingback: IBM spectrum protect
Pingback: Projects birthday for ProShow Producer
Pingback: png frames
Pingback: jason guck success
Pingback: aerobyte
Pingback: miami wedding photographers
Pingback: wallpapers
Pingback: cloud backup
Pingback: jason guck training
Pingback: masterclas trafego rapido
Pingback: Best Casino in Malaysia
Pingback: Best Casino in Malaysia
Pingback: mini site de sucesso
Pingback: rent to own condo
Pingback: Affordable Dentist North Little Rock
Pingback: ????? ???? ????????
Pingback: Best Dentists North Little Rock
Pingback: rent to own condo
Pingback: ???? ????? ????????
Pingback: Mounts Dental Care
Pingback: Best Dentists North Little Rock
Pingback: keynote speaker
Pingback: project topics for kindergarten
Pingback: Find the right button cell Battery
Pingback: project topics computer science
Pingback: event speaker
Pingback: keynote speaker
Pingback: Find Lithium battery compatible
Pingback: project topics mba
Pingback: Ricette senza glutine sono preparate con prodotti privi di glutine al 100% quindi Gluten free. Chiedi la consulenza alla Dott.ssa scopri i sintomi Celiachia
Pingback: Ricette gluten free con alimenti senza glutine per le persone che hanno la celiachia. Trova la tua ricetta preferita tra le tante presenti
Pingback: Celiachia cos'è e come diagnosticarla, quali sono i sintomi di chi ha intolleranza al glutine, quali sono gli esami da fare per la celiachia, leggi
Pingback: Celiachia le cure quali sono e quale dieta fare, una dieta senza glutine risolve il problema o c'è bisogno di altro nella dieta per intolleranza al glutine
Pingback: Fotografia
Pingback: Biologa nutrizionista per ricette senza glutine e per dare informazioni veramente utili a chi è affetto da questa malattia, condivido la mia esperienza
Pingback: Edição Vídeo Blender
Pingback: Fotografia
Pingback: Como baixar Músicas Gratuitamente
Pingback: Ricette veloci senza glutine per le persone celiachi e i celiaci che hanno la celiachia, se sei intollernate al glutine devi fare un dieta
Pingback: Diagnosi celiachia non è mai facile, non c'è ancora una corretta informazione su come diagnosticare la celiachia, vediamo quindi quali sono i test efficaci
Pingback: Sintomi celiachia quali sono e come riconoscerli, ci sono diversi segnali quali, diarrea, vomito, nausea ma sono solo alcuni, scopri tutti i sintomi
Pingback: herbal incense fast delivery
Pingback: mr happy incense
Pingback: cheap herbal incense
Pingback: cheap spice
Pingback: Climb
Pingback: buy spice online
Pingback: Situs Judi Poker Online Terpercaya
Pingback: cheap spice
Pingback: trash bin rental
Pingback: dumpster rental Ocoee
Pingback: cheap potpourri
Pingback: credit repair software
Pingback: Judi Poker Online Terpercaya
Pingback: Situs Judi QiuQiu Poker Online Indonesia
Pingback: dumpster rental nj
Pingback: credit repair letters
Pingback: dumpster rental nj
Pingback: 30 yard roll off dumpster
Pingback: need to rent a dumpster
Pingback: dumpster rental glen ellyn
Pingback: www.cpacomentarios.pt/
Pingback: scooby snax
Pingback: dumpster rental winnetka
Pingback: herbal incense online
Pingback: ??µ? Eco Slim
Pingback: Prostect ??????
Pingback: commercial dumpster
Pingback: trash dumpster dimensions
Pingback: price of dumpster rental
Pingback: 5 yard dumpster
Pingback: roll off dumpster prices
Pingback: 30 yard dumpster cost
Pingback: roll off dumpster for sale
Pingback: 3DRendering
Pingback: Perth TOILET PLUMBING
Pingback: Anastacia Griest
Pingback: Venice fishing charters
Pingback: Kimberlee Rux
Pingback: mediabarterexchange
Pingback: cbd oil
Pingback: Gas and plumbing services
Pingback: natural ways to reduce inflammation
Pingback: deep sea fishing charters
Pingback: natural cure for sleeplessness
Pingback: School badges
Pingback: New Orleans charter fishing
Pingback: Shemika Lipsett
Pingback: Blocked Pipes Perth
Pingback: how to manage arthritis pain naturally
Pingback: gas plumbing perth
Pingback: snowboard boots and bindings
Pingback: Enamel badges
Pingback: New Orleans charter fishing
Pingback: gas plumbing perth
Pingback: c bd
Pingback: gas plumbing perth
Pingback: Almeta Hoefler
Pingback: c bd
Pingback: what does cbd help with
Pingback: University
Pingback: Licensed Money Lender Singapore
Pingback: page about a good service provider
Pingback: rent dumpster cost
Pingback: trash pick up services
Pingback: Interior Design Consultancy Singapore
Pingback: High Quality Trench Drains
Pingback: dumpster rental Edgebrook
Pingback: dumpster rental Alsip
Pingback: heavy duty chains for sale
Pingback: Thailand Rajabhat
Pingback: Drainage Solutions to Protect Your Home
Pingback: roll away dumpster
Pingback: temple run game
Pingback: summer dress
Pingback: formal dress
Pingback: maxi Dresses
Pingback: maxi Dresses
Pingback: truck service and repair
Pingback: summer dress
Pingback: best price dumpster rental
Pingback: dumpster trash removal
Pingback: rac roadside assistance
Pingback: cheap tow
Pingback: top insurance companies
Pingback: Cheap websites
Pingback: fake phone number
Pingback: ACV Mole Removal
Pingback: Louisiana fishing charter
Pingback: Where to buy a website for my small business
Pingback: ACV Mole Removal
Pingback: Sony Mobile Phone Price in Sri Lanka
Pingback: Where to buy a website for my small business
Pingback: Flat Mole Removal Apple Cider Vinegar
Pingback: Sony Xperia XZ Price In Sri Lanka
Pingback: Flat Mole Removal Apple Cider Vinegar
Pingback: ÃÒªÀѯàªÕ§ãËÁè
Pingback: Remove Moles On Face With Apple Cider Vinegar
Pingback: Sony Xperia XA1 Price in Sri Lanka
Pingback: Apple Ipad Air Price in Sri Lanka
Pingback: OnePlus 5Price in Sri Lanka
Pingback: Dildo
Pingback: Apple Iphone 7 Price in Sri Lanka
Pingback: Apple Iphone 7 Plus Lowest Price in Sri Lanka
Pingback: quality plumbing contractors
Pingback: international real estate
Pingback: licensed plumbers
Pingback: betboo
Pingback: youwin giriş
Pingback: goodyear computer repair
Pingback: hair loss treatment lombard
Pingback: PRP injection westmont
Pingback: avondale computer repair
Pingback: portable dumpster rental
Pingback: rijschool Rotterdam
Pingback: large dumpster rental
Pingback: coolsculpting weight loss
Pingback: hair loss in children
Pingback: Goedkope Rijschool Rotterdam
Pingback: www hair fall treatment
Pingback: insurance quotes auto
Pingback: auto recycler parts
Pingback: kids play set
Pingback: toddler swing set
Pingback: dirt dumpster rental
Pingback: wooden swing
Pingback: kids swings
Pingback: towing west bloomfield
Pingback: towing rochester hills
Pingback: cirugia laser de ojos en matamoros
Pingback: universidades en el valle de texas
Pingback: dich vu seo top 3
Pingback: Commercial Realtor Los Angeles
Pingback: SEO fanpage facebook
Pingback: place database
Pingback: doge casino
Pingback: tamilrockers kannada
Pingback: forex
Pingback: tamilrockers.wi
Pingback: doge casino
Pingback: kanavu variyam tamilrockers
Pingback: forex
Pingback: forex
Pingback: forex
Pingback: best weed grinder
Pingback: forex
Pingback: forex
Pingback: Rastreo de envio servientrega
Pingback: rastreo de envio
Pingback: envio de paquetes urgentes
Pingback: magento
Pingback: chelsea futbol club
Pingback: prepayment meter
Pingback: prepayment meter
Pingback: amazon
Pingback: water meters
Pingback: gas meters
Pingback: regalos para mujeres
Pingback: udemy coupon for students
Pingback: Microsoft Surface Book Laptop Backpack
Pingback: prepayment meter
Pingback: Dell Laptop Backpack
Pingback: 15.6 Laptop Backpack
Pingback: udemy coupon react
Pingback: New
Pingback: Samsung DSLR Camera Backpack
Pingback: udemy coupon excel
Pingback: Extended Stay Toronto
Pingback: Extended Stay Toronto
Pingback: smestaj starih lica
Pingback: pram stroller
Pingback: Tricycle Stroller
Pingback: buy taxi equipmemt
Pingback: taxi led light
Pingback: Pinoy Tambayan
Pingback: wireline cable counter
Pingback: dom za stare cene
Pingback: dom mitrovic
Pingback: gm cables
Pingback: air pressure gauges
Pingback: www.youtube.com/channel/UCGHehRRwBrrTVIXXuu_FDkw
Pingback: Golf Drivers 2017
Pingback: Best Golf Drivers
Pingback: Mango tea
Pingback: Melbourne Tea
Pingback: Best Japanese tea
Pingback: chromium sputter target
Pingback: aluminium sputter target
Pingback: aluminium sputter target
Pingback: tungsten sputter target
Pingback: Wedding venues in Essex
Pingback: low testosterone in men
Pingback: Spas in Essex
Pingback: online booklet printing services
Pingback: Home - Country House Essex
Pingback: classic postcards
Pingback: next day postcards
Pingback: Pharmapex Consumer Health
Pingback: athletics betting tips
Pingback: predictions
Pingback: deals
Pingback: dollars off
Pingback: promo codes
Pingback: predictions
Pingback: promotional codes
Pingback: darts betting tips
Pingback: vouchers
Pingback: online offers
Pingback: tipping
Pingback: betting tips uk
Pingback: percent off
Pingback: online offers
Pingback: percent off
Pingback: Betting tips site
Pingback: Mole Treatment Using Baking Soda And Castor Oil
Pingback: forex
Pingback: free auto insurance quotes
Pingback: cheap auto insurance rate
Pingback: online offers
Pingback: lowest auto insurance rates
Pingback: auto insurance quotes online
Pingback: GE Centricity Revenue Cycle Management
Pingback: resalvaged building materials
Pingback: View page
Pingback: Best original wedding cake ideas in 2017
Pingback: GE Centricity Medical Records
Pingback: social media marketing bali
Pingback: property management
Pingback: Best simple rustic wedding ideas in 2017
Pingback: upcycled furniture
Pingback: www.goo.gl/TfYHuW
Pingback: bathroom holder
Pingback: cherry hill construction
Pingback: bathroom towel rack
Pingback: custom furniture
Pingback: property management
Pingback: leg workout routine
Pingback: Best ideas for wedding centerpieces on a budget in 2017
Pingback: Best wedding gift ideas in 2017
Pingback: Castor Oil Mole Removal
Pingback: Baking Soda And Castor Oil For Moles
Pingback: How To Remove A Mole With Baking Soda And Castor Oil
Pingback: Mole Removal At Home With Castor Oil And Baking Soda
Pingback: Driveway Drains
Pingback: Orlando plumber
Pingback: Entertainment in Canton OH
Pingback: kids subscription box
Pingback: Party places for kid
Pingback: portable dumpster rental
Pingback: Holiday gifts 2017
Pingback: affordable dumpsters
Pingback: Holiday gifts for men
Pingback: trampoline park Canton
Pingback: bfi trash removal
Pingback: dumpster for yard waste
Pingback: dumpster rental attica
Pingback: dumpster rental highland park
Pingback: valentines day surprise boxes
Pingback: dumpster rental Hickory Withe
Pingback: dumpster sizes
Pingback: dumpster rental Brentwood
Pingback: valentines day surprise boxes
Pingback: rent a dumpster cost
Pingback: プラダスーパーコピー
Pingback: rent trash dumpster
Pingback: bfi dumpster rental
Pingback: Driveway Trench Drains
Pingback: Drains
Pingback: dumpster rental toronto
Pingback: エルメスコピー
Pingback: Job Placement Opportunities
Pingback: UoN
Pingback: zdes
Pingback: シャネルコピー
Pingback: blog
Pingback: visit source
Pingback: best holiday boxes
Pingback: surprise boxes for boyfriend
Pingback: Partytime Casino Dealers
Pingback: istochnik
Pingback: source
Pingback: SEO tips for beginners in 2017
Pingback: Holiday gifts for men
Pingback: vyisshee obrazovanie za granitsey
Pingback: SEO tips for website in 2017
Pingback: light
Pingback: Northern Ireland
Pingback: my blog
Pingback: Business Directory
Pingback: click
Pingback: IELTS preparation in Karachi
Pingback: Why do people become lawyers
Pingback: Questions to ask a divorce lawyer during initial consultation
Pingback: Ask a real estate lawyer free
Pingback: make money online
Pingback: online income
Pingback: Realestate
Pingback: panel
Pingback: guages
Pingback: console
Pingback: Click Here
Pingback: Buy Sex Toy Mumbai
Pingback: marker
Pingback: fridge repair perth
Pingback: Shop Now
Pingback: Click Here to Shop Now
Pingback: Shop Now
Pingback: Click Here
Pingback: dumpster rental algonac
Pingback: commercial real estate prices
Pingback: real estate training
Pingback: virtual world
Pingback: dumpster rental new haven
Pingback: real estate contract
Pingback: commercial business for rent
Pingback: vr games
Pingback: vr station
Pingback: roll away dumpster
Pingback: junk bin rental
Pingback: dumpster rental wolverine
Pingback: fifa 18 free download xbox
Pingback: dumpster rental Zilwaukee
Pingback: 30 cubic yard dumpster
Pingback: roll off dumpster
Pingback: trash dumpster service
Pingback: Next Day Flooring
Pingback: Global Market System
Pingback: Florida Divorce Law
Pingback: Terry Sacka AAMS
Pingback: Hardwood Floors
Pingback: SDR
Pingback: video porno de amadoras
Pingback: New Floors
Pingback: IMF
Pingback: hydration backpack
Pingback: leather backpack
Pingback: Divorce Lawyer
Pingback: Timesharing Florida
Pingback: umzug koln stuttgart kosten
Pingback: Make Money IN Online
Pingback: motu patlu games online
Pingback: hampton bay fan wiring
Pingback: umzug dusseldorf beginn
Pingback: authentic discount designer handbags
Pingback: healthcare retirement
Pingback: Locksmith in Mayfair
Pingback: city locksmith
Pingback: locksmith se22
Pingback: Locksmith in Woolwich
Pingback: London photo studio
Pingback: paydaycgtloansnhj.com
Pingback: model portfolio
Pingback: portrait photography
Pingback: tubepatrol.net
Pingback: quickbooks nonprofit
Pingback: qualifications for ssi disability benefits
Pingback: dumpster rental roseville
Pingback: Johnston Accounting
Pingback: camping gear
Pingback: tax preparation near me
Pingback: dumpster rental near me
Pingback: recycling dumpsters
Pingback: pokemon games of 2016
Pingback: camping tents
Pingback: hiking gear
Pingback: federal tax return
Pingback: how to get ash greninja in pokemon brick bronze
Pingback: chennai female escorts
Pingback: camping store
Pingback: construction trash bin rental
Pingback: internet marketing company in raleigh
Pingback: how to get ash greninja in pokemon brick bronze
Pingback: far infrared sauna benefits
Pingback: far infrared therapy
Pingback: how to crack minecraft windows 10 edition
Pingback: waste dumpster rental
Pingback: relationship
Pingback: panzoid for mac
Pingback: wet sauna
Pingback: infrared sauna home
Pingback: rolloff dumpster
Pingback: omarxc store spotify
Pingback: Web Design Long Island
Pingback: Custom web development
Pingback: cedar steam room
Pingback: Web Development
Pingback: Internet Marketing Long Island
Pingback: Iphone & IOS Apps
Pingback: Palhetas
Pingback: Fotor Review
Pingback: manuten??o preventiva dire??o hidr?ulica
Pingback: how to make money with Level rewards
Pingback: how to make money with Level rewards
Pingback: Internet Marketing Long Island
Pingback: Ar Condicionado SP
Pingback: Carga de G?s Ar Condicionado Automotivo
Pingback: xxx video hd
Pingback: Locksmith in Penge
Pingback: Locksmith in Shoreditch
Pingback: locksmith n12
Pingback: Top appetite suppressants
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant Los Angeles
Pingback: Fashion Business
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant Los Angeles
Pingback: Fashion Business
Pingback: Startup Fashion
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant NYC
Pingback: Retail Consultant Los Angeles
Pingback: Fashion Business Consulting
Pingback: Startup Fashion
Pingback: Startup Fashion
Pingback: Fashion Business
Pingback: Retail Consultant NYC
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant NYC
Pingback: Retail Consultant Los Angeles
Pingback: Retail Consultant Los Angeles
Pingback: Fashion Business Consulting
Pingback: Fashion Business
Pingback: Fashion Business Consultant
Pingback: Fashion Business Consultant
Pingback: Mesothelioma Lawyer
Pingback: Retail Consultant Los Angeles
Pingback: Graphic design
Pingback: Startup Fashion
Pingback: Startup Fashion
Pingback: Fashion Business
Pingback: Retail Consultant NYC
Pingback: Fashion Business
Pingback: Advertising on Boeing
Pingback: How attract even more tourists
Pingback: Startup Fashion
Pingback: basement finishing suwanee
Pingback: Prices Digital Inflight
Pingback: Tourism marketing blog
Pingback: Youtube to mp3
Pingback: lab store
Pingback: common laboratory apparatus
Pingback: bikini modelleri
Pingback: hemÅire kostümü
Pingback: lab equipment used
Pingback: from cusco to puno
Pingback: lab glass equipment
Pingback: xxx hd video
Pingback: kayaking lake titicaca
Pingback: 1 day lake titicaca kayak
Pingback: laboratory apparatuses
Pingback: chemistry apparatus
Pingback: seo company in pune
Pingback: scientific equipment manufacturing company
Pingback: Mesothelioma Law Firm
Pingback: social psychology research
Pingback: psychology website
Pingback: anxiety research news
Pingback: yoga stuff
Pingback: latest news
Pingback: world news
Pingback: telephone reverse lookup
Pingback: free online movies
Pingback: online movies
Pingback: trash containers for rent
Pingback: 2 person sauna
Pingback: sauna detox
Pingback: popular movies
Pingback: rent trash container
Pingback: dry heat sauna kits
Pingback: popular movies
Pingback: смотреть онлайн фильмы 2017
Pingback: movie
Pingback: near infrared sauna therapy
Pingback: well data management software
Pingback: local dumpster rental companies
Pingback: fern c mlm
Pingback: Maharashtra SSC Results 2017
Pingback: cool sculpting Clarendon Hills
Pingback: PRP treatment chicago
Pingback: freeze body sculpting
Pingback: freeze off fat
Pingback: best hair loss shampoo
Pingback: movies
Pingback: indoor sauna kits
Pingback: portable wood sauna
Pingback: yonsalon trusted
Pingback: yonsalon safe store
Pingback: gifts for grandma
Pingback: American Pacific International Capital, Inc.
Pingback: bracelets jewelry
Pingback: Best Headphones
Pingback: charcoal face mask
Pingback: graphics cards reviews
Pingback: Yigang Tang
Pingback: Yigang Tang
Pingback: zeloporn.com
Pingback: universal remote control
Pingback: blackhead mask
Pingback: gifts for mom
Pingback: learning remote control
Pingback: teeth whitening
Pingback: tooth charcoal
Pingback: Michigan mesothelioma attorney
Pingback: probate help
Pingback: MB6-890 dumps
Pingback: charcoal teeth whitening
Pingback: charcoal face mask
Pingback: necklaces for women
Pingback: Apple Watch Strap
Pingback: London Shaping
Pingback: His Secret Obsession
Pingback: British plastic surgery
Pingback: London Shaping
Pingback: Apple iWatch Band
Pingback: here
Pingback: here
Pingback: TAI Robotic Review
Pingback: Binary Options
Pingback: android porn app
Pingback: TAI Robotic Software
Pingback: android porn
Pingback: beegcom
Pingback: Mesothelioma Law Firm
Pingback: Morocco Ecommerce website Design Company
Pingback: tv studio
Pingback: green screen studio
Pingback: Agence Web Maroc
Pingback: Morocco Website Design Company
Pingback: Maroc Web Agence conception
Pingback: hemp
Pingback: london bathrooms and kitchens showroom
Pingback: personalised gift
Pingback: cannabis
Pingback: printigo
Pingback: accept debit cards for mmj
Pingback: mj payment processing
Pingback: roca installations
Pingback: london kitchen installations
Pingback: make money
Pingback: condominio online
Pingback: fornecedores condom?nio
Pingback: Nick
Pingback: window washer
Pingback: Nick
Pingback: telephone engineer cheltenham
Pingback: Photography
Pingback: long range wifi installation
Pingback: rc drones uav
Pingback: garcinia cambogia calcium
Pingback: Landline Man Telephone Engineer
Pingback: landline man reviews
Pingback: telephone engineer hereford
Pingback: garcinia cambogia extract buy online
Pingback: best deals on drones
Pingback: garcinia cambogia for men
Pingback: telephone engineer bath
Pingback: telephone engineer gloucester
Pingback: getnugg
Pingback: e9 locksmith
Pingback: High discount Amazon Giftcards
Pingback: pot valet promo
Pingback: Super Cheap iTunes Giftcards
Pingback: hackney locksmith
Pingback: marijuana
Pingback: faster rural broadband connection anywhere
Pingback: english tutor
Pingback: telephone engineer gloucester
Pingback: AmazingTalker
Pingback: antique auctioneer
Pingback: trash pickup
Pingback: English
Pingback: chinese tutor
Pingback: marijjuana discounts
Pingback: getnugg
Pingback: dumpsters rental prices
Pingback: Japanese
Pingback: sales enablement
Pingback: home trash removal
Pingback: dumpster rental phoenix
Pingback: spanish tutor
Pingback: mayweather vs mcgregor free stream
Pingback: chinese
Pingback: korean
Pingback: spanish
Pingback: dumpster sizes
Pingback: dumpster rental phoenix
Pingback: junk hauling services
Pingback: VipBad Hot Clips
Pingback: dumpster bin rental
Pingback: trash containers rental
Pingback: jailbreak 10.3.2
Pingback: bin rental prices
Pingback: HD Tube Videos 2017
Pingback: HD Tube Videos 2017
Pingback: Chiropractic Worcester
Pingback: Chiropractic Orlando
Pingback: carriage clock repair
Pingback: HD Tube Videos 2017
Pingback: Clock Repair Farmington Twp
Pingback: similarpornsites.net
Pingback: japanese tutor
Pingback: list57com
Pingback: Clock Repair Madison Heights
Pingback: Chiropractic Odesa
Pingback: anniversary clock repair
Pingback: list57.com
Pingback: list57com
Pingback: list57
Pingback: Hand-picked Laptops for College Students
Pingback: moving company
Pingback: clock Repair Flower Mound
Pingback: moving reinvented
Pingback: dryer vents
Pingback: antique clock repair & restoration
Pingback: local movers app
Pingback: local movers in charlotte
Pingback: dry heat sauna
Pingback: chelsea clock repair
Pingback: movers
Pingback: sunlighten sauna
Pingback: is infrared sauna safe
Pingback: local moving company
Pingback: movers in charlotte
Pingback: dryer roof vents
Pingback: Increased drying time
Pingback: mobile app for movers
Pingback: Vent
Pingback: on demand moving company
Pingback: home steam room cost
Pingback: warren emergency roadside service
Pingback: moving company
Pingback: Yellow nails cured
Pingback: nail fungus treatment
Pingback: dryer vent size
Pingback: marriage
Pingback: towing redford
Pingback: yellow nails remedy
Pingback: marriagememes
Pingback: Yellow Toenails
Pingback: home remedy for nail fungus
Pingback: marriagememes.org
Pingback: intimacy in marriage
Pingback: marriage
Pingback: Hong Kong Web Design
Pingback: marriage forums
Pingback: marriage help
Pingback: marriage
Pingback: nonton movie semi hd
Pingback: marriagememes.org
Pingback: Facebook
Pingback: marriagememes
Pingback: cuba rentals
Pingback: Timberland
Pingback: advice
Pingback: marriagememes.org
Pingback: marriage forums
Pingback: marriagememes.org
Pingback: marriage advice
Pingback: cuba rentals
Pingback: Logo
Pingback: Marriage Humor
Pingback: marriage memes
Pingback: blues
Pingback: Marriage Humor
Pingback: cuba vacation rentals
Pingback: marriagememes
Pingback: marriage help
Pingback: chartered bus
Pingback: aibeauty
Pingback: marriagememes
Pingback: Harley Davidson Motorcycles
Pingback: marriagememes
Pingback: tieba.baidu.com/p/5200557354
Pingback: marriage
Pingback: marriagememes
Pingback: marriage help
Pingback: car rentals in cuba
Pingback: vacation in cuba
Pingback: marriagememes
Pingback: AZ Movies
Pingback: tieba.baidu.com/p/5200491387
Pingback: Marriage Humor
Pingback: Go Pro
Pingback: marriage
Pingback: Corrugated Packaging Box
Pingback: swarovsky jewelry
Pingback: Marriage Humor
Pingback: alona aaron
Pingback: intimacy in marriage
Pingback: alona chaim aaron
Pingback: marriage
Pingback: Trauma
Pingback: PP Corrugated sheet
Pingback: how to sing like a pro
Pingback: how to sing
Pingback: Coroplast Packaging Box
Pingback: learn to sing harmony
Pingback: coroplast 4x8 sheet
Pingback: south American travel
Pingback: learning to read
Pingback: singing coach
Pingback: baby products
Pingback: sleep miracle
Pingback: mobile car detailing toronto
Pingback: ascom
Pingback: ciberseguridad
Pingback: Tiler Navan
Pingback: Tiler Navan
Pingback: Tiler Navan
Pingback: fashion dresses
Pingback: Glass balustrades coquitlam
Pingback: environmental impact assessment
Pingback: marketing agency
Pingback: dryer vent installation
Pingback: Dryer fire
Pingback: environmental impact assessment
Pingback: infrared spa
Pingback: Golf courses
Pingback: top quality glass railings
Pingback: ch digital marketing agency
Pingback: ch digital marketing
Pingback: ch digital creative design
Pingback: buy home sauna
Pingback: dryer systems
Pingback: glass guardrails
Pingback: Environmental impact Assessment
Pingback: metal ducting
Pingback: volaris
Pingback: Brand Expansion
Pingback: horse emoji instagram
Pingback: garbage dumpster
Pingback: Franchise opportunities in India
Pingback: Environmental consulting
Pingback: emoji horse black white
Pingback: Golf apps
Pingback: trash haulers
Pingback: horse emoji - fun mojis & stickers
Pingback: How to start a conversation with a girl you like
Pingback: princess cut engagement ring
Pingback: problem with dishwasher
Pingback: bedding and bath
Pingback: environmental impact assessment
Pingback: These are the best 4 ways to meet someone
Pingback: moving dumpster
Pingback: cooking dining and kitchen equipment
Pingback: horse and equestrian lovers
Pingback: Facilities for Hire
Pingback: Environmental impact Assessment
Pingback: lg tromm dryer repair
Pingback: speed queen dryer repair manual
Pingback: home depot kitchen design tool online
Pingback: Franchise Opportunities
Pingback: ch digtial brand
Pingback: Abu Dhabi and The UAE
Pingback: school facilities to hire
Pingback: real instagram followers
Pingback: chdigital.com
Pingback: instagram growth
Pingback: near infrared sauna
Pingback: graphic design
Pingback: horse face emoji meaning
Pingback: horse emoji gun emoji
Pingback: same day appliance repair
Pingback: Instagram marketing
Pingback: health and beauty tips
Pingback: hire school hall
Pingback: Graphic Design
Pingback: buy generic propecia
Pingback: Saudi Arabia
Pingback: NEW SPORT
Pingback: Harley Davidson Custom Motorcycles
Pingback: Harleys
Pingback: WINTER FUN
Pingback: iwit well integrity
Pingback: phd in europe
Pingback: Harleys
Pingback: Motorhome Dash covers
Pingback: fees for mba in usa
Pingback: Up and Up
Pingback: Mens tungsten rings
Pingback: Titanium rings
Pingback: copier ou innover
Pingback: play lotto max online quebec
Pingback: class a motorhome dash covers
Pingback: Harley Davidson Walkarounds
Pingback: counter strike global offensive skins
Pingback: oxand well integrity system
Pingback: play lottery online louisiana
Pingback: INNOVATIVE TOYS
Pingback: oil well integrity test
Pingback: oxand well integrity pdf
Pingback: reussir sa carriere
Pingback: Motorhome Dash covers
Pingback: Security service
Pingback: play lotto max online quebec
Pingback: study in canada for international students
Pingback: Mens gold rings
Pingback: KIDS TOYS
Pingback: tubetria.mobi
Pingback: Buy csgo skins
Pingback: Harley Davidson
Pingback: Security surveillance
Pingback: mba in uk
Pingback: adwords
Pingback: play lotto online zimbabwe
Pingback: Mens wedding rings
Pingback: decomworld well integrity system
Pingback: Mens fashion accessories
Pingback: Harley Davidson Motorcycles
Pingback: Mens titanium rings
Pingback: Harley Davidson
Pingback: study in new zealand and get pr
Pingback: Security surveillance
Pingback: Mens fashion accessories
Pingback: Mens jewelry
Pingback: divorce attorney
Pingback: bankruptcy lawyer
Pingback: Harley Davidson Walkarounds
Pingback: chapter 13 bankruptcy
Pingback: Wedding rings
Pingback: Mens fashion accessories
Pingback: Mens rings
Pingback: best binary option brokers
Pingback: Harley Davidson Walkarounds
Pingback: povecanje obiska
Pingback: forex no deposit bonus
Pingback: top medical colleges abroad
Pingback: broker reviews forex
Pingback: best binary option brokers
Pingback: spletni marketing
Pingback: Mens wedding bands
Pingback: Harley Davidson Walkarounds
Pingback: online lotto play euro mega powerball
Pingback: motorhome dashmat
Pingback: Harley Davidson Custom Motorcycles
Pingback: facebook oglasevanje
Pingback: study in france cost
Pingback: active rv dash covers
Pingback: top 10 mba in usa
Pingback: HiTutor - Interactive English Education
Pingback: Mens wedding bands
Pingback: Harley Davidson Custom Motorcycles
Pingback: motorhome dashmat
Pingback: best forex trading reviews
Pingback: Harley Davidson Motorcycles
Pingback: custom flags
Pingback: buy custom flag
Pingback: harleywalkaround.com
Pingback: rv dash cover by active
Pingback: buy custom flag
Pingback: Motorhome Dash covers
Pingback: Dieta para emagrecer
Pingback: RV dash covers
Pingback: Harley Davidson
Pingback: Harley Davidson Motorcycles
Pingback: Curriculum
Pingback: propeciahub.com
Pingback: Fox 6 milwaukee
Pingback: newspaper job adverts
Pingback: rent
Pingback: sell motorcycle
Pingback: boil remover
Pingback: boil removal
Pingback: top 40 songs today
Pingback: BEST FREE FOREX SIGNALS PROVIDERS
Pingback: Pesta babulang
Pingback: OIL SIGNALS
Pingback: Top 10 Forex Trading Indicators
Pingback: southwindresort
Pingback: youtube top 40
Pingback: Forex Books
Pingback: Cheap hotels in kuching
Pingback: u k top 40
Pingback: Funniesty Jokes
Pingback: funny adult jokes
Pingback: TRADER
Pingback: Tourist spots in kuching
Pingback: Mississippi vacation rentals
Pingback: Top 10 Binary Options Bonuses
Pingback: Kuching seafood
Pingback: Binary Options Education
Pingback: Biloxi Apartments
Pingback: Laksa sarawak
Pingback: Independence Day Images 2017
Pingback: Places to eat seafood
Pingback: OIL SIGNALS
Pingback: FOREC CHARTING
Pingback: Places to eat in kuching
Pingback: Learn Binary Options Trading
Pingback: Jokes
Pingback: Funniesty Jokes
Pingback: Economic Calendar
Pingback: jobs after uni
Pingback: Funniesty Jokes
Pingback: e-commerce near me
Pingback: funnyjoke.online
Pingback: Funniesty Jokes
Pingback: automobiles general fashion
Pingback: summer handcrafted
Pingback: Kuching travel tips
Pingback: general fashion clothing
Pingback: Sarawak cultural village
Pingback: Southwind Resort
Pingback: Managed Forex Accounts Provider
Pingback: Biloxi Corporate rentals
Pingback: Jokes
Pingback: online shopping tools
Pingback: Currency Trading Software
Pingback: Spiritual Quotes
Pingback: Spiritual Quotes
Pingback: shelter homeless
Pingback: Kuching sarawak
Pingback: Quotes
Pingback: sweepstake online
Pingback: cong ty in bao bi giay
Pingback: Biloxi vacation rentals
Pingback: in offset
Pingback: in an tui giay
Pingback: bags health and
Pingback: Laksa soup
Pingback: cong ty in an
Pingback: other iphone electronic
Pingback: Funniesty Jokes
Pingback: electronic automobiles general
Pingback: toys other
Pingback: spiritual-quotes.org
Pingback: Quotes
Pingback: Top 10 Forex Hedge Funds
Pingback: How To Get Rid Of Skin Moles With Honey And Flaxseeds
Pingback: e-commerce near me
Pingback: general fashion
Pingback: maps london
Pingback: Best Binary Options Affiliate Programs
Pingback: health and
Pingback: Best Way To Remove Moles
Pingback: health and toys
Pingback: themavencircle.com
Pingback: Forex Forum
Pingback: clothing accessories bags
Pingback: online best
Pingback: cheap iphone 7
Pingback: Anxiety Support Website
Pingback: Adventures philippines
Pingback: themavencircle.com
Pingback: Best Social Trading Networks
Pingback: Anxiety
Pingback: cheap macbook pro
Pingback: Quotes
Pingback: calm mind
Pingback: Anxiety Support Website
Pingback: other iphone
Pingback: Lovely Brasov
Pingback: The Maven Circle
Pingback: Quotes
Pingback: calm mind
Pingback: themavencircle.com
Pingback: Digital Marketing Agency
Pingback: Depression
Pingback: bay of fundy tide times
Pingback: spiritual-quotes.org
Pingback: Cheap Amazon Giftcards and Discounted iTunes Giftcards
Pingback: Spiritual Quotes
Pingback: bay of fundy facts
Pingback: Digital Marketing Agency
Pingback: themavencircle.com
Pingback: Marketing
Pingback: Anxiety Support Website
Pingback: calm mind
Pingback: top hotel websites
Pingback: spiritual-quotes.org
Pingback: Remove Moles Using Flaxseed and Honey
Pingback: Quotes
Pingback: meditation
Pingback: hyperbody preco
Pingback: Best Way To Remove Moles
Pingback: calm mind
Pingback: calm mind
Pingback: best wart removal
Pingback: wart removal home remedies
Pingback: spiritual-quotes.org
Pingback: calm mind
Pingback: Inspirational Quotes
Pingback: best priced hotels
Pingback: work from home
Pingback: removing warts
Pingback: Quotes
Pingback: Depression
Pingback: vr teen movie sex
Pingback: The Maven Circle
Pingback: online surveys
Pingback: fashion clothing
Pingback: how to get rid of hpv warts
Pingback: Anxiety Support Website
Pingback: make money online
Pingback: calm mind
Pingback: calm mind
Pingback: Inspirational Quotes
Pingback: home security
Pingback: The Maven Circle
Pingback: Inspirational Quotes
Pingback: other fun
Pingback: virtual reality porn movie
Pingback: virtual reality porn sex
Pingback: e marketing
Pingback: spiritual-quotes.org
Pingback: Depression
Pingback: Anxiety Support Website
Pingback: Remove Moles Using Flaxseed and Honey
Pingback: Anxiety Support Website
Pingback: themavencircle.com
Pingback: Nudists spreading legs to show pussy and asshole Join GigPorn Now!
Pingback: Spiritual Quotes
Pingback: digital agency
Pingback: utah photographers
Pingback: online advertising agency
Pingback: Anxiety
Pingback: dedicated
Pingback: Flaxseeds and Honey Skin Mole Remover
Pingback: dedicated servers
Pingback: dedicated servers
Pingback: Anxiety Support Website
Pingback: auto Affiliate Program
Pingback: Wedding Photographers in park city
Pingback: vr porn 360
Pingback: Webmaster Show Case World Global New Sensations Films Access!
Pingback: sociotraffic.com
Pingback: Wedding Photographers in Salt Lake
Pingback: utah family photographer
Pingback: Depression
Pingback: dedicated servers
Pingback: virtual reality stream
Pingback: themavencircle.com
Pingback: Anxiety Support Website
Pingback: buy facebook page likes
Pingback: cheap servers
Pingback: spiritual-quotes.org
Pingback: vr porn smartphones
Pingback: The Maven Circle
Pingback: psychic texts UK
Pingback: vr porn smartphones 180
Pingback: buy adult fidget spinner
Pingback: spiritual-quotes.org
Pingback: Anxiety
Pingback: fidget toys for adults
Pingback: Mini Countryman pareri
Pingback: VR Bangers review
Pingback: LED light fidget spinner
Pingback: meditation
Pingback: airport limousine miami
Pingback: car service ft lauderdale to miami
Pingback: raid repair
Pingback: airport service miami
Pingback: Inspirational Quotes
Pingback: Inspirational Quotes
Pingback: data recovery specialist
Pingback: data recovery services
Pingback: Wow Girls Have Massive Orgasms Love Massive Cock Fucking Fun!
Pingback: cloud servers
Pingback: Danielle FTV 4K Porn Cams Films Superstar Access Join Now!
Pingback: Anxiety
Pingback: plantar fasciitis socks
Pingback: spiritual-quotes.org
Pingback: Spiritual Quotes
Pingback: spiritual-quotes.org
Pingback: Inspirational Quotes
Pingback: Youtube World 4K Porn Portal Network Informations!
Pingback: spiritual-quotes.org
Pingback: plantar sleeves
Pingback: plantar fasciitis socks
Pingback: Mexican Latino Sweet Yummy 4K HD Squirting Pussy Porn!
Pingback: cheap dedicated servers
Pingback: spiritual-quotes.org
Pingback: Sports Video App
Pingback: Hustler Megapass Presents By Larry Flint The King Of Porn Join Now!
Pingback: ebony big tits
Pingback: Spiritual Quotes
Pingback: Dogfart Network Entertainment Presents Over 22 Sites 1,416 Girls Join Now!
Pingback: Virtual Porn 360 review
Pingback: Spiritual Quotes
Pingback: spiritual-quotes.org
Pingback: Mobile Games
Pingback: Tiny Teens 18 Get There Pussy Banged Like Its The End Of The World!
Pingback: Inspirational Quotes
Pingback: Spiritual Quotes
Pingback: spiritual-quotes.org
Pingback: merch
Pingback: virtual reality gay
Pingback: Spiritual Quotes
Pingback: Spiritual Quotes
Pingback: Spiritual Quotes
Pingback: Anxiety Support Website
Pingback: Mobile Games
Pingback: Internet Search Engines Porn Search Links!
Pingback: Education canine puppy
Pingback: Blue Blood's New Gothic Sluts Pornstars All Access Films Join Now!
Pingback: Quotes
Pingback: Spiritual Quotes
Pingback: themavencircle.com
Pingback: Phone Mount
Pingback: grainsofearth.org
Pingback: Evil Doctos Bang Pussy Like Hell Fire ON Here LOok Now Hot Stuff!
Pingback: grainsofearth.org
Pingback: Inspirational Quotes
Pingback: grainsofearth.org
Pingback: grainsofearth.org
Pingback: grainsofearth.org
Pingback: grainsofearth.org
Pingback: BongaCams Thousands Of Girls-Guys Live Explicit Nude Webcams 4K HD!
Pingback: Join Now to Watch Full HI-DEF Version of this Movies BigCocks Loves Pussy
Pingback: Promotion
Pingback: Go Here
Pingback: themavencircle.com
Pingback: Grains of Earth
Pingback: Google Search Engine Porn 4K HD Portals!
Pingback: JAPAN'S SEXIEST SHAVED PUSSIES SMELL LIKE CHERRY LOOK NOW JOIN!
Pingback: Inspirational Quotes
Pingback: Grains of Earth
Pingback: Welcome to HQPornsites Plus Get Tons Of FREE BONUS PORN SITES !
Pingback: Grains of Earth
Pingback: Grains of Earth
Pingback: best stretch mark cream
Pingback: grainsofearth.org
Pingback: Depression
Pingback: Live Casino
Pingback: grainsofearth.org
Pingback: best stretch mark treatment
Pingback: stretch mark treatment
Pingback: Grains of Earth
Pingback: stretch mark removal
Pingback: grainsofearth.org
Pingback: Read More Here
Pingback: hersey customs
Pingback: steel
Pingback: PornHub 4k Hd Entertainment Information Movies!
Pingback: stretch mark removal
Pingback: grainsofearth.org
Pingback: Grains of Earth
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: best stretch mark treatment
Pingback: Marlyn Deveaux
Pingback: grainsofearth.org
Pingback: Bunny Benard
Pingback: Grains of Earth
Pingback: Grains of Earth
Pingback: Roselle Prost
Pingback: Grains of Earth
Pingback: west virgina roots
Pingback: grainsofearth.org
Pingback: grainsofearth.org
Pingback: Codi Broaddus
Pingback: Grains of Earth
Pingback: Jessenia Beede
Pingback: Grains of Earth
Pingback: steel sign
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: Carmen Callaway Films Also Free Bonus Of Over 25 Sites Deal Special!
Pingback: What One Million Dollars Buys
Pingback: Hustler Mega Porn World Massive Entertainment Movies!
Pingback: west virgina roots
Pingback: Marcella Cogburn
Pingback: whatonemillionbuys.com
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: Network Support Barnsley
Pingback: herb grinder
Pingback: grainsofearth.org
Pingback: Tank Trouble Unblocked
Pingback: grainsofearth.org
Pingback: grainsofearth.org
Pingback: What One Million Dollars Buys
Pingback: What One Million Dollars Buys
Pingback: Laptop Repairs Barnsley
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: Happy Wheels full version
Pingback: What One Million Dollars Buys
Pingback: grainsofearth.org
Pingback: What One Million Dollars Buys
Pingback: whatonemillionbuys.com
Pingback: IT Support Barnsley
Pingback: Browser games
Pingback: What One Million Dollars Buys
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: Grains of Earth
Pingback: Nutri Genetics
Pingback: grainsofearth.org
Pingback: whatonemillionbuys.com
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: lingotes de oro degussa
Pingback: How to eliminate skin tags
Pingback: How to get rid of skin tags
Pingback: Cal Berkeley
Pingback: Skin tag surgery
Pingback: red lingerie
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: mad hatter jacket
Pingback: indoor steam sauna
Pingback: What One Million Dollars Buys
Pingback: in house sauna
Pingback: grainsofearth.org
Pingback: Grains of Earth
Pingback: howl's moving castle sophie dress
Pingback: Grains of Earth
Pingback: What One Million Dollars Buys
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: Grains of Earth
Pingback: grainsofearth.org
Pingback: infrared sauna pod
Pingback: Grains of Earth
Pingback: whatonemillionbuys.com
Pingback: grainsofearth.org
Pingback: What One Million Dollars Buys
Pingback: tobacco flavor vaping pen
Pingback: http://onhudson.typepad.com/onhudsoncom/2011/01/new-york-winter-jazzfest-2011-january-7-8-b-there-or-b-square.html
Pingback: cost to build a home sauna
Pingback: What One Million Dollars Buys
Pingback: cheating husband
Pingback: pre built sauna
Pingback: whatonemillionbuys.com
Pingback: domestic sauna
Pingback: M5 at Jalan Mutiara
Pingback: http://onhudson.typepad.com/onhudsoncom/2009/02/ice-sailing-conditions-as-good-as-they-come.html
Pingback: What One Million Dollars Buys
Pingback: appliance doctor
Pingback: pet seat cover
Pingback: whatonemillionbuys.com
Pingback: fragoulakis
Pingback: What One Million Dollars Buys
Pingback: http://onhudson.typepad.com/onhudsoncom/2010/11/short-line-bus-tours-new-york-port-authority-woodbury-commons-midnight-madness-sale-departures-thurs.html
Pingback: What One Million Dollars Buys
Pingback: whatonemillionbuys.com
Pingback: actual-news.pro
Pingback: whatonemillionbuys.com
Pingback: New Launch Condo
Pingback: whatonemillionbuys.com
Pingback: What One Million Dollars Buys
Pingback: monoseis
Pingback: maytag performa dryer
Pingback: whatonemillionbuys.com
Pingback: What One Million Dollars Buys
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: whirlpool gold
Pingback: the appliance center
Pingback: whirlpool washing machine troubleshooting
Pingback: Shop women's clothes online
Pingback: Boatload online shopping store
Pingback: whatonemillionbuys.com
Pingback: whatonemillionbuys.com
Pingback: Shop all latest gadgets online
Pingback: What One Million Dollars Buys
Pingback: M5 at Jalan Mutiara Floor Plans
Pingback: Shop women's clothes online
Pingback: Freehold Condo Singapore
Pingback: M5 Condo Floor Plans
Pingback: http://onhudson.typepad.com/onhudsoncom/2009/10/bear-mountain-skating-rink-schedule.html
Pingback: http://onhudson.typepad.com/onhudsoncom/2011/04/richard-branson-calculating-a-partner-to-slay-goliath-.html
Pingback: http://onhudson.typepad.com/onhudsoncom/2010/03/first-annual-virtual-artists-exhibit-saturday-april-10th-2010.html
Pingback: http://onhudson.typepad.com/onhudsoncom/2009/03/httpwwwlohudcomarticle20090301news029030103311018news02tarrytown-riverfront-project-keeps-flowingstacy-a-anderson.html
Pingback: What One Million Dollars Buys
Pingback: Dr Jawahar Thomas
Pingback: judgment
Pingback: Dr J Thomas
Pingback: sexo gratis porn pt porno portugues
Pingback: putas no porn pt festa pornografica portuguesa
Pingback: travestis
Pingback: dymo label
Pingback: Jawahar Thomas
Pingback: dymo label
Pingback: label printing
Pingback: videos gays
Pingback: videos amadoras
Pingback: Elder Scrolls Online Guide 2017
Pingback: Junkyards in new york
Pingback: junkyards in maine
Pingback: working of access control system
Pingback: smart card access control system
Pingback: biometrics access control
Pingback: door access control system with camera
Pingback: ankle protection
Pingback: 2017 ankle braces
Pingback: affordable ankle brace
Pingback: arch support
Pingback: 2 week Diet
Pingback: Viddyoze Live Action Software by Joey Xoto OTO Upsell
Pingback: home roofs
Pingback: residential roofing materials
Pingback: 2 week Diet Plan
Pingback: what does a roof cost
Pingback: Poker Online
Pingback: multi angle template tool
Pingback: multi angle template tool
Pingback: steel roofing
Pingback: stainless steel angle template tool
Pingback: hansons roofing
Pingback: roof replacement brisbane
Pingback: Red Oaks Roofing of Madison heights mi 248-655-7057
Pingback: certified roofing
Pingback: wedding up lighting
Pingback: Hvac Philadelphia
Pingback: wedding lighting
Pingback: 24 hour ac repair in Philadelphia
Pingback: Decal Design
Pingback: agen togel terbesar
Pingback: free xbox microsoft points
Pingback: GPA76 Alkaline Battery
Pingback: poker online
Pingback: GPA76 Alkaline Cell
Pingback: how to get free microsoft points
Pingback: microsoft point generator
Pingback: free xbox microsoft points
Pingback: how to get free microsoft points
Pingback: L1154 Vinnic Battery
Pingback: WCLR44 Button Cell Battery
Pingback: 357A Button Cell
Pingback: free xbox microsoft points
Pingback: poker online tips
Pingback: situs Judi Poker online
Pingback: cougar dating sites
Pingback: cougar dating sites
Pingback: agen togel terpercaya 2017
Pingback: AG13 Button Cell
Pingback: Best Poker Website in Town
Pingback: 76A Battery
Pingback: millionaire dating sites
Pingback: telugu movies online
Pingback: telugu film
Pingback: houston pre-employment screening
Pingback: part time jobs for students
Pingback: driving records
Pingback: landlord credit check
Pingback: jobs near me part time
Pingback: Cinematic Pop
Pingback: Imagino
Pingback: locksmith
Pingback: houston credit checks
Pingback: Musica Latina
Pingback: company credit check
Pingback: la tattoo ink
Pingback: sell egift cards
Pingback: business credit check
Pingback: Analysis
Pingback: foam back roller
Pingback: houston background screening
Pingback: get a free trial and sell egift cards for your business
Pingback: Campo de Fuerza
Pingback: Miami
Pingback: landlord credit check service
Pingback: Analysis
Pingback: sell egift cards for your business
Pingback: send an egift card
Pingback: venezolano
Pingback: elektronik sigara
Pingback: commercial credit reports
Pingback: pre-employment screening
Pingback: watches watches wristwatches
Pingback: offer a promotion to my customers
Pingback: eleaf istick pro
Pingback: credit screening services
Pingback: watches bracelets
Pingback: set up a birthday club for my business
Pingback: pocket watches men
Pingback: credit check for landlord
Pingback: learn more about how egift cards can drive revenue for your business
Pingback: background checks houston tx
Pingback: children wooden toys
Pingback: Electrician near me
Pingback: Plugged up dryer vent
Pingback: landscape contractors near me
Pingback: corporate landscape
Pingback: children out door toys
Pingback: klobic.com/how-add-background-image-klobic/
Pingback: children's toy boxes
Pingback: klobic.com/blog/
Pingback: landscape trees
Pingback: raised bed garden
Pingback: cleaning dryer lint
Pingback: dryer vent connection
Pingback: klobic.com/how-to-design-and-post-ads-in-instagram-stories/
Pingback: electrician in Westlake Village
Pingback: electrician in Van Nuys
Pingback: klobic.com/create-responsive-html5-banner-ads/
Pingback: women's digital watches
Pingback: dryer installation
Pingback: landscape professionals
Pingback: klobic.com/perfectionism-kills-creativity-overcome/
Pingback: space saving dryer vent
Pingback: review
Pingback: streaming film semi
Pingback: ductwork fittings
Pingback: electricians in Van Nuys
Pingback: electricians in Port Hueneme
Pingback: vent covers
Pingback: Recommended Reading
Pingback: lawn mower heavy duty
Pingback: most reliable zero turn mower
Pingback: ride on zero turn mowers
Pingback: electricians in Port Hueneme
Pingback: electricians in Glendale
Pingback: refrigerator repair
Pingback: Recommended Reading
Pingback: bosch dishwasher repair
Pingback: electricians in Calabasas
Pingback: reset.me/story/study-long-term-marijuana-smoking-doesnt-significantly-harm-lungs/
Pingback: washer and dryer repair service
Pingback: www.blackenterprise.com/small-business/entrepreneurs-conference-how-janice-bryant-howroyd-built-a-billion-dollar-business/
Pingback: www.thegatewaypundit.com/2012/06/your-right-to-know-more-racy-photos-of-obamas-mother-discovered-video/
Pingback: reset.me/story/negative-thinking-the-number-one-cause-of-chronic-depression-and-how-to-overcome-it/
Pingback: www.thegatewaypundit.com/2013/01/michelle-obamas-inaugural-wear-cost-more-than-half-of-median-us-income/
Pingback: whirlpool refrigerators troubleshooting
Pingback: electricians in Thousand Oaks
Pingback: www.beautezine.com/chanel-launches-reformulated-rouge-coco-lipstick-this-spring/
Pingback: 12 foot dump trailer for sale
Pingback: electrician in Camarillo
Pingback: Accounting firms in Chicago
Pingback: buy learning toys children's
Pingback: reset.me/story/addiction-interruption-ibogaine-a-promising-treatment-for-opiate-addiction/
Pingback: www.thegatewaypundit.com/2012/12/union-thug-who-beat-steven-crowder-ided-his-name-is-tony-cummings-video/
Pingback: 5 by 10 trailers for sale
Pingback: electricians in Camarillo?
Pingback: reset.me/story/vitamin-hemp-6-ways-nutritive-hemp-seed-oil-good-eat-daily-basis/
Pingback: reset.me/story/watch-thc-kills-cancer-cells/
Pingback: reset.me/story/heres-why-cannabis-plants-are-growing-wild-all-over-britains-cities/
Pingback: www.blackenterprise.com/event/women-of-power/suzanne-shanks-siebert-bradford-shank-co/
Pingback: www.thegatewaypundit.com/2012/09/unreal-obama-invites-muslim-brotherhood-egyptian-leader-to-meet-next-week-refuses-to-meet-netanyahu/
Pingback: 4 car trailer
Pingback: 24 enclosed trailer for sale
Pingback: 2 car race trailer
Pingback: reset.me/story/psilocybin-the-magic-effect-of-mushrooms/
Pingback: www.thegatewaypundit.com/2012/03/catholic-bishops-cry-foul-amish-are-exempt-from-obamacare-but-catholics-are-not/
Pingback: utility trailer 5x8 for sale
Pingback: reset.me/story/parkinsons-disease-and-the-potential-of-cannabis-therapy/
Pingback: www.thegatewaypundit.com/2012/07/another-obama-record-number-of-americans-on-disability-exceeds-number-of-people-in-new-york/
Pingback: reset.me/video/how-psychedelics-are-saving-lives/
Pingback: where to buy enclosed trailers
Pingback: reset.me/story/archeological-evidence-suggests-prehistoric-humans-used-drugs/
Pingback: www.thegatewaypundit.com/2013/01/obama-administration-repositioning-homeland-security-ammunition-containers/
Pingback: best lehenga online shopping
Pingback: online lehenga shopping
Pingback: semi movie
Pingback: online snapdeal sarees
Pingback: bollywood actress lehenga online shopping
Pingback: reset.me/story/activate-your-vagus-nerve-to-stave-off-pain-and-inflammation/
Pingback: reset.me/story/man-cures-colon-cancer-with-cannabis-oil/
Pingback: reset.me/story/7-people-say-owe-huge-success-psychedelics/
Pingback: www.blackenterprise.com/news/black-farmers-to-receive-payouts-in-1-2-billion-from-federal-lawsuit-settlement/
Pingback: Check This Out
Pingback: Learn More Here
Pingback: article source
Pingback: More Bonuses
Pingback: Our site
Pingback: supernatural
Pingback: football Transfer News
Pingback: how to stop hijackers
Pingback: paranormal
Pingback: Tech
Pingback: choctaw tribe
Pingback: paranormal stories
Pingback: motion detection
Pingback: Satta Matka
Pingback: ghost stories
Pingback: security camera
Pingback: Dryer air flow
Pingback: towel holders
Pingback: grey bathroom accessories
Pingback: toilet paper holder
Pingback: reset.me/story/this-is-how-ayahuasca-heals-your-brain/
Pingback: dryer vent roof
Pingback: bathroom sets
Pingback: need cleaning
Pingback: reset.me/story/frankincense-the-king-of-essential-oils/
Pingback: dryer vent material
Pingback: WordPress Website Design
Pingback: reset.me/story/marijuana-the-super-antibiotic-of-the-future/
Pingback: www.thegatewaypundit.com/2011/09/more-crony-socialism-obama-gives-737-million-to-pelosis-brother-in-laws-solar-firm/
Pingback: Football Transfer Rumours
Pingback: reset.me/story/10-reasons-eating-daily-turmeric-make-happier-healthier/
Pingback: reset.me/story/what-doesnt-kill-you-really-can-make-you-stronger/
Pingback: internet marketing plan
Pingback: child abduction
Pingback: Interesting Read
Pingback: www.terrysacka.com
Pingback: online ordering
Pingback: places that deliver near me
Pingback: free delivery
Pingback: Hillary Clinton Email Corruption
Pingback: Timesharing
Pingback: Divorce Lawyer
Pingback: Divorce Attorney
Pingback: Florida Divorce Law
Pingback: Hiruscar
Pingback: Thai products
Pingback: bumebime soap
Pingback: small business consultant
Pingback: Omo
Pingback: Yanhee Acne Cream
Pingback: IDOL SLIM
Pingback: kitbag dortmund
Pingback: Sailboats for Sale
Pingback: Alada
Pingback: www.mypsychicadvice.com/category/psychic-vampire-chat-rooms.aspx
Pingback: Sailboats for Sale
Pingback: food photographer
Pingback: Thai products wholesale
Pingback: www.mypsychicadvice.com/
Pingback: Cathy Doll
Pingback: www.mypsychicadvice.com/
Pingback: www.mypsychicadvice.com/category/psychics-used-to-solve-crimes.aspx
Pingback: www.mypsychicadvice.com/
Pingback: social content creator
Pingback: Gel Hut Mun
Pingback: Sailboats for Sale
Pingback: Legacy Financial Advisors
Pingback: Adam and eve sex toys
Pingback: socket tool
Pingback: deep socket wrench
Pingback: Adam and eve sex toys
Pingback: Thaiwholesaler
Pingback: New England Schooner
Pingback: Adam and eve sex toys
Pingback: Adam and eve sex toys
Pingback: Wirral Escorts
Pingback: metric socket set
Pingback: Alternative Medicine
Pingback: Bucharest Elite Escorts
Pingback: Pocket Pussies
Pingback: Pocket Pussies
Pingback: best hunting knives
Pingback: Escorts Liverpool
Pingback: Bucharest Escort
Pingback: financial advisor in boston
Pingback: financial advisor in boston
Pingback: Orthopedic
Pingback: Pocket Pussies
Pingback: bread knife
Pingback: Urology
Pingback: 1xbet canli bahis
Pingback: TrackerTags Dog Walkers Pack
Pingback: TrackerTags Privacy Policy
Pingback: how to get a man to commit
Pingback: TrackerTags Blog
Pingback: Become a TrackerTags Seller
Pingback: Buy TrackerTags
Pingback: casinomilyon
Pingback: blankets for babies
Pingback: blankets for kids
Pingback: Justinbet giris
Pingback: Become a TrackerTags Dropshipper
Pingback: TrackerTags Single Tag
Pingback: pink baby blanket
Pingback: personalized baby blankets
Pingback: casinodunya
Pingback: Become a TrackerTags Promoter
Pingback: pink baby blanket
Pingback: white baby blanket
Pingback: Mybahis giris
Pingback: Buy 4 Smart Pet Tags
Pingback: eye liner
Pingback: TrackerTags Terms
Pingback: magnetic ankle brace
Pingback: arch support
Pingback: Twin Pack Smart Pet Tags
Pingback: eye shadows
Pingback: TrackerTags Mobile App Features
Pingback: Smart Pet Tag Features
Pingback: Hiperbet giris
Pingback: janitorial products
Pingback: eyeliner pencil
Pingback: TrackerTags is live
Pingback: floor cleaning equipment
Pingback: combination wrench
Pingback: Report Your Pet Found
Pingback: UK Lifestyle & Parenting blog
Pingback: Saraycasino canli bahis
Pingback: Launch for TrackerTags Imminent
Pingback: TrackerTags is born
Pingback: Adding Contact Details
Pingback: janitorial products
Pingback: Smart Tag Geo Location Testing
Pingback: adjustable wrench
Pingback: chain wrench
Pingback: Parent blog
Pingback: Payables Automation
Pingback: EIPP
Pingback: Dynamic Discounting
Pingback: drill driver
Pingback: Wellness
Pingback: Get the free Decluttering ebook
Pingback: Affordable Rustic Decor
Pingback: 4 simple creative Affordable Rustic Home Decor Ideas
Pingback: online moovie
Pingback: watch movies online
Pingback: embroidery design services
Pingback: how to digitize a logo for embroidery
Pingback: online digitizing
Pingback: digitizing embroidery services
Pingback: digitizers for embroidery
Pingback: embroidery machine digitizing
Pingback: digitizing embroidery
Pingback: digitize image for embroidery
Pingback: stubble beard trimmer
Pingback: embroidery conversion
Pingback: digitize for embroidery
Pingback: embroidery digitizing service
Pingback: Filling tax return
Pingback: digitize logo for embroidery
Pingback: embroidery conversion
Pingback: digitize jpeg
Pingback: DIGITIZER WATCH
Pingback: Nice watches for good prices
Pingback: KATOKA RETRO WATCH
Pingback: EXCURSIONIST BRACELET
Pingback: thai dating
Pingback: CAPTAIN AMERICA CUFFLINKS
Pingback: CATHENNA AUTOMATIC WATCH
Pingback: CALIBER BULLET NECKLACE
Pingback: AIRFORCE WATCH
Pingback: APOLLINE MECHANICAL WATCH
Pingback: best survival food
Pingback: SUPERMAN CUFFLINKS
Pingback: aplikasi akuntansi
Pingback: glass food storage containers
Pingback: AFFLUENT BOXING MITTS NECKLACE
Pingback: aplikasi inventory barang
Pingback: SELFIE LED LIGHT
Pingback: IRON MAN CUFFLINKS
Pingback: dslr camera
Pingback: good digital camera
Pingback: Watches Under $100
Pingback: CAPTAIN AMERICA SHIELD CUFFLINKS
Pingback: IRON MAN CUFFLINKS
Pingback: Charger Keychains
Pingback: digital slr
Pingback: digital slr camera
Pingback: needle nose pliers
Pingback: snap ring pliers
Pingback: vieri-centurion
Pingback: viajar
Pingback: Hot flash relief
Pingback: dumpster rental lansing
Pingback: dumpster rental South Lyon
Pingback: www.sixsistersstuff.com/2014/02/buffalo-chicken-quesadillas-recipe.html
Pingback: Night Butterflies
Pingback: dick
Pingback: pnc atm near me
Pingback: nyce atm network
Pingback: vieri-criptovaluta
Pingback: www.good4utah.com/gtu
Pingback: viagem
Pingback: hammer s
Pingback: dumpster rental brammel
Pingback: troncoso
Pingback: www.sixsistersstuff.com/2013/04/living-room-makeover-by-four-chairs.html
Pingback: Paris
Pingback: buy hammer
Pingback: hammer tool
Pingback: 2 yard dumpster
Pingback: hometrendsutah.blogspot.com/2013/02/living-room-decor-before-after.html
Pingback: houseofturquoise.com/2014/11/four-chairs-furniture-2.html
Pingback: link atm finder
Pingback: dumpster central
Pingback: www.allthingsthrifty.com/2016/03/all-things-color-19-colorful-pillows.html
Pingback: dumpster companies
Pingback: vieri-centurion
Pingback: carpet cleaning services
Pingback: viagens
Pingback: how to keep a guy interested
Pingback: open top container rental
Pingback: www.babesandkidsreview.com/2013/05/fresh-looks-for-your-home-from-downeast-home/
Pingback: bellcustomhomes.com/2016/03/17/home-paint-color-ideas-with-pictures/
Pingback: tool box
Pingback: vieri-starbit
Pingback: star atm locations
Pingback: business-solutions
Pingback: gas dryer not heating enough
Pingback: how to replace the heating element in a dryer
Pingback: www.sixsistersstuff.com/2014/07/juicy-marinated-steak-recipe.html
Pingback: collectibles
Pingback: spiral ducting
Pingback: solar
Pingback: flexible insulated duct
Pingback: bike
Pingback: www.architectureartdesigns.com/15-chic-transitional-dining-room-interior-designs-full-of-ideas/
Pingback: www.thecarpetbagger.org/2013/05/north-carolina-giant-furniture-tour.html
Pingback: commona-myhouse.blogspot.com/2013/06/design-101-design-terms-pronounciation.html
Pingback: industrial ductwork
Pingback: SociViral Coupon
Pingback: for-seniors
Pingback: premier-home
Pingback: www.sixsistersstuff.com/2014/07/homemade-fresh-blueberry-pancakes-with-blueberry-syrup.html
Pingback: problems with dryer
Pingback: houseofturquoise.com/2012/02/four-chairs-furniture-fun-stuff.html
Pingback: onekindesign.com/2015/08/14/light-filled-living-rooms-40-absolutely-brilliant-ideas/
Pingback: eatlivesplurge.blogspot.com/2014/07/july-obsessions.html
Pingback: www.sixsistersstuff.com/2013/10/four-chairs-furniture-dining-room-sale-and-giveaway.html
Pingback: whirlpool dishwasher repair
Pingback: advanced-surveillance
Pingback: 79ideas.org/2013/09/one-diferent-idea-round-kitchen-table.html
Pingback: houseofturquoise.com/2012/02/four-chairs-furniture-day-two.html
Pingback: www.amazinghousedesign.com/interior-design/fresh-furniture/
Pingback: commona-myhouse.blogspot.com/2016/03/throwback-thursday-today-calls-for-my.html
Pingback: Make up
Pingback: houseofturquoise.com/2015/08/dream-home-tour-day-one.html
Pingback: www.homebunch.com/tag/beach-cottage/
Pingback: houseofturquoise.com/2012/02/four-chairs-furniture-3.html
Pingback: residencestyle.com/incredible-dream-home-highland-utah/
Pingback: houseofturquoise.com/2015/12/four-chairs-furniture-millhaven-homes.html
Pingback: www.armelleblog.com/2011/03/diy-ikea-rast-dresser-to-bedside-table.html
Pingback: houseofturquoise.com/2011/06/day-two-dream-home-tour.html
Pingback: houseofturquoise.com/2012/12/four-chairs-furniture-hiya-papaya-2.html
Pingback: www.beautezine.com/sneak-peek-at-the-mac-tropical-taboo-collection-for-summer-2013/
Pingback: www.beautezine.com/spring-newbies-new-products-available-this-month/
Pingback: Video
Pingback: blog.explore.org/the-powerpuff-girls-cerebellar-hypoplasia/
Pingback: 30A
Pingback: blog.hcomicbook.com/2009/02/12/hardcore-banging-gay-bozos/
Pingback: White Sand
Pingback: nautica bedding
Pingback: 30A News
Pingback: affordable web designer
Pingback: daypack
Pingback: designer kids clothes
Pingback: teen bedding sets
Pingback: www.awardsdaily.com/2016/02/28/the-good-the-bad-and-the-goodbye-to-oscars-2016/
Pingback: blog.hcomicbook.com/2008/12/04/these-couples-love-full-games/
Pingback: kids store
Pingback: affordable website design
Pingback: blog.hcomicbook.com/2009/03/25/nice-3d-model-mandy-on-studio-shooting/
Pingback: www.beautezine.com/conair-infiniti-pro-the-ultimate-brush/
Pingback: empleo2.ugr.es/blog/2011/12/premios-billete-adecuado-2011/
Pingback: backpack purse
Pingback: www.awardsdaily.com/2016/10/25/tom-hanks-spoofs-sully-on-snl-and-david-pumpkins/
Pingback: natural hair
Pingback: how to grow your hair
Pingback: children's clothing stores
Pingback: www.awardsdaily.com/2016/10/09/duvernays-13th-is-an-urgent-call-for-reform-now-on-netflix/
Pingback: children's clothing
Pingback: reset.me/story/ayahuasca-shows-potential-to-treat-als/
Pingback: nail art kit price
Pingback: www.beautezine.com/make-up-for-ever-water-blend-foundation/
Pingback: www.blackenterprise.com/billboard/black-history-month-esther-jones-betty-boop/
Pingback: nail art machine
Pingback: skateboard trucks and wheels
Pingback: skateboard parts
Pingback: affordable web designer
Pingback: nail stickers
Pingback: www.blackenterprise.com/event/entrepreneurs-summit/entrepreneurs-summit-day-1/
Pingback: affordable website design
Pingback: www.blackenterprise.com/event/entrepreneurs-summit/personal-brand-celebrity-entrepreneur/
Pingback: nail decorations
Pingback: homemade beer
Pingback: Vacation
Pingback: www.bmxoutsiders.com/blog/sayonara-speed-tribes-deus-ex-machina-venice-ca/
Pingback: new skateboard
Pingback: windowsarena.ir/?????-news/??????-htc-one-m8-??????-???
Pingback: brewing kit
Pingback: skate clothing
Pingback: skateboards for kids
Pingback: fingernail decals
Pingback: affordable webdesigner
Pingback: girls toddler bedding
Pingback: toddler boy bedding sets
Pingback: Vacation
Pingback: toddler comforter
Pingback: Prague Escorts
Pingback: affordable webdesigner
Pingback: zapthink.com/2008/09/15/zapthink-soa-implementation-roadmap-30/
Pingback: mendlerfamily.com/cameron/blog/neca/cabal-kickball-online-fail-to-server-information/
Pingback: www.beautezine.com/sneak-peek-at-the-shu-uemura-eye-conic-30th-anniversary-collection-for-summer-2013/
Pingback: www.thecoli.com/threads/classyme-can-you-resend-that-pic.77437/page-2
Pingback: skyscraperpage.com/forum/showthread.php?p=6802346&mode=linear
Pingback: kellyrand.pressfolios.com/
Pingback: idea.informer.com/users/morninj
Pingback: www.mustangworld.com/forums/printthread.php?t=699022
Pingback: zzt.org/?p=database&search=ActionDemo
Pingback: www.beautezine.com/new-beauty-products-may-2016/
Pingback: johniac.blogspot.com/2011/10/position-paper-reforming-system-that-is.html
Pingback: www.alz.org/judyfund/overview.asp
Pingback: www.beautezine.com/nars-summer-2016-review/
Pingback: atheistfoundation.org.au/forums/showthread.php?t=20420
Pingback: www.thehouseofgames.org/index.php?t=1&a=10&s=a
Pingback: blog.hcomicbook.com/2009/04/04/check-out-these-gay-drawn-hotties/
Pingback: zapthink.com/2010/12/02/does-rest-provide-deep-interoperability/
Pingback: organizacjawypraw.pl/kontakt/
Pingback: www.webnamelist.com/alexa/Alexa_163.html
Pingback: www.awardsdaily.com/2015/11/29/jennifer-lawrence-joy-and-the-best-actress-race-poll/
Pingback: educational trips
Pingback: www.freerepublic.com/focus/f-news/3386888/posts
Pingback: stop doing things you hate
Pingback: www.blackenterprise.com/career/heres-why-leaders-are-made-not-born/
Pingback: www.joenickp.com/travel/therealtexas.html
Pingback: www.freerepublic.com/focus/news/3538163/posts?page=43
Pingback: adindex.citypages.com/rusty-taco-103215/2482321
Pingback: zzt.org/?p=database&search=Riegs
Pingback: hotchickswithdouchebags.com/blog/category/thoughts-and-links/page/3/
Pingback: www.mustangworld.com/forums/showthread.php?p=12255961
Pingback: wildhunt.org/tag/union-witch-trial
Pingback: 2016
Pingback: www.pics-about-space.com/what-are-pluto-s-moons-called?p=2
Pingback: kickerdaily.com/posts/2013/11/look-whos-campaigning-brazils-mr-balls-is-new-testicle-mascot/
Pingback: www.freerepublic.com/focus/news/3538163/posts?page=53
Pingback: thehouseofgames.org/index.php?t=10&id=68
Pingback: www.thehouseofgames.org/index.php?t=9&id=121
Pingback: rbutr.com/rbutr/WebsiteServlet?requestType=showLink&linkId=5816
Pingback: becuo.com/penny-2012
Pingback: beta.bitesquad.com/food/r-taco/26/reviews
Pingback: thehouseofgames.org/index.php?t=9&id=0
Pingback: Jong
Pingback: www.rddmag.com/development/features/583-restaurants-2-0
Pingback: most affordable top professional expert cv writing services
Pingback: skyscraperpage.com/forum/showthread.php?p=6772637
Pingback: skyscraperpage.com/forum/showthread.php?p=6773281
Pingback: cv distribution in services
Pingback: quotesgram.com/stalin-quotes-on-communism/
Pingback: maamoul cookies
Pingback: blog.amandapalmer.net/20141031/
Pingback: axelandash.com/sneakpeak/
Pingback: Cheapest hotels booking
Pingback: www.thehouseofgames.org/index.php?t=10&id=416
Pingback: local cable
Pingback: Mixed baklava
Pingback: www.correntewire.com/conference_for_a_constitutional_convention
Pingback: cinematreasures.org/theaters/7962
Pingback: power rangers download
Pingback: www.thegatewaypundit.com/2011/08/obamas-illegal-uncle-onyango-worked-at-liquor-store-sold-booze-to-kids/
Pingback: thehouseofgames.org/index.php?t=10&id=427
Pingback: oreaddaily.blogspot.com/2013_05_12_archive.html
Pingback: xcelsior loans
Pingback: www.thegatewaypundit.com/2010/08/500-of-us-black-farmers-sign-up-for-obamas-usda-reparations-video/
Pingback: igramlikes.com
Pingback: beta.bitesquad.com/food/r-taco/26/catering
Pingback: www.burnbrosbrew.com/2014/07/
Pingback: thehouseofgames.org/index.php?t=10&id=86
Pingback: in hop giay nhanh
Pingback: in an hop giay
Pingback: nimba-bike.org/events-2/calendar/
Pingback: loans hawaii
Pingback: www.australianmining.com.au/news/rio-tinto-rubbishes-merger-talks-boasts-shareholder-returns-2/
Pingback: sex video download
Pingback: in hop giay dep
Pingback: zzt.org/?p=database&search=TMQUESTREUPLOAD.zip
Pingback: in hop khau trang
Pingback: forum.skyscraperpage.com/showthread.php?p=6772498&page=5
Pingback: www.travel-directory.org/travel/162096.html
Pingback: www.lawresearch.com/cities/counties/tx.htm
Pingback: zzt.org/?p=database&search=PATHWAYS.zip
Pingback: justpornwap HD Sex Moviles
Pingback: zzt.org/?p=database&search=SLIDER.zip
Pingback: thehouseofgames.org/index.php?t=10&id=369
Pingback: Помощь психолога
Pingback: www.thehouseofgames.org/index.php?t=9&id=11
Pingback: cats crash arena turbo stars windows
Pingback: Bahis haberleri
Pingback: Cheapest hotels booking
Pingback: James A Bonfiglio
Pingback: WMS System
Pingback: idataFive
Pingback: EVENTS NEW YORK CITY
Pingback: NYC CATERING
Pingback: Julius Dein
Pingback: HOUSEKEEPING SERVICE BROOKLYN
Pingback: it.locr.com/profile/wdallas28
Pingback: businessblogtips.com/7-simple-tips-to-increase-engagement-with-your-content-marketing/
Pingback: ERP System Singapore
Pingback: influenceur
Pingback: madynasty.com/story.php?title=www-foxtailmarketing-com
Pingback: cannabis médical
Pingback: HOUSEKEEPING SERVICE NEW YORK CITY
Pingback: www.primesquaream.com/index.php/component/k2/itemlist/user/313903
Pingback: digital media sri lanka
Pingback: dsahueida.info/story/26602/
Pingback: booter
Pingback: James A. Bonfiglio
Pingback: digital media marketing sri lanka
Pingback: www.beautezine.com/shu-uemura-eye-conic-false-eyelashes-review-photos/
Pingback: 951109.members.page4.me/54.html
Pingback: feedio.net/how-does-search-engine-marketing-work/
Pingback: www.beautezine.com/maybelline-fit-me-shine-free-foundation-review-photos-swatches/
Pingback: www.entrepreneur.com/article/279736
Pingback: number 1 booter
Pingback: 2dopeboyz.com/2011/07/19/phil-ade--a-different-world-mixtape/
Pingback: indulgy.com/post/EbAjy6Lqh3/ways-to-upcycle-vintage-cookie-and-tea-tins
Pingback: www.playindavis.com/places-to-play/listing/eaglewood-golf-course-1
Pingback: www.jasa-seo-indonesia.com/search-engine-optimization-is-not-very-hard-learn-about-it-with-these-tips/
Pingback: theoldreader.com/profile/rnordman?page=121
Pingback: James A. Bonfiglio
Pingback: www.iglobal.co/united-states/new-york-city/search-category/online-marketing
Pingback: vocational-courses.nearoff.com/component/k2/itemlist/user/1785590
Pingback: logopond.com/hberry56/profile/219688/?gallery=profilefeatured&filter=I
Pingback: ybs.us/content-marketing-strategies/
Pingback: ezlocal.com/ca/los-angeles/sales/094434743
Pingback: ogcseoultcpc.info/story.php?id=35211
Pingback: toprightnews.com/michael-browns-mother-and-grandma-brawl-over-dont-shoot-t-shirt-cash/
Pingback: celluliterimedis.info/story/21983/
Pingback: www.russia-pro.ru/?option=com_k2&view=itemlist&task=user&id=299323
Pingback: vengreso.com/blog/youre-driving-leads-via-social-all-wrong
Pingback: blog.hcomicbook.com/2008/10/16/cartoon-bozo-ready-to-cum-over-drawn-chicks/
Pingback: logopond.com/hberry56/profile/pads/219688/?filter=
Pingback: James A Bonfiglio
Pingback: reset.me/story/medical-mushrooms-5-fungi-capable-of-healing/
Pingback: www.socialbookmark365.com/story.php?title=to-learn-more-13
Pingback: logopond.com/hberry56/profile/219688/?filter=W
Pingback: Skurt has raised a $10M Series A to grow its rental car delivery service
Pingback: pinstake.com/infographic-the-best-content-marketing-tools-48065/aHR0cDp8fHd3d15yYWdhbl5jb218VXBsb2Fkc3xQdWJsaWN8Q29udGVudF9NYXJrZXRpbmdfVG9vbHNfSW5mb2dyYXBoaWNfY3JvcF5qcGc=/
Pingback: www.iglobal.co/united-states/new-york-city/search-category/video-marketing-new-york-city
Pingback: Skurt Just Launched new form of transportation in Miami
Pingback: www.iglobal.co/united-states/los-angeles-ca/search-category/digital-marketing
Pingback: theoldreader.com/profile/rnordman?page=400
Pingback: theoldreader.com/profile/rnordman?page=405
Pingback: Skurt is now available on android
Pingback: Trouvez et recrutez les meilleurs influenceurs
Pingback: paraisoweb.com.br/whazzup/2012/10/ganhe-dinheiro-em-30-dias-saiba-como/
Pingback: Skurt on Instagram
Pingback: www.blackenterprise.com/career/negotiate-with-confidence/
Pingback: James A. Bonfiglio
Pingback: film semi
Pingback: hinoplast.com/index.php/component/k2/itemlist/user/420899
Pingback: agri29-legumes.com/auxilliaires/
Pingback: www.midwestsportsfans.com/2009/07/video-george-bush-throwing-out-first-pitch-at-2001-world-series/
Pingback: Skurt named in 50 LA Startups to watch in 2017
Pingback: www.similarsites.com/site/oakfieldlanes.com
Pingback: SSC test Series
Pingback: yourcreditguys.com/component/k2/itemlist/user/585944
Pingback: www.beautezine.com/nars-satin-lip-pencils-review-photos-swatches/
Pingback: www.clasica885.com/?option=com_k2&view=itemlist&task=user&id=86806
Pingback: alicjawkrainieszpargalow.blogspot.com/2016/05/
Pingback: www.thegatewaypundit.com/2008/04/singer-keys-insists-her-racist-remarks-were-really-your-fault/
Pingback: www.grainsofearth.com/
Pingback: bogorkota.jabar.polri.go.id/apel-gelar-ops-patuh-lodaya-2017/
Pingback: www.playindavis.com/places-to-play/listing/cinemark-bountiful-8
Pingback: aclass.com.sg/?option=com_k2&view=itemlist&task=user&id=1122613
Pingback: zh-tw.locr.com/profile/wdallas28
Pingback: thai retirement visa
Pingback: thailand retirement visa
Pingback: nonton film semi
Pingback: hdimagegallery.net/bird+feeder+trays
Pingback: Donate
Pingback: thailand retirement visa
Pingback: gallerygogopix.net/50s+style+wedding+dress+patterns
Pingback: houseofturquoise.com/2011/06/day-four-dream-home-tour.html
Pingback: application
Pingback: thai retirement visa
Pingback: Roslyn Estates
Pingback: www.sorrywatch.com/2013/02/14/12-artful-apologies/
Pingback: www.beautezine.com/benefit-stay-flawless-15-hour-primer-stick-review-photos-swatches/
Pingback: houseofturquoise.com/2014/12/dream-home-tour-day-three-2.html
Pingback: additional resources
Pingback: www.entrepreneur.com/article/289637
Pingback: read this post here
Pingback: loveofhomes.blogspot.com/2014/01/vanity-makeover.html
Pingback: www.homebunch.com/search/shingle/page/202/
Pingback: website here
Pingback: internet-marketing.alltop.com/
Pingback: www.homebunch.com/tag/cottage-decor/page/343/
Pingback: ministryofads
Pingback: www.homebunch.com/category/coastal-interiors-2/page/404/
Pingback: find out here now
Pingback: boxing.overtime-dv.ru/user/suit8robert/
Pingback: Great Neck Estates
Pingback: click here for more
Pingback: check my source
Pingback: livemodern.com/forums/utah/694690208
Pingback: www.homebunch.com/tag/coastal-decor/page/358/
Pingback: macros
Pingback: Mill Neck
Pingback: visit their website
Pingback: bradyandash.blogspot.com/2010/09/
Pingback: killerstartups.com/bootstrapping-money-makers/foxtail-marketing-founder-michael-templeman
Pingback: www.playindavis.com/places-to-play/listing/historic-bountiful-main-street
Pingback: tech.co/build-thought-leadership-2014-08
Pingback: resource
Pingback: visit this web-site
Pingback: www.greylikesbaby.com/author/brooke/page/47/
Pingback: fijitheartist.com/barry-black-fever-feat-fiji/
Pingback: see this page
Pingback: SC
Pingback: a knockout post
Pingback: www.homebunch.com/tag/benjamin-moore-paint-color/page/280/
Pingback: caseperlatesta.com/my-moodboard-on-wednesday-linky-party-4/?lang=zh
Pingback: Togel online
Pingback: browse around here
Pingback: fragerfactor.blogspot.com/2015/08/warning-to-searchers-of-fake-online.html
Pingback: ac companies St. petersburg
Pingback: spin class
Pingback: impossible-simplymylife.blogspot.com/2015/08/9-zrob-to-sam-taboret.html
Pingback: internet.itbusinessnet.com/article/Digital-Marketing-Trends-that-Steal-the-Show-in-2017-4969350
Pingback: www.homebunch.com/category/interior-ideas/page/331/
Pingback: Air Conditioner repair Clearwater FL
Pingback: general insurance
Pingback: informative post
Pingback: loveofhomes.blogspot.com/2011/10/ive-been-given-blogger-award-from-jane.html
Pingback: www.homebunch.com/category/french-interiors-2/page/41/
Pingback: try this
Pingback: have a peek at this web-site
Pingback: mayweather vs mcgregor
Pingback: learn this here now
Pingback: wordpress developer from hyderabad
Pingback: mcgregor vs mayweather live stream
Pingback: air conditioning companies brandon florida
Pingback: nongomasiyavayatours.com/index.php/component/k2/itemlist/user/252528
Pingback: www.homebunch.com/tag/canadian-interior-designer/page/119/
Pingback: www.homebunch.com/category/home-decor/page/132/
Pingback: loveofhomes.blogspot.com/2013/08/getting-rid-of-bees.html
Pingback: armandotnfw999blog.shotblogs.com/examine-this-report-on-foxtailmarketing-409750
Pingback: rocaempreendimentos.com.br/?option=com_k2&view=itemlist&task=user&id=70095
Pingback: www.thegatewaypundit.com/2012/03/obama-is-sending-a-shipload-of-arms-to-anti-israel-anti-american-egyptian-regime/
Pingback: go to my site
Pingback: digitized logo
Pingback: www.homebunch.com/category/coastal-interior-ideas/page/189/
Pingback: carinsuranceroute.us/designer-furniture-stores-atlanta/designer-furniture-stores-atlanta-home-design-great-classy-simple
Pingback: digitizing a logo
Pingback: www.homebunch.com/page/462/
Pingback: custom embroidery design
Pingback: tampa air conditioner
Pingback: MYOB Exo Magento integration
Pingback: fat burner
Pingback: loveofhomes.blogspot.com/2015/07/4th-of-july-decor.html
Pingback: reset.me/story/dopamine-deficiency-and-your-mental-health/
Pingback: Oyster Bay
Pingback: carinsuranceroute.us/designer-furniture-stores-atlanta/designer-furniture-stores-atlanta-venice-sofa-bed-amazon
Pingback: reset.me/story/7-people-say-cannabis-threated-life-threatening-illness/
Pingback: www.midwestsportsfans.com/2008/10/redskins-14-browns-11/
Pingback: XERO Magento integration
Pingback: www.midwestsportsfans.com/2011/05/in-honor-of-dirk-points-per-miss/
Pingback: reset.me/story/study-painkiller-overdose-deaths-decrease-dramatically-420-friendly-states/
Pingback: www.homebunch.com/category/bathrooms-2/page/293/
Pingback: Covert Fitness
Pingback: reset.me/story/entering-psychedelic-state-without-psychedelics-inside-holotropic-breathwork/
Pingback: www.thegatewaypundit.com/2012/12/union-thug-who-beat-steven-crowder-ided-his-name-is-tony-cummings-video/
Pingback: www.homebunch.com/page/65/?s=patio
Pingback: embroidery digitize
Pingback: reset.me/personal-story/personal-story-ayahuasca-addiction-awakening/
Pingback: custom embroidery digitizing
Pingback: embroidery digitizing companies
Pingback: jayandmeganlott.blogspot.com/2008/02/family-christmas-pictures.html
Pingback: jewelry software
Pingback: www.homebunch.com/search/shingle/page/134/
Pingback: reset.me/story/10-reasons-eating-daily-turmeric-make-happier-healthier/
Pingback: embroidery digitizing companies
Pingback: jayandmeganlott.blogspot.com/2008/12/brooklyn-and-brynlee-started-dance.html
Pingback: jayandmeganlott.blogspot.com/2008/11/updates.html
Pingback: Read More Here
Pingback: jayandmeganlott.blogspot.com/2009/04/britains-got-talent.html
Pingback: garage door installation
Pingback: More Info
Pingback: axelandash.com/merry-christmas-2/
Pingback: digitizing service
Pingback: Clicking Here
Pingback: loveofhomes.blogspot.com/2014/06/a-kitchen-remodel-update.html
Pingback: www.thegatewaypundit.com/2012/12/explosive-new-book-following-orders-the-death-of-vince-foster/
Pingback: agen togel
Pingback: embroidery machine digitizing
Pingback: 2dopeboyz.com/2011/04/21/do-you-want-your-music-on-2dopeboyz/
Pingback: 2dopeboyz.com/2010/06/17/kid-cudi-revofev/
Pingback: digitize logo for embroidery
Pingback: testosterone boosters
Pingback: loveofhomes.blogspot.com/2011/10/pizza.html
Pingback: jayandmeganlott.blogspot.com/2010/03/globetrotters.html
Pingback: buy twitter retweets cheap
Pingback: www.australianmining.com.au/news/contractors-more-likely-to-die-on-mine-sites-report/
Pingback: embroidery digitizers
Pingback: buy 1000 facebook page likes
Pingback: fabric
Pingback: garage door installation
Pingback: www.midwestsportsfans.com/2009/02/indiana-basketball-self-reports-extra-phone-call-tom-crean/
Pingback: embroidery digitizing companies
Pingback: digitizing a logo
Pingback: digitizing services
Pingback: design
Pingback: bradyandash.blogspot.com/2010/05/for-my-mother.html
Pingback: toprightnews.com/justice-in-a-moderate-muslim-nation-woman-beheaded-in-broad-daylight-while-police-watch/
Pingback: sezoentje.blogspot.com/2014/12/dream-home-tour-day-four.html
Pingback: digitizing logo for embroidery
Pingback: tinyandfree.blogspot.com/2013/07/four-chairs-furniture-hiya-papaya.html
Pingback: loveofhomes.blogspot.com/2013/10/adding-hardware-to-your-garage-doors.html
Pingback: buy instagram video views
Pingback: katiephelon.blogspot.com/2011/06/
Pingback: buy twitter favorites
Pingback: www.thegatewaypundit.com/2007/11/the-london-times-accuses-hillary-of-lesbian-affair/
Pingback: modern interior
Pingback: reset.me/story/how-processed-food-hijacks-your-brain/
Pingback: loveofhomes.blogspot.com/2015/12/christmas-house-tour.html
Pingback: caseperlatesta.com/my-moodboard-on-wednesday-linky-party-4/
Pingback: singapore visa for indians
Pingback: garage roller doors
Pingback: automatic garage door
Pingback: reset.me/story/watch-thc-kills-cancer-cells/
Pingback: reset.me/study/study-pharmaceuticals-kill-more-teens-than-illegal-substances-in-the-us/
Pingback: thecollectedhouse.com/page/4/
Pingback: naurahomedesign.com/bar-stools/metal-backless-bar-stools.html
Pingback: upholstery
Pingback: reset.me/video/cannabis-oil-cures-infants-inoperable-brain-tumor/
Pingback: how to digitize for embroidery
Pingback: dumpster rental ortonville
Pingback: www.homebunch.com/category/house/page/146/
Pingback: dumpster rental lake orion
Pingback: furniture recycle
Pingback: www.homebunch.com/search/Beach+house+dining+room/page/69/
Pingback: vehicle insurance company
Pingback: www.homebunch.com/category/patio-2/page/181/
Pingback: dumpster rental lincoln park
Pingback: digitizing logos for embroidery
Pingback: embroidery digitizing companies
Pingback: dumpster rental oakland county
Pingback: iphone repair screen repair in waterbury
Pingback: www.homebunch.com/tag/benjamin-moore-paint-color/page/147/
Pingback: ERP Software Singapore
Pingback: digitize logo
Pingback: dumpster rental mount clemens
Pingback: digitize logo for embroidery
Pingback: dumpster rental Gibraltar
Pingback: www.homebunch.com/category/house/page/475/
Pingback: hard drive repair near me
Pingback: www.homebunch.com/category/small-interior-ideas/page/59/
Pingback: idataFive
Pingback: used repo trucks
Pingback: computer virus removal near me
Pingback: www.homebunch.com/category/classic-design/page/507/
Pingback: dumpster rental new boston
Pingback: embroidery digitizing services
Pingback: custom embroidery design
Pingback: embroidery digitizing usa
Pingback: trash bins for rent
Pingback: custom embroidery digitizing
Pingback: www.homebunch.com/page/16/?s=navy+and+white
Pingback: embroidery digitizing usa
Pingback: casino online
Pingback: dumpster rental trenton
Pingback: computer virus removal near me
Pingback: embroidery digitization
Pingback: dumpster rental wolverine
Pingback: garage door remotes
Pingback: dumpster rental saginaw
Pingback: surveillance camera installation near me
Pingback: dumpster rental grosse pointe
Pingback: bandarq
Pingback: digitize jpeg
Pingback: dumpster rental macomb twp
Pingback: security camera companies near me
Pingback: bertriesbuildonabudget.blogspot.com/
Pingback: bandarq
Pingback: dubai visa
Pingback: cheap dumpster rental
Pingback: thailand tourist visa
Pingback: embroidery digitization
Pingback: embroidery digitize
Pingback: jayandmeganlott.blogspot.com/2010/
Pingback: dumpster rental Zilwaukee
Pingback: garage door
Pingback: trash pickup
Pingback: professional digitizing
Pingback: garage door remotes
Pingback: small dumpster rental prices
Pingback: dumpster delivery
Pingback: construction debris dumpster
Pingback: digitize embroidery designs
Pingback: garage door repair
Pingback: digitizing a logo
Pingback: digitize for embroidery
Pingback: Read More
Pingback: Proxy forum
Pingback: www.pingable.org/
Pingback: New proxy
Pingback: digitizer embroidery
Pingback: mashable.com/2012/03/02/content-marketing-non-profits/
Pingback: embroidery digitizers
Pingback: embroidery digitizing usa
Pingback: bandarq
Pingback: mashable.com/2010/05/20/twitpic-interview-noah-everett/
Pingback: digitize embroidery
Pingback: www.cision.com/us/2012/04/top-100-social-media-internet-marketing-seo-blogs-2012/
Pingback: Public proxies
Pingback: digitizing logos
Pingback: Web Site
Pingback: www.johnhaydon.com/about-john-haydon/
Pingback: free online raw food classes
Pingback: Togel online
Pingback: diesel flatbed for sale
Pingback: how do raw foods boost enzyme activity
Pingback: embroidery digitizing
Pingback: towing rosedale park
Pingback: embroidery digitize
Pingback: blog.capterra.com/nonprofit-statistics-for-2015/
Pingback: plus.google.com/+BrendanSchneider
Pingback: how do raw foods boost enzyme activity
Pingback: www.jobsatnonprofits.com/
Pingback: npengage.uberflip.com/t/26617-npengage
Pingback: bandarq
Pingback: 495 towing
Pingback: www.futurefundraisingnow.com/future-fundraising/2017/06/does-face-to-face-donor-acquisition-work-a-look-at-the-facts.html
Pingback: how long detox raw food
Pingback: anngreennonprofit.com/
Pingback: digitizing design
Pingback: tow truck company hamtramck
Pingback: www.care2services.com/care2blog/its-about-impact-not-influence
Pingback: classroom.synonym.com/ask-donations-4425378.html
Pingback: bandarq
Pingback: www.futurefundraisingnow.com/future-fundraising/2017/06/how-you-yes-you-and-i-can-talk-about-fundraising.html
Pingback: flatbed diesel trucks for sale
Pingback: embroidery machine digitizing
Pingback: bandarq
Pingback: get car insurance
Pingback: embroidery digitizer florida
Pingback: digitizing for embroidery
Pingback: embroidery digitizer florida
Pingback: mashable.com/2010/09/23/small-non-profits-social-media/
Pingback: bloomerang.co/blog/100-fundraising-blogs-you-should-be-reading-in-2017/
Pingback: togel singapura
Pingback: online embroidery digitizing
Pingback: www.futurefundraisingnow.com/future-fundraising/
Pingback: www.entrepreneur.com/article/290412
Pingback: digitized logos
Pingback: www.wildapricot.com/articles/event-checklist
Pingback: bandarq
Pingback: www.communityorganizer20.com/2011/09/06/infographics-for-nonprofits-the-new-storytelling/
Pingback: digitizing embroidery
Pingback: www.softwareadvice.com/nonprofit/industryview/fundraising-event-report-2015/
Pingback: www.bethkanter.org/crowdfunding-info/
Pingback: embroidery design services
Pingback: searchenginewatch.com/sew/how-to/2388727/5-ways-small-businesses-can-build-their-brands-in-2015
Pingback: nonprofitquarterly.org/2013/12/06/giving-tuesday-2013-more-infrastructure-more-money-more-groups-in-the-mix/
Pingback: bandarq
Pingback: sunlightfoundation.com/2017/07/13/word-gets-around-chattanooga-adopts-facebook-chatbot-for-open-data/
Pingback: bandarq
Pingback: best passive income
Pingback: Togel online
Pingback: mining
Pingback: sbobet
Pingback: Full Report
Pingback: sbobet
Pingback: monkey rocker
Pingback: Company signage Sydney
Pingback: Taxi services in Inver Grove Heights
Pingback: Super Vibrator
Pingback: casino online
Pingback: Personal Trainer in State College, PA
Pingback: Reposition a brand Sydney
Pingback: cars in the future
Pingback: Fitness Coach
Pingback: Brand audit
Pingback: Quicksilver Scientific NanoMojo
Pingback: toy rabbit
Pingback: Online Training
Pingback: Weight Lifting
Pingback: DUTCH test coupon code
Pingback: Togel online
Pingback: Togel online
Pingback: sbobet
Pingback: climax the series
Pingback: Togel online
Pingback: matka boss
Pingback: kalyan jodi trick
Pingback: SATTA KALYAN
Pingback: MAIN MATKA
Pingback: recuperarelpelo
Pingback: dubai tourist visa
Pingback: matka tips today
Pingback: cheap airline tickets
Pingback: dubai tour packages
Pingback: recuperarelpelo
Pingback: recuperarelpelo
Pingback: where to buy dog nail clippers
Pingback: home pet grooming
Pingback: America furniture
Pingback: vive sin ansiedad
Pingback: dog shampoo oatmeal
Pingback: train-from-nha-trang-to-da-nang
Pingback: maintenance free water softener
Pingback: best shampoo for dandruff in hard water
Pingback: craniosacrale Osteopathie
Pingback: salt free water softener
Pingback: the online pet store
Pingback: Lakiesha Browner
Pingback: pet grooming services near me
Pingback: Alyson Swopes
Pingback: pet groomers near me prices
Pingback: cheap online pet store
Pingback: Leila Sandor
Pingback: Furniture online shopping
Pingback: wahing clothes in hard water conditions
Pingback: bus-from-nha-trang-to-da-lat
Pingback: Leora Adkisson
Pingback: Schedule
Pingback: water softener for hotel india
Pingback: Furniture online shopping
Pingback: Johnna Nunnally
Pingback: digital coupons
Pingback: Cristobal Sane
Pingback: bore water problem
Pingback: water softener for hotel india
Pingback: water softener for water tank
Pingback: europe furniture
Pingback: Gift Cards
Pingback: Testimonials
Pingback: www.jeremybruce.com/
Pingback: Korean hairdresser
Pingback: Drone photography
Pingback: Poju Zabludowicz
Pingback: how to lose weight
Pingback: Drone photography
Pingback: top4
Pingback: Sound production
Pingback: Anita Zabludowicz
Pingback: Lung Cancer
Pingback: Zabludowicz Collection
Pingback: Bluetooth Headsets
Pingback: Lung Cancer
Pingback: Anita Zabludowicz
Pingback: Cancer Center
Pingback: Mobile Application
Pingback: porn star gets dirty anal punishment - watch sex tube and porn videos at pcit.net
Pingback: mirando mi pene con ganas - watch sex tube and porn videos at pcit.net
Pingback: pcit
Pingback: best water purifier
Pingback: fruits & vegetable purifier
Pingback: iptv not working
Pingback: bitcoin exchange
Pingback: prix carte grise
Pingback: martin modern condo singapore
Pingback: smnx
Pingback: Skin care
Pingback: comment faire sa carte grise en ligne
Pingback: Effective Skin Care Habits
Pingback: iptv app
Pingback: solomon exchange
Pingback: Slim couture
Pingback: duplicata carte grise
Pingback: prix du cheval carte grise
Pingback: Latest
Pingback: download apk for android
Pingback: Celebrities
Pingback: market free download
Pingback: exclusive
Pingback: Latest
Pingback: The Battle of Polytopia
Pingback: Olamide
Pingback: Your Domain Name
Pingback: Taxi services in Hennepin
Pingback: this
Pingback: magic mops cleaning
Pingback: websites
Pingback: apk.fun/Get_Funimate_APK-Free.html
Pingback: click here
Pingback: royal revolt 2 hack
Pingback: exclusive
Pingback: Records
Pingback: eventos zona sur
Pingback: Download MyQuran Al Quran Indonesia Apk Latest Version For Android
Pingback: read
Pingback: iluminacion profesional para eventos
Pingback: lamparas roboticas
Pingback: sonido para fiestas df
Pingback: renta de luces neon
Pingback: check list para boda
Pingback: pop over here
Pingback: Hospice dallas
Pingback: cheap hood county Tx Weddings,
Pingback: Budget Granbury Wedding chapel
Pingback: you can find out more
Pingback: Cheap Granbury Wedding chapel
Pingback: Granbury Church Weddings
Pingback: Monogram Apple iPhone Case
Pingback: Amino Apps
Pingback: Party Dress
Pingback: Hosting coupon code
Pingback: ClickFunnels discount
Pingback: ClickFunnels free
Pingback: ClickFunnels review
Pingback: dumpster rental Detroit
Pingback: best beauty products
Pingback: dumpster rental warren
Pingback: junk bin rental
Pingback: rent a trash dumpster
Pingback: narraciones en portuguÈs
Pingback: ClickFunnels site
Pingback: ClickFunnels free
Pingback: pick up junk
Pingback: dumpster rental company
Pingback: construction dumpsters for rent
Pingback: NAPSR
Pingback: NAPSR Review
Pingback: CNPR
Pingback: CNPR
Pingback: Pharmaceutical Sales Training
Pingback: NAPSR Certification
Pingback: NAPSR Scam
Pingback: NAPSR Training
Pingback: NAPSR Certification
Pingback: construction debris containers
Pingback: CNPR Scam
Pingback: Pharmaceutical Sales Training
Pingback: CNPR
Pingback: face shape sunglasses
Pingback: y doblajes en portuguÈs
Pingback: taylor townearg service provider near
Pingback: buy trendy fashion accessories online
Pingback: accessorise like a pro
Pingback: wrecker truck
Pingback: party hire hk
Pingback: overhead lifting
Pingback: recovery tow hook
Pingback: party hire hk
Pingback: Fuel optimization
Pingback: tile flooring
Pingback: auto liens
Pingback: Read Full Article
Pingback: Get More Information
Pingback: jackets for women
Pingback: Mens wedding rings
Pingback: outerwear for women
Pingback: Mens casual rings
Pingback: leather jackets for women
Pingback: daily offers
Pingback: long winter coats
Pingback: Snekker
Pingback: womens coats
Pingback: casa ristorante
Pingback: Click Here
Pingback: Related Site
Pingback: leather jackets for women
Pingback: Down parkas
Pingback: Mens casual rings
Pingback: Related Site
Pingback: singapore real estate agent
Pingback: Read This
Pingback: Click Here
Pingback: ladies jackets
Pingback: signalvault
Pingback: Big bows for cars
Pingback: dick enlargement
Pingback: leather jacket women
Pingback: Brooklyn Dryer Vent Cleaning Wizard
Pingback: coats for women
Pingback: Custom flags
Pingback: signalvault
Pingback: Custom flags
Pingback: womens winter coats
Pingback: sexy
Pingback: never pay retail
Pingback: winter coats for women
Pingback: Car bows
Pingback: jackets for women
Pingback: vent a dryer
Pingback: never pay retail
Pingback: ladies jackets
Pingback: Car bows
Pingback: dryer vent problems
Pingback: clothes dryer vent cover
Pingback: clothes dryer fires
Pingback: Dealer products
Pingback: dryer vent flap
Pingback: clash of clans royale
Pingback: appliance repair East Brunswick
Pingback: Custom car bows
Pingback: action appliance repair
Pingback: washer appliance repair
Pingback: a plus appliance repair
Pingback: lg washer repair
Pingback: dumpster rental argentine
Pingback: whirlpool dishwasher repair parts
Pingback: dumpster rental orion twp
Pingback: waste container
Pingback: ramp hire
Pingback: Walk-in bathtub Hilliard OH
Pingback: trash dumpsters
Pingback: ageing in place definition
Pingback: trash dump
Pingback: disabled bathroom design
Pingback: threshold ramp rubber
Pingback: ada shower pans
Pingback: building ramps
Pingback: ????δα
Pingback: Animated Lure
Pingback: February Birthstone
Pingback: painting
Pingback: comprar bitcoins
Pingback: Sapphire Birthstone
Pingback: poster
Pingback: trash removal business
Pingback: Tanzanite
Pingback: Cheap Car Rental Dubai
Pingback: ?στ?σε??δα
Pingback: 6 yard dumpster rental
Pingback: Outdoor Sports 4K Camera
Pingback: click here
Pingback: TB Fan Club
Pingback: Euro lottery
Pingback: PC & Videogames deals
Pingback: Athletics deals
Pingback: ladies fitness clothing
Pingback: Books deals
Pingback: Sporting Goods deals
Pingback: Massage School in McAllen
Pingback: ladies fitness clothing
Pingback: Laptops deals
Pingback: mini slant tweezers
Pingback: Massage School in McAllen
Pingback: Massage School in McAllen
Pingback: plastic pointed tweezers
Pingback: slanted tip tweezers
Pingback: dic phoenix
Pingback: osimi sea view
Pingback: osimi sea view
Pingback: osimi sea view
Pingback: osimi sea view
Pingback: osimi seaview
Pingback: Free Tv channel patriots vs falcons live
Pingback: hire USA WordPress developer
Pingback: wordpress customer service
Pingback: custom web design
Pingback: NFL us football games live
Pingback: best web development company
Pingback: NFL nfl football games
Pingback: Game patriots vs falcons live
Pingback: Football nfl football games
Pingback: How to install WordPress
Pingback: 4G
Pingback: Curved Glass
Pingback: custom web design
Pingback: web development company usa
Pingback: WordPress contact number
Pingback: Watch us football games live
Pingback: NFL us football games live
Pingback: college Football nfl football games
Pingback: Live patriots vs falcons live
Pingback: Live us football games live
Pingback: NFL patriots vs falcons live
Pingback: Online patriots vs falcons live
Pingback: Game nfl football games
Pingback: Free Tv channel patriots vs falcons live
Pingback: click the next website page
Pingback: click to read
Pingback: college Football nfl football games
Pingback: [source]
Pingback: Click On this site
Pingback: had me going
Pingback: Law questions and answers
Pingback: link homepage
Pingback: mouse click the up coming web site
Pingback: link home
Pingback: more helpful hints
Pingback: free cccam
Pingback: Source
Pingback: just click the up coming internet page
Pingback: just click the following article
Pingback: click the next web page
Pingback: click to read
Pingback: Low cost kitchen ideas
Pingback: please click the next internet page
Pingback: Check Out Your URL
Pingback: more
Pingback: agree with
Pingback: Read Home Page
Pingback: helpful resources
Pingback: active
Pingback: look at here now
Pingback: click here to find out more
Pingback: look at these guys
Pingback: anchor
Pingback: linked web site
Pingback: Going In this article
Pingback: click through the next website page
Pingback: Full Guide
Pingback: our website
Pingback: My Site
Pingback: more info here
Pingback: my latest blog post
Pingback: Auto Finanzierung
Pingback: discover this
Pingback: Gas dryer
Pingback: maytag repairman
Pingback: browse around this web-site
Pingback: certified appliance repair
Pingback: Wirral Escorts
Pingback: Dryer fire prevention
Pingback: Check Out %url_domain%
Pingback: clean dryer vent pipe
Pingback: description
Pingback: frigidaire service
Pingback: hester Escorts
Pingback: dryer lint remover
Pingback: dryer vent booster
Pingback: appliance warranty
Pingback: nghi dung vung tau
Pingback: content marketer
Pingback: spring bed
Pingback: dryer vent filter
Pingback: The Best Escorts In Liverpool
Pingback: rain gutter cleaning service
Pingback: dumpster rental owosso
Pingback: funny post
Pingback: local school open days
Pingback: Best wedding cake idea in 2017
Pingback: dumpster rental brownstown
Pingback: just click the following web site
Pingback: dumpster rental Flint
Pingback: construction dumpster sizes
Pingback: click here to investigate
Pingback: click over here
Pingback: wolverhampton schools
Pingback: cost for dumpster rental
Pingback: More methods
Pingback: Click Webpage
Pingback: waste management company
Pingback: need a dumpster
Pingback: schools
Pingback: microblading
Pingback: manchester schools
Pingback: maytag fridge filter
Pingback: moveis odontol?gicos
Pingback: how to tow truck
Pingback: car moving service
Pingback: primary schools
Pingback: Moveis para farm?cia
Pingback: best auto insurance rates
Pingback: Best comparision site
Pingback: www.auto-insurance-quotes.com
Pingback: emergency roadside assistance detroit
Pingback: schools
Pingback: emergency roadside assistance detroit
Pingback: school open days near me
Pingback: urandir ufologos
Pingback: urandir fernandes de oliveira
Pingback: non owners insurance
Pingback: roadside assistance 24/7
Pingback: urandir oliveira
Pingback: Editors choice
Pingback: It's In Your Hands 5 Strategies
Pingback: Surgical Technologist Certifying Exam Study Guide
Pingback: Weight Dip belt with chain
Pingback: Phlebotomy Test Prep Exam Review Practice Questions
Pingback: Limo Hire Sheffield
Pingback: Limo Hire Bradford
Pingback: Padded Dip belt with chain
Pingback: Management of Assaultive Behavior Instructor DVD
Pingback: Limo Hire Grantham
Pingback: Limo Hire Sheffield
Pingback: Jokes for Nurses 50 Jokes & Shift Notes
Pingback: Limo Hire Doncaster
Pingback: Acute Care Nurse Assistant
Pingback: IV Therapy and Blood Withdrawal Review Questions
Pingback: Limo Hire Manchester
Pingback: Limo Hire Manchester
Pingback: Limo Hire Derby
Pingback: Limo Hire Nottingham
Pingback: Medical Assistant Certification
Pingback: MLT Exam Study Guide Medical Laboratory
Pingback: Choosing a Healthcare Career
Pingback: Weight Loss Inspiration Step by Step
Pingback: Nurse Romance Dr Mark: Book 1
Pingback: CMA Exam Preparation 2017 Medical Assistant
Pingback: Affiliate Marketing
Pingback: CNA Exam Prep (Volume 2) Nurse Assistant
Pingback: Patient Care Technician Certification
Pingback: CNA Exam Preparation 2017
Pingback: Patient Care Technician Exam Study Guide Volume One
Pingback: Nurse Romance: Craig's Love Story
Pingback: CEHRS Study Guide
Pingback: CNA Nursing Assistant Exam Practice Book
Pingback: Crisis Prevention & Intervention
Pingback: Pharmacy Technician Certification Study Guide
Pingback: women's rights
Pingback: Personality Types
Pingback: bitcoin
Pingback: emergency plumbers near me
Pingback: Director of Staff Development DSD
Pingback: Design Your Own Methods
Pingback: ACLS Provider Manual Study Guide
Pingback: Email Marketing
Pingback: tankless water heaters
Pingback: EKG Test Prep EKG Technician Practice
Pingback: EKG Technician Study Guide EKG
Pingback: internet
Pingback: How to grow your small business
Pingback: Hangar for tennis
Pingback: Tent hangars
Pingback: Phlebotomy Test Prep Exam Review Practice
Pingback: Hangar for cows
Pingback: Tent sports arena
Pingback: Hangar for pigs
Pingback: Phlebotomy Test Prep Exam Review
Pingback: water heater replacement
Pingback: water heater replacement
Pingback: How To Become A Better Husband
Pingback: Home Health Aide Textbook Home Care Principles
Pingback: Nurse Romance Dr. Mark: Book 2
Pingback: Warehouses price
Pingback: leak detection
Pingback: von kroft free porn videos for free
Pingback: Tent hangar for machinery
Pingback: schoolgirl fucking big dick on brazzer . com free porn videos for free
Pingback: Bandar Bola Online
Pingback: plumbing company
Pingback: hot moms riding teen son domination tied son tied to the bed porn free porn videos for free
Pingback: gemidos free porn videos for free
Pingback: slab leak repair
Pingback: Video Blogging
Pingback: Awning warehouse
Pingback: Hightime You Made a Move! A motivational book
Pingback: plumbing repair
Pingback: emergency plumbers
Pingback: IV Therapy Practice Questions 1000 Review Questions
Pingback: emergency plumbers
Pingback: How To Make a Million in Nursing The First 5 Steps
Pingback: Surgical Technologist Certifying Exam Review Questions
Pingback: Workbook Home Health Aide Textbook
Pingback: Medical Lab Assistant Exam Study Guide
Pingback: boobs
Pingback: Inspirational quotes
Pingback: Leiderschap
Pingback: Life sayings
Pingback: printable coloring pages
Pingback: GCLUB
Pingback: coloring pages for teenagers
Pingback: Quotes on life
Pingback: Health coach
Pingback: Leiderschap
Pingback: Online coaching
Pingback: online coloring pages
Pingback: coloring pages
Pingback: Great quotes
Pingback: online coloring pages
Pingback: Greatest quotes about life
Pingback: hund älskare
Pingback: Short inspirational message
Pingback: Affiliate Marketing Breakout Online
Pingback: Solutions Manual
Pingback: Accept Challenges A Motivational Book
Pingback: Test bank online
Pingback: Curved Glass
Pingback: Leiderschap
Pingback: Inspirational quotes
Pingback: 5 inches
Pingback: seo
Pingback: Quotes on life
Pingback: Continue
Pingback: Source
Pingback: Test Bank
Pingback: Check This Out
Pingback: Testbank
Pingback: Executive coaching
Pingback: CNA Study Guide
Pingback: Don't Worry Be Happy 9 Principles of Living
Pingback: Agent
Pingback: Trucking
Pingback: the best psychic email readings
Pingback: vegan cookies
Pingback: aloe vera mole removal
Pingback: aloe vera mole removal
Pingback: aloe vera to remove moles
Pingback: Y???Y???
Pingback: GCLUB
Pingback: aloe vera mole removal
Pingback: QQ????
Pingback: aloe vera benefits
Pingback: ??????
Pingback: ?????
Pingback: ???q ????q ?
Pingback: VPN??
Pingback: ???????
Pingback: ??????
Pingback: ????
Pingback: barn wedding
Pingback: ??????
Pingback: ?????
Pingback: dumpster rental Flint
Pingback: dryer installation
Pingback: ??????
Pingback: dumpster bin rentals
Pingback: dryer vent hose
Pingback: 20-80%
Pingback: Slim couture
Pingback: ???????
Pingback: dumpster rental swartz creek
Pingback: ????????????????
Pingback: dumpster in a bag
Pingback: ??????
Pingback: ????
Pingback: Dryer on fire
Pingback: Slim couture
Pingback: dryer vent metal
Pingback: dumpster temporary service
Pingback: how to clean dryer vent duct
Pingback: dumpster rental southfield
Pingback: clothes dryer lint trap
Pingback: itunes??
Pingback: Slim couture
Pingback: repo lifts
Pingback: repo wrecker for sale
Pingback: Slim couture
Pingback: Gas dryer
Pingback: hvac duct installation
Pingback: rocklin heating and air
Pingback: as air conditioning
Pingback: dryer vent indoor
Pingback: need a jump
Pingback: Blogpost
Pingback: uma erasmus 2016
Pingback: cost of tow truck
Pingback: Terry Sacka AAMS
Pingback: Buy Silver
Pingback: www.lambangdaihoc.joomla.com/
Pingback: subsidio autonomos mayores de 55 a?os
Pingback: www.lambangdaihocaz.emyspot.com/
Pingback: Website
Pingback: Hidden Money Secrets
Pingback: Sports recruitment Video
Pingback: ayuda por nacimiento
Pingback: Safe Christian Investments
Pingback: ayuda por nacimiento
Pingback: plumbers
Pingback: boston edison valued community member of
Pingback: plumbers
Pingback: Taruhan Bola
Pingback: More Information
Pingback: plumbers
Pingback: ieduex
Pingback: judi online
Pingback: becasfaro
Pingback: plan alquila de la comunidad de madrid
Pingback: Florida Laws
Pingback: About Us
Pingback: runner girl clothing
Pingback: dubai massage
Pingback: Wearable Inspiration necklaces
Pingback: www.dvlambangcapgia.blogspot.com/
Pingback: inspiration mantra jewlery
Pingback: brutalxxxporn
Pingback: wearable inspiration tree-of-life/
Pingback: tweezer for men
Pingback: Running earings
Pingback: fine eyebrow tweezers
Pingback: amateur porn video
Pingback: inspiration mantra jewlery
Pingback: wearable inspiration bracelets
Pingback: eyebrow tweezers with light
Pingback: wearable inspiration tree-of-life/
Pingback: gold investment
Pingback: Run Inspired Designs
Pingback: Quick Divorce
Pingback: Look At This
Pingback: bucketlist.org/idea/zB5P/explaining-rapid-solutions-in-gardenscapes-hack/
Pingback: www.brownpapertickets.com/blogcomments/451663
Pingback: www.evernote.com/shard/s495/sh/eabee677-e352-4621-9694-20ec26a57e38/5d001b42931bda868189008f41f2fdcb
Pingback: www.gaiaonline.com/journal/?mode=view&post_id=39563737&u=39155097
Pingback: basement remodeling canton
Pingback: recipes for matcha latte
Pingback: 50'
Pingback: Virtual PA
Pingback: uhrenmarken teuer
Pingback: gute uhrenmarken
Pingback: Calendar Management
Pingback: roll off dumpster sizes
Pingback: dumpster rental saginaw
Pingback: Event Organisation
Pingback: German Shepherd Coffee Cup
Pingback: 1000 day clock repair
Pingback: modern clocks repaired
Pingback: Life Management
Pingback: alte uhrenmarken verzeichnis
Pingback: dumpster rental wyandotte
Pingback: boston clock repair
Pingback: rent trash dumpster
Pingback: lead lightning
Pingback: Clock Repair Highland
Pingback: debris box
Pingback: Best Android Apps - Android Node
Pingback: Michigan clock repair
Pingback: waste container
Pingback: how to buy traffic
Pingback: make money online
Pingback: waste management small dumpster
Pingback: dumpster rental allen park
Pingback: Best Diary App with lock
Pingback: construction site dumpster
Pingback: Business Plan Training Guide
Pingback: price of dumpster
Pingback: dumpster rental davis
Pingback: matkaguru
Pingback: one day clock repair
Pingback: clock and watch repair
Pingback: nesaporn.mobi
Pingback: Clock Repair Richardson
Pingback: sattasatta
Pingback: clock repair service
Pingback: antique clock repair and restoration
Pingback: dumpster rental otter lake
Pingback: rolloff dumpsters
Pingback: Search Friends Online
Pingback: 1000 day clock repair
Pingback: dumpster rental ecorse
Pingback: discount dumpsters
Pingback: dumpster rental las vegas
Pingback: dumpster rental toronto
Pingback: american clock repair
Pingback: pendulum repair
Pingback: french clock repair
Pingback: antique clock repair & restoration
Pingback: Militancy
Pingback: Twitter
Pingback: Militancy
Pingback: uttar pradesh news in hindi
Pingback: lahore escorts
Pingback: Career coaching
Pingback: lahore escorts
Pingback: rodent pest control exterminator Fontana
Pingback: hypoallergenic cooling towel for sensitive skin
Pingback: free porn videos
Pingback: timeless luxury watches
Pingback: asian porn tube
Pingback: duv porn
Pingback: best chicago criminal defense lawyers
Pingback: movie showtimes near me
Pingback: cannabis real estate, financing, and insurance
Pingback: criminal appeal lawyers chicago
Pingback: Mobile Application Development Company
Pingback: free criminal lawyer chicago
Pingback: shamale hot porn
Pingback: bbw free sex
Pingback: arab sex movies
Pingback: new movie news
Pingback: smartphone
Pingback: iphone
Pingback: gold
Pingback: iphone reparation falkoner alle
Pingback: criminal law paralegal chicago
Pingback: seriale online subtitrate
Pingback: vunporn
Pingback: porno integrale
Pingback: Angel Pearls offer authentic pearls
Pingback: gold rings
Pingback: cheap dui lawyers chicago
Pingback: best criminal attorney in chicago
Pingback: grabador de llamadas
Pingback: asian porn tube
Pingback: drogas
Pingback: Tape a call
Pingback: Best online store builder
Pingback: babes free porn videos
Pingback: mens jewellery
Pingback: melo porn
Pingback: heroína
Pingback: lesbian sex movies
Pingback: hot cumshot videos
Pingback: masterporner.com
Pingback: art
Pingback: pix de copiat
Pingback: Sisteme de copiat
Pingback: Whole Life Insurance phoenix az
Pingback: how to be successful and sell more.
Pingback: ebony interracial porn
Pingback: Universal Life Insurance peoria az
Pingback: Pekin Life Insurance glendale az
Pingback: Life Insurance quote phoenix az
Pingback: gangbang hot porn
Pingback: Term Life Insurance peoria az
Pingback: best luxury cars
Pingback: download book
Pingback: showbox for android
Pingback: car discount
Pingback: football scores
Pingback: The Paradigm Ancient Blueprint Jonathan Cahn
Pingback: download pdf
Pingback: Paradigm Ancient Blueprint Jonathon Cahn
Pingback: Paradigm Ancient Blueprint Jonathon Cahn
Pingback: football school
Pingback: men's health
Pingback: Ecommerce Strategy
Pingback: FleetUp
Pingback: Melbourne Digital Marekting Agency
Pingback: FleetUp
Pingback: Affordable Digital Marekting Agency Melbourne
Pingback: Branding and design
Pingback: healthy weight
Pingback: ELD Mandate
Pingback: nagging hip pain
Pingback: ELD
Pingback: ELD Mandate
Pingback: hip flexor stretches
Pingback: FleetUp
Pingback: libido
Pingback: ELD Mandate
Pingback: SEO Service Melbourne
Pingback: ELD
Pingback: FleetUp
Pingback: ELD
Pingback: free games download for android phones
Pingback: ELD Mandate
Pingback: ELD Mandate
Pingback: ELD Mandate
Pingback: ELD Mandate
Pingback: ontario
Pingback: contractor
Pingback: FleetUp
Pingback: FleetUp
Pingback: ELD Mandate
Pingback: ELD
Pingback: FleetUp
Pingback: contractor
Pingback: https://www.netfondsbank.fi/quotes/release.php?id=20170713.GlobeNewswire.HUG2120144
Pingback: nagging hip pain
Pingback: unlock your hip flexors
Pingback: hip pain
Pingback: hip flexor stretches
Pingback: nagging hip pain
Pingback: ELD
Pingback: Rottestop
Pingback: ELD
Pingback: ELD
Pingback: ELD
Pingback: FleetUp
Pingback: FleetUp
Pingback: ELD
Pingback: FleetUp
Pingback: ELD Mandate
Pingback: ELD
Pingback: FleetUp
Pingback: Palas de padel
Pingback: Spell casting services
Pingback: ELD Mandate
Pingback: Spell casting services
Pingback: ELD Mandate
Pingback: ELD Mandate
Pingback: FleetUp
Pingback: daddy b sunglasses
Pingback: Martin Costanzo Contentmarketing
Pingback: cazal vintage sunglasses 616
Pingback: c&g sunglasses
Pingback: ELD
Pingback: ELD
Pingback: FleetUp
Pingback: Hype
Pingback: pandasilk.com
Pingback: panda silk
Pingback: Jugg Culture Clothing
Pingback: 3m eyewear
Pingback: pandasilk.com
Pingback: www.pandasilk.com/
Pingback: Hype Clothing
Pingback: www.pandasilk.com
Pingback: nike vintage 74 sunglasses
Pingback: CDG
Pingback: ELD Mandate
Pingback: ELD
Pingback: ELD
Pingback: FleetUp
Pingback: FleetUp
Pingback: ELD Mandate
Pingback: Modern Slip
Pingback: florida contractor background checks
Pingback: company bankruptcy records
Pingback: carte grise en ligne
Pingback: Modern Slip
Pingback: three lengths
Pingback: Loti
Pingback: background checking service
Pingback: injecthack com mobilelegends mobile legends
Pingback: St. Bernard Rescue Group
Pingback: Saint Bernard
Pingback: Saint Bernard Rescue Group
Pingback: company driving records
Pingback: drug screening
Pingback: image
Pingback: Bali helicopter price
Pingback: 8ballpoolhacks club 8 ball pool
Pingback: Telugu movie reviews
Pingback: dresses
Pingback: clasherhack4me com clash royale
Pingback: Dazzling 13 Satin Half-Slip in Light Blue
Pingback: progems info clash of clans
Pingback: Dazzling 13 Satin Half-Slip in Light Blue
Pingback: image
Pingback: kostenloscoins com fifa 17
Pingback: Andhra News
Pingback: florida backgound checks
Pingback: image
Pingback: maddencoinprovider com madden nfl mobile 18
Pingback: latest world gossip
Pingback: business background check
Pingback: www.LotiSlips.com
Pingback: Andhra English news paper
Pingback: www.LotiSlips.com
Pingback: football
Pingback: hire web designer
Pingback: Andhra English news paper
Pingback: latest worlds news and gossip
Pingback: new Bollywood movies trailer
Pingback: Telugu movie reviews
Pingback: Andhra English news paper
Pingback: Andhra Political News
Pingback: Telugu news online websites
Pingback: Calcio
Pingback: background checking service
Pingback: image
Pingback: falun dafa
Pingback: Medical Jobs?
Pingback: Free Full Movies Online
Pingback: Watch movies Online Free
Pingback: Music Promotion
Pingback: Watch Wonder Woman Online Free
Pingback: RN Jobs Fort Worth?
Pingback: Physicians Careers Dallas?
Pingback: Watch It 2017 Online Free
Pingback: Watch Wonder Woman Online Free
Pingback: fanny pack
Pingback: elephant boho bedding
Pingback: website guided tour todos-santos
Pingback: best tours colonia-del-sacramento
Pingback: local guides innsbruck
Pingback: best tours dublin
Pingback: best webhosting
Pingback: mega depot coupons
Pingback: meditation
Pingback: best perfumes
Pingback: Michael Hall
Pingback: manufacturer coupons
Pingback: Retro Gas Pumps
Pingback: Custom Complete Pro Scooters
Pingback: Pro Scooter Accessories
Pingback: 14k gold watches
Pingback: Coca-Cola furniture
Pingback: Pro Scooter Parts
Pingback: Retro Gas Pumps
Pingback: Compression for Pro Scooters
Pingback: Animal Life
Pingback: Alyce Lemus
Pingback: Dinettes
Pingback: Pro Scooter Headsets
Pingback: News
Pingback: Mothership on YouTube
Pingback: Pro Scooter Griptape
Pingback: Mothership on Instagram
Pingback: Stanley Shao
Pingback: Ping Geyer
Pingback: Relationship Hacks
Pingback: Pro Rider Chase Robertson
Pingback: About Mothership
Pingback: Dusty Sitzes
Pingback: Mothership Pro Scooters
Pingback: Rosanne Peele
Pingback: Retro Gas Pumps
Pingback: Complete Pro Scooters
Pingback: Pro Rider Alex Blome
Pingback: Idell Rodrigues
Pingback: order Lacing hook at insulpins.com
Pingback: order insulation pins at insulpins.com
Pingback: how to train your dog at home
Pingback: potty training dogs
Pingback: Retro Booths
Pingback: dog house training
Pingback: Jayden Lee
Pingback: order Mild Steel Lacing Anchors at insulpins.com
Pingback: potty training dogs
Pingback: dog chewing
Pingback: Pro Rider Alex Fish
Pingback: Pro Scooter Apparel
Pingback: led ceiling lights
Pingback: dog training
Pingback: Bar Chairs
Pingback: Tom Krol
Pingback: Real Estate
Pingback: dog house training
Pingback: dog obedience training
Pingback: Real Estate
Pingback: Retro Appliances
Pingback: Mothership on Facebook
Pingback: Real Estate
Pingback: Travis Minion
Pingback: Wholesaling Inc
Pingback: Custom Kitchens
Pingback: How to Make Money Wholesaling Real Estate
Pingback: Tom Krol Wholesaling
Pingback: Dean Brittin
Pingback: Wholesaling
Pingback: Goa Government Jobs
Pingback: Kingsley Okocha
Pingback: Wholesaling
Pingback: escort canada
Pingback: order Square Self-Locking Washers at insulpins.com
Pingback: Slim couture
Pingback: Tamil Nadu Sarkari Naukri
Pingback: Real Estate
Pingback: order Quilting Pins at insulpins.com
Pingback: best engagement rings toronto
Pingback: Real Estate
Pingback: escorts in italy
Pingback: Private Lessons
Pingback: Koa campgrounds
Pingback: escort bucharest
Pingback: escort netherlands
Pingback: Sue Evelyn Gil
Pingback: Slim couture review
Pingback: MODA
Pingback: IDIOMAS
Pingback: Slim couture
Pingback: Koa San Diego
Pingback: Travel
Pingback: Koa Kampgrounds
Pingback: A??ES
Pingback: incubator startup
Pingback: MODA
Pingback: Pro Scooter Decks
Pingback: MODA
Pingback: startup help
Pingback: innovative business ideas
Pingback: JT Sitton
Pingback: startup financing
Pingback: business startup ideas
Pingback: how to print on tyvek wristbands
Pingback: brick paver
Pingback: Slim couture review
Pingback: mat frasier t shirt
Pingback: Pro Scooter Pegs
Pingback: SEO Service Melbourne
Pingback: Pro Scooter Forks
Pingback: Pro Rider Danila Popov
Pingback: Lum Law Group
Pingback: weightlifting t shirt
Pingback: 2014 Ford Rims & Tires
Pingback: mens crossfit
Pingback: weightlifting t shirt
Pingback: search optimization
Pingback: chat net
Pingback: mobile accessories
Pingback: Lum Law Group
Pingback: Lum Law Group
Pingback: 10 best birthday gifs for man
Pingback: windproof golf umbrella
Pingback: jaranwala chat rooms
Pingback: what do women want
Pingback: desi chat room
Pingback: fill in the blank quiz maker
Pingback: custom quiz maker
Pingback: SEO Service Melbourne
Pingback: traders
Pingback: Best VPN provider
Pingback: foreign exchange market
Pingback: VPN free
Pingback: currency exchange
Pingback: can ho du an avenue thu duc
Pingback: forex rates
Pingback: VPN torrents
Pingback: vinyl
Pingback: super alpha reseller hosting india
Pingback: reseller hosting
Pingback: Free Blesta reseller hosting
Pingback: Best Dutch VPN
Pingback: Job App
Pingback: Dutch VPN
Pingback: Master Reseller Hosting
Pingback: GoodVPN
Pingback: modafinil purchase
Pingback: Job Seeking
Pingback: provigil online
Pingback: modafinil online
Pingback: Beste Nederlandse VPN
Pingback: VPN NL
Pingback: Online Recruitment
Pingback: GOOSE review
Pingback: Belfast Jobs
Pingback: GOOSE NL
Pingback: IPVanish
Pingback: www.hotvoyeurporno.com
Pingback: Dutch VPN
Pingback: IPVanish
Pingback: Affordable Portland Psychic
Pingback: Affordable Portland Psychic
Pingback: NL VPN
Pingback: GOOSE review
Pingback: football370
Pingback: football3365
Pingback: trezory Praha
Pingback: moderni turnikety
Pingback: articoli rover
Pingback: moderni turnikety
Pingback: artwork for sale by artist
Pingback: ICO Token Sale
Pingback: artwork for sale canada
Pingback: prodotti bricolage
Pingback: trezory
Pingback: artwork for sale dublin
Pingback: articoli rover
Pingback: trezory
Pingback: turnikety
Pingback: bricolage a verona
Pingback: duplicazione telecomandi
Pingback: umbrella
Pingback: bare minerals brushes
Pingback: spiky massage ball
Pingback: kabuki brush mineral powder
Pingback: cheap CPR certification
Pingback: massage roller
Pingback: bare essentials mineral veil
Pingback: core coverage brush
Pingback: bounce house rentals Upland
Pingback: edc fidget spinner
Pingback: cyber Monday deal
Pingback: best fidget spinner
Pingback: kabuki brush mineral powder
Pingback: makeup brush case
Pingback: iphone 7 Plus hulle bedrucken
Pingback: apple louis vuitton iphone hulle
Pingback: flip hulle iphone 7 Plus
Pingback: iphone 7 Plus hulle galaxy
Pingback: iphone 7 Plus hulle lv
Pingback: filzhulle louis vuitton iphone 6 plus
Pingback: gifts for mom
Pingback: aheap appliance repair
Pingback: 2015 tax return
Pingback: financial planning magazine
Pingback: intuit
Pingback: birthday gifts for women
Pingback: Clube dos Novos Ricos
Pingback: cyber Monday
Pingback: dj wed menomonee falls
Pingback: tax planning
Pingback: federal tax
Pingback: tweezers precision
Pingback: your dj menomonee falls
Pingback: free social network
Pingback: tree root removal
Pingback: waste management dumpster rental
Pingback: samsung appliance repair
Pingback: tree and stump removal
Pingback: Waukesha getting rid of tree roots
Pingback: landers appliance repair
Pingback: a and a appliance
Pingback: lg appliance customer service
Pingback: appliance repair kansas city mo
Pingback: formata??o para tcc
Pingback: Como fazer uma monografia passo a passo
Pingback: trash dumpster rental
Pingback: dumpster
Pingback: construction dumpster rental
Pingback: garbage containers for rent
Pingback: dumpster trash
Pingback: dumpster dimensions waste management
Pingback: chipsi
Pingback: stainless tube sizes
Pingback: Condominium for rent
Pingback: Watermark @ Robertson Quay
Pingback: District 02
Pingback: Watermark @ Robertson Quay
Pingback: Photo slideshow maker
Pingback: Discover More
Pingback: Zanzibar pizza
Pingback: Zanzibar restaurant
Pingback: Wedding Slideshow
Pingback: School event Photo Collage with music
Pingback: Online Photo Collage for Graduation
Pingback: blocked drains sydney
Pingback: Cheap Photo Slideshow with Music
Pingback: Learn More Here
Pingback: sydney blocked drains
Pingback: blocked drains sydney
Pingback: Soccer Game Photo Collage
Pingback: sydney blocked drains
Pingback: Visit This Link
Pingback: Create Video Slideshow
Pingback: loft conversions london
Pingback: click for source
Pingback: Recommended Site
Pingback: KB Tan
Pingback: Rivergate
Pingback: chrome toilet roll holder
Pingback: Buffet Corporativo
Pingback: bathroom wastebaskets
Pingback: accessories for bathroom
Pingback: Buffet Corporativo
Pingback: bathroom ornaments
Pingback: bathroom collections
Pingback: Free /r/WeAreTheMusicMakers Music Promotion
Pingback: screen printed t-shirts
Pingback: I Will Upload Your Music On My 50,000 Plus Youtube Channel
Pingback: embroidered polo shirts
Pingback: roll off
Pingback: trash dump
Pingback: West Palm Beach WordPress Design
Pingback: Free HipHop Music Promotion
Pingback: West palm beach sexy photographer
Pingback: visado para rusia
Pingback: dumpster rental cost
Pingback: 8 yard dumpster
Pingback: zonnepanelen kopen? Soloya, uw expert zonnepanelen
Pingback: Photo Editing
Pingback: garbage container rental
Pingback: Fasting for health
Pingback: Coconut Protein
Pingback: trash container rentals
Pingback: get a dumpster
Pingback: Fasting
Pingback: Plant-based protein
Pingback: West palm beach media kit design
Pingback: dumpster rental san jose
Pingback: peliculas online
Pingback: rusalia
Pingback: dump containers for rent
Pingback: carta de invitacion rusia
Pingback: bfi bin rental
Pingback: Benefits of coconut
Pingback: price for dumpster rental
Pingback: Plant based protein
Pingback: dumpster rental Sandy Springs
Pingback: Pea protein
Pingback: dumpster rental prices
Pingback: visado para entrar en rusia
Pingback: Health benefits of baobab
Pingback: Efile 2290
Pingback: couch dollars
Pingback: free samples
Pingback: carta invitacion rusia
Pingback: competitions
Pingback: rusalia
Pingback: teclado espa?ol qwerty
Pingback: couch-dollars
Pingback: tren moscu san pertersburgo
Pingback: couch-dollars
Pingback: airconditioning Limburg
Pingback: dumpster rental canton
Pingback: carta de invitacion rusia
Pingback: que ver en mosc?
Pingback: recorrido del transiberiano
Pingback: couch-dollars
Pingback: airco installatie
Pingback: need a dumpster
Pingback: dumpster rental Ashford
Pingback: 2 yard dumpster
Pingback: santa monica wordpress development
Pingback: carta de invitacion rusia
Pingback: zonnepanelen Limburg
Pingback: airco unit
Pingback: santa monica wordpress development
Pingback: construction waste containers
Pingback: rent trash container
Pingback: rent a construction dumpster
Pingback: visado turista rusia
Pingback: santa monica wordpress developer
Pingback: dump containers for rent
Pingback: entradas kremlin
Pingback: santa monica wordpress development
Pingback: bulk trash
Pingback: warmtepomp installatie
Pingback: roll off dumpster waste management
Pingback: dumpster rental ypsilanti
Pingback: dumpster rental bingham
Pingback: bulk sms registration in nigeria
Pingback: sms love
Pingback: Lucht/water warmtepompen
Pingback: tramitar visado rusia
Pingback: love sms
Pingback: bulk sms nigeria
Pingback: Hybride warmtepomp
Pingback: flashback tonight
Pingback: new music
Pingback: dumpster rental grosse point
Pingback: dumpster rental canton
Pingback: website
Pingback: previous guests
Pingback: dumpster rental oakland county
Pingback: veteriner ankara
Pingback: bin rental
Pingback: waste removal
Pingback: anti aging moisturizer
Pingback: daily moisturizer
Pingback: veteriner ankara
Pingback: Ketones
Pingback: moisturizing cream
Pingback: Paleo
Pingback: veteriner
Pingback: dumpster containers for rent
Pingback: garbage bin rental prices
Pingback: Best Rap Playlist 2017
Pingback: caffeine pills
Pingback: Plant based protein
Pingback: 30 yard dumpster rental
Pingback: sell house fast
Pingback: Best Spotify Rap Playlist
Pingback: sell quick for cash
Pingback: I buy houses
Pingback: simple security
Pingback: free cybersecuritiy
Pingback: Nutrition
Pingback: thay man hinh iphone 7
Pingback: Plant-based protein
Pingback: 106R01504 XEROX
Pingback: 783064425667 PLUSTEK
Pingback: EV3237FXBK EIZO
Pingback: emergency plumber
Pingback: TVS871I58GUS QNAP
Pingback: local plumbers
Pingback: emergency plumber biggleswade
Pingback: WIRELESS-4972044.html
Pingback: hotporntube.mobi
Pingback: credit score
Pingback: eviction history check
Pingback: sex toys
Pingback: short film
Pingback: screenwriting competition
Pingback: bluedigitalnetwork.com/
Pingback: www.bluedigitalnetwork.com
Pingback: Hiphop playlist
Pingback: blue digital network,LLC
Pingback: background check texas
Pingback: Dope rap playlist
Pingback: documentary
Pingback: bluedigitalnetwork.com/
Pingback: bluedigitalnetwork
Pingback: impact investing
Pingback: sasha grey sex toy
Pingback: background screening for employment
Pingback: Remote Vibrating Egg
Pingback: adamandeve
Pingback: dog walking
Pingback: bowfishing addict
Pingback: bowfishing addict
Pingback: bowfishing addict
Pingback: Medicaid Orthodontist
Pingback: bowfishing addict
Pingback: bowfishing addict
Pingback: bowfishing addict
Pingback: Oleg Mitnik
Pingback: buy a domian name
Pingback: tv shows
Pingback: buy a domian name
Pingback: derinny
Pingback: register a australian domain
Pingback: hotel packages
Pingback: cheap luxury hotels
Pingback: Goa holiday package
Pingback: get ready to fall for bhutan
Pingback: how to buy www.name
Pingback: UXOriskmanagment
Pingback: top fight stick
Pingback: purchasing a domian name
Pingback: surveillance
Pingback: kidnapping
Pingback: external graphics card
Pingback: gaming routers
Pingback: surveillance
Pingback: yachtrecovery
Pingback: kidnapping
Pingback: www.hsse-global.com
Pingback: Read More
Pingback: www.hsse-global.com
Pingback: www.hsse-global.com
Pingback: Job Platform on Blockchain
Pingback: kidnap
Pingback: HSSEtraining
Pingback: UXOriskmanagment
Pingback: Glow in the Dark Canvas Painting Maple Tree Wall Art
Pingback: Stretched Framed Giclee Canvas Print Red Maple
Pingback: Canvas Painting Master Bedroom Living Room Decor Solar System
Pingback: youpornmove.net
Pingback: professional indian wedding photography
Pingback: rajwap.xyz
Pingback: Pre Wedding
Pingback: Stretched Framed Giclee Canvas Print The Sun
Pingback: Les actus de Khalifa sall
Pingback: Informations sante et sport du senegal
Pingback: Slim couture reviews
Pingback: Les actus de Abdoulaye wade
Pingback: wedding album cover page
Pingback: Informations sante et sport du senegal
Pingback: Les lions du senegal
Pingback: best EA for forex trading
Pingback: celebrity photographer in chandigarh
Pingback: Cancun airport taxi
Pingback: destination wedding photographers
Pingback: Promote Your Business To Worldwide
Pingback: Cancun airport private transportation
Pingback: Free URL Shortener
Pingback: kabuki brush kit
Pingback: elf kabuki brush
Pingback: kabuki brush set
Pingback: Cancun airport private transportation
Pingback: mermaid kabuki brush
Pingback: ecotool kabuki brush
Pingback: kabuki brush sets
Pingback: indian wedding album design
Pingback: wedding photographers in Chandigarh
Pingback: pre-wedding shoot
Pingback: Airco
Pingback: social media marketing
Pingback: Airconditioning prijzen
Pingback: free bookmarking sites list
Pingback: Alarmsysteem prijs
Pingback: Airco Limburg
Pingback: bahaya behel murah
Pingback: harga pasang behel gigi asli
Pingback: bahaya behel murah
Pingback: Koelinstallaties
Pingback: harga behel permanen
Pingback: Kizi game
Pingback: Alarmsystemen voor de woning en het huis
Pingback: Citrus Hills carpet cleaning
Pingback: Koelsystemen
Pingback: design custom development
Pingback: Vriescellen Vriesinstallaties om te koelen? A-Aircool
Pingback: Lucht-water warmtepomp
Pingback: Frigobouw
Pingback: Read This
Pingback: Learn More
Pingback: harga pasang behel gigi asli
Pingback: Visit This Link
Pingback: Clicking Here
Pingback: Visit This Link
Pingback: finding a language school
Pingback: This Site
Pingback: Click This Link
Pingback: Home Page
Pingback: Discover More Here
Pingback: beer home brewing kit
Pingback: home brew beer kit
Pingback: Beveiliging Woning
Pingback: best language schools
Pingback: beer brewing
Pingback: best home brewing kit
Pingback: best spanish school
Pingback: Discover More Here
Pingback: Spanish Schools in Buenos Aires
Pingback: wine making equipment
Pingback: Read Full Report
Pingback: top 40 charts us
Pingback: too 40 charts
Pingback: Read This
Pingback: Alarminstallaties
Pingback: Tips Lissabon
Pingback: Stedentrip Lissabon
Pingback: Camerabewaking thuis
Pingback: Visit Website
Pingback: Attracties Lissabon
Pingback: Get More Info
Pingback: Cryptocurrency
Pingback: Click Here
Pingback: companies that buy life insurance policies
Pingback: Earn Easy Cash
Pingback: best film directors
Pingback: Read More
Pingback: Click For More Information
Pingback: selling life insurance policy
Pingback: corporate film production
Pingback: companies that buy life insurance policies
Pingback: best production companies
Pingback: best film directors
Pingback: Click For More Information
Pingback: Film production company
Pingback: los angeles film directors
Pingback: Read More
Pingback: sell life insurance policy
Pingback: who buys life insurance policies
Pingback: best production companies
Pingback: mako beast
Pingback: best production companies
Pingback: Airco-airconditioning.be
Pingback: softball bat
Pingback: independent film company
Pingback: Click For More Information
Pingback: carpet cleaning Crystal River
Pingback: baseball skull cap
Pingback: www.airco-airconditioning.be/installateurs-airco-antwerpen
Pingback: softball bat
Pingback: Sell Your Life Insurance
Pingback: Port Richey carpet cleaning
Pingback: companies that buy life insurance policies
Pingback: companies that buy existing life insurance policies
Pingback: Beverly Hills production company
Pingback: Airco installateurs Limburg
Pingback: get youtube subscribers free
Pingback: Ethereum
Pingback: professional makeup brushes
Pingback: kabuki brush bare minerals
Pingback: air conditioning repair finance
Pingback: air conditioning repair finance
Pingback: health insurance
Pingback: cushie Airbnb
Pingback: Airbnb Property management service
Pingback: types of health insurance
Pingback: best healthcare
Pingback: bare minerals lasting line forever brandy
Pingback: health benefits
Pingback: bare essentials makeup brushes
Pingback: carte grise en ligne
Pingback: cushie Airbnb management package
Pingback: silicone sex dolls
Pingback: changer adresse carte grise
Pingback: japanese sex dolls
Pingback: acrylic nail clippers
Pingback: nail clipper blades
Pingback: Norway Casinos
Pingback: carte grise Saint-Martin-Bellevue
Pingback: carte grise Saint-Martin-De-Lixy
Pingback: carte grise Berrwiller
Pingback: ingrown toenail clipper set
Pingback: carte grise Blousson-Serian
Pingback: floating artificial flowers
Pingback: carte grise Geveze
Pingback: dildos
Pingback: carte grise Norrois
Pingback: waterproof vibrators
Pingback: flower float
Pingback: Apple iPod
Pingback: hijama birmingham
Pingback: carte grise Montceaux
Pingback: air conditioning repair finance
Pingback: Apple accessories
Pingback: pool bathroom decor
Pingback: hijama birmingham
Pingback: Replica Graham London
Pingback: vibrator kits
Pingback: Apple Watch Edition
Pingback: Replica reloj Longines
Pingback: tez i?indekiler haz?rlama
Pingback: changer carte grise
Pingback: giri? b?l?m? ?rnekleri
Pingback: Bell & Ross Replica
Pingback: sell my stuff manila
Pingback: bondage
Pingback: knock off Blancpain
Pingback: quality sex toys shop
Pingback: carte grise Saint-Martin-D'ollieres
Pingback: fetish sex toys online
Pingback: carte grise Notre-Dame-D'aliermont
Pingback: carte grise Bellonne
Pingback: buy, sell, trade in manila
Pingback: sex toys
Pingback: dildo
Pingback: buy car in manila
Pingback: sell your stuff manila
Pingback: tez yazd?rma
Pingback: intihal program?
Pingback: manta geotextil
Pingback: Replica Corum
Pingback: online casino
Pingback: imitation Rado
Pingback: Casino norsk
Pingback: tubo dreno
Pingback: manta geotextil
Pingback: Scratch Map
Pingback: carte grise Saint-Symphorien
Pingback: www.soloya.be/airco-antwerpen-airconditioning-antwerpen
Pingback: Parc Botannia floor plan
Pingback: Applerok rewards
Pingback: carte grise Ludes
Pingback: Read More
Pingback: Apple Watch Series 1
Pingback: carte grise Guyencourt
Pingback: a dragons dinner t shirt
Pingback: a dragons dinner t shirt
Pingback: carte grise Saint-Vincent-De-Salers
Pingback: www.soloya.be/prijs-airco-kopen-prijzen-aircondtioning-kosten-airco-unit-aircosystemen-split
Pingback: iPhone X
Pingback: Cabra Golf Course
Pingback: Cabra Golf Course
Pingback: Adam and Eve Code
Pingback: Apple Watch Bands
Pingback: Rendement Zonnepanelen Opbrengst - Soloya
Pingback: golf membership
Pingback: 24hr refrigeration repairs mandurah
Pingback: Warmtepomp Antwerpen - Warmtepompen Antwerpen? Soloya
Pingback: Apple Watch Hermes
Pingback: Applerok Sitemap
Pingback: wall split conditioning maintenance
Pingback: Golf Course Sydney
Pingback: wall split conditioning maintenance
Pingback: golf course cabramatta
Pingback: 15 Minute Manifestation
Pingback: refrigerators
Pingback: tarif carte grise
Pingback: plano de sa?de para cachorro
Pingback: Lean Belly Breakthrough
Pingback: health for pet
Pingback: a dragons dinner t shirt
Pingback: a dragons dinner t shirt
Pingback: refrigerators
Pingback: a dragons dinner t shirt
Pingback: consultas
Pingback: ducted air conditioning mandurah
Pingback: consultas
Pingback: a dragons dinner t shirt
Pingback: a dragons dinner t shirt
Pingback: seguro pet
Pingback: Divorce Coach Partners
Pingback: a dragons dinner t shirt
Pingback: Apple iPod
Pingback: Teds Woodworking
Pingback: a dragons dinner t shirt
Pingback: Marketing for Divorce Lawyers
Pingback: skateboard decks for sale
Pingback: stainless tweezers
Pingback: vetus tweezers
Pingback: solingen tweezers
Pingback: skateboard bag
Pingback: tweezerman slant tweezers
Pingback: rilastil stretch mark cream
Pingback: skate shopping
Pingback: best stretch marks cream
Pingback: cheap skateboards
Pingback: dr max powers stretch mark cream
Pingback: stretch mark cream organic
Pingback: beauty facial extreme stretch mark and scar repair cream
Pingback: sieva skincare stretch mark & scar removal cream
Pingback: breastfeeding nipplecream
Pingback: pink nipplecream
Pingback: A-Aircool.be Warmtepomp Limburg
Pingback: the nursing mother's companion
Pingback: www.a-aircool.be/koelcellen-koelsystemen-koeltechnieker
Pingback: nursing pads washable
Pingback: copie de Longines
Pingback: copie de U-Boat
Pingback: nursing pillow cover
Pingback: A-Aircool Koeling
Pingback: Airco installateur Limburg
Pingback: Airconditioning prijs
Pingback: A-Aircool.be Warmtepompen
Pingback: Koeltechniek? Reken op A-Aircool Koeltechnieken
Pingback: Pembroke Pines
Pingback: Alexandria
Pingback: Pittsburgh
Pingback: bin
Pingback: Kent
Pingback: www.muvemint.com/contact-us
Pingback: Reno
Pingback: control
Pingback: Savannah
Pingback: www.muvemint.com
Pingback: button
Pingback: airbags
Pingback: molding
Pingback: www.muvemint.com
Pingback: Arlington
Pingback: Denton
Pingback: www.muvemint.com
Pingback: Baltimore
Pingback: airbags
Pingback: buttons
Pingback: panel
Pingback: panel
Pingback: Minneapolis
Pingback: switch
Pingback: interior
Pingback: actuator
Pingback: console
Pingback: belts
Pingback: a place for gamers to talk about video games
Pingback: Extra resources
Pingback: Continue
Pingback: Continued
Pingback: Continue Reading
Pingback: More about the author
Pingback: helpful hints
Pingback: a place for gamers to talk about video games
Pingback: before after photos newport beach
Pingback: Website creation and Hosting
Pingback: Website creation and Hosting
Pingback: Catering Equipment
Pingback: Industrial Food Processing Equipment
Pingback: Commercial Kitchen Equipment
Pingback: smykker til kjole
Pingback: vesker til ballkjole
Pingback: Commercial Cooking Equipment
Pingback: Commercial Kitchen Equipment
Pingback: Top Brands Industrial Cooking Equipment
Pingback: selskapskjoler 2018
Pingback: ballkjoler oslo butikk
Pingback: whiteboard animation
Pingback: fungal nail infection
Pingback: Facebook chatbot
Pingback: toenail fungus treatment
Pingback: Chatbot Solution Platform
Pingback: Chatbot Solution
Pingback: toenail fungus treatment
Pingback: Facebook chatbot
Pingback: best toenail fungus treatment
Pingback: Facebook chatbot
Pingback: best coffee machine
Pingback: coffee grinder
Pingback: cafe supplies
Pingback: whiteboard animation singapore
Pingback: como Hackear whatsapp
Pingback: coffee machine accessories
Pingback: wholesale coffee supplies
Pingback: whatsapp
Pingback: como Hackear whatsapp
Pingback: hackear una cuenta de whatsapp
Pingback: Espiar conversaciones de whatsapp
Pingback: como Hackear whatsapp
Pingback: como espiar conversaciones de whatsapp
Pingback: hackear una cuenta de whatsapp
Pingback: espiar whatsapp solo con el numero de celular
Pingback: vlogging camera with flip screen
Pingback: Shine
Pingback: espiar whatsapp solo con el numero de celular
Pingback: hackear Facebook online
Pingback: best cheap camera for youtube
Pingback: Animation touristique
Pingback: fungal nail infection
Pingback: DJ Soir?
Pingback: Drone
Pingback: best blogging camera
Pingback: DJ Soir?
Pingback: nail fungus treatment over the counter
Pingback: foot fungus cure
Pingback: raprock
Pingback: hackear una cuenta Facebook
Pingback: OIA PRIVATE TRANSFER
Pingback: Como hackear un Facebook
Pingback: Como espiar conversaicones de whatsapp 2018
Pingback: singapore web development company
Pingback: tweezerman tweezers
Pingback: espiar whatsapp solo con el numero de celular
Pingback: tooltron tweezers
Pingback: branding agencies in singapore
Pingback: Como espiar conversaciones de una cuenta de whatsapp
Pingback: web design company in singapore
Pingback: eurotool tweezers
Pingback: Check This Out
Pingback: tweezers eyelash extension
Pingback: espiar whatsapp android ios
Pingback: round tip tweezers
Pingback: Check This Out
Pingback: hackear una cuenta de Facebook 2018
Pingback: como espiar conversaciones de whatsapp
Pingback: latest hip hop music
Pingback: hip hop songs 2016
Pingback: Animation commerciale
Pingback: Dйcoration ballons
Pingback: vlogging camera with flip screen
Pingback: vlogging with iPhone
Pingback: Como hackear facebook
Pingback: web design companies in singapore
Pingback: Como hackear un Facebook
Pingback: lemonade web design
Pingback: Como hackear un Facebook
Pingback: order a dumpster
Pingback: junk disposal
Pingback: roofing specialists
Pingback: como hackear un Facebook gratis
Pingback: junk removal toronto
Pingback: Local University
Pingback: local dumpster
Pingback: dumpster in a bag
Pingback: Facebook
Pingback: installing steel roofing
Pingback: commercial roofing company
Pingback: ten yard dumpster
Pingback: roof design
Pingback: International Rajabhat Univerty
Pingback: como hackear un Facebook gratis
Pingback: towing company in detroit mi
Pingback: Academic
Pingback: road assistance service
Pingback: como hackear Facebook 2018
Pingback: used flatbeds for sale
Pingback: hackear una cuenta de Facebook 2018
Pingback: pick truck parts
Pingback: part select
Pingback: Local University
Pingback: como hackear un Facebook gratis
Pingback: where to sell car parts
Pingback: lg certified appliance repair
Pingback: washer dryer parts
Pingback: whirlpool home appliances
Pingback: whirlpool washer repair service
Pingback: wheel lift truck
Pingback: tow truck wreckers for sale
Pingback: Thailand Rajabhat
Pingback: eyeliner
Pingback: duvet sets
Pingback: grey bedding
Pingback: General Surgery Jobs
Pingback: king size duvet
Pingback: best beauty products
Pingback: facebook
Pingback: masturbation
Pingback: Lahore Escorts
Pingback: mobile app developers
Pingback: iPhone app development companies
Pingback: Bitcoin
Pingback: lezioni di musica novara
Pingback: create a website
Pingback: top 10 app development companies toronto
Pingback: Bitcoin
Pingback: scuola di canto bambini novara
Pingback: ICO Marketing
Pingback: Bitcoin
Pingback: foxtailmarketing.com
Pingback: Bitcoin
Pingback: Doctors in Durban
Pingback: Occupational Therapist
Pingback: Foxtail Marketing
Pingback: Bitcoin
Pingback: Optometry Practice
Pingback: Dietician
Pingback: bitmining
Pingback: www.foxtailmarketing.com
Pingback: bitmining
Pingback: bitmining
Pingback: bitmining
Pingback: Cryptocurrency Marketing
Pingback: bitmining
Pingback: bitmining
Pingback: bitclub
Pingback: bitclub
Pingback: Foxtail Marketing
Pingback: Foxtail Marketing
Pingback: www.foxtailmarketing.com
Pingback: Foxtail Marketing
Pingback: cryptocurrency
Pingback: ICO Marketing
Pingback: cryptocurrency
Pingback: www.foxtailmarketing.com
Pingback: cryptocurrency
Pingback: cryptocurrency
Pingback: ICO Marketing
Pingback: introduction to bitcoin
Pingback: introduction to bitcoin
Pingback: introduction to bitcoin
Pingback: foxtailmarketing.com
Pingback: Cryptocurrency Marketing
Pingback: introduction to bitcoin
Pingback: speed jump rope
Pingback: Foxtail Marketing
Pingback: foxtailmarketing.com
Pingback: benefits of jump rope
Pingback: Bitcoin
Pingback: bitmining
Pingback: www.foxtailmarketing.com
Pingback: Bitcoin
Pingback: foxtailmarketing.com
Pingback: www.foxtailmarketing.com
Pingback: Bitcoin
Pingback: Cryptocurrency Marketing
Pingback: introduction to bitcoin
Pingback: cryptocurrency
Pingback: bitclub
Pingback: introduction to bitcoin
Pingback: cryptocurrency
Pingback: volunteer tourism
Pingback: Siebtlingsgeburt
Pingback: helpful hints
Pingback: Cryptocurrency Marketing
Pingback: ICO Marketing
Pingback: Loan Bitcoin
Pingback: pinzette tweezers
Pingback: www.foxtailmarketing.com
Pingback: helping
Pingback: traveling
Pingback: medical volunteer
Pingback: abroad
Pingback: Visit This Link
Pingback: mink eyelash tweezers
Pingback: animal protection
Pingback: More Information
Pingback: Ecuador
Pingback: cadeau personnalisй pour enfant
Pingback: cadeau avec prenom
Pingback: YOURURL.com
Pingback: Apple iPhone
Pingback: livre personnalisй prйnom bйbй
Pingback: Related Site
Pingback: livre personnalisй pas cher
Pingback: gambling theme
Pingback: livres personnalisйs avec prйnom
Pingback: apprendre le piano pour debutant
Pingback: mйthode de piano dйbutant
Pingback: piano apprendre a jouer
Pingback: wall clings
Pingback: wall paint design
Pingback: xcelite tweezers
Pingback: retractable kabuki brush set
Pingback: dumpster cost
Pingback: large dumpster rental
Pingback: ken
Pingback: modern wall décor
Pingback: dumpster rental
Pingback: wall decorations for bedroom
Pingback: Click Here
Pingback: cleaning services Melbourne
Pingback: kitchen wall stickers
Pingback: cleaning services Melbourne Fl
Pingback: 3 yard dumpster rental
Pingback: 30 yard dumpster rental
Pingback: wall décor for bedroom
Pingback: 20 yard dumpster rental prices
Pingback: 30 cubic yard dumpster
Pingback: kabuki brushes
Pingback: mac kabuki brush
Pingback: junk removal toronto
Pingback: cleaning services Melbourne Fl
Pingback: Magic Mops House Cleaning
Pingback: Bewerbung schreiben lassen erfahrungen
Pingback: big dumpster rental
Pingback: laura mercier kabuki brush
Pingback: rounded kabuki brush
Pingback: world urdu news
Pingback: magic mops cleaning
Pingback: refrigerator repair service
Pingback: Bewerbung hilfe
Pingback: Click Here
Pingback: professional cleaning services near me
Pingback: fashion News in Urdu
Pingback: maid service Melbourne Fl
Pingback: floating flower heads
Pingback: affordable appliance service
Pingback: floating lotus flowers
Pingback: pool house decor
Pingback: swimming pool wall decor
Pingback: magic mops cleaning
Pingback: microwave oven repair
Pingback: appliance parts direct
Pingback: floating pool decor
Pingback: apliance repair
Pingback: cleaning services Melbourne
Pingback: electric appliances
Pingback: Click Here
Pingback: nails cutter
Pingback: floating paper flowers
Pingback: dog nail clippers
Pingback: Orlando Fl maid service
Pingback: h&b care nail cutter kit
Pingback: Bewerbung hilfe
Pingback: floating flowers set
Pingback: pool wall decor
Pingback: roof shingles
Pingback: nail clipper case
Pingback: swimming pool decorations
Pingback: residential cleaning services near me
Pingback: pool room decor
Pingback: pool party decorations for kids
Pingback: Orlando Fl cleaning service
Pingback: flat roof repair
Pingback: cleaning services Melbourne
Pingback: custom wordpress themes
Pingback: Orlando Fl cleaning service
Pingback: trilastin stretch mark cream
Pingback: roof coatings
Pingback: metal roofing shingles
Pingback: Photo booth wordpress theme
Pingback: cleaning businesses near me
Pingback: burts bees stretch mark cream
Pingback: house cleaning services Melbourne Fl
Pingback: the maids cleaning service
Pingback: cleaning businesses near me
Pingback: premium stretch mark cream
Pingback: cocoa butter stretch mark cream
Pingback: tow truck service provider near midtown
Pingback: the best trucks
Pingback: Car rental website template
Pingback: womens nursing pads
Pingback: nipplecreams cocoa butter
Pingback: reusable nursing pads
Pingback: Speed rope for double unders
Pingback: revlon nail clippers
Pingback: boppy nursing pillow cover
Pingback: datuk seri fd iskandar
Pingback: direct insurance roadside assistance
Pingback: Financial wordpress theme
Pingback: ingrown hair tweezers long
Pingback: Boxing jump rope
Pingback: tweezers ingrown hairtweezers
Pingback: MMA jump rope
Pingback: majestic bombay stainless steel ingrown hair tweezers
Pingback: custom wordpress themes
Pingback: bug repellent lamp
Pingback: Fateh iskandar
Pingback: bug insect repellent
Pingback: Crossfit jump rope
Pingback: Fateh iskandar
Pingback: material de beleza
Pingback: outdoor bug repellent spray
Pingback: thin point tweezers
Pingback: material para maquinario
Pingback: Premium quality jump rope
Pingback: Crossfit jump rope
Pingback: bug repellent stick
Pingback: Speed rope
Pingback: tweezerman tweezer
Pingback: toddler bug repellent
Pingback: tweezer set
Pingback: Speed jump rope by 6MAC
Pingback: material para violino
Pingback: best tweezers
Pingback: Boxing jump rope
Pingback: Buy Marijuana Online
Pingback: extension tweezers
Pingback: eyebrow tweezers for women
Pingback: nyx eyeliner brush
Pingback: eyeliner brush tip
Pingback: cake eyeliner brush
Pingback: japanese eyeliner brush
Pingback: the rabbit vibrator
Pingback: auto tow service
Pingback: reviews
Pingback: buy roadside assistance
Pingback: lift pickup truck
Pingback: company reviews on google
Pingback: wireless earphones
Pingback: reviews website
Pingback: truck wrecker service
Pingback: bluetooth headphones
Pingback: reviews uk
Pingback: penis sleeve extender
Pingback: Women Dress
Pingback: duck scarf vivy yusof
Pingback: Hoodies with custom screen printing
Pingback: how to make money online with no money
Pingback: duck brand
Pingback: Visit Website
Pingback: Visit This Link
Pingback: thrusting vibrator
Pingback: app developer usa cost
Pingback: songket duckscarves
Pingback: Learn More Here
Pingback: Website
Pingback: Website
Pingback: Web Site
Pingback: cyberskin dildo
Pingback: Home Page
Pingback: amazing selling machine review
Pingback: Website
Pingback: Click This Link
Pingback: Read More
Pingback: Web Site
Pingback: Visit Website
Pingback: Web Site
Pingback: Recharge Coupons
Pingback: Wap5.in
Pingback: Learn More
Pingback: Home Page
Pingback: Jio unlimited Internet Tricks
Pingback: Click Here
Pingback: Home Page
Pingback: Visit This Link
Pingback: Click Here
Pingback: Learn More
Pingback: Home Page
Pingback: Read More Here
Pingback: Website
Pingback: Click This Link
Pingback: MT-911.COM/
Pingback: More Information
Pingback: baseball gloves
Pingback: Wilson A2000
Pingback: baseball gloves
Pingback: dato' khor siang gin
Pingback: Massages Limburg
Pingback: contatti peer to peer lending
Pingback: bin rental
Pingback: blog peer to peer lending
Pingback: dryer vent cap
Pingback: adam and eve promo code
Pingback: garbage dumpster
Pingback: dato seri khor teng tong
Pingback: Ero massages
Pingback: khor siang gin
Pingback: khor teng tong
Pingback: rent a dumpster
Pingback: dryer vent lint trap
Pingback: in-europa/
Pingback: investire mintos
Pingback: adam and eve discount
Pingback: waste management roll off dumpsters
Pingback: waste removal
Pingback: dryer vent lint
Pingback: dryer vent fires
Pingback: home dryer vent
Pingback: need a dumpster
Pingback: pizmedia group sac
Pingback: pizmedia group sac
Pingback: Platte daken Superdak
Pingback: gutters sacramento
Pingback: pizmedia group sac
Pingback: ventilation ducting
Pingback: gutter cleaning roseville ca
Pingback: Renoveren dak
Pingback: all star catcher mask
Pingback: Dakwerker Limburg
Pingback: dryer vents cleaning
Pingback: pizmedia group sac
Pingback: pizmedia group sac
Pingback: Superdak overzetdaken
Pingback: Clothes dryer maintenance
Pingback: dryer vent cleaner
Pingback: louisville slugger catcher gear
Pingback: Dakwerker Hasselt
Pingback: gamebag org paradise bay hack paradise bay
Pingback: home air conditioning repairs
Pingback: Dakwerken Heist-op-den-Berg
Pingback: golfclash hackmobile online golf clash
Pingback: how do you clean dryer vent
Pingback: Dakwerken Turnhout
Pingback: bestfifamobile top fifa mobile
Pingback: gas dryer venting
Pingback: www.massagesalon-limburg.be/massages-erotische-massage-limburg/tantra/
Pingback: dryer duct fan
Pingback: dryer vent wall
Pingback: vertical jump workout
Pingback: Dakwerker Mol
Pingback: mobilestrikehacker xyz mobile strike
Pingback: dumpster hire
Pingback: mycafe progenz com my cafe
Pingback: hempire kjhack com hempire
Pingback: Massage met 2 masseuses
Pingback: rekonstrukce bytu
Pingback: free microsoft points
Pingback: presbyt
Pingback: scuola di italiano
Pingback: about presbyterian church
Pingback: binoculars price
Pingback: presbyterian church louisville
Pingback: presby main
Pingback: reviews of italian language schools
Pingback: Drinking glasses
Pingback: italian lessons for beginners
Pingback: waterford wesleyan church
Pingback: free microsoft points
Pingback: how to start a food blog
Pingback: microsoft points code generator
Pingback: striptease-stripster.be/braziliaanse-samba-show-braziliaanse-danseressen/
Pingback: italian lessons for beginners
Pingback: steel lake federal way
Pingback: Beer glasses
Pingback: churches within 50 miles of me
Pingback: italian language class
Pingback: www.striptease-stripster.be/stripacts/#all/1/list
Pingback: repair online reputation
Pingback: free microsoft points codes
Pingback: italian lessons
Pingback: Custom magnets
Pingback: italian teacher
Pingback: web reputation management
Pingback: italian conversation
Pingback: parish church near me
Pingback: baptist church website
Pingback: Lingua italiana imparara
Pingback: why learn italian
Pingback: online business reputation
Pingback: language school
Pingback: Lingua italiana imparara
Pingback: reviews of italian language schools
Pingback: online brand management services
Pingback: flexible duct
Pingback: cleaning gutter
Pingback: italian language lessons pdf
Pingback: Soloya
Pingback: italian language courses online
Pingback: clothes dryer venting options
Pingback: birds in dryer vent
Pingback: linguaincorso.it
Pingback: Flyer printing near me
Pingback: italian conversation
Pingback: Flyer printing near me
Pingback: Affordable Insurance Joilet IL
Pingback: get more netherlands traffic
Pingback: get more fyuse followers
Pingback: Best Insurance Elgin IL
Pingback: Flyer cheap printing near me
Pingback: study in usa powerpoint
Pingback: Best Insurance Aurora IL
Pingback: study journalism usa
Pingback: green card lottery citizenship
Pingback: job in usa for 10th fail
Pingback: green card lottery yahoo
Pingback: usa visa sponsorship
Pingback: usa f-1 visa interview questions
Pingback: Bed bug companies
Pingback: Bed bug companies
Pingback: philippines to usa visa
Pingback: us visa 4 thai
Pingback: Design and develop wordpress website
Pingback: Bed Bug Pest Control
Pingback: Design and develop ecommerce wordpress website
Pingback: Bed Bug Exterminator
Pingback: Bed Bug Pest Control
Pingback: Bed Bug Company
Pingback: cross body bag thick strap
Pingback: women's cross body bag for travelling
Pingback: womens crossbody bag zipper
Pingback: Overkappingen
Pingback: Bed bug companies
Pingback: mini backpack mint green
Pingback: Pergola bouwen
Pingback: SSM Reseller
Pingback: Asset Preservation
Pingback: Hillary Clinton Email Corruption
Pingback: www.terrysacka.com
Pingback: Homepage
Pingback: This is interesting
Pingback: Lachha paratha
Pingback: Read More About Cornerstone
Pingback: Terry Sacka AAMS
Pingback: 2015 prophecies
Pingback: Wealth Transfer
Pingback: Donald Trump Election
Pingback: Tuinen Hendrix tuinontwerpen
Pingback: Latest NBA News
Pingback: Press Release
Pingback: tempered glass film
Pingback: Revitol Stretch Mark
Pingback: norske sex sider
Pingback: About Terry Sacka
Pingback: sexkontakt norge
Pingback: Latest NFL News
Pingback: iphone 10 screen saver
Pingback: phone screen protector
Pingback: www.tuinen-hendrix.be/tuinarchitecten_tuinarchitectuur
Pingback: Aanleggen zwemvijvers
Pingback: iphone 10 gorilla glass
Pingback: iphone 10 gorilla glass
Pingback: sex treff oslo
Pingback: Latest Cycling News
Pingback: Renovatie tuin
Pingback: Latest Baseball News
Pingback: Iphone 10 screen replacement
Pingback: wood floor repair
Pingback: professional teeth whitening kit
Pingback: Iphone 10 tempered glass
Pingback: Iphone glass screen protector
Pingback: hardwood floor new york
Pingback: dumpster rental willowbrook
Pingback: sex nettsider
Pingback: plasic
Pingback: Exclusieve zwembaden
Pingback: Zwembad
Pingback: plasic
Pingback: dumpster rental Plymouth
Pingback: Tempered glass iphone 7
Pingback: residential dumpster
Pingback: phone screen guard
Pingback: Polypropyleen zwembad
Pingback: metal dumpster
Pingback: glass protection film
Pingback: phone screen glass
Pingback: cell phone screen protector
Pingback: Zwembad bouwen
Pingback: iphone 10 glass protector
Pingback: phone screen guard
Pingback: glass screen protector
Pingback: container rental
Pingback: waste services
Pingback: roll off dumpster cost
Pingback: Zwembad in de tuin
Pingback: dumpster rental South Lyon
Pingback: dumpster rental ortonville
Pingback: cheap dumpster rental
Pingback: shopping cart covers for baby
Pingback: disposal bin rental
Pingback: waste container
Pingback: trash dumpsters to rent
Pingback: cost to rent a dumpster
Pingback: trash dumpsters for rent
Pingback: roll off dumpster sizes
Pingback: container dumpster rental
Pingback: garbage dump
Pingback: op?ration hyperm?tropie
Pingback: eveil musical
Pingback: OS X Server Setup
Pingback: eveil musical ecole
Pingback: decouvrir la musique
Pingback: Lars Holm Larsson
Pingback: firmagolf
Pingback: best resveratrol
Pingback: op?ration myopie prix
Pingback: laser ophtalmologie
Pingback: eveil musique
Pingback: how to setup mac mini server for family home
Pingback: City Golf
Pingback: op?ration laser myopie
Pingback: Dak vervangen prijs
Pingback: Dakwerken
Pingback: Andreas Kali
Pingback: eveil musical moyenne section MS
Pingback: operation cataracte
Pingback: clinique des yeux
Pingback: City Golf
Pingback: presbytie
Pingback: eveil musicale
Pingback: op?ration myopie prix
Pingback: op?ration myopie remboursement
Pingback: meilleur clinique laser yeux
Pingback: Wedding Car Hire Sheffield
Pingback: Vernieuwen dak
Pingback: Nicki Hansen
Pingback: op?ration hyperm?tropie
Pingback: Wedding Car Hire Bradford
Pingback: Horizontal Shangri-la Window Blinds Quality Fabric Made to Measure Roller Shade
Pingback: Nieuw dak
Pingback: Dakwerkers Limburg
Pingback: Wedding Car Hire Sheffield
Pingback: Dak renoveren
Pingback: Oil Proof Window Blackout Curtains Customize Size High Quality Easy Installation
Pingback: Carina Vagner
Pingback: Horizontal Shade Zebra Blind Window Roller Custom Cut Size Woodlook Curtain
Pingback: Indoor Golf
Pingback: Wedding Car Hire Sheffield
Pingback: Wedding Car Hire Derby
Pingback: Overzetdaken prijzen
Pingback: Zebra Roller Window Blinds Shade Room Darkening Looped Chain Blind Color
Pingback: Indoor Golf Kokkedal
Pingback: golftræning
Pingback: Wedding Car Hire Bradford
Pingback: Wedding Car Hire Bradford
Pingback: 100% Blackout Roller Blinds In European Design Solid Color Made to Order Blinds
Pingback: djga
Pingback: Wedding Car Hire Derby
Pingback: Wedding Car Hire Leeds
Pingback: Durable Toddler Faucet Extender 4 colors 1pcs Washing Sink Kids Bathroom Tap
Pingback: Lyngbygaard Golf
Pingback: Wedding Car Hire Nottingham
Pingback: Wedding Car Hire Birmingham
Pingback: golf træner
Pingback: Click Here
Pingback: Nicki Hansen
Pingback: Wedding Car Hire Derby
Pingback: Ikast Golf Klub
Pingback: Indoor Golf Kokkedal
Pingback: Wedding Car Hire Sheffield
Pingback: Wedding Car Hire Derby
Pingback: Wedding Car Hire Sheffield
Pingback: Wedding Car Hire Birmingham
Pingback: Click Here
Pingback: iphone glass screen protector
Pingback: Password Generator
Pingback: Warmtepompboiler.net warmtepomp
Pingback: tempered glass
Pingback: Xe chính ch?, SYM Shark, 2014
Pingback: iphone tempered glass
Pingback: iphone tempered glass
Pingback: African latest news
Pingback: phone protection
Pingback: Flat UI Design
Pingback: Free Mobile UI Kit
Pingback: Nigeria politics
Pingback: Ð?t n?n Th?y PhÆ°Æ¡ng, xây d?ng t? do, sang s? ngay
Pingback: Nhà bi?t th?, Royal Park, 112m2,7m m?t ti?n bao s?
Pingback: material design ui kit
Pingback: new phone screen protector
Pingback: food mobile apps design
Pingback: android ui kit psd
Pingback: USA politics newsnow
Pingback: iphone 5 cũ 99% lock hay qu?c
Pingback: Warmtepomp offerte
Pingback: Ði?n tho?i còn m?i chÆ°a bung vít l?n nào.
Pingback: android material design ui kit
Pingback: www.warmtepompboiler.net
Pingback: ransomware
Pingback: phone screen protector
Pingback: Iphone glass screen protector
Pingback: iphone 10 screen saver
Pingback: panic detection mode android
Pingback: instagram updates
Pingback: Zonnepanelen installateur
Pingback: instagram updates
Pingback: tempered glass film
Pingback: Zonnepanelen installaties
Pingback: iphone 7 glass
Pingback: Zonnepanelen kopen
Pingback: Iphone 10 screen protector zeesa
Pingback: iphone 10 screen saver
Pingback: Prijs zonnepanelen
Pingback: healthy powdered drink mix
Pingback: Samsung Galaxy S4 tr?ng
Pingback: baby bandana bibs
Pingback: digestive supplements
Pingback: powdered vitamins
Pingback: tempered glass film
Pingback: Zonnepanelen installateurs Limburg
Pingback: Read More
Pingback: kiddies spa cape town
Pingback: Opbrengst zonnepanelen
Pingback: water drink mixes
Pingback: powdered drink mix packets
Pingback: Frederikssund Golfklub
Pingback: paper cups
Pingback: oppo fi
Pingback: energy supplements
Pingback: Vitamin c powder
Pingback: Powdered drink mix recipes
Pingback: Sky a770 ram 1g
Pingback: Mobile Vetur A9 công ty
Pingback: home decor online
Pingback: yoga gift for women
Pingback: Read More
Pingback: Dell Vostro 3568 core i5 th? h? 7 new 100%
Pingback: dubai lifestyle app
Pingback: Ä?ng h? chính h?ng G shock
Pingback: dubai lifestyle app
Pingback: dubai lifestyle app
Pingback: blue yoga bag
Pingback: Chip cpu e5200
Pingback: dubai lifestyle app
Pingback: micro nhÆ° hình
Pingback: yoga bag with zipper
Pingback: dubai lifestyle app
Pingback: dubai lifestyle app
Pingback: make
Pingback: 2 con chim tr?i tra
Pingback: d? s? d?ng hài hòa phù h?p v?i túi ti?n
Pingback: Xe và d?ng c? trà s?a
Pingback: Music Agency
Pingback: Xà ÄÆ¡n treo tÆ°?ng
Pingback: Ip6 plus gold lên v? 7 plus qu?c t?
Pingback: wealth
Pingback: đi?n tho?i asus. zenphone 2 ram 4g
Pingback: Kauai
Pingback: bathroom hand towel holder
Pingback: people
Pingback: baby bib pattern
Pingback: Jarvis Radio
Pingback: copper bathroom accessories
Pingback: link
Pingback: bathroom accessories prices
Pingback: top charts
Pingback: free internet radio
Pingback: glass storage box
Pingback: dehydrated food storage
Pingback: food containers
Pingback: freeze dried food bulk
Pingback: lingerie store
Pingback: backpack for girls
Pingback: plastic food storage containers
Pingback: best emergency food
Pingback: Giày
Pingback: storage of food
Pingback: water bottle for kids
Pingback: food for survival
Pingback: Icelandic horses
Pingback: Iceland Geysirs
Pingback: yard waste removal
Pingback: 30 yard dumpster
Pingback: revitol stretch mark
Pingback: trash dumpster rental cost
Pingback: Iceland Mountains
Pingback: on site dumpster rental
Pingback: adding machine
Pingback: roll off dumpsters for rent
Pingback: dumpster pickup
Pingback: roll off dumpster rental
Pingback: trash dump
Pingback: dumpster rental Schererville
Pingback: garbage bins for rent
Pingback: dumpster rental san jose
Pingback: construction trash containers
Pingback: MEN'S HOODIES & SWEATSHIRTS
Pingback: demolition dumpster rental
Pingback: MEN'S JEANS & TROUSERS
Pingback: WOMEN'S SKIRTS
Pingback: flat roof solutions
Pingback: teeth whitening
Pingback: commercial roofing contractors
Pingback: roofing material
Pingback: Computer 24x7
Pingback: Computer 24x7
Pingback: Best Deals on Computer Laptops and Desktops
Pingback: Best Deals on Computer Laptops and Desktops
Pingback: Best Deals on Computer Laptops and Desktops
Pingback: clear roof panels
Pingback: Customer Satisfaction Tool
Pingback: Build Surveys Online
Pingback: corrugated roof
Pingback: Build your own surveys
Pingback: rolloff rental
Pingback: dumpster trash
Pingback: dumpster bag
Pingback: mobile app development company india
Pingback: Culver City production company
Pingback: waste removal containers
Pingback: Beverly Hills production company
Pingback: Commercial Solar EPC
Pingback: 20 yard dumpster
Pingback: dumpster rental holly
Pingback: best production companies
Pingback: android app developer
Pingback: app developers india
Pingback: dumpster rental brownstown
Pingback: app development agency
Pingback: Los Angeles production company
Pingback: hire a director
Pingback: Music video production company
Pingback: mobile app development company india
Pingback: video production
Pingback: corporate film production
Pingback: best production companies
Pingback: young film director
Pingback: best film directors
Pingback: Check This Out
Pingback: hire a director
Pingback: Beverly Hills production company
Pingback: independent film company
Pingback: corporate film production
Pingback: los angeles film directors
Pingback: Click Here
Pingback: hire a director
Pingback: House Music
Pingback: Read More
Pingback: best production companies
Pingback: roll off dumpster service
Pingback: dumpster rental near me
Pingback: disposal bin rental
Pingback: marka tescili
Pingback: marka tescili
Pingback: booter.ninja/login.php
Pingback: Cases Accessories
Pingback: Fitness Bands
Pingback: marka tescili
Pingback: nokia cases
Pingback: 30 yard dumpster rental prices
Pingback: AUTOCAD
Pingback: debris removal
Pingback: iPhone 6
Pingback: car holders
Pingback: booter.ninja/terms.php
Pingback: iPhone
Pingback: iPhone for sale
Pingback: lg
Pingback: Mobile Phones Cases
Pingback: iPhone 6
Pingback: les meilleurs 10 hotels à marrakech
Pingback: iphone 6 for sale
Pingback: Accessories Shop
Pingback: tablet cases
Pingback: memory card
Pingback: cables
Pingback: iPhone cases
Pingback: Mobile Phones Cases
Pingback: Mobile Phones Cases
Pingback: mobile cases
Pingback: Life hacks girl
Pingback: Mindfulness and depression
Pingback: DIY enamel pins
Pingback: Being a black writer
Pingback: Rick and Morty accessories
Pingback: Being a writer as a career
Pingback: Life hacks instagram
Pingback: Taxi Service in Taunton
Pingback: Superior Singing Method
Pingback: whisky gifts
Pingback: whisky gifts
Pingback: Taxi Service in Taunton
Pingback: whisky online
Pingback: Self improvement books to read
Pingback: Personal Development
Pingback: Personal Development
Pingback: Read More
Pingback: Read More
Pingback: whiskey
Pingback: Click Here
Pingback: whiskey
Pingback: photography
Pingback: Mindfulness based stress reduction
Pingback: gin
Pingback: whiskey
Pingback: bourbon
Pingback: whisky online
Pingback: Lagavulin 16yrs
Pingback: veneer
Pingback: whisky online
Pingback: dental implant
Pingback: bourbon
Pingback: cheap dumpster rental
Pingback: dumpster rental prices
Pingback: Chape Braspenning: Chape voor Nieuwbouw of Renovatie?
Pingback: best teeth bleaching kit
Pingback: professional teeth whitening kit
Pingback: construction waste bins
Pingback: dumpster home
Pingback: Cups
Pingback: 5 yard dumpster rental
Pingback: trash roll off
Pingback: trash roll off
Pingback: best fast teeth whitening
Pingback: Tool Kits
Pingback: Inflatables
Pingback: teeth whitening kits from the dentist
Pingback: 15 yard dumpster rental cost
Pingback: dumpster truck
Pingback: roll out dumpster
Pingback: dumper rental
Pingback: dumpster rental san jose
Pingback: Watches
Pingback: Funnels
Pingback: Dog Tags
Pingback: youtube mp3 download
Pingback: youtube mp3 download
Pingback: drywall installation
Pingback: kitchen paint
Pingback: drywall contractors denver
Pingback: Lottery Dominator
Pingback: drywallers in my area
Pingback: roof calculator
Pingback: polycarbonate roofing panels
Pingback: Soccer Articles
Pingback: elite painting services
Pingback: FIFA World Cup News
Pingback: vc3266l mini digital multimeter voltmeter ammeter ohm diode voltage tester 200a auto range acdc test clamp meter tester
Pingback: rolex watchband nato strap stainless steel pin buckle belt replacement wrist bracelet
Pingback: clear roofing
Pingback: oakley crosslink temple replacement arm detachable usa
Pingback: 250v 10a digital thermometer thermoregulator for incubator temperature controller 50110 celsius degree thermostat with sensor
Pingback: roofing companies houston
Pingback: Chapewerk
Pingback: metal roofs for homes
Pingback: t60 high fidelity professional 8gb time display recording digital voice audio recorder dictaphone mp3 player
Pingback: 3 in 1 camera straps vintage hippie style canvas shoulder neck durable cotton for nikonpentaxsonycanon dslr camera
Pingback: Vloerisolatie - Kies voor isolerende chape en Bespaar
Pingback: teeth whitening kits that work
Pingback: ski goggles double lens anti fog uv 400 ski glasses men women skiing snowboard skateboard snow goggles ski mask
Pingback: teeth polishing kit
Pingback: best teeth bleaching kit
Pingback: oakley-store
Pingback: Stemless Wine Glasses
Pingback: oakley-prescription-glasses-discount
Pingback: Gloria Kim
Pingback: Pullovers
Pingback: Calculators
Pingback: Glazen deuren prijs
Pingback: crosslink-pitch-54
Pingback: Akoestische vloerisolatie
Pingback: oakley-8027-crosslink
Pingback: oakley-crosslink-lenses
Pingback: 2017 professional front snorkel swimming diving equipment hanging racing snorkel breathing tube set for underwater diving
Pingback: small vibrator
Pingback: Pur isolatie
Pingback: Chape vloerverwarming
Pingback: sex toys for women
Pingback: Embroidery
Pingback: Televisions
Pingback: grosir sepatu roda murah
Pingback: coffeeyam4.suomiblog.com/transportation-3745087
Pingback: hiddenflowerszulu.unblog.fr/2017/08/26/logistics-companies-chattanooga-tn/
Pingback: Glaswanden
Pingback: Stemless Wine Glasses
Pingback: www.pushnovel6.canariblogs.com/warehousing-transportation-packaging-logistics-3837443
Pingback: www.chieftemple2.bravesites.com/entries/general/Freight-Transport-Company
Pingback: Instagram story views
Pingback: www.tomatosmell4.shotblogs.com/freight-broker-agent-3637288
Pingback: Printing Services Near You
Pingback: Printing Cheap Services Near You
Pingback: www.tankfox8.blogzet.com/top-freight-dealer-in-the-united-states-3592305
Pingback: Printing Cheap Services Near You
Pingback: Ramen en deuren Limburg in pvc of aluminium plaatsen? Tripo
Pingback: Gezandstraald glas
Pingback: Cheap Printing Services Near You
Pingback: Spiegels op maat
Pingback: Buy facebook likes
Pingback: basketball layup drills
Pingback: basket drills
Pingback: Commercial Real Estate
Pingback: Glazen leuningen
Pingback: youth basketball drills
Pingback: basketball drills for 5 years olds
Pingback: PVC ramen en deuren
Pingback: 4th grade basketball drills
Pingback: thailand property
Pingback: Jomtien properties
Pingback: firefighters girl friend t shirt
Pingback: my mac is running slow
Pingback: pattaya real estate
Pingback: electric jellyfish ride t shirt
Pingback: bbq gloves heat resistant
Pingback: doc strange t shirt
Pingback: condominium for sale in pattaya
Pingback: clean up mac
Pingback: www.vestdream57.jigsy.com/entries/general/5-Easy-Steps-To-Hire-Your-California-Freight-Dealer
Pingback: silicone heat resistant gloves
Pingback: color tv t shirt
Pingback: bio x4
Pingback: grill mitts
Pingback: SEO Zoekmachine Optimalisatie? Sempris
Pingback: apk versions
Pingback: home page
Pingback: apk versions
Pingback: latest version
Pingback: apps
Pingback: showbox
Pingback: Acheter vin
Pingback: construction dumpster
Pingback: mini massager
Pingback: rent a trash bin
Pingback: home page
Pingback: Learn More Here
Pingback: Brand Awareness
Pingback: Northern Ireland
Pingback: Introduction
Pingback: Clicking Here
Pingback: most powerful vibrator ever
Pingback: construction dumpster rental
Pingback: dumpster rental Georgia
Pingback: Recommended Reading
Pingback: hauling junk
Pingback: gcode
Pingback: Web Site
Pingback: bornreadyentertainment
Pingback: This Site
Pingback: Website
Pingback: Check This Out
Pingback: Read More
Pingback: bornready
Pingback: cost to rent dumpster
Pingback: Click Here
Pingback: dumpster roll off rental
Pingback: physiotherapy
Pingback: junk removal
Pingback: Semi Trucks For Sale
Pingback: 30 cubic yard dumpster
Pingback: Click Here
Pingback: trash dumpster rental
Pingback: Kenworth Trucks For Sale
Pingback: large dumpster
Pingback: international Trucks For Sale
Pingback: concrete disposal
Pingback: monthly dumpster rental
Pingback: laptop repair shop near me
Pingback: construction trash bin rental
Pingback: trash container rental
Pingback: laptop repair shop near me
Pingback: dumpster rental argentine
Pingback: Free FIFA 18 Coins and Points fifa 18 unlimited coins & points generator Fifa Hack.
Pingback: 20 cubic yard dumpster
Pingback: dumpster rental macomb
Pingback: dumpster rental Zilwaukee
Pingback: laptop repair shop near me
Pingback: Read More
Pingback: Freightliner Trucks For Sale
Pingback: international Trucks For Sale
Pingback: waste disposal containers
Pingback: iphone repair screen repair in waterbury
Pingback: Free FIFA 18 Coins and Points fifa 18 unlimited coins & points generator Fifa Hack.
Pingback: roll of dumpster
Pingback: tablet screen repair in Waterbury
Pingback: best vertical workouts
Pingback: Peterbilt Trucks For Sale
Pingback: how to increase vertical at home
Pingback: one day dumpster rental
Pingback: Click Here
Pingback: cost of dumpster
Pingback: waste bin rental
Pingback: computer virus removal service
Pingback: $69.99 any computer repair
Pingback: debris removal
Pingback: roofing detroit
Pingback: leg workouts to dunk
Pingback: Click Here
Pingback: steel roofing shingles
Pingback: roof installation
Pingback: best vertical workouts
Pingback: influencer marketing
Pingback: dirt dumpster rental
Pingback: international Trucks For Sale
Pingback: installing steel roofing
Pingback: share big file
Pingback: cheap roofing
Pingback: how to build a patio roof
Pingback: tips for file gst offiline return
Pingback: is forex trading illegal in india
Pingback: roofing business
Pingback: national roofing contractors association
Pingback: metal roofing portland oregon
Pingback: public pranks
Pingback: chuporn.net
Pingback: denver roofing companies
Pingback: Boardbooster tutorial
Pingback: Join tailwind tribes
Pingback: Pinterest tailwind
Pingback: iphone repair screen repair in waterbury
Pingback: junk be gone
Pingback: 40 yard trash container
Pingback: construction garbage container
Pingback: Orlando Botox
Pingback: Cheap Postcard Bridal Shower Invitations
Pingback: Cheap Postcard Bridal Shower Invitations
Pingback: best demat account in india
Pingback: Cheap Postcard Bridal Shower Invitations
Pingback: what is swing trading stragies
Pingback: Orlando Botox
Pingback: Orlando Botox
Pingback: top free nifty intraday tips
Pingback: tips for choosing best performing mutual fund
Pingback: Cheap Flyers Design And Print
Pingback: Company logo Design
Pingback: top 10 best performing mutual funds in india
Pingback: top 10 best performing mutual funds in india
Pingback: Cheap Flyers Design And Print
Pingback: Cheap Flyers Design And Print
Pingback: Surfer
Pingback: computer virus removal near me
Pingback: Cheap Flyers Design And Print
Pingback: jump rope crossfit
Pingback: what are mutual funds
Pingback: compra de ouro
Pingback: Cheap Flyers Design And Print
Pingback: jump ropes for exercise
Pingback: comprar ouro
Pingback: computer virus removal near me
Pingback: Prijs airco
Pingback: www.rtpcrepair.com
Pingback: Venda de ouro
Pingback: Saigon avenue lan phuong
Pingback: Airco prijs
Pingback: Airconditioning prijs
Pingback: Canvas Painting Giclee Print
Pingback: Airco installatie
Pingback: computer virus removal service
Pingback: Iphone Repair near me
Pingback: computer virus removal near me
Pingback: security camera companies near me
Pingback: Futures Review
Pingback: Shoma Kaikini
Pingback: sap program
Pingback: Love to travel
Pingback: Belmar NJ Pro
Pingback: Kilter
Pingback: Foil boards
Pingback: Fitbit India
Pingback: Ashwini Kaikini
Pingback: SEO Harrisburg
Pingback: PDD
Pingback: Fitbit
Pingback: birthday cakes
Pingback: dog boarding durham nc
Pingback: Rijschool Rotterdam
Pingback: Shoma Kaikini
Pingback: Fitness
Pingback: Reading Pa.
Pingback: Goedkope Rijschool Rotterdam
Pingback: Earth Brilliant
Pingback: Green Cleaning Service
Pingback: commercial cleaning
Pingback: Best Travel Blogs
Pingback: Vegan Christmas Recipes
Pingback: brazil cleaning in Connecticut
Pingback: bitcoin
Pingback: best perfume for women
Pingback: revlon makeup kit
Pingback: best foundation
Pingback: Wedding Entertainment Melbourne
Pingback: Read more
Pingback: best nootropics
Pingback: Wedding Entertainment Melbourne
Pingback: nottropics supplements
Pingback: Wedding Entertainment Melbourne
Pingback: nootropics+
Pingback: nootropics review
Pingback: Soloya lucht/lucht warmtepomp
Pingback: artist
Pingback: nootropics_
Pingback: www.nootropicsreviewsite.com/neuro67-review/
Pingback: best secure cloud storage
Pingback: potomac MD airport taxi cab
Pingback: social media marketing
Pingback: Read More
Pingback: ellicott city md airport taxi cab
Pingback: Designing
Pingback: white oak MD airport taxi cab
Pingback: Bitmex
Pingback: black car service, airport car service
Pingback: fort Washington MD airport taxi cab
Pingback: futures
Pingback: Dulles airport car service
Pingback: laurel md airport taxi cab
Pingback: BWI airport taxi cab
Pingback: Zonneboiler
Pingback: montgomery village MD airport taxi cab
Pingback: Bitmex
Pingback: Warmtepompboilers
Pingback: greenbelt MD airport taxi cab
Pingback: Wheaton md airport taxi cab
Pingback: annapolis MD airport taxi cab
Pingback: apron
Pingback: germantown MD airport taxi cab
Pingback: Reagan airport car service
Pingback: Washington DC limousine
Pingback: college park MD airport taxi cab
Pingback: bethesda MD airport taxi cab
Pingback: BWI airport car service
Pingback: delhi
Pingback: destination wedding photographer
Pingback: wedding photographers packages
Pingback: wedding photography in india
Pingback: candid wedding photography
Pingback: delhi
Pingback: car diffusers
Pingback: ibcbetstep
Pingback: ibcbetstep
Pingback: maxbet888
Pingback: rife machine for cancer
Pingback: airport limo service minneapolis
Pingback: maxbet mobile
Pingback: maxbet mobile
Pingback: illustrator
Pingback: Laptop ext and Tech learning
Pingback: maxbet888
Pingback: gears
Pingback: bridal copper
Pingback: alternative jewelry
Pingback: bronze steampunk
Pingback: jewelry fantasy
Pingback: actu sen
Pingback: car service minneapolis airport
Pingback: Steampunk gift idea for her
Pingback: senego video senegal
Pingback: top 40 chart music
Pingback: home catering services
Pingback: airport car service minneapolis
Pingback: chart music top 40
Pingback: flash actu senegal
Pingback: top 40 charts uk
Pingback: top 50 uk singles
Pingback: actusenegal
Pingback: airport limo service minneapolis
Pingback: Johannesburg wedding
Pingback: Going Here
Pingback: sbo
Pingback: Traditional weddings
Pingback: Wedding Cinematography
Pingback: car service minneapolis airport
Pingback: rife machine
Pingback: Punjabi Wedding Photographer
Pingback: Wedding venues
Pingback: airport car service minneapolis
Pingback: engagement photographer in toronto
Pingback: wedding photographer review
Pingback: top chart 40
Pingback: Punjabi Wedding Video
Pingback: Physician survey
Pingback: wedding photographer
Pingback: Wedding Highlights 2017
Pingback: Wedding Highlights 2017
Pingback: minneapolis corporate transportation service
Pingback: Physician survey
Pingback: engagement photographer in toronto
Pingback: realstate photography
Pingback: Headshots at reasonable rates
Pingback: toronto
Pingback: toronto
Pingback: car service minneapolis airport
Pingback: msp airport car service
Pingback: Non traditional physician jobs
Pingback: Pet seat cover for cars
Pingback: Ryda discount codes
Pingback: Shop New Balance coupon code
Pingback: maxbet mobile
Pingback: Urns
Pingback: iTunes
Pingback: Funky Pigeon coupon codes
Pingback: Jaggad.com deals
Pingback: The Tight Spot coupon
Pingback: Xenia Boutique deals
Pingback: Urn Candles
Pingback: Mixbook discount codes
Pingback: Reiki
Pingback: maxbet888
Pingback: online radio
Pingback: Cremations
Pingback: galaxy cat t-shirt
Pingback: Traditional weddings
Pingback: Potato Parcel coupon codes
Pingback: Zonnepanelen Soloya
Pingback: e-cig
Pingback: SOFTWARE
Pingback: Laptop Repair Pakenham
Pingback: space cat hoodie
Pingback: Eliquid
Pingback: It looks like Apple killed its cheapest laptop for consumers
Pingback: design t-shirts
Pingback: Here what you can do with the crazy new Portrait mode for the iPhone 7 Plus
Pingback: hespress
Pingback: ready
Pingback: SOFTWARE
Pingback: designing
Pingback: Google AI creates its own inhuman encryption
Pingback: gift ideas for her amazon
Pingback: This is the new MacBook Pro with the Magic Toolbar mini display
Pingback: manta de drenagem
Pingback: APPZVENTURE
Pingback: where quality works
Pingback: Europe proposes expanding telco data privacy rules to WhatsApp, Facebook et al
Pingback: Click Here
Pingback: chat 12
Pingback: hosting solutions
Pingback: Cemeteries
Pingback: game development
Pingback: Majestic condominium in Jomtien
Pingback: supernatural
Pingback: PRODUCTS
Pingback: Brad Bass
Pingback: company
Pingback: condo for sales in pattaya
Pingback: pro scooter shop
Pingback: pro scooter
Pingback: custom scooter
Pingback: professional scooters
Pingback: custom scooter
Pingback: scooter store
Pingback: pro scooter
Pingback: scooter brands
Pingback: pro scooter shop
Pingback: pro scooter shop
Pingback: pro scooter shop
Pingback: pro scooter shop
Pingback: ginger juice
Pingback: ginger cocktail syrup
Pingback: organic gingerale
Pingback: traxxas m41 boat
Pingback: carpet upholstery cleaner
Pingback: dumpster rental McDonough
Pingback: ginger dipping sauce
Pingback: business carpet cleaning
Pingback: home treatments for nail fungus
Pingback: disposal bins
Pingback: traxxas dcb m41 catamaran
Pingback: superfast r/c boats
Pingback: zetaclear anti-fungal solution
Pingback: construction debris dumpster
Pingback: organic ginger candy
Pingback: rent dumpster cost
Pingback: how to train to dunk a basketball
Pingback: steam cleaner services
Pingback: on site dumpster rental
Pingback: fingernail fungus treatment
Pingback: 20 yard dumpster cost
Pingback: organic ginger syrup
Pingback: roofing dumpster
Pingback: carpet cleaning vacuum
Pingback: yellow nail syndrome
Pingback: home toenail fungus treatment
Pingback: carbohydrates
Pingback: home foot fungus treatment
Pingback: cost for dumpster rental
Pingback: Eco Slim Gotas
Pingback: Eco Slim Gotas
Pingback: supplements for weight loss
Pingback: supplements alliston
Pingback: Eco Slim Gotas
Pingback: Eco Slim
Pingback: dumpster rental chesterfield
Pingback: traxxas dcb m41
Pingback: zetaclear best over the counter nail fungus treatment
Pingback: creatine kinase
Pingback: ocean r/c boat
Pingback: junk trash removal
Pingback: vip carpet cleaning
Pingback: supplements and what they do
Pingback: carpet cleaners industrial
Pingback: carpet cleaning best
Pingback: leg workouts to dunk
Pingback: drone fireworks
Pingback: yard waste removal
Pingback: cost of dumpster rental
Pingback: home steam cleaning services
Pingback: clean dry carpet cleaning
Pingback: clean the house
Pingback: trash pick up services
Pingback: rolloff dumpster
Pingback: workouts to dunk in 2 weeks
Pingback: buy a drone online
Pingback: buy micro drone
Pingback: i need a dumpster
Pingback: dumpster delivery and pick up
Pingback: quadcopter with camera reviews
Pingback: construction trash bins
Pingback: Idol Lash
Pingback: nano quadcopter
Pingback: where to buy a drone in houston
Pingback: roll off truck
Pingback: drywall repair tools
Pingback: quadcopters with cameras
Pingback: smallest quadcopter
Pingback: Highest paying companies in USA
Pingback: deck paint
Pingback: drones
Pingback: Top 100 highest paying employers in USA (Indexed official data from government)
Pingback: dumpster for sale
Pingback: repaint house
Pingback: drone quadcopter review
Pingback: IT Consulting
Pingback: drywall contractors phoenix
Pingback: IT Consulting
Pingback: top ten sex toys
Pingback: drywall prices near me
Pingback: IT Consulting
Pingback: residential drywall contractors
Pingback: residential drywall repair
Pingback: exercise that helps you jump higher
Pingback: how to dunk a basketball in 2 weeks
Pingback: portland maine
Pingback: eagle elite
Pingback: free drywall contract
Pingback: drywall contractors gta
Pingback: aeropuerto de moscu
Pingback: find a painter decorator
Pingback: maine
Pingback: maine
Pingback: cours de piano pour debutant
Pingback: cat nasal congestion home treatment
Pingback: IT Services
Pingback: silver bullet vibrator
Pingback: book reviews
Pingback: Funerals & Bereavements
Pingback: reviews
Pingback: cours de piano debutant
Pingback: maine
Pingback: cour de solfege debutant
Pingback: piano electrique pour debutant
Pingback: vibe
Pingback: synthetiseur pour debutant
Pingback: payroll company Singapore
Pingback: piano pour apprendre
Pingback: piano apprentissage
Pingback: payroll software singapore
Pingback: lego chima
Pingback: Biometric Singapore
Pingback: quel piano pour debuter
Pingback: methode piano adulte debutant
Pingback: cours de piano pour debutant
Pingback: piano numerique pour debuter
Pingback: Eco Slim Gotas
Pingback: Eco Slim Gotas
Pingback: Eco Slim Gotas
Pingback: rife machine
Pingback: Eco Slim Gotas
Pingback: home remedies for scabies itching
Pingback: pelvic floor physical therapy nj
Pingback: prolapse physical therapy
Pingback: cure all disease
Pingback: lego classic
Pingback: lego city
Pingback: incontinence physical therapy
Pingback: lego angry birds
Pingback: erp singapore
Pingback: Eco Slim Gotas
Pingback: lego house
Pingback: What is erp software
Pingback: lego grand prix
Pingback: erp software system
Pingback: Erp Software in Singapore
Pingback: lego harry potter
Pingback: lego creator
Pingback: mattress disposal
Pingback: erp singapore
Pingback: idatafive
Pingback: lego legoland
Pingback: lego jurassic
Pingback: northern Kentucky
Pingback: Erp accounting software Singapore
Pingback: Enterprise software solutions
Pingback: idatafive
Pingback: Erp Software in Singapore
Pingback: mattress disposal
Pingback: Erp in Singapore
Pingback: lego technic
Pingback: erp software system
Pingback: pelvic physical therapy
Pingback: lego star wars
Pingback: ERP Software Singapore
Pingback: android market google play hack free apps
Pingback: lego spiderman
Pingback: lego videos
Pingback: Hackers
Pingback: Erp accounting software Singapore
Pingback: BABY NURSERY DECOR
Pingback: MONOCHROMATIC NURSERY
Pingback: baby boy nursery
Pingback: erp system software
Pingback: erp software system
Pingback: NURSERY DECOR IDEAS
Pingback: NURSERY MODERN BLACK AND WHITE
Pingback: NURSERY ROOMS
Pingback: profile creation sites list
Pingback: Only the Best for Your Pet
Pingback: best online blog
Pingback: contact us
Pingback: kayseri ceza avukatı
Pingback: Today's Best Deals & Coupons
Pingback: best g spot vibrator
Pingback: hit music
Pingback: kayseri bosanma avukatı
Pingback: web 2.0 sites list
Pingback: find commentluv enabled blogs
Pingback: K-POP
Pingback: deals
Pingback: ùÛéýÒö
Pingback: ÔÔÛ°ãêÑÃ
Pingback: JPNKOR
Pingback: Everything That I love,
Pingback: kayseri avukat
Pingback: magic wand vibrator
Pingback: doggy dan dog training
Pingback: dog trainer online
Pingback: Superdak betonnen dakpannen
Pingback: dog problems biting
Pingback: Boston Party Bus
Pingback: Overzetdaken Superdak
Pingback: bullet vibrator
Pingback: onlinedogtrainer
Pingback: doggy dan complaints
Pingback: how to train a puppy to walk on a leash
Pingback: Stoughton Massachusetts Party Bus Limo
Pingback: doggie dan
Pingback: Providence Limo
Pingback: operational excellence courses
Pingback: dove cresswells dog training review
Pingback: labrador puppies
Pingback: best g spot vibrator
Pingback: customer service training courses
Pingback: english labrador retriever
Pingback: 5 golden rules to becoming pack leader
Pingback: project management training in dubai
Pingback: risk management course dubai
Pingback: supply chain courses in dubai
Pingback: leadership training in dubai
Pingback: graphgame
Pingback: g gasm delight incognito
Pingback: dumpster rental new baltimore
Pingback: kayseri miras avukatı
Pingback: Superdak dak renoveren
Pingback: dumpster pricing
Pingback: New tub
Pingback: Minneapolis Walk-in tubs
Pingback: Bath Remodel
Pingback: trash bin rental
Pingback: CAPS certified handyman
Pingback: MQL4 Programmer
Pingback: Wheel-in showers
Pingback: rent dumpster
Pingback: trash roll off
Pingback: Best Forex Brokers
Pingback: Directorio Forex
Pingback: Tub liner
Pingback: rent a garbage dumpster
Pingback: rent a garbage container
Pingback: Walk in bathtub Installer Minneapolis
Pingback: Top 10 Forex Expert Advisors
Pingback: Walk in tub Installation Minneapolis
Pingback: Minneapolis Contractor
Pingback: Minneapolis Contractor
Pingback: rollaway dumpster rental
Pingback: Superdak dakpannen vervangen
Pingback: HandyPro Handyman
Pingback: waste management bins
Pingback: roll off trash containers
Pingback: Forex Trading Bonus
Pingback: digital marketing IL
Pingback: waste management bins
Pingback: digital marketing IL
Pingback: electric skateboards
Pingback: dumpster rental Dunwoody
Pingback: Click Here
Pingback: dumpster rental Lithonia
Pingback: Forex Trading Platforms
Pingback: jet surfboards
Pingback: Aging in Place handyman
Pingback: Read More
Pingback: Walk in tub Installation Minneapolis
Pingback: Shower liner
Pingback: Walk in bathtub
Pingback: social media marketing service
Pingback: Shower liner
Pingback: Bath Remodeling
Pingback: What are the best political forums?
Pingback: AKC French bulldogs for sale
Pingback: create website in Nigeria
Pingback: Freebird is a free speech political forum
Pingback: Go Here
Pingback: political debate forums
Pingback: Read More
Pingback: garbage containers
Pingback: rent a garbage dumpster
Pingback: waste dumpster
Pingback: Click Here
Pingback: Forex Trading Seminars
Pingback: Freebird is a free speech political forum
Pingback: 15 yard dumpster rental
Pingback: waste containers for rent
Pingback: rolling dumpster
Pingback: pink vibrator
Pingback: roll off waste containers
Pingback: political forums
Pingback: 30 cubic yard dumpster
Pingback: glory days of /pol
Pingback: 10 yard dumpster dimensions
Pingback: dumpster rental company
Pingback: waste removal bins
Pingback: politics forum
Pingback: Forex Market Signals
Pingback: Forex Trading Webinars
Pingback: Forex Contests
Pingback: how much does it cost to rent a dumpster
Pingback: Forex Trendline Trading
Pingback: Forex Trading Tips
Pingback: Forex Trading Basics
Pingback: politics forums
Pingback: dumpster rental Gallatin
Pingback: waste bin rental
Pingback: political debate forum
Pingback: Pip Calculator
Pingback: Margin Calculator
Pingback: garbage dumpster sizes
Pingback: garbage dumpster rental prices
Pingback: A Vitathatatlan 4
Pingback: dumpster manufacturers
Pingback: A Vitathatatlan 4
Pingback: glory days of /pol
Pingback: dumpster rental milwaukee
Pingback: garbage dumper
Pingback: Forex Strategies
Pingback: online mozifilmek
Pingback: residential waste removal
Pingback: Forex Training Videos
Pingback: roll on roll off containers
Pingback: political board
Pingback: CFD Brokers
Pingback: CFD Trading
Pingback: political discussion forum
Pingback: garbage dump
Pingback: smallest dumpster size
Pingback: I Love You, Daddy teljes film
Pingback: dumpster rental business
Pingback: Forex Trading Glossary
Pingback: commercial trash removal
Pingback: Bitcoin Glossary
Pingback: Justice League teljes film
Pingback: garbage recycling
Pingback: I Love You, Daddy teljes film
Pingback: Stock Trading
Pingback: politics forum
Pingback: dumpster dimensions
Pingback: successful immigrants
Pingback: worldwide breaking news
Pingback: political boards
Pingback: political discussion forum
Pingback: junk hauling
Pingback: snow removal
Pingback: Binary Options Signals
Pingback: garbage containers rental
Pingback: Binary Options Trading Webinars
Pingback: Binary Options Trading Software
Pingback: chess rules
Pingback: dumpster rates
Pingback: Managed Binary Options Accounts
Pingback: landscape design
Pingback: trash dumpster service
Pingback: roll away dumpster rental
Pingback: waste disposal containers
Pingback: Binary Options Books
Pingback: Binary Options Expert Advisors
Pingback: portable dumpster rental
Pingback: dumpsters San Diego
Pingback: controlled house
Pingback: Weekly Market Analysis
Pingback: trash bin
Pingback: Binary Options Strategies
Pingback: landscape omaha
Pingback: Hvad er scrum
Pingback: 3 yard dumpster
Pingback: Binary Options Articles
Pingback: Social Trading
Pingback: trash hauling
Pingback: cek ip saya
Pingback: Binary Options News
Pingback: cek site header
Pingback: garbage disposal bins
Pingback: Android App Developers
Pingback: ip saya
Pingback: best vibrating penis ring
Pingback: Mobile App Development Company
Pingback: dirt dumpster
Pingback: App Development
Pingback: App Development
Pingback: trash pick up services
Pingback: Mobile App Development Company
Pingback: App Development
Pingback: iOS App Development
Pingback: snow removal
Pingback: Android App Developers
Pingback: App Development
Pingback: App Development
Pingback: iOS App Development
Pingback: Application Development
Pingback: Bigg Boss
Pingback: landscape omaha
Pingback: how penis ring works
Pingback: politics forums
Pingback: cheap hotels in nyc
Pingback: Colors Tv Serials Online
Pingback: Mobile App Development Companies
Pingback: Mobile App Development Company
Pingback: Preise Umzugsofferte Uster
Pingback: landscape omaha
Pingback: Mobile App Development Company
Pingback: More Information
Pingback: Top App Development
Pingback: iOS App Development
Pingback: Top App Development
Pingback: App Development
Pingback: Application Development
Pingback: how to increase penis size
Pingback: Clogged dryer vent
Pingback: celtic earrings for women 14K Gold
Pingback: Irving Dryer repair serviceDryer Vent Wizard
Pingback: vent for dryer
Pingback: dryer vent covers
Pingback: viagens internacionais
Pingback: cancun
Pingback: dryer vent t
Pingback: glory days of /pol
Pingback: the best dryer vent
Pingback: dumpster rental white lake
Pingback: dumpster rental new haven
Pingback: exterior dryer vent
Pingback: clothes dryer vent hose
Pingback: inline dryer vent filter
Pingback: dryer outside vent
Pingback: lakedumpster rental
Pingback: dryer vent system
Pingback: preço baixo
Pingback: Geekz Twitter Profile
Pingback: bfi dumpster rental
Pingback: 14K Gold fine jewelry
Pingback: junk removal service
Pingback: Geekz Google+ Page
Pingback: rent a garbage dumpster
Pingback: Geekz-A technology blog
Pingback: dump rental
Pingback: cultural wear
Pingback: His Secret Obsession
Pingback: FitBit Ionic review
Pingback: bfi dumpster
Pingback: Geekz content submission
Pingback: washer machine repair
Pingback: Marketing danbury ct
Pingback: Seo agency Connecticut
Pingback: Digital marketing agency danbury
Pingback: Two ducks digital marketing
Pingback: Digital marketing agency ct
Pingback: refrigerator problems
Pingback: gold plated fashion earrings
Pingback: wash machine repair
Pingback: ice machine repair
Pingback: Seo Connecticut
Pingback: gold womens earings
Pingback: Search engine optimization danbury ct
Pingback: political discussion forum
Pingback: appliance dealers
Pingback: Freebird is a free speech political forum
Pingback: gclub
Pingback: refrigerator repair nyc
Pingback: no vent dryer
Pingback: politics forum
Pingback: appliance cleaning service
Pingback: lg appliance service
Pingback: fast appliance service
Pingback: gifts ideas
Pingback: beauty
Pingback: gifts from amazon
Pingback: political forum
Pingback: dryer vent clamps
Pingback: cleaning lint from dryer
Pingback: rectangular duct
Pingback: tech startup management
Pingback: domain name extensions
Pingback: tech startup newsletter
Pingback: how to register a right domain name
Pingback: tech startup financing
Pingback: Tech Startup Webinars
Pingback: must have wordpress plugins
Pingback: one travel
Pingback: politics forum
Pingback: freebird political forum
Pingback: tech startup healthcare
Pingback: clothes dryer lint trap
Pingback: dryer vent periscope
Pingback: Local SEO in Daytona Beach, FL
Pingback: dryer vent connector
Pingback: www.bonneterre-wessanen.com
Pingback: Local SEO in Port Orange, FL
Pingback: stove repair
Pingback: custom wordpress design
Pingback: maytag appliance repair
Pingback: Tech Startup Conference
Pingback: political discussion forum
Pingback: Rose Gold Toothbrush Elite Oval Make up Brushes Set - 10 Piece
Pingback: window dryer vent
Pingback: dual HD capture and quad SD video capture
Pingback: Social Media Marketing
Pingback: live video capture of lectures
Pingback: appliance repair questions
Pingback: Freebird is a free speech political forum
Pingback: Kat Von D Shade + Light Refillable Face Contour Palette
Pingback: the appliance doctor
Pingback: Mac Eyeliner Kohl (Smolder)
Pingback: passagens com preços mais em conta
Pingback: Kylie Jenner KOKO Kollection
Pingback: game console capture
Pingback: 4 channel 2K capture card
Pingback: What are the best political forums?
Pingback: Email Marketing in Port Orange, FL
Pingback: appliance repair training online
Pingback: dumpster rental Greenview
Pingback: Dumpster rental Imperial Beach
Pingback: Tarte Cosmetics - Tartelette Tease Clay Palette
Pingback: viagens
Pingback: Local SEO in Daytona Beach, FL
Pingback: Social Media Marketing in Ormond Beach, FL
Pingback: dumpster prices
Pingback: roll off
Pingback: advanced appliance service
Pingback: local dumpster rental
Pingback: Unicorn Brush Brush Set - 10 Piece
Pingback: i need a dumpster rental
Pingback: video capture 4K HDMI games consoles in real time
Pingback: metropolitan appliance service
Pingback: Pay Per Click Management PPC in Ormond Beach, FL
Pingback: webdesign
Pingback: kayseri avukat
Pingback: website gestalten
Pingback: viagens e turismo
Pingback: webdesign cms
Pingback: capture 4096x2160 HDMI
Pingback: passagens com preços mais em conta
Pingback: affordable dumpster rental
Pingback: Social Media Marketing in Ormond Beach, FL
Pingback: trabalhar com turismo
Pingback: kayseri bosanma avukati
Pingback: dumpsters rental prices
Pingback: Android App Developers
Pingback: construction trash bin rental
Pingback: capture VGA + audio
Pingback: rubbish removal
Pingback: Huda Beauty - Lip Contour Kit
Pingback: one channel UHD capture card
Pingback: waste dumpster prices
Pingback: construction dumpster rental prices
Pingback: HUDA BEAUTY - Textured Shadows Palette - Desert Dusk Edition
Pingback: tech startup hr
Pingback: startup course online
Pingback: kayseri ceza avukati
Pingback: tech startup management
Pingback: USB Capture HDMI Gen 2 Dongle: USB Capture HDMI Gen 2 Dongle
Pingback: dumpster prices
Pingback: More Information
Pingback: Read More
Pingback: live video capture of distance learning
Pingback: trash removal
Pingback: More Information
Pingback: mining
Pingback: Mobile App Development Companies
Pingback: iOS App Development
Pingback: Top App Development
Pingback: dumpster rental Upper Arlington
Pingback: Top App Development
Pingback: 5 yard dumpster rental
Pingback: ćwiczenia na biceps
Pingback: kayseri avukat
Pingback: Application Development
Pingback: 2 yard dumpster
Pingback: ćwiczenia na biceps
Pingback: rent a trash dumpster
Pingback: aprender english
Pingback: iOS App Development
Pingback: kayseri arabulucu
Pingback: iOS App Development
Pingback: construction containers for rent
Pingback: aprende ingles online
Pingback: como aprender ingles
Pingback: estudiar ingles
Pingback: dumster
Pingback: curso ingles ninos
Pingback: aprenda ingles
Pingback: aprender idiomas
Pingback: tam
Pingback: Read More
Pingback: bfi dumpster
Pingback: same day dumpster
Pingback: Australian Web Development Company
Pingback: Mobile App Development Company
Pingback: roaring springs
Pingback: Top App Development
Pingback: lg varmepumpe
Pingback: varmepumper
Pingback: Search Engine Optimization
Pingback: rotating vibrater
Pingback: Woocommerce Developers Sydney
Pingback: More Information
Pingback: varmepumpeoversikt
Pingback: Search Engine Optimization in Ormond Beach, FL
Pingback: varmepumpeoversikt.no
Pingback: kayseri miras avukati
Pingback: samsung varmepumpe
Pingback: Search Engine Optimization
Pingback: cursos aprender ingles
Pingback: WordPress Developers Sydney
Pingback: a&e magic massager
Pingback: aprender ingles gratis
Pingback: Australian Web Development Company
Pingback: Local Search Engine Optimization in Ormond Beach, FL
Pingback: B-School
Pingback: passagens aéreas baratas
Pingback: Local Search Engine Optimization in Daytona Beach, FL
Pingback: Australian Web Development Company
Pingback: Cheap Flights
Pingback: E-commerce Development Sydney
Pingback: domain name picks
Pingback: women's athleisure
Pingback: aprender ingles gratis
Pingback: cursos para aprender ingles
Pingback: free web hosting
Pingback: curso ingles gratuito
Pingback: pesquise preços
Pingback: Social Media Marketing in Port Orange, FL
Pingback: affordable drones
Pingback: camera quadcopters for sale online
Pingback: male enhancement
Pingback: extenze fast acting
Pingback: enlargement pills
Pingback: Cheap Flight deals
Pingback: buy camera quadcopters online
Pingback: viajar
Pingback: Web Design in Daytona Beach, FL
Pingback: ñåðèàë
Pingback: male enhancement pills that work
Pingback: enhancement pills
Pingback: extenze male enhancement pills reviews
Pingback: dick growth pills
Pingback: enhanced male
Pingback: herbal male enhancement
Pingback: Social Media Marketing in Port Orange, FL
Pingback: made in usa athleisure
Pingback: yoga fashion brand
Pingback: extenze pills
Pingback: all natural male enhancement
Pingback: online quadcopters
Pingback: fitness trainer Walnut Creek
Pingback: Pay Per Click Management PPC in Daytona Beach, FL
Pingback: Local SEO in Ormond Beach, FL
Pingback: Cheap Flights
Pingback: Email Marketing in Daytona Beach, FL
Pingback: sliquid h20
Pingback: shop online yoga activewear
Pingback: activewear
Pingback: Cheap Flights
Pingback: dieta na odchudzanie
Pingback: suction cup massage
Pingback: varmepumpeoversikt
Pingback: varmepumper
Pingback: mitsubishi varmepumpe
Pingback: shop online layogic
Pingback: Vintage Style Casual Shirt
Pingback: Double Cereal Dispenser
Pingback: Yoga Luxury Athleisure Activewear Fashion Brand
Pingback: Afghanistan
Pingback: Women Flat Comfortable Scandals
Pingback: Christmas Tree Dinnerware Ceramic Dishes
Pingback: 6 Pcs Christmas Cutlery bags
Pingback: Earrings Ethnic Black Enameling Gold Silver Color
Pingback: White Pearl Long Pendant Necklace For Women
Pingback: employee engagement
Pingback: benefits of aloe vera
Pingback: how to use ginger
Pingback: Health blog
Pingback: coconut oil
Pingback: Cagney Global Logistics
Pingback: livre personnalisable enfant
Pingback: livre personnalise prenom
Pingback: livre personnalisable
Pingback: coconut tree
Pingback: Rodney raanan Yelp
Pingback: mosaic tile border
Pingback: livre personnalise prenom
Pingback: pomegranate fruit benefits
Pingback: copra. Desiccated coconut.
Pingback: Rodney raanan Yelp
Pingback: livre personnalise petite fille
Pingback: perfume
Pingback: Rodney raanan
Pingback: histoire personnalisee enfant
Pingback: copra. Desiccated coconut.
Pingback: livre avec prenom personnalise
Pingback: Rodney raanan Facebook
Pingback: livre personnalise garcon
Pingback: livre personnalise
Pingback: cinnamon powder
Pingback: stress relieving activity
Pingback: athleisure wear
Pingback: Rodney raanan Yelp
Pingback: fast weight loss
Pingback: letter board and chalkboard combo
Pingback: made in usa activewear
Pingback: who invented the piano
Pingback: Rodney raanan Facebook
Pingback: Rodney raanan Yelp
Pingback: Best sunglasses store
Pingback: How to Use Rabbit Vibrator
Pingback: Ayurveda medicine for diabetes
Pingback: power of the mind
Pingback: learn to play violin online
Pingback: Ayurveda tablets
Pingback: $5 sunglasses
Pingback: shop online layogic
Pingback: Where to buy clout goggles
Pingback: bright Instagram feed accessory
Pingback: Ayurveda medicine for cancer
Pingback: 5 dollar sunglasses
Pingback: 5 dollar sunglasses
Pingback: Rodney raanan Facebook
Pingback: Spuitkurk Unicorks
Pingback: How to Make Your Penis Bigger
Pingback: turkey hair transplant reviews
Pingback: Rodney raanan Facebook
Pingback: cours de piano debutant
Pingback: Couvreur du patrimoine bâti
Pingback: cour de solfege debutant
Pingback: Tourneur céramique
Pingback: apprendre le piano sur internet
Pingback: Rodney raanan Facebook
Pingback: Musique gitane
Pingback: Jazz
Pingback: Rodney raanan
Pingback: Rodney raanan Yelp
Pingback: Rodney raanan Yelp
Pingback: stroker
Pingback: cours de synthetiseur pour debutant
Pingback: bon synthetiseur pour debutant
Pingback: laid-back
Pingback: Cornier
Pingback: refrigerator repair Seattle yelp
Pingback: frigidaire refrigerator repair Seattle
Pingback: Fabricant de luminaires
Pingback: rocknroll
Pingback: samsung refrigerator repair Seattle
Pingback: dryer repair in Seattle area
Pingback: emerald city appliance repair
Pingback: small appliance repair Seattle WA
Pingback: Rodney raanan Facebook
Pingback: appliance repair south Seattle
Pingback: AR-670-1 compliant uniform boots
Pingback: Rodney raanan Yelp
Pingback: Gevelbekleding offerte
Pingback: Rodney raanan Yelp
Pingback: Rodney raanan
Pingback: read about
Pingback: Kurk gevelwerken
Pingback: ranger school
Pingback: appliance repair in LA
Pingback: Rodney raanan
Pingback: Rodney raanan Yelp
Pingback: Bekleding gevel
Pingback: Rodney raanan Yelp
Pingback: Rodney raanan
Pingback: wine refrigerator repair Seattle
Pingback: Rodney raanan Yelp
Pingback: 24 hr appliance repair Seattle
Pingback: Gevelrenovatie
Pingback: refrigerator repair Seattle
Pingback: Gevelbepleistering
Pingback: Read More Here
Pingback: Schilderwerken
Pingback: earthite
Pingback: Go Here
Pingback: Find Out More
Pingback: g spot stimulator
Pingback: Read This
Pingback: Clicking Here
Pingback: Learn More
Pingback: presentasi iklan
Pingback: Go Here
Pingback: Rodney raanan
Pingback: Read More Here
Pingback: Learn More Here
Pingback: presentasi power point
Pingback: Read This
Pingback: Read This
Pingback: Rodney raanan Facebook
Pingback: Rodney raanan Facebook
Pingback: Discover More
Pingback: Rodney raanan Facebook
Pingback: Clicking Here
Pingback: Rodney raanan Facebook
Pingback: Rodney raanan Yelp
Pingback: Rodney raanan Yelp
Pingback: tube ace porn plugin
Pingback: Find Out More
Pingback: Learn More
Pingback: Read More
Pingback: presentasi bisnis komunikasi bisnis
Pingback: coconut oil
Pingback: rampant rabbit
Pingback: Perehara festivals
Pingback: beginner violin lessons learn how to play violin
Pingback: Northwest Florida wedding photographer
Pingback: Destin Wedding photographer
Pingback: Northwest Florida wedding photographer
Pingback: Pensacola Beach photographer
Pingback: Safe and proven natural cure for diabetes
Pingback: Wedding photographer in Destin
Pingback: Romanian Escorts
Pingback: Best Romanian Escorts
Pingback: Female Escorts in Romania
Pingback: Escorts Romania
Pingback: dxf file for laser engraving
Pingback: Escorts Romania
Pingback: cad files
Pingback: dxf file for water-jet cutting
Pingback: Escorts Romania
Pingback: methode piano facile
Pingback: cours piano internet
Pingback: 3d plans
Pingback: apprendre piano debutant
Pingback: initiation au piano
Pingback: amazon daily deals
Pingback: 3d plans
Pingback: apprentissage de piano
Pingback: dental oral surgery
Pingback: dental practice management
Pingback: Lawyers Kerr and Thomas
Pingback: methode de solfege
Pingback: apprendre piano en ligne
Pingback: piano pour adulte debutant
Pingback: dental practice for sale
Pingback: cool birthday party places
Pingback: piano electrique debutant
Pingback: green color contact lenses
Pingback: Dryer vent
Pingback: Bayswater
Pingback: dryer vent cleaning
Pingback: Vermont
Pingback: apprendre le piano pour debutant
Pingback: How to clean a dryer vent
Pingback: dental practice marketing
Pingback: Vermont
Pingback: dental practice regulations
Pingback: local oral surgeons
Pingback: sky zone birthday packages
Pingback: air vent for dryer
Pingback: dental marketing strategies
Pingback: vent air systems
Pingback: Health Insurance Malaysia
Pingback: Read More
Pingback: vent vent
Pingback: dryer vent size
Pingback: affordable dental implants
Pingback: dental practice regulations
Pingback: jump birthday party
Pingback: Allianz Singapore
Pingback: dental marketing strategies
Pingback: jump zone party
Pingback: tips for private dentist
Pingback: Real Estate
Pingback: vent vent
Pingback: Real Estate
Pingback: dental practice management
Pingback: Electric dryer
Pingback: all on 4 dental implants cost
Pingback: dental oral surgery
Pingback: pump sex toy
Pingback: trash removal
Pingback: Longer drying cycles
Pingback: dumpster rental Chula Vista
Pingback: dental marketing strategies
Pingback: dryer vent clean
Pingback: rent dumpster
Pingback: how to clean dryer vents
Pingback: Dumpster Rent Pro of San Diego
Pingback: dumpster
Pingback: Dumpster rental price San Diego
Pingback: dumpster rental San Diego
Pingback: tips for private dentist
Pingback: Wholesaling Real Estate
Pingback: how to clean out dryer vent
Pingback: affordable dental implants
Pingback: Flatbush Dryer Vent Cleaning Wizard
Pingback: what is dryer vent cleaning
Pingback: garbage pickup
Pingback: Dryer Vent Pro in Flatbush
Pingback: commercial dumpster rental
Pingback: rent a dumpster prices
Pingback: local oral surgeons
Pingback: associate dentist jobs
Pingback: dumpster container rental
Pingback: dental marketing strategies
Pingback: Dryer lint
Pingback: periodontist near me
Pingback: How to clean a dryer vent
Pingback: Air flow in clothes dryer
Pingback: affordable dumpster rental
Pingback: dumpster bin
Pingback: waste containers for rent
Pingback: Wholesaling Real Estate
Pingback: dental practice management
Pingback: yard debris removal
Pingback: dumpster trash
Pingback: container rental
Pingback: adam and eve rabbit
Pingback: lint dryer brush
Pingback: hvac duct installation
Pingback: dental practice for sale
Pingback: roof dryer vent
Pingback: dumpster trash
Pingback: dental practice marketing
Pingback: all on 4 dental implants cost
Pingback: how do you clean the dryer vent
Pingback: Tom Krol Coaching
Pingback: what is a dryer vent
Pingback: window dryer vent
Pingback: dryer booster fan
Pingback: dental practice regulations
Pingback: livre a personnaliser avec photo
Pingback: dryer lint remover
Pingback: Longer drying cycles
Pingback: Investor Grit Coaching
Pingback: histoire personnalisee enfant
Pingback: Slim Couture
Pingback: livre personnalise enfant
Pingback: livre enfant avec son prenom
Pingback: dryer venting solutions
Pingback: hvac duct installation
Pingback: telescoping dryer vent
Pingback: Wordpress Tutorials
Pingback: how to clean out a dryer vent
Pingback: livre avec prenom personnalise
Pingback: livre personnalise noel
Pingback: dental practice for sale
Pingback: 1 clean air
Pingback: Wordpress Snippets
Pingback: air conditioning offers
Pingback: dryer vent problems
Pingback: livre personnalise fille
Pingback: livre personnalise petit garcon
Pingback: livre avec prenom enfant
Pingback: vent installation
Pingback: Wordpress Tips
Pingback: dryer booster fan
Pingback: associate dentist jobs
Pingback: stimulate the brain
Pingback: How to Wholesale Real Estate
Pingback: livre personnalise noel
Pingback: livre enfant avec son prenom
Pingback: livre personnalise garcon
Pingback: livre personnalisable
Pingback: livre personnalise garcon
Pingback: dryer vent fires statistics
Pingback: livre personnalise
Pingback: jokes
Pingback: histoire personnalisee enfant
Pingback: comedy video
Pingback: appliance repair
Pingback: advogados trabalhistas
Pingback: Real Estate
Pingback: venting clothes dryer
Pingback: Investor Grit
Pingback: Dryer installation
Pingback: appliance repair shops
Pingback: Dryer installation
Pingback: funny ghost videos
Pingback: vine
Pingback: appliance parts and repair
Pingback: Dryer vent clog
Pingback: direito do trabalho
Pingback: cheap color copies prints
Pingback: cheap color copies print
Pingback: cheap color copies prints
Pingback: refrigerator repair cost
Pingback: headaches
Pingback: Dryer fires
Pingback: Dryer vent clog
Pingback: color copies print
Pingback: How to get free sponsorship earn lots of money from any social account
Pingback: how do you clean dryer vent
Pingback: dacor repair
Pingback: hair dryer brush
Pingback: Neuro67
Pingback: cheapest color copies
Pingback: HRMS
Pingback: Reduces operational risk
Pingback: dryer vent cleaning reviews
Pingback: appliances service repair
Pingback: headaches
Pingback: cleaning dryer lint
Pingback: Prevail K9
Pingback: best nail fungus treatment reviews
Pingback: twin cities appliance service
Pingback: coconut oil for nail fungus
Pingback: stress
Pingback: New Home Grant
Pingback: Wholesaling Real Estate
Pingback: listerine for nail fungus
Pingback: brain power
Pingback: New Home
Pingback: Queensland New Home Affordabilty Program
Pingback: teatree oil for nail fungus
Pingback: teatree oil for nail fungus
Pingback: headaches
Pingback: FIrst Home
Pingback: listerine for nail fungus
Pingback: stimulate the brain
Pingback: Click Here
Pingback: Real Estate Wholesaling
Pingback: Great Start Grant
Pingback: ko-recover-kare/
Pingback: FIrst Home
Pingback: Queensland New Home Affordabilty Program
Pingback: Lowongan Terbaru
Pingback: Top 5 weird woman's in the world
Pingback: No Deposit Finance
Pingback: More Information
Pingback: kpop birthdays
Pingback: mywira
Pingback: More Information
Pingback: Harga Terbaru
Pingback: Real Easy Homes
Pingback: New Home
Pingback: megabytestreaming
Pingback: Jobs in Singapore
Pingback: Real Easy Homes
Pingback: No Deposit Finance
Pingback: New Home Grant
Pingback: No Deposit Finance
Pingback: singacareers
Pingback: kodi iptv
Pingback: bitcoin value today
Pingback: Kpop profiles
Pingback: bitcoin video
Pingback: Maintains accurate financial estimates
Pingback: Inventory Control integrated
Pingback: tv online
Pingback: kpop members
Pingback: zebpay bitcoin rate
Pingback: free bitcoin xapo
Pingback: bitcoin vs litecoin
Pingback: bitcoin price chart
Pingback: Cyber Crime
Pingback: make money online doing tasks
Pingback: FCPX Plugins
Pingback: bitcoin radio
Pingback: Sobha International City
Pingback: kpop lightsticks
Pingback: bitcoin wallet setup
Pingback: Criando um canal do zero
Pingback: Blog gratuito
Pingback: make money online gta 5 xbox one
Pingback: Motion 5 Effects
Pingback: make money online system review
Pingback: FCPX Plugins
Pingback: Teacher Vlog
Pingback: men's shorts
Pingback: intelligence
Pingback: Irvine Eye Doctor
Pingback: bamboo sunglasses
Pingback: men's elegant watches
Pingback: dlf magnolias gurgaon
Pingback: men's bracelets
Pingback: high school teacher blogs
Pingback: knitwear for men
Pingback: men's elegant watches
Pingback: Math blogs for teachers
Pingback: educational videos
Pingback: Anaheim Dental
Pingback: Teacher blog
Pingback: Teacher Vlog
Pingback: online men fashion
Pingback: men's elegant watches
Pingback: Teacher websites
Pingback: techrevel,smartphone.mobile review
Pingback: buy men's clothes
Pingback: winter ankle boots
Pingback: leather sandals
Pingback: Sobha International City
Pingback: vehicle crime
Pingback: best teacher blogs
Pingback: Nakakihara
Pingback: Teacher Vlog
Pingback: Nakakihara
Pingback: high school teacher blogs
Pingback: diplom
Pingback: Supply Chain Management
Pingback: Digital Marketing
Pingback: ERP
Pingback: Financial Accounting System
Pingback: ERP
Pingback: 411 your local
Pingback: sign in gmail
Pingback: gmail sign up
Pingback: gmail sign in
Pingback: gmail.com signup
Pingback: gmail signup tips
Pingback: gmail login
Pingback: gmail create username
Pingback: gmail password recovery
Pingback: gmail login tips
Pingback: how to login gmail
Pingback: Love our Wine
Pingback: Nakakihara
Pingback: headphones under 500
Pingback: eromassages Gent
Pingback: Home healthcare in Lahore, Pakistan
Pingback: erotische massages Antwerpen
Pingback: baseball caps men
Pingback: best drone under 150
Pingback: Usi Tech Coin
Pingback: Nursing Care in Home in Pakistan
Pingback: ero massages Leuven
Pingback: best cameras under 200 dollars
Pingback: eromassage Hasselt
Pingback: Usi-tech Sign Up
Pingback: emergency medical service lahore
Pingback: emergency medical service lahore
Pingback: ricoh theta s
Pingback: Usitech
Pingback: migliori visori vr economici
Pingback: samsung gear 360
Pingback: playstation vr
Pingback: app per unire foto
Pingback: outdoor drone with camera
Pingback: article rewrite
Pingback: Healthcare at home in Lahore, Pakistan
Pingback: Personal Injury
Pingback: migliori schede sd
Pingback: realtà virtuale
Pingback: Inland Empire Personal Injury Attorney
Pingback: pornbitter.com
Pingback: Usi-tech Register
Pingback: RVT
Pingback: Bicycle Accidents
Pingback: Los Angeles Personal Injury Attorney
Pingback: More Information
Pingback: Sexual Harassment
Pingback: Ambulance service lahore pakistan
Pingback: Read More
Pingback: Electronics
Pingback: Brain Injury and Catastrophic Injuries
Pingback: Bicycle Accidents
Pingback: Personal Injury
Pingback: Checkpoints
Pingback: Coinbase
Pingback: best video quadcopter
Pingback: More Information
Pingback: Brain Injury and Catastrophic Injuries
Pingback: Brain Injury and Catastrophic Injuries
Pingback: EarnHoney
Pingback: Elder home in Pakistan
Pingback: Riverside Personal Injury Attorney
Pingback: Bitconnect
Pingback: San Bernardino Personal Injury Attorney
Pingback: Free html form builder
Pingback: Precious metals companies
Pingback: Bicycle Accidents
Pingback: Ontario California Personal Injury Attorney
Pingback: Construction Litigation
Pingback: Click Here
Pingback: Bicycle Accidents
Pingback: ambulance service Pakistan
Pingback: More Information
Pingback: San Bernardino Personal Injury Attorney
Pingback: Auto Accidents
Pingback: Los Angeles Personal Injury Attorney
Pingback: Bicycle Accidents
Pingback: Wrongful Death
Pingback: Bicycle Accidents
Pingback: Emergency ambulance lahore pakistan
Pingback: Massage 97222
Pingback: accountants in birmingham
Pingback: Portland Massage
Pingback: black israelites
Pingback: Happy Valley Massage
Pingback: bookkeeping services birmingham
Pingback: hijama birmingham
Pingback: unlimited lifestyle
Pingback: Oregon City Massage
Pingback: hijama birmingham
Pingback: Massage 97086
Pingback: urban christian clothing
Pingback: urban christian clothing websites
Pingback: helix light url
Pingback: helix light bitcoin tumbler
Pingback: helix light grams
Pingback: christian motivational speakers
Pingback: flyer design singapore
Pingback: official helix light
Pingback: bitcoin mixer
Pingback: urban christian clothing
Pingback: hebrew israelites
Pingback: urban christian clothing
Pingback: aceite de argan
Pingback: protein powder benefits
Pingback: natural cures for high cholesterol
Pingback: make money with no money
Pingback: earn extra money
Pingback: dumpster rental romulus
Pingback: dumpster rental Shelby Twp
Pingback: make money fast and easy
Pingback: tips to lower cholesterol
Pingback: soothers
Pingback: roll off container
Pingback: online surveys for cash
Pingback: exercise
Pingback: cholesterol levels
Pingback: severe lower back pain treatment
Pingback: dumpster rental marlette
Pingback: Pet Care Supplies
Pingback: 2 yard dumpster
Pingback: dumpster rental linden
Pingback: storage Winnipeg
Pingback: rolloff dumpsters
Pingback: i want to make money
Pingback: trash container rentals
Pingback: earn quick cash
Pingback: order a dumpster
Pingback: how to work from home
Pingback: office setup
Pingback: dumpster disposal
Pingback: cholesterol ratio
Pingback: dumpster sizes
Pingback: black dating hotline
Pingback: meet south african friends
Pingback: get a dumpster
Pingback: garbage rental
Pingback: whey protein isolate benefits
Pingback: dumpsters to rent
Pingback: meet africa's youngest billionaire
Pingback: black dating hub
Pingback: dumpster bag
Pingback: drones
Pingback: dumster
Pingback: dating black man
Pingback: african dating black
Pingback: dumpster rental atlanta
Pingback: lacna reklama
Pingback: how to lower triglycerides
Pingback: roll off waste containers
Pingback: waste dumpster sizes
Pingback: african dating website
Pingback: dumpster waste management
Pingback: site de rencontre femme africaine en france
Pingback: repair pendulum clock movement
Pingback: Broadway Brokerage Inc
Pingback: orris entertainland
Pingback: dumpster rental Kenesaw
Pingback: roll off dumpster prices
Pingback: Clock Repair West Bloomfield
Pingback: dumpster removal
Pingback: trash hauling
Pingback: a magia da gratidao
Pingback: french carriage clock repair
Pingback: upcoming commercial projects in gurgaon
Pingback: french carriage clock repair
Pingback: Joel Conway
Pingback: pendulum repair
Pingback: small dumpsters for rent
Pingback: commercial projects in gurgaon
Pingback: Clock Repair West Bloomfield
Pingback: herschede clock reapir
Pingback: elan mercado
Pingback: grandfather clock repair
Pingback: 400 day clock repair
Pingback: beneficios da gratidao
Pingback: dumpster waste management
Pingback: 1800junk
Pingback: gratidao na bíblia
Pingback: modern clock repair
Pingback: bulk trash
Pingback: local clock repair
Pingback: bulk trash
Pingback: rolloff service
Pingback: large dumpsters for rent
Pingback: atmos clock repair manual
Pingback: Clock Repair Madison Heights
Pingback: Clock Repair Pontiac
Pingback: digital agency brisbane
Pingback: roll off dumpster waste management
Pingback: marketing strategy
Pingback: marketing strategy
Pingback: online marketing brisbane
Pingback: condicionado brasilia
Pingback: under the bed restraint gear
Pingback: Wealth Transfer
Pingback: Latest Mental Health News
Pingback: medical-hotspot.com
Pingback: Terry Sacka AAMS
Pingback: Terry Sacka AAMS
Pingback: Latest Child health News
Pingback: the silver bullet sex toy
Pingback: instagram post scheduler
Pingback: Latest Allergy and Asthma News
Pingback: Sabbatical Year Sheviit
Pingback: Wealth Transfer
Pingback: instagram post scheduling software
Pingback: GLD ETF
Pingback: instagram post scheduling
Pingback: healthmate
Pingback: gram poster
Pingback: massage stimulato
Pingback: Read More
Pingback: More Information
Pingback: Latest Cancer News
Pingback: More Information
Pingback: best rated vibrator for women
Pingback: Latest Diabetes News
Pingback: tens device
Pingback: tens electrodes
Pingback: muscle stimulator
Pingback: tens for pain
Pingback: massage stimulato
Pingback: Read More
Pingback: prostate massager
Pingback: muscle stimulator
Pingback: tens nerve stimulator
Pingback: healthmateforever
Pingback: instagrampostscheduling
Pingback: NAPSR Review
Pingback: how does a penis ring work
Pingback: gramposter
Pingback: tens for pain
Pingback: muscle stimulator
Pingback: how to schedule instagram posts
Pingback: canyouscheduleinstagramposts
Pingback: canyouscheduleinstagramposts
Pingback: instagram poster
Pingback: free vpn
Pingback: nyjer seed for wild birds
Pingback: CNPR
Pingback: instagramposter
Pingback: instagram post scheduling tool
Pingback: instagrampostscheduling
Pingback: apple cider vinegar for cats
Pingback: free vpn
Pingback: Souq
Pingback: Kuwait
Pingback: Souq
Pingback: Saudi Arabia
Pingback: seresto dog collar reviews
Pingback: Namshi
Pingback: Black Friday
Pingback: cat litter for odour control
Pingback: NAPSR
Pingback: Jumia
Pingback: Kuwait
Pingback: bird care
Pingback: CNPR
Pingback: horse care tips
Pingback: CNPR Review
Pingback: apple cider vinegar for kittens
Pingback: cat care tips
Pingback: Sexy Lingerie
Pingback: capture dual channel 3G-SDI
Pingback: one channel UHD capture card
Pingback: CNPR Review
Pingback: H1B salary records - Highest Paying Employers
Pingback: H1B data info
Pingback: gary sasser wife
Pingback: H1B Salary Data - Linkedin Salary
Pingback: H1B Salary Data - Netflix Salary
Pingback: CNPR Training
Pingback: pool fencing sydney
Pingback: Pool fencing companies
Pingback: pool fencing toorak
Pingback: glass pool fencing
Pingback: pool fence guide
Pingback: Pharmaceutical Sales Training
Pingback: ons
Pingback: kapesníÄky do saka
Pingback: science rats
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: LGBT
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: castle bounce house
Pingback: masaje
Pingback: minnie mouse bounce house
Pingback: waterslides
Pingback: inflatable movie screen
Pingback: Armenia news in English
Pingback: Mongolia news in English
Pingback: Libya news in English
Pingback: Papua New Guinea news in English
Pingback: Iraq news in English
Pingback: Peru news in English
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: muslim sex
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: Accra Travel
Pingback: inflatable movie screen
Pingback: Accra Travel
Pingback: waterslides
Pingback: bets10 giriş
Pingback: Accra Travel
Pingback: Click This Link
Pingback: g spot vibrator
Pingback: Discover More Here
Pingback: superbetin güncel giriÅ
Pingback: Read More Here
Pingback: hiperbet güncel giriÅ
Pingback: Casinomilyon giriş
Pingback: Home Page
Pingback: Visit Website
Pingback: Learn More
Pingback: Click This Link
Pingback: Click This Link
Pingback: Click This Link
Pingback: Read More Here
Pingback: Disruptive
Pingback: Human hair extensions
Pingback: youwin
Pingback: doc johnson b7
Pingback: Senior Programme Leader of the International Energy Agency
Pingback: Wedding makeup Toronto
Pingback: Supertotobet güncel giriÅ
Pingback: Clicking Here
Pingback: casinodunya giriş
Pingback: Read More Here
Pingback: Makeup and hair Toronto
Pingback: Read This
Pingback: casinodunya bahis
Pingback: Read More Here
Pingback: Bridal hair and makeup
Pingback: Clip in hair canada
Pingback: betboo giriş
Pingback: vectorize an image
Pingback: mybahis online bahis sitesi giriş
Pingback: Makeup and hair Toronto
Pingback: DudeComedy
Pingback: 72 round folding table
Pingback: teacher chair
Pingback: betpluton bahis
Pingback: superbahis giriş
Pingback: Baby bottle brush
Pingback: Pull Up Stand
Pingback: piabet
Pingback: Pull Up Banner
Pingback: půjÄovna dodávek praha
Pingback: Jennifer Thomas Rockford IL
Pingback: justintbet
Pingback: kids chairs for school
Pingback: green chair
Pingback: Mildred Metal Table Lamp Set of 2
Pingback: Gavivi Metal Table Lamp Set of 2
Pingback: good laptop for music production
Pingback: best laptop for producing music
Pingback: hiperbet canlı bahis
Pingback: best laptop for making music
Pingback: best laptops for music production
Pingback: best laptop for producing music
Pingback: best laptop for music production
Pingback: best laptop for making music
Pingback: best laptop for music production and recording
Pingback: best laptops for producing music
Pingback: best laptop for producing music
Pingback: sekabet bahis
Pingback: restaurantes fuengirola recomendados
Pingback: tempobet canlı bahis
Pingback: best laptop for music
Pingback: Pull Up Banner Stand
Pingback: T-type Ca++ CP α1H Polyclonal Antibody
Pingback: NKp30 Polyclonal Antibody
Pingback: SR-3A Polyclonal Antibody
Pingback: 2 week diet plan
Pingback: Neurotensin Polyclonal Antibody
Pingback: AAT Polyclonal Antibody
Pingback: C/EBP ε (phospho Thr74) Polyclonal Antibody
Pingback: it support
Pingback: Joogastuudio Tallinnas
Pingback: realistic dildo
Pingback: IP3R-I Polyclonal Antibody
Pingback: Joogastuudio Tallinnas
Pingback: electronics
Pingback: drones
Pingback: WISP-3 Polyclonal Antibody
Pingback: cameras
Pingback: MDM2 (Phospho-Tyr394) Antibody
Pingback: kids toys deals
Pingback: Human Neuroblastoma suppressor of tumorigenicity 1 (NBL1) ELISA Kit
Pingback: baju kurung online
Pingback: www.joogastuudio.ee/uuemad/hommiku-voi-ohtu-nimesed/
Pingback: www.bbq.co.il
Pingback: Read More
Pingback: www.joogastuudio.ee/elustiil/jooga-jennifer-aniston-sisemine-rahu/
Pingback: Travel blog
Pingback: columbia
Pingback: Gyms in Des Moines
Pingback: best lingerie
Pingback: bitcoin iraa
Pingback: Proform 505 CST Treadmill
Pingback: tech influencer
Pingback: Cardio Machines
Pingback: tested and safe
Pingback: kickboxing
Pingback: free forex ebook
Pingback: spread trading
Pingback: trading for beginners
Pingback: original magic wand attachments
Pingback: mixed martial arts
Pingback: Craps
Pingback: grosbet giriş
Pingback: baju kurung cotton
Pingback: baju kurung
Pingback: craps table
Pingback: rocks-off jira massager
Pingback: baju kurung 2017
Pingback: www.sachayacu.org
Pingback: kickboxing
Pingback: mma
Pingback: Forex
Pingback: gpunltd.com
Pingback: vibrating dick ring
Pingback: urban christian clothing websites
Pingback: remove complaints board
Pingback: Remove Complaints
Pingback: black israelites
Pingback: urban christian clothing
Pingback: click here for free download
Pingback: BEST PLACE TO BUY GENERIC VIAGRA
Pingback: BUY CHEAP XANAX
Pingback: unlimited lifestyle
Pingback: adventure lifestyle
Pingback: small hand massager
Pingback: urban christian clothing websites
Pingback: triple stimulation dildo
Pingback: download now
Pingback: TRAMADOL PAIN RELIEF
Pingback: christian hipsters
Pingback: Where can i Buy Cheap Xanax
Pingback: black outdoors
Pingback: Where can i Buy Cheap Xanax
Pingback: Where can i Buy Cheap Xanax
Pingback: gpunltd.com
Pingback: christian clothes
Pingback: x wordpress theme free
Pingback: cool christian clothing
Pingback: mini vibrator sex toy
Pingback: christian hip hop
Pingback: download now
Pingback: Where can i Buy Cheap Xanax
Pingback: mastubation toys for men
Pingback: unlimited lifestyle
Pingback: download app from here
Pingback: Where can i Buy Cheap Xanax
Pingback: Where can i Buy Cheap Xanax
Pingback: remove consumer complaints
Pingback: go to official site
Pingback: black israelites
Pingback: Remove Online Complaints
Pingback: christian hip hop
Pingback: download now
Pingback: download app from here
Pingback: hırdavat
Pingback: APK
Pingback: deals
Pingback: jump rope
Pingback: nipple play
Pingback: download now
Pingback: jump ropes crossfit
Pingback: remove consumer complaints
Pingback: click here for free download
Pingback: download app from here
Pingback: apps like tinder
Pingback: APK
Pingback: download now
Pingback: adam and eve vibrators
Pingback: clitoris massager
Pingback: ?????????? BOOKING
Pingback: best online trading platform
Pingback: invest online low brokerage
Pingback: Kinderhilfe Bayern
Pingback: trading online
Pingback: Kids No Drugs
Pingback: highest rated vibrator
Pingback: Kinderhilfe Bayern
Pingback: Kinderhilfe
Pingback: KidsNoDrugs
Pingback: Online trading platform
Pingback: trading online platform low brokerage
Pingback: Valentus
Pingback: how to use a dong
Pingback: Learn Piano from Home
Pingback: Learn Music from Home
Pingback: Learn Piano from Home
Pingback: Learn Music Online
Pingback: valentus
Pingback: Learn Piano
Pingback: maintain brest shape after marriage
Pingback: click for source
Pingback: Our site
Pingback: Learn Piano for All
Pingback: more
Pingback: digital marketing agency birmingham
Pingback: More Help
Pingback: Continue Reading
Pingback: web design manchester
Pingback: helpful hints
Pingback: online bookkeeping
Pingback: bookkeeping software
Pingback: designer perfume oil
Pingback: click for source
Pingback: payroll services birmingham
Pingback: aga engineer perth
Pingback: more helpful hints
Pingback: Clive Income Tax Services
Pingback: Melksham
Pingback: More about the author
Pingback: tax withholding calculator 2016
Pingback: blockchain
Pingback: how to file taxes online
Pingback: shiblan clean
Pingback: shiblan-clean.com
Pingback: tax consultant
Pingback: dumpster rental Newark
Pingback: dumpster dimensions
Pingback: money management
Pingback: půjÄovna lodí Suice
Pingback: dumpster rental Gahana
Pingback: shiblan-clean
Pingback: shiblan-clean
Pingback: SHIBLAN-CLEAN.COM
Pingback: SHIBLAN-CLEAN.COM
Pingback: dumpster container
Pingback: shiblan-clean
Pingback: dumpster rental near me
Pingback: Pune airport to shirdi cab
Pingback: SHIBLAN-CLEAN.COM
Pingback: oil drops
Pingback: oil drops
Pingback: social security tax
Pingback: tax audit
Pingback: quickbooks pro
Pingback: elixinol
Pingback: bfi dumpster rental prices
Pingback: dumpster dimensions
Pingback: roll off container manufacturers
Pingback: garbage bins rental
Pingback: shiblan-clean.com
Pingback: dumster
Pingback: privacy policy
Pingback: Click Here
Pingback: dumpster rental Collierville
Pingback: home
Pingback: medihemp
Pingback: dumpster rental
Pingback: local dumpster rental
Pingback: dump containers for rent
Pingback: Sillas De Oficina
Pingback: 16 foot trailer for sale used
Pingback: Sillas De Oficina
Pingback: construction debris containers
Pingback: 6 yard dumpster rental
Pingback: 6 by 12 trailer for sale
Pingback: dumpster roll off rental
Pingback: Muebles Para Oficina
Pingback: rent a roll off
Pingback: Muebles De Oficina
Pingback: Read More
Pingback: Escritorios de Oficina
Pingback: dump container rental
Pingback: 4 ton dump trailer
Pingback: trash pickup
Pingback: dumpster
Pingback: dumpster rental st charles
Pingback: automobile trailers for sale
Pingback: atv hauling trailers for sale
Pingback: dumpster
Pingback: Click Here
Pingback: best small utility trailer
Pingback: box trailer prices
Pingback: Escritorios de Oficina
Pingback: dumpster sizes
Pingback: atv dump trailer for sale
Pingback: build enclosed utility trailer
Pingback: autotrader trailers
Pingback: Escritorios de Oficina
Pingback: dumpster rental norridge
Pingback: dumpster rental st charles
Pingback: appliance repair Blairstown
Pingback: appliance repair certification
Pingback: garbage dumpster rental prices
Pingback: lg appliances repair
Pingback: dumpster rental service
Pingback: Mobiliario Oficina
Pingback: dumpsters near me
Pingback: Mobiliario Para Oficina
Pingback: rent trash container
Pingback: Mobiliario Oficina
Pingback: Muebles Para Oficina
Pingback: construction roll off dumpsters
Pingback: Escritorios de Oficina
Pingback: roll off trailer
Pingback: Thermal Binocular
Pingback: roll of dumpster rental
Pingback: price of dumpster
Pingback: appliance parts and repair
Pingback: cost of a dumpster rental
Pingback: appliance repair refrigerator
Pingback: SHIBLAN-CLEAN.COM
Pingback: rotating anal vibrator
Pingback: shiblan clean
Pingback: kris kellar
Pingback: all appliances
Pingback: Coldwell banker
Pingback: mls
Pingback: construction loan los Angeles
Pingback: house
Pingback: investment property loans los Angeles
Pingback: Bir Billing Paragliding
Pingback: shiblan-clean
Pingback: SHIBLAN-CLEAN.COM
Pingback: fm7
Pingback: clothes washer
Pingback: SHIBLAN-CLEAN.COM
Pingback: Paragliding adventure
Pingback: appliance service station seattle
Pingback: Silent Paint Remover Rental Home Depot
Pingback: Whitefield Pellet Stove
Pingback: Breckwell P2700 Pellet Stove
Pingback: P35i Pellet Insert
Pingback: rechargeable g spot vibrator
Pingback: weight loss
Pingback: commercial real estate loan
Pingback: 247Th District Court
Pingback: nhim kieng gia re
Pingback: Denby Imperial Blue Discontinued
Pingback: Trueman Welters Powersports
Pingback: Bnmbargains
Pingback: Pellet Stove Whitfield
Pingback: Chair Clips
Pingback: Burr King Model 760
Pingback: Golden Malrin Raccoon Recipe
Pingback: Spenard Builders Supply Hours
Pingback: Car Scratch Repair Melbourne
Pingback: buy garden storage
Pingback: fm7 credits
Pingback: g spot vibrator review
Pingback: pornonaft.net
Pingback: consultwebs seo
Pingback: valentus sample
Pingback: aluminum trailer wheels
Pingback: Thrift Store POS software
Pingback: marketing web
Pingback: Diseño Grafico Zipaquira
Pingback: marketing web
Pingback: Paginas Web chia
Pingback: marketing web
Pingback: Realtor
Pingback: Clit Sensitizer
Pingback: comment appeler senegal
Pingback: credit repair
Pingback: senegal pourcentage musulmans
Pingback: quelle temperature au senegal en fevrier
Pingback: house
Pingback: Devices
Pingback: wholesale
Pingback: Professional photo editing
Pingback: qu'est ce que le pouvoir legislatif au senegal
Pingback: Home
Pingback: land
Pingback: Realtor
Pingback: food
Pingback: unboxing haul
Pingback: house
Pingback: search
Pingback: kris kellar
Pingback: Harry Potter books
Pingback: parker co realtor
Pingback: Corset Dress
Pingback: Background removal
Pingback: Potterheads
Pingback: senegal sans visa
Pingback: Corset Dress
Pingback: senegal sanex
Pingback: Corset Dress
Pingback: Harry Potter books
Pingback: senegal autoroute
Pingback: senegal et tourisme
Pingback: romantic couple games to play
Pingback: Corset Dress
Pingback: Harry Potter
Pingback: Real estate
Pingback: senegal emergent
Pingback: Realtor
Pingback: land
Pingback: Coldwell banker
Pingback: senegal en janvier
Pingback: refinancing
Pingback: Corset Dresses
Pingback: senegal ouganda direct
Pingback: Real estate
Pingback: senegal capitale
Pingback: kris kellar
Pingback: livre personnalise enfant
Pingback: Harry Potter Quiz
Pingback: adam and eve sex toy shop
Pingback: livre avec prenom personnalise
Pingback: Harry Potter facts
Pingback: livre personnalisable enfant
Pingback: infosenegal
Pingback: www actu net sn
Pingback: livre personnalise pas cher
Pingback: Facelift Newport Beach
Pingback: Realtor
Pingback: senegal nigeria 2002
Pingback: Coldwell banker
Pingback: senegal kolda
Pingback: livre personnalise prenom
Pingback: timewise
Pingback: perfume
Pingback: parker co realtor
Pingback: waterproof bunny vibrator
Pingback: refinancing
Pingback: mary kay perfume buy fragrances
Pingback: how to use a vibrator
Pingback: mary kay satin hands
Pingback: parker co realtor
Pingback: Morocco Insurance for Travel
Pingback: parker co realtor
Pingback: Attic Insulation by LABS - Attic and Crawlspace Solutions
Pingback: property
Pingback: Attic Insulation Los Angeles
Pingback: kris kellar
Pingback: Attic Cleaning - Attic Insulation by LABS
Pingback: Ferry to Ceuta
Pingback: Attic Insulation by LABS - Attic and Crawlspace Solutions
Pingback: Scientific Instruments Manufacturers
Pingback: sexy slave kit
Pingback: magento integration
Pingback: big commerce integrations
Pingback: ecommerce integrations
Pingback: big commerce integrations
Pingback: giant dildo
Pingback: Background removal
Pingback: Crossfit
Pingback: Cycle Lock
Pingback: Leggings
Pingback: Hiking Boot
Pingback: Url Shortener
Pingback: special surveillance group
Pingback: lashes
Pingback: branding
Pingback: Leggings
Pingback: kolkata escort
Pingback: Leggings
Pingback: hydration bag
Pingback: hydration bag
Pingback: kolkata escorts
Pingback: Leggings
Pingback: Crossfit
Pingback: newyork
Pingback: Crossfit
Pingback: cute bags
Pingback: hunting tee shirt
Pingback: Leggings
Pingback: Hatha Yoga
Pingback: hydration bag
Pingback: fitness
Pingback: hydration bag
Pingback: Cycling
Pingback: Crossfit
Pingback: Hiking Boot
Pingback: coffee mug with photo online
Pingback: Cycle Lock
Pingback: Hatha Yoga
Pingback: kik sexting
Pingback: kik usernames
Pingback: sexting forum
Pingback: gif
Pingback: images
Pingback: funny
Pingback: hydration bag
Pingback: Leggings
Pingback: fitness
Pingback: Photo coffee mug template
Pingback: not safe
Pingback: trending
Pingback: photo lens coffee mug
Pingback: Souq uae
Pingback: White Friday
Pingback: Souq egypt
Pingback: son dog tag
Pingback: Souq ksa
Pingback: Souq ksa
Pingback: Souq egypt
Pingback: son dog tags
Pingback: son dog tag pendants
Pingback: Black Friday
Pingback: luna balls
Pingback: off road gear
Pingback: toys for girls
Pingback: motocross helmet for kids
Pingback: where to donate car
Pingback: vehicle donation
Pingback: rent a dumper
Pingback: 1moto
Pingback: rent a roll off
Pingback: donate my car
Pingback: roll off trash dumpster
Pingback: uflixit.com
Pingback: best charities to donate a car
Pingback: donation truck
Pingback: tax deduction for donating a car
Pingback: watch online trending list
Pingback: donate car tax write off
Pingback: dumpster rental minneapolis
Pingback: donate a vehicle to charity
Pingback: uflixit.com/solarmovie-free-online
Pingback: waste management dumpster bag
Pingback: pbs donate car
Pingback: watch free online
Pingback: dumpster delivery
Pingback: where to donate my car
Pingback: disposal services
Pingback: uflixit.com/gostream-is
Pingback: dumpster rental for concrete
Pingback: legitimate car donation charities
Pingback: uflixit.com/xmovies8-free-movies
Pingback: rent a dumpster cost
Pingback: sex leash
Pingback: tax credit for donating car
Pingback: rent roll off dumpster
Pingback: green waste dumpster
Pingback: dumpster rental nj
Pingback: car donation tax deduction 2014
Pingback: trash pick up services
Pingback: My current location
Pingback: roll off container service
Pingback: creepypasta stories
Pingback: container trash rental
Pingback: creepypasta cz
Pingback: garbage pickup
Pingback: the rake creepypasta
Pingback: 10 yard dumpster prices
Pingback: dumpster rental grosse pointe
Pingback: roll off container prices
Pingback: dumpster rental Xenia
Pingback: dumpsters to rent
Pingback: dumpster rental near me
Pingback: hotel deals
Pingback: creepypastapunch
Pingback: haul trash
Pingback: small dumpster rental prices
Pingback: roofing dumpster
Pingback: large trash removal
Pingback: creepypasta wiki
Pingback: FIFA lucky patcher
Pingback: rent garbage dumpster
Pingback: Lucky patcher
Pingback: rent trash bins
Pingback: candy crush lucky patcher
Pingback: rent a garbage bin
Pingback: Lucky Patch
Pingback: creepypasta names
Pingback: Lucky Patch
Pingback: candy crush lucky patcher
Pingback: concrete dumpster rental
Pingback: top 10 creepypasta
Pingback: dumpster rental toronto
Pingback: yard debris removal
Pingback: roofing dumpster rental
Pingback: roll off dumpster prices
Pingback: FIFA lucky patcher
Pingback: roll off
Pingback: 10 yard roll off
Pingback: 3 yard dumpster
Pingback: roll of dumpster
Pingback: waste management bin rental
Pingback: dumpster rental norridge
Pingback: waste management 10 yard dumpster
Pingback: rent garbage dumpster
Pingback: dumpster rental Merrionette Park
Pingback: roll off container rental
Pingback: dumpster rental DePaul
Pingback: dumpster rental DePaul
Pingback: digital marketing danbury
Pingback: small dumpster rental prices
Pingback: trash removal
Pingback: Click Here
Pingback: Interview
Pingback: Interview
Pingback: roll off
Pingback: Direct Cellars
Pingback: dumpster container
Pingback: 3 yard dumpster rental
Pingback: donate the car
Pingback: truck donation
Pingback: getting a donated car
Pingback: automobile donations to charity
Pingback: Digital Marketing Services
Pingback: 30 yard roll off dumpster
Pingback: charities that accept cars
Pingback: RFID wallets for men
Pingback: skanner för film
Pingback: short creepypasta
Pingback: best cruise lines
Pingback: lg hom bot robot vacuum cleaner
Pingback: artificial intelligence stocks
Pingback: træfældning
Pingback: Pop Up Stand
Pingback: where to donate old cars
Pingback: donate my old car
Pingback: agency
Pingback: tax write off car donation
Pingback: star wars
Pingback: Gold Dealers
Pingback: Precious metals services
Pingback: data manager
Pingback: value of donated car
Pingback: how to donate car to goodwill
Pingback: artificial intelligence programming
Pingback: how much tax deduction for car donation
Pingback: e-globaltravel.gr/athina-xenodoxeia-kratiseis-booking/
Pingback: hamstring injury
Pingback: ACL tear
Pingback: Click Here
Pingback: charity auto donation
Pingback: javstreaming.mobi
Pingback: buzz grub.com
Pingback: external aquarium filters
Pingback: achilles tendinitis
Pingback: fort collins painting contractor
Pingback: Read More
Pingback: kayseri boşanma avukatı
Pingback: overgrip
Pingback: spinal stenosis
Pingback: filter for aquarium
Pingback: aquarium filters for sale
Pingback: best filter for fish aquarium
Pingback: fort collins painting contractor
Pingback: best fish tank filter
Pingback: best fish tank filters
Pingback: Bracelets Fashion
Pingback: best insoles for ball of foot pain
Pingback: choosing an aquarium filters
Pingback: best aquarium filter
Pingback: how to choose aquarium filters
Pingback: aquarium filter for sale
Pingback: gallon fish tank filters
Pingback: the best fish tank filters
Pingback: how to choose aquarium filter
Pingback: gallon aquarium filter
Pingback: aquarium filter for sale
Pingback: best filter for fish tank
Pingback: hang on back filters
Pingback: Parenting Skills
Pingback: kayseri ceza avukatı
Pingback: Parenting Styles
Pingback: Parenting Advice
Pingback: blockchain
Pingback: Mona Fowler
Pingback: Danny Willis
Pingback: Thuy Wiseley
Pingback: Beatriz Vandeusen
Pingback: kayseri avukat
Pingback: Shemika Lipsett
Pingback: Becki Hammers
Pingback: Gregoria Rosner
Pingback: Elmira Alcantara
Pingback: Mona Fowler
Pingback: Michael Agee
Pingback: Renovation Singapore
Pingback: Renovation Singapore
Pingback: Renovation Singapore
Pingback: Renovation Singapore
Pingback: Renovation Singapore
Pingback: demolition contractor singapore
Pingback: interior design singapore
Pingback: driving lessons campbelltown
Pingback: interior design singapore
Pingback: Renovation Singapore
Pingback: Nichiyu Forklift Singapore
Pingback: driving lessons campbelltown
Pingback: onroad driving school
Pingback: Rivercove Residences
Pingback: northwave ec
Pingback: Movie Posters for sale
Pingback: Rivercove Residences
Pingback: Science Fiction: Rogue One
Pingback: ec singapore
Pingback: ec singapore
Pingback: ec singapore
Pingback: comprar bitcoins en mexico
Pingback: kayseri arabulucu
Pingback: Science Fiction: Revenge of the Sith
Pingback: ec singapore
Pingback: ec singapore
Pingback: ec singapore
Pingback: Explainer Video Singapore
Pingback: Science Fiction
Pingback: Forex signals
Pingback: Revenge of the Sith Movie Poster shop
Pingback: Return of the Jedi Movie Poster shop
Pingback: A New Hope Film Posters
Pingback: Trading Signals
Pingback: Cleaning Services Singapore
Pingback: bitcoin mexico
Pingback: Forexsignal
Pingback: Forexsignal
Pingback: The Empire Strikes Back Movie Posters
Pingback: holky na sex
Pingback: The Last Jedi Movie Posters for sale
Pingback: The Force Awakens Movie Posters for sale
Pingback: pelechy pro psy
Pingback: Painting Services
Pingback: kayseri miras avukatı
Pingback: comprar bitcoins en mexico
Pingback: Return of the Jedi Mugs for sale
Pingback: The Phantom Menace Film Posters
Pingback: Revenge of the Sith Mugs for sale
Pingback: Star Wars Mugs for sale
Pingback: bitcoin
Pingback: Mugs for sale
Pingback: Toys shop
Pingback: The Force Awakens Cups
Pingback: Eswara Bracelet Women
Pingback: Eswara Bracelet Men
Pingback: amazon app store
Pingback: black friday pc deals
Pingback: Game Stop
Pingback: Jooga vähendab stressi ja teeb õnnelikuks
Pingback: Cyber Monday
Pingback: Joogatunnid pühapäeviti Tallinnas
Pingback: Joogastuudio Tallinnas
Pingback: amazon app
Pingback: Black Friday deals
Pingback: www.joogastuudio.ee/uuemad/meditatsioon-tershula-kriya/
Pingback: Revenge of the Sith Toy shop
Pingback: The Force Awakens Toy shop
Pingback: Thanksgiving
Pingback: Yoga center
Pingback: stores
Pingback: best deals
Pingback: Yoga
Pingback: amazon fan
Pingback: Unique and Unusual
Pingback: www.joogastuudio.ee/elustiil/jooga-jennifer-aniston-sisemine-rahu/
Pingback: black friday 2017 deals
Pingback: Kundalini jooga Tallinnas
Pingback: CageYourBird
Pingback: black friday laptop deals
Pingback: Jooga
Pingback: black friday deals
Pingback: amazon smartphone
Pingback: Jooga mõjub meie kehale rahustavalt
Pingback: turbo tax
Pingback: amazon shopping
Pingback: black Friday 2017 Target
Pingback: www.joogastuudio.ee/uncategorized/himaalaja-elujou-tuur-ponev-kogemus/
Pingback: Joogastuudio Tallinnas
Pingback: www.joogastuudio.ee/uuemad/mediteerimine-teadliku-ning-onneliku-elu-lahutamatu-osa/
Pingback: View website
Pingback: bali turtle island tour
Pingback: tanah lot tour
Pingback: www.joogastuudio.ee/uuemad/hea-vorm-saab-alguse-tervest-seljast/
Pingback: www.joogastuudio.ee/uuemad/meditatsioon-tershula-kriya/
Pingback: bali watersport uluwatu tour
Pingback: bali hourse riding tour
Pingback: www.joogastuudio.ee/uuemad/joogatunnid-meestele/
Pingback: bali parasailing adventure
Pingback: www.joogastuudio.ee/uuemad/meditatsioon_kundalini_joogatunnid/
Pingback: bali elepant ride tour
Pingback: Kundalini jooga
Pingback: Jooga loob meeleolu ja rahutunde
Pingback: bali atv ride tour
Pingback: bali bird park tour
Pingback: www.joogastuudio.ee/uuemad/kolm-lihtsat-nippi-kuidas-talv-roomsaks-muuta/
Pingback: amazon boys clothes
Pingback: www.joogastuudio.ee/uuemad/hommiku-voi-ohtu-nimesed/
Pingback: amazon nike shoes
Pingback: black friday camera deals 2017
Pingback: Joogatunnid
Pingback: Joogastuudio
Pingback: Joogatunnid algajatele
Pingback: daddy's girl
Pingback: black friday on Amazon
Pingback: www.joogastuudio.ee/uncategorized/man-jeetai-jag-jeet-allutad-meele-vallutad-maailma/
Pingback: Yoga in Tallinn
Pingback: Money spell caster
Pingback: dogsled
Pingback: black magic spell caster
Pingback: real spell caster
Pingback: vote4rose travel
Pingback: travel
Pingback: Joogastuudio Tallinnas
Pingback: most powerful spell caster in the world
Pingback: love spells caster online
Pingback: Lost love spell caster
Pingback: love spells caster that work in 24 hours
Pingback: Magic rings
Pingback: most powerful spell caster in the world
Pingback: real spell caster
Pingback: Love spells
Pingback: lottery spell caster
Pingback: Accurate Psychic Reading
Pingback: Lost love spell caster
Pingback: Magic rings
Pingback: most powerful spell caster in the world
Pingback: real spell caster
Pingback: most powerful spell caster in the world
Pingback: Lottery spells
Pingback: Magic rings
Pingback: Lost love spell caster
Pingback: privately renting your property
Pingback: howtomakemoneyfastonline
Pingback: best realistic dildo
Pingback: makemoneysellingonline
Pingback: deals
Pingback: want to rent my property
Pingback: Rent my house
Pingback: escort agency birmingham
Pingback: web design agency
Pingback: digital marketing agency birmingham
Pingback: beginners bondage kit
Pingback: waystomakegoodmoneyonline
Pingback: canyoumakemoneyonline
Pingback: washing machine repair leeds
Pingback: whatcanidoonlinetomakemoney
Pingback: makemoneyonlinefree
Pingback: hijama birmingham
Pingback: howtomakeeasymoneyonline
Pingback: makeearnmoneyonline
Pingback: How to Use a Prostate Massager
Pingback: makequickmoneyonline
Pingback: GREEK SANTORINI TOURS
Pingback: blog assurance
Pingback: informations assurance
Pingback: canwemakemoneyonline
Pingback: makeearnmoneyonline
Pingback: assurance habitation
Pingback: rent a dumpster
Pingback: dumpster rental davis
Pingback: assurance auto
Pingback: local dumpster rental
Pingback: dumpster rental macomb twp
Pingback: dumpster rental dearborn
Pingback: dumpster rental ortonville
Pingback: waystomakequickmoneyonline
Pingback: construction bin rental
Pingback: makemoneyonlinenow
Pingback: whatcanidoonlinetomakemoney
Pingback: roll off service
Pingback: makeearnmoneyonline
Pingback: trash dumpster rental prices
Pingback: waste bin rental
Pingback: dumpster disposal
Pingback: 10 yard dumpster dimensions
Pingback: waste disposal
Pingback: donate car for charity
Pingback: donate a boat
Pingback: dumpster sizes
Pingback: dumpster rental prices
Pingback: dumpster rental Beavercreek
Pingback: ?Σ????Σ
Pingback: dumpster sizes 10 yard
Pingback: donating your vehicle
Pingback: donate old cars for charity
Pingback: average cost of dumpster rental
Pingback: pleasure balls
Pingback: mini swan wand
Pingback: dumpster rental fairborn
Pingback: Get more instagram followers
Pingback: vehicle donation form
Pingback: rent a dump
Pingback: residential dumpster
Pingback: auto charity donation
Pingback: donate a car for charity
Pingback: 10 yard dumpster
Pingback: car to charity
Pingback: dumpster rental nj
Pingback: tax write off for donating a car
Pingback: tax write off car donation
Pingback: DIGITAL MARKETING
Pingback: vibrating tongue ring
Pingback: best realistic vibrator
Pingback: auto donations tax deductions
Pingback: rent trash dumpster
Pingback: car donations for veterans
Pingback: trash dumpster sizes
Pingback: trash dump
Pingback: dumpster rental Villa Rica
Pingback: ESCORTS
Pingback: cardonation
Pingback: where to donate a car
Pingback: triple treat vibrator
Pingback: free charity cars
Pingback: donate car for tax credit
Pingback: pool enclosure naples
Pingback: social media reseller panel
Pingback: boat donation programs
Pingback: used car donation
Pingback: fastest smm panel
Pingback: ytpanel
Pingback: waste bin rental
Pingback: car donation kidney foundation
Pingback: dumpster cost
Pingback: rent a trash bin
Pingback: smm panel
Pingback: youtube smm panel
Pingback: youtube smm panel
Pingback: reseller panel
Pingback: fastest smm panel
Pingback: Free Instagram Followers
Pingback: donate non working car
Pingback: donate a vehicle tax deduction
Pingback: online car donations auto charity
Pingback: Vibrating Dong
Pingback: construction waste disposal
Pingback: dumpster home
Pingback: pick up junk
Pingback: dumpster rental waste management
Pingback: cars vehicle donation
Pingback: dumpster rental cost
Pingback: dumpster rental Myakka City
Pingback: cost of renting a dumpster
Pingback: garbage pickup
Pingback: Organic followers
Pingback: where to donate used cars
Pingback: Portable Pizza Ovens
Pingback: Best Pizza Ovens
Pingback: rent a roll off dumpster
Pingback: rent a garbage dumpster
Pingback: yard waste dumpster rental
Pingback: Countertop Pizza Ovens
Pingback: waste management bin rental
Pingback: dumpster roll off
Pingback: Erotische massages
Pingback: Get more instagram followers
Pingback: Free Insta followers
Pingback: Chiaroveggenza
Pingback: waste management dumpster cost
Pingback: i need to rent a dumpster
Pingback: local dumpster
Pingback: roll off container sizes
Pingback: How to get more followers
Pingback: More comments
Pingback: Instagram followers
Pingback: adelaide website design
Pingback: high end sex toys
Pingback: melbourne app development
Pingback: jtribe reviews
Pingback: apple app developer
Pingback: cross platform apps
Pingback: digital marketing agency adelaide
Pingback: appster competitors
Pingback: sweat worth
Pingback: fitness app designers
Pingback: magic massager
Pingback: app developers
Pingback: best mobile app development tools
Pingback: kurzové sázky
Pingback: ARK: Survival Evolved - Mysterious Island - Part 1
Pingback: Escort ads
Pingback: ARK: Survival Evolved - TERRORS of the DEEP! - Part 2
Pingback: Daycare First Aid
Pingback: jump rope for beginners
Pingback: top rated vibrators
Pingback: labor lawyer
Pingback: thai property group
Pingback: condo pattaya
Pingback: best anal beads
Pingback: large metal containers with lids
Pingback: apartment pattaya
Pingback: entry level camcorder
Pingback: ebay microwave
Pingback: real estate agent
Pingback: penthouse
Pingback: studio for rent jomtien
Pingback: under 1 million baht
Pingback: pattaya jomtien beach
Pingback: pratumnak pattaya
Pingback: jelly vibraters
Pingback: penis venus
Pingback: cbd oil UK
Pingback: cbd wholesale
Pingback: cbd oils for anxiety
Pingback: sbd oil dabs
Pingback: buy cbd oil
Pingback: rain shower
Pingback: Striptease - Stripster huren? Huur de beste Stripster van Belgi?
Pingback: cbdoil dosages
Pingback: cbd oil private label
Pingback: Striptease
Pingback: cbd oil for sale
Pingback: cbd white label
Pingback: cbd no opiods
Pingback: cbdoil pain management
Pingback: okmoney
Pingback: Nootropics
Pingback: faire un concours facebook nouvelle-calédonie
Pingback: cbd oil for dogs
Pingback: cdb oil vaping
Pingback: NUDE GALS
Pingback: Read More Here
Pingback: online tshirt store
Pingback: travel mug
Pingback: personalised mugs
Pingback: methode piano adulte
Pingback: lecon piano debutant
Pingback: methode piano sans solfege
Pingback: ceramic coffee cup with lid
Pingback: cours piano debutant
Pingback: printed coffee cup
Pingback: 14 oz coffee cups
Pingback: initiation au piano
Pingback: silly t shirts
Pingback: synthetiseur pour debutant
Pingback: fall coffee cups
Pingback: tea and coffee mugs
Pingback: bon piano numerique
Pingback: dirty apparel clothing
Pingback: outdoor store
Pingback: winter hunting gear
Pingback: dirrty clothing
Pingback: black friday outdoor gear
Pingback: cabela's camouflage clothing
Pingback: marilyn monroe iphone 6 plus case
Pingback: gold shark tooth charm
Pingback: heart screw back earrings
Pingback: beds that have storage underneath
Pingback: gold chain with small cross
Pingback: end of tenancy cleaning south west london
Pingback: professional cleaning services london end tenancy
Pingback: tenancy cleaning london
Pingback: tenancy cleaning prices
Pingback: tenancy cleaning london
Pingback: Visit This Link
Pingback: Read More
Pingback: Clicking Here
Pingback: professional cleaning services london end tenancy
Pingback: end of tenancy cleaning north london
Pingback: end of tenancy carpet cleaning
Pingback: Read More Here
Pingback: tenancy cleaning services london
Pingback: Learn More Here
Pingback: post tenancy cleaning
Pingback: Pharmaceutical Report
Pingback: Pharma market research
Pingback: american whopper dildo
Pingback: Go Here
Pingback: pharma report
Pingback: Visit Website
Pingback: end of tenancy cleaning south london
Pingback: Click This Link
Pingback: car service in abu dhabi
Pingback: best benz service
Pingback: Discover More Here
Pingback: benz service in abu dhabi
Pingback: Discover More Here
Pingback: Read More
Pingback: Find Out More
Pingback: hotels in Amman
Pingback: post tenancy cleaning
Pingback: radiator plants
Pingback: Manlift for rent
Pingback: Limo Hire Nottingham
Pingback: best dildo harness
Pingback: Read More
Pingback: Visit This Link
Pingback: Solutions
Pingback: Siding Replacement Virginia Beach
Pingback: wordpress themes free download
Pingback: piano pour debutant
Pingback: Aerial Platforms
Pingback: Construction equipment rental dubai
Pingback: Construction equipment rental dubai
Pingback: Cranes for rent
Pingback: initiation au piano
Pingback: piano pour debutant
Pingback: see now
Pingback: website
Pingback: to know more
Pingback: VIP Financing Solutions reviews
Pingback: VIP Financing Solutions reviews
Pingback: Seo søgemaskineoptimering
Pingback: web
Pingback: click here
Pingback: click now
Pingback: Elf on the Shelf
Pingback: Top gyms in Newark, new jersey
Pingback: jsa tour
Pingback: work home moms home business
Pingback: franchise business in india
Pingback: make money online surveys
Pingback: photo lamp best price
Pingback: Buy gift online
Pingback: make money online business
Pingback: best business affiliate programs
Pingback: all natural handmade soap
Pingback: handmade soap bars
Pingback: moisturizing bar soap
Pingback: rated affiliate program
Pingback: online work moms home
Pingback: make money online easy money
Pingback: learn affiliate marketing
Pingback: phylakes
Pingback: influencer marketing platform
Pingback: cheats
Pingback: rechargeable bullet vibe
Pingback: cremation bracelete
Pingback: prestige propertys pattaya
Pingback: orthopaede
Pingback: orthopaede
Pingback: orthopaede
Pingback: orthopaede
Pingback: lançamentos
Pingback: Memorial Necklace
Pingback: orthopaede
Pingback: strongest vibrating egg
Pingback: playstation 3
Pingback: orthopaede
Pingback: trofeus
Pingback: tutorial assassin's creed
Pingback: room for rent pattaya
Pingback: orthopaede
Pingback: orthopaede
Pingback: Assassins Creed Unity
Pingback: Assassins Creed Syndicate
Pingback: Assassins Creed: Bloodlines
Pingback: strap ons for sale
Pingback: trainer
Pingback: assassin's creed world
Pingback: expansões Assassins Creed
Pingback: phylakes
Pingback: orthopaede
Pingback: Pets Cremation Jewelry
Pingback: orthopaede
Pingback: orthopaede
Pingback: park lane condo pattaya
Pingback: Assassin's Creed Origins
Pingback: encryption virus
Pingback: how to do kegels for women
Pingback: Memorial Jewelry for lost baby
Pingback: ransomware viruses
Pingback: view talay place
Pingback: wannacry virus
Pingback: always in my heart cremation necklace
Pingback: personalized cremation jewelry
Pingback: helepolis
Pingback: cremation jewelry with engraving
Pingback: ransomware protection
Pingback: personalized memorial jewelry
Pingback: Pets Cremation Jewelry
Pingback: personalized memorial jewelry
Pingback: male masturbator
Pingback: Memorial Jewelry
Pingback: personalized memorial jewelry
Pingback: Cremation Necklace
Pingback: view talay
Pingback: helepolis
Pingback: helepolis
Pingback: acumind technology
Pingback: encryption virus
Pingback: wannacry virus
Pingback: ransomware virus
Pingback: petya virus
Pingback: ransomware protection
Pingback: buy bitcoin
Pingback: helepolis mobile
Pingback: helepolis
Pingback: controlled lockdown
Pingback: data theft prevention
Pingback: wannacry virus
Pingback: acumind technology
Pingback: acumind technology
Pingback: IOS App development michigan
Pingback: spy cam
Pingback: dildo
Pingback: Memorial Jewelry for lost baby
Pingback: custom cremation jewelry
Pingback: custom cremation jewelry
Pingback: Flyttevask Oslo
Pingback: cyberskin stroker
Pingback: Cremation Jewelry
Pingback: custom cremation jewelry
Pingback: Dr. kameugne kounchou evrad
Pingback: Dr. evrad kameugne kounchou
Pingback: faa 107 test
Pingback: rechargeable bullet sex toy
Pingback: pittsburgh seo
Pingback: g spot,clitoris
Pingback: advanced chimney sweeps
Pingback: Printing services London
Pingback: ufc official
Pingback: pittsburgh pest services
Pingback: commercial roofing company
Pingback: wedding dj pittsburgh pa
Pingback: new york city mold removal
Pingback: plastic packaging supplier
Pingback: mongolian virgin hair extensions
Pingback: ulefone armor
Pingback: best wheel brands
Pingback: Best automotive products
Pingback: Singapore tour packages
Pingback: Singapore holiday Packages
Pingback: wholesale real estate websites
Pingback: Relationship
Pingback: calcetines originales
Pingback: Shirt
Pingback: Shirt
Pingback: indian virgin hair extensions
Pingback: live casino
Pingback: brazilian virgin hair extensions
Pingback: how to last longer in bed for men
Pingback: agen judi
Pingback: judi qq
Pingback: Vip Picks
Pingback: Vehicle Wraps
Pingback: Corner
Pingback: Sesson
Pingback: Lines
Pingback: Half-time
Pingback: Winner
Pingback: Tips
Pingback: Win
Pingback: Soccer Goal
Pingback: 7 inch dildo
Pingback: Top Odds
Pingback: Vinyl Lettering
Pingback: weave
Pingback: Strapless strap on
Pingback: human hair extensions
Pingback: rabbit vibrator review
Pingback: best rabbit vibe
Pingback: togel singapore
Pingback: Bets
Pingback: Odds
Pingback: judi bola
Pingback: Transfer market
Pingback: Soccer Tips
Pingback: Customer Service
Pingback: 3D Design
Pingback: vibrating butt plug
Pingback: phpMyAdmin
Pingback: ring erection
Pingback: market
Pingback: used
Pingback: resale
Pingback: refer
Pingback: bandar piala dunia
Pingback: best powerful vibrator
Pingback: Super Awesome Toys
Pingback: pokerkoffer kaufen
Pingback: Roofers In Middlesbrough
Pingback: how to use a rabbit vibrator
Pingback: blindtimer
Pingback: hyip
Pingback: consumer loyalty programs
Pingback: custom loyalty cards
Pingback: make money internet
Pingback: ways make money online
Pingback: online business
Pingback: digital marketing services
Pingback: pokern zubehör
Pingback: tshirt pokermotiv
Pingback: what to use as an anal dildo
Pingback: digital advertising
Pingback: online marketing
Pingback: online business
Pingback: digital marketing jobs
Pingback: customer loyalty programs
Pingback: digital marketing agency
Pingback: earn money online
Pingback: customer loyalty solutions
Pingback: business growth strategies
Pingback: customer rewards program
Pingback: how to use sex vibrator
Pingback: business growth strategy
Pingback: business strategy
Pingback: loyalty programs
Pingback: business expansion strategies
Pingback: head honcho masterbator
Pingback: headhunter
Pingback: work home
Pingback: business growth strategy
Pingback: entrepreneurship
Pingback: customer loyalty program
Pingback: business growth strategy
Pingback: consumer loyalty programs
Pingback: entrepreneur
Pingback: loyalty programs
Pingback: website hosting
Pingback: Directory
Pingback: sourcing
Pingback: headhunter
Pingback: anal sex toys for sale
Pingback: content management
Pingback: Online Yellow Pages
Pingback: board pack app
Pingback: suction cup dildo
Pingback: bookmarklets
Pingback: adam and eve discount codes
Pingback: list apps
Pingback: corporate branding companies
Pingback: how to give a blowjob
Pingback: eBook sales
Pingback: Topaz KR 30
Pingback: couples massage
Pingback: Promotions
Pingback: Necklace
Pingback: Pin
Pingback: kennels and cattery
Pingback: about hvac
Pingback: furnace clean
Pingback: Electric dryer
Pingback: Sale
Pingback: flexible dryer vent
Pingback: flexible duct
Pingback: Sale
Pingback: how to fix dryer vent duct
Pingback: dryer vent covers
Pingback: inside dryer vents
Pingback: dryer outside vent
Pingback: roof mounted dryer vents
Pingback: gutter cleaning roseville ca
Pingback: how to clean out your dryer vent
Pingback: gutters cleaning service
Pingback: dryer vent piping
Pingback: naturexan
Pingback: what is dryer vent
Pingback: Dryer Vent Wizard of Northville
Pingback: Business performance enhancement
Pingback: How to clean a dryer vent
Pingback: Dryer service
Pingback: cleaning dryer vent
Pingback: dirty dryer vent
Pingback: furnace cleaners
Pingback: cleaning the dryer vent
Pingback: dryer vent options
Pingback: furnace and duct
Pingback: dryer vent clogged
Pingback: spiral ductwork
Pingback: outside dryer vent
Pingback: dryer lint trap brush
Pingback: Dryer repair service
Pingback: hvac installation services
Pingback: air conditioning repair and installation
Pingback: air vent
Pingback: wizard air
Pingback: vent dryer
Pingback: clean dryer vent pipe
Pingback: vent home
Pingback: linteater
Pingback: croatia world cup
Pingback: home air conditioning reviews
Pingback: dryer vent size
Pingback: furnace repair services
Pingback: best rabbit vibrator
Pingback: croatia world cup
Pingback: 1 clean air
Pingback: Dryer performance problems
Pingback: dryer vent brushes
Pingback: ductwork supplies
Pingback: How to clean a dryer vent
Pingback: oval dryer vent
Pingback: jess hilarious instagram
Pingback: Make Money On Youtube
Pingback: indoor gas dryer vent
Pingback: jess hilarious famous
Pingback: air ducts installation
Pingback: gutters cleaning service
Pingback: luxe princess vibrator
Pingback: how to clean dryer vents
Pingback: livre personnalise enfant
Pingback: livre personnalise
Pingback: vent vent
Pingback: livre personnalise
Pingback: best vent
Pingback: livre personnalisable enfant
Pingback: livre personnalise petit garcon
Pingback: spiral ductwork
Pingback: livre personnalise enfant
Pingback: ductwork parts
Pingback: livre personnalise
Pingback: livre enfant avec son prenom
Pingback: vent air systems
Pingback: livre avec prenom
Pingback: Dryer Vent Pro in Flatbush
Pingback: Dryer repair Flatbush
Pingback: rabbit vibrator
Pingback: dryer vent clean out
Pingback: Dryer Vent Cleaning Sheepshead bay
Pingback: landal park belgie ardennen
Pingback: indoor dryer vent
Pingback: car tow truck for sale
Pingback: dryer vent elbow
Pingback: gutter cleaning
Pingback: wrecker truck
Pingback: dryer vent metal
Pingback: wrecker rollback for sale
Pingback: HYDRAULICS
Pingback: furnace duct cleaning service
Pingback: metal dryer vent
Pingback: Minecraft Server List
Pingback: ventilation ductwork
Pingback: duct cleaning truck
Pingback: dryer vent boxes
Pingback: Dryer cleaning
Pingback: return air duct
Pingback: wrecker wheel lift
Pingback: flatbed towing truck
Pingback: auto tow service
Pingback: tow truck company hamtramck
Pingback: toe truck
Pingback: Dryer air flow
Pingback: what is a dryer vent
Pingback: microsoft office 2016
Pingback: dryer hood vent
Pingback: dryer vent attachment
Pingback: venting a gas dryer
Pingback: Sheepshead Bay Dryer service
Pingback: clothes dryer venting
Pingback: dryer vent ducts
Pingback: telescopic dryer vent
Pingback: roof dryer vents
Pingback: office 2016 pro
Pingback: oval dryer vent
Pingback: furnace ducts
Pingback: air ducting
Pingback: Vent
Pingback: microsoft office software
Pingback: growth strategies
Pingback: Naastrehvid
Pingback: telecom customer trust ratings
Pingback: another wireless win
Pingback: business phone service supports second harvest
Pingback: voiceonyx level3 communications
Pingback: customer loyalty
Pingback: How To Lose 10 Pounds In A Week Without Exercise
Pingback: palm beach business phone system needs
Pingback: outbound calling campaigns
Pingback: top secrets voip implementation success
Pingback: optimum orthopedics spine longwood florida
Pingback: make successful business call daytona beach
Pingback: marketing jobs
Pingback: shouldnt use iphone as business phone
Pingback: business voip system pompano beach
Pingback: fax email business phone features
Pingback: switch voiceonyxs digital phone service
Pingback: west palm beach office phone systems
Pingback: business phone etiquette tips
Pingback: 7 innovative facts polycom video conferencing
Pingback: voiceonyx offers impressive customization features
Pingback: voiceonyx makes easy international businesses connect with the world
Pingback: customer spotlight voiceonyx backs telecommunications infinity mortgage group
Pingback: can business make sure incoming calls get answered
Pingback: powerful clitoral vibrator
Pingback: connecting florida emerging markets latin america
Pingback: hollywood business phone service systems
Pingback: Rehvid
Pingback: easiest way quickly reach contacts
Pingback: voiceonyx servers were functional during hurricane irma
Pingback: can keep cell phone number private yet make sure customers can always reach
Pingback: st pete business phone service systems
Pingback: west palm beach business phone service systems
Pingback: vibrator usb
Pingback: voiceonyx sponsors 7th annual cows n cabs benefiting local youth charities
Pingback: can monitor call centers call queue stats
Pingback: headlight
Pingback: Lamellrehvid
Pingback: Talverehvid
Pingback: seat
Pingback: www.kumm.ee/blog-and-news/talvine-valjakutse/
Pingback: car
Pingback: Veljeremont Tallinnas
Pingback: part
Pingback: glovebox
Pingback: overhead
Pingback: guages
Pingback: Naastrehvid
Pingback: Soodsad rehvid Tallinnas
Pingback: belt
Pingback: headlight
Pingback: www.kumm.ee/rehvivahetus-nipid/nouanded/rehvirohk/
Pingback: Rehvide vahetus
Pingback: door
Pingback: www.kumm.ee/rehvi-blogi-uudised/tehnikamaailma-suverehvitest-2013/
Pingback: switch
Pingback: interior
Pingback: Suverehvide müük
Pingback: button
Pingback: Soodsad rehvid
Pingback: control
Pingback: www.kumm.ee/rehvivahetus-nipid/nouanded/spidomeetri-kontroll/
Pingback: Suverehvide ost
Pingback: Autode käsipesu
Pingback: radio
Pingback: Valuvelgede remont
Pingback: www.kumm.ee/blog-and-news/ara-lukka-suverehvide-ostmist-kevadesse/
Pingback: lights
Pingback: Odavad rehvid Tallinnas
Pingback: Land for tiny home
Pingback: actuator
Pingback: Rehvihotell Tallinnas
Pingback: Talverehvide müük
Pingback: Rehvide paigaldus Tallinnas
Pingback: bin
Pingback: Rehvihotell Tallinnas
Pingback: www.kumm.ee/rehvivahetus-nipid/nouanded/spidomeetri-kontroll/
Pingback: BACKWATER TOURS
Pingback: www.kumm.ee/rehvi-blogi-uudised/tehnikamaailma-suverehvitest-2013/
Pingback: discounted Tour Packages
Pingback: truck
Pingback: modules
Pingback: guages
Pingback: www.kumm.ee/rehvi-blogi-uudised/tehnikamaailma-test-102012-age-jouk/
Pingback: Talverehvide müük
Pingback: maf
Pingback: Rich Shades
Pingback: Hadbaa Shades
Pingback: Garden Shades
Pingback: Car Umbrellas
Pingback: PILGRIMAGE TOURS
Pingback: parts
Pingback: PILGRIMAGE TOURS
Pingback: www.kumm.ee/blog-and-news/ara-lukka-suverehvide-ostmist-kevadesse/
Pingback: Cross Shades
Pingback: Land for $49 a month
Pingback: Rehvide vahetus Tallinnas
Pingback: Rehvide transport
Pingback: www.kumm.ee/blog-and-news/ara-lukka-suverehvide-ostmist-kevadesse/
Pingback: Rent to own land
Pingback: OUT BOUND HOLIDAYS
Pingback: Kvaliteetsed rehvid Tallinnas
Pingback: Veljeremont Tallinnas
Pingback: Veljeremont Tallinnas
Pingback: Odavad rehvid Tallinnas
Pingback: www.kumm.ee/blog-and-news/ara-lukka-suverehvide-ostmist-kevadesse/
Pingback: Cheap land
Pingback: Waheed Shades
Pingback: Kerala trip
Pingback: trims
Pingback: Swimmingpool shades
Pingback: Rent to own land
Pingback: Swimmingpool shades
Pingback: Rehvide vahetus Tallinnas
Pingback: Kvaliteetsed rehvid Tallinnas
Pingback: www.kumm.ee/rehvivahetus-nipid/tahised-ja-indeksid/
Pingback: Rehvide transport
Pingback: Rehvide transport
Pingback: Kvaliteetsed rehvid Tallinnas
Pingback: motors
Pingback: AYURVEDA PACKAGES
Pingback: mirrior
Pingback: WINTER HOLIDAYS
Pingback: marker
Pingback: Odavad rehvid Tallinnas
Pingback: molding
Pingback: Land with 0% interest
Pingback: Cross Shades
Pingback: Autode käsipesu
Pingback: Car Umbrellas
Pingback: trim
Pingback: Rehvihotell Tallinnas
Pingback: www.kumm.ee/rehvivahetus-nipid/tahised-ja-indeksid/
Pingback: bezel
Pingback: Rehvide paigaldus Tallinnas
Pingback: Talverehvide müük
Pingback: South India Tour Packages
Pingback: Rent to own land
Pingback: Rehvid
Pingback: controller
Pingback: PVC Shades
Pingback: SEO in HK
Pingback: doors
Pingback: marker
Pingback: belt
Pingback: Search Engine Optimization in Hong Kong
Pingback: Manamah Shades
Pingback: lights
Pingback: controller
Pingback: panel
Pingback: SEO experts in Hong Kong
Pingback: SEO experts in Hong Kong
Pingback: guage
Pingback: Car Shades
Pingback: panels
Pingback: Minor Variance
Pingback: Site Plan
Pingback: buttons
Pingback: buttons
Pingback: button
Pingback: Sundivision
Pingback: repair
Pingback: Crime Prevention Through Environmental Design
Pingback: dash
Pingback: modual
Pingback: Urban Planning
Pingback: Conceptual Design
Pingback: parts
Pingback: Design Out Crime
Pingback: seats
Pingback: Niagara Escarpment Commission Permit
Pingback: maf
Pingback: garbage containers rental
Pingback: trim
Pingback: Crisis Communications
Pingback: do it yourself appliance repair
Pingback: appliance store
Pingback: Patriot Brokerage Inc CA
Pingback: learn hebrew online
Pingback: Speech Therapist Adelaide
Pingback: maytag washer repair
Pingback: kitchenaid repair
Pingback: salvage
Pingback: auto
Pingback: amana refrigerator
Pingback: waste services
Pingback: button
Pingback: i need a dumpster
Pingback: control
Pingback: motor
Pingback: richards appliance repair
Pingback: lights
Pingback: refuse dumpster
Pingback: maytag replacement parts
Pingback: replacement
Pingback: all appliance service
Pingback: dumpster rental phoenix
Pingback: waste managment
Pingback: radios
Pingback: maf
Pingback: rumpke dumpster rental
Pingback: control
Pingback: headlights
Pingback: guage
Pingback: appliance cleaning service
Pingback: real estate investing companies Wayne County
Pingback: real estate investing classes Oakland County
Pingback: appliance company
Pingback: real estate investing books Michigan
Pingback: actuator
Pingback: major appliance parts
Pingback: vibrator with rotating beads
Pingback: lg refrigerator repair
Pingback: large appliance repair
Pingback: Leesburg appliance repair
Pingback: exterior
Pingback: switch
Pingback: maytag service
Pingback: dryer
Pingback: guages
Pingback: maytag washing machine repair
Pingback: Macomb County real estate investing
Pingback: how to fix refrigerator
Pingback: sam cohen-brown
Pingback: aviv appliance repair
Pingback: trims
Pingback: shopify store
Pingback: graphic tshirt
Pingback: marker
Pingback: lg appliance customer service
Pingback: bfi dumpster rental
Pingback: washer dryer repair service
Pingback: orvilles appliance service
Pingback: 10 yard dumpster
Pingback: dumpster cost
Pingback: commercial oven repair
Pingback: modual
Pingback: motors
Pingback: store
Pingback: switch
Pingback: shopify store
Pingback: residential trash pickup
Pingback: 10 cubic yard dumpster
Pingback: glovebox
Pingback: container garbage rental
Pingback: commercial dumpster
Pingback: roll off trash containers
Pingback: dumpster trash service
Pingback: yard waste removal
Pingback: roll up dumpster
Pingback: replacement
Pingback: actuator
Pingback: junk removal service
Pingback: dumpster rental miami
Pingback: dumpster delivery and pick up
Pingback: gotjunk
Pingback: junk removal business
Pingback: waste rental containers
Pingback: furniture disposal
Pingback: roll off dumpsters for rent
Pingback: container dumpster
Pingback: waste dumpster prices
Pingback: yard dumpster
Pingback: waste management dumpster cost
Pingback: headlights
Pingback: part
Pingback: dumpster rental las vegas
Pingback: dumpster rental Mishawaka
Pingback: yard waste disposal
Pingback: junk bin
Pingback: roll off
Pingback: dumpster rental Lake Station
Pingback: dump rental
Pingback: concrete dumpster
Pingback: dumpster home
Pingback: garbage dumpster rental prices
Pingback: dumpsters rental
Pingback: controllers
Pingback: modules
Pingback: dryer vent cleaning ann arbor
Pingback: headlamps
Pingback: order a dumpster
Pingback: roll off dumpster sizes
Pingback: affordable dumpsters
Pingback: venting a dryer
Pingback: map
Pingback: control
Pingback: moldings
Pingback: furnace cleaners
Pingback: 40 yard roll off dumpster
Pingback: truck
Pingback: airbags
Pingback: waste management roll off dumpsters
Pingback: trash rental bins
Pingback: how to clean out the dryer vent
Pingback: how to dryer vent cleaning
Pingback: as air conditioning
Pingback: auto
Pingback: dryer vent hood
Pingback: belts
Pingback: markers
Pingback: seats
Pingback: duct work
Pingback: Click Here
Pingback: Click Here
Pingback: doors
Pingback: altcoins
Pingback: tumblr pictures
Pingback: business directory
Pingback: maf
Pingback: replacement
Pingback: bezel
Pingback: RUSSIAN ESCORT
Pingback: maf
Pingback: molding
Pingback: buy
Pingback: switch
Pingback: astaxanthin
Pingback: Products
Pingback: sell
Pingback: glovebox
Pingback: seats
Pingback: astaxanthin
Pingback: opportunity
Pingback: switch
Pingback: button
Pingback: doors
Pingback: motor
Pingback: vezi pe ora 7
Pingback: small law firm marketing
Pingback: trims
Pingback: law firm web marketing
Pingback: sensors
Pingback: Best Bucharest Escorts
Pingback: astaxanthin
Pingback: internet marketing for law firms
Pingback: astaxanthin
Pingback: kostenlose Kleinanzeigen
Pingback: markers
Pingback: astaxanthin
Pingback: small law firm marketing
Pingback: astaxanthin
Pingback: metal para sayma
Pingback: astaxanthin
Pingback: doors
Pingback: law firm marketing plan
Pingback: lyrics
Pingback: Sasha Sloan
Pingback: astaxanthin
Pingback: mirrors
Pingback: Law firm marketing
Pingback: VIP Financing Solutions reviews
Pingback: Hemstadning Solna
Pingback: Soodsad rehvid Tallinnas
Pingback: trim
Pingback: seats
Pingback: Adult Toys
Pingback: Lawyer marketing
Pingback: auto
Pingback: seats
Pingback: Talverehvide müük
Pingback: w88 club
Pingback: Rehvid
Pingback: pipedreams company
Pingback: myrtle
Pingback: headlamp
Pingback: motor
Pingback: social media marketing for large law firms
Pingback: Hemstadning Solna
Pingback: learning the Oud
Pingback: Kaubiku rehvid
Pingback: law firm online marketing
Pingback: Rehvid
Pingback: Suvekummid
Pingback: Oud instrument
Pingback: pink mini vibrator
Pingback: law firm web marketing
Pingback: Talverehvid
Pingback: law firm marketing ideas
Pingback: Mass email service
Pingback: dresses
Pingback: law of attraction
Pingback: Online Movies
Pingback: Soodsad rehvid
Pingback: shin chan movie in tamil 2016 download
Pingback: chin chan in tamil
Pingback: hungama tamil
Pingback: shin chan in tamil full movie
Pingback: save a marriage
Pingback: shin chan in tamil new episodes 2012
Pingback: shin chan in tamil song
Pingback: shin chan in tamil new episodes 2016
Pingback: Tourism Theme WordPress Travel and Leisure Theme from Gorilla Themes
Pingback: huge dildos
Pingback: 10 Hot Fitness Accounts on Instagram | Black Women | Izzie's World
Pingback: Media Traffic Meltdown System Get Website Traffic
Pingback: www.bebinak.com/result/?????
Pingback: bandar casino dagbet online terpercaya
Pingback: short meditation
Pingback: Panduan bermain sbobet
Pingback: Trapped Puppies Animal Rescue
Pingback: Judi 88tangkas terpercaya
Pingback: www.bebinak.com/result/???????
Pingback: yoga site
Pingback: www.bebinak.com/result/?????_?_????_????
Pingback: guided meditation for healing
Pingback: www.bebinak.com/result/universal_motor
Pingback: www.bebinak.com/result/?????_????
Pingback: www.bebinak.com/result/?????_?????
Pingback: yoga practice online
Pingback: www.bebinak.com/result/huayra_??????_??????_???
Pingback: G-spot vibrator
Pingback: Provillus Hair Loss Treatment for Women
Pingback: www.bebinak.com/result/??_????
Pingback: Susannah Mushatt Jones July 6, 1899 - May 12, 2016 | World's Oldest People
Pingback: www.bebinak.com/result/??????_?????
Pingback: Subscribe To Izzie Vlogs & More! On YouTube for My Weight Loss Journey 2018
Pingback: Pasang taruhan di situs judi roulette online
Pingback: www.bebinak.com/result/???_????
Pingback: www.bebinak.com/result/??_????????_????_??
Pingback: www.bebinak.com/result/?????_???
Pingback: guided meditation for stress
Pingback: weddingcar
Pingback: Bandar judi kasino dagbet terpercaya
Pingback: Protect your body from painful inflammation with Curcumin 2000
Pingback: Inilah tips dan trik terbaru agar menang judi online
Pingback: Get Cash Back On Purchases with Ebates
Pingback: Setlist Theme WordPress Music Theme from Gorilla Themes
Pingback: Affilorama Affiliate Marketing Training Program
Pingback: Affilorama Affiliate Marketing Training Program
Pingback: www.bebinak.com/result/??????_???_????
Pingback: Promo menarik bermain tangkas online
Pingback: My Weight Loss Journey Introduction 2017-2018
Pingback: www.bebinak.com/result/????_??
Pingback: american whopper
Pingback: Natural Cold & Sore Throat Remedy
Pingback: Cara bermain sic bo live
Pingback: www.bebinak.com/result/?????_???_????
Pingback: www.bebinak.com/result/????????
Pingback: www.bebinak.com/result/????_?????
Pingback: Taruhan sbobet card cuma seribu
Pingback: www.bebinak.com/result/????_????_????
Pingback: Terry Sacka AAMS
Pingback: www.bebinak.com/result/???_??????
Pingback: Asset Preservation
Pingback: Cara bermain judi baccarat online
Pingback: www.bebinak.com/result/???_?????
Pingback: www.bebinak.com/result/??????_????
Pingback: Masturbators for Men
Pingback: Cara bermain togel isian4d
Pingback: BRICS
Pingback: President of United States
Pingback: Click Here
Pingback: Inilah situs bandar togel singapura
Pingback: Bandar judi dadu live
Pingback: Silver Investing
Pingback: Cara menang judi sabung ayam
Pingback: www.bebinak.com/result/???????_???_????
Pingback: www.bebinak.com/result/????
Pingback: www.bebinak.com/result/??????
Pingback: www.bebinak.com/result/???????_????_?????
Pingback: Syrian Refugee Immigration
Pingback: House Bill 224
Pingback: US Dollar
Pingback: Petrodollar Future
Pingback: Cornerstone Asset Metals
Pingback: 7 year sabbatical cycle
Pingback: House Bill 224
Pingback: www.bebinak.com/result/????_??????
Pingback: Family Mediation
Pingback: www.bebinak.com/result/???????_???????_???
Pingback: Matthew Brickman
Pingback: Law Service
Pingback: Imediate Inc
Pingback: http://ge.tt/5cMuHsm2
Pingback: Timesharing
Pingback: bathmate pump
Pingback: hot cocktail dress
Pingback: vintage lace dress short
Pingback: wedding dresses online custom
Pingback: sexy wedding dress
Pingback: black lace prom dress
Pingback: latest mobile technoies
Pingback: Nebraska
Pingback: BMW Tires Dubai
Pingback: sex wand
Pingback: mint dresses
Pingback: buy website traffic
Pingback: buy website traffic
Pingback: Sexy Wedding Dresses
Pingback: carpet cleaning oxfordshire
Pingback: Bridal Wedding Dresses
Pingback: traffic
Pingback: engagement dresses
Pingback: quality wedding dresses
Pingback: SEO EXPERT
Pingback: dj course
Pingback: how to get a six pack in a month
Pingback: how to get a six pack in a month
Pingback: Click Here
Pingback: Read More
Pingback: Click Here
Pingback: ken calhoun
Pingback: ken calhoun
Pingback: Click Here
Pingback: Agen SBOBET IBCBET
Pingback: Fashion
Pingback: Fashion
Pingback: video game reviews
Pingback: ken calhoun
Pingback: latest video game news
Pingback: acne scars
Pingback: Situs Judi Terpercaya
Pingback: Casino GD88
Pingback: Clear Bra San Diego
Pingback: Tangkas88
Pingback: Agen SBOBET IBCBET
Pingback: Judi Togel Online
Pingback: Bola Tangkas
Pingback: Judi Online Indonesia Terpercaya Terbaik
Pingback: world news
Pingback: w3newspapers
Pingback: government website list Bangladesh
Pingback: all bangla newspapers
Pingback: video
Pingback: Bangla newspaper
Pingback: dumpster rental Rosewell
Pingback: ch digital seo
Pingback: ch digital american idol
Pingback: dumpster rental Lithonia
Pingback: ch digital llc
Pingback: chdigital.net
Pingback: rolloff dumpsters
Pingback: ch digital creative design
Pingback: ch digital american idol
Pingback: tinnitus miracle buy
Pingback: shopify
Pingback: dumpster delivery and pick up
Pingback: rent a dumper
Pingback: tinnitus miracle book reviews
Pingback: tinnitus miracle book online
Pingback: tinnitus miracle review
Pingback: saying
Pingback: construction waste containers
Pingback: tinnitus miracle book by thomas
Pingback: dumpster rental ri
Pingback: demolition container rental
Pingback: roll off service
Pingback: average cost of dumpster rental
Pingback: free junk removal
Pingback: Leone Leather
Pingback: Briefcases
Pingback: About Us
Pingback: tinnitus miracle book
Pingback: junk container rental
Pingback: furniture disposal
Pingback: Tote Bags
Pingback: Messenger Bags
Pingback: tinnitus miracle book
Pingback: dumpster rental holly
Pingback: Canvas
Pingback: junk hauling
Pingback: trash hauling
Pingback: michigan dumpsters
Pingback: bankers adda sbi po mock test
Pingback: tinnitus miracle cure 5
Pingback: dumpster home
Pingback: dumpster delivery
Pingback: waste management dumpster prices
Pingback: 8 yard dumpster
Pingback: rent a dumpster cost
Pingback: garbage bin
Pingback: 8 yard dumpster rental
Pingback: rent a bin prices
Pingback: open top container rental
Pingback: 20 cubic yard dumpster
Pingback: Pet seat cover for cars
Pingback: home interior painting
Pingback: Seat Cover for Cars
Pingback: Seat Cover for Cars
Pingback: masonry paint
Pingback: hammock seat cover
Pingback: drywall contractors seattle
Pingback: dumpster rental sterling hts
Pingback: dumpster rental washington twp
Pingback: dumpster rental brammel
Pingback: dumpster rental Clio
Pingback: find a drywall contractor
Pingback: dumpster rental orion twp
Pingback: need my house painted
Pingback: painting businesses near me
Pingback: dumpster companies
Pingback: 10 yard dumpster cost
Pingback: home improvement painting
Pingback: garbage container rentals
Pingback: garbage bin rental
Pingback: recycling dumpsters
Pingback: rent small dumpster
Pingback: affordable dumpsters
Pingback: residential dumpsters for rent
Pingback: Dryer Vent Wizard NYC
Pingback: Flatbush Dryer Vents
Pingback: dryer vent installation
Pingback: Dryer installation
Pingback: dryer vent installation
Pingback: Dryer vent
Pingback: Dryer performance problems
Pingback: rent a dumpster prices
Pingback: Dryer vent clog
Pingback: construction waste disposal
Pingback: rent construction dumpster
Pingback: waste removal services
Pingback: yard debris removal
Pingback: pick up trash
Pingback: waste management dumpster service
Pingback: Seat Cover
Pingback: pet car seat cover
Pingback: dumpster bins for rent
Pingback: average cost of dumpster rental
Pingback: Seat Cover for Pets
Pingback: how to increase penis size at home
Pingback: Allthingscrypto.tech
Pingback: Allthingscrypto.tech
Pingback: clit sex toys
Pingback: Allthingscrypto.tech
Pingback: Allthingscrypto
Pingback: tablet screen repair in Waterbury
Pingback: ipad repair near me
Pingback: computer virus removal service
Pingback: yoga masturbation
Pingback: copyright attorney
Pingback: Cape cod
Pingback: laptop repair shop near me
Pingback: hard drive repair near me
Pingback: pu sandwich panel production line
Pingback: Allthingscrypto.tech
Pingback: Allthingscrypto
Pingback: laptop repair shop near me
Pingback: security camera companies near me
Pingback: astaxanthin
Pingback: computer virus removal service
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: Allthingscrypto
Pingback: Allthingscrypto
Pingback: astaxanthin
Pingback: birmingham wedding photography
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: jsa tour
Pingback: astaxanthin
Pingback: famille
Pingback: enfant
Pingback: Videos
Pingback: Allthingscrypto
Pingback: Hip Hop
Pingback: astaxanthin
Pingback: Click Here
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: astaxanthin
Pingback: Hotel Tuscany
Pingback: Hotel Maremma
Pingback: Allthingscrypto
Pingback: NUDE PHOTOGRAPHY
Pingback: prescription lenses
Pingback: blue light glasses
Pingback: Allthingscrypto
Pingback: Allthingscrypto.tech
Pingback: ali yalçındaÄ
Pingback: mehmet yalçındaÄ
Pingback: mehmet yalçındaÄ
Pingback: Lean Belly Breakthrough
Pingback: Stanley Steamer Specials
Pingback: dumpster rental Marietta
Pingback: rollaway dumpster rental
Pingback: dumpster rental Johns Creek
Pingback: dumpster rental canton
Pingback: roll away trash containers
Pingback: Candler-McAfee dumpsters
Pingback: dumpster rental orion twp
Pingback: 20 yard dumpster
Pingback: construction debris disposal
Pingback: used roll off trucks
Pingback: dumpster rental prices
Pingback: dumpster rental Zilwaukee
Pingback: trash containers for rent
Pingback: dumpster prices
Pingback: 5 yard dumpster
Pingback: waste management roll off
Pingback: trash company
Pingback: gotjunk
Pingback: black mens cowboy boots
Pingback: roll off dumpster
Pingback: dumpster bag
Pingback: waste management service
Pingback: all waste dumpster rental
Pingback: dumpster rental houston
Pingback: dumpster central
Pingback: Allthingscrypto.tech
Pingback: garbage dumpster
Pingback: garbage dumpster
Pingback: waste management dumpster rental
Pingback: license to fly drone
Pingback: dump container rental
Pingback: price to rent a dumpster
Pingback: cost of roll off dumpster
Pingback: roll off dumpster rental prices
Pingback: garbage disposal rental
Pingback: small dumpster
Pingback: rent a garbage dumpster
Pingback: 20 yard dumpster rental
Pingback: garbage bin rental prices
Pingback: residential waste removal
Pingback: all brands appliance repair
Pingback: Allthingscrypto.tech
Pingback: lg refrigerator repair
Pingback: gas appliance repair
Pingback: rent a dumpster
Pingback: dumpster rental washington twp
Pingback: SEO in Hong Kong
Pingback: finger sleeves
Pingback: appliance service center
Pingback: samsung washer repair
Pingback: SEO experts in Hong Kong
Pingback: garbage dumpster sizes
Pingback: garbage dumper
Pingback: Search Engine Optimization in HK
Pingback: aviv appliance repair
Pingback: kitchenaid service
Pingback: SEO in HK
Pingback: dumpster rental new boston
Pingback: quality appliance service
Pingback: trash container rental
Pingback: lg appliance customer service
Pingback: cheap washing machines
Pingback: Concinnity Limited
Pingback: rent waste container
Pingback: dumpster rental richmond twp
Pingback: anal training toys
Pingback: dishwasher parts
Pingback: watch z hindi movie movies
Pingback: a war full movies
Pingback: construction trash removal
Pingback: dumpster rental indianapolis
Pingback: watch movies online hindi
Pingback: rent a roll off dumpster
Pingback: dumpster for sale
Pingback: need a dumpster
Pingback: full movies furious 6
Pingback: smallest dumpster size
Pingback: the dumpster
Pingback: penis sleeve
Pingback: waste bins rental
Pingback: industrial dumpster
Pingback: debris removal services
Pingback: garbage dumpster
Pingback: 4 yard dumpster
Pingback: dumpster waste management
Pingback: recycling roll off containers
Pingback: commercial dumpster sizes
Pingback: nipple toys
Pingback: yard waste dumpster
Pingback: hire a dumpster
Pingback: rent a roll off dumpster
Pingback: 2 yard dumpster rental
Pingback: dumpster rental maryland
Pingback: 8 yard dumpster rental
Pingback: portable trash dumpster
Pingback: dumpster rental southfield
Pingback: 10 yard roll off dumpster
Pingback: dumpster rental detroit
Pingback: Dietary Supplement
Pingback: get rid of it dumpsters
Pingback: Lipstick production
Pingback: Cosmetic production
Pingback: dumpsters near me
Pingback: rollaway dumpster rental
Pingback: roll off containers sizes
Pingback: trash hauling
Pingback: waste management dumpster rental cost
Pingback: construction debris removal
Pingback: 15 yard dumpster rental
Pingback: rent a garbage dumpster
Pingback: Bored pile
Pingback: trash dump
Pingback: dumpster cost
Pingback: substance abuse professional
Pingback: trash dumpster sizes
Pingback: dumpster rental richmond twp
Pingback: premium gambling bonuses
Pingback: top casino bonuses
Pingback: casino bonus
Pingback: bingo bonuses
Pingback: gambling bonuses
Pingback: casino bonuses
Pingback: best casino bonus
Pingback: top casino bonuses
Pingback: top casinos
Pingback: granite worktops glasgow
Pingback: home
Pingback: mobile car valet solihull
Pingback: cupping birmingham
Pingback: home
Pingback: best product reviews 2018
Pingback: Christie projector
Pingback: home
Pingback: home
Pingback: best selling weight-loss supplements
Pingback: audio/Visual
Pingback: church sound system design and installation
Pingback: cupping birmingham
Pingback: townhomes for sale
Pingback: best online grammar service
Pingback: landlord
Pingback: houses for sale near me
Pingback: trade with currency
Pingback: home
Pingback: best brain power supplements
Pingback: foreclosure
Pingback: best online reviews
Pingback: best reviews on amazon
Pingback: home
Pingback: Small church video system
Pingback: rent a boat
Pingback: hacking articles
Pingback: church sound system design
Pingback: car insurance reviews
Pingback: data breach
Pingback: how to hack
Pingback: the hacker news
Pingback: best tech blog
Pingback: home
Pingback: home
Pingback: home
Pingback: best selling wedding rings discount
Pingback: latest hacking news
Pingback: home
Pingback: data breach
Pingback: audio video and film technology
Pingback: hack facebook
Pingback: trade with currency
Pingback: latest hacking news
Pingback: build your own website
Pingback: fine gold and diamond jewelry
Pingback: Top Luxury watches online
Pingback: Digital signage display
Pingback: Best church sound system
Pingback: hacking news
Pingback: hack facebook
Pingback: tech hacks
Pingback: best selling gardening tools
Pingback: viral tech
Pingback: the hacker news
Pingback: data breach
Pingback: hacking articles
Pingback: audio video news
Pingback: latest hacking news
Pingback: Small church video system
Pingback: computer security
Pingback: hacking articles
Pingback: best selling electronic
Pingback: viral tech
Pingback: computer security breaches
Pingback: tech hacks
Pingback: see
Pingback: latest news
Pingback: url
Pingback: Latest Gadgets
Pingback: latest news
Pingback: latest news
Pingback: link
Pingback: see
Pingback: Best affiliate program
Pingback: Online game reviews
Pingback: visit
Pingback: home
Pingback: home
Pingback: see
Pingback: best online service guide
Pingback: Online Reviews Shopping Guide
Pingback: latest technology
Pingback: url
Pingback: url
Pingback: How to build online business
Pingback: see
Pingback: start
Pingback: technology reviews
Pingback: Top Star Reviews By Consumers
Pingback: crear pagina web para mi negocio
Pingback: blog de naturaleza
Pingback: por que es importante la naturaleza
Pingback: Latest Gadgets
Pingback: where to get bitcoins
Pingback: where to get bitcoins
Pingback: leer resumen de libro
Pingback: latest technology news
Pingback: cual es el puente mas largo
Pingback: las mejores ciudades
Pingback: how can i get bitcoins
Pingback: Lugares que Tienes que Visitar en Argentina
Pingback: Las mejores ciudades para visitar en invierno
Pingback: Noruega
Pingback: purchase bitcoin with credit card
Pingback: buy bitcoin now
Pingback: buy bitcoin with card
Pingback: millonarios
Pingback: bitcoin
Pingback: earn btc
Pingback: bitcoin price today
Pingback: Que hacer en Nueva York
Pingback: travel reviews
Pingback: buy bitcoin with card
Pingback: pagina para amantes de la naturaleza
Pingback: trade with currency
Pingback: weight-loss ideas
Pingback: bitcoin fast
Pingback: trade with currency
Pingback: libros de negocios
Pingback: best home insurance
Pingback: buy bitcoin with cc
Pingback: Trade with gold reviews
Pingback: made to measure table cloths
Pingback: Nappe Pas Cher
Pingback: Nappe Sur Mesure
Pingback: web design
Pingback: web design agency birmingham
Pingback: mobile car valet solihull
Pingback: cupping birmingham
Pingback: pay monthly websites
Pingback: domestic cleaning birmingham
Pingback: digital marketing
Pingback: business
Pingback: business opportunities
Pingback: buy followers instagram
Pingback: buy active instagram followers
Pingback: affiliate
Pingback: business
Pingback: cb passive income
Pingback: buy instagram followers cheap
Pingback: anal plug starter kit
Pingback: online business
Pingback: affiliate internet marketing
Pingback: online business opportunities
Pingback: part time jobs
Pingback: SWITCH CELL PHONE
Pingback: Real Money 8 Ball Pool
Pingback: Real Money 8 Ball Pool Android App
Pingback: disposable microwave containers
Pingback: oven and microwave safe food containers
Pingback: Real Money 8 Ball Pool Android App
Pingback: House of worship sound systems
Pingback: Video projection system for church
Pingback: jerusalem
Pingback: plastic plate set
Pingback: plastic bins
Pingback: eco containers
Pingback: Labrador Zuchter Osterreich
Pingback: Labrador Bilder
Pingback: box with lid
Pingback: Labrador Videos
Pingback: Labradorzucht vom Wolfgangsee
Pingback: microwavable take out containers
Pingback: Labrador Zuchter Osterreich
Pingback: Labrador Zuchter Salzburg
Pingback: Labradorzucht Scheutz
Pingback: Labrador Zuchter Oberosterreich
Pingback: Labradorzucht Scheutz
Pingback: Labradorzucht Scheutz
Pingback: garbage companies
Pingback: dumpster rental washington twp
Pingback: Shiaaka
Pingback: auto insurance liability
Pingback: georgette wear
Pingback: Learn More Here
Pingback: contact us
Pingback: towing a car long distance
Pingback: waste container rental
Pingback: rollback tow truck
Pingback: Learn More
Pingback: free insurance quotes for cars
Pingback: dumpsters for rent
Pingback: kurtis
Pingback: pick truck parts
Pingback: buy kurtis for women online
Pingback: trash disposal
Pingback: dumpster rental cleveland
Pingback: price of dumpster rental
Pingback: buy backlinks
Pingback: hire freelancers
Pingback: frocks
Pingback: Going Here
Pingback: rent a trash dumpster
Pingback: Go Here
Pingback: dumpster rental long island
Pingback: geometric shapes
Pingback: dumpster rental cleveland
Pingback: job posting
Pingback: Read More Here
Pingback: trash dumpster rental cost
Pingback: trash dumpster prices
Pingback: 40 yard dumpster rental price
Pingback: kashmiri silk sarees
Pingback: dumpster trash removal
Pingback: handpicked sarees women
Pingback: trash container service
Pingback: garden sarees india
Pingback: Learn More
Pingback: Learn More
Pingback: free job posting sites
Pingback: 40 yard container
Pingback: buy traditional sarees online
Pingback: waste bin rental
Pingback: rolloff container
Pingback: job posting
Pingback: SOLUTIONS OF ILIOUPOLI COSTA
Pingback: waste bin rental
Pingback: Wolfgang Halbig
Pingback: roll off containers
Pingback: Go Here
Pingback: grow
Pingback: garbage dumpster rental prices
Pingback: junk king
Pingback: dumpster rental waste management
Pingback: hauling junk
Pingback: dumpster hauling
Pingback: url
Pingback: Click Here
Pingback: garbage roll off containers
Pingback: dumpster rental Detroit
Pingback: commercial dumpster sizes
Pingback: url
Pingback: roll off trash containers
Pingback: dirt bin rental
Pingback: Wolfgang Halbig
Pingback: home dumpster service
Pingback: waste dumpster sizes
Pingback: garbage skip
Pingback: garbage containers
Pingback: portable dumpster
Pingback: dumpster rental nj
Pingback: url
Pingback: waste dumpster rental
Pingback: same day dumpster rental
Pingback: url
Pingback: we haul junk
Pingback: Dumpster Rent Pro of San Diego
Pingback: roll off
Pingback: dumpster rental brighton
Pingback: pick up junk
Pingback: container trash rental
Pingback: dumpster rental prices
Pingback: roll away dumpster cost
Pingback: dumpster rental nj
Pingback: construction dumpster rental
Pingback: Leonard Pozner
Pingback: 10 yard dumpster
Pingback: dumpster rental bingham
Pingback: emergency roadside assistance near ecorse
Pingback: truck towing company
Pingback: roll back trucks for sale
Pingback: used auto part search
Pingback: dumpster trash
Pingback: i need a dumpster rental
Pingback: page about a good service provider
Pingback: disposal services
Pingback: local car insurance companies
Pingback: Fort wayne weight loss
Pingback: athenix body sculpting
Pingback: body sculpting exercises
Pingback: how to buy auto insurance
Pingback: best diets to lose weight
Pingback: diet plan to lose weight
Pingback: non surgical liposuction
Pingback: free insurance quotes for cars
Pingback: weight loss camps
Pingback: tickets for davis cup
Pingback: best roadside assistance service
Pingback: weigh loss
Pingback: help to lose weight
Pingback: car insurance with roadside assistance
Pingback: lose weight easily
Pingback: greenly coupon
Pingback: davis cup first round
Pingback: hide a lift
Pingback: emergency roadside service indian village
Pingback: getnugg promo
Pingback: pe bible download
Pingback: pot
Pingback: buy cr2016 battery
Pingback: promo code
Pingback: best 2016 battery
Pingback: pot valet
Pingback: Ultimate Phone Space Saver app
Pingback: Cloud Backup app
Pingback: apothecarry coupon codes
Pingback: coupon code
Pingback: A.I.
Pingback: buy 2cr5 battery
Pingback: vape
Pingback: cheap cr123 battery
Pingback: buy cr2016 battery
Pingback: pot coupons
Pingback: pocket pal
Pingback: retailmepot
Pingback: eaze
Pingback: buy cheap cr 2016 battery
Pingback: buy cr2032 battery
Pingback: cannabis coupons
Pingback: the bible app
Pingback: vape
Pingback: 3v lithium battery
Pingback: cheap cr2016 battery
Pingback: pe exercises to last longer
Pingback: pe bible without supplements
Pingback: are pe exercises safe
Pingback: 24hourbatteries.com
Pingback: bhang
Pingback: manifestation miracle law of attraction
Pingback: buy manifestation miracle
Pingback: legal cannabis
Pingback: nugg coupon codes
Pingback: The Importance of Food Hygiene & Safety
Pingback: pot
Pingback: manifestation miracle audiobook
Pingback: manifestation miracle scam
Pingback: instant manifestation miracle
Pingback: donate mass shooting
Pingback: manifestation miracle sign in
Pingback: eaze
Pingback: manifestation miracle workbook
Pingback: cannabis coupons
Pingback: manifestation miracle
Pingback: miracle manifestation journal
Pingback: manifestation miracle workbook
Pingback: Unplugged
Pingback: Philanthropist
Pingback: manifestation miracle refund
Pingback: manifestation miracle contact
Pingback: miracle manifestation meditation
Pingback: Steve and Friends
Pingback: Unplugged
Pingback: fat diminisher system ebook free download
Pingback: Steve and Friends
Pingback: fat diminisher system review
Pingback: fat diminisher facebook
Pingback: fat diminisher blog
Pingback: fat diminisher system
Pingback: fat diminisher book
Pingback: fat diminisher wes virgin
Pingback: fat diminisher what is it
Pingback: get fat diminisher free
Pingback: fat diminisher forum
Pingback: fat diminisher minerals
Pingback: fat diminisher what to eat
Pingback: fat diminisher system leaked
Pingback: fat diminisher diet reviews
Pingback: language of desire customer reviews
Pingback: language of desire website
Pingback: language of desire online free
Pingback: the language of desire free online
Pingback: language of desire money back
Pingback: language of desire
Pingback: language of desire kindle
Pingback: language of desire reviews amazon
Pingback: youtube language of desire review
Pingback: language of desire money back guarantee
Pingback: language of desire amazon
Pingback: language of streetcar named desire
Pingback: language of desire website
Pingback: read language of desire online free
Pingback: 3d freelance
Pingback: ATHENS HOTEL PRICES
Pingback: gps
Pingback: management
Pingback: marijuana online
Pingback: coupon code
Pingback: driving safety
Pingback: online coupons
Pingback: cannabis coupons
Pingback: employee safety
Pingback: arrive gps
Pingback: gps tracking
Pingback: driving safety
Pingback: weedmaps
Pingback: HYDRAULIC ATHENS WORK
Pingback: save on marijuana
Pingback: Lotto Dominator
Pingback: vape oil
Pingback: apothecarry coupon codes
Pingback: california marijuana delivery
Pingback: greenly promo
Pingback: yamanime sub indo batch Size kecil
Pingback: yamanime sub indo batch
Pingback: btech college in Delhi
Pingback: yamanime sub indo batch Size kecil
Pingback: yamanime sub indo Batch TV
Pingback: otakunime sub indo batch Size kecil
Pingback: Yamanime Sub Indo Batch
Pingback: otakunime subtitle indonesia batch
Pingback: Best BTech College in India
Pingback: Best Electronics & Communication Engineering College in Delhi NCR
Pingback: Best Engineering College in Bahadurgarh
Pingback: otakunime sub indo batch Size kecil
Pingback: Yamanime Sub Indo Batch
Pingback: Yamanime Com
Pingback: list of engineering colleges in Delhi
Pingback: yamanime sub indo sendit
Pingback: Best BTech College in Bahadurgarh
Pingback: otakunime sub indo batch BD
Pingback: Yamanime Sub Indo Batch
Pingback: Click here
Pingback: Buy Cottages in Dehradun
Pingback: Buy Cottages in Dehradun
Pingback: Real Estate Company in Delhi NCR India
Pingback: Cottage in Hills
Pingback: Luxury cottages
Pingback: Elegant Cottages in India
Pingback: Dream Cottages
Pingback: Cottages
Pingback: wabbit sex toy
Pingback: jelly vibrator
Pingback: ERP in Singapore
Pingback: Life Science Jobs Belgium
Pingback: Medical Device Jobs Spain
Pingback: Pharma Jobs Europe
Pingback: Life Science Jobs France
Pingback: Life Science Jobs Belgium
Pingback: kitchenaid artisan stand mixer
Pingback: Maid service Dallas
Pingback: stand mixer
Pingback: DFW Maids
Pingback: best kitchen mixer
Pingback: kitchen stand mixers
Pingback: Maids in Dallas
Pingback: breville stand mixers
Pingback: quickmixers.com
Pingback: DFW Maids
Pingback: kitchen stand mixer
Pingback: kitchenaid artisan stand mixer
Pingback: Grasscutter farming in Nigeria
Pingback: How to produce cold water starch in Nigeria
Pingback: kitchenaid artisan
Pingback: stand mixer reviews
Pingback: kitchen stand mixers
Pingback: Search Engine Optimization Service in Nigeria
Pingback: Why small Businesses fail in Nigeria
Pingback: Tomato farming in Nigeria
Pingback: Tangela Allman
Pingback: Inocencia Blaker
Pingback: Top lucrative Business ideas
Pingback: Steven Cutts
Pingback: Josiah Klem
Pingback: Shanta Shaddix
Pingback: Steven Cutts
Pingback: Jenise Pero
Pingback: Roselle Prost
Pingback: Steven Cutts
Pingback: Darline Kunst
Pingback: Georgette Loiacono
Pingback: Steven Cutts
Pingback: Malisa Shrum
Pingback: PSYCHOLOGIST ATHENS
Pingback: Julio Ramos
Pingback: Kourtney Blay
Pingback: Katelin Vanzile
Pingback: Madlyn Spann
Pingback: Malisa Shrum
Pingback: ball of foot pads for women
Pingback: ESCORT SEX TUBE
Pingback: foot metatarsal support
Pingback: best metatarsal foot pads
Pingback: Hawaii Wedding Photographer
Pingback: buy vpn
Pingback: buy vpn
Pingback: buy vpn
Pingback: Night Version Camera
Pingback: fitnet vpn
Pingback: Anti-Drone Jammer
Pingback: Unmanned Surface Vesse
Pingback: Anti-Drone Gun
Pingback: Unmanned Surface Boat
Pingback: Night Version Camera
Pingback: Agricultural Drone
Pingback: fitnet
Pingback: posture corrector medbr
Pingback: pressure relief with metatarsal pad
Pingback: Anti-Drone Jammer
Pingback: Explosion Proof Camera
Pingback: shoulder posture corrector men
Pingback: best available ways to treat fleas on dog
Pingback: Agriculture Drone Companies
Pingback: home remedies to get rid of fleas on dogs
Pingback: Treating dog fleas
Pingback: Through-Wall Radar
Pingback: Thermal Camera
Pingback: myths about fleas
Pingback: Top home remedies to get rid of fleas on dogs
Pingback: Radar Detector
Pingback: Anti-Drone Weapons
Pingback: treat fleas on dog| home flea treatment for dogs
Pingback: best flea and tick control kits
Pingback: flea and tick prevention treatment for dogs
Pingback: EasyDefense Ultimate dog flea and tick
Pingback: getting fleas off your dog| science of the flea lifecycle
Pingback: Unmanned Surface Boat
Pingback: effective ways of getting fleas off dog
Pingback: natural flea and tick review
Pingback: mouth mask black
Pingback: gel padding material
Pingback: Gustavo de Aristegui
Pingback: hepa face masks
Pingback: Night Version Camera
Pingback: Thermal Camera
Pingback: Anti-drone System
Pingback: how to reduce leg fat
Pingback: Explosion Proof Camera
Pingback: Agricultural Drone
Pingback: Agricultural Drone
Pingback: posture corrector extra large
Pingback: posture corrector camp ben
Pingback: arch support wraps
Pingback: how to reduce leg fat
Pingback: arch support wraps
Pingback: posture corrector office
Pingback: gel pad ball of foot cushions
Pingback: medical wrist brace
Pingback: elastic foot support
Pingback: forefoot cushion
Pingback: pad for pain
Pingback: safety mask pink
Pingback: Night Version Camera
Pingback: Agricultural Drone
Pingback: Thermal Camera
Pingback: Agriculture Drone Companies
Pingback: Explosion Proof Camera
Pingback: Explosion Proof Camera
Pingback: Agriculture Drone Companies
Pingback: Night Version Camera
Pingback: Radar Detector
Pingback: Explosion Proof Camera
Pingback: Explosion Proof Camera
Pingback: Anti-drone System
Pingback: Thermal Camera
Pingback: Radar Detector
Pingback: Casa98
Pingback: garbage dumpster rental prices
Pingback: dumpster rental douglasville
Pingback: garbage bin rental
Pingback: search psychic
Pingback: rent dumpster
Pingback: tarot reader
Pingback: garbage dumpsters rentals
Pingback: roll off dumpster service
Pingback: psychic reading
Pingback: consultant
Pingback: spirituality
Pingback: dumpsters to rent
Pingback: psychic reader
Pingback: open top dumpster rental
Pingback: Gaming
Pingback: Homesteading
Pingback: roll off containers for sale
Pingback: waste management dumpster rental prices
Pingback: Homestead tessie
Pingback: trash bin
Pingback: disposal bin rental
Pingback: The Life Of Scott
Pingback: Top Youtuber
Pingback: Vlogs
Pingback: Youtube
Pingback: construction debris dumpster
Pingback: need a dumpster
Pingback: Facebook
Pingback: Top Youtuber
Pingback: Wengertime89
Pingback: waste management dumpster service
Pingback: The Life Of Scott
Pingback: Facebook Page
Pingback: construction waste dumpster rental
Pingback: construction roll off dumpsters
Pingback: roll off trash dumpster
Pingback: Wengertime89
Pingback: Homestead tessie
Pingback: dumpster rental romulus
Pingback: dumpster rental grand rapids
Pingback: Videos
Pingback: Youtube
Pingback: dumpster rental owosso
Pingback: Vlogs
Pingback: Top Youtuber
Pingback: i need to rent a dumpster
Pingback: dumpster cost
Pingback: local dumpster rental
Pingback: rent a dumpster cost
Pingback: rolling dumpster
Pingback: Anna university Results 2018
Pingback: refuse container rental
Pingback: 30 yard roll off dumpster
Pingback: dumpster for sale
Pingback: dumpster rental bingham farms
Pingback: Office movers in Virginia
Pingback: dumpster rental huron charter twp
Pingback: dumpster rental algonac
Pingback: cost to rent a dumpster
Pingback: rent a trash dumpster
Pingback: roll off dumpster service
Pingback: cost of dumpster
Pingback: all waste dumpster
Pingback: commercial dumpster sizes
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B0050GK5AO/Rubber-piping-for-shim-slotted-in-black-for-KR.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00YUSET50/Simple-Kind-to-Skin-Micellar-Cleansing-Wipes-25-wipes-Pack-of-3-75-Wipes.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00B5OL28Y/Paul-Lamond-Laser-Maze-Game.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00K6IF5D8/1000-Mile-Womens-Ultimate-Tactel-Approach-Sock-Comfortable-Fibre-Training.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00QMV9Y4Y/New-Years-Eve-Party-Gold-Photo-Booth-Props-Kit-20-Count.php
Pingback: Spinal Meningitis Symptoms
Pingback: Super Heroes: Suicide Squad
Pingback: Spinal Meningitis
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B006KC6C5Y/Fisherman-love-to-get-their-tackle-out-Socks.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B004QI7NK2/Canon-PG510-CL511-Ink-Cartridges-Value-Pack-Black.php
Pingback: broken iphone screen
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B00GLTZFWC/Tutu-Tulle-Roll-6-x-95-Yards-Spool-Wedding-Craft-Netting-Fabric-Rose-Pink.php
Pingback: Justice League Movie Posters
Pingback: st louis cell phone repair
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B00LLWRL58/Sharpie-1926406-Permanent-Marker-Special-Edition-Pack-Fine-Point-Pack-of-23-Assorted.php
Pingback: Captain America Movie Posters
Pingback: Superman Movie Posters
Pingback: Suicide Squad Movie Poster shop
Pingback: fix my device
Pingback: Wonder Woman Movie Poster shop
Pingback: www.underbrand.co.uk/p/Cables/detail/B0076W9Q4Q/Corsair-CMXS8GX3M1A1600C10-8GB-Vengeance-Performance-So-Dimm-1600MHz-CL10-DDR3-Memory-Module.php
Pingback: termites
Pingback: liver cancer
Pingback: diabetes
Pingback: mouth surgery
Pingback: www.underbrand.co.uk/p/Cables/detail/B004TPN978/Monster-High-Hair-Studio.php
Pingback: www.underbrand.co.uk/p/Cables/detail/B004XKWN3A/Derbystar-Prestige-Short-Sleeved-Mens-Jersey.php
Pingback: Incredible Hulk Movie Posters
Pingback: passive income ideas
Pingback: st louis cell phone repair
Pingback: www.underbrand.co.uk/p/Cables/detail/B00SRIKSGI/The-Eye-Mask-A-Hot-Eye-Compress-Heat-Bag-for-Dry-Eye-Blepharitis-MGD-and-other-eye-conditions.php
Pingback: Daredevil Mugs
Pingback: mlm prospecting tips
Pingback: how to make money on the internet
Pingback: good online business ideas
Pingback: The Flash Mugs
Pingback: www.underbrand.co.uk/p/Cables/detail/B00VI8DVF4/Walt-Disney-Alice-in-Wonderland-Smile-Pyjamas-black.php
Pingback: www.underbrand.co.uk/p/Cables/detail/B0161H1O8W/FENCE-WALL-SPIKE-PACK-1M-BIRD-PIGEON-REPELLER-DETERRENT-WINDOW-DEFENDER-SECURITY.php
Pingback: Spiderman Mugs
Pingback: www.underbrand.co.uk/p/Cables/detail/B00QZLY54U/Tamaris-Womens-25216-Unlined-chukka-boots-short-length.php
Pingback: mlm sponsoring
Pingback: www.underbrand.co.uk/p/Cables/detail/B014IQ916U/PacaPod-Idaho-Marine-Lite-Designer-Baby-Changing-Bag-Luxury-Lightweight-Blue-Hobo-3-in-1-Organising-System.php
Pingback: online business opportunities
Pingback: www.underbrand.co.uk/p/Cables/detail/B01IFANZ58/Humphrey-Searle-Symphonies-Nos-3-Venetian-No5-Zodiac-Variations-for-Small-Orchestra-Op53-Labyrinth-for-Orchestra-Op56.php
Pingback: fix my iphone st louis
Pingback: www.underbrand.co.uk/p/Comfort-Bikes/detail/B014J5XU1M/Viga-2-in-1-Wooden-3D-Alphabet-Numbers-Turtle-Puzzle.php
Pingback: Wonder Woman Mugs for sale
Pingback: www.underbrand.co.uk/p/Cables/detail/B01JLYOFKG/Hieha-Q-Box-Android-51-Smart-TV-BOX-Amlogic-S905-Streaming-Media-Player-2GB-16GB-4K-Wifi-Bluetooth-XBMC-KODI-Quad-Core-Speed.php
Pingback: www.underbrand.co.uk/p/Comfort-Bikes/detail/B006E87JA6/David-Mason-Design-Majestic-HIS-LORDSHIP-Tankard-Mug.php
Pingback: Green Lantern Cup shop
Pingback: Lenny Pozner
Pingback: Batman Cups
Pingback: www.underbrand.co.uk/p/Greases/detail/B009Z73KYW/Isotoner-Womens-Popcorn-Secret-Sole-Open-Toe-Mule-Slippers.php
Pingback: www.underbrand.co.uk/p/Gloves/detail/B00SUB67F8/komforthaus-Radiator-Thermostat-Comet-Blue-Programming-via-Smartphone-or-Tablet-Bluetooth-connection-Made-in-Germany.php
Pingback: fix my phone
Pingback: www.underbrand.co.uk/p/Greases/detail/B000ANDBE4/Volume-8-The-Decca-Years.php
Pingback: The Flash T-shirts
Pingback: www.underbrand.co.uk/p/Mens/detail/B0001P0UJU/Town-Country-Medium-Premium-Heavy-Duty-Gauntlet-Gardening-Gloves.php
Pingback: Guardians of the Galaxy T-shirt shop
Pingback: Superman T-shirt shop
Pingback: Supergirl T-shirt shop
Pingback: www.underbrand.co.uk/p/Mens/detail/B000SHSOSK/Rexel-Agenda2-Eco-Friendly-Letter-Tray-A4-Charcoal.php
Pingback: www.underbrand.co.uk/p/Mens/detail/B009VHUZ7Q/Portwest-S460YERL-Hi-Vis-Traffic-Jacket-with-concealed-hood.php
Pingback: www.underbrand.co.uk/p/Mens/detail/B0046GDU8S/Fazer-School-Chalks-440g.php
Pingback: Volet roulant en algerie
Pingback: www.underbrand.co.uk/p/Mens/detail/B0136CAITG/Xinhenchen-Caro-Solar-Powered-Bike-Cycle-Clip-On-Back-Rear-Tail-Light-Bicycle-Safety-LED-Rear-Tail-Lamp.php
Pingback: Daredevil T-shirts for sale
Pingback: samsung screen repair
Pingback: Justice League T-shirts
Pingback: www.underbrand.co.uk/p/Mens/detail/B01IF2W24Q/Hunkydory-The-Essential-Book-Of-Christmas-Sentiments-2016.php
Pingback: Spiderman T-shirt shop
Pingback: Wolverine Toy shop
Pingback: Volet roulant en algerie
Pingback: Amenagement interieur en algerie
Pingback: fix my device
Pingback: Thor Toys
Pingback: Construction metallique en algerie
Pingback: Spiderman Toys for sale
Pingback: Verres et vitrage en algerie
Pingback: samsung screen repair
Pingback: Construction metallique en algerie
Pingback: Menuiserie aluminium en algerie
Pingback: Volet roulant en algerie
Pingback: fix my iphone st louis
Pingback: samsung screen repair
Pingback: fastest phone repair
Pingback: top 40 songs this week uk
Pingback: cracked iphone screen
Pingback: uk top 40 pop
Pingback: Creación de apps
Pingback: Creación de apps
Pingback: cracked samsung screen
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/1910536768/James-Hunt.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B007XTE6YW/Pro-Ject-Debut-Carbon-Premium-WITH-Ortofon-2M-RED-Turntable.php
Pingback: brain tumor
Pingback: truthers
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00LVVHO8S/Nike-Brasilia-6-Duffel-Bag.php
Pingback: Lamb Handbag
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/0091933145/I-Never-Knew-That-About-the-Lake-District.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B004I5BQ1K/Masterplug-Indoor-Power-BSG3-MS-6-Gang-13-amp-Socket-with-3-m-Extension-Lead-White.php
Pingback: Water Distiller USA
Pingback: Natural Crossbody
Pingback: Saftey Razor
Pingback: Series 3
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B00O25BZK8/Sew-Cool-Fashion-Kit.php
Pingback: Broadband Service Provider in Punjab
Pingback: Custom Passport
Pingback: Buy Water Distiller
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B016BQTCFU/Palio-Expert-2-Table-Tennis-Bat-Case.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/1907598405/The-Twelve-Poems-of-Christmas-Volume-8.php
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B01B5IFU3W/Haichen-24W-Real-Grow-Light-120-Degree-LED-Grow-Light-Bulbs-for-Greenhouse-Bonsai-and-Hydroponic-Garden-Full-Spectrum-Indoor-Garden-Growing-Lamps-with-Wide-Area-Coverage.php
Pingback: Handstitched wallet
Pingback: Field Notes
Pingback: Keychain
Pingback: www.underbrand.co.uk/p/Bike-Accessories/detail/B00969IIIC/Twinings-fresh-fruity-Strawberry-Mango-20-tea-bags.php
Pingback: NDA Coaching in Chandigarh
Pingback: www.underbrand.co.uk/p/Base-Layers/detail/B01CQ99L16/Ski-Gloves-Hicool-Waterproof-Thermal-Winter-Ski-Gloves-Snowboard-Snowmobile-Motorcycle-Cycling-Outdoor-Sports-Gloves-Mens.php
Pingback: www.underbrand.co.uk/p/Bike-Frames/detail/B01MCRGFQC/Star-Wars-Advent-Calendar-Stormtrooper-with-24-festive-Milk-Chocolate-shapes.php
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/1473646480/Ginos-Hidden-Italy-How-to-cook-like-a-true-Italian-discover-the-recipes-the-Italians-really-eat.php
Pingback: www.underbrand.co.uk/p/Bike-Fenders/detail/B00S1GMVZ2/Arebos-Glass-Ceramic-Hob-Vitroeramic-Built-in-Hob-Self-sufficient-Sensor-Touch-4-Cooking-Zones.php
Pingback: www.underbrand.co.uk/p/Bike-Frames/detail/B00ODVI8R4/EasyAcc-Ultra-Slim-iPad-Air-2-Smart-Case-Cover-with-Stand-Auto-Sleep-Wake-up-for-Apple-iPad-Air-2-iPad-6-Top-Premium-PU-Leather-Folded-Cover-Design-Black.php
Pingback: www.underbrand.co.uk/p/Bike-Accessories/detail/B0047ETODO/Loreal-eversleek-humidity-defying-leave-in-hair-creme-6-oz.php
Pingback: Leather Care
Pingback: handmade wallet
Pingback: www.underbrand.co.uk/p/Adult-Helmets/detail/B01LY1JDWH/Sven-Vth-in-the-Mix-The-Sound-Of-The-17th-Season.php
Pingback: Designer Tote
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B000ZDME7Y/Perler-Bead-Jar-Multi-Colour.php
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B001AZ3SOE/Honeywell-HT-216E-Oscillating-Table-Fan-12-inch-Chrome.php
Pingback: www.underbrand.co.uk/p/Arm-Warmers/detail/B00AEXZHCY/Toronto-Charcoal-BBQ-Grill-With-Side-Table.php
Pingback: new homes builder in charlotte nc
Pingback: www.underbrand.co.uk/p/Bike-Lighting/detail/B019V8GAPA/Scabies-Treatment-Mites-Pubic-Lice-Parasites-Cream-Lotion-60g-An-Effective-48-Hours-Treatment-agaist-Scabies-100-Satisfaction-Guaranteed-1-x-60g.php
Pingback: best custom home builders in charlotte nc
Pingback: bathroom remodel builder charlotte nc
Pingback: custom home builder in charlotte nc
Pingback: home builder in charlotte nc
Pingback: Leather Card Holder
Pingback: www.underbrand.co.uk/p/Cables/detail/B000LFYOX8/Silverline-675068-Decking-and-Flooring-Installation-Tool-600-mm.php
Pingback: www.underbrand.co.uk/p/Brakes/detail/B01ICXZECK/ANMER-Settled-Base-CS-662-Vegetable-SlicerGraterShredder-Cheese-Cutter-Professional-Vegetable-Salad-Shooter.php
Pingback: Saftey Razor
Pingback: men's wallet
Pingback: kitchen and bath remodeling builder in charlotte
Pingback: www.underbrand.co.uk/p/Cables/detail/B0016KVU7U/Striped-Birthday-Candles-in-Holders-Assorted-Pack-of-20.php
Pingback: Natural Beeswax Balm
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B00P1802RW/Duronic-DM35V2X1-Double-Twin-LCD-LED-Vertical-Desk-Mount-Arm-Monitor-Stand-Bracket-with-Tilt-and-Swivel-Tilt-15Swivel-180Rotate-360-10-Year-Warranty.php
Pingback: www.underbrand.co.uk/p/Bikes/detail/B005FYNT3G/SanDisk-SDCZ50-B35-32-GB-Cruzer-Blade-USB-20-Flash-Drive-Black.php
Pingback: Series 1
Pingback: www.underbrand.co.uk/p/Bike-Stabilisers/detail/B00A1LGNIG/Home-Alone-Home-Alone-2-Lost-in-New-York-Double-pack-DVD-1990.php
Pingback: www.underbrand.co.uk/p/Bike-Pump-Accessories/detail/B00YX2PCSG/PM-Rainbow-SWAROVSKI-ELEMENTS-Crystal-Rose-Gold-Plated-Women-Jewellery-Set-Necklace-Earrings.php
Pingback: www.underbrand.co.uk/p/Cables/detail/B000005CEU/6-Feet-Deep.php
Pingback: www.underbrand.co.uk/p/Bikes/detail/B01LEZ3DJO/Exposed-VINYL.php
Pingback: www.underbrand.co.uk/p/Cables/detail/B0002DUPZU/Ernie-Ball-2148-Earthwood-Phosphor-Bronze-Light-11-52-Set.php
Pingback: Womens Leather Tote
Pingback: www.underbrand.co.uk/p/Brakes/detail/B01CVKB47O/Fischer-Alpine-Eco-Unisex-Boot-Helmet-Bag.php
Pingback: www.underbrand.co.uk/p/Bike-Seats/detail/B015915H0W/spraying-spray-nozzles-tips-total-of-8-nozzles-110-Flat-fan-Defletor-nozzles-tips-One-of-each-colour-or-MIX-AND-MATCH-perfect-set-for-knapsack-spraying-weed-killing-etc.php
Pingback: Lip Balm
Pingback: luxury handbag
Pingback: Buy Water Distiller
Pingback: Leather Mens Shaving
Pingback: Buy Water Distiller
Pingback: Home Water Distiller
Pingback: Women's Crossbody
Pingback: Water Distiller Canada
Pingback: Leather Bags
Pingback: Survival Kit
Pingback: Handmade in the USA
Pingback: villa for sale in uae
Pingback: free download Physics games for windows full
Pingback: free download football games for windows full
Pingback: free download food games for windows full
Pingback: audi
Pingback: Honda
Pingback: free download Cooking games for windows full
Pingback: online octane
Pingback: Pokershop Sachsen-Anhalt
Pingback: ford
Pingback: koenigsegg
Pingback: audi
Pingback: pokerkoffer 300 chips kaufen
Pingback: Pokerzubehör Mecklenburg-Vorpommern
Pingback: free download Power Rangers games for windows full
Pingback: free download small games for windows full
Pingback: car blog
Pingback: Bathroom Remodeling
Pingback: Kitchen Remodelingl
Pingback: Pokerzubehör Baden-Württemberg
Pingback: free download mind games for windows full
Pingback: free download video games for windows full
Pingback: jaguar
Pingback: free download indie games for windows full
Pingback: ford
Pingback: free download Classic games for windows full
Pingback: performance cars
Pingback: performance cars
Pingback: Trick to Unlock your Smartphone
Pingback: A Simple Way to Earn Money Online
Pingback: free download action games for pc
Pingback: car pictures
Pingback: koenigsegg
Pingback: free download Princess games for pc
Pingback: Honda
Pingback: car blog
Pingback: audi
Pingback: free download mind games for windows
Pingback: Remodeling Services
Pingback: fast cars
Pingback: Free Estimate
Pingback: lamborghini
Pingback: ferrari
Pingback: Flipkart Big Shopping Days offer
Pingback: Best Offers on Arrow Jeans
Pingback: free download Classic games for windows
Pingback: free download animal games for windows
Pingback: online octane
Pingback: car news
Pingback: free download Detective games for windows
Pingback: Escort Annonces
Pingback: free download arcade games for windows
Pingback: car forum
Pingback: free download bowling games for windows
Pingback: car forum
Pingback: sypany caj
Pingback: audi
Pingback: bmw
Pingback: sports cars
Pingback: online octane
Pingback: car reviews
Pingback: car news
Pingback: fast cars
Pingback: ferrari
Pingback: car forum
Pingback: polarized sunglasses
Pingback: Honda
Pingback: jaguar
Pingback: car reviews
Pingback: performance cars
Pingback: matrace za nejlepsi cenu
Pingback: lamborghini
Pingback: car pictures
Pingback: fast cars
Pingback: egypt holidays 2017
Pingback: egypt best travel agency 2018
Pingback: online octane
Pingback: egypt tours
Pingback: egypt packages
Pingback: egypt flight ticket
Pingback: egyptian pyramids
Pingback: my amazon
Pingback: egypt holiday today
Pingback: egypt package from france
Pingback: intravenous vitamin c
Pingback: buy cbd oil
Pingback: vitamins cancer
Pingback: supplements cancer
Pingback: buy iv vitamin c
Pingback: alternative therapy cancer
Pingback: Artisan General
Pingback: Remodeling Services
Pingback: videos teds woodworking
Pingback: teds woodworking deck plans
Pingback: Download Aadhaar Card Online
Pingback: Amazon shopping Offers
Pingback: online octane
Pingback: teds woodworking spam
Pingback: teds woodworking free pdf
Pingback: performance cars
Pingback: car blog
Pingback: audi
Pingback: online octane
Pingback: koenigsegg
Pingback: car news
Pingback: ford
Pingback: car forum
Pingback: bmw
Pingback: car forum
Pingback: performance cars
Pingback: car news
Pingback: ferrari
Pingback: online octane
Pingback: audi
Pingback: ford
Pingback: sports cars
Pingback: BJJ GI
Pingback: car pictures
Pingback: bmw
Pingback: sports cars
Pingback: car blog
Pingback: online octane
Pingback: koenigsegg
Pingback: sports cars
Pingback: lamborghini
Pingback: Honda
Pingback: lamborghini
Pingback: audi
Pingback: car news
Pingback: sports cars
Pingback: bmw
Pingback: SBG IRELAND
Pingback: Dell Support
Pingback: car reviews
Pingback: microsoft support
Pingback: webroot install
Pingback: yahoo support
Pingback: freelance programer
Pingback: Svenson Mexico
Pingback: EXAM ROOM PACKAGES
Pingback: handpiece
Pingback: online diamonds
Pingback: loose diamonds wholesale
Pingback: Services
Pingback: Sell
Pingback: Rent
Pingback: Nashville newborn photographer
Pingback: laser treatment acne
Pingback: pakistani suits
Pingback: laser treatment acne scar
Pingback: acne laser scar removal cost
Pingback: Bathroom Remodels
Pingback: back acne laser treatment
Pingback: Fireplace fire place countertop
Pingback: laser treatment for acne and scars
Pingback: Customized Countertops
Pingback: Nashville wedding photographers
Pingback: acne scars laser treatment
Pingback: how much is laser treatment for acne
Pingback: jualvapor
Pingback: Fireplace fire place countertop
Pingback: does laser acne treatment work
Pingback: Marble and granite fabricators
Pingback: acne scar laser treatment before and after pictures
Pingback: Fire Pit countertop
Pingback: laser acne scar removal cost
Pingback: fraxel laser acne scars before after
Pingback: how to tighten skin
Pingback: Murfreesboro newborn photographers
Pingback: body skin tightening
Pingback: best way to tighten skin
Pingback: how to tighten loose breast skin naturally
Pingback: how to tighten skin on arms
Pingback: how can i tighten the skin on my stomach
Pingback: tighten sagging skin on arms
Pingback: tighten skin under chin without surgery
Pingback: can loose skin be tightened without surgery
Pingback: leg skin tightening
Pingback: Drone Schools
Pingback: tighten the skin
Pingback: Nashville wedding photography
Pingback: radiofrequency facial rejuvenation
Pingback: Phone Display
Pingback: Quad Copter
Pingback: Murfreesboro newborn photographers
Pingback: rejuvenate facial treatments
Pingback: Photographers Dream
Pingback: lip enhancement reviews
Pingback: rejuvenate facial treatments
Pingback: Multi Collagen Protein Powder
Pingback: bad lip enhancement
Pingback: non surgical upper eye lift
Pingback: what is photo rejuvenation facial
Pingback: how to enhance lips
Pingback: BODYBUILDING COACH
Pingback: london cryptocurrency
Pingback: rukavniky
Pingback: conception site web
Pingback: excel to tally ram
Pingback: excel to tally bank entry
Pingback: excel to tally data export utility youtube
Pingback: excel to tally erp 9 software free download
Pingback: how to export tally address to excel
Pingback: excel to tally converter software
Pingback: excel formula to tally words
Pingback: export to excel from tally 7.2
Pingback: technology
Pingback: excel to tally 9 import
Pingback: excel to tally 9 import
Pingback: excel to tally erp 9 software free download
Pingback: yalla shoot
Pingback: valentus slimroast cocoa
Pingback: slimroast hot chocolate
Pingback: online shop
Pingback: Website design
Pingback: valentus slimroast cocoa
Pingback: commercial gym equipment manufacturers
Pingback: slimroast cocoa
Pingback: multi gym equipment
Pingback: seo
Pingback: kids gym equipment
Pingback: discount gym equipment
Pingback: fitness watches for sale
Pingback: gym equipment names
Pingback: fit and fresh ice packs
Pingback: pro gym equipment
Pingback: fit and fresh ice packs
Pingback: gym equipment machines
Pingback: new gym equipment
Pingback: kooora
Pingback: fitness watches for women
Pingback: gym equipment machines
Pingback: home gym equipment
Pingback: gym equipment names
Pingback: pro gym equipment
Pingback: SUPREME BOX LOGO HOODIE
Pingback: multi gym equipment
Pingback: full gym equipment price
Pingback: ADIDAS X BAPE JACKET
Pingback: SUPREME X CHAMPION BOX LOGO
Pingback: LOUIS VUITTON X SUPREME SWEATER
Pingback: fitness watches for sale
Pingback: SUPREME X THE NORTH FACE JACKET
Pingback: gym clothing lines
Pingback: SUPREME X THE NORTH FACE JACKET
Pingback: home gym equipment
Pingback: Lean Belly Breakthrough
Pingback: Projektowanie Stron Internetowych
Pingback: Webdesign
Pingback: Webdesign
Pingback: NSAPorn
Pingback: 7 chakra bracelet meaning and benefits
Pingback: www.chakrabracelet.net
Pingback: how to open your 7 chakras
Pingback: 7 chakras
Pingback: Smoking pipes india
Pingback: Escorts Directory
Pingback: porta e janela de vidro
Pingback: tipos de cercas
Pingback: Rijschool Stolwijk
Pingback: cerca de segurança para muro
Pingback: muros residenciais bonitos
Pingback: Rijschool Nieuwerkerk a/d IJssel
Pingback: imagens de muros de casas
Pingback: significado da palavra caracteristica
Pingback: cerca de proteção para muros
Pingback: Pantana Rainforest
Pingback: diâmetro
Pingback: cerca de serpentina
Pingback: galvanizado significado
Pingback: arame concertina
Pingback: concertina com
Pingback: concertina com
Pingback: muros modernos e baratos
Pingback: preço de arame farpado
Pingback: seguranca casa
Pingback: Goedkope Rijschool Rotterdam
Pingback: o que é aço
Pingback: empenas
Pingback: Play Antakshari on Your Phone
Pingback: concertina perimetral
Pingback: cerca para muro
Pingback: grade para janela de vidro
Pingback: caco de vidro no muro
Pingback: Drone Photography
Pingback: Play Antakshari on Your Phone
Pingback: cerca eletrica uberaba
Pingback: portas modernas para sala
Pingback: Play Antakshari on Your Phone
Pingback: Lets Antakshri - Test your Bollywood Music Knowledge with Friends
Pingback: Lets Antakshri - Test your Bollywood Music Knowledge with Friends
Pingback: dicas de segurança pessoal
Pingback: concertina goiania
Pingback: sobre a violencia no brasil
Pingback: porta da frente de madeira
Pingback: Play Antakshari on Your Phone
Pingback: Lets Antakshri - Test your Bollywood Music Knowledge with Friends
Pingback: Play Antakshari on Your Phone
Pingback: grade de arame
Pingback: formas e cortantes
Pingback: estilos de muros
Pingback: grade residencial
Pingback: instalação de concertina
Pingback: Play Antakshari on Your Phone
Pingback: concertina
Pingback: qual é o significado de
Pingback: grades de segurança para portas
Pingback: modelo de muro com grade
Pingback: conceito de segurança patrimonial
Pingback: aço enferruja
Pingback: as cidades mais violentas do mundo
Pingback: cerca aspiral
Pingback: rede para alambrado
Pingback: cerca de proteção para muros
Pingback: estilos de muros
Pingback: grade de proteção para porta de vidro
Pingback: video instalação
Pingback: casas com grades bonitas
Pingback: cerca consertina
Pingback: modelo de porta e janela
Pingback: Gaming Mouse
Pingback: barreiras de segurança
Pingback: Gaming Headphones
Pingback: Gaming Headphones
Pingback: tela para cercado
Pingback: Gaming Collections
Pingback: Smart Watches
Pingback: proteção residencial
Pingback: Bluetooth Speakers
Pingback: Combobreakergne home
Pingback: Gaming Accessories
Pingback: Smart Watches
Pingback: Gaming Accessories
Pingback: hosted ecommerce platforms
Pingback: how to start internet business in india
Pingback: multi vendor ecommerce script
Pingback: concretina
Pingback: ecommerce web development company india
Pingback: GREECE ESCORTS
Pingback: Wedding Car Hire Leicester
Pingback: Nudge japan
Pingback: Behavior design Colorado
Pingback: freelance 3d
Pingback: Offline behavior
Pingback: behavior design team
Pingback: Adfærdsdesign
Pingback: guzzlord,1,1,100%,16
Pingback: man with a van sutton in Ashfield
Pingback: fantasy football news,1,1,100%,28
Pingback: super bowl parties 2018,1,1,100%,2
Pingback: Anti Wrinkle Injections Leicester
Pingback: empty seats galore week 13,1,12,8.33%,4.6
Pingback: nick caserio,2,2,100%,2
Pingback: super bowl playoff predictions,1,4,25%,66
Pingback: marshawn lynch no script ep 8,1,5,20%,7.6
Pingback: designing behavior
Pingback: Choice architecture spain
Pingback: gedragsontwerp
Pingback: super bowl 2018 predictions,11,57,19.30%,19
Pingback: behavior design expert
Pingback: Behavior design
Pingback: dakota johnson and chris martin,1,1,100%,140
Pingback: Behavioral design consultancy
Pingback: nfl wild card 2018,0,5,0%,39
Pingback: Nudging Denver
Pingback: super bowl power rankings,1,7,14.29%,51
Pingback: Choice architecture sweden
Pingback: TM Express Inc
Pingback: jt barrett injury,1,1,100%,2
Pingback: Choice architecture seoul
Pingback: you
Pingback: madden 18 spread scheme,1,3,33.33%,27
Pingback: Choice architecture Netherland
Pingback: mmmx,0,1,0%,98
Pingback: madden 17 connected franchise draft,0,1,0%,71
Pingback: Nudging India
Pingback: Nudge sydney
Pingback: eating behavior
Pingback: Choice editing IL
Pingback: Financial decision making
Pingback: Behavior design
Pingback: dwayne allen patriots,0,1,0%,4
Pingback: kevin carter espn,0,3,0%,19
Pingback: design thinking
Pingback: Nudge London
Pingback: wilton speight,0,3,0%,84
Pingback: rams vs patriots super bowl,0,1,0%,61
Pingback: Choice architecture consultant
Pingback: ben roethlisberger fantasy,0,1,0%,94
Pingback: 1992 kansas city chiefs,0,1,0%,55
Pingback: jace norman,0,1,0%,100
Pingback: Choice architecture TX
Pingback: carolina panthers schedule,0,1,0%,100
Pingback: super bowl halftime show,0,20,0%,140
Pingback: Behavior design hong kong
Pingback: Choice architecture firm
Pingback: paul richardson football,0,1,0%,85
Pingback: taysom hill,0,7,0%,81
Pingback: eyeshield 21 wiki,0,1,0%,45
Pingback: Biographien bekannter Pokerspieler wie Phil Ivey
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Poker Strategie Dein Pokerspiel verbessern
Pingback: organic instagram growth
Pingback: Poker Strategie Dein Pokerspiel verbessern
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Poker Glossar Erklarung der wichtigsten Pokerfachbegriffe
Pingback: Behavior design Mumbai
Pingback: instagram auto follower
Pingback: instagram auto follower
Pingback: Poker Glossar Erklarung der wichtigsten Pokerfachbegriffe
Pingback: Poker Strategie Dein Pokerspiel verbessern
Pingback: Biographien bekannter Pokerspieler wie Phil Ivey
Pingback: Pokerregeln zu allen Poker Varianten
Pingback: instagram scheduler
Pingback: Poker Strategie Dein Pokerspiel verbessern
Pingback: Poker Hand Ranking Reihenfolge und Wertigkeit der Pokerhande
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Poker-Nachrichten News aus der Pokerwelt
Pingback: organic instagram growth
Pingback: instagram bot
Pingback: gain instagram followers
Pingback: Gute deutsche Pokerbücher von Harrington Sklansky Moorman
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Pokerregeln zu allen Poker Varianten
Pingback: Poker Glossar Erklarung der wichtigsten Pokerfachbegriffe
Pingback: Pot Limit Omaha Anleitung für Anfanger und Einsteiger PLO lernen
Pingback: Poker-Nachrichten News aus der Pokerwelt
Pingback: Biographien bekannter Pokerspieler wie Phil Ivey
Pingback: Biographien bekannter Pokerspieler wie Phil Ivey
Pingback: instagram scheduler
Pingback: grow instagram
Pingback: real instagram followers
Pingback: grow instagram
Pingback: instagram likes
Pingback: instagram auto liker
Pingback: Tbilisi Virtual Office
Pingback: cost to rent a dumpster
Pingback: grow instagram
Pingback: instagram followers
Pingback: instagram scheduler
Pingback: instagram auto follower
Pingback: trash dump
Pingback: instagram followers
Pingback: dumpster rental Winter Haven
Pingback: grow instagram
Pingback: Movers and Packers
Pingback: Lakeland Dumpster Rental
Pingback: grow instagram
Pingback: yard waste removal
Pingback: junk bin
Pingback: grow instagram
Pingback: real instagram followers
Pingback: daÅový odklad
Pingback: dumpster trash
Pingback: instagram likes
Pingback: residential dumpster service
Pingback: get a dumpster
Pingback: 10 yard dumpster rental
Pingback: affordable dumpster rental
Pingback: construction container rental
Pingback: hunks hauling junk
Pingback: 5 yard dumpster rental
Pingback: dumpers for rent
Pingback: roll off trash containers
Pingback: construction waste dumpster
Pingback: residential dumpsters for rent
Pingback: February Birthstone
Pingback: rollaway dumpster
Pingback: waste management dumpster
Pingback: Peridot
Pingback: roll off dumpster prices
Pingback: donate your car today
Pingback: August Birthstone
Pingback: dumpster central
Pingback: vehicle donation to charity
Pingback: donate automobile to charity
Pingback: garbage dumpster sizes
Pingback: car to
Pingback: dumpster containers
Pingback: charity for cars
Pingback: donating car to charity tax deduction 2015
Pingback: household junk removal
Pingback: Opal Bracelet
Pingback: how to donate car to goodwill
Pingback: how much tax deduction for car donation
Pingback: rent a garbage bin
Pingback: how can i get a car donated to me
Pingback: Birthstone Jewelry
Pingback: how to donate vehicle
Pingback: get a car donated to you
Pingback: dumpster rental Plymouth
Pingback: 30 yard dumpster
Pingback: Roll-off Dumpster Rental of San Diego
Pingback: rolloff dumpsters
Pingback: residential dumpster service
Pingback: dumpsters to rent
Pingback: construction debris dumpster
Pingback: 10 yard dumpster rental price
Pingback: affordable dumpster rental
Pingback: affordable dumpsters
Pingback: residential dumpster service
Pingback: garbage dumpsters for rent
Pingback: 5 yard dumpster
Pingback: construction waste disposal
Pingback: rollaway dumpster
Pingback: commercial dumpster service
Pingback: 30 yard dumpster cost
Pingback: 15 yard dumpster rental
Pingback: rollaway dumpster rental
Pingback: dumpster sizes 10 yard
Pingback: waste dumpster sizes
Pingback: waste disposal bins
Pingback: 30 yard dumpster cost
Pingback: dirt dumpster
Pingback: furniture disposal
Pingback: trash pick up services
Pingback: dumpster rental Dunwoody
Pingback: garbage bin rental
Pingback: car donation tax write off
Pingback: donate vehicle to charity
Pingback: dumpster rental lawrenceville
Pingback: trash dumpsters
Pingback: where to donate a car
Pingback: donate a car for cash
Pingback: dumpster rental Rosewell
Pingback: dumpster rental Austell
Pingback: roll off
Pingback: donate truck to charity
Pingback: give my car to charity
Pingback: trash dumpster sizes
Pingback: where to get a donated car
Pingback: garbage dumpster rental
Pingback: donate automobile to charity
Pingback: garbage pickup
Pingback: cars for kids charity
Pingback: where to donate old cars
Pingback: dumpsters near me
Pingback: dumpster removal
Pingback: npr donate a car
Pingback: charities that take cars for donation
Pingback: donate junk car tax deduction
Pingback: rv donation
Pingback: big dumpster
Pingback: 20 yard dumpster dimensions
Pingback: car tax deduction
Pingback: donatea
Pingback: trash removal dumpster rental
Pingback: rent a dumper
Pingback: blog list trust 2018
Pingback: home dumpster service
Pingback: where to rent a trash dumpster
Pingback: where to rent a trash dumpster
Pingback: Download Videos
Pingback: Nudging Seto
Pingback: Choice editing adelaide
Pingback: Nudge pa
Pingback: Behavior design seoul
Pingback: Choice architecture Stockholm
Pingback: wydnd
Pingback: Lifestyle
Pingback: Nudging designers
Pingback: Habit change
Pingback: consumer decisions
Pingback: Nudging Amsterdam
Pingback: Behavior design pa
Pingback: Choice architecture Stockholm
Pingback: Behavioral design
Pingback: Choice architecture Switzerland
Pingback: design services
Pingback: Choice architecture china
Pingback: Behavior change turkey
Pingback: Masterclass i nudging
Pingback: Titanium Backup Pro Apk
Pingback: Titanium Backup Pro Apk
Pingback: shiatsu massage chair
Pingback: Best ghost producers
Pingback: best full body massage chair review
Pingback: Graphic design for DJ
Pingback: shiatsu massage chair review
Pingback: Door hanger Distribution
Pingback: shiatsu massage chair
Pingback: Who is edm producer
Pingback: Work with ghost production edm
Pingback: Vocals for DJs
Pingback: Pamphlet distributors
Pingback: best massage chair
Pingback: Nudging designers
Pingback: best full body massage chair review
Pingback: best massage chair
Pingback: best full body massage chair review
Pingback: best full body massage chair review
Pingback: best massage chair review
Pingback: best massage chair
Pingback: shiatsu massage chair
Pingback: Door hanger Distribution
Pingback: hemstädning vasastan
Pingback: pellet warszawa
Pingback: Print and distribute flyers
Pingback: Pamphlet distribution
Pingback: Wholesale Earphones
Pingback: Original Beats by Dr. Dre urBeats In-Ear Wired Headphones Black Seller Refurbished
Pingback: Wholesale Md818 lightning usb cable
Pingback: Original Beats by Dre iBeats In Ear Headphones v1.0- BLACK- Bulk
Pingback: Original 1M Apple Lightning to USB cable MD818ZM/A
Pingback: Original Beats by Dr. Dre Powerbeats3 Wireless Earphones (Shock Yellow) Sealed
Pingback: Original Beats by Dre UrBeats In Ear Headphones Earphones v1.0-BLACK-Bulk
Pingback: Original Samsung EP-LN920BBEGUS Fast Charging Dual Port Vehicle Charger (Detachable Micro USB and USB-C Cable) Black Bulk
Pingback: Grade 11
Pingback: MCV4U
Pingback: Applied ENG2P
Pingback: Revel Round
Pingback: University Preparation SPH4U
Pingback: University Preparation SBI4U
Pingback: University Preparation SPH4U
Pingback: Pelham Bay Park Round
Pingback: ? ?????????? ?????? ? Bay Area Round
Pingback: Grade 11
Pingback: Academic ENG1D
Pingback: Global Ctr for Academic & Spiritual Life, 238 Thompson St, Grand
Pingback: McCormick Place, 2301 S Lake Shore Dr Chicago Round
Pingback: Bankett- und Eventmanager
Pingback: Human Resources
Pingback: online private school
Pingback: online high school health course
Pingback: online high school programs
Pingback: accredited high school diploma online accepted by colleges
Pingback: 6 MetroTech Center, MakerSpace, Brooklyn Round
Pingback: 3100 Webster Street, San Francisco Round
Pingback: 839 Clay St., Oakland, CA Round
Pingback: Pigott Hall (Bldg. 260) room 252 Round
Pingback: Meets at Union Square (corner of Post and Powell) Round
Pingback: East 16th Road to East 18th Road on Cross Bay Boulevard (in Broad Channel Park) Round
Pingback: Office Tavern & Grill Round
Pingback: distance learning high school diploma
Pingback: 819 Madison Ave, 4C Round
Pingback: 205 Cypress Ave Brooklyn NY Round
Pingback: real online highschool diploma programs
Pingback: 400 Beach Street, Santa Cruz, CA Round
Pingback: 548 West 22nd Street Round
Pingback: Two Sigma, 100 6th Ave, 3rd Fl Round
Pingback: free online college courses for high school students for credit
Pingback: 515 West 26th Street, Floor 2 Round
Pingback: australia top 40 music
Pingback: L'Amico, 849 6th Ave Round
Pingback: 508 West 26th Street, Ground floor and 8th Floor Round
Pingback: 1040 Metropolitan Avenue Round
Pingback: online colleges no high school diploma
Pingback: accredited online diploma
Pingback: Bryant Park Grill, 25 W 40th St Round
Pingback: best online middle schools
Pingback: top 100 australia
Pingback: Rose Theater, Jazz at Lincoln Centers Frederick P. Rose Hall Round
Pingback: 12505 Vista Del Mar Playa del Rey, CA 90293 Round
Pingback: More hints
Pingback: More about the author
Pingback: top 40 music australia
Pingback: top 50 australia
Pingback: Lawn Behind the Track and Field Area (in Pelham Bay Park) Round
Pingback: 1139 Bushwick Ave, Brooklyn, NY 11221 Round
Pingback: More Help
Pingback: 18 9th Avenue New York, NY 10014 Round
Pingback: The Future Perfect Round
Pingback: Our site
Pingback: 64 East 77th Street Round
Pingback: helpful hints
Pingback: Continue
Pingback: Schuss Round
Pingback: Our site
Pingback: NYRR Run Center Round
Pingback: High Line Art Round
Pingback: 300 US-46, Totowa, NJ 07512, Totowa, NJ 07512, United Round
Pingback: Continue
Pingback: Continued
Pingback: Arlo Hotel Nomad Round
Pingback: Tasende Gallery Round
Pingback: Continue
Pingback: Art in General Round
Pingback: Flying University - Robyn C. Spencer: The Women of the Black Panther Party Round
Pingback: Bonuses
Pingback: additional reading
Pingback: next page
Pingback: Ideal Rodespaten
Pingback: Spaten kaufen
Pingback: our website
Pingback: Spatenblatt kaufen
Pingback: Spatenblatt
Pingback: additional reading
Pingback: Doppelfederspaten
Pingback: Spaten Bestseller Amazon
Pingback: Ideal Rode- und Baumschulspaten
Pingback: y movies release on friday
Pingback: u movies means
Pingback: movies coming out in december 2017
Pingback: movies with will smith
Pingback: i movies.net
Pingback: 9 movies on netflix
Pingback: movies 30062
Pingback: movies grand junction
Pingback: f movies 8
Pingback: movies portland maine
Pingback: du an dreamhomeriverside
Pingback: gia ban dreamhome riverside
Pingback: dreamhome riverside quan 8
Pingback: super bowl xlvii
Pingback: home
Pingback: home appraisal
Pingback: super bowl 88
Pingback: magnetic wooden trains
Pingback: super bowl qbs
Pingback: 55printing.com/cheap-color-copies/
Pingback: book cart
Pingback: super bowl venues
Pingback: www.55printing.com/cheap-color-copies
Pingback: FIFA55
Pingback: fifty fiveprinted
Pingback: super bowl qbs
Pingback: FIFA55
Pingback: super bowl broncos
Pingback: super bowl green bay packers
Pingback: FIFA55
Pingback: fiftyfive printing
Pingback: FIFA55
Pingback: FIFA55
Pingback: fifty five printing
Pingback: 55 print
Pingback: FIFA55
Pingback: FIFA55
Pingback: seo wp
Pingback: best seo wordpress theme
Pingback: super bowl halftime show list
Pingback: super bowl quarterbacks
Pingback: FIFA55
Pingback: FIFA55
Pingback: super bowl 18
Pingback: super bowl 51 score
Pingback: super bowl gospel celebration
Pingback: best laptops under 20000 rupees
Pingback: paytm promo code for wallet
Pingback: wholesale halal food suppliers
Pingback: micromax tablet under 10000
Pingback: online bus booking discount coupons
Pingback: grill gloves
Pingback: paytm promo code for bus ticket
Pingback: grill gloves
Pingback: grill mitts
Pingback: grill mitts
Pingback: promo codes for paytm
Pingback: snapdeal coupon code
Pingback: coupon codes for freecharge
Pingback: 55printing.com/cheap-color-copies
Pingback: www.55printing.com/cheap-color-copies/
Pingback: 55printing.com/cheap-color-copies/
Pingback: bitsler caraycruz
Pingback: 55printing.com/cheap-color-copies
Pingback: bitsler lottery
Pingback: buy ethereum
Pingback: 55printing.com/cheap-color-copies/
Pingback: bitsler roulette
Pingback: bitsler forum
Pingback: 55printing.com/cheap-color-copies
Pingback: 55printing.com/cheap-color-copies
Pingback: Tile
Pingback: super bowl yearly winners
Pingback: bitsler forum
Pingback: cold wallet
Pingback: bitsler lottery
Pingback: litecoin
Pingback: javunsensored.mobi
Pingback: super bowl 95
Pingback: bitsler social
Pingback: litecoin
Pingback: ethereum
Pingback: super bowl zuschauer
Pingback: super bowl xlvii
Pingback: litecoin
Pingback: casino
Pingback: Coinbase
Pingback: super bowl 19
Pingback: bitcoin
Pingback: bitsler dice
Pingback: bitsler caraycruz
Pingback: bitsler
Pingback: dogecoin
Pingback: birdhouse for sale
Pingback: bitsler
Pingback: birdhouse wood
Pingback: birdhouse outdoor
Pingback: Flower delivery netherlands
Pingback: super bowl l
Pingback: litecoin
Pingback: bitsler dice
Pingback: bitsler multicolor
Pingback: send flowers netherlands
Pingback: casino
Pingback: bitsler caraycruz
Pingback: bitsler forum
Pingback: litecoin
Pingback: super bowl host cities
Pingback: birdhouse handmade
Pingback: super bowl indianapolis
Pingback: tips voor windows
Pingback: bitsler lottery
Pingback: super bowl predictions
Pingback: bitsler lottery
Pingback: bitsler multicolor
Pingback: Dog food brands
Pingback: pet supplies
Pingback: bitsler forum
Pingback: healthy dog food
Pingback: dog shock collar with remote
Pingback: litecoin
Pingback: super bowl kingston ny
Pingback: small dog training collar
Pingback: super bowl experience
Pingback: pampered pets
Pingback: pet products
Pingback: burst
Pingback: wall stencils
Pingback: Systeembeheer haarlem
Pingback: bitsler dice
Pingback: wall decal
Pingback: decals
Pingback: windows center
Pingback: powertronic revisie
Pingback: Voith diwa 3
Pingback: koppeling
Pingback: SEO Marketing
Pingback: bitsler
Pingback: Netwerkbeheer haarlem
Pingback: ondersteuning voor nabestaanden
Pingback: ZF wg211
Pingback: transmissie
Pingback: dogecoin
Pingback: football
Pingback: bitsler social
Pingback: bitsler dice
Pingback: bitsler
Pingback: Voith diwa 5
Pingback: Eset Cyber Security
Pingback: deliver flowers amsterdam netherlands
Pingback: bitsler dice
Pingback: ethereum
Pingback: laat een berichtje achter voor je nabestaanden
Pingback: dogecoin
Pingback: you could try here
Pingback: burst
Pingback: cccam server
Pingback: encouraging quotes
Pingback: iptv providers
Pingback: bitsler dice
Pingback: lions game
Pingback: cccam free
Pingback: wolf habitat
Pingback: litecoin
Pingback: daily quotes
Pingback: where wolves live
Pingback: click here to find out more
Pingback: lion
Pingback: motivational quotes
Pingback: dog
Pingback: visit homepage
Pingback: bitsler
Pingback: free shipping
Pingback: bitcoin
Pingback: see here
Pingback: Source
Pingback: click
Pingback: my explanation
Pingback: virtuálni sidlo firmy
Pingback: bitsler multicolor
Pingback: navigate to this site
Pingback: dogecoin
Pingback: blog link
Pingback: litecoin
Pingback: litecoin
Pingback: click here to investigate
Pingback: bitsler forum
Pingback: click here now
Pingback: discover this info here
Pingback: find more info
Pingback: additional reading
Pingback: content
Pingback: HONR Network
Pingback: this hyperlink
Pingback: bitsler forum
Pingback: ethereum
Pingback: litecoin
Pingback: burst
Pingback: browse around these guys
Pingback: HONR Network
Pingback: bitsler dice
Pingback: that site
Pingback: continue reading this
Pingback: hop over to these guys
Pingback: look here
Pingback: litecoin
Pingback: watch the walking dead online free
Pingback: watch the walking dead online free
Pingback: PWC Parts
Pingback: Micropigmentación Capilar Marbella
Pingback: Misc. Parts
Pingback: ATV Kawasaki Piston Kits
Pingback: Outboard Johnson Evinrude Fuel Pumps
Pingback: free vpn
Pingback: PWC Yamaha Wear Rings
Pingback: MERCURY
Pingback: ATV Kawasaki Piston Kits
Pingback: Outboard Johnson Evinrude Rectifier
Pingback: Outboard Mercury Fuel Pumps
Pingback: PWC Kawasaki Bearings
Pingback: watch tv shows online free
Pingback: watch movies online free
Pingback: ATV Honda Clutch - Brake Levers
Pingback: Outboard Chrysler Force Bearings
Pingback: ATV Yamaha Piston Pins
Pingback: ATV Yamaha Brake Pads & Shoes
Pingback: watch movies online free
Pingback: watch the big bang theory online free
Pingback: PWC Kawasaki Bearings
Pingback: Zonnepanelen Vlaams-Brabant
Pingback: ATV Kawasaki Voltage Regulators
Pingback: ATV Yamaha Voltage Regulators
Pingback: PWC Yamaha Crankshafts
Pingback: Geothermische warmtepomp
Pingback: Outboard Mercury Engine Parts
Pingback: SEAL KITS
Pingback: ATV Honda Voltage Regulators
Pingback: Prosumententarief
Pingback: Outboard Chrysler Force Connecting Rod Kits
Pingback: PWC Polaris O-Rings
Pingback: Airconditoning Tienen
Pingback: Warmtepomp prijs
Pingback: Outboard Mercury Piston Kits
Pingback: watch ncis online free
Pingback: removal van uk
Pingback: ATV Yamaha Voltage Regulators
Pingback: uk police virus removal iphone
Pingback: france to uk removals
Pingback: uk removal companies directory
Pingback: uk removals to spain
Pingback: Outboard Mercury Rectifier
Pingback: Outboard Johnson Evinrude Impellers
Pingback: removal in uk
Pingback: Outboard Mercury Needles
Pingback: uk removals cost
Pingback: PWC Kawasaki CDI Boxes
Pingback: EBAY MOTORS
Pingback: ATV Polaris Clutch - Brake Levers
Pingback: Outboard Chrysler Force Engine Parts
Pingback: watch modern family online free
Pingback: ATV Suzuki Electrical Parts
Pingback: watch modern family online free
Pingback: cyprus to uk removals
Pingback: Outboard Mercury Rebuild Kits
Pingback: Wolfgang Halbig
Pingback: PWC Kawasaki Crankshafts
Pingback: personalised birthday balloons
Pingback: PWC Yamaha Piston Pins
Pingback: personalised balloons
Pingback: personalised balloons
Pingback: personalised balloons
Pingback: custom birthday balloons
Pingback: watch modern family online free
Pingback: personalised balloons
Pingback: litecoin
Pingback: Wolfgang Halbig
Pingback: best breast cancer gift
Pingback: WOLFGANG HALBIG
Pingback: Website Creators
Pingback: vehicle donation
Pingback: donate your car for cash
Pingback: Leonard Pozner
Pingback: web site designers
Pingback: Website Creators
Pingback: dumpster rental southfield
Pingback: michigan dumpster rental
Pingback: donate car to goodwill
Pingback: dumpster rental taylor
Pingback: dumpster rental warren
Pingback: dumpster rental canton
Pingback: donate your car tax deduction
Pingback: dumpster rental West Bloomfield
Pingback: dumpster rental grand blanc
Pingback: dumpster rental yates
Pingback: i want to donate my car to charity
Pingback: tax deduction for donated car
Pingback: Our Services
Pingback: Graphic Design
Pingback: brand identity design
Pingback: site dekorace
Pingback: charity car donation tax deduction
Pingback: www.woodwaste.ca
Pingback: commercial dumpster rental
Pingback: get a car donated to you
Pingback: where to donate used cars for charity
Pingback: best way to donate car
Pingback: i need a car donated to me
Pingback: best place to donate my car
Pingback: roll off container rental
Pingback: donate old car tax deduction
Pingback: web design for service industry
Pingback: dumpster container rental
Pingback: dryer vent cleaning monroe
Pingback: Crowdfunding Press
Pingback: Clothes dryer repair
Pingback: Increased drying time
Pingback: garbage rental
Pingback: VIP Financing Solutions
Pingback: Monroe dryer vent service
Pingback: Strategy
Pingback: Vent
Pingback: construction debris removal
Pingback: vent installation
Pingback: dryer air vent
Pingback: banner design services
Pingback: repair dryer vent
Pingback: garbage containers rental
Pingback: web design services
Pingback: Career Opportunities
Pingback: indoor dryer vents
Pingback: dryer vent installation service
Pingback: web design for startups
Pingback: roll off container rental
Pingback: garbage dumpsters for rent
Pingback: Website Hosting
Pingback: gas dryer venting
Pingback: affordable logo design
Pingback: home dumpster rental
Pingback: garbage dumpster sizes
Pingback: dumpster pricing
Pingback: brand identity design
Pingback: dumpster rental Xenia
Pingback: rent a dumpster
Pingback: roll off containers
Pingback: VIP Financing Solutions
Pingback: rolloff dumpster
Pingback: waste bins rental
Pingback: Steroids for sale online
Pingback: price List
Pingback: waste pickup
Pingback: rent a garbage dumpster
Pingback: 30 yard dumpster
Pingback: 2 yard dumpster
Pingback: rent a small dumpster
Pingback: 4 yard dumpster
Pingback: trash hauling
Pingback: 15 yard dumpster rental
Pingback: dirt dumpster
Pingback: roll off service
Pingback: 30 yard dumpster dimensions
Pingback: dumpster rental company
Pingback: 20 yard dumpster cost
Pingback: small dumpsters for rent
Pingback: garbage disposal bins
Pingback: construction dumpster cost
Pingback: commercial dumpster sizes
Pingback: fleck water softener
Pingback: HandyPro of Columbus OH
Pingback: water softener salt
Pingback: Home water filtration
Pingback: Wheelchair ramps
Pingback: Water conditioning products
Pingback: Bathroom Remodel Dublin OH
Pingback: Walk in tubs Worthington
Pingback: Zwembaden polypropyleen
Pingback: water softener no salt
Pingback: water softener installation
Pingback: best home water softener
Pingback: water softener brands
Pingback: wheelchair aluminum
Pingback: Zwembadaanleg Limburg
Pingback: handyman australia
Pingback: kerb ramp
Pingback: water softener home
Pingback: handyman hire
Pingback: water softeners salt
Pingback: Leonard Pozner
Pingback: meter water softener
Pingback: Aanleggen zwembad
Pingback: water softener settings
Pingback: design services
Pingback: bamboo lifestyle centre melville
Pingback: the ramp shop
Pingback: steps to writing a book
Pingback: book printers cape town
Pingback: bamboo lifestyle centre melville
Pingback: book printing and binding pretoria
Pingback: inexpensive web design
Pingback: book printing and binding cape town
Pingback: Isaacs
Pingback: bathrooms for the disabled
Pingback: bathrooms for the disabled
Pingback: book printing and binding cape town
Pingback: www.flightera.net/img/anchor.txt
Pingback: web design for small businesses and individuals
Pingback: Leonard Pozner
Pingback: help writing a book about my life
Pingback: Book launch
Pingback: book printers cape town
Pingback: CSGO Swift.trade
Pingback: thermador appliance repair
Pingback: salt lake refrigerator repair
Pingback: African book publishers
Pingback: book writers in south africa
Pingback: appliance repair services
Pingback: CSGO Swift
Pingback: book printing and binding cape town
Pingback: Poetry
Pingback: www.csgoswift.trade
Pingback: solar appliance repair
Pingback: beauty for women
Pingback: appliance repair manuals
Pingback: appliance repair near me
Pingback: buy property in goa
Pingback: CSGO Swift
Pingback: property for sale in goa
Pingback: maytag washer repair
Pingback: Leonard Pozner
Pingback: CSGOSwift.trade
Pingback: washer machine parts
Pingback: wash machine repair
Pingback: Chakrir Khobor Government and Non Government
Pingback: part select
Pingback: buy independent house in goa
Pingback: arbeiten in deutschland wohnen in der schweiz
Pingback: appliance repair okc
Pingback: commercial refrigerator repair
Pingback: maytag dryer repair
Pingback: schweiz wohnen
Pingback: rozvoz květin
Pingback: wohnen in deutschland und arbeiten in der schweiz
Pingback: property for sale in goa
Pingback: whirlpool customer service number
Pingback: whirlpool appliances parts
Pingback: Entertainment
Pingback: pensionskasse rückkehr nach deutschland
Pingback: Tuinaanleg
Pingback: whirlpool refrigerator ice maker repair
Pingback: kitchenaid appliances repair
Pingback: whirlpool repair atlanta
Pingback: grenzgänger schweiz deutschland
Pingback: arbeiten schweiz grenzgänger
Pingback: Leonard Pozner
Pingback: in deutschland arbeiten in der schweiz wohnen
Pingback: schweiz wohnen
Pingback: schweiz arbeiten und leben
Pingback: Career
Pingback: Job in USA
Pingback: Striptease Antwerpen
Pingback: Motorschaden Verkaufen
Pingback: Auto Jetzt Verkaufen
Pingback: Striptease Limburg
Pingback: Auto mit Motorschaden Verkaufen
Pingback: Autoankauf
Pingback: Stripact
Pingback: Mercedes mit Motorschaden
Pingback: Defektes Auto Verkaufen
Pingback: Audi mit Motorschaden
Pingback: Erotische massage
Pingback: Auto Verkaufen
Pingback: BMW mit Motorschaden
Pingback: Wir Kaufen Dein Auto
Pingback: Escort in Toronto
Pingback: www.steemit.com/dianabol/@parasitepower/dianabol-steroid-profile
Pingback: game dev companies
Pingback: chat senza registrazione
Pingback: chat italiana
Pingback: Jim Fetzer
Pingback: Glazen binnendeuren
Pingback: Glazen vloer
Pingback: Jim Fetzer
Pingback: Jim Fetzer
Pingback: Jim Fetzer
Pingback: Aluminium ramen
Pingback: Jim Fetzer
Pingback: Jim Fetzer
Pingback: Jim Fetzer
Pingback: chat italiana
Pingback: Jim Fetzer
Pingback: flowers
Pingback: www.tomato-plants-direct.co.uk/
Pingback: Jim Fetzer
Pingback: Tomato Plants Direct the mail order tomato specialists
Pingback: Tomato Plants Direct the mail order tomato specialists
Pingback: Jim Fetzer
Pingback: www.tomato-plants-direct.co.uk/
Pingback: Jim Fetzer
Pingback: www.tomatosite.com/
Pingback: www.tomatosite.com/
Pingback: Tomato Plants Direct the mail order tomato specialists
Pingback: chat italiana
Pingback: Vegetable plants direct mail order vegetable plant specialists
Pingback: www.vegetableplantsdirect.co.uk/
Pingback: Vegetable plants direct mail order vegetable plant specialists
Pingback: chat senza registrazione
Pingback: chat italiana
Pingback: Click Here
Pingback: Click Here
Pingback: Parental Child Abduction
Pingback: Jim Fetzer
Pingback: Read More
Pingback: Read More
Pingback: Parental Child Abduction
Pingback: Read More
Pingback: Parental Child Abduction
Pingback: More Information
Pingback: Parental Child Abduction
Pingback: Click Here
Pingback: Flightera - Flight information and Aircraft statistics
Pingback: vychytavky
Pingback: Click Here
Pingback: Flightera - Plane Database
Pingback: Flightera - Flight status, live updates
Pingback: Flightera - Plane Database
Pingback: Flightera - Plane Database
Pingback: Parental Child Abduction
Pingback: Flightera - Flight statistics
Pingback: Flightera - Plane Database
Pingback: Flightera - Flight information and Aircraft statistics
Pingback: Flightera - Flight information and Aircraft statistics
Pingback: 15 Minute Manifestation
Pingback: Lenny Pozner
Pingback: Leonard Pozner
Pingback: follow
Pingback: car donations for charity
Pingback: donate car for charity
Pingback: how to donate a vehicle
Pingback: dumpster containers
Pingback: how to get a donated car
Pingback: dumpster rental Gahana
Pingback: click
Pingback: dumpster rental Beavercreek
Pingback: follow
Pingback: disposal bins
Pingback: visit
Pingback: waste removal
Pingback: car donation deduction
Pingback: small dumpster rental
Pingback: follow
Pingback: follow
Pingback: astaxathin
Pingback: url
Pingback: where to donate old cars
Pingback: website
Pingback: best place to donate car for tax deduction
Pingback: get a dumpster
Pingback: astaxathin
Pingback: charities to donate cars
Pingback: astaxathin
Pingback: dumpster pickup
Pingback: donate an old car
Pingback: follow
Pingback: tax write off for car donation
Pingback: motorcycle donation
Pingback: dumpster rental ri
Pingback: dumpster rental mn
Pingback: cancer society car donation
Pingback: dumpster rental nj
Pingback: 40 yard dumpster cost
Pingback: donate car for cancer
Pingback: trash removal dumpster rental
Pingback: tax break for donating car
Pingback: motorcycle donation to charity
Pingback: donation of car to charity tax deductible
Pingback: value of donated car
Pingback: concrete dumpster rental
Pingback: Home
Pingback: debris dumpster
Pingback: dumpster rental Lake Hamilton
Pingback: waste container
Pingback: rent a construction dumpster
Pingback: skin tightening treatment
Pingback: fat burner for women
Pingback: junk pick up
Pingback: tighten belly skin
Pingback: roll off dumpster prices
Pingback: facial skin tightening
Pingback: tighten skin under eyes
Pingback: laser skin tightening cost
Pingback: rent trash bins
Pingback: skin tightening procedures
Pingback: trash hauling
Pingback: ways to tighten loose skin
Pingback: roll off boxes
Pingback: how to naturally tighten skin
Pingback: Services
Pingback: does laser resurfacing tighten skin
Pingback: how to tighten under eye skin
Pingback: 3 yard dumpster
Pingback: ATS Grandstand
Pingback: tighten skin after pregnancy
Pingback: natural skin tightening face mask
Pingback: 6 yard dumpster rental
Pingback: rental of dumpster
Pingback: yard dumpster
Pingback: ways to tighten stomach skin
Pingback: waste dumpster sizes
Pingback: pricing
Pingback: abdominal skin tightening
Pingback: laser neck skin tightening
Pingback: skin tightening for stomach
Pingback: loose skin tightening after weight loss
Pingback: natural products to tighten facial skin
Pingback: dumpster in a bag
Pingback: dumoster rental Hiram
Pingback: dumpster rental lawrenceville
Pingback: dumpster rental Mableton
Pingback: local dumpster rental
Pingback: non surgical skin tightening stomach
Pingback: Botox near me
Pingback: dumpster rental Conyers
Pingback: Operating-procedures
Pingback: dumpster rental Lithonia
Pingback: where to rent a dumpster
Pingback: penis enlargement chicago
Pingback: trash rental
Pingback: female hair loss treatment Oakbrook
Pingback: cool sculpting Oakbrook
Pingback: cool sculpting Oakbrook
Pingback: trash collection
Pingback: Botox hinsdale
Pingback: concrete dumpster rental
Pingback: yard dumpster
Pingback: cold sculpt
Pingback: get a dumpster
Pingback: Ratings-and-Reviews
Pingback: freeze fat cost
Pingback: PRP injection lombard
Pingback: cool liposuction
Pingback: chat per tutti
Pingback: roll on roll off dumpster
Pingback: coolsculpting fat removal
Pingback: rollaway dumpster rental
Pingback: chat per tutti
Pingback: where to rent a trash dumpster
Pingback: ice sculpting fat
Pingback: chat gratis
Pingback: chat senza registrazione
Pingback: cooling body sculpting
Pingback: chattimo
Pingback: coolsculpting areas
Pingback: schedule-an-inspection
Pingback: chattimo
Pingback: chat per ragazzi
Pingback: chat per tutti
Pingback: Entertainment Bookings Toronto
Pingback: Event Planning Company Toronto
Pingback: Health
Pingback: Event Planning Markham
Pingback: chat per ragazzi
Pingback: chat italia
Pingback: Photobooth Business
Pingback: Photobooth Companies
Pingback: chattimo
Pingback: Corporate Party Entertainment Company Toronto
Pingback: Certified Event Planning Company
Pingback: chat per incontri
Pingback: apple cider vinegar vs red wine vinegar
Pingback: apple cider vinegar vs vinegar
Pingback: baan suan
Pingback: bang saray beach
Pingback: royal hill
Pingback: apple cider vinegar 32
Pingback: apple cider vinegar 500 mg capsules
Pingback: apple cider vinegar 100%
Pingback: apple cider vinegar challenge
Pingback: apple cider vinegar 32
Pingback: pratumnak pattaya
Pingback: jomtien beach condominium studio for rent
Pingback: jomtien property pattaya
Pingback: jomtien thailand
Pingback: jomtien
Pingback: studio apartment
Pingback: pattaya property
Pingback: jomtien condo rentals
Pingback: watch & download hot videos
Pingback: Leonard Pozner
Pingback: Second Chance Marketing
Pingback: Website Development
Pingback: Sleep Mask
Pingback: Chefs choice knife sharpener
Pingback: snowboard improvement
Pingback: hip hoodies
Pingback: snowboard health
Pingback: snowboard tips
Pingback: womens tees
Pingback: expert snowboard lessons
Pingback: defy cursive clothing
Pingback: defy blood hoodies
Pingback: snowboard
Pingback: intermediate snowboard lessons
Pingback: snowboard IQ
Pingback: learn snowboarding
Pingback: Pool Service
Pingback: tarnished defy logo hoodies
Pingback: Pool Salt System
Pingback: Pool Cleaning
Pingback: Pool Repair
Pingback: snowboard education
Pingback: snowboard gear
Pingback: advanced snowboard lessons
Pingback: Pool Salt System
Pingback: snowboard
Pingback: Pool Renovation
Pingback: Pool Salt System
Pingback: outdoor clothing
Pingback: snowboard gear
Pingback: virtual snowboard school
Pingback: snowboard improvement
Pingback: virtual snowboard school
Pingback: England Transportation LLC
Pingback: snowboard tips
Pingback: snowboard lessons
Pingback: snowboarding
Pingback: snowboard
Pingback: intermediate snowboard lessons
Pingback: Wolfgang Halbig
Pingback: 4wd Accessories
Pingback: Virgo
Pingback: Franquicia
Pingback: Negocio
Pingback: Inmueble
Pingback: auto insurance agency
Pingback: Franquicia
Pingback: Empresa
Pingback: page about a good service provider
Pingback: Emprendimiento
Pingback: QuieroTuNegocio
Pingback: emergency lockout service
Pingback: mobile roadside assistance
Pingback: Negocio
Pingback: Compra
Pingback: baju kurung 2018
Pingback: page about a good service provider
Pingback: baju kurung sofia
Pingback: breakdown truck
Pingback: roadside service
Pingback: Negocio
Pingback: rollback truck sale
Pingback: Franquicia
Pingback: Ecuador
Pingback: Oportunidad
Pingback: towing service downtown detroit mi
Pingback: pizza tepsi
Pingback: the most reliable tow truck company near eastpointe
Pingback: Oportunidad
Pingback: Franquicia
Pingback: flatbed for sale
Pingback: truck lift shop
Pingback: the tow truck
Pingback: Venta
Pingback: rollback tow truck
Pingback: Franquicia
Pingback: ethereum
Pingback: towing truck company
Pingback: towing a car with a dolly
Pingback: towing
Pingback: trucks with lifts
Pingback: Luxury Apartments New York City
Pingback: Luxury Homes for Rent Crotia
Pingback: warren tow truck
Pingback: luxury villa rentals
Pingback: Luxury Villas For Rent Thailand
Pingback: road service
Pingback: Learn More
Pingback: man tow truck
Pingback: tow truck in detroit
Pingback: Rochelle
Pingback: collision insurance coverage
Pingback: Blog
Pingback: Luxury Villas For Rent Thailand
Pingback: luxury villa rentals Cape Town
Pingback: BYOB Fitness
Pingback: the tow truck
Pingback: towing service downtown detroit mi
Pingback: cost of tow truck
Pingback: where to sell car parts
Pingback: heavy duty chains for sale
Pingback: BYOB Fitness
Pingback: Luxury Apartments New York City
Pingback: BYOB Fitness
Pingback: car insurance with roadside assistance
Pingback: free insurance quote
Pingback: moving company long distance
Pingback: victory auto wreckers commercial
Pingback: Tank Trouble hacked
Pingback: Tank Trouble 3
Pingback: tow dolly rental
Pingback: used tow truck equipment
Pingback: tow truck service provider near farmington hills
Pingback: learn more about towing here
Pingback: click link to play
Pingback: Tank Trouble 3
Pingback: unblocked Tank Trouble
Pingback: Midwest Data Corp
Pingback: Willhaul Transportation
Pingback: Ssc online
Pingback: Wish Promo Code
Pingback: Wish Promo Codes 2018
Pingback: Tax lawyers in Mumbai
Pingback: Design patterns in java
Pingback: Design pattern
Pingback: Design patterns
Pingback: Pups sale sg
Pingback: Design pattern
Pingback: Design pattern
Pingback: Pups Singapore
Pingback: wow legion cheap us
Pingback: antorus heroic wow legion
Pingback: Online reading tutors
Pingback: Hashflare Delayed Withdrawal
Pingback: antorus heroic boost
Pingback: antorus heroic loot
Pingback: wow boost service eu
Pingback: prono tube
Pingback: VIP Financing Solutions
Pingback: 4lr 44 6v alkaline battery
Pingback: ag13 battery equivalent
Pingback: find the best cr1 3n battery 3v lithium battery
Pingback: where to find ag10 alkaline battery
Pingback: find 2cr5 battery 6v
Pingback: where to find ag10 alkaline battery
Pingback: mn27 12v alkaline battery
Pingback: battery cross reference
Pingback: 24hour batteries
Pingback: buy 2cr5 battery
Pingback: buy ag3 battery equivalent
Pingback: buy cr2016 battery
Pingback: alkaline a76 battery
Pingback: sr76 silver oxide button cell battery
Pingback: energizer c alkaline e93
Pingback: gpa76 button battery
Pingback: ag13 lr44 battery
Pingback: vinnic alkaline 9v battery
Pingback: Clicking Here
Pingback: find the right l1028 battery
Pingback: Learn More Here
Pingback: find ag13 lr44 battery
Pingback: a675 hearing aid battery
Pingback: vinnic extra heavy duty n size
Pingback: ag13 button cell
Pingback: buy ag13 battery
Pingback: 357a battery
Pingback: travel blog
Pingback: Lifestyle & Travel vlog
Pingback: Find Out More
Pingback: Learn More
Pingback: Lifestyle blog
Pingback: Lifestyle blog
Pingback: Find Out More
Pingback: Discover More Here
Pingback: Find Out More
Pingback: Learn More
Pingback: Go Here
Pingback: Scrapbookblog.co.uk
Pingback: travel blog
Pingback: Find Out More
Pingback: Read More Here
Pingback: Clicking Here
Pingback: Lifestyle blog
Pingback: Scrapbookblog.co.uk
Pingback: travel blog
Pingback: Discover More Here
Pingback: Go Here
Pingback: Learn More Here
Pingback: Find Out More
Pingback: Scrapbookblog.co.uk
Pingback: Our site
Pingback: Our site
Pingback: More Bonuses
Pingback: travel blog
Pingback: Lauren Scrapbook Blog
Pingback: Lifestyle & Travel vlog
Pingback: parenting blog
Pingback: more helpful hints
Pingback: helpful resources
Pingback: helpful resources
Pingback: More Bonuses
Pingback: john turek boca raton
Pingback: more helpful hints
Pingback: Business Automation
Pingback: Our site
Pingback: helpful resources
Pingback: italya turu
Pingback: notre dame
Pingback: Secondary Sales Management
Pingback: More Bonuses
Pingback: Salesforce
Pingback: ispanya portekiz turu
Pingback: Products Management
Pingback: stories for kids
Pingback: preschool bible felt stories
Pingback: felt board for preschool
Pingback: bulgaristan
Pingback: Business Automation
Pingback: John Turek Boca Raton Police
Pingback: monaco
Pingback: preschool felt board stories
Pingback: vatikan
Pingback: felt board stories for sale
Pingback: helpful hints
Pingback: toddler felt board stories
Pingback: çek cumhuriyeti
Pingback: flannel story for infants
Pingback: felt board stories
Pingback: Anti-aging
Pingback: additional reading
Pingback: felt board stories for preschool
Pingback: Task Management
Pingback: Products Management
Pingback: felt sets for Pre-K
Pingback: Customer Database Management
Pingback: felt board stories for preschool
Pingback: Business Growth
Pingback: flannel stories for teaching
Pingback: Anti aging remedies
Pingback: Complaint and Service Management
Pingback: Project Management
Pingback: anti aging secrets
Pingback: felt board stories for preschool
Pingback: simply anti aging
Pingback: John Turek Boca Raton Police
Pingback: anti aging pill
Pingback: Remove wrinkles
Pingback: felt board stories for toddlers
Pingback: felt board story sets
Pingback: felt stories
Pingback: 24 hour gyms
Pingback: flannel board for teaching
Pingback: felt story board set for prek
Pingback: bible felt story for preschoolers
Pingback: preschool activity ideas
Pingback: anti aging pills for women
Pingback: personal trainers in newark nj
Pingback: felt board stories for toddlers
Pingback: new jersey gym
Pingback: we pay cash for houses Dallas
Pingback: felt sets for Pre-K
Pingback: sell your house fast Dallas
Pingback: printable worksheets
Pingback: preschool felt board stories
Pingback: printable worksheets
Pingback: felt sets for Pre-K
Pingback: felt stories
Pingback: felt board story sets
Pingback: we buy dallas homes
Pingback: printable worksheets
Pingback: felt board stories for preschool
Pingback: we buy dallas homes
Pingback: we pay cash for houses Dallas
Pingback: felt sets
Pingback: cheap gym membership
Pingback: Leonard Pozner
Pingback: we buy dallas homes
Pingback: sell your house fast Dallas
Pingback: we buy dallas homes
Pingback: preschool worksheets
Pingback: preschool worksheets
Pingback: what is the best gym in newark nj
Pingback: printable worksheets
Pingback: best gyms in newark nj
Pingback: felt board story sets
Pingback: felt sets
Pingback: toddler felt board stories
Pingback: we buy dallas homes
Pingback: preschool worksheets
Pingback: preschool worksheets
Pingback: felt board stories for sale
Pingback: sell your house fast Tampa
Pingback: toddler felt board stories
Pingback: felt stories
Pingback: felt board stories
Pingback: we pay cash for houses Tampa
Pingback: preschool printables
Pingback: printable worksheets
Pingback: sell your house fast Tampa
Pingback: sell your house fast Tampa
Pingback: sell your house fast Tampa
Pingback: health club in newark nj
Pingback: we buy Tampa homes
Pingback: sell your house fast Tampa
Pingback: we buy Tampa homes
Pingback: we pay cash for houses Tampa
Pingback: san diego personal injury lawyers
Pingback: Seamless Rain Gutters
Pingback: preschool felt board stories
Pingback: felt board stories for preschool
Pingback: preschool worksheets
Pingback: preschool printables
Pingback: felt sets for Pre-K
Pingback: printable worksheets
Pingback: felt sets
Pingback: Seamless Rain Gutters
Pingback: felt sets
Pingback: preschool worksheets
Pingback: best injury lawyers in san diego
Pingback: felt sets for Pre-K
Pingback: felt board stories for preschool
Pingback: felt board stories for toddlers
Pingback: preschool felt board stories
Pingback: printable worksheets
Pingback: felt stories
Pingback: preschool printables
Pingback: felt board stories for preschool
Pingback: felt sets for Pre-K
Pingback: felt board stories for sale
Pingback: preschool worksheets
Pingback: felt stories
Pingback: preschool felt board stories
Pingback: preschool felt board stories
Pingback: san diego's number one injury law firm
Pingback: felt stories
Pingback: preschool felt board stories
Pingback: toddler felt board stories
Pingback: felt board story sets
Pingback: Ragnarok Online
Pingback: printable worksheets
Pingback: felt board story sets
Pingback: felt stories
Pingback: medical center in dubai
Pingback: felt sets
Pingback: preschool printables
Pingback: injury law firm in san diego
Pingback: preschool worksheets
Pingback: preschool worksheets
Pingback: preschool felt board stories
Pingback: Fix My Profile
Pingback: best injury lawyers in san diego
Pingback: Over 1 million reviews
Pingback: 250k hotels
Pingback: 250k hotels
Pingback: felt board story sets
Pingback: felt board stories for preschool
Pingback: preschool printables
Pingback: preschool printables
Pingback: toddler felt board stories
Pingback: felt board stories for sale
Pingback: preschool felt board stories
Pingback: preschool printables
Pingback: felt board stories for sale
Pingback: small business accountant
Pingback: Outboard Yamaha Electrical Parts
Pingback: MARINE ENGINE REBUILD KITS
Pingback: electrical and electronics
Pingback: CHRYSLER FORCE
Pingback: auto parts online
Pingback: Outboard Yamaha Trim Motors
Pingback: Boston CPA
Pingback: Hanlon and Associates
Pingback: VOLTAGE REGULATORS
Pingback: hardware online
Pingback: tool kit with drill machine
Pingback: RINGS
Pingback: VOLTAGE REGULATORS
Pingback: moving
Pingback: Outboard Yamaha Seal Kits
Pingback: Outboard Mercury Engine Parts
Pingback: products
Pingback: PISTONS
Pingback: Outboard Yamaha Piston Pins
Pingback: Outboard Mercury Piston Kits
Pingback: Hingham Massachusetts movers
Pingback: click here
Pingback: long distance movers
Pingback: Outboard Johnson Evinrude Piston Pins
Pingback: Outboard Johnson Evinrude Gaskets
Pingback: Outboard Johnson Evinrude Lower Units
Pingback: Outboard Mercury Coils
Pingback: eyewear for tactical swat teams
Pingback: Outboard Johnson Evinrude Gear and Clutch
Pingback: AR-670-1 compliant uniform boots
Pingback: Outboard Johnson Evinrude Shafts
Pingback: M Score
Pingback: Outboard Mercury Filters
Pingback: Applications?
Pingback: Outboard Johnson Evinrude Rebuild Kits
Pingback: Home owners insurance
Pingback: Outboard Mercury Alternators
Pingback: Outboard Mercury Gear and Clutch
Pingback: Management courses
Pingback: Plainville auto insurance
Pingback: Applications?
Pingback: Biochemistry
Pingback: Outboard Mercury Filters
Pingback: Education?
Pingback: Human Resources Courses
Pingback: interior decorator
Pingback: SA Bursaries online application Ð forms, apply, 2018,2019Ê
Pingback: Diploma
Pingback: Outboard Johnson Evinrude Trim Motors
Pingback: High School?
Pingback: Outboard Johnson Evinrude Trim Motors
Pingback: Outboard Chrysler Force Pins
Pingback: Outboard Chrysler Force Seal Kits
Pingback: Outboard Chrysler Force Pins
Pingback: Outboard Chrysler Force Ring Sets
Pingback: Outboard Chrysler Force Water Pumps
Pingback: Outboard Johnson Evinrude Electrical Parts
Pingback: Outboard Johnson Evinrude Coils
Pingback: Outboard Johnson Evinrude Power Packs
Pingback: James Fetzer
Pingback: Outboard Chrysler Force Water Pumps
Pingback: Outboard Chrysler Force Impellers
Pingback: Outboard Chrysler Force Bearings
Pingback: Outboard Johnson Evinrude Filters
Pingback: Outboard Johnson Evinrude Solenoids
Pingback: Outboard Johnson Evinrude Trim Motors
Pingback: PWC Seadoo Trim Motor
Pingback: PWC Kawasaki Parts
Pingback: PWC Seadoo Valves
Pingback: PWC Seadoo Bearings
Pingback: PWC Seadoo Parts
Pingback: PWC Seadoo Sensors
Pingback: PWC Seadoo Drive Shafts
Pingback: Media
Pingback: PWC Seadoo CDI Boxes
Pingback: Dubai Advertising
Pingback: PWC Seadoo Electrical Parts
Pingback: PWC Seadoo Tools
Pingback: hotel oswiecim
Pingback: golf chipping
Pingback: golf putting drills
Pingback: PWC Seadoo O-Rings
Pingback: golf sand shot ball position
Pingback: golf chipping exercises
Pingback: jouer 1xbet
Pingback: PWC Seadoo Parts
Pingback: PWC Seadoo Crankshaft Rebuild Kits
Pingback: PWC Kawasaki Crankshafts
Pingback: PWC Seadoo Piston Clips
Pingback: golf chipping drills
Pingback: golf swing fundamentals
Pingback: inscription 1xbet
Pingback: golf swing downswing
Pingback: golf chipping and pitching
Pingback: PWC Seadoo Jet Pump Repair Kits
Pingback: 1xbet tunisie
Pingback: golf putting grip
Pingback: golf swing review
Pingback: golf chipping around the green
Pingback: PWC Seadoo Wear Rings
Pingback: Explainer Video Services
Pingback: golf swing finish
Pingback: PWC Seadoo Drive Shafts
Pingback: Explainer Video Services
Pingback: Jasa Pembuatan Video
Pingback: PWC Seadoo Bearings
Pingback: Best PC Games Download
Pingback: PWC Seadoo Armature Coil
Pingback: PWC Seadoo Top End Rebuild Kits
Pingback: Berita Viral Terbaru
Pingback: Best Social Media Tools
Pingback: PWC Kawasaki Parts
Pingback: golf swing follow through
Pingback: golf swing for seniors
Pingback: PWC Seadoo Fuel Injectors
Pingback: KIK For PC
Pingback: deals in india
Pingback: PWC Seadoo Drive Shafts
Pingback: KIK For Computer
Pingback: KIK For Computer
Pingback: KIK For Computer
Pingback: KIK For Windows
Pingback: PWC Kawasaki Starters
Pingback: PWC Yamaha Oil Seal Kits
Pingback: PWC Kawasaki Oil Seal Kits
Pingback: iMessage for PC
Pingback: iMessage for Windows
Pingback: Convention Center
Pingback: PWC Kawasaki O-Rings
Pingback: PWC Kawasaki Solenoids
Pingback: iMessage for PC
Pingback: iMessage on PC
Pingback: iMessage on PC
Pingback: PWC Kawasaki Piston Pins
Pingback: PWC Kawasaki Oil Seal Kits
Pingback: PWC Yamaha Top End Rebuild Kits
Pingback: Event Planner
Pingback: PWC Yamaha Piston Pins
Pingback: PWC Kawasaki Starters
Pingback: PWC Yamaha Parts
Pingback: PWC Yamaha Sleeves
Pingback: html?_fsub=11245174013&_sid=147306953&_trksid=p4634.c0.m322
Pingback: PWC Kawasaki Sleeves
Pingback: Lean Belly Breakthrough
Pingback: PWC Yamaha Cables
Pingback: PWC Kawasaki Voltage Regulators
Pingback: ATV Yamaha Cables
Pingback: Off Road Yamaha Parts
Pingback: ATV Honda Engine Parts
Pingback: Red Tea Detox
Pingback: ATV Honda Piston Kits
Pingback: ATV Yamaha Piston Rings
Pingback: PWC Tigershark Piston Kits
Pingback: PWC Polaris Gaskets
Pingback: PWC Yamaha Valves
Pingback: Bondage
Pingback: PWC Yamaha Wear Rings
Pingback: PWC Polaris Solenoids
Pingback: PWC Tigershark Motor Mounts
Pingback: PWC Polaris Piston Kits
Pingback: PWC Yamaha Engine Cases
Pingback: cheap wheelchair singapore
Pingback: ATV Suzuki Top End Rebuild Kits
Pingback: Tour & Expense Management
Pingback: Contact Manager
Pingback: ATV Suzuki Clutch - Brake Levers
Pingback: teifoc
Pingback: Salesforce
Pingback: Business Automation
Pingback: SEO
Pingback: ATV Polaris Boot Kits
Pingback: Contact Follow ups Management
Pingback: Writing retreat
Pingback: Nutrition
Pingback: Complaint and Service Management
Pingback: ATV Honda Voltage Regulators
Pingback: ATV Kawasaki Clutch - Brake Levers
Pingback: ATV Suzuki Gaskets
Pingback: ATV Polaris Boot Kits
Pingback: Misc. Parts
Pingback: ATV Polaris Brake Pads
Pingback: Nature
Pingback: Mental Health
Pingback: web development
Pingback: Cabo Yacht Rental
Pingback: bitcoins 2014
Pingback: Proofreading
Pingback: robocoin
Pingback: Check This Out
Pingback: Web Site
Pingback: Web Site
Pingback: dorian nakamoto
Pingback: site
Pingback: Continued
Pingback: paul krugman quotes internet
Pingback: review
Pingback: Related Site
Pingback: Writing
Pingback: Check This Out
Pingback: Discover More
Pingback: btcchina
Pingback: Full Article
Pingback: Clicking Here
Pingback: More hints
Pingback: Continue Reading
Pingback: new form of currency
Pingback: circle 50 million
Pingback: latest technology news
Pingback: Paramotor training
Pingback: mcoin
Pingback: block chaining bitcoin
Pingback: bitchain
Pingback: 10 bitcoins in gbp
Pingback: gadget reviews
Pingback: blackchain
Pingback: apex status
Pingback: bitcoin internet
Pingback: Logan Paul Suicide
Pingback: beauty videos
Pingback: beauty videos
Pingback: Alexis Haller
Pingback: pets as gifts
Pingback: products for sale
Pingback: good gifts for dogs
Pingback: pet sympathy gifts
Pingback: pet sympathy gifts
Pingback: vallisia.club
Pingback: Eliezer Pozner
Pingback: cat toys 10K 100K
Pingback: quartz worktops glasgow
Pingback: Eliezer Pozner
Pingback: quartz worktops manchester
Pingback: Leonard Pozner
Pingback: dog feeders
Pingback: dog grooming supplies
Pingback: dog grooming supplies
Pingback: escort agency east midlands
Pingback: Vallisia
Pingback: online dog shop
Pingback: lpa services
Pingback: legal power of attorney
Pingback: Leonard Pozner
Pingback: Len Pozner
Pingback: Len Pozner
Pingback: Leonard Pozner
Pingback: custom dog collars
Pingback: cat lovers store
Pingback: gifts for dog owners
Pingback: Leonard Pozner
Pingback: Leonard Pozner
Pingback: dog dresses
Pingback: cat presents for her
Pingback: Latest make joke of
Pingback: Len Pozner
Pingback: Leonard Pozner
Pingback: Eliezer Pozner
Pingback: Len Pozner
Pingback: Len Pozner
Pingback: dog birthday gifts
Pingback: dog present ideas
Pingback: pet presents
Pingback: puppy gifts
Pingback: cat gifts
Pingback: pet food stores
Pingback: Leonard Pozner
Pingback: cat pet shop
Pingback: Len Pozner
Pingback: christmas gifts for cats
Pingback: Cat gym 1K 10K
Pingback: Len Pozner
Pingback: Eliezer Pozner
Pingback: dog crate
Pingback: Leonard Pozner
Pingback: small dog carriers
Pingback: dog cage
Pingback: Eliezer Pozner
Pingback: Leonard Pozner
Pingback: Eliezer Pozner
Pingback: Leonard Pozner
Pingback: Eliezer Pozner
Pingback: Leonard Pozner
Pingback: Eliezer Pozner
Pingback: noam kouris
Pingback: Choreography
Pingback: DJ's
Pingback: Audition
Pingback: apple cider vinegar 1 week results
Pingback: Market
Pingback: front porch
Pingback: patio doors
Pingback: bead board
Pingback: apple cider vinegar 32
Pingback: apple cider vinegar pregnant
Pingback: apple cider vinegar zurich
Pingback: patio doors
Pingback: door installers
Pingback: apple cider vinegar 1 week results
Pingback: Dance
Pingback: apple cider vinegar belly fat
Pingback: apple cider vinegar cayenne
Pingback: Photographer
Pingback: painting contractors
Pingback: ADA installers
Pingback: Studio hire
Pingback: Acting
Pingback: Casting
Pingback: wood floor installers
Pingback: how to draw a dog sitting
Pingback: apple cider vinegar jerky recipe
Pingback: apple cider vinegar 600
Pingback: dance class Columbus
Pingback: aipl joy Square sec 63a
Pingback: aipl Gurgaon
Pingback: aipl joy square
Pingback: The Gigland
Pingback: apple cider vinegar mold
Pingback: Organizer
Pingback: apple cider vinegar 5 acidity weight loss
Pingback: Emcee
Pingback: Music
Pingback: apple cider vinegar 5 gallon bucket
Pingback: apple cider vinegar 500 mg capsules
Pingback: aipl joy square Gurgaon
Pingback: Music Promotion
Pingback: aipl joy square sector 63a Gurgaon
Pingback: Casting
Pingback: Music
Pingback: apple cider vinegar weight loss
Pingback: aipl developers
Pingback: apple cider vinegar potassium
Pingback: apple cider vinegar kenya
Pingback: apple cider vinegar zinc deficiency
Pingback: apple cider vinegar for health
Pingback: The Gigland
Pingback: Event
Pingback: apple cider vinegar youtube
Pingback: Emcee
Pingback: latest Bollywood Movie News
Pingback: Festive
Pingback: Gig
Pingback: Book
Pingback: Children's
Pingback: Filmogrpahy
Pingback: ponyva
Pingback: ponyva
Pingback: Event professionals
Pingback: Producer
Pingback: cipzar
Pingback: ponyva
Pingback: cerna
Pingback: closet door installers
Pingback: lace
Pingback: exterior door installers
Pingback: raspberry pi kits
Pingback: Building Electronics
Pingback: raspberry pi kits
Pingback: Ardunio Uno
Pingback: bathroom designers
Pingback: flooring
Pingback: soldering kits
Pingback: Ardunio
Pingback: walk in showers
Pingback: Building Electronics
Pingback: off the shoulder dress
Pingback: Motors
Pingback: Ardunio Uno
Pingback: raspberry pi help
Pingback: Ardunio Nano
Pingback: rooftop solar panels in india
Pingback: raspberry pi kits
Pingback: solar panel installation in india
Pingback: Human sensor modules
Pingback: Ardunio Nano
Pingback: Raspberry pi
Pingback: Resistors
Pingback: Ardunio help
Pingback: raspberry pi kits
Pingback: raspberry pi kits
Pingback: Ardunio
Pingback: best solar panel in india
Pingback: stiletto
Pingback: solar system installation
Pingback: Bread boards
Pingback: elegant dress
Pingback: women's fashion
Pingback: nightclub dress
Pingback: Test the iPhone X
Pingback: credenciados arcelormittal
Pingback: cirurgia miopia unimed
Pingback: vaslip generico
Pingback: angitens
Pingback: sindicato dos metalurgicos gravatai
Pingback: aerolin principio ativo
Pingback: mirena valor
Pingback: bradesco saude tel
Pingback: vaslip generico
Pingback: stola betim
Pingback: www.arcelormittal.com.br
Pingback: arcelormittal sa
Pingback: www bradescoseguros com br prestadores
Pingback: seguro saude parto periodo carencia
Pingback: teste de solda eletrodo revestido
Pingback: jurisprudenciais
Pingback: acelormittal
Pingback: tabela de reembolso bradesco
Pingback: kearny macbook repair
Pingback: newark cell phone repair
Pingback: classe farmacologica
Pingback: clinica femina volta redonda
Pingback: vagostesyl
Pingback: newark macbook repair
Pingback: plano bradesco saude empresarial
Pingback: guia bradesco
Pingback: orange iphone repair
Pingback: cell phone repair shop in newark nj
Pingback: medicos bradesco saude
Pingback: arcelormittal juiz de fora
Pingback: site do bradesco saude
Pingback: formulario para reembolso bradesco saude
Pingback: belgo itauna
Pingback: arcelormittal piracicaba
Pingback: seguros unimed endereço
Pingback: eletrodo revestido tipos
Pingback: mesa de dobrar
Pingback: places that fix iphone near me
Pingback: convenio bradesco saúde
Pingback: bradesco saude odonto
Pingback: cerca concertina como instalar
Pingback: tabela de aço para construção civil
Pingback: www belgo bekaert arames com br
Pingback: marcar consulta bradesco
Pingback: arame ovalado preço
Pingback: bradesco saude top rede nacional
Pingback: definição de jurisprudencia
Pingback: concertina
Pingback: convênio bradesco saúde
Pingback: lipanon generico
Pingback: tabela tela soldada gerdau
Pingback: cerca arame farpado
Pingback: bradesco consultas
Pingback: angipress cd
Pingback: preço da tonelada de aço
Pingback: wwwbradescosaude
Pingback: grampo de cerca
Pingback: limite pessoal bradesco
Pingback: concertina fabrica
Pingback: abnt 6118
Pingback: saude bradesco rede credenciada rj
Pingback: nutricionista pelo bradesco saude
Pingback: code
Pingback: mourão de aço
Pingback: aço construção civil
Pingback: comprar arame farpado
Pingback: vergalhão 10mm
Pingback: como solda
Pingback: vasectomia bradesco saude
Pingback: fabrica de telas rj
Pingback: code
Pingback: telas para construção civil
Pingback: tela soldada galvanizada preço
Pingback: nelori
Pingback: bradesco saude com br
Pingback: mourao cerca
Pingback: code en ligne
Pingback: houston auto glass repair
Pingback: fast windshield replacement
Pingback: windshield replacement 77008
Pingback: windshield replacement
Pingback: windshield replacement 77056
Pingback: windshield replacement spring branch
Pingback: windshield replacement 77057
Pingback: windshield replacement near me
Pingback: houston auto glass repair
Pingback: houston auto glass repair
Pingback: houston auto glass repair
Pingback: auto glass replacement
Pingback: windshield replacement 77056
Pingback: front windshield repair
Pingback: windshield replacement spring branch
Pingback: windshield replacement 77056
Pingback: avon store
Pingback: www.arcelormittal.com.br
Pingback: unlock free huawie mate 10 pro att network
Pingback: belgo aço
Pingback: aços para construção civil
Pingback: unimed cobre rpg
Pingback: unimed pratico
Pingback: arcelormittal brasil endereço
Pingback: plano bradesco dental
Pingback: segurosunimed.com.br
Pingback: bradesco saude telefone
Pingback: consulta rat
Pingback: unimed pratico
Pingback: tree surgeons
Pingback: arcelormittal portal
Pingback: window cleaners
Pingback: cartão bradesco seguros
Pingback: arcelormittal portal
Pingback: 15 Minute Manifestation
Pingback: belgo com
Pingback: www.arcelormittal.com.br
Pingback: sindicato dos metalurgicos de mogi das cruzes
Pingback: dental plus santo andre
Pingback: portal bradesco dental
Pingback: portal bradesco dental
Pingback: zoxipan 20mg
Pingback: guia sadt arcelormittal
Pingback: portal bradesco dental
Pingback: nutricionista plano bradesco
Pingback: bradesco premium
Pingback: michigan rentals
Pingback: homes for rent in detroit mi
Pingback: apts for rent in detroit mi
Pingback: Stone Towing serving Lathrup Village
Pingback: townhomes detroit mi
Pingback: apartments for rent in mn
Pingback: Stone Towing near Beverly Hills
Pingback: Single Invoice Finance
Pingback: Credit Insurance
Pingback: mi flat
Pingback: Factoring
Pingback: towing price
Pingback: Stone Towing serving 10 Mile Rd
Pingback: Stone Towing near US-24
Pingback: Asset Finance
Pingback: apartments and townhomes for rent in michigan
Pingback: houses for rent in detroit mi westside
Pingback: loft apartments detroit
Pingback: Business Loans
Pingback: condos for rent in metro detroit area
Pingback: house rentals
Pingback: Stone Towing near Telegraph Rd
Pingback: hard water shower filter
Pingback: Stone Towing near Telegraph Rd
Pingback: Stone Towing serving 13 Mile Rd
Pingback: huntington woods towing
Pingback: houses for rent near detroit
Pingback: Stone Towing near Telegraph Rd
Pingback: m39 auto wrecker
Pingback: cheap single bedroom apartments for rent
Pingback: Stone Towing serving M10 Southfield
Pingback: cheap studio apartments detroit mi
Pingback: apartment hunters
Pingback: roll off rental
Pingback: residential dumpster rental
Pingback: unimed cobre psicologo
Pingback: commercial dumpster
Pingback: tow truck dynamic
Pingback: roll off service
Pingback: towing
Pingback: road truck service
Pingback: cheapest tow
Pingback: sushi roll
Pingback: 30 yard dumpster dimensions
Pingback: construction debris containers
Pingback: the most reliable tow truck company near eastpointe
Pingback: dumpster sizes 10 yard
Pingback: dearborn tow truck service in
Pingback: lift hook
Pingback: rv towing service
Pingback: dumpster bag
Pingback: direct insurance roadside assistance
Pingback: waste companies
Pingback: yard waste
Pingback: junk pickup
Pingback: yard waste
Pingback: campbell towing
Pingback: heavy duty rollback tow trucks for sale
Pingback: moving a car
Pingback: roll off container prices
Pingback: shower heads
Pingback: plano de saude bradesco lista de medicos
Pingback: cordarex principio ativo
Pingback: car rescue
Pingback: cars transportation
Pingback: residential dumpster rental cost
Pingback: flatbed diesel
Pingback: tow all price
Pingback: salvation army car donation
Pingback: cartao bradesco seguros
Pingback: eletros saude rede credenciada
Pingback: donate old cars to charity
Pingback: road assistance service
Pingback: valor reembolso bradesco saude
Pingback: victory auto wreckers commercial
Pingback: donate used car
Pingback: aço ca 50
Pingback: donate car for charity
Pingback: tow truck company near downtown detroit mi
Pingback: pino de aço
Pingback: red nose day actually
Pingback: donate old cars for charity
Pingback: donating a car to goodwill
Pingback: red nose day 2018 usa
Pingback: car donation rules
Pingback: emergency townearg near farmington hills
Pingback: towing rosedale park
Pingback: cars for kids charity
Pingback: red nose day history
Pingback: red nose day 2018
Pingback: how to donate a car to goodwill
Pingback: red nose day 2018 usa
Pingback: astm a36 propriedades
Pingback: plano de saude bradesco lista de medicos
Pingback: trucks sale
Pingback: used auto parts online search
Pingback: used tow truck equipment
Pingback: red nose day coldplay
Pingback: tipos de soldadura existentes
Pingback: www bradescovidaeprevidencia com br
Pingback: red nose day england
Pingback: insurance for
Pingback: astm a36 propriedades
Pingback: red nose day movie
Pingback: red nose day biscuit competition
Pingback: red nose day 2018 usa
Pingback: red nose day campaign
Pingback: insurance for
Pingback: red nose day uk
Pingback: carencia bradesco saude
Pingback: red nose day challenge 2018
Pingback: donate my junk car
Pingback: npr donate my car
Pingback: plymouth rd tow truck service
Pingback: red nose day earrings
Pingback: Huron Towing Detroit
Pingback: red nose day 2018 usa
Pingback: chicago rd towing
Pingback: takipçi satın al
Pingback: here
Pingback: instagram takipçi satın alma
Pingback: residential rental property management
Pingback: used wrecker sales
Pingback: find a property manager
Pingback: bradesco rede nacional
Pingback: Huron Towing near Detroit
Pingback: flatbed for f350
Pingback: dearborn towing service
Pingback: property management companies dallas
Pingback: crovu
Pingback: complete property management
Pingback: estribo de ferro
Pingback: real property management and realty inc
Pingback: instagram takipçi alma
Pingback: site do segurado bradesco
Pingback: tow truck service in dearborn heights
Pingback: emergency towing near detroit mi
Pingback: towing in warrendale detroit
Pingback: panske penezenky
Pingback: towing service provider dearborn heights mi
Pingback: residential property management firms
Pingback: manage apartment property
Pingback: nationwide property management companies
Pingback: premier property management michigan
Pingback: Huron Towing near Dearborn Heights
Pingback: Huron Towing (734) 619-6419
Pingback: cars parts
Pingback: portal de compras arcelormittal
Pingback: PANSKE PENAZENKY
Pingback: graphic design nz
Pingback: ferro 10mm
Pingback: saude bradesco.com.br
Pingback: como pedir reembolso bradesco saude
Pingback: arcelormittal juiz de fora
Pingback: bradesco essencial plus
Pingback: www bradescosaude com br prestador
Pingback: 7 Day Diabetic Meal Plan
Pingback: Diabetic Meal Recipes
Pingback: bradesco flex saude
Pingback: saude bradesco.com.br
Pingback: can diabetics eat brown rice
Pingback: buy instagram followers famoid
Pingback: buy instagram followers credit card
Pingback: numero do bradesco saude
Pingback: acelor mittal
Pingback: lista de medicos conveniados bradesco saude
Pingback: nbr concreto armado
Pingback: seguro saude internacional unimed
Pingback: buy instagram followers credit card
Pingback: buy instagram followers
Pingback: diabetes weight loss diet
Pingback: buy real instagram followers
Pingback: real instagram followers buy
Pingback: Gestational diabetes
Pingback: Preventing Type 2 Diabetes
Pingback: dietary fibers
Pingback: DIABETIC DIETS
Pingback: teeth whitening products that work
Pingback: best way to whiten teeth
Pingback: best way to whiten teeth
Pingback: teeth whitening remedies
Pingback: is teeth whitening safe
Pingback: teeth whitening products that work
Pingback: Type 2 Diabetes
Pingback: dietary plans for diabetic patients
Pingback: best teeth whitening
Pingback: teeth whitening without leaving sensitive teeth
Pingback: how to get white teeth
Pingback: teeth whitening remedies
Pingback: filipino culture
Pingback: teeth whitening before and after
Pingback: best teeth whitening
Pingback: Best Weight Loss Plan
Pingback: diet
Pingback: Lose 10lbs In 10 Days
Pingback: Quick Tips To Lose Weight
Pingback: how to lose weight fast
Pingback: Diet Tips To Lose Weight Quickly
Pingback: Energy Booster Supplement
Pingback: Green Tea Supplement
Pingback: HCG Drops
Pingback: Weight Loss Kit
Pingback: Best Diet Tips To Lose Weight Fast
Pingback: Fast Weight Loss Diet Plan
Pingback: 2 week diet
Pingback: how to lose weight
Pingback: Weight Loss Supplements
Pingback: Colon Cleanse
Pingback: Fat Loss Diet Plan
Pingback: Tips For Losing Belly Fat
Pingback: Forskolin
Pingback: how to 7 star ffbe
Pingback: how to 2fa binance
Pingback: 10 Days To Lose Weight
Pingback: how to build credit
Pingback: How To Lose Weight In 10 Days At Home
Pingback: how to 1306/7
Pingback: how to 360 flip
Pingback: how to 95 confidence interval
Pingback: how to calculate percentages
Pingback: how to draw a rose
Pingback: how to 0xc000007b
Pingback: how to lucid dream
Pingback: how to make ice cream
Pingback: how to xcode
Pingback: RLTrading
Pingback: RLTrading Server
Pingback: how to get robux
Pingback: how to obtain a birth certificate
Pingback: RLTrading Server
Pingback: how to no clip in roblox
Pingback: how to eat fried worms
Pingback: how to reset iphone 6
Pingback: RocketLeague
Pingback: how to get rid of acne
Pingback: website
Pingback: best travel blog portugal
Pingback: RLTrading
Pingback: best view in porto
Pingback: best places in portugal
Pingback: this content
Pingback: Get More Info
Pingback: best vacation tips for Porto
Pingback: visit this travel blog
Pingback: portugal adventure vacation guide
Pingback: click site
Pingback: best portugal travel blog
Pingback: awesome view in lisbon
Pingback: this content
Pingback: best view in porto
Pingback: about portugal
Pingback: here
Pingback: exploring porto in portugal
Pingback: best city to visit in portugal
Pingback: here
Pingback: belga mineiro
Pingback: vacations in portugal
Pingback: about portugal
Pingback: find the best portugal sighseeing
Pingback: caldeamento
Pingback: travel by train to portugal
Pingback: find more
Pingback: portugaltravelsecrets
Pingback: weblink
Pingback: portugal travelling guide
Pingback: best vacation tips for Porto
Pingback: donáka kvetov
Pingback: Silk Road
Pingback: Chinese Yuan
Pingback: Virtual Mediation
Pingback: Online Mediator
Pingback: dryer vent cleaning naperville
Pingback: ip camera
Pingback: keyless lock
Pingback: Dryer Vent Cleaning
Pingback: Dryer vent cleaning how to
Pingback: cover latter sample
Pingback: VIP Financing Solutions
Pingback: home products
Pingback: home security
Pingback: Dryer safety
Pingback: dryer vent cleaning oak park
Pingback: Dryer Vent Wizard
Pingback: Dryer Vent Cleaning
Pingback: pmma injections hips
Pingback: Vent
Pingback: Clothes dryer
Pingback: Dryer vent cleaning how to
Pingback: dryer vent cleaning brookfield
Pingback: hot sale
Pingback: smart door lock
Pingback: smart door lock
Pingback: cover latter sample
Pingback: smart door lock
Pingback: Dryer vent cleaning river forest
Pingback: wholesale
Pingback: Sandy Hook
Pingback: dryer vent cleaning woodridge
Pingback: Dryer vent cleaning La Grange
Pingback: Sandy Hook
Pingback: Eladia Pertuit
Pingback: cover latter format
Pingback: Chrissy Bowlby
Pingback: Delma Christiansen
Pingback: Sandy Hook
Pingback: Kaila Brockman
Pingback: Sandy Hook
Pingback: roll off dumpster
Pingback: garbage bin
Pingback: arcelormittal aços longos
Pingback: Sandy Hook
Pingback: Jessenia Beede
Pingback: www belgo com br
Pingback: dumpster rental Woodstock
Pingback: Sandy Hook
Pingback: Rodrigo Ernst
Pingback: pick up junk
Pingback: Sandy Hook
Pingback: Darline Kunst
Pingback: dumpster bin
Pingback: Sandy Hook
Pingback: Ping Geyer
Pingback: garbage containers rental
Pingback: construction trash containers
Pingback: Youlanda Kahan
Pingback: open top dumpster rental
Pingback: roll off container rental prices
Pingback: .22 caliber bullet stickers
Pingback: roll away trash containers
Pingback: bullet hole decals
Pingback: container rental
Pingback: Sandy Hook
Pingback: .22 caliber bullet stickers
Pingback: decals for cars
Pingback: decals for cars
Pingback: bullet hole stickers
Pingback: glass bullet stickers
Pingback: towing
Pingback: mobile lockout service
Pingback: bullet hole stickers
Pingback: 24 tow truck service
Pingback: bullet hole decals
Pingback: bullet hole stickers
Pingback: gun shot decals
Pingback: .22 caliber bullet stickers
Pingback: decals for cars
Pingback: bullet hole decals
Pingback: Sandy Hook
Pingback: gun shot decals
Pingback: mobile lockout service
Pingback: auto wrecker service in farmington hills
Pingback: auto insurance agency
Pingback: roll back tow truck for sale
Pingback: Sandy Hook
Pingback: glass bullet decals
Pingback: family insurance coverage
Pingback: kuplex chain
Pingback: free quote on car insurance
Pingback: gun shot decals
Pingback: emergency roadside service in detroit
Pingback: gun shot decals
Pingback: vinyl bullet stickers
Pingback: vinyl bullet decals
Pingback: bullet hole decals
Pingback: Sandy Hook
Pingback: glass bullet stickers
Pingback: bullet hole decals
Pingback: mobile mechanic
Pingback: towing service 24/7
Pingback: doruceni kvetin Praha
Pingback: types of car insurance
Pingback: flatbed towing truck
Pingback: auto insurance agency
Pingback: used auto part search
Pingback: portland auto wrecking yards
Pingback: farmington hills emergency tow truck near
Pingback: truck car carrier
Pingback: Chinese Yuan
Pingback: Silk Road
Pingback: click here
Pingback: Silk Road
Pingback: towing service in taylor
Pingback: Silk Road
Pingback: towing service 24/7
Pingback: Silk Road
Pingback: tow truck rental
Pingback: Silk Road
Pingback: Chinese Yuan
Pingback: Silk Road
Pingback: Silk Road
Pingback: Silk Road
Pingback: Silk Road
Pingback: towing service provider midtown
Pingback: Chinese Yuan
Pingback: Silk Road
Pingback: emergency roadside assistance hazel park mi
Pingback: flatbed towing truck
Pingback: rosedale park towing in
Pingback: sell your house for cash louisville ky
Pingback: Oracle Hyperion Managed Services
Pingback: magnet signs edmonton
Pingback: edmonton magnetic signs
Pingback: Hotels with Shuttles to Don Muang Airport
Pingback: magnetic signs
Pingback: magnetic signs
Pingback: edmonton magnetsigns
Pingback: magnetic signs
Pingback: More Information
Pingback: magnet signs
Pingback: magnetsigns edmonton
Pingback: magnetsigns edmonton
Pingback: magnet signs edmonton
Pingback: magnetic signs
Pingback: edmonton magnet sign
Pingback: magnet signs edmonton
Pingback: magnet signs edmonton
Pingback: edmonton magnet sign
Pingback: edmonton magnetic signs
Pingback: magnetic signs
Pingback: magnetsigns
Pingback: Medicare Agent Training
Pingback: instagram followers buy
Pingback: buy followers instagram
Pingback: free instagram likes
Pingback: instagram followers hack
Pingback: best instagram followers buy
Pingback: buy likes on instagram
Pingback: followers real
Pingback: instagram buying followers
Pingback: Watch: Only Fools & Horses On 1983 Harty Christmas Special
Pingback: Current Affairs
Pingback: youtube abone satin al
Pingback: youtube kanal abonesi satin alma
Pingback: youtube abone arttir
Pingback: headset com identificador de chamadas
Pingback: youtube kanal abonesi satin alma
Pingback: youtube abone al
Pingback: youtube abone satın alma
Pingback: youtube abone arttırma
Pingback: youtube abone arttırma
Pingback: youtube abone satın alma
Pingback: youtube abone arttir
Pingback: youtube kanal abonesi al
Pingback: youtube abone arttırma
Pingback: youtube kanal abonesi al
Pingback: youtube abone arttırma
Pingback: youtube abone arttırma
Pingback: youtube abone arttırma
Pingback: buy instagram followers
Pingback: beauty sale
Pingback: buy instagram followers
Pingback: buy instagram followers
Pingback: buy followers instagram
Pingback: buy instagram followers
Pingback: famoid buy instagram followers
Pingback: buy instagram followers without paypal
Pingback: instagram followers buy
Pingback: instagram followers buy
Pingback: buy real instagram followers
Pingback: buy instagram followers without paypal
Pingback: buy instagram followers without paypal
Pingback: buy real instagram followers
Pingback: buy followers instagram
Pingback: JMS marine square layout
Pingback: JMS marine square reviews
Pingback: JMS new project sec 102
Pingback: JMS marine square
Pingback: JMS new project sec 102
Pingback: JMS Developers
Pingback: JMS 102 Gurgaon
Pingback: JMS new launch
Pingback: JMS sector 102 Gurgaon
Pingback: Bucharest Escort
Pingback: Escort Romania
Pingback: tela gradil
Pingback: cerca de arame preço
Pingback: Escorts Romania
Pingback: Escort Bucharest
Pingback: Escorts Romania
Pingback: tela de plastico para cerca
Pingback: tela alambrado gerdau
Pingback: belgo salvador
Pingback: Escorte France
Pingback: www belgo bekaert arames com br
Pingback: tela de arame preço metro
Pingback: Escortes France
Pingback: Rencontre Intime
Pingback: arame belgo
Pingback: Escortes France
Pingback: www belgo bekaert arames com br
Pingback: bola de arame
Pingback: tela para cercar terreno preço
Pingback: telas soldadas gerdau
Pingback: Preis für Schlüsselnotdienst
Pingback: guter schlüsseldienst
Pingback: tela para cerca preço
Pingback: tela para cercar terreno preço
Pingback: www belgo bekaert arames com br
Pingback: Schlüsseldienst Blog
Pingback: Feuershow Silberhochzeit
Pingback: Feuershow goldene Hochzeit
Pingback: Feuershow zur hochzeit
Pingback: Decking & Fencing
Pingback: Outdoor Power Tools
Pingback: Furniture Sets
Pingback: Garden Swimming Pools
Pingback: Garden Bird Baths
Pingback: Garden Jacuzzis
Pingback: Swimming Pool Covers
Pingback: Garden Storage & Housing
Pingback: Pressure Washers
Pingback: Steam Cleaners
Pingback: Garden Bird Houses
Pingback: outdoor bargains
Pingback: cabela promotion code
Pingback: body building coupons
Pingback: promo code target
Pingback: abebooks.com coupon code
Pingback: coupon code for snapfish
Pingback: ERP
Pingback: Toiminnanohjausjarjestelma
Pingback: ebags coupon codes
Pingback: Toiminnanohjaus
Pingback: Toiminnanohjaus
Pingback: tatkal software download
Pingback: ERP
Pingback: ERP
Pingback: Field service
Pingback: ERP
Pingback: Scheduling
Pingback: ERP
Pingback: Scheduling
Pingback: Scheduling
Pingback: Scheduling
Pingback: how was hydrocodone discovered
Pingback: Èãðà Ïðåñòîëîâ 7 ñåçîí 8 ñåðèÿ
Pingback: substance abuse treatment
Pingback: substance abuse treatment
Pingback: Stork rental
Pingback: non profit
Pingback: Baby Stork
Pingback: telemedicine
Pingback: youth couch
Pingback: substance abuse treatment
Pingback: non profit
Pingback: Telehealth
Pingback: Storks NJ
Pingback: referral
Pingback: therapy
Pingback: Storks NJ
Pingback: Stork
Pingback: how to eliminate bed bugs
Pingback: bed bug eradication
Pingback: bed bug treatment
Pingback: bed mites
Pingback: where do bed bugs come from
Pingback: how to kill bed bugs
Pingback: where do bed bugs come from
Pingback: bed bug bites treatment
Pingback: bed bug eggs
Pingback: bed bug eggs
Pingback: bed bug eggs
Pingback: can you see bed bugs
Pingback: where do bed bugs come from
Pingback: bed bug eggs
Pingback: substance abuse treatment
Pingback: bed bug treatment
Pingback: timeshare exit
Pingback: sell my timeshare
Pingback: philadelphia eagles led sign
Pingback: corona neon sign
Pingback: led signs pittsburgh
Pingback: Dumpster Rent Pro of San Diego
Pingback: philadelphia eagles led sign
Pingback: San Diego dumpsters
Pingback: dumpster dimensions
Pingback: mental health conditions
Pingback: dumpster rental sizes
Pingback: neon signs dallas
Pingback: behavioral health ehr
Pingback: nascar signs
Pingback: behavior software
Pingback: timeshare transfers
Pingback: waste container rentals
Pingback: dumpster rental
Pingback: get rid of my timeshare
Pingback: Dumpster price San Diego
Pingback: dumpster rental Chula Vista
Pingback: therapy billing software
Pingback: medicare mental health
Pingback: coca cola neon sign
Pingback: mental health disorders
Pingback: trash removal dumpster rental
Pingback: rocket league led sign
Pingback: mental health abbreviations
Pingback: led neon sign
Pingback: therapist helper cost
Pingback: trash bin rental prices
Pingback: rocket league led sign
Pingback: military mental health
Pingback: need a dumpster
Pingback: neon sign
Pingback: dump rental
Pingback: rent a construction dumpster
Pingback: waste removal companies
Pingback: therapist helper reviews
Pingback: 30 yard roll off dumpster
Pingback: timeshare questions
Pingback: waste management dumpster rates
Pingback: dumpster rental mn
Pingback: software practices
Pingback: rent a waste container
Pingback: trash truck
Pingback: big dumpster
Pingback: icanotes
Pingback: healthcare software solutions
Pingback: practise management system
Pingback: professional tax software
Pingback: Bookkeping Service West Des Moines
Pingback: timeshare relief
Pingback: appliance repair saratoga springs
Pingback: appliance repair roy utah
Pingback: quickbooks payroll online
Pingback: affordable appliance repair
Pingback: 24 hour appliance repair
Pingback: CPA West Des Moines
Pingback: appliance repair experts
Pingback: timeshare broker associates
Pingback: free file taxes
Pingback: timeshare cancellation letter
Pingback: e file taxes
Pingback: pitstop appliance repair
Pingback: maytag
Pingback: frigidaire
Pingback: home repairs
Pingback: tax consultant
Pingback: refrigerator repair
Pingback: home appliance repair service
Pingback: kitchenaid dishwasher repair
Pingback: estate planning
Pingback: repair appliance
Pingback: quickbooks support
Pingback: gas dryer repair
Pingback: refrigerator service
Pingback: sample will
Pingback: how to get rid of my wyndham timeshare
Pingback: financial planning magazine
Pingback: tax return calculator
Pingback: timeshare exit
Pingback: garbage bin rental
Pingback: gas stove repair
Pingback: servall appliance
Pingback: appliance repair business
Pingback: aa appliance repair
Pingback: timeshare deed transfer
Pingback: major appliance repair
Pingback: small appliance repair
Pingback: maytag appliance repair
Pingback: dumpster rental
Pingback: 15 yard dumpster
Pingback: appliance repair service
Pingback: dumpster rental Hamilton
Pingback: appliance repair orem utah
Pingback: kitchenaid appliance repair
Pingback: electrical appliance repair
Pingback: trash container rentals
Pingback: samsung refrigerator
Pingback: dumpster rental near me
Pingback: waste management dumpster rental cost
Pingback: appliance repair manuals
Pingback: construction waste
Pingback: trash rental bins
Pingback: trash pick up services
Pingback: maytag oven parts
Pingback: roll away trash containers
Pingback: waste removal dumpster rental
Pingback: debris dumpster
Pingback: maytag repair parts
Pingback: frigidaire dishwasher repair
Pingback: appliance part
Pingback: appliance package deals
Pingback: diamond appliance repair
Pingback: road service
Pingback: dumpster rental Fayetteville
Pingback: dumpster rental
Pingback: dumpster rental Dunwoody
Pingback: heavy truck service
Pingback: tow truck 24 hour
Pingback: trucks with lifts
Pingback: car for junk
Pingback: dumpster rental Sandy Springs
Pingback: balenciaga
Pingback: fuel service
Pingback: order a dumpster
Pingback: southfield townearg company near
Pingback: Tree Trimming Tampa
Pingback: lift and tow
Pingback: 40 yard dumpster rental
Pingback: roll off rental
Pingback: roll back trucks for sale
Pingback: local dumpster rental
Pingback: roll off dumpster sizes
Pingback: breakdown cover
Pingback: get a dumpster
Pingback: rental of dumpster
Pingback: dumpster disposal
Pingback: Melanie Tipton
Pingback: roll off containers for rent
Pingback: Young adults
Pingback: Melanie Tipton
Pingback: Melanie Tipton
Pingback: parts
Pingback: Tree Trimming Tampa
Pingback: Millennial
Pingback: Jesus G.S.
Pingback: waste management bin rental
Pingback: 4x4 flatbed truck
Pingback: used trucks
Pingback: lift pickup truck
Pingback: online Christian store
Pingback: Storm Preparation
Pingback: Christian clothing line
Pingback: Jesus Gift Store
Pingback: Christian store
Pingback: Christian merchandise
Pingback: www.surelifequote.com/
Pingback: Brandon
Pingback: affordable wedding photography perth
Pingback: southwest wedding photographer
Pingback: asian wedding photographer in perth
Pingback: perth wedding photojournalism
Pingback: recommended wedding photographer perth
Pingback: perth affordable wedding photography
Pingback: wedding photographer perth wa
Pingback: margaret river wedding photographer
Pingback: engagement photographer perth
Pingback: perth affordable wedding photography
Pingback: LED mirror
Pingback: VIP Financing Solutions
Pingback: Magnetic wrist bracelets
Pingback: Copper Magnetic Jewelry
Pingback: Magnetic Health Jewelry
Pingback: Mens magnetic therapy jewelry
Pingback: Wellness jewelry
Pingback: therapeutic magnets
Pingback: Copper Magnetic Jewelry
Pingback: dat nen nha be gia re
Pingback: womens magnetic therapy bracelets
Pingback: womens magnetic therapy bracelets
Pingback: Wellness jewelry
Pingback: Magnetic bracelet for energy
Pingback: Mens magnetic therapy jewelry
Pingback: Magnetic therapy bracelets
Pingback: Wellness jewelry
Pingback: Magnetic Therapy Jewelry
Pingback: Best magnetic therapy bracelet
Pingback: Magnetic bracelet for health
Pingback: Magnetic wrist bracelets
Pingback: Magnetic Therapy Jewelry
Pingback: womens magnetic therapy bracelets
Pingback: VIP Financing Solutions
Pingback: Best magnetic therapy bracelet
Pingback: Black magnetic therapy bracelet
Pingback: parking
Pingback: Mens magnetic therapy jewelry
Pingback: Magnetic wrist bracelets
Pingback: Wellness jewelry
Pingback: Best magnetic therapy bracelet
Pingback: Photo backup
Pingback: Best magnetic therapy bracelet
Pingback: Black magnetic therapy bracelet
Pingback: vietnam visa
Pingback: Professional Retouch
Pingback: EU Policy 70 Risk Assessment
Pingback: cheap photo retouch services
Pingback: Clinical Trial Transparency
Pingback: Website
Pingback: More About
Pingback: Quantitative Risk Assessment
Pingback: professional airbrush
Pingback: Photoshop Tutorials
Pingback: Brighten Skin
Pingback: Sandy Hook
Pingback: photo background removal
Pingback: Photoshop Tutorials
Pingback: Facial Retouch
Pingback: Chill Beat
Pingback: professional photo editing
Pingback: photo retouch services
Pingback: kpss çýkmýþ sorular
Pingback: kpss çýkmýþ sorular
Pingback: kpss genel kültür
Pingback: kpss güncel bilgiler
Pingback: kpss genel kültür
Pingback: kpss ilkler
Pingback: kpss güncel bilgiler
Pingback: kpss tarih sorularý
Pingback: Leonard Pozner
Pingback: buy Bitcoins
Pingback: Sandy Hook Shooting
Pingback: Leonard Pozner
Pingback: Sandy Hook Shooting
Pingback: test bank
Pingback: Sandy Hook Shooting
Pingback: Wolfgang Halbig
Pingback: Lenny Pozner
Pingback: Wolfgang Halbig
Pingback: instagram nasıl takipçi satın alınır
Pingback: Lenny Pozner
Pingback: Sandy Hook Shooting
Pingback: instagram takipçi satın alma crovu
Pingback: instagram takipçi satın alma crovu
Pingback: Wolfgang Halbig
Pingback: instagram takipçi satın alın
Pingback: instagram takipçi satın al
Pingback: Eliezer Pozner
Pingback: instagram takipçi satın alma
Pingback: instagram takipci satin al
Pingback: instagram takipçi satın alma
Pingback: Sandy Hook Shooting
Pingback: instagram takipçi satın alma crovu
Pingback: Eliezer Pozner
Pingback: instagram takipci satin alin
Pingback: instagram takipçi satın alma
Pingback: Sandy Hook Shooting
Pingback: instagram takipçi al
Pingback: dog whining
Pingback: Wolfgang Halbig
Pingback: Lenny Pozner
Pingback: Export
Pingback: South Yorkshire
Pingback: Doncaster
Pingback: Manual
Pingback: Saloons
Pingback: Family Business
Pingback: 01405 457359
Pingback: best wedding photographers and photography perth
Pingback: Eliezer Pozner
Pingback: Leonard Pozner
Pingback: Leonard Pozner
Pingback: Ebay Deals on Diamond Rings
Pingback: Gaming
Pingback: Freezer pack
Pingback: Cristobal Sane
Pingback: Cool pack
Pingback: Diamond Engagement Ring for sale
Pingback: Mariann Mcdavis
Pingback: Ice pack
Pingback: Inocencia Blaker
Pingback: Darline Kunst
Pingback: Pre-owned Diamond Engagement Ring
Pingback: Ice pack
Pingback: Teodoro Marenco
Pingback: Johnna Nunnally
Pingback: Cleora Pilling
Pingback: Leighann Deines
Pingback: Ebay Deals on Diamond Rings
Pingback: Teofila Yetman
Pingback: Adelaida Pillot
Pingback: Randal Ousley
Pingback: Katelin Vanzile
Pingback: Dusty Sitzes
Pingback: Randi Farone
Pingback: 14k White Gold Diamond Ring
Pingback: Georgette Loiacono
Pingback: Ebay Deal on Engagement Ring Diamond
Pingback: DoubleDown Casino Promo Codes
Pingback: Jeffreestarcosmetics Promo Code March 2018
Pingback: Dickssportinggoods Coupons
Pingback: Wanda Kuehn
Pingback: Maxie Wingham
Pingback: Kaila Brockman
Pingback: Freezer pack
Pingback: 20 % Off Cult Beauty Discount Code 2018
Pingback: Diamond Engagement Ring for sale
Pingback: Jeffreestarcosmetics Promo Code March 2018
Pingback: Ebay Deals on Diamond Rings
Pingback: Promo Code 2018
Pingback: 20 % Off Cult Beauty Discount Code 2018
Pingback: Frost pack
Pingback: Promo Code For 2018
Pingback: 14k White Gold Diamond Ring
Pingback: kaufen EU führerschein
Pingback: spam
Pingback: Promo Code 2018
Pingback: Promo Code
Pingback: Ebay Deal on Engagement Ring Diamond
Pingback: Norwegen Kanada
Pingback: Diplome und andere Produkte für
Pingback: DoubleDown Casino Promo Codes
Pingback: Lean Belly Breakthrough
Pingback: Deutschland
Pingback: Mexiko
Pingback: spam
Pingback: pass ((WHATSAPP : + 1412-385-7163))
Pingback: Frankreich
Pingback: Engagement Diamond Ring
Pingback: Israel
Pingback: Diamond Solitaire Ring
Pingback: Niederlande
Pingback: Ausweise und andere Ausweispapiere
Pingback: Führerschein
Pingback: Ebay Deal on Engagement Ring Diamond
Pingback: 14k White Gold Diamond Ring
Pingback: phazz music
Pingback: Frost pack
Pingback: Ice pack
Pingback: Ice pack
Pingback: Ice pack
Pingback: Freezer pack
Pingback: Frost pack
Pingback: decals
Pingback: sticker wallpaper
Pingback: wall quotes
Pingback: yarra valley wine tours
Pingback: sticker wallpaper
Pingback: tree wall decal
Pingback: decals
Pingback: decals
Pingback: wall stencils
Pingback: Freezer pack
Pingback: Ice pack
Pingback: 3d wall stickers
Pingback: B2B Marketing
Pingback: Agile marketing
Pingback: sticker wallpaper
Pingback: Shukawi
Pingback: marketing services
Pingback: decals
Pingback: tree wall decal
Pingback: Freezer pack
Pingback: 3d wall stickers
Pingback: B2B Marketing
Pingback: Petrodollar Collapse
Pingback: Silver Investing
Pingback: Terry Sacka AAMS
Pingback: gold investment
Pingback: marketing services
Pingback: Marketing Center of excellence
Pingback: silver investment
Pingback: 7 Cycles of Empire
Pingback: Real Price Silver
Pingback: His comments were
Pingback: best marketing agency in New York
Pingback: marketing services
Pingback: Limo Hire Nottingham
Pingback: Agile marketing
Pingback: Mesotherapy Manchester
Pingback: Cornerstone Crowns
Pingback: Gold Investing
Pingback: Online shopping deals
Pingback: Asset Preservation
Pingback: buy electronics online
Pingback: sports equipment deals
Pingback: Terry Sacka AAMS
Pingback: houses4rentflorida.com
Pingback: Four Blood Moons date
Pingback: Video Link
Pingback: Terry Sacka AAMS
Pingback: skin care sets
Pingback: buy mens accessories online
Pingback: events in September 2015
Pingback: buy kids furniture online
Pingback: Blogpost
Pingback: houses 4 rent florida
Pingback: Syrian Refugee Immigration
Pingback: Global Market System
Pingback: parceria
Pingback: Conflict Resolution
Pingback: Timesharing Florida
Pingback: Florida Divorce Attorney
Pingback: fotografia
Pingback: telford escort
Pingback: livros
Pingback: joana dark
Pingback: filmes
Pingback: yarra valley wine tours & best yarra valley wine tours
Pingback: filmes
Pingback: viagem
Pingback: Palm Beach Gardens
Pingback: viagem
Pingback: Click here
Pingback: telford escorts
Pingback: Alimony
Pingback: Divorce Forms
Pingback: Homepage
Pingback: birmingham escort agency
Pingback: Miami
Pingback: Florida Divorce Law
Pingback: Divorce Lawyer
Pingback: Go Here
Pingback: web designer adelaide
Pingback: Learn More
Pingback: Read More
Pingback: Read This
Pingback: Click to learn more
Pingback: Read More
Pingback: Read This
Pingback: Find Out More
Pingback: Clicking Here
Pingback: Go Here
Pingback: Going Here
Pingback: Going Here
Pingback: Read More
Pingback: Go Here
Pingback: information security
Pingback: Read This
Pingback: Learn More
Pingback: Car Accident Replacement Vehicle
Pingback: Clicking Here
Pingback: Read More Here
Pingback: Read This
Pingback: Share Transportation MA
Pingback: Sandy Hook Shooting
Pingback: cpasbien
Pingback: Sandy Hook Shooting
Pingback: Sandy Hook Shooting
Pingback: Hindu baby girl names
Pingback: ?baby girl names
Pingback: Hindu baby girl names
Pingback: chalis
Pingback: valium for sale
Pingback: porn
Pingback: chalis
Pingback: viagra for sale
Pingback: docce orizzontali
Pingback: viagra
Pingback: instagram takipçi satın alın
Pingback: instagram takipçi satın alma crovu
Pingback: instagram nasıl takipçi satın alınır
Pingback: instagram takipçi satın al
Pingback: instagram takipci satin almak
Pingback: instagram takipci almak
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: work from home
Pingback: Donate Shooting
Pingback: More Information
Pingback: Our Daily Bread Devotional Reading for Today
Pingback: AR/VR
Pingback: availability
Pingback: incident response/recovery
Pingback: work from home
Pingback: detroit housing
Pingback: furnished apartments in michigan
Pingback: townhomes for rent in michigan
Pingback: condos in michigan
Pingback: intro to prostate kit
Pingback: buy real instagram views
Pingback: buy real instagram views
Pingback: buy instagram views
Pingback: buy views on instagram
Pingback: buy instagram video views
Pingback: instagram views
Pingback: apartments for rent in oahu
Pingback: michigan housing locator
Pingback: instagram quality views
Pingback: instagram views
Pingback: apartments for rent in detroit area
Pingback: 3 bedroom houses for rent in detroit michigan
Pingback: homes for rent in west michigan
Pingback: buy real instagram views
Pingback: buy views on instagram
Pingback: buy instagram video views
Pingback: buy instagram views
Pingback: buy real instagram views
Pingback: buy instagram views
Pingback: rabbit sex toy
Pingback: modern apartments in michigan
Pingback: apartments for rent in wisconsin
Pingback: apartments on the westside of detroit
Pingback: luxury condos for rent in michigan
Pingback: SEO DALLAS
Pingback: Dallas Search Engine Optimization
Pingback: homes for rent northern mi
Pingback: 2 bedroom apartments for rent detroit mi
Pingback: available apartments in detroit
Pingback: lofts for rent detroit mi
Pingback: northern michigan apartments
Pingback: Dallas Search Engine Optimization
Pingback: 4 bedroom houses for rent in detroit
Pingback: Dallas SEO AGENCY
Pingback: Bridal Cathedral Veils
Pingback: Wedding Fingertip Veils
Pingback: Dallas Search Engine Optimization
Pingback: Bridal GLOVES
Pingback: affordable townhomes in michigan
Pingback: cheap houses for rent in detroit mi
Pingback: Bridal Cathedral Veils
Pingback: ptz camera
Pingback: wireless cctv camera
Pingback: security camera price
Pingback: house security system
Pingback: Bridal Tiara Combs
Pingback: cctv security cameras
Pingback: Wedding Jewelry & Tiara Sets
Pingback: cctv camera for home security
Pingback: home video security
Pingback: Banner Printing
Pingback: Pull Up Banner Stand
Pingback: Portable Backdrop Display
Pingback: Roll Up Banner Stand
Pingback: Portable Exhibition Stand
Pingback: door sensor
Pingback: Portable Exhibition Stand
Pingback: security camera packages
Pingback: Donate Shooting
Pingback: residential alarm systems
Pingback: Pop Up Backdrop
Pingback: home security products
Pingback: pinhole spy camera
Pingback: mini spy camera
Pingback: Roll Up Banner Stand
Pingback: Banner Printing
Pingback: cctv and security systems
Pingback: security and surveillance
Pingback: Brochure Stand
Pingback: camera and security systems
Pingback: Poster Printing
Pingback: garbage dumpster
Pingback: dumpster rental White
Pingback: Pull Up Banner
Pingback: rent a dumpster
Pingback: waste dumpster rental
Pingback: junk pick up
Pingback: dumpster service
Pingback: Pull Up Banner
Pingback: trash hauling
Pingback: trash dumpsters for rent
Pingback: rent dumpster prices
Pingback: Retractable Stand
Pingback: Poster Printing
Pingback: garbage dumpster rental prices
Pingback: Portable Display Stand
Pingback: i need a dumpster rental
Pingback: waste management bin rental
Pingback: rent dumpster prices
Pingback: dumpster rates
Pingback: waste disposal containers
Pingback: garbage rental
Pingback: temporary dumpster
Pingback: dumpster pick up
Pingback: roll off containers for rent
Pingback: garbage disposal bins
Pingback: yard debris removal
Pingback: Bookkeping Service Ankeny
Pingback: free tax advice
Pingback: Accounting and Payroll Ankeny
Pingback: free online tax preparation
Pingback: Bookkeping Service Clive
Pingback: Tax Preparation West Des Moines
Pingback: cpa marketing
Pingback: Accountant Johnston
Pingback: Small Business Accounting Urbandale
Pingback: Accountant Des Moines
Pingback: payroll check
Pingback: free online taxes
Pingback: 2015 taxes
Pingback: 2015 tax forms
Pingback: 2015 federal tax forms
Pingback: online accounting software
Pingback: quickbooks free
Pingback: quickbooks payroll support
Pingback: free federal tax filing
Pingback: file state taxes
Pingback: will lawyer
Pingback: enrolled agent
Pingback: tax preparation near me
Pingback: estimated tax calculator
Pingback: taxes for free
Pingback: ?????Σ ?ΣΦ?????Σ ?Θ???
Pingback: Android News
Pingback: Android Phones
Pingback: Technology News
Pingback: buy vpn
Pingback: fitnet
Pingback: vpn
Pingback: virtual private network
Pingback: vpn
Pingback: best porn
Pingback: gta 5 money cheat ps4 code
Pingback: gta san andreas xbox cheats
Pingback: mods e cheats gta san andreas
Pingback: gta 4 cheats ps3 tank cheat code
Pingback: gta 5 cheats xbox 360 unlock map
Pingback: gta san andreas pc cheats unblocked
Pingback: gta 3 cheats on playstation
Pingback: gta vice city rage cheats pc
Pingback: gta 4 eflc tbogt cheats pc
Pingback: gta 3 cheats pc wiki
Pingback: karcher-foam-gun-kit-lavaggio-eco
Pingback: Poker party staffing South Florida
Pingback: insta-finish-fabric-spot-remover
Pingback: Cheapest casino companies South Florida
Pingback: vacuum-cleaner
Pingback: buffingmachine
Pingback: detailers-kart-tool-kart-from-auto-tool
Pingback: rubbing-compounds
Pingback: app-black-hex-pad-7-5-inch-dia190mm-finishing-polishing
Pingback: wrc-beige-door-guard
Pingback: Local poker tournament planners South Florida
Pingback: 3m-double-sided-tape-1-roll-of-24-mm-x-4-mtr
Pingback: Charity poker night planners South Florida
Pingback: meguiar-s-7-inch-rotary-foam-polishing-pads
Pingback: dr-marcus-senso-deluxe-black-gel-perfume-for-car-50-ml
Pingback: 3-inch-wool-loop-pad-yellow
Pingback: bumper-protection
Pingback: wiper-blade-16-inch-without-blade
Pingback: Hire blackjack dealers South Florida
Pingback: Hire blackjack dealer South Florida
Pingback: Hire poker dealer South Florida
Pingback: Poker services company South Florida
Pingback: Poker event staffing South Florida
Pingback: Local casino night companies South Florida
Pingback: Charity poker night planners South Florida
Pingback: Poker charity fundraisers South Florida
Pingback: Hire local poker dealers South Florida
Pingback: Best local casino night companies South Florida
Pingback: Blackjack dealers for hire
Pingback: Flats for rent in Riyadh
Pingback: Rooms for rent in Riyadh Saudi Arabia
Pingback: flats for rent in Jeddah
Pingback: flats for rent or sell in Riyadh Saudi arabia
Pingback: single rooms for rent in Jeddah
Pingback: Add your property or real estate advertisement
Pingback: eternity wedding band
Pingback: Unique diamond rings
Pingback: soft wash
Pingback: sapphire engagement rings
Pingback: wedding bands
Pingback: cushion diamond ring
Pingback: wedding bands
Pingback: Harum Singapore Online Perfume Store
Pingback: no pressure roof cleaning
Pingback: professional roof cleaning
Pingback: Bridal Cathedral Veils
Pingback: Wedding Jewelry & Tiara Sets
Pingback: Wedding Tiaras
Pingback: Bridal GLOVES
Pingback: Bridal Mantilla Veils
Pingback: zpravodajstv?
Pingback: soft wash
Pingback: roof soft wash
Pingback: Wakanda Forever
Pingback: metal roof cleaning
Pingback: Caliberhitter
Pingback: buying instagram likes
Pingback: instagram likes real
Pingback: click here to read
Pingback: instagram likes buy
Pingback: you should read that
Pingback: soft wash
Pingback: you should read that
Pingback: you must read about that
Pingback: why instagram likes is important
Pingback: you need to buy instagram likes
Pingback: buy real instagram likes
Pingback: you should read that
Pingback: instagram likes to buy
Pingback: buy real instagram likes
Pingback: instagram likes to buy
Pingback: instagram likes real
Pingback: buying instagram likes
Pingback: shingle roof cleaning
Pingback: instagram likes to buy
Pingback: considering to buy ig likes?
Pingback: professional roof cleaning sarasota
Pingback: ESSAY3
Pingback: www.entertainmentkiraat.com/tag/padma-shri/
Pingback: ESSAY3
Pingback: ESSAY3
Pingback: www.entertainmentkiraat.com/tag/india-pakistan-border/
Pingback: ESSAY3
Pingback: ESSAY3
Pingback: ESSAY3
Pingback: ESSAY3
Pingback: ESSAY3
Pingback: www.entertainmentkiraat.com/tag/taimur-ali-khan/
Pingback: ESSAY3.PRO
Pingback: ESSAY3.PRO
Pingback: www.entertainmentkiraat.com/tag/current-affairs/
Pingback: ESSAY3.PRO
Pingback: ESSAY3.PRO
Pingback: www.entertainmentkiraat.com/tag/telangana-naxal-violence/
Pingback: ESSAY3.PRO
Pingback: ESSAY3.PRO
Pingback: www.entertainmentkiraat.com/tag/indian-national-flag/
Pingback: www.entertainmentkiraat.com/tag/-/
Pingback: www.entertainmentkiraat.com/tag/array/
Pingback: ESSAY3.PRO
Pingback: ESSAY3.PRO
Pingback: top engagement rings
Pingback: www.entertainmentkiraat.com/tag/gst-rate-on-pre-owned-cars/
Pingback: www.entertainmentkiraat.com/tag/bagamathie-movie/
Pingback: www.entertainmentkiraat.com/tag/women-security/
Pingback: www.entertainmentkiraat.com/tag/rakesh-jhunjhunwala/
Pingback: best diamond ring on ebay
Pingback: beautiful engagement ring
Pingback: Dewhurst
Pingback: Trafalgar
Pingback: Menzies Creek
Pingback: MODELING
Pingback: golf course
Pingback: Safest cryptocurrency hard wallets
Pingback: game
Pingback: golf clubs
Pingback: Buy Altcoins from the top Cryptocurrency exchanges
Pingback: Altcoins
Pingback: Cryptocurrency
Pingback: Crypto Mining
Pingback: game
Pingback: golf course
Pingback: golf score
Pingback: Learn to invest in ICO's
Pingback: golf score
Pingback: golf clubs
Pingback: golf game
Pingback: Learn to trade Altcoins,
Pingback: Watch Full Movies Online Free
Pingback: discount golf
Pingback: golf score
Pingback: golf clubs for sale
Pingback: Learn cryptocurrency
Pingback: Block Chain Technology
Pingback: Selling Crypto
Pingback: golf clubs
Pingback: Detroit florist
Pingback: Michigan wedding planner
Pingback: Learn how to invest in Bitcoin,
Pingback: Selling Crypto
Pingback: Kalamazoo wedding planner
Pingback: classique vibrator review
Pingback: How to buy altcoins
Pingback: Detroit wedding planner
Pingback: Cryptocurrency exchanges
Pingback: Learn how to invest in Bitcoin,
Pingback: Michigan wedding planner
Pingback: Learn bitcoin videos
Pingback: Michigan wedding planner
Pingback: Altcoins
Pingback: Bitcoin Videos
Pingback: Buy Bitcoin from verified exchange
Pingback: Cryptocurrency market
Pingback: clitoris
Pingback: Detroit florist
Pingback: Detroit wedding planner
Pingback: Detroit invitation designer
Pingback: Detroit invitation designer
Pingback: Buy Altcoins from the top Cryptocurrency exchanges
Pingback: Kalamazoo wedding planner
Pingback: Crypto Mining
Pingback: Detroit invitation designer
Pingback: Michigan wedding planner
Pingback: Buy Altcoins from the top Cryptocurrency exchanges
Pingback: ohmibod lovelife adventure triple stimulation vibe
Pingback: ICO's
Pingback: Teeth Whitening
Pingback: White Teeth
Pingback: Learn about bitcoin, Altcoins and the Blockchain technology.
Pingback: Best Teeth Whitening Kit
Pingback: Crypto Mining
Pingback: The best ways to get started in the cryptocurrency market today.
Pingback: Best Teeth Whitening Kit
Pingback: Teeth Whitening
Pingback: Teeth Whitening Kit
Pingback: Cryptocurrency exchanges
Pingback: Block Chain Technology
Pingback: Block Chain Technology
Pingback: Teeth Whitening Kit
Pingback: ICO's
Pingback: White Teeth
Pingback: realistic dildo
Pingback: White Teeth
Pingback: prostate massagers
Pingback: kovovyroba
Pingback: manutencoes preventivas
Pingback: dicas desentupimentos conselhos uteis
Pingback: desentupimentos aveleda
Pingback: limpeza de fossas porto
Pingback: noticias desentope porto
Pingback: desentupimentos porto
Pingback: desentupimentos gaia
Pingback: desentupimentos figueira
Pingback: desentupimentos fonte arcada
Pingback: desentupimentos alvarenga
Pingback: desentupimentos lagares
Pingback: desentupimentos vila cova
Pingback: desentupimentos paco de sousa
Pingback: desentupimentos pias
Pingback: desentupimentos casteloes
Pingback: desentupimentos irivo
Pingback: desentupimentos cabeca santa
Pingback: Jalaram Khichdi
Pingback: island
Pingback: Business Ideas
Pingback: can't believe God believe
Pingback: Train your mind
Pingback: Talk to our selves
Pingback: Golden Temple
Pingback: Anger Destroy relationships
Pingback: Talk to our selves
Pingback: open door to forgiveness
Pingback: practical ways apply spirituality life
Pingback: start morning good vibes
Pingback: Radhe Maa
Pingback: service and sacrifice
Pingback: the path to enlightenment
Pingback: life is a pilgrimage
Pingback: journey darkness light
Pingback: serving God service truth
Pingback: copper processing plant
Pingback: funny games
Pingback: ponchos family pack
Pingback: rain ponchos
Pingback: ponchos
Pingback: throw away ponchos
Pingback: best affordable website design companies
Pingback: affordable website design packages
Pingback: web design nyc
Pingback: emergency poncho
Pingback: Insurance agency management software
Pingback: cheap website design services
Pingback: insurance broker software
Pingback: ny web designer
Pingback: insurance commission tracking software
Pingback: carrier productivity solution
Pingback: Insurance agency management software
Pingback: carrier productivity solution
Pingback: car wreckers hamilton
Pingback: Car wreckers waikato
Pingback: carrier productivity solution
Pingback: carrier productivity software
Pingback: insurance commission tracking software
Pingback: insurance broker software
Pingback: wreckers nz
Pingback: car wreckers hamilton
Pingback: Snap Dismantlers
Pingback: carrier productivity software
Pingback: best insurance agency broker software
Pingback: carrier productivity solution
Pingback: CRM insurance
Pingback: insurance commission tracking software
Pingback: car wreckers rotorua
Pingback: snap dismantlers
Pingback: insurance commission tracking software
Pingback: Black Girl Magic T Shirt
Pingback: Influencers
Pingback: Influencer marketing
Pingback: Hire celebrity
Pingback: Hire influencer
Pingback: giant dildo
Pingback: Grawerowanie
Pingback: sinclair vibrator
Pingback: how to get ready for anal
Pingback: clone-a-willy
Pingback: anal sex toy
Pingback: Xplorer LED Driving Light
Pingback: hyperdrive Led Driving light
Pingback: telford escort agency
Pingback: birmingham escort agency
Pingback: Navigator bar Driving Light
Pingback: LightSYNC
Pingback: coventry escort agency
Pingback: personal trainer birmingham
Pingback: cupping birmingham
Pingback: Mirror Jewelry Wall Mount Cabinet Storage Organizer
Pingback: Pull Up Chin Up Bar Ceiling Mount Workout Fitness Exercise
Pingback: painters and decorators london
Pingback: web design birmingham
Pingback: Hoppe Gun Bore Cleaner Cleaning
Pingback: Printer Toner Cartridge Ink Canon ImageClass
Pingback: Bathroom Sink Faucet
Pingback: vibrator challenge but greater challenge
Pingback: wholesale used tires by container
Pingback: wholesale used tires by container
Pingback: vibrator massager
Pingback: part worn tyres wholesale germany
Pingback: how to use the adam and eve bullett
Pingback: masturbator meski
Pingback: Felt Flowers
Pingback: download lagu
Pingback: text
Pingback: cruise to bali
Pingback: hyip monitor
Pingback: companies house webcheck name
Pingback: cruise to st thomas
Pingback: Noah Pozner
Pingback: webcheck company
Pingback: specialty cruises
Pingback: cruise to taormina
Pingback: news/av/magazine-39458098/father-of-sandy-hook-victim-fights-conspiracy-theorists
Pingback: company formation
Pingback: ewf companies house
Pingback: cruise to arles france
Pingback: news/av/magazine-39458098/father-of-sandy-hook-victim-fights-conspiracy-theorists
Pingback: cheap business address
Pingback: service address
Pingback: news/av/magazine-39458098/father-of-sandy-hook-victim-fights-conspiracy-theorists
Pingback: cruise to regensburg
Pingback: st thomas usvi cruises
Pingback: business deal with support
Pingback: virtual offices uk
Pingback: cruise to memphis
Pingback: cruise to san juan
Pingback: cheapest virtual office
Pingback: cruise to istanbul
Pingback: virtual office london
Pingback: tips for cruising solo
Pingback: Noah Pozner
Pingback: youth service bureau software
Pingback: sexual assault tracking for colleges
Pingback: virtual office provider in uk
Pingback: Noah Pozner
Pingback: Title IX software
Pingback: gel pomade
Pingback: hanz de fuko
Pingback: sponge wax
Pingback: hair loss
Pingback: case management software update
Pingback: hair clay
Pingback: domestic violence
Pingback: hair paste
Pingback: Clery Act Software
Pingback: residential services
Pingback: Mariann Mcdavis
Pingback: Oneida Kahler
Pingback: Cleora Pilling
Pingback: case management software update
Pingback: matte pomade
Pingback: Georgine Jasso
Pingback: Kary Oh
Pingback: treatment styling balm
Pingback: Sherrill Zabel
Pingback: hanz de fuko
Pingback: solid cologne uk
Pingback: Randal Ousley
Pingback: texture powder
Pingback: tom henricksen
Pingback: escape the 9 to 5
Pingback: jeffrey kelly
Pingback: Hilde Muniz
Pingback: sidekick
Pingback: welcome entrepreneurs
Pingback: four hour body
Pingback: hug wraps
Pingback: treatment styling balm
Pingback: sidekick
Pingback: original styling meraki
Pingback: Rosina Howser
Pingback: Bronwyn Hoye
Pingback: Sebrina Weiss
Pingback: lisa barrington
Pingback: natural beeswax pomade
Pingback: Leena Yale
Pingback: the twelve days of internet marketing christmas
Pingback: solid cologne uk
Pingback: agents change 2016
Pingback: matte pomade
Pingback: paige arnof fenn
Pingback: Georgette Loiacono
Pingback: hair loss
Pingback: indian wedding presents
Pingback: india
Pingback: wedding ceremony
Pingback: seven vows saat phera
Pingback: wedding ceremony
Pingback: indian wedding invitations
Pingback: hair loss
Pingback: resort accommodations
Pingback: office ally practice mate
Pingback: solah shringar for an indian bride
Pingback: the mangalsutra
Pingback: indian wedding invitations
Pingback: raas garba a sangeet party
Pingback: stunning
Pingback: birthday cake delivery
Pingback: order cake online
Pingback: marina del rey rent a boat
Pingback: clipping path in photoshop
Pingback: bathroom remodel
Pingback: painting interior doors
Pingback: personalised birthday cakes
Pingback: drywall sander
Pingback: drywall installation
Pingback: drywall ceiling
Pingback: clipping path indesign
Pingback: birthday cake delivery
Pingback: drywall tools
Pingback: clipping path in photoshop
Pingback: interior painting tips
Pingback: birthday cake decorations
Pingback: IT Support Services San Diego
Pingback: fixing drywall cracks
Pingback: drywall materials
Pingback: Youtube Mp3
Pingback: painting drywall
Pingback: removing drywall
Pingback: local drywall contractors
Pingback: drywall tape repair
Pingback: Youtube to Mp3
Pingback: drywall contractors near me
Pingback: repair drywall ceiling
Pingback: Youtube to Mp3
Pingback: Youtube Mp3 downloader
Pingback: exterior painting estimate
Pingback: wallpaper contractor
Pingback: painting contractor supplies
Pingback: clit stimulator
Pingback: drywall contractors mn
Pingback: Youtube to Mp3
Pingback: drywall plaster repair
Pingback: marina del rey rent a boat
Pingback: drywall hangers near me
Pingback: painting contractor salary
Pingback: home décor
Pingback: painting bids
Pingback: residential drywall contractors
Pingback: wall décor
Pingback: local painting companies
Pingback: wall art
Pingback: residential duct cleaning
Pingback: clean air duct treatment
Pingback: housekeeping services
Pingback: air duct cleaning methods
Pingback: quality air duct cleaning
Pingback: wall decoration
Pingback: wall decoration
Pingback: Elk Grove Heating and cooling service
Pingback: apartment decorating
Pingback: area carpet cleaning service
Pingback: clipping path service
Pingback: clipping path
Pingback: apartment decorating
Pingback: remote control sex toys
Pingback: how to clean the carpet
Pingback: clipping path illustrator
Pingback: clipping path in indesign
Pingback: clipping path india
Pingback: air conditioner ductwork
Pingback: clipping paths
Pingback: air duct service
Pingback: bedroom design
Pingback: clipping path indesign
Pingback: air conditioning vent cleaning
Pingback: how to clean air conditioning ducts and vents
Pingback: cleaning reviews
Pingback: how to clean your vents
Pingback: air vent cleaning service
Pingback: healthy life
Pingback: sacramento cleaning
Pingback: psychology billing software
Pingback: importance of mental health
Pingback: therapy management software
Pingback: mental health questions
Pingback: mental health statistics
Pingback: mental health management software
Pingback: mental health illnesses
Pingback: therapy notes cost
Pingback: what is positive mental health
Pingback: private practice billing software
Pingback: ehr mental health
Pingback: mental health stress
Pingback: therapy notes cost
Pingback: therapy appointment software
Pingback: mental health codes
Pingback: healthcare software companies
Pingback: emr healthcare software
Pingback: mental health baltimore
Pingback: scheduling and billing
Pingback: physical therapy billing software
Pingback: meditation
Pingback: mobile roadside assistance
Pingback: towing service provider in southfield
Pingback: emergency roadside assistance near ecorse
Pingback: wreckers
Pingback: fuel service
Pingback: list of car insurance companies
Pingback: car insurance quote online
Pingback: local car insurance companies
Pingback: rent a flatbed tow truck
Pingback: paragon roadside assistance
Pingback: towing forks
Pingback: auto wrecker near hazel park
Pingback: used wrecker bodies
Pingback: service provider in midtown
Pingback: used wrecker bodies
Pingback: man tow truck
Pingback: heavy duty wrecker for sale
Pingback: cheap 24 hour towing
Pingback: tow
Pingback: all car parts
Pingback: pick and tow
Pingback: wrecker towing
Pingback: rosedale park townearg near
Pingback: crosby hooks
Pingback: overhead lifting
Pingback: where to buy a tow truck
Pingback: kuplex chain
Pingback: tow truck company near detroit mi
Pingback: dj music mp3 download
Pingback: free download travis scott and quavo album 1
Pingback: Airport transfer
Pingback: download music mp3 files
Pingback: good website to download music
Pingback: place to download free music
Pingback: free hiphop beats download mp3
Pingback: best dance music mp3 download free
Pingback: copyright music download
Pingback: dj music mp3 download
Pingback: places to download free music
Pingback: free download travis scott and quavo album 1
Pingback: mp3 free music download
Pingback: album music download
Pingback: latest hip hop and r&b songs
Pingback: South Africa Music
Pingback: MP3 download
Pingback: download flame clouds speacial ep 1
Pingback: Latest south african music
Pingback: copyright music download
Pingback: copyright music download
Pingback: music on hold download
Pingback: best dance music mp3 download free
Pingback: Kaalia
Pingback: place to download free music
Pingback: Latest south african music
Pingback: download site music
Pingback: Kaalia Modeling Agency
Pingback: Best Modelling agency in India
Pingback: Crazy Bulk Reviews - Is it a Scam or Legit?
Pingback: Crazy Bulk Review - Are The Best Legal Steroids Legit or Scam?
Pingback: Kaalia Modeling Agency
Pingback: water filter for shower
Pingback: Kaalia
Pingback: Kaalia Modelling
Pingback: Kaalia Modelling
Pingback: Crazy Bulk Reviews: the Truth [EXPOSED]
Pingback: Kaalia
Pingback: Crazy Bulk Reviews - Get The Truth And Hard Facts Here
Pingback: Best Modelling agency in India
Pingback: CrazyBulk Winsol (Winidrol) SHOCKING Reviews 2018
Pingback: High Quality Phone Cases for iPhone 8
Pingback: Crazy Bulk Review 2018: Does It Work?
Pingback: Wonderful Phone Cases for iPhone 5s
Pingback: Phone Cases made in USA for iPhone 4s
Pingback: Are Crazy Bulk supplements a scam?
Pingback: Phone Cases made in USA for iPhone 8 plus
Pingback: Phone Cases made in USA
Pingback: High Quality Leggings for Gym
Pingback: Beautiful Leggings for Gym
Pingback: Phone Cases made in USA for iPhone 7
Pingback: Phone Cases made in USA
Pingback: Amazing Tshirts
Pingback: High Quality Phone Cases for iPhone 5
Pingback: Catchy Phone Cases for iPhone 6 plus
Pingback: how buy lubricant
Pingback: bondage and sex
Pingback: best body wand
Pingback: wallpapers for iphone
Pingback: Reklamy
Pingback: Adam & Eve Silicone Recharge Bunny
Pingback: New Tires
Pingback: best strap on
Pingback: sex whip
Pingback: Garage Door Services
Pingback: Garage Door Services
Pingback: Emergency Garage Door Repair
Pingback: Garage Door Company
Pingback: click here
Pingback: click here
Pingback: check now
Pingback: errorfixzone.jimdo.com
Pingback: go to solution
Pingback: Learn More Here
Pingback: Learn More Here
Pingback: Read More Here
Pingback: check now
Pingback: go to solution
Pingback: Find Out More
Pingback: errorfixzone.jimdo.com
Pingback: check now
Pingback: Learn More
Pingback: Discover More Here
Pingback: Read More Here
Pingback: click here
Pingback: click here
Pingback: check now
Pingback: click here
Pingback: check now
Pingback: Read More
Pingback: click here
Pingback: Discover More Here
Pingback: Find Out More
Pingback: click here for solution
Pingback: click here
Pingback: Going Here
Pingback: click here
Pingback: go to solution
Pingback: kerala houseboat tour packages
Pingback: kerala holiday packages
Pingback: Discover More Here
Pingback: Clicking Here
Pingback: best tourist operator in kerala
Pingback: Discover More Here
Pingback: Read More Here
Pingback: kerala holiday packages
Pingback: Find Out More
Pingback: holiday packages for munnar
Pingback: kerala outstation taxi service
Pingback: Ayurveda packages in kerala
Pingback: kerala tour packages wit price
Pingback: cheapest kerala packages
Pingback: famous tour operators in kerala
Pingback: best tourist operator in kerala
Pingback: munnar tour packages from kochi
Pingback: adam and eve the dancing dolphin
Pingback: investing in bitcoin
Pingback: What is Crazy Bulk
Pingback: Crazy Bulk Video Review
Pingback: Peppa
Pingback: Coloring
Pingback: Color
Pingback: Peppa Pig
Pingback: Color
Pingback: A
Pingback: Coloring Pages
Pingback: Garage Door Repair
Pingback: Peppa
Pingback: Coloring Pages
Pingback: Peppa Pig
Pingback: Garage Door Service
Pingback: Peppa
Pingback: Garage Door Spring Repair
Pingback: Garage Door Spring Repair
Pingback: peppapig
Pingback: Peppa Pig
Pingback: Garage Door Repair
Pingback: Color Markers
Pingback: top sex toy for women
Pingback: Garage Door Company
Pingback: Champion Garage Door Repair
Pingback: adam and eve toys
Pingback: huge dildo
Pingback: best rabbit vibrator
Pingback: trevor ragno
Pingback: trevor ragno
Pingback: online income
Pingback: affiliate marketing without a website
Pingback: affiliate marketing for beginners
Pingback: online income jobs
Pingback: trevor ragno
Pingback: trevor ragno
Pingback: work from home data entry
Pingback: work from home jobs amazon
Pingback: trevor ragno
Pingback: affiliate marketing examples
Pingback: sex cushion
Pingback: online income earning
Pingback: online income earning
Pingback: Fishing Washington
Pingback: Best Budget Centerpin Reel
Pingback: online income earning jobs
Pingback: work from home miami fl
Pingback: Best Budget Baitcasting Reels
Pingback: work from home miami fl
Pingback: Fly Fishing Kayak
Pingback: Fly Fishing Lessons
Pingback: affiliate marketing websites
Pingback: guided kayak trips
Pingback: fishing guide
Pingback: Skookumchuck River Steelhead Fishing
Pingback: affiliate marketing for beginners
Pingback: vac u loc dildo
Pingback: online income streams
Pingback: fishing guide
Pingback: work from home customer service
Pingback: online income deposit
Pingback: make money online
Pingback: work from home miami fl
Pingback: make money online from home
Pingback: Compras em Woodbury Outlet
Pingback: Guia brasileiro em Las Vegas - Turismo Las Vegas
Pingback: Compras em Woodbury Outlet
Pingback: Transfer Out em Nova York
Pingback: water lubrication for sex
Pingback: City Tour em Nova York
Pingback: Guia brasileiro em Miami - Turismo Miami
Pingback: Guia brasileiro para executivo
Pingback: Garage Door Service
Pingback: Compras em Woodbury Outlet
Pingback: wet wabbit toy
Pingback: Garage Door Services
Pingback: Garage Door Service
Pingback: Garage Door Company
Pingback: Garage Door Services
Pingback: Garage Door Services
Pingback: Guia Brasileiro em Nova York
Pingback: Garage Door Opener Repair
Pingback: Garage Door Service
Pingback: Transfer In em Nova York
Pingback: Ver neve nas Montanhas NY
Pingback: Roteiros Personalizados usando o Metrô em Nova York
Pingback: Motorista Brasileiro em Nova York
Pingback: Great Tour em Nova York
Pingback: Guia brasileiro em Los Angeles - Turismo Los Angeles
Pingback: Tour de NY para Philadelphia
Pingback: Transfer Out em Nova York
Pingback: Great Tour em Nova York
Pingback: Ver neve nas Montanhas NY
Pingback: Guia brasileiro para executivo
Pingback: Guia brasileiro em Los Angeles - Turismo Los Angeles
Pingback: Transfer In em Nova York
Pingback: Transfer In em Nova York
Pingback: Guia brasileiro em Las Vegas - Turismo Las Vegas
Pingback: kerala outstation taxi service
Pingback: kegel exercises for men
Pingback: best honeymoon packages kerala
Pingback: houseboat packages in kerala
Pingback: kerala tour packages wit price
Pingback: cochin taxi tour packages
Pingback: kerala car hire packages
Pingback: kerala tour packages wit price
Pingback: cochin taxi tour packages
Pingback: best honeymoon packages kerala
Pingback: houseboat packages in kerala
Pingback: Perfume Ships World Wide
Pingback: Best Perfume In the world
Pingback: realistic dildos
Pingback: Best Perfume and fast delivery
Pingback: Best Perfume In the world
Pingback: Best Perfume In the world
Pingback: role play ideas
Pingback: Best Perfume In the world
Pingback: Best Perfume and fast delivery
Pingback: thành lập công ty tnhh mtv
Pingback: the coyote
Pingback: Read Full Article
Pingback: Homepage
Pingback: Read Full Report
Pingback: More Bonuses
Pingback: get more info
Pingback: Discover More Here
Pingback: in this site
Pingback: Read More
Pingback: Clicking Here
Pingback: More hints
Pingback: Going Here
Pingback: etc
Pingback: more
Pingback: Bonuses
Pingback: Calgary Landscaping
Pingback: most paid sportsmen 2016
Pingback: top 100 most paid athletes
Pingback: Calgary Home Remodeling
Pingback: sylvester stallone net worth
Pingback: highest paid athletes
Pingback: highest paid athletes
Pingback: Keep dryer from catching fire
Pingback: Clogged dryer vent
Pingback: Calgary Home Remodeling
Pingback: Calgary Home Renovations
Pingback: kerb ramp
Pingback: forbes sports rich list
Pingback: Calgary Renovations
Pingback: rich star
Pingback: richest current athletes
Pingback: Austin Dryer repair service
Pingback: shop ramps
Pingback: top earning athletes in the world
Pingback: richest tv stars
Pingback: disabled access ramp gradient
Pingback: Clogged dryer vent
Pingback: Click Through the Following Webpage
Pingback: dryer vent covers
Pingback: top richest djs
Pingback: top 10 richest athletes ever
Pingback: stairs and ramps
Pingback: See More Information
Pingback: Refer to This Site for Additional Information
Pingback: Click the Following Website
Pingback: wheelchair portable ramps lightweight
Pingback: indoor dryer vents
Pingback: highest net worth sportsmen
Pingback: indoor dryer vents
Pingback: Visit This Site
Pingback: how to clean out dryer vent
Pingback: Visit This Web Page
Pingback: bath shower tub
Pingback: ductwork design
Pingback: handyman fees
Pingback: top earning athletes in the world
Pingback: Check Out These Helpful Tips
Pingback: Read More About This
Pingback: flexible air duct
Pingback: duct fittings
Pingback: top earning athletes in the world
Pingback: showers with bathtubs
Pingback: top 10 highest paid sports
Pingback: bathroom and shower
Pingback: used wheel chair ramps
Pingback: top ten paid sportsmen
Pingback: top celebrity net worth
Pingback: See More Tips
Pingback: See More Tips
Pingback: Check Out This Article
Pingback: commercial appliance repair
Pingback: garbage bin
Pingback: home dumpster rental
Pingback: junk hauling
Pingback: Visit This Page
Pingback: what's the richest sport in the world
Pingback: 20 yard dumpster rental
Pingback: small dumpster rental
Pingback: red tea detox program
Pingback: Lebah Kelulut
Pingback: Raw organic Kelulut honey
Pingback: dumpster dimensions
Pingback: dumpster bin
Pingback: Bee bread
Pingback: Read More About This
Pingback: Check Out This Information
Pingback: red tea detox reviews
Pingback: garbage containers for rent
Pingback: Click the Following Page
Pingback: Click the Following Internet Site
Pingback: washer and dryer repair service
Pingback: kitchen appliance package deals
Pingback: junk bin rental
Pingback: maytag washing machine repair
Pingback: order dumpster
Pingback: yard waste dumpster
Pingback: skyline appliance repair
Pingback: waste management dumpster rental cost
Pingback: massage wand vibrator
Pingback: affordable dumpster rental
Pingback: rent trash bins
Pingback: trigona honey benefits
Pingback: trigona bee farm
Pingback: the appliance repair doctor
Pingback: kelulut honey malaysia
Pingback: cost to rent dumpster
Pingback: concrete dumpster rental
Pingback: Honey bees
Pingback: Propolis
Pingback: fridge parts
Pingback: dumpster rental ma
Pingback: Madu kelulut
Pingback: north shore appliance repair
Pingback: appliance repair and parts
Pingback: appliance parts columbus ohio
Pingback: appliance replacement parts
Pingback: cost for dumpster rental
Pingback: Lebah Kelulut
Pingback: Trigona honey
Pingback: garbage bin rental prices
Pingback: medical records software
Pingback: mental health worksheets
Pingback: mental health worker
Pingback: psychotherapy software
Pingback: mental health counselor
Pingback: vibrating butt plug
Pingback: therap software
Pingback: who mental health
Pingback: deck paint
Pingback: therapy notes
Pingback: how to patch drywall
Pingback: mental health
Pingback: drywall texture
Pingback: roof paint
Pingback: mental health notes
Pingback: drywall cost estimator
Pingback: mental health chicago
Pingback: drywall repair texture
Pingback: description of mental health
Pingback: electronic mental health records
Pingback: drywall patch tape
Pingback: ehr programs
Pingback: painting contractors license
Pingback: drywall contractors nj
Pingback: netsmart
Pingback: interior painting tips
Pingback: psychotherapy billing
Pingback: house painting supplies
Pingback: cricket betting tips
Pingback: health notes
Pingback: drywall contractors maryland
Pingback: psychotherapy billing
Pingback: medical software companies
Pingback: drywall contractors maryland
Pingback: residential drywall contractors
Pingback: paint your home
Pingback: painting contractor forms
Pingback: painting business license
Pingback: therapist helper
Pingback: mental health agencies
Pingback: simple practice
Pingback: mental disorders
Pingback: How to clean a dryer vent
Pingback: Avoid a dryer fire
Pingback: mental health problems
Pingback: children's mental health
Pingback: mental health systems
Pingback: mental health treatment
Pingback: Dryer safety
Pingback: mental health jobs
Pingback: mental health definition
Pingback: counseling notes software
Pingback: software for therapists
Pingback: NYC Dryer repair service
Pingback: electronic health records software
Pingback: mental health
Pingback: therapist helper
Pingback: how clean dryer vent
Pingback: hvac duct installation
Pingback: mental health employment
Pingback: mental health practice management
Pingback: dryer vent cleaner brush
Pingback: how do you clean out a dryer vent
Pingback: how to vent dryer
Pingback: simple practice vs therapy notes
Pingback: therapy scheduler
Pingback: heating repair services
Pingback: therapy notes cost
Pingback: mental health bill
Pingback: electric dryer vent
Pingback: mental health progress note template
Pingback: water in dryer vent
Pingback: dryer fires
Pingback: exterior dryer vent
Pingback: health clinic software
Pingback: valantmed
Pingback: practice suite login
Pingback: psyquel
Pingback: oval dryer vent
Pingback: clothes dryer lint brush
Pingback: duct insulation
Pingback: online clinic management software
Pingback: Click Through to the Following Web Page
Pingback: Refer to This Article for More Information
Pingback: See More Hints
Pingback: See This Article
Pingback: Click the Following Page
Pingback: CW Jobs
Pingback: pujcovna elektrocentrál
Pingback: baby suit onesie
Pingback: cute baby onesies
Pingback: baby girl onesies
Pingback: baby stuff for sale online
Pingback: baby girl clothing stores online
Pingback: baby clothes stuff
Pingback: awesome baby onesies
Pingback: newborn baby clothes
Pingback: baby attire
Pingback: infants clothes online
Pingback: cute baby onesies
Pingback: baby boy online shopping
Pingback: affordable baby clothes
Pingback: baby girl clothes 3-6 months
Pingback: portrét
Pingback: short white dresses
Pingback: new style dress for party
Pingback: wooden watches
Pingback: short evening dresses
Pingback: royal blue party dress
Pingback: navy blue dress
Pingback: bardot off the shoulder dress
Pingback: white beach dresses
Pingback: Propolis
Pingback: prom dresses
Pingback: long black evening dress
Pingback: long sleeve party dresses
Pingback: Kelulut honey
Pingback: casual maxi dresses with sleeves
Pingback: long prom dresses 2016
Pingback: Madu kelulut
Pingback: black summer dresses
Pingback: long ball dresses
Pingback: beach cocktail dresses
Pingback: evening dresses with sleeves
Pingback: white strapless dress
Pingback: short summer dresses
Pingback: sexy long sleeve dresses
Pingback: Kelulut honey
Pingback: new years eve cocktail dresses
Pingback: pink prom dresses
Pingback: Madu kelulut
Pingback: go to solution
Pingback: vibrator review
Pingback: go to solution
Pingback: check now
Pingback: kelulut honey benefit
Pingback: check now
Pingback: click here
Pingback: go to solution
Pingback: click here
Pingback: kelulut farm
Pingback: click here for solution
Pingback: check now
Pingback: click here
Pingback: go to solution
Pingback: bee farm selangor
Pingback: real penis
Pingback: click here
Pingback: go to solution
Pingback: kelulut honey malaysia
Pingback: click here
Pingback: go to solution
Pingback: click here for solution
Pingback: click here
Pingback: check now
Pingback: wedding dresses, hair and more
Pingback: live
Pingback: temporary wall paper
Pingback: Mattress Store Financing
Pingback: Auto Repair Financing
Pingback: Furniture Store Financing
Pingback: HVAC Financing No Credit Check
Pingback: decals
Pingback: wallpaper for walls
Pingback: how long do hemorrhoids last
Pingback: cure hemorrhoids
Pingback: do hemorrhoids go away
Pingback: how to treat hemorrhoids
Pingback: internal hemorrhoids
Pingback: decals
Pingback: wall quotes
Pingback: hemorrhoidectomy
Pingback: anal fissure
Pingback: Vocational School Financing
Pingback: how long do hemorrhoids last
Pingback: hemorrhoids
Pingback: do hemorrhoids go away
Pingback: cure hemorrhoids
Pingback: internal hemorrhoids
Pingback: external hemorrhoid
Pingback: twitter followers
Pingback: twitter followers buy
Pingback: ecommerce
Pingback: how to treat hemorrhoids
Pingback: how to buy twitter followers
Pingback: buy real twitter followers
Pingback: prolapsed hemorrhoids
Pingback: prolapsed hemorrhoids
Pingback: Hemerrhoid treatment
Pingback: internal hemorrhoids
Pingback: how do you get hemorrhoids
Pingback: buy twitter followers instant
Pingback: gain twitter followers
Pingback: twitter followers buy instant
Pingback: how do you get hemorrhoids
Pingback: treat hemorrhoids
Pingback: prolapsed hemorrhoids
Pingback: treat hemorrhoids
Pingback: gain twitter followers
Pingback: how do you get hemorrhoids
Pingback: Hemerrhoid treatment
Pingback: Hemerrhoid treatment
Pingback: cure hemorrhoids
Pingback: external hemorrhoid
Pingback: E-Commerce WordPress Themes
Pingback: Shop for T3 Tiromel
Pingback: Multi-Purpose WP Themes
Pingback: Agency WordPress Themes
Pingback: hemorrhoid relief
Pingback: prolapsed hemorrhoids
Pingback: Hemerrhoid treatment
Pingback: how do you get hemorrhoids
Pingback: thrombosed hemorrhoid
Pingback: Blog WordPress Themes
Pingback: Portfolio WordPress Themes
Pingback: Agency WordPress Themes
Pingback: hemorroides
Pingback: Custom WordPress Themes
Pingback: Business WordPress Themes
Pingback: thrombosed hemorrhoid
Pingback: Hemerrhoid treatment
Pingback: hemorrhoids
Pingback: anal hemorrhoids
Pingback: how long do hemorrhoids last
Pingback: hemorroides
Pingback: optimind
Pingback: Where can I record my song in montreal
Pingback: lump on anus
Pingback: how do you get hemorrhoids
Pingback: Fête de noel
Pingback: Oat Straw
Pingback: alpha brain
Pingback: SERVICE DE DJ POUR MARIAGES DESTINATIONS
Pingback: anal fissure
Pingback: do hemorrhoids go away
Pingback: smart drugs reviews
Pingback: king of Montreal music
Pingback: brain health supplements
Pingback: nootrobox
Pingback: montreal wedding dj
Pingback: Best canadian dj
Pingback: brain supplements
Pingback: Dj plink music
Pingback: Dj plink youtube
Pingback: nootrobox
Pingback: SERVICE DE DJ POUR MARIAGES INDIENS
Pingback: how long do hemorrhoids last
Pingback: Meilleur dj au Quebec
Pingback: optimind
Pingback: external hemorrhoid
Pingback: SERVICE DE DJ POUR MARIAGES INDIENS
Pingback: how do you get hemorrhoids
Pingback: best nootropics
Pingback: hemorrhoid relief
Pingback: hemorrhoids
Pingback: hemorroides
Pingback: lump on anus
Pingback: website
Pingback: Cats Claw
Pingback: joe rogan supplements
Pingback: hemorrhoids medicine
Pingback: prolapsed hemorrhoids
Pingback: how long do hemorrhoids last
Pingback: carl's website
Pingback: hemorrhoid relief
Pingback: carl johan
Pingback: best brain vitamins
Pingback: whois information
Pingback: whois
Pingback: website
Pingback: onnit
Pingback: joe rogan supplements
Pingback: internal hemorrhoids
Pingback: alpha brain review
Pingback: whois
Pingback: carlfreer.com
Pingback: website
Pingback: brain vitamins
Pingback: joe rogan supplements
Pingback: carl's website
Pingback: carl
Pingback: hemorrhoid relief
Pingback: carlfreer.com
Pingback: whois information
Pingback: here
Pingback: do hemorrhoids go away
Pingback: hemorroides
Pingback: how do you get hemorrhoids
Pingback: website
Pingback: carlfreer.com
Pingback: prolapsed hemorrhoids
Pingback: carl's website
Pingback: lump on anus
Pingback: hemorrhoid relief
Pingback: carl
Pingback: whois information
Pingback: thrombosed hemorrhoid
Pingback: joe rogan supplements
Pingback: carl's website
Pingback: internal hemorrhoids
Pingback: thrombosed hemorrhoid
Pingback: Improve your attention Span
Pingback: tea tox
Pingback: colon cleanse weight loss
Pingback: plantation shutters oviedo fl
Pingback: remove toxins from body
Pingback: skinny fit tea
Pingback: sex
Pingback: belly fat flush
Pingback: remove toxins from body
Pingback: super colon cleanse
Pingback: belly fat flush
Pingback: detoxification
Pingback: detoxification
Pingback: red tea detox
Pingback: teatox
Pingback: remove toxins from body
Pingback: best detox drink
Pingback: best detox drink
Pingback: medical weight loss
Pingback: detoxification
Pingback: dieters tea
Pingback: red tea
Pingback: hitachi magic wand
Pingback: SEO Nottingham
Pingback: Limo Hire Derby
Pingback: Hummer Limo Hire Leicester
Pingback: Web Design Nottingham
Pingback: the best beginner kegel balls
Pingback: carl freer opinion
Pingback: carl johan freer
Pingback: Johan Carl
Pingback: entrepreneur carl freer
Pingback: here
Pingback: see for yourself
Pingback: see for yourself
Pingback: Carl Freer FB
Pingback: carl freer interview
Pingback: interview with carl freer
Pingback: Facebook
Pingback: Johan Carl
Pingback: check it out
Pingback: official carl freer facebook page
Pingback: fb page of carl freer
Pingback: carl johan freer
Pingback: Carl Freer FB
Pingback: carl
Pingback: carl freer opinion
Pingback: carl
Pingback: carl freer presentation
Pingback: Facebook
Pingback: Diamond rings Fort Lauderdale
Pingback: Wedding rings Fort Lauderdale
Pingback: Entanglement rings
Pingback: Jewelry stores Fort Lauderdale
Pingback: Wholesale diamonds
Pingback: Diamond rings Fort Lauderdale
Pingback: Best engagement rings
Pingback: Wedding rings Fort Lauderdale
Pingback: Wholesale diamonds
Pingback: Wedding rings Fort Lauderdale
Pingback: Entanglement rings
Pingback: Loose diamonds Fort Lauderdale
Pingback: Loose diamonds Fort Lauderdale
Pingback: wholesale diamonds fort Lauderdale
Pingback: thrombosed hemorrhoid
Pingback: hemorrhoids medicine
Pingback: anal hemorrhoids
Pingback: hemorrhoidectomy
Pingback: Engagement rings Fort Lauderdale
Pingback: learn website design
Pingback: Diamond rings Fort Lauderdale
Pingback: web design jobs
Pingback: erpnext
Pingback: external hemorrhoid
Pingback: hemorrhoid relief
Pingback: wordpress web design
Pingback: hemorrhoids
Pingback: freelance web developer
Pingback: do hemorrhoids go away
Pingback: hemorrhoids
Pingback: web design basics
Pingback: Engagement rings Fort Lauderdale
Pingback: web design company
Pingback: portfolio website design
Pingback: print design
Pingback: calze uomo invernali
Pingback: calze uomo invernali
Pingback: reggiseno in silicone
Pingback: web design prices
Pingback: Engagement rings Fort Lauderdale
Pingback: web design london
Pingback: portable garages ireland
Pingback: reggiseno invisibile
Pingback: portable garages for motorcycles
Pingback: Diamond rings Fort Lauderdale
Pingback: portable garage depot watertown ct
Pingback: portable garages nz
Pingback: carport canopy frame
Pingback: reggiseno adesivo
Pingback: portable garages nz
Pingback: slip uomo intimissimi
Pingback: portable carports prices
Pingback: Entanglement rings
Pingback: perizoma
Pingback: portable carports texas
Pingback: portable carport qld
Pingback: portable vinyl garages
Pingback: reggiseno adesivo
Pingback: chat libera
Pingback: webchat over 40
Pingback: videochat senza registrazione
Pingback: jadea tute
Pingback: chat senza registrazione
Pingback: chat italia
Pingback: intimo donna
Pingback: culottes
Pingback: intimo uomo slip
Pingback: video chat per ragazzi
Pingback: video webchat gratis
Pingback: perizoma
Pingback: perizoma
Pingback: slip uomo microfibra
Pingback: jadea tute
Pingback: chat per tutti
Pingback: video chat per donne
Pingback: chat gratis
Pingback: slip uomo microfibra
Pingback: videochat per donne
Pingback: videochat per tutti
Pingback: chat webcam
Pingback: videochat over 30
Pingback: chat italia
Pingback: slip uomo
Pingback: video chat senza registrazione
Pingback: chat
Pingback: videochat per donne
Pingback: chat donne
Pingback: video chat per donne
Pingback: best strapon for pegging
Pingback: rotating vibrators
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO for Laptop
Pingback: mobile legends download
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: IMO For PC
Pingback: dich vu seo tại tphcm
Pingback: Making Sense of Cents
Pingback: Top
Pingback: Investment
Pingback: Top
Pingback: Making Sense of Cents
Pingback: Mutual Funds
Pingback: Making Sense
Pingback: Financial Plan
Pingback: kegel kit for hers
Pingback: Personal Finance
Pingback: mobile legends download
Pingback: Financial Planning
Pingback: Investments
Pingback: Retirement Planning
Pingback: Investment
Pingback: Money
Pingback: Finance
Pingback: Stocks
Pingback: Plasma Cut
Pingback: Investments
Pingback: Wealth
Pingback: Mens Bracelets
Pingback: Amazing Offers
Pingback: Fine Jewellery
Pingback: Free Item's
Pingback: Beautiful jewellery
Pingback: Beautiful jewellery
Pingback: Mens Rings
Pingback: Mens Neckless
Pingback: Online Shopping for dress rings
Pingback: Mens Neckless
Pingback: MIG Welder
Pingback: Womens Rings
Pingback: Mens Rings
Pingback: Mens Rings
Pingback: Free jewellery
Pingback: index sticker
Pingback: cat sticky notes
Pingback: escorts booking
Pingback: cheap london escorts
Pingback: london escorts
Pingback: london escorts
Pingback: cheap london escorts
Pingback: sex positions
Pingback: scroll down
Pingback: check this out
Pingback: read more
Pingback: click here
Pingback: funny birthday wishes for girlfriend
Pingback: birthday wishes for girlfriend poems
Pingback: romantic birthday wishes for girlfriend
Pingback: classic movie trivia
Pingback: happy friendship day quotes
Pingback: don't trust quotes
Pingback: good trivia questions
Pingback: friendship day best wallpaper
Pingback: 1099 filing deadline
Pingback: heart touching quotes about life in hindi
Pingback: movie quizes
Pingback: handmade greeting cards ideas
Pingback: good trivia questions
Pingback: hollywood trivia
Pingback: classic hollywood movies
Pingback: random questions and answers
Pingback: copyright music download
Pingback: trivia and answers
Pingback: music on hold download
Pingback: easy movie trivia questions and answers
Pingback: trivia with answers
Pingback: movie quizes
Pingback: easy movie trivia
Pingback: Accounting services
Pingback: today's trivia questions and answers
Pingback: where to download free music for android
Pingback: copyright music download
Pingback: download youtube mp3
Pingback: Financial alchemy
Pingback: Financial consulting
Pingback: rnb album download zip file
Pingback: hiphop album download zip file
Pingback: hiphop mp3 download
Pingback: free mp3 music download
Pingback: rnb album download zip file
Pingback: Sales tax management
Pingback: 1099 filing deadline
Pingback: Mp3 Music download
Pingback: hiphop mixtape download zip file
Pingback: Outsourced accounting management
Pingback: The pencil is mightier
Pingback: smartidea jobs
Pingback: random trivia questions and answers
Pingback: kids movie trivia
Pingback: free vpn
Pingback: jeopardy questions and answers
Pingback: movie facts
Pingback: good trivia questions
Pingback: movie quizzes
Pingback: movie trivia games
Pingback: kids movie trivia
Pingback: smartidea
Pingback: trivia questions and answers
Pingback: kids movie trivia
Pingback: entertainment trivia
Pingback: movie trivia quiz
Pingback: vpn
Pingback: smartidea review
Pingback: Einstein Success Code Reviews
Pingback: easy movie trivia
Pingback: smartidea pte ltd
Pingback: movie fun facts
Pingback: the einstein success code
Pingback: the einstein success code
Pingback: Einstein Success Code Review
Pingback: random questions and answers
Pingback: nerdy facts
Pingback: movie trivia multiple choice questions and answers
Pingback: easy movie trivia
Pingback: classic movie trivia
Pingback: movie trivia game
Pingback: nerdy facts
Pingback: general movie trivia
Pingback: hollywood trivia
Pingback: disney trivia questions and answers 2016
Pingback: movie trivia questions and answers 2016
Pingback: vpn
Pingback: general movie trivia
Pingback: einstein success code
Pingback: general movie trivia
Pingback: entertainment trivia questions
Pingback: movie fun facts
Pingback: most common trivia questions
Pingback: Einstein Success Code Program
Pingback: the coyote
Pingback: Einstein Success Code Program
Pingback: browser
Pingback: Einstein Success Code System
Pingback: proxy
Pingback: standoutlook.com
Pingback: free vpn
Pingback: hotspot vpn
Pingback: einstein success code
Pingback: vpn master
Pingback: super vpn
Pingback: proxy
Pingback: vpn
Pingback: proxy
Pingback: bamboo vibrator
Pingback: hotspot vpn
Pingback: women's watches
Pingback: michael kors
Pingback: nox-bridge
Pingback: marc jacobs
Pingback: skagen
Pingback: watches
Pingback: coach watches
Pingback: travel accessories
Pingback: Daniel wellington
Pingback: the watches men & Co
Pingback: Daniel wellington
Pingback: watches
Pingback: Get More Info
Pingback: visit
Pingback: Go Here
Pingback: Website
Pingback: this site
Pingback: Visit Website
Pingback: additional reading
Pingback: Resources
Pingback: Read Full Article
Pingback: Learn More
Pingback: Homepage
Pingback: Homepage
Pingback: Clicking Here
Pingback: Learn More Here
Pingback: Recommended Reading
Pingback: Extra resources
Pingback: Full Article
Pingback: Click & connect with rated hospitality staff
Pingback: g spot and clitoral stimulation
Pingback: Click & connect with rated hospitality staff
Pingback: Unlock Opportunities
Pingback: Connecting the hospitality community
Pingback: Passione Supreme G Spot Massager
Pingback: entertainment attorney
Pingback: copyright attorney
Pingback: LLG
Pingback: copyright attorney
Pingback: Lawyer Pasadena
Pingback: Justin Lum
Pingback: copyright attorney
Pingback: Albert Justin Lum
Pingback: trademark lawyer las vegas
Pingback: patent attorney
Pingback: patent attorney
Pingback: asylum lawyer
Pingback: san gabriel valley attorney
Pingback: immigration attorney lv
Pingback: LLG
Pingback: lawyer las vegas
Pingback: business attorney
Pingback: ip las vegas lawyer
Pingback: Chinese Lawyer
Pingback: immigration lawyer
Pingback: asylum attorney
Pingback: Lawsuits
Pingback: Business
Pingback: Debt Collection
Pingback: Trustbuster
Pingback: Kingman
Pingback: Wrongful death
Pingback: Prescott AZ
Pingback: family
Pingback: first time anal sex
Pingback: Máscara
Pingback: essencia
Pingback: mascara de hidratacao
Pingback: Hidratante
Pingback: Máscara
Pingback: Sewa Apartemen Jogja
Pingback: Youtube artist
Pingback: dual bullets vibration
Pingback: dental implants
Pingback: Sewa Apartemen Jogja
Pingback: New Artist
Pingback: dental implants
Pingback: Apartemen Di Yogyakarta
Pingback: Sewa Apartemen Yogyakarta
Pingback: Apartemen Di Jogja
Pingback: Apartemen Studio Di Jogja
Pingback: oral pahology
Pingback: Apartemen Dekat Kampus Jogja
Pingback: Magazine business
Pingback: How to upload music on blogs
Pingback: oral pahology
Pingback: Sound cloud rappers
Pingback: Music producer
Pingback: veneers in beverly hills
Pingback: cosmetic reconstructive dentistry
Pingback: pinhole gum recession surgery
Pingback: full mouth reconstruction
Pingback: Hot artist this month
Pingback: Urban magazine
Pingback: tmj in los angeles
Pingback: all on 6 implants
Pingback: Billboard charts
Pingback: Hot artist this month
Pingback: dental implants
Pingback: all on 4 implants
Pingback: Trending
Pingback: Cornelius Beatz
Pingback: oral pahology
Pingback: como redactar un curriculum sin experiencia
Pingback: tmj in los angeles
Pingback: Safe Christian Investments
Pingback: ejemplo curriculum vitae
Pingback: Wealth Transfer
Pingback: Wealth Transfer
Pingback: universidad roosevelt
Pingback: President of United States
Pingback: Christian Investments
Pingback: Christian Silver
Pingback: Interesting Read
Pingback: IMF
Pingback: plantillas curriculum
Pingback: This is interesting
Pingback: opta glassdoor
Pingback: all on 6 implants
Pingback: plantillas gratis
Pingback: 2016 US Dollar Crash
Pingback: como hacer un curriculum vitae
Pingback: 2015 Four Blood Moons
Pingback: Read More
Pingback: Barack Obama 2016
Pingback: redactar carta de presentación
Pingback: tech news site
Pingback: news on tech mahindra share
Pingback: pinhole gum recession surgery
Pingback: Sabbatical Year Sheviit
Pingback: Interesting Read
Pingback: oral pahology
Pingback: full mouth reconstruction
Pingback: texas tech news
Pingback: www.terrysacka.com
Pingback: tidewater tech newport news va
Pingback: news on tech mahindra share
Pingback: what is the best tech news website
Pingback: tech products news
Pingback: Homepage
Pingback: Wealth Transfer
Pingback: bank tech news
Pingback: Safe Christian Investments
Pingback: Great Wealth Transfer
Pingback: future tech news
Pingback: cnet tech news
Pingback: Blogpost
Pingback: Read More
Pingback: full mouth reconstruction
Pingback: tech news uk
Pingback: news on tech mahindra share
Pingback: tidewater tech newport news va
Pingback: tech news nepal
Pingback: sci tech news
Pingback: cosmetic dentistry
Pingback: the latest tech news
Pingback: it and tech news
Pingback: gym equipment in china
Pingback: gym equipment producer China
Pingback: Website
Pingback: fitness equipment manufacturer China
Pingback: gym equipment supplier
Pingback: Florida Divorce Attorney
Pingback: gym equipment producer
Pingback: gym equipment suppliers in China
Pingback: gym equipment producers in China
Pingback: Website
Pingback: gym equipment Chinese
Pingback: gym equipment producer in China
Pingback: Paternity
Pingback: china fitness equipment
Pingback: fitness equipment manufacturer China
Pingback: gym equipment suppliers
Pingback: gym equipment suppliers in China
Pingback: gym equipment factory China
Pingback: gym equipment in Chinese
Pingback: gym equipment manufacturing in China
Pingback: Homepage
Pingback: Conflict Resolution
Pingback: Imediate Inc
Pingback: china fitness equipment
Pingback: polerowanie granitu kraków
Pingback: szlifowanie betonu kraków
Pingback: renowacja granitu
Pingback: szlifowanie granitu kraków
Pingback: szlifowanie betonu kraków
Pingback: szlifowanie granitu kraków
Pingback: szlifowanie betonu kraków
Pingback: globos luminosos
Pingback: luces para fiestas
Pingback: globos luz led blancos
Pingback: Coloring Videos
Pingback: Color cars
Pingback: Coloring
Pingback: Graffiti
Pingback: globos luz
Pingback: Learn colors
Pingback: Color cars YouTube
Pingback: Coloring Videos
Pingback: Coloring Pages
Pingback: Coloring
Pingback: Paint cars and learn colors
Pingback: globos con luz
Pingback: globos led España
Pingback: merchandising luminoso
Pingback: Coloring Pages
Pingback: mobiliario led
Pingback: Paint cars and learn colors
Pingback: Paint cars and learn colors
Pingback: Graffiti
Pingback: Color
Pingback: Coloring Videos
Pingback: Coloring Videos
Pingback: Graffiti
Pingback: Graffiti
Pingback: Coloring
Pingback: Color for Kids
Pingback: Color cars YouTube
Pingback: Color cars for Children
Pingback: Color cars YouTube
Pingback: Paint cars and learn colors
Pingback: Learn colors
Pingback: Color cars for Children
Pingback: Color for Kids
Pingback: ez battery reconditioning review battery reconditioning
Pingback: texting girls
Pingback: washing machine repair
Pingback: vehicle donation
Pingback: best place to donate car
Pingback: donate old cars to charity
Pingback: discount appliance repair
Pingback: Coloring Pages
Pingback: survival life
Pingback: Coloring
Pingback: penis enlargement bible
Pingback: washer repair service
Pingback: kitchen appliances
Pingback: perfect weight forever
Pingback: amana refrigerator
Pingback: sear appliance repair
Pingback: car donation value
Pingback: wake appliance repair
Pingback: donate my boat
Pingback: used car donations to charity
Pingback: bosch appliances
Pingback: donate my car
Pingback: mohinga chennai street food burmese street food atho mohinga
Pingback: the detox water recipe weight loss recipe skincare routine297
Pingback: all brand appliance service
Pingback: refrigerator repair cost
Pingback: how to receive a donated car
Pingback: detox water recipes 4 ways to detox everyday
Pingback: how to receive a donated car from a charity
Pingback: donate vehicle for cash
Pingback: jillian michaes detox water
Pingback: appliance service software
Pingback: edta heart liver cleanse toxic cleanse cleanse detox products whole body detox
Pingback: foods you thought were healthy but actually arent
Pingback: page26
Pingback: breaking down diabetes endocrine system diseases nclex rn khan academy
Pingback: 20 disgusting foods that people actually eat
Pingback: car donations for veterans
Pingback: feeling sick on a ketogenic diet
Pingback: improve your digestive tract with pineapple blueberry infused water recipe
Pingback: appliance parts direct
Pingback: William Saito
Pingback: donation of a car
Pingback: all tech appliance service
Pingback: cheap stainless steel appliances
Pingback: http://suckhoethuongthuc.org/kham-phu-khoa-o-dau-tot.html
Pingback: repair appliances
Pingback: mycardoeswhat org
Pingback: make a wish vehicle donation
Pingback: consumer energy appliance service plan
Pingback: appliances brands
Pingback: commercial appliance parts and service
Pingback: donate your car ct
Pingback: appliance service by paul inc
Pingback: oven service
Pingback: car donation denver
Pingback: give car
Pingback: donate car mn
Pingback: car give away charity
Pingback: discount kitchen appliances
Pingback: refrigerator ice maker
Pingback: veterans donate car
Pingback: electric appliance repair service
Pingback: bosch appliances parts
Pingback: appliance by paul
Pingback: fridge repair cost
Pingback: kidney cars
Pingback: mental health progress notes software
Pingback: buy real instagram likes
Pingback: best charity to donate car
Pingback: cars for kids donation
Pingback: huawei phone screen repair
Pingback: how to donate a car to charity
Pingback: mental health practice
Pingback: donate your vehicle
Pingback: donate your car tax deduction
Pingback: Laboratory
Pingback: places to donate a car
Pingback: buy instagram followers 1$
Pingback: jobs in mental health
Pingback: instagram followers
Pingback: donating your car for a tax write off
Pingback: mental health in children
Pingback: Buy 100 Instagram Followers
Pingback: cognitive behavioral therapy software
Pingback: donate your boat to charity
Pingback: mental health progress note template
Pingback: software emr
Pingback: group echo
Pingback: donated cars for sale
Pingback: Compaq
Pingback: give car away for charity
Pingback: Acer tab battery replacement
Pingback: Mitigation and Restoration Plans
Pingback: donate your car salvation army
Pingback: cloud based healthcare software
Pingback: natural skin treatment
Pingback: ophthalmology emr
Pingback: titanium software counseling
Pingback: ehr website
Pingback: dermatology emr
Pingback: car donation charities ratings
Pingback: donate household items
Pingback: substance abuse billing companies
Pingback: kpbs vehicle donation
Pingback: Environmental Services
Pingback: phone screen replacement
Pingback: psychologist appointment
Pingback: psychological software solutions
Pingback: Network unlock code
Pingback: hospital ehr
Pingback: organizations that donate cars
Pingback: best mental health websites
Pingback: donations vehicle
Pingback: Chicago Mound Towing Service near 8 Mile Rd
Pingback: donate used car
Pingback: where to donate a car
Pingback: m97 emergency towing
Pingback: donate car
Pingback: common rd tow truck
Pingback: salvation army car donation
Pingback: Chicago Mound Towing Service near 12 Mile Rd
Pingback: Wetland Plant Restoration
Pingback: donate my car for cash
Pingback: donating a car to goodwill
Pingback: Acer Laptop Battery
Pingback: auto wrecker in madison hts
Pingback: topco cyberskin
Pingback: water damage iphone repair
Pingback: best charity to donate a car to
Pingback: insurance quotes auto
Pingback: Chicago Mound Towing Service near 10 Mile Rd
Pingback: can you donate a car without a title
Pingback: cars to donate
Pingback: tax deduction for donated car
Pingback: american cancer society car donation
Pingback: here
Pingback: how to donate a car for tax deduction
Pingback: get a car donated to you
Pingback: tow truck company near warren
Pingback: donation of car to charity tax deductible
Pingback: emergency tow truck fraser
Pingback: Chicago Mound Towing Service
Pingback: Misc Activities in Wetlands Permits (HCEPC)
Pingback: donate rv to charity
Pingback: donate rv tax deduction
Pingback: click here
Pingback: warren auto wrecker service
Pingback: donate car ca
Pingback: web-design
Pingback: car donation ca
Pingback: Chicago Mound Towing Service near Hazel Park
Pingback: warren auto wrecker service
Pingback: car donation san diego
Pingback: donate a car to veterans charity
Pingback: penis vibrator apps for android
Pingback: Chicago Mound Towing Service near Warren
Pingback: Chicago Mound Towing Service near M-97
Pingback: tow truck sale
Pingback: Chicago Mound Towing Service near 8 Mile Rd
Pingback: should i donate my car
Pingback: Chicago Mound Towing Service near 10 Mile Rd
Pingback: tow truck martin rd
Pingback: eastpointe tow truck
Pingback: auto wrecker in warren mi
Pingback: hyip Advertise
Pingback: Chicago Mound Towing Service near Hoover Rd
Pingback: school ipad fix
Pingback: HYIP
Pingback: service company 9 mile rd
Pingback: Chicago Mound Towing Service near Groesbeck
Pingback: Chemical and Bacteriological Lab
Pingback: Chicago Mound Towing Service near 14 Mile Rd
Pingback: corrupt hardrive files recovery
Pingback: emergency roadside assistance in center line mi
Pingback: Chicago Mound Towing Service near Madison Hts
Pingback: Chicago Mound Towing Service serving Saint Clair Shores
Pingback: emergency roadside assistance in warren
Pingback: investment
Pingback: tow truck service m-97
Pingback: towing service in grosse pointe woods mi
Pingback: Chicago Mound Towing Service serving St. Clair Shores
Pingback: seattle ants exterminators
Pingback: ants exterminators
Pingback: bali exotic wedding
Pingback: bali wedding organizer
Pingback: bali beach wedding
Pingback: bali private wedding
Pingback: bali wedding
Pingback: bali beach wedding
Pingback: bali beach wedding
Pingback: married in bali
Pingback: buy and sell free online
Pingback: youtube wild videos
Pingback: pranks gone wild
Pingback: unbelievable videos
Pingback: videos youtube videos
Pingback: top 5 funniest youtube videos ever
Pingback: funny videos online
Pingback: pet magasin clipper kit
Pingback: buy video views youtube
Pingback: funny videos family friendly
Pingback: how to buy youtube views on Famoid
Pingback: funny news videos on youtube
Pingback: Best investment uk
Pingback: funny baby videos for kids
Pingback: youtube views
Pingback: funny video games videos
Pingback: buy youtube views
Pingback: how to buy youtube views on Famoid
Pingback: best videos of 2017
Pingback: how to buy youtube views
Pingback: buy youtube views
Pingback: Best investment uk
Pingback: youtube best funny video ever
Pingback: buy views on youtube
Pingback: youtube views
Pingback: youtube views
Pingback: the most funniest videos ever
Pingback: top 10 funny videos
Pingback: pranks gone wrong youtube
Pingback: buy youtube views
Pingback: buy video views youtube
Pingback: buy youtube views
Pingback: funny kids on youtube
Pingback: funny pranks for parents to pull on their kids
Pingback: the best funniest videos ever
Pingback: the most funniest videos ever
Pingback: sipp
Pingback: how to buy facebook likes
Pingback: facebook likes
Pingback: youtube best funny video ever
Pingback: the most funniest jokes ever
Pingback: hail damage roof repair indianapolis Indiana
Pingback: how to buy facebook likes on Famoid
Pingback: roofing companies indianapolis Indiana
Pingback: facebook likes
Pingback: 317-315-5030
Pingback: buy facebook likes
Pingback: Indiana roofing company near me
Pingback: youtube video hot video
Pingback: Roofing contractors in Indianapolis Indiana
Pingback: buy facebook likes
Pingback: facebook likes buy
Pingback: forex trade
Pingback: indianapolis Indiana roofing jobs
Pingback: buy likes on facebook
Pingback: tile roof repair indianapolis Indiana
Pingback: funny baby video
Pingback: Indiana roofing companies
Pingback: buy facebook likes
Pingback: roofing indianapolis angie's list
Pingback: residential roofers indianapolis Indiana
Pingback: buy likes on facebook
Pingback: facebook likes
Pingback: metal roofing contractors indianapolis Indiana
Pingback: best roofing contractors indianapolis Indiana
Pingback: how to buy facebook likes on Famoid
Pingback: gold forex
Pingback: indianapolis Indiana roofing contractor reviews
Pingback: buy facebook fanpage likes
Pingback: buy fan page likes
Pingback: buy facebook fanpage likes
Pingback: wholesale real estate buyer
Pingback: buy fan page likes
Pingback: facebook fan page likes buy
Pingback: we buy ugly houses
Pingback: indianapolis Indiana roofing codes
Pingback: Buy facebook fan page likes
Pingback: buy facebook fanpage likes
Pingback: indianapolis roofing license
Pingback: Emergency Roof repair Indianapolis Indiana
Pingback: home investor
Pingback: commercial roofing contractors indianapolis Indiana
Pingback: residential roofers indianapolis Indiana
Pingback: abandoned home buyer
Pingback: forex rates
Pingback: Roofing Contractors Indianapolis Indiana
Pingback: how to buy facebook fan page likes
Pingback: roofing contractors Greenwood In
Pingback: Roofing Contractors Indianapolis
Pingback: indianapolis Indiana roofers angie's list
Pingback: buy facebook fanpage likes
Pingback: indianapolis roofing consultants
Pingback: facebook fan page likes
Pingback: White River Roofers Indianapolis Indiana
Pingback: buy facebook fanpage likes
Pingback: roofing contractors indianapolis Indiana
Pingback: roof repair indianapolis in
Pingback: buy fan page likes
Pingback: Finances
Pingback: best first sex toy
Pingback: facebook fan page likes buy
Pingback: brick repair masonry contractor in midtown detroit
Pingback: facebook fanpage likes
Pingback: brick repair chimney michigan
Pingback: brick repair and maintenance
Pingback: brick chimney masonry repair detroit michigan
Pingback: repair exterior brick wall
Pingback: brick repair contractors in detroit
Pingback: facebook fanpage likes
Pingback: brick repair handyman
Pingback: brick paver edging repair
Pingback: matka result
Pingback: brick repair masonry contractor in Boston-Edison detroit
Pingback: brick mailbox repair
Pingback: masonry repair detroit michigan
Pingback: forex
Pingback: brick repair contractors in detroit
Pingback: brick mailbox repair
Pingback: Ultrarecovery
Pingback: chimney masonry repair
Pingback: brick repair grout
Pingback: brick repair work in detroit mi
Pingback: Ultrarecovery
Pingback: Ultrarecovery
Pingback: best
Pingback: best
Pingback: InfusionSoft
Pingback: best
Pingback: top ten
Pingback: brick repair in winter
Pingback: brick repair masonry contractors Boston-Edison detroit michigan
Pingback: la mejor
Pingback: webdesign landshut
Pingback: chimney repair metro detroit
Pingback: top five
Pingback: opiniones
Pingback: repair brick house wall
Pingback: repair brick garden wall
Pingback: brick paver edging repair
Pingback: Old Town Brokerage Inc Pasadena
Pingback: top product reviews
Pingback: mejor
Pingback: top five
Pingback: reviews
Pingback: Ultrarecovery
Pingback: Ultrarecovery
Pingback: top five
Pingback: mejores productos
Pingback: top product reviews
Pingback: opiniones
Pingback: brick repair chimney detroit
Pingback: madmoses landshut
Pingback: brick repair masonry contractor in Boston-Edison detroit
Pingback: best casino welcome bonus
Pingback: la mejor
Pingback: best
Pingback: best
Pingback: opiniones
Pingback: Jam Logistics LLC Green Bay
Pingback: chat gay
Pingback: la mejor
Pingback: la mejor
Pingback: top product reviews
Pingback: los mejores
Pingback: Rencontres francophones
Pingback: el mejor
Pingback: chat hommes
Pingback: el mejor
Pingback: top five
Pingback: reviews
Pingback: site Rencontres
Pingback: webdesign landshut
Pingback: los mejores
Pingback: el mejor
Pingback: rendez-vous sexuelles
Pingback: los mejores
Pingback: How to create miracles bk shivani
Pingback: giant cat mural penang
Pingback: buenos
Pingback: opiniones
Pingback: los mejores
Pingback: best cryptocurrency exchange 2018
Pingback: best
Pingback: antminer s9
Pingback: top product reviews
Pingback: buenos
Pingback: mejor
Pingback: agentur landshut
Pingback: buy bitcoins instantly
Pingback: sam e cat wallpaper
Pingback: top reviews
Pingback: best
Pingback: reviews
Pingback: mejores productos
Pingback: earn bitcoins referrals
Pingback: la mejor
Pingback: IPL 2018 Fantsay Cricket
Pingback: top five
Pingback: reviews
Pingback: buenos
Pingback: Dream11 ipl tips
Pingback: buy bitcoins instantly
Pingback: CSK vs SRH dream11 tips
Pingback: SRH vs DD dream11 tips
Pingback: top ten
Pingback: Dream11
Pingback: Fantasy Cricket leagues
Pingback: popular online shopping
Pingback: la mejor
Pingback: buenos
Pingback: RCB vs KXIP dream11 tips
Pingback: top five
Pingback: Dream11 ipl tips
Pingback: la mejor
Pingback: la mejor
Pingback: buenos
Pingback: Dream11 ipl tips
Pingback: antminer s9 for sale
Pingback: IPL Fantasy Cricket 2018
Pingback: popular online shopping
Pingback: top reviews
Pingback: chung cu tdh riverview
Pingback: mejor
Pingback: USA best shopping site
Pingback: top product reviews
Pingback: top ten
Pingback: Dream11 ipl tips
Pingback: CSK vs MI dream11 tips
Pingback: SRH vs MI dream11 tips
Pingback: SRH vs CSK dream11 tips
Pingback: top reviews
Pingback: myteam11
Pingback: IPL 2018 Myteam11 tips
Pingback: Mens Fitness clothing
Pingback: Printed Elastic Yoga Pants
Pingback: los mejores
Pingback: 3D Printed Compression Top
Pingback: el mejor
Pingback: Buy Fitness Supplies online
Pingback: women watches
Pingback: los mejores
Pingback: Breathable Compression T-Shirt
Pingback: best
Pingback: hobies product
Pingback: unbelievable discounts
Pingback: top reviews
Pingback: top ten
Pingback: top five
Pingback: los mejores
Pingback: women watches
Pingback: man accesories
Pingback: top five
Pingback: top ten
Pingback: activites equipment
Pingback: top belly fat burning exercise
Pingback: Printed Elastic Yoga Pants
Pingback: travel with sex toys
Pingback: top product reviews
Pingback: top five
Pingback: la mejor
Pingback: Fitness Supplies
Pingback: Fitness Supplies
Pingback: pet products
Pingback: la mejor
Pingback: pet products
Pingback: los mejores
Pingback: Fitness Supplies
Pingback: Printed Elastic Yoga Pants
Pingback: buenos
Pingback: Online shopping
Pingback: coyote xp kart for sale
Pingback: bahis siteleri
Pingback: review
Pingback: mejor
Pingback: top reviews
Pingback: el mejor
Pingback: los mejores
Pingback: top five
Pingback: Bonuses
Pingback: insurance quote
Pingback: el mejor
Pingback: top ten
Pingback: Full Article
Pingback: buenos
Pingback: mejor
Pingback: cryptocurrency
Pingback: la mejor
Pingback: thc liquid uk
Pingback: top ten
Pingback: thc liquid amsterdam
Pingback: thc liquid weed
Pingback: mejores productos
Pingback: thc liquid vape
Pingback: thc liquid jual
Pingback: thc liquid vape uk
Pingback: mejores productos
Pingback: thc liquid vape uk
Pingback: thc liquid capsules
Pingback: thc liquid vape
Pingback: thc liquid for vaporizer
Pingback: how to use a vibrating cock ring
Pingback: thc liquid uk
Pingback: novel
Pingback: thc liquid pen
Pingback: 75 Alexis Suder Towing of Toledo OH
Pingback: 75 Alexis Suder Towing Downtown Toledo
Pingback: book
Pingback: towing in
Pingback: novel online
Pingback: toledo auto wrecker service
Pingback: tow truck company near downtown toledo oh
Pingback: auto wrecker service downtown toledo
Pingback: emergency roadside assistance in downtown toledo oh
Pingback: thc liquid jual
Pingback: thc liquid weed
Pingback: mejores productos
Pingback: thc liquid for vaporizer
Pingback: romance novels
Pingback: book
Pingback: top product reviews
Pingback: thc liquid vape
Pingback: best
Pingback: thc liquid uk
Pingback: free online novels
Pingback: thc liquid capsules
Pingback: novels to read
Pingback: read online free
Pingback: opiniones
Pingback: thc liquid effects
Pingback: read online free
Pingback: free books
Pingback: esports wagering
Pingback: ethereum based games
Pingback: car salvage yards
Pingback: learn about towing here
Pingback: 75 Alexis Suder Towing of Toledo
Pingback: emergency tow truck near summit st toledo
Pingback: towing company
Pingback: thc liquid weed
Pingback: thc liquid for vaporizer
Pingback: salvage yard search
Pingback: 75 Alexis Suder Towing near I-280
Pingback: 75 Alexis Suder Towing near Summit St
Pingback: baixar tree of life o inicio
Pingback: thc liquid
Pingback: thc liquid jual
Pingback: thc liquid for vaporizer
Pingback: thc liquido
Pingback: 75 Alexis Suder Towing near Interstate 75
Pingback: thc liquid vape uk
Pingback: tow truck service provider near toledo
Pingback: emergency roadside assistance in i75
Pingback: 192.168.1.1
Pingback: edgewater dr towing service provider
Pingback: ethereum based games
Pingback: thc liquid vape
Pingback: thc liquid vape uk
Pingback: thc liquid weed
Pingback: ethereum based games
Pingback: 75 Alexis Suder Towing (419) 491-3253
Pingback: thc liquid vape uk
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: thc liquid weed
Pingback: 192.168.0.1
Pingback: thc liquid weed
Pingback: 192.168.1.1
Pingback: thc liquid vape uk
Pingback: thc liquid uk
Pingback: what does the tree of life necklace represent
Pingback: APK Games
Pingback: top ten
Pingback: thc liquid uk
Pingback: hyip monitor
Pingback: thc liquid weed
Pingback: APK Apps
Pingback: APK Apps
Pingback: thc liquid effects
Pingback: 75 Alexis Suder Towing
Pingback: thc liquid uk
Pingback: APK
Pingback: thc liquid jual
Pingback: top five
Pingback: los mejores
Pingback: Manhattan Stickney Towing
Pingback: Manhattan Stickney Towing
Pingback: yotbub
Pingback: 192.168.1.254
Pingback: Manhattan Stickney Towing serving US-24
Pingback: APK Apps
Pingback: used tow truck equipment for sale
Pingback: Recommended Reading
Pingback: thc liquid amsterdam
Pingback: mejores productos
Pingback: APK Apps
Pingback: hdkino720.info
Pingback: top product reviews
Pingback: Manhattan Stickney Towing
Pingback: thc liquid vape uk
Pingback: Best hyip
Pingback: mejores productos
Pingback: Manhattan Stickney Towing of Toledo
Pingback: hyip tool
Pingback: thc liquid
Pingback: 3 Step Stamina
Pingback: Manhattan Stickney Towing
Pingback: Recommended Reading
Pingback: thc liquid effects
Pingback: thc liquid for vaporizer
Pingback: buy youtube views and likes
Pingback: thc liquid vape uk
Pingback: best towing company in sylvania oh
Pingback: thc liquid jual
Pingback: greenbelt pkwy emergency towing
Pingback: thc liquid uk
Pingback: thc liquid for vaporizer
Pingback: thc liquid
Pingback: Manhattan Stickney Towing
Pingback: Manhattan Stickney Towing
Pingback: IPO Turnier
Pingback: thc liquid capsules
Pingback: thc liquid vape uk
Pingback: thc liquid capsules
Pingback: thc liquido
Pingback: emergency tow truck in mcgregor rd
Pingback: thc liquid capsules
Pingback: Manhattan Stickney Towing
Pingback: Hundeseminare suchen
Pingback: Working Dog, Gebrauchshund
Pingback: Suchmaschine Hunde
Pingback: Manhattan Stickney Towing
Pingback: imessage on pc
Pingback: Manhattan Stickney Towing (419) 333-8158
Pingback: kik for pc
Pingback: kik for pc
Pingback: towing service toledo oh
Pingback: Manhattan Stickney Towing serving Toledo
Pingback: Rally Obedience Turnier
Pingback: Manhattan Stickney Towing
Pingback: Hundeschule München
Pingback: Manhattan Stickney Towing
Pingback: Hundeschulen und Hundeerziehung
Pingback: Suchmaschine Hunde
Pingback: kik for pc
Pingback: IPO Turnier
Pingback: product label design
Pingback: Working Dog, Gebrauchshund
Pingback: leading webdesign company in world
Pingback: kik for pc
Pingback: Hundetrainer
Pingback: kik for pc
Pingback: promotional video maker
Pingback: imessage on pc
Pingback: Video editing
Pingback: towing service provider central ave
Pingback: Manhattan Stickney Towing
Pingback: Veranstaltungen rund um den Hund
Pingback: imo for laptop
Pingback: imo for pc
Pingback: route 25 towing service provider
Pingback: website design
Pingback: imo for laptop
Pingback: website design company in kolkata
Pingback: imo for pc
Pingback: Working Dog, Gebrauchshund
Pingback: towing in southgate mi
Pingback: facetime for pc
Pingback: product label design
Pingback: emergency towing near lincoln park mi
Pingback: imo for pc
Pingback: works here
Pingback: imo for pc
Pingback: imo for laptop
Pingback: garageband for pc
Pingback: best homes for sale
Pingback: emergency tow truck near i75
Pingback: tow truck service romulus mi
Pingback: study mbbs in russia
Pingback: Hundeschule München
Pingback: Hundesport
Pingback: nutrition
Pingback: Dog trainer and dog school
Pingback: Events rund um den Hund
Pingback: Rally Obedience Turnier
Pingback: Eureka Telegraph Towing serving Southland Mall
Pingback: Obedience, Agility Turnier
Pingback: tow truck company in southgate
Pingback: Eureka Telegraph Towing serving Southgate
Pingback: Hundesport
Pingback: how to find a good towing service
Pingback: IPO Turnier
Pingback: Hundeschule München
Pingback: Dog trainer and dog school
Pingback: service charges a fair price
Pingback: service charges a fair price
Pingback: Suchmaschine Hunde
Pingback: Suchmaschine Hunde
Pingback: tmobile roadside assistance
Pingback: car assistance
Pingback: black rabbit vibrator
Pingback: contractor
Pingback: the most reliable tow truck company near taylor mi
Pingback: Eureka Telegraph Towing near Pelham Rd
Pingback: Eureka Telegraph Towing near Heritage Park
Pingback: website design
Pingback: search real estate for sale
Pingback: 1 Hour Belly Blast Diet
Pingback: Eureka Telegraph Towing near WCCCD
Pingback: tow truck service allen park mi
Pingback: email marketing
Pingback: tow truck service provider near i94
Pingback: golubaya-laguna
Pingback: articles
Pingback: oh-795 emergency towing
Pingback: tow truck used
Pingback: Dixie Sandusky Towing serving Toledo
Pingback: downtown
Pingback: Dixie Sandusky Towing near Boundary St
Pingback: how to make dick bigger
Pingback: Dixie Sandusky Towing in Perrysburg
Pingback: Dixie Sandusky Towing serving Front St
Pingback: bunny oren led
Pingback: emergency roadside service wallbridge oh
Pingback: oh st rte 25 towing
Pingback: Dixie Sandusky Towing near I-475
Pingback: Website Design
Pingback: search homes for sale
Pingback: shining rabbit 70 cm led
Pingback: towing in perrysburg oh
Pingback: emergency tow truck near i475
Pingback: Dixie Sandusky Towing near Maumee
Pingback: Grow more, know more with Truth Right Here
Pingback: Start making sense of Scripture
Pingback: Bridging Scholarship and the Church
Pingback: wilmington towing services
Pingback: tow truck service near wallbridge oh
Pingback: Dixie Sandusky Towing
Pingback: nonton bioskop LK21 sub indo
Pingback: streaming movie
Pingback: Follow us for Biblical insight
Pingback: Learn more about how to learn the Bible
Pingback: Truth Right Here is a Biblical education nonprofit
Pingback: runs
Pingback: Learn more about how to learn the Bible
Pingback: big houses for sale
Pingback: film bioskop gratis
Pingback: movie indo
Pingback: anal free fuck interracial movie
Pingback: film bioskop gratis
Pingback: mothers teaching daughters how to fuck
Pingback: anal retro porno video
Pingback: old guys fuck young sluts
Pingback: movie brother an sister fuck
Pingback: mothers i like to fuck i
Pingback: anal big cock fuck videos
Pingback: anal hd porno video online
Pingback: Türkçe Psikoterapi
Pingback: tranny with big dick
Pingback: porno teen model video
Pingback: mothers i like to fuck 18
Pingback: house sales
Pingback: porno teen skinny video
Pingback: mothers teaching daughters how to fuck
Pingback: old lady free fuck movies
Pingback: jennifer lopez
Pingback: works here
Pingback: male enhancement supplements
Pingback: service company
Pingback: Dixie Sandusky Towing serving Stoney Ridge
Pingback: vigrx plus pills side effects
Pingback: (419) 504-3716
Pingback: apple music artist to watch
Pingback: songwriter
Pingback: nonton film cinema 21
Pingback: dick enlargement
Pingback: dick enhancement
Pingback: rihanna
Pingback: nonton movie ganool
Pingback: nonton movie online
Pingback: male enhancement pills reviews
Pingback: breakout artist
Pingback: layarkaca21 streaming movie
Pingback: juliane
Pingback: Previdencia complementar
Pingback: best male performance pills
Pingback: nontonmovie.com
Pingback: male enhancement surgery
Pingback: Modest
Pingback: conecta porto seguro
Pingback: Ituran com Seguro
Pingback: Seguro de vida pequenas empresas
Pingback: Ituran com Seguro
Pingback: homes for sale near
Pingback: download film barat
Pingback: beyonce
Pingback: Plano de Saude para animal
Pingback: male enhancement products
Pingback: enlargement pills for male
Pingback: Seguro Viagem Empresarial
Pingback: Ituran Seguro HDI
Pingback: Rastreador Ituran
Pingback: dick growth pills
Pingback: ariana grande
Pingback: spotify
Pingback: dick growth pills
Pingback: porto seguro automovel
Pingback: nonton film my stupid boss
Pingback: r&b
Pingback: nonton movie ganool
Pingback: vigrx plus pills
Pingback: vigrx plus in malaysia
Pingback: enhanced male reviews
Pingback: vigrx plus in malaysia
Pingback: download film tentang cinta
Pingback: nonton film bioskop
Pingback: male enlargement pills
Pingback: Ituran Seguro Cardif
Pingback: vigrx plus price
Pingback: top male enhancement
Pingback: Seguro Plano de Saude
Pingback: male enhancement surgery
Pingback: Ituran Seguro Cardif
Pingback: conecta porto seguro
Pingback: office furniture
Pingback: Seguro de vida em Grupo
Pingback: Seguro Viagem em Grupo
Pingback: male enhancement pills
Pingback: Plano de Saude para animal
Pingback: Rastreador Ituran
Pingback: Ituran Seguro HDI
Pingback: best led camping headlight
Pingback: best led camping headlight
Pingback: 12 led headlight hiking camping cycling
Pingback: Rechargeable Headlight
Pingback: Previdencia privada
Pingback: Best Headlamp 2017
Pingback: headlamp led for camping
Pingback: best led camping headlight
Pingback: Seguro Viagem
Pingback: Plano de Saude Cães
Pingback: Seguro para Casa
Pingback: hinode produtos
Pingback: Plano de Saude para animal
Pingback: Rechargeable Headlight
Pingback: consorcio porto
Pingback: Camping Light
Pingback: Seguro Viagem Receptivo
Pingback: Seguro Viagem
Pingback: led headlights
Pingback: grupo hinode
Pingback: best led headlights
Pingback: headlamp camping and
Pingback: free camping headlight
Pingback: Seguro equipamentos
Pingback: Rastreador Ituran
Pingback: Seguro equipamento portatil
Pingback: Seguro equipamentos portateis
Pingback: Previdencia complementar
Pingback: Seguro automovel
Pingback: Ganhe 100% de comissão na venda
Pingback: Seguro auto
Pingback: Seguro para Casa
Pingback: Seguro automovel
Pingback: lahore escorts
Pingback: Ituran Seguro HDI
Pingback: Seguro Viagem em Grupo
Pingback: hinode produtos
Pingback: Plano de Saude Cães
Pingback: Ituran Seguro Liberty
Pingback: Seguro Viagem Escolar
Pingback: Seguro Viagem Estudante
Pingback: Seguro Residencial
Pingback: Ituran Seguro HDI
Pingback: Perfumes Hinode: Grupo Hinode Vendas - Loja Virtual Hinode
Pingback: Seguro Educacional
Pingback: Seguro Viagem Escolar
Pingback: event tickets online
Pingback: nonton film india terbaru
Pingback: download film tentang cinta
Pingback: nontonmovie.com
Pingback: movie bioskop cinema 21 online
Pingback: Ituran Seguro Liberty
Pingback: Ituran com Seguro
Pingback: streaming film online
Pingback: nonton film online gratis
Pingback: Rastreador Ituran
Pingback: bioskopkeren
Pingback: download film box office
Pingback: Seguro de vida pequenas empresas
Pingback: Funny fashion
Pingback: nontonmovie.com
Pingback: hinode cadastro
Pingback: lk21 online
Pingback: nonton movie horror
Pingback: Seguro equipamentos portateis
Pingback: nonton cinemaindo
Pingback: streaming film online
Pingback: bioskop online sub indo
Pingback: Porto Seguro Pet
Pingback: Seguro de vida pequenas empresas
Pingback: china clothes wholesaler
Pingback: Bollywood News
Pingback: consorcio porto seguro
Pingback: Seguro equipamentos
Pingback: Seguro Viagem Estudante
Pingback: Plano de Saude Cachorro
Pingback: personal finance newsletters
Pingback: Seguro Viagem Internacional
Pingback: Seguro Viagem Intercambio
Pingback: daily stock market commentary
Pingback: Online Travel agency for Flight
Pingback: Seguro eletronicos
Pingback: Ituran com Seguro
Pingback: investment newsletter
Pingback: Port Matilda PA
Pingback: WEDDING DJS NEAR ME
Pingback: Porto seguro conecta
Pingback: IN THE GROOVE EVENTS
Pingback: Ultrarecovery
Pingback: Ultrarecovery
Pingback: BEST EVENT EXPERIENCE
Pingback: NW DJ
Pingback: ALL-INCLUSIVE EVENT COMPANY
Pingback: Plano de Saude Gatos
Pingback: #1 DJ SERVICE
Pingback: human hair weave
Pingback: Pediatrics
Pingback: human hair weave
Pingback: human hair weave
Pingback: MOBILE DJ
Pingback: DJ SERVICE
Pingback: ac service arlington tx
Pingback: Gas dryer
Pingback: Dryer installation
Pingback: dryer wizard
Pingback: Gas dryer
Pingback: Dryer air flow
Pingback: Dryer vent
Pingback: Chicago dryer vent installation
Pingback: car sales website
Pingback: home ac repair grand prairie tx
Pingback: periscope dryer vent
Pingback: small businesses online
Pingback: NW DJ
Pingback: Gas dryer
Pingback: Vent
Pingback: Dryer lint
Pingback: dryer installation
Pingback: how to dryer vent cleaning
Pingback: hvac grand prairie tx
Pingback: air vent installation
Pingback: clothes dryer vent booster
Pingback: dryer lint remover
Pingback: g spot vibrator
Pingback: CORPORATE EVENT DJS
Pingback: dryer vent pipes
Pingback: grand praire ac
Pingback: dallas web design firms
Pingback: website design grand prairie
Pingback: air conditioner repair services
Pingback: air conditioner repair services
Pingback: gutters cleaning service
Pingback: WEDDING DJS NEAR ME
Pingback: clothes dryer vent hose
Pingback: WEDDING DJS NEAR ME
Pingback: dryer vent bucket
Pingback: how to fix dryer vent duct
Pingback: air conditioning grand prairie
Pingback: compact dryer vent
Pingback: roof mounted dryer vents
Pingback: dryer duct cleaning brush
Pingback: website design fort worth
Pingback: periscope dryer vents
Pingback: Clothes dryer repair
Pingback: Dryer
Pingback: Dryer maintenance
Pingback: cleaning dryer vent
Pingback: arlington air conditioning services
Pingback: dryer vent cleaning san francisco
Pingback: website design grand prairie
Pingback: cheap air fryer
Pingback: small businesses website
Pingback: vent dryer cleaning
Pingback: commercial air fryer
Pingback: air fryer xl
Pingback: Dryer Vent Repair
Pingback: air fryer fish
Pingback: Dryer repair service
Pingback: website design dallas texas
Pingback: metal dryer vent
Pingback: seo fort worth
Pingback: TOP DJ COMPANIES
Pingback: dryer vent cleaning supplies
Pingback: air fryer
Pingback: best air fryer recipes
Pingback: who fixes dryer vents
Pingback: power air fryer recipes
Pingback: dryer vent replacement
Pingback: air fryer recipes
Pingback: philips air fryer
Pingback: IN THE GROOVE EVENTS
Pingback: how to clean out dryer
Pingback: how clean dryer vent
Pingback: xnxx anak sekolah
Pingback: dryer brush
Pingback: sekolah sex
Pingback: air fryer price
Pingback: xnxx anak sekolah
Pingback: hood vent cleaning
Pingback: anak sekolah nude
Pingback: the best air fryer
Pingback: search engine optimization dallas
Pingback: fort worth web design
Pingback: porno sekolah
Pingback: best air fryer recipes
Pingback: power air fryer recipes
Pingback: video porno anak sekolah indonesia
Pingback: dryer vent attachment
Pingback: duct pipe
Pingback: phillips air fryer
Pingback: healthy air fryer recipes
Pingback: vidio anak sekolah
Pingback: commercial air fryer
Pingback: ducting supplies
Pingback: digital air fryer
Pingback: these are the best type of cowboy boots
Pingback: how to wear cowboy boots for men
Pingback: energy saving dryer vent
Pingback: air fryer
Pingback: Cowboy Boots For Women With Wide Feet
Pingback: xnxx anak sekolah
Pingback: dallas web design firms
Pingback: air fryer prices
Pingback: best air fryer recipes
Pingback: best air fryer recipes
Pingback: home air systems
Pingback: video bokep sekolah jepang
Pingback: amazon.com air fryer
Pingback: drier vent
Pingback: philip air fryer
Pingback: air deep fryer
Pingback: air fryer recipes
Pingback: anak sekolah nude
Pingback: income opportunities
Pingback: cooks essential air fryer
Pingback: craigslist phoenix free
Pingback: air fryer xl
Pingback: good cowboy boots
Pingback: philip air fryer
Pingback: how long do mobile homes last
Pingback: charity home
Pingback: free bobux
Pingback: video porno anak sekolah indonesia
Pingback: vanderbilt modular homes
Pingback: craigslist free stuff phoenix
Pingback: home improvement stores near me
Pingback: search engine optimization dallas
Pingback: porn sekolah
Pingback: bokep jepang
Pingback: home building supplies
Pingback: free robux roblox
Pingback: mobile home companies
Pingback: where to wear cowboy boots
Pingback: how to get free robux
Pingback: mobile home recycling
Pingback: website design fort worth
Pingback: what is a manufactured home
Pingback: clayton homes financing
Pingback: - ALOukik@123
Pingback: home of grace
Pingback: video porn anak sekolah
Pingback: free trailer houses to be moved
Pingback: how to get free robux
Pingback: mobile home salvage mesa az
Pingback: scrapping a mobile home trailer
Pingback: dfw seo
Pingback: how to wear a cowboy hat correctly
Pingback: glendale junction second hand
Pingback: the meadows mobile home park
Pingback: how to get free robux
Pingback: best womens cowboy boots
Pingback: servers
Pingback: how to get free robux
Pingback: website design fort worth
Pingback: how to get free robux
Pingback: how to get free robux
Pingback: how to donate a mobile home
Pingback: stardust phoenix
Pingback: NW DJ
Pingback: video anak sekolah pacaran
Pingback: memek sekolah
Pingback: video bokep sekolah jepang
Pingback: how to get free robux
Pingback: getting rid of old mobiles
Pingback: how to get free robux
Pingback: free robux roblox
Pingback: how to get free robux
Pingback: free bobux
Pingback: free robux roblox
Pingback: old mobile home removal
Pingback: grand prairie web design
Pingback: MOBILE DJ
Pingback: ewean anak sekolah
Pingback: abg arab ngentot
Pingback: cost to remove manufactured home
Pingback: abg crot di mulut
Pingback: arlington seo company
Pingback: free bobux
Pingback: bokep abg indonesia
Pingback: free robux roblox
Pingback: free bobux
Pingback: ngentot abg montok
Pingback: where to send old mobile phones for charity
Pingback: how to get free robux
Pingback: vidio porno abg
Pingback: charitable donations tax deduction calculator
Pingback: video crot mp4
Pingback: where to bring old cell phones
Pingback: recycle mobile phone charity freepost
Pingback: recycle cell phones for charity
Pingback: charity clothes collection from home
Pingback: charity organizations
Pingback: phones for charity
Pingback: free xbox live codes
Pingback: free robux
Pingback: car donation
Pingback: recycle mobiles for charity
Pingback: old mobiles for charity
Pingback: film porno china
Pingback: vidio china sex
Pingback: recycle for charity
Pingback: recycling old phones for money
Pingback: where to dispose of old cell phones
Pingback: how should cowboy boots fit
Pingback: abg ngemut kontol
Pingback: charity events
Pingback: best car donation charities
Pingback: phones for charity
Pingback: best car donation charities
Pingback: bokep indo abg
Pingback: recycle for charity
Pingback: cell phone donation drop off locations
Pingback: donate your phone
Pingback: best mobile phone recycling
Pingback: china hot videos
Pingback: disposable cell phone
Pingback: How To Care For Cowboy Boots
Pingback: abg cantik ml
Pingback: free psn codes
Pingback: free xbox live codes
Pingback: most popular cowgirl boots
Pingback: bokep indo china
Pingback: chapter 6 courage and moral leadership
Pingback: carpet clean
Pingback: courage z
Pingback: free instagram followers
Pingback: hvac vents
Pingback: cleaning company
Pingback: how to turn old desktop into mining rig
Pingback: BEST EVENT EXPERIENCE
Pingback: air duct cleaning canton
Pingback: courage kenny rehabilitation institute
Pingback: air duct cleaning carleton
Pingback: free robux
Pingback: abg toge ngewe
Pingback: free psn codes
Pingback: air duct cleaning
Pingback: old desktop bitcoin mining rig
Pingback: courage sentence
Pingback: vent cleaning
Pingback: free psn codes
Pingback: blaze u - courage
Pingback: ALL-INCLUSIVE EVENT COMPANY
Pingback: china porn videos
Pingback: courage poem
Pingback: duct cleaning brushes
Pingback: duct repair
Pingback: china girl nude
Pingback: TOP DJ COMPANIES
Pingback: courage zombie director
Pingback: bitcoin mining old computer
Pingback: 47 courage rd waco ky
Pingback: e e cummings courage
Pingback: abg porn indonesia
Pingback: air duct cleaning milan
Pingback: house cleaning services
Pingback: mountain air duct services
Pingback: airduct cleaning
Pingback: download video gay china
Pingback: pro duct cleaning
Pingback: abg bugil ngentot
Pingback: hood duct cleaning
Pingback: china porn hot
Pingback: free psn codes
Pingback: n courage driving school
Pingback: t c stallings courageous
Pingback: air duct cleaning process
Pingback: massage sex china
Pingback: clean air company
Pingback: the secret of happiness movie
Pingback: do it yourself duct cleaning
Pingback: air duct system
Pingback: courage b the profit update
Pingback: home carpet cleaning company
Pingback: free instagram followers
Pingback: china porno sex
Pingback: Old computer mining rig cheap
Pingback: courage d'esprit
Pingback: roseville cleaning services
Pingback: 192.168.0.1
Pingback: abg montok sex
Pingback: video seks abg indo
Pingback: old desktop computer mining rig PC
Pingback: china sex massage
Pingback: pro air services
Pingback: memek abg video
Pingback: porn abg smp
Pingback: 192.168.0.1
Pingback: free cleaning
Pingback: 192.168.0.1
Pingback: video abg mandi telanjang
Pingback: cleaning the dryer
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: cleaning service california
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: mining rig old desktop
Pingback: latest govt jobs
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: model bokep
Pingback: 192.168.0.1
Pingback: abg bugil bareng
Pingback: download vidio bokeb
Pingback: abg smp 3gp
Pingback: desentupimentos rio moinhos
Pingback: desentupimentos sao nicolau
Pingback: dowload video bokep barat
Pingback: Computer Budget Mining Rig
Pingback: desentupimentos boelhe
Pingback: desentupimentos torno
Pingback: desentupimentos massarelos
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: china xxx hot
Pingback: mining farm from old desktop
Pingback: website design dallas texas
Pingback: desentupimentos sousela
Pingback: china porno
Pingback: 192.168.0.1
Pingback: 192.168.0.1
Pingback: redwab
Pingback: bokep jepang hot
Pingback: happy fathers day
Pingback: 192.168.0.1
Pingback: china bondage
Pingback: computer plug and play mining rig
Pingback: Old Desktop Mining Rig
Pingback: download video ngentot
Pingback: video bokep artis china
Pingback: 192.168.1.254
Pingback: 192.168.1.254
Pingback: 192.168.1.1
Pingback: download bokef
Pingback: desentupimentos aveleda
Pingback: celebrated fathers day
Pingback: china sex massage
Pingback: japanese mom porn
Pingback: pocket pussy reviews
Pingback: xxx bokep
Pingback: vido bokep
Pingback: download video bf china
Pingback: desentupimentos alfena
Pingback: desentupimentos macieira
Pingback: desentupimentos frazao arreigada
Pingback: desentupimentos santa maria avioso
Pingback: video sekolah sex
Pingback: desentupimentos nevogilde 2
Pingback: 192.168.1.254
Pingback: 192.168.1.254
Pingback: download video bokep terbaru
Pingback: 192.168.1.254
Pingback: jepang bokep
Pingback: kumpulan bokep
Pingback: jav 1080p
Pingback: desentupimentos senhora da hora
Pingback: 192.168.1.1
Pingback: desentupimentos canelas 2
Pingback: adul bokep
Pingback: desentupimentos capela
Pingback: desentupimentos terroso povoa de varzim
Pingback: desentupimentos carvalhosa
Pingback: desentupimentos vila nova da telha maia
Pingback: desentupimentos termas sao vicente
Pingback: simpliesgoto
Pingback: vidie bokep
Pingback: desentupimentos amadora
Pingback: desentupimentos covelas
Pingback: desentupimentos paranhos porto
Pingback: watch rape porno online
Pingback: video sekolah sex
Pingback: desentupimentos braga
Pingback: nafsu pelajar sekolah
Pingback: mom sex tube
Pingback: vidio porno anak sekolah indonesia
Pingback: galeria
Pingback: desentupimentos maia
Pingback: watch gay porno online
Pingback: xnxx anak sekolah
Pingback: desentupimentos cascais
Pingback: watch porno online free
Pingback: watch porno online hd
Pingback: teens porno online watch
Pingback: watch porno video online
Pingback: desentupimentos crestuma gaia
Pingback: the best porno watch online
Pingback: watch japanese porno online
Pingback: cewek bugil di sekolah
Pingback: film porno online free watch
Pingback: desentupimentos lever gaia
Pingback: watch films porno online
Pingback: desentupimentos povoa de varzim povoa de varzim
Pingback: desentupimentos penamaior
Pingback: watch online first time porno
Pingback: lesbian porno watch online
Pingback: desentupimentos grijo gaia
Pingback: desentupimentos fanzeres gondomar
Pingback: watch online first time porno
Pingback: porno sex video watch online
Pingback: desentupimentos lever gaia 2
Pingback: porno sex video watch online
Pingback: watch old porno online
Pingback: cochacker top
Pingback: desentupimentos bonfim porto
Pingback: teens porno online watch
Pingback: desentupimentos sermonde gaia
Pingback: desentupimentos medas
Pingback: desentupimentos vilar de andorinho gaia
Pingback: desentupimentos santa cruz do bispo matosinhos 2
Pingback: desentupimentos bonfim
Pingback: widehackscomclashroyale
Pingback: mobilestriketool online
Pingback: memek abg jerman
Pingback: desentupimentos aveiro
Pingback: desentupimentos vilar vila do conde
Pingback: bokep di sekolah
Pingback: desentupimentos pedroucos maia
Pingback: onlyrobux site
Pingback: desentupimentos aveleda viladoconde
Pingback: bokep mahasiswa
Pingback: sekolah porn
Pingback: desentupimentos aveiro
Pingback: desentupimentos touguinha vila do conde
Pingback: desentupimentos rio mau vila do conde
Pingback: desentupimentos castelo da maia
Pingback: anak sekolah smp
Pingback: desentupimentos louredo
Pingback: secret of happiness in hindi
Pingback: rbuxcheats club
Pingback: desentupimentos ramalde
Pingback: desentupimentos marco de canaveses
Pingback: desentupimentos matosinhos
Pingback: desentupimentos avintes
Pingback: desentupimentos baiao
Pingback: ngentot abg cabe cabean
Pingback: courage 53
Pingback: desentupimentos lousada
Pingback: 8ballpool4cash com
Pingback: video bokep terbaru
Pingback: quotes on courage
Pingback: bokep sekolah indo
Pingback: desentupimentos estrela
Pingback: bercinta abg
Pingback: golfclashtool com
Pingback: desentupimentos valbom
Pingback: desentupimentos lamelas
Pingback: nba 2k17
Pingback: courage d'esprit
Pingback: watch porno movies online for free
Pingback: desentupimentos bougado
Pingback: desentupimentos ribeira do porto 2
Pingback: desentupimentos antas
Pingback: desentupimentos rebordosa
Pingback: worldhack online hayday
Pingback: desentupimentos covelas
Pingback: telanjang di sekolah
Pingback: porno sex video watch online
Pingback: desentupimentos sao tome de negrelos
Pingback: desentupimentos oeiras
Pingback: csr2 site
Pingback: watch gay porno online
Pingback: www sex anak sekolah com
Pingback: DominoBet
Pingback: desentupimentos valbom gondomar
Pingback: 1 courage court
Pingback: fort courage f troop
Pingback: what is the best weight loss pill
Pingback: desentupimentos leca da palmeira
Pingback: desentupimento sao pedro fins maia
Pingback: Dewa Poker
Pingback: penis pump
Pingback: TruVision Weight Loss Reviews 2018
Pingback: ml anak sekolah
Pingback: desentupimentos arvore viladoconde
Pingback: How Do You Take TruFix?
Pingback: desentupimentos vilar do pinheiro vila do conde
Pingback: are protein shakes good for weight loss
Pingback: how to loose weight in a week
Pingback: how to lose baby weight
Pingback: Poker88
Pingback: success
Pingback: TruVision Weight Loss
Pingback: jilbob anak sekolah
Pingback: desentupimentos agucadoura povoa de varzim
Pingback: u mobile coverage
Pingback: www bokep anak sekolah com
Pingback: contactos
Pingback: TruVision health Login
Pingback: porn sekolah
Pingback: Agen Bola
Pingback: inspiration
Pingback: nafsu pelajar sekolah
Pingback: how do i loose weight
Pingback: desentupimentos balazar povoa de varzim
Pingback: Pizza Tools
Pingback: TruVision Weight Loss Supplements
Pingback: Listing of ICO Marketing Companies
Pingback: TruVision Weight Loss Products
Pingback: TruVision Side Effects
Pingback: ICO Marketing
Pingback: Pizza Tools
Pingback: Bar Spoons
Pingback: Listing of ICO Marketing Companies
Pingback: internet page
Pingback: porno sekolah
Pingback: negosyo sa bahay
Pingback: food photographer
Pingback: patok na negosyo
Pingback: asenso
Pingback: empleyado o amo
Pingback: IT integration
Pingback: IT support
Pingback: IT integration
Pingback: website directory
Pingback: ofw pag kakakitaan
Pingback: smart business
Pingback: ofw
Pingback: IT integration
Pingback: porno sekolah
Pingback: ICO Marketing Information
Pingback: earn money at home
Pingback: ofw pag kakakitaan
Pingback: ICO Marketing
Pingback: simple business
Pingback: ICO Marketing
Pingback: sekolah 3gp
Pingback: vidio porno anak sekolah indonesia
Pingback: xnxx anak sekolah
Pingback: houngan
Pingback: magic
Pingback: satta matka
Pingback: magic
Pingback: perkosa anak sekolah
Pingback: jilboobs sekolah
Pingback: ngintip anak sekolah
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: anak sekolah jepang porn
Pingback: ICO Marketing
Pingback: satta matka
Pingback: sma bugil di sekolah
Pingback: l¹sk Tynki Gipsowe
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Spatulas
Pingback: Cake Stands
Pingback: Best Quality Kitchen Utensils
Pingback: Listing of ICO Marketing Companies
Pingback: look at here
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Pagina personala
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: what are ben wa balls
Pingback: Onion Goggles
Pingback: ICO Marketing Information
Pingback: sekolah sexx
Pingback: 3gp sekolah
Pingback: Kinfe
Pingback: Susanne Seawright
Pingback: Listing of ICO Marketing Companies
Pingback: Rosemarie Orduno
Pingback: video ngentot di sekolah
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: pelajar sekolah buat maksiat
Pingback: Dwain Bibb
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: earn per week
Pingback: Keeley Frederic
Pingback: Codi Broaddus
Pingback: Gregoria Rosner
Pingback: ICO Marketing Information
Pingback: bokep pelajar sekolah
Pingback: Sebrina Weiss
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Serina Mealy
Pingback: click for more
Pingback: toket sekolah
Pingback: Katelin Vanzile
Pingback: Marylouise Hasegawa
Pingback: desentupimentos beire
Pingback: click for more
Pingback: ICO Marketing
Pingback: desentupimentos ferreira
Pingback: ICO Marketing Information
Pingback: desentupimentos areias sequeiro lama e palmeira
Pingback: ICO Marketing
Pingback: Georgine Jasso
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: desentupimentos penamaior
Pingback: Pastry Blenders
Pingback: Bronwyn Hoye
Pingback: desentupimentos azurara
Pingback: Double Boilers
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Delma Christiansen
Pingback: ICO Marketing Information
Pingback: Discover More
Pingback: ICO Marketing Information
Pingback: Good-bye Direct Messages on Instagram: Welcome to Direct
Pingback: ICO Marketing Information
Pingback: Learn More
Pingback: Learn More
Pingback: Cocktails Picks
Pingback: 5 Reasons Why Buying Fake Followers Will Kill Your Account
Pingback: profits
Pingback: Workmacro - Real Organic Instagram Growth
Pingback: Step by Step Guide to Building a Super Learning Plan
Pingback: Listing of ICO Marketing Companies
Pingback: sony
Pingback: Read More
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: Click Here
Pingback: Listing of ICO Marketing Companies
Pingback: Regram as a Core Instagram Feature Coming Soon in 2018
Pingback: ICO Marketing Information
Pingback: xnxx anak sekolah
Pingback: Homepage
Pingback: Click This Link
Pingback: Go Here
Pingback: Read More
Pingback: Read More
Pingback: video bokeb anak sekolah
Pingback: Read This
Pingback: bokep indo streming
Pingback: Discover More Here
Pingback: How to Schedule Instagram Carousel Posts
Pingback: ICO Marketing
Pingback: Going Here
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: Clicking Here
Pingback: Visit This Link
Pingback: Find Out More
Pingback: Going Here
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: lesbian toys
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Read More
Pingback: This Tool Automatically Deletes All Your Old Tweets for Free
Pingback: Learn More
Pingback: ICO Marketing
Pingback: Learn More Here
Pingback: 3 Predictions on the Marketing Impacts of Instagram Hashtags
Pingback: Click This Link
Pingback: cryptocurrencies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Read This
Pingback: Click Here
Pingback: Homepage
Pingback: Listing of ICO Marketing Companies
Pingback: Click This Link
Pingback: Clicking Here
Pingback: ICO Marketing Information
Pingback: Discover More Here
Pingback: Click Here
Pingback: jilbab bugil
Pingback: How to Create the Perfect Username for Instagram
Pingback: Listing of ICO Marketing Companies
Pingback: Going Here
Pingback: Therefore dissertation web-sites as a result of online to set-up safe and sound ostensibly taped in the website. rehab near me
Pingback: LED Flame Effect Flickering Fire Light Bulb with Gravity Sensor
Pingback: ICO Marketing Information
Pingback: LED Strip Lights kit with Wireless Remote Controller
Pingback: ICO Marketing
Pingback: Learn More
Pingback: ICO Marketing Information
Pingback: Visit This Link
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: 18 Resources for the Best Attribution Free Content
Pingback: What is Instagram and Why it is Critical for your Business
Pingback: Homepage
Pingback: Discover More
Pingback: 5 Panel Ice Hockey Canvas Art HD Printed Wall Painting
Pingback: streaming bokep indo
Pingback: Learn More Here
Pingback: Read More
Pingback: How to Supercharge your Instagram Layout to Gain Followers
Pingback: Learn More Here
Pingback: Night Light 3D Printing Moon Lamp
Pingback: Discover More
Pingback: Read More
Pingback: Instagram's Top 9: Is it a Complete Waste of Time?
Pingback: Listing of ICO Marketing Companies
Pingback: OG Instagram: Is it Worth Replacing your Instagram App?
Pingback: ICO Marketing Information
Pingback: Discover More
Pingback: Cernitin Pantip
Pingback: Instagram Business Account: Should You Switch?
Pingback: Clicking Here
Pingback: Learn More Here
Pingback: ICO Marketing
Pingback: Learn More
Pingback: Learn More
Pingback: petsafe dog collar battery
Pingback: Click This Link
Pingback: Find Out More
Pingback: Click This Link
Pingback: film bokep indonesia terbaru mp4
Pingback: Discover More Here
Pingback: Listing of ICO Marketing Companies
Pingback: buy dog collar battery
Pingback: buy 4lr44 dog collar battery
Pingback: Click Here
Pingback: Learn More Here
Pingback: Go Here
Pingback: buy cr1/3n battery
Pingback: 4K Stogram: The Best Software to Download Instagram Photos
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Find Out More
Pingback: Click This Link
Pingback: Discover More Here
Pingback: Discover More
Pingback: Read This
Pingback: Go Here
Pingback: Perfect Sleep Full Body Pillow
Pingback: petsafe dog collar battery
Pingback: Listing of ICO Marketing Companies
Pingback: petsafe dog collar battery
Pingback: ICO Marketing
Pingback: dog collar battery
Pingback: nonton bokep
Pingback: Save Hours on Instagram with this New Hootsuite Update
Pingback: Thick Heels Casual Sandals
Pingback: Clicking Here
Pingback: buy 4lr44 battery
Pingback: Listing of ICO Marketing Companies
Pingback: Website Design
Pingback: jilbab bugil
Pingback: Listing of ICO Marketing Companies
Pingback: Discover More Here
Pingback: A Simple Trick on Instagram to Cut Back on your Data Usage
Pingback: Clicking Here
Pingback: How to Upload Photos From Your PC to Instagram
Pingback: Clicking Here
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Summer Gladiator Women Casual Cut-outs Open Toe Thick Heels 13cm Shoes
Pingback: dog collar battery
Pingback: Learn More Here
Pingback: Visit This Link
Pingback: Live Stream Instagram Stories Directly from your Sunglasses
Pingback: petsafe dog collar battery
Pingback: buy dog collar battery
Pingback: buy 4lr44 battery
Pingback: buy 4lr44 battery
Pingback: How to Save Instagram Photos on Your Phone or Desktop
Pingback: Find Out More
Pingback: Find Out More
Pingback: Learn More Here
Pingback: 8 Dumb Ways You Can Get Banned on Instagram
Pingback: No-Bulls&#! Guide to Making Real Money on Instagram
Pingback: Going Here
Pingback: buy 4lr44 dog collar battery
Pingback: petsafe dog collar battery
Pingback: pet safe battery
Pingback: pet safe battery
Pingback: Read This
Pingback: buy 4lr44 dog collar battery
Pingback: 3 Ways to Manage Instagram Direct Messages from your Desktop
Pingback: Find Out More
Pingback: petsafe dog collar battery
Pingback: ICO Marketing
Pingback: dịch vụ marketing online giá rẻ
Pingback: buy cr1/3n battery
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: buy 4lr44 battery
Pingback: Command for IG: The Only Instagram Analytic Tool You Need
Pingback: nonton film bokep
Pingback: ICO Marketing
Pingback: The Truth to Instagram Automation - The Pros and Cons
Pingback: drbokep online
Pingback: buy cr1/3n battery
Pingback: The Most Popular Instagram Bots Compared (2018)
Pingback: Listing of ICO Marketing Companies
Pingback: The Perfect Aspect Ratio for Your Instagram Photos and Stories
Pingback: ICO Marketing
Pingback: instagram fake followers check
Pingback: The Perfect Number of Hashtags to Use in Your Instagram Post
Pingback: Ultimate Guide to Setting Multi User Access for Instagram
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Top 100 Inspiration Quotes From 'Shark Tank' on ABC
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Windowed: The Best Instagram Emulator on Computer
Pingback: swimming pools fairfax va
Pingback: fortnite generator
Pingback: ICO Marketing Information
Pingback: buy high quality backlinks
Pingback: How to Find and Convert Your Most Active Instagram Followers
Pingback: What Your Follower/Following Ratio Say About Your Instagram Account
Pingback: Meet Richie: Our First Customer
Pingback: ICO Marketing Information
Pingback: 5 Tips to Stop People from Unfollowing You on Instagram
Pingback: drbokep online
Pingback: streaming bokep indo
Pingback: The Complete Guide to Designing the Perfect Logo for your Business
Pingback: Listing of ICO Marketing Companies
Pingback: in ground pool builders
Pingback: The Truth Behind the Follow/Unfollow Method on Instagram
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: youtube header maker
Pingback: ICO Marketing
Pingback: swimming pool builders near me
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Directv
Pingback: Directv premium chanels
Pingback: Directv international
Pingback: bokep nyepong
Pingback: Directv nfl sunday ticket
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Directv phone
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: inground swimming pool designs
Pingback: ICO Marketing Information
Pingback: Directv premium chanels
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: nonton bokep indonesia
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Directv premium chanels
Pingback: Listing of ICO Marketing Companies
Pingback: bokep mahasiswi
Pingback: film bokep indonesia terbaru mp4
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: Latest movies
Pingback: ICO Marketing
Pingback: Directv
Pingback: ICO Marketing Information
Pingback: pool 3d model
Pingback: Listing of ICO Marketing Companies
Pingback: Tv + internet
Pingback: Directv sports
Pingback: Directv nfl sunday ticket
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Directv packages
Pingback: bokep semprot
Pingback: Listing of ICO Marketing Companies
Pingback: video bokep indonesia
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Tv + internet
Pingback: ICO Marketing
Pingback: Directv international
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Hd movies
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Latest movies
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: launch own ico
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: Listing of ICO Marketing Companies
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: Wheels and Tires Financing
Pingback: ICO Marketing Information
Pingback: Wheels and Tires Consumer Financing
Pingback: Click Here
Pingback: ICO Marketing Information
Pingback: Read More
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Listing of ICO Marketing Companies
Pingback: Click Here
Pingback: ICO Marketing Information
Pingback: ICO Marketing
Pingback: Dallas Drug Lawyer
Pingback: chaines television africaines
Pingback: Wheels and Tires Consumer Financing
Pingback: Read More
Pingback: Dallas Dwi Attorney
Pingback: ICO Marketing
Pingback: DALLAS SOCIAL MEDIA MARKETING
Pingback: ICO Marketing Information
Pingback: ICO Marketing Information
Pingback: Wheels and Tires Financing
Pingback: Listing of ICO Marketing Companies
Pingback: Web Design Dallas
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Consumer Financing
Pingback: ICO Marketing
Pingback: ICO Marketing Information
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Consumer Financing
Pingback: Web Design Dallas
Pingback: Wheels and Tires Consumer Financing
Pingback: small inground pool designs
Pingback: ICO Marketing
Pingback: Wheels and Tires Financing
Pingback: Listing of ICO Marketing Companies
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Marketing Dallas
Pingback: Wheels and Tires Financing
Pingback: DWi Attorney Dallas
Pingback: SEO Dallas
Pingback: Finger Vibrator Review
Pingback: Dallas Drug Lawyer
Pingback: Wheels and Tires Financing
Pingback: maturnity stores
Pingback: DALLAS EMAIL MARKETING
Pingback: SOCIAL MEDIA MARKETING DALLAS
Pingback: Logo Design Dallas
Pingback: Dallas Criminal Defense
Pingback: Best Dallas Dwi Lawyer
Pingback: Local Search Engine Optimization
Pingback: Dallas Criminal Defense Attorney Dwi
Pingback: Dallas SEO
Pingback: Dallas Website Design
Pingback: Dallas Drug Lawyer
Pingback: DALLAS VIDEO MARKETING
Pingback: Dallas DWI Criminal Defense Attorney
Pingback: DWI Dallas County
Pingback: Dallas Website Design
Pingback: Local SEO
Pingback: DALLAS BLOG
Pingback: Dallas Criminal Defense Attorney Dwi
Pingback: Dwi Lawyer in Dallas
Pingback: Wheels and Tires Consumer Financing
Pingback: Wheels and Tires Consumer Financing
Pingback: Local Search Engine Optimization
Pingback: Wheels and Tires Consumer Financing
Pingback: SEO Dallas
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Https://marketingonlinehcm.net/dich-vu-marketing-online/
Pingback: SEARCH ENGINE OPTIMIZATION
Pingback: Wheels and Tires Consumer Financing
Pingback: DALLAS VIDEO MARKETING
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Consumer Financing
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Financing
Pingback: Wheels and Tires Consumer Financing
Pingback: bảng giá marketing online
Pingback: Desratizacao
Pingback: fifa17.newzgames.com fifa 17
Pingback: verifiedpromo.com pocketmorty pocket mortys
Pingback: Descupinizacao
Pingback: freepokecoinsditch.com pokemon go
Pingback: avengers.cheatyourway.com marvel avengers academy
Pingback: Dedetizacao
Pingback: DALLAS SOCIAL MEDIA MARKETING
Pingback: injusticehack.net supplies metal for zombie gunship survival
Pingback: gamescrash.org idle idle heroes
Pingback: hackcheats.co freefire fire battlegrounds
Pingback: freegems.online clash royale
Pingback: Dedetizadora santana
Pingback: Descupinizacao
Pingback: ffb.apkcare.com fire battlegrounds
Pingback: dedetizacao baratas
Pingback: sword art online memory defrag
Pingback: garden.oghacks.org gardenscape
Pingback: transformersew.extremehack.net transformers earth wars
Pingback: monleghack.club monster legends
Pingback: appsmob.info designhomehack design home
Pingback: xiaomi magazine
Pingback: pdevo.com kombat mortal kombat x
Pingback: xiaomi magazine
Pingback: bladesandrings.updatedhack.com blades and rings
Pingback: xiaomi product compare
Pingback: xiaomi phone
Pingback: justappz.com yugioh yugioh duel links
Pingback: SEARCH ENGINE OPTIMIZATION
Pingback: animationthrowdown.progenz.com animation throwdown
Pingback: DALLAS EMAIL MARKETING
Pingback: yugiohhack.net yugioh duel links
Pingback: xiaomi
Pingback: ogcheats.xyz gardenscape
Pingback: mtpgame.com gardenscape
Pingback: wwesupercard.appcheater.com
Pingback: xiaomi product compare
Pingback: top xiaomi investor
Pingback: mi phone
Pingback: xiaomi stock
Pingback: jetpackjoyridecheats.online jetpack joyride
Pingback: mi phone
Pingback: top xiaomi investor
Pingback: codes gift.com pokemon pokemon magikarp jump
Pingback: gamebag.org piggy boom hack tool piggy boom
Pingback: gameboost.org bridge blitz brigade
Pingback: novahack.online nova legacy trilithium
Pingback: Dallas Website Design
Pingback: Dallas Website Design
Pingback: travel vibrator
Pingback: cops.famtools.com critical ops
Pingback: nosurveysnodownload.com football strike
Pingback: pubg.gghack.com pubg mobile
Pingback: veriedpromo.com pokrmon pokemon magikarp jump
Pingback: cool4apps.com offroad outlaws hack offroad outlaws
Pingback: tricktools.xyz gamecheats marvelpuzzlehack online marvel puzzle quest
Pingback: bravefrontier.supercheats.org brave frontier
Pingback: Ar 15 mount
Pingback: Jewelry fashion unique
Pingback: Ar 15 mount
Pingback: police vest
Pingback: ar 15 handgurad
Pingback: ar15 handguard
Pingback: ar mount
Pingback: FREE LIVE CAM GIRLS
Pingback: roll off dumpster rental Myrtle Beach SC
Pingback: construction disposal Myrtle Beach SC
Pingback: roll off containers rental Myrtle Beach SC
Pingback: construction dumpster rental Myrtle Beach SC
Pingback: first bullet vibrator
Pingback: star wars galactic defense
Pingback: gardenscapes new acres
Pingback: soccer stars online
Pingback: indocinema21
Pingback: guns of boom
Pingback: mlb tap sports baseball
Pingback: kill shot bravo
Pingback: boom beach
Pingback: wwe super card
Pingback: mobile legends
Pingback: nba live mobile
Pingback: bleach brave souls
Pingback: best first time sex toys
Pingback: pokemon magikarp jump
Pingback: farmville 2 country escape
Pingback: line play
Pingback: zombie gunship survival
Pingback: film semi sub indo
Pingback: roller coaster tycoon
Pingback: art of conquest
Pingback: cocoppa play
Pingback: eCom Profit Sniper
Pingback: writeaessay
Pingback: videos
Pingback: shant tv
Pingback: Azizyannere
Pingback: thiet ke web gia re tai da nang
Pingback: elenioragir@
Pingback: hosting
Pingback: Nran Hatik
Pingback: Merjvace
Pingback: shant tv
Pingback: Azizyannere
Pingback: Karmir Blur
Pingback: hayvid
Pingback: armeniatv
Pingback: armeniatv
Pingback: anons
Pingback: Tandem
Pingback: thiet ke website gia re tai quang tr?
Pingback: shant tv
Pingback: hayvid com
Pingback: Raya island tour
Pingback: hosting
Pingback: armeniatv
Pingback: hayvid com
Pingback: eleni oragir@ seria
Pingback: Video Hosting
Pingback: Kisabac Lusamutner
Pingback: Chiang Mai tours
Pingback: Azizyannere
Pingback: Presale list on Epic - vetted blockchain investments by Epic
Pingback: eleni oragir@ seria
Pingback: Epic - professional blockchain token presale community
Pingback: Epic News - leader in blockchain news
Pingback: haykakan hosting
Pingback: shant tv
Pingback: eleni oragir@ seria
Pingback: Merjvace
Pingback: yerevan
Pingback: shant
Pingback: eleni oragir
Pingback: Video Hosting
Pingback: Azizyannere
Pingback: Voske Dproc
Pingback: Harsike
Pingback: Eleni oragire épisode
Pingback: Epic FAQs - Find the answer for your questions about the Epic platform
Pingback: Anuxelinere
Pingback: hayvid
Pingback: About Epic - experienced investors, global executives, and technology experts
Pingback: Armenian Video Hosting
Pingback: eleni oragir@ seria
Pingback: Anuxelinere
Pingback: yerevan
Pingback: Epic Guide - Get yourself familiar with token transactions on Epic platform
Pingback: armenia tv
Pingback: Merjvace
Pingback: hosting
Pingback: Nran Hatik
Pingback: yerevan
Pingback: Follow Epic on Facebook
Pingback: Mexramis
Pingback: shanttv
Pingback: Follow Epic on Twitter
Pingback: Join Epic Telegram
Pingback: eleni oragir
Pingback: Eleni oragiry
Pingback: hayvid com
Pingback: upload
Pingback: haykakan hosting
Pingback: Major Toto Site
Pingback: Harsike
Pingback: Harsike
Pingback: eleni oragir@ seria
Pingback: armeniatv
Pingback: hay vid
Pingback: Eleni oragire épisode
Pingback: brown stains between teeth
Pingback: hayvid com
Pingback: brown spots between teeth
Pingback: amature
Pingback: brown spots on teeth
Pingback: mobile videos
Pingback: Voske Dproc
Pingback: hayvid
Pingback: 8teen
Pingback: shanttv
Pingback: cleaning a dryer vent
Pingback: blow dryer brush
Pingback: amature-porn
Pingback: brown stains between teeth
Pingback: ass-fuck
Pingback: Increased drying time
Pingback: dryer vent clean
Pingback: Dryer vent system
Pingback: best bunny vibrator
Pingback: brown spots between teeth
Pingback: Dryer Vent Pro in Brooklyn
Pingback: Dryer Vent Repair Flatbush
Pingback: asiáticos
Pingback: brown spots on teeth
Pingback: brown stains between teeth
Pingback: dumpster rental Clarendon Hills
Pingback: vent a dryer
Pingback: junk removal
Pingback: installing air ducts
Pingback: air conditioning clean
Pingback: brown spots on teeth
Pingback: dryer exhaust vent
Pingback: commercial dumpster
Pingback: bribe
Pingback: air air conditioning
Pingback: bucetinha
Pingback: need cleaning
Pingback: celeb
Pingback: clothes dryer venting
Pingback: small dumpster rental prices
Pingback: dryer lint remover
Pingback: dryer vent tube
Pingback: rooftop dryer vent
Pingback: bfi waste management
Pingback: butt-sex
Pingback: one day dumpster rental
Pingback: web design Evensville, In
Pingback: ventilation ductwork
Pingback: metal ductwork
Pingback: birds in dryer vent
Pingback: web design Owensboro, KY
Pingback: garbage rental bins
Pingback: foot-fetish
Pingback: dancing
Pingback: toys for couples
Pingback: facebook
Pingback: web design Elizabethtown, ky
Pingback: haul away junk
Pingback: dryer vent clamps
Pingback: web design Evensville, In
Pingback: web design Elizabethtown, ky
Pingback: wall dryer vent
Pingback: disposal container rental
Pingback: free-amateur-videos
Pingback: how to fix drywall
Pingback: dumpster roll off rental
Pingback: local painters
Pingback: drywall sheetrock
Pingback: dumpster rental phoenix
Pingback: ceiling drywall repair
Pingback: chat webcam
Pingback: dumpster rental redford
Pingback: videochat libera
Pingback: dumpster rental michigan
Pingback: videochat gratis
Pingback: videochat per ragazzi
Pingback: drywall contractors near me
Pingback: Bitcoin HYIP
Pingback: chat online senza registrazione
Pingback: gay-bareback
Pingback: replacing drywall
Pingback: drywall subcontractors
Pingback: video chat gratis
Pingback: jugs
Pingback: jackoff
Pingback: roll off dumpster rental
Pingback: chat over 30
Pingback: webchat
Pingback: repaint house
Pingback: dumpster rental sterling hts
Pingback: leche
Pingback: industrial painting companies
Pingback: drywall cracks
Pingback: cam chat
Pingback: gay-black
Pingback: FAST MONEY
Pingback: triple pleasure rabbit
Pingback: chat per donne
Pingback: drywall insulation
Pingback: 10 yard dumpster
Pingback: cost to replace drywall
Pingback: custom drywall
Pingback: drywall installers near me
Pingback: trash dumpsters to rent
Pingback: video chat italia
Pingback: painting companies looking for painters
Pingback: company painting
Pingback: chat per tutti
Pingback: drywall services inc
Pingback: home wall painting
Pingback: contractor referral
Pingback: drywall companies mn
Pingback: 20 yard dumpster cost
Pingback: chat online senza registrazione
Pingback: garbage containers for rent
Pingback: chat
Pingback: webchat over 30
Pingback: fixing a hole in the wall drywall
Pingback: video chatta
Pingback: 20 yard dumpster
Pingback: home painting estimate
Pingback: video chat libera
Pingback: easy drywall repair
Pingback: WORKED AT HOME
Pingback: waste bin rental
Pingback: dumpsters rental
Pingback: Men Tops
Pingback: licensed drywall contractors
Pingback: roll of dumpster
Pingback: public-porn
Pingback: Hyip bitconnect
Pingback: Men Clothing Accessories
Pingback: Men Clothing Accessories
Pingback: outdoorsex
Pingback: Men Suits
Pingback: play
Pingback: dumpster in a bag
Pingback: sexcam
Pingback: Back pain treatment
Pingback: Men Shoes
Pingback: best glass dildo review
Pingback: Men Shoes
Pingback: shaved-pussy
Pingback: dumpster service near me
Pingback: dumpster pick up
Pingback: garbage bin rental prices
Pingback: waste management bins
Pingback: Men Bottoms
Pingback: Men Suits
Pingback: the dumpster
Pingback: Men Suits
Pingback: HYIP WORLD
Pingback: stepbrother
Pingback: stepson
Pingback: Men Shoes
Pingback: Men Shoes
Pingback: jovem
Pingback: vietnam
Pingback: Men Watches
Pingback: Men Watches
Pingback: snatch
Pingback: Men Bottoms
Pingback: Automobiliu nuoma kaune
Pingback: roof repair indianapolis indiana
Pingback: automobilio nuoma
Pingback: flat roof repair indianapolis Indiana
Pingback: Roofing contractos in Carmel Indiana
Pingback: indianapolis Indiana roofers bbb
Pingback: flat roof repair indianapolis Indiana
Pingback: Roofing contractors near me Indianapolis Indiana
Pingback: Indiana roofing company near me
Pingback: Automobiliu nuoma kauno oro uoste
Pingback: indianapolis roofing reviews
Pingback: indianapolis Indiana roofers angie's list
Pingback: White River roofing contractor in INdianapolis Indiana
Pingback: White River roofing contractor Indianapolis IN
Pingback: indianapolis Indiana roofing codes
Pingback: commercial roofing contractors indianapolis indiana
Pingback: White River Roofers Indianapolis Indiana
Pingback: Automobiliu nuoma kauno oro uoste
Pingback: Automobiliu nuoma kauno oro uoste
Pingback: White River roofing contractors indianapolis Indiana
Pingback: i love my momma dog
Pingback: best roofing contractors indianapolis
Pingback: Automobiliu nuoma kaune
Pingback: White River Roofing Contractors in Indianapolis IN
Pingback: Roofing Indianapolis Indiana
Pingback: automobilio nuoma kaune
Pingback: Automobiliu nuoma
Pingback: automobilio nuoma
Pingback: Automobiliu nuoma kaune
Pingback: Roofing contractos in Carmel Indiana
Pingback: Roofing contractos in Carmel Indiana
Pingback: White River Roofers in Indianapolis In
Pingback: indianapolis roofing reviews
Pingback: how to register marriage in delhi
Pingback: how to register marriage in delhi
Pingback: automobilio nuoma
Pingback: roofing and siding contractors indianapolis Indiana
Pingback: marriage registration in delhi
Pingback: Automobiliu nuoma kauno oro uoste
Pingback: Roofing contractos in Carmel Indiana
Pingback: Automobiliu nuoma
Pingback: indianapolis Indiana roofing codes
Pingback: roofing contractors near me Indianapolis Indiana
Pingback: White River roofing contractor Indianapolis IN
Pingback: indianapolis commercial roofing companies
Pingback: indianapolis Indiana roofing permit
Pingback: hail damage roof repair indianapolis Indiana
Pingback: indianapolis commercial roofing companies
Pingback: Donald sing
Pingback: roofing indianapolis
Pingback: Indiana roofing company near me 46205
Pingback: indianapolis Indiana roofers angie's list
Pingback: indianapolis Indiana roofing repair
Pingback: online marriage registration in delhi
Pingback: Roofing Contractors in Avon In
Pingback: Marriage Registration
Pingback: how to register marriage in delhi
Pingback: automobilio nuoma
Pingback: automobilio nuoma
Pingback: automobilio nuoma kaune
Pingback: first time anal
Pingback: marriage registration in delhi
Pingback: Online appointment for marriage registration Delhi
Pingback: marriage certificate in ghaziabad
Pingback: Limo Lounge
Pingback: Marriage Registration
Pingback: Marriage Registration
Pingback: Automobiliu nuoma
Pingback: marriage certificate in ghaziabad
Pingback: Online appointment for marriage registration Delhi
Pingback: Stretch
Pingback: tatkal marriage certificate in delhi
Pingback: how to register marriage in delhi
Pingback: marriage registration in delhi
Pingback: Tips for Healthy Heart.
Pingback: Kidney stone, The Different Types Of Kidney Stones and Symptoms
Pingback: Top 10 benefits of morning walk:
Pingback: Easy Ways to Lower Blood Sugar Naturally.
Pingback: marriage registration fees in delhi
Pingback: 15: Simple remedies to lose belly fat fast !
Pingback: sex lube
Pingback: Some exercise tips for getting six pack abs?
Pingback: Health Easy Tips
Pingback: marriage certificate in delhi
Pingback: Top 12 Superfoods for Weight Lose.
Pingback: automobilio nuoma
Pingback: tatkal marriage certificate in delhi
Pingback: document require for marriage certificate
Pingback: marriage certificate in delhi
Pingback: Top Health and Fitness Tips, Make your life Best
Pingback: far cry 5 gameplay
Pingback: marriage certificate in delhi
Pingback: 5 Skin care tips to control Acne/Pimples.
Pingback: how to register marriage in delhi
Pingback: tatkal marriage certificate in delhi
Pingback: Best Fitness Tips.
Pingback: DC Transportation
Pingback: Court Marriage
Pingback: 10 Health Benefits of Drinking Water
Pingback: Chauffeurs
Pingback: Nikah Marriage Registration
Pingback: Simple Home Remedies for Oily Skin
Pingback: 9 Life-Changing Ways Your dog Can Improve Your Health
Pingback: 11 Best Muscle Building Tips.
Pingback: alternative kmu finanzierung
Pingback: betrieb finanzieren
Pingback: alternative startup finanzierung
Pingback: got caught masturbating
Pingback: korektura
Pingback: characteristics of an entrepreneur
Pingback: how to be an entrepreneur
Pingback: Wedding
Pingback: how to be an entrepreneur
Pingback: smooth jazz radio
Pingback: business development plan
Pingback: qualities of an entrepreneur
Pingback: Luxury Car Service
Pingback: Jupiter Taweez for money
Pingback: business development plan
Pingback: Healing by Gemstone
Pingback: business proposal sample
Pingback: Muslim girl name
Pingback: business plan für bank erstellen
Pingback: Best name for new born
Pingback: creating a brand
Pingback: alternative betriebs finanzierung
Pingback: eigenes restaurant erööfnen
Pingback: Limo Lounge
Pingback: Islamic Baby names
Pingback: DMV Transportation
Pingback: Distance Healings
Pingback: business plan ppt
Pingback: Jupiter Taweez for money
Pingback: alternative kmu finanzierung
Pingback: characteristics of an entrepreneur
Pingback: qualities of an entrepreneur
Pingback: Gemstone Healing
Pingback: alternative startup finanzierung
Pingback: business proposal sample
Pingback: alternative kmu finanzierung
Pingback: alternative startup finanzierung
Pingback: eigenes restaurant erööfnen
Pingback: business proposal sample
Pingback: alternative startup finanzierung
Pingback: Pentagon City
Pingback: Limo from VA
Pingback: Http://suckhoethuongthuc.org/phu-khoa
Pingback: specialized knowledge
Pingback: coir pith bricks exporters
Pingback: Cut the Rope
Pingback: Family, Cosmetic & Implant Dentist in Temple Terrace, FL
Pingback: Specialized Knowledge
Pingback: specialized knowledge
Pingback: specialized knowledge and skills
Pingback: fantasy role playing games
Pingback: specialized knowledge and skills
Pingback: Dominion
Pingback: specialized knowledge
Pingback: specialized knowledge definition
Pingback: specialized knowledge and skills
Pingback: specialized knowledge and skills
Pingback: specialized knowledge definition
Pingback: specialized knowledge
Pingback: Specialized Knowledge
Pingback: Root Canals Temple Terrace and Tampa
Pingback: specialized knowledge assessment
Pingback: specialized knowledge think and grow rich
Pingback: Specialized Knowledge
Pingback: specialized knowledge assessment
Pingback: Specialized Knowledge
Pingback: specialized knowledge and skills
Pingback: specialized knowledge
Pingback: specialized knowledge
Pingback: gaming company
Pingback: specialized knowledge
Pingback: Specialized Knowledge
Pingback: Personal Injury Attorney Tampa
Pingback: specialized knowledge assessment
Pingback: specialized knowledge assessment
Pingback: coir fibre bale manufacturers
Pingback: specialized knowledge assessment
Pingback: specialized knowledge
Pingback: specialized knowledge definition
Pingback: specialized knowledge assessment
Pingback: Specialized Knowledge
Pingback: specialized knowledge think and grow rich
Pingback: Logan's Quest
Pingback: Buy Medical Marijuana Online
Pingback: Veneers/Lumineers® Temple Terrace and Tampa
Pingback: rpg
Pingback: design games
Pingback: Personal Injury Lawyer Tampa, FL
Pingback: Day's End
Pingback: peanuts suppliers
Pingback: Team
Pingback: Bridges Temple Terrace and Tampa
Pingback: Projects
Pingback: platformer
Pingback: Keighley Bradford Sowerby Bridge Hebden Bridge Servicing Company
Pingback: Wrongful Death Attorney Tampa, FL
Pingback: best rpg games
Pingback: specialized knowledge assessment
Pingback: specialized knowledge assessment
Pingback: See More...
Pingback: specialized knowledge assessment
Pingback: specialized knowledge definition
Pingback: pÅisluenství k herním konzolím
Pingback: SMV EXPORTS
Pingback: Specialized Knowledge
Pingback: specialized knowledge assessment
Pingback: specialized knowledge assessment
Pingback: Hvac Service
Pingback: specialized knowledge
Pingback: CONTACT
Pingback: specialized knowledge and skills
Pingback: Specialized Knowledge
Pingback: specialized knowledge assessment
Pingback: specialized knowledge
Pingback: Specialized Knowledge
Pingback: Day's End
Pingback: specialized knowledge assessment
Pingback: specialized knowledge and skills
Pingback: edmonton game design
Pingback: OUR GAMES
Pingback: best rpg games
Pingback: 21st Century Pizza
Pingback: alchemy
Pingback: A/C Installation Tampa
Pingback: Painting Contractors Tampa
Pingback: Towing Tampa and Wesley Chapel
Pingback: Pizza 21st Century Menu
Pingback: TEAM
Pingback: gaming companies
Pingback: Roof Maintenance Tampa
Pingback: Spas/swimming pools wiring Tampa
Pingback: Civil Mediation Lawyer Tampa
Pingback: 21st Century Pizza
Pingback: making games
Pingback: Cooling System Repair Tampa and Wesley Chapel
Pingback: fantasy role playing games
Pingback: Water filtration Tampa
Pingback: Garage door screens Tampa
Pingback: Emergency Towing Tampa and Wesley Chapel
Pingback: Carpal tunnel Tampa
Pingback: Weatherproofing Tampa
Pingback: Premises Liability Mediation Attorney Tampa
Pingback: Carpet Sales and Installation Tampa
Pingback: Pool Deck Painting Tampa
Pingback: Temporary and permanent Fence Tampa
Pingback: iptv kodi addons for watching live tv
Pingback: Kitchen and Bath Fixtures Tampa
Pingback: Whiplash Injury Attorneys Tampa
Pingback: Bankruptcy Attorneys Tampa
Pingback: Personal Injury Attorney Tampa
Pingback: Harmful Drugs Lawyers Tampa
Pingback: Nursing Home Abuse Attorneys Tampa
Pingback: Rear-end collisions Tampa
Pingback: 1/2 Mile Car Racing
Pingback: Xem truyền hình vtv3 hd
Pingback: graphics & design
Pingback: designer ux
Pingback: free logo design
Pingback: where to find designers
Pingback: Made in USA
Pingback: USA Apparel
Pingback: Made in USA
Pingback: USA Apparel
Pingback: Manufacturing USA
Pingback: USA Brand
Pingback: Permanent scarring and disfigurement Tampa
Pingback: Intellectual Property Attorneys Tampa
Pingback: Car Show Gila Bend, Arizona
Pingback: USA Apparel
Pingback: designs
Pingback: Made in USA
Pingback: illustrator logo design
Pingback: Business Bankruptcy Lawyers Tampa
Pingback: Manufacturing USA
Pingback: Made in USA
Pingback: Made in USA
Pingback: USA Brand
Pingback: designer
Pingback: Manufacturing USA
Pingback: Paternity Attorneys Tampa
Pingback: USA Apparel
Pingback: Made in USA
Pingback: Assault Attorneys Tampa
Pingback: Manufacturing USA
Pingback: Manufacturing USA
Pingback: Manufacturing USA
Pingback: USA Apparel
Pingback: USA Apparel
Pingback: USA Apparel
Pingback: USA Brand
Pingback: reusable
Pingback: Made in USA
Pingback: rife machine
Pingback: Discrimination Lawyers Tampa
Pingback: Living Trust Attorneys Tampa
Pingback: rife machine
Pingback: Commercial Land Disputes Lawyers Tampa
Pingback: streaming film semi japang
Pingback: outoftheblue
Pingback: Special Dietary For Private Customers
Pingback: Outside Events
Pingback: of
Pingback: san diego wedding cost
Pingback: wedding cost
Pingback: catering wedding
Pingback: blue catering wedding
Pingback: Italian Food
Pingback: catering
Pingback: wedding budget
Pingback: Waiter Service
Pingback: new york rock stations
Pingback: hard rock news
Pingback: breaking rock news
Pingback: awkward sex experiences
Pingback: Vaginal Exercise Balls
Pingback: Comex Dynamics Solutions LLC
Pingback: Get More Information
Pingback: Click the Following Internet Page
Pingback: go here
Pingback: sasha grey pocket pussy review
Pingback: indocinema21
Pingback: read more
Pingback: Get More Information
Pingback: go here
Pingback: Click the Following Internet Site
Pingback: go here
Pingback: Read My Article
Pingback: Visit This Webpage
Pingback: go to my blog
Pingback: go to my blog
Pingback: go here
Pingback: home page
Pingback: Click Here For More Information
Pingback: Click Here For More Info
Pingback: Check Out These Helpful Tips
Pingback: Expedited Exempt Inc Broker
Pingback: go to my blog
Pingback: Read This Page
Pingback: Click Here For More Information
Pingback: Check Out This Article
Pingback: sex toys
Pingback: Read More About This
Pingback: Click the Following Internet Site
Pingback: go to my blog
Pingback: Click the Following Article
Pingback: Visit This Webpage
Pingback: Read Much More
Pingback: Click Here For More Information
Pingback: find more
Pingback: Visit This Webpage
Pingback: home page
Pingback: Click Here For More Info
Pingback: Visit URL
Pingback: Click the Following Internet Page
Pingback: Zayan Metal Exports Inc dba Texas Freight Carriers
Pingback: stylish casual outfits
Pingback: instagram profile viewer
Pingback: political analysis
Pingback: natural
Pingback: etui na telefon
Pingback: Consumer Financing
Pingback: lesbian straps
Pingback: shopping halal
Pingback: farmac?utico Alex Sandro Alves
Pingback: Servi?os Farmac?uticos
Pingback: shopify dropshipping tutorial for beginners
Pingback: ecommerce
Pingback: entrevista
Pingback: capas originais huawei p9 lite
Pingback: Palavra-chave
Pingback: #NAME?
Pingback: capas huawei ascend p7
Pingback: capas huawei ascend +w1
Pingback: capas huawei y530
Pingback: silicone vibrator
Pingback: Pop's
Pingback: capas para telemoveis
Pingback: Palavra-chave
Pingback: influencer marketing
Pingback: e-commerce
Pingback: capas huawei ascend p6
Pingback: influencer marketing
Pingback: shopping halal
Pingback: #NAME?
Pingback: capas huawei ascend g6
Pingback: Servi?os Farmac?uticos
Pingback: capas huawei ascend p6
Pingback: farmacia
Pingback: lmobile
Pingback: farmac?utico Alex Sandro Alves
Pingback: capas telemoveis
Pingback: capas huawei p10 lite
Pingback: capas de telemoveis
Pingback: capas de telemoveis
Pingback: Capas Huawei Mate 8
Pingback: capas para telemoveis
Pingback: capas de telemoveis
Pingback: capas iphone x
Pingback: l mobile
Pingback: capas huawei p10 lite
Pingback: bateria i9300
Pingback: lmobile
Pingback: forex
Pingback: cbse school in kumbakonam
Pingback: best school in kumbakonam
Pingback: top cbse schools in kumbakonam
Pingback: capas telemoveis
Pingback: greekdrill1.blog5.net/11811060/about-school-in-kumbakonam
Pingback: top cbse schools in kumbakonam
Pingback: good schools in kumbakonam
Pingback: top5 schools in kumbakonam
Pingback: capas huawei p10 lite
Pingback: good schools in kumbakonam
Pingback: bateria i9300
Pingback: good schools in kumbakonam
Pingback: good schools in kumbakonam
Pingback: greekdrill1.blog5.net/11811060/about-school-in-kumbakonam
Pingback: greekdrill1.blog5.net/11811060/about-school-in-kumbakonam
Pingback: capas telemovel
Pingback: capas huawei ascend p6
Pingback: lmobile
Pingback: l mobile
Pingback: kumbakonam private schools list
Pingback: capas de telemoveis
Pingback: good schools in kumbakonam
Pingback: Capas Huawei Mate 8
Pingback: Palavra-chave
Pingback: Best Roofing Contractors in chennai
Pingback: capas huawei ascend p7
Pingback: Palavra-chave
Pingback: hochzeit standesamt musik
Pingback: capas de telemoveis
Pingback: capas huawei y530
Pingback: Best Roofing Contractors in chennai
Pingback: industrial roofing contractors chennai
Pingback: capas nokia lumia 620
Pingback: hochzeitsmusik wien
Pingback: [capas para lumia 625]
Pingback: metal roofing contractors chennai
Pingback: bolsa para telemovel corrida
Pingback: bolsa para telemovel corrida
Pingback: [capas iphone 8 plus worten]
Pingback: +peliculas +xiaomi +note 5
Pingback: peliculas alcatel ot pop c7
Pingback: capas sony xperia j
Pingback: metal terrace roofing chennai
Pingback: residential terrace roofing contractors chennai
Pingback: residential terrace roofing contractors chennai
Pingback: partyband buchen
Pingback: capas sony xperia j
Pingback: bolsa para telemovel corrida
Pingback: polycarbonate terrace roofing contractors
Pingback: peliculas alcatel ot pop c7
Pingback: pelicula alcatel one touch pop c7
Pingback: +capas +note 4 mediatek
Pingback: peliculas samsung galaxy y
Pingback: agape wien live
Pingback: Paramedic salary
Pingback: pelicula alcatel one touch pop c7
Pingback: pel?culas para samsung galaxy s duos
Pingback: +xiaomi redmi 4 pro +capa
Pingback: [capas iphone 8 plus worten]
Pingback: capas para iphone +8 plus
Pingback: photo booth hire sydney
Pingback: photo booth hire sydney
Pingback: musik zur standesamtlichen trauung
Pingback: hochzeit party musik
Pingback: capas para iphone +8 plus
Pingback: capa alcatel one touch pop c7
Pingback: coverband für hochzeit
Pingback: musik trauung
Pingback: baterias para samsung s5
Pingback: +pelicula asus zenfone 4 ze554kl
Pingback: capas huawei ascend +g300
Pingback: capas huawei ascend y300
Pingback: +pelicula +zenfone +4max
Pingback: musik für das standesamt
Pingback: +zenfone +4max +pelicula
Pingback: capas huawei ascend y300
Pingback: musikband für hochzeit
Pingback: +pelicula +asus +zenfone +4 max
Pingback: Fengshui bangalore
Pingback: Dr rathi prabhu
Pingback: baterias para samsung s5
Pingback: capas para huawei ascend g6
Pingback: hochzeitsband österreich
Pingback: [pelicula de vidro huawei p9]
Pingback: +asus +4 max +peliculas
Pingback: open air booth
Pingback: the the booth fairy
Pingback: j5 2016 peliculas
Pingback: [capas para o huawei p9 lite]
Pingback: Vastu bangalore
Pingback: [pelicula de vidro huawei p9]
Pingback: Vastu shop bangalore
Pingback: j5 2016 peliculas
Pingback: +pelicula +asus +zenfone +4 max
Pingback: +asus +4 max +peliculas
Pingback: +asus +4 max +peliculas
Pingback: +idol 5+ capas
Pingback: How to spot a fake louis vuitton
Pingback: capa para huawei g750
Pingback: capas para huawei ascend g6
Pingback: [capa para nokia lumia 625]
Pingback: +xiaomi note 4 mediatek +capas
Pingback: capas para telemoveis huawei ascend y530
Pingback: louis vuitton authentication services
Pingback: Fengshui bangalore
Pingback: capas Sony Xperia +M5
Pingback: shop pre-owned designer bags
Pingback: capas para telemoveis huawei ascend y530
Pingback: [capa lumia 620 comprar]
Pingback: +note 4 mediatek +capa
Pingback: the the booth fairy
Pingback: Eco Wood Alternative
Pingback: snappy booths
Pingback: Melamine Wood Alternative
Pingback: capas para nokia lumia 830
Pingback: Wholesale Melamine Panels
Pingback: the rabbit vibrator
Pingback: +xiaomi redmi 5C +capas
Pingback: Eco Friendly Melamine
Pingback: legos in my louis partnerships
Pingback: capas alcatel c7
Pingback: nwpsocal.com
Pingback: +xiaomi redmi note 4 mediatek +capa
Pingback: National Wood Products Melamine Panels
Pingback: contact legos in my louis
Pingback: Wholesale Melamine Panels
Pingback: +xiaomi redmi note 4 mediatek +capa
Pingback: authenticating antique louis vuitton
Pingback: +xiaomi redmi note 4 mediatek +capas
Pingback: capas nokia lumia +925
Pingback: Melamine Cabinet Material
Pingback: [capas para nokia lumia 625]
Pingback: Eco Wood Alternative
Pingback: painting a union jack dresser
Pingback: Stevenswood Melamine Wood
Pingback: 10 things no one tells you about having a second kid
Pingback: +xiaomi redmi note 4 mediatek +capa
Pingback: Wholesale Melamine Panels
Pingback: Melamine Cabinet Material
Pingback: capas nokia lumia +925
Pingback: [capa para nokia lumia 625]
Pingback: capas nokia lumia +925
Pingback: Melamine Wood Alternative
Pingback: snappy booths
Pingback: National Wood Products Melamine
Pingback: bolsa telemovel desporto
Pingback: Melamine Southern California
Pingback: photbooth hire sydney
Pingback: [pelicula de vidro lg g3]
Pingback: Textured Melamine Wood Alternative
Pingback: the the booth fairy
Pingback: a to z style guide
Pingback: flying with kids internationally
Pingback: san diego kid friendly beach hotel
Pingback: first time rabbit vibrator
Pingback: bumper iphone
Pingback: microsoft points code generator
Pingback: capas para nokia lumia 620
Pingback: +bateria +iPhone +5C
Pingback: Textured Melamine Wood Alternative
Pingback: bateria samsung s3 mini
Pingback: capas para telemoveis nokia
Pingback: +pelicula +Idol 5S
Pingback: Melamine Formica Type Material
Pingback: +bateria +iPhone +5C
Pingback: Eco Friendly Melamine
Pingback: +comprar +bateria +iphone 4s
Pingback: Wholesale Melamine Panels
Pingback: National Wood Products Melamine
Pingback: capas nokia lumia 900
Pingback: capas para nokia 5230
Pingback: capas para alcatel one touch pop c9
Pingback: Thermafused Melamine
Pingback: +comprar +bateria +iphone 4s
Pingback: Melamine Panels
Pingback: marble balloons
Pingback: free xbox microsoft points
Pingback: capas Huawei Ascend G8
Pingback: bumper iphone 4
Pingback: how to get free microsoft points
Pingback: photocorner
Pingback: open air photo booth
Pingback: [pelicula de vidro lg g3]
Pingback: peliculas samsung galaxy s
Pingback: photbooth hire sydney
Pingback: vedo vibrators
Pingback: peliculas samsung galaxy w
Pingback: capas sony xperia m2
Pingback: +pelicula +asus +4 max
Pingback: +idol 5 +capa
Pingback: pau para selfies
Pingback: extens?vel para selfie
Pingback: +alcatel idol 5 +pelicula
Pingback: peliculas samsung galaxy gio
Pingback: photo booth
Pingback: peliculas samsung galaxy s
Pingback: +alcatel idol 5 +pelicula
Pingback: photo booth sydney
Pingback: +alcatel idol 5 +pelicula
Pingback: [capa para nokia lumia 925]
Pingback: unicorn balloons birthday party supplies
Pingback: extens?vel para selfie
Pingback: +pelicula +asus +4 max
Pingback: bumper iphone 5
Pingback: capa huawei ascend p7
Pingback: +capas +idol 5
Pingback: peliculas samsung galaxy w
Pingback: peliculas samsung galaxy w
Pingback: capas para huawei y530
Pingback: capas huawei p8 lite
Pingback: bateria galaxy s4
Pingback: protector para nokia lumia 625
Pingback: capa huawei ascend g6
Pingback: peak massager
Pingback: capas nokia asha 501
Pingback: affordable photobooth
Pingback: bateria samsung s3
Pingback: open air booth
Pingback: capa flip nokia lumia 630
Pingback: capas para alcatel one touch
Pingback: bateria samsung galaxy ace
Pingback: +j7 2017 +peliculas
Pingback: bateria samsung s3
Pingback: capas nokia asha 501
Pingback: capas para alcatel one touch
Pingback: bateria samsung s3
Pingback: capa nokia lumia 630
Pingback: capas sony xperia u
Pingback: capas nokia asha 501
Pingback: capas nokia asha 501
Pingback: capa huawei ascend g6
Pingback: capa huawei ascend g6
Pingback: bateria samsung galaxy ace
Pingback: +j7 2017 +peliculas
Pingback: capas sony xperia u
Pingback: bateria para s3 mini
Pingback: capa alcatel pop c7
Pingback: +capas +xiaomi note 4 mediatek
Pingback: little kids TV weather forecast
Pingback: capas sony xperia e
Pingback: +pelicula zenfone 4 ze554kl
Pingback: capa para sony xperia e4
Pingback: pau para tirar selfies
Pingback: capas sony xperia e1
Pingback: capas sony xperia e
Pingback: extensor para selfies
Pingback: +Alcatel +Idol 5S +peliculas
Pingback: +capa +wiko +lenny 4
Pingback: capas huawei ascend g510
Pingback: capa para sony xperia e4
Pingback: +capa +wiko +lenny 4
Pingback: +baterias +iPhone +5C
Pingback: +peliculas +zenfone +4 max
Pingback: drone learns imitating cars and bikes
Pingback: nasa drone mate for mars rover mission
Pingback: +capas +lenny 4
Pingback: capas sony xperia e
Pingback: satellite-beach-car-title-loans
Pingback: Erectile Dysfunction Treatment
Pingback: sitemap
Pingback: +asus +zenfone +4max +pelicula
Pingback: hollywood-car-title-loans
Pingback: sunrise-car-title-loans
Pingback: capas huawei ascend g7
Pingback: think and grow rich summary
Pingback: +peliculas asus 4 ze554kl
Pingback: +zenfone +4 max +peliculas
Pingback: +peliculas asus 4 ze554kl
Pingback: capas telemoveis huawei
Pingback: +peliculas +asus +zenfone +4max
Pingback: capas para telemovel huawei
Pingback: davie-car-title-loans
Pingback: FPV apricot blossoms in mountains
Pingback: capas para telemovel huawei
Pingback: capas alcatel one touch
Pingback: +peliculas zenfone 4 ze554kl
Pingback: make an outdoor blackboard
Pingback: homemade arduino parking assistant
Pingback: capas huawei ascend g6 4g
Pingback: massachusetts-car-title-loans
Pingback: +capa +LG Nexus +5X
Pingback: imagination money
Pingback: make an indoor and outdoor concrete light
Pingback: peliculas samsung j5 2016
Pingback: capas telemoveis huawei
Pingback: car-title-loan
Pingback: see the passage of time
Pingback: dade-county-car-title-loans
Pingback: california-car-title-loans
Pingback: boss pays all staff's vacation
Pingback: georgia-car-title-loans
Pingback: west-palm-beach-car-title-loans
Pingback: tickling on your butt
Pingback: arizona-car-title-loans
Pingback: [capas para samsung j5 2017]
Pingback: capas para samsung +s4 mini
Pingback: capa lg l fino
Pingback: +bateria +galaxy j7 2016
Pingback: best-credit-repair-company
Pingback: capas huawei ascend y530
Pingback: capas sony xperia t3
Pingback: +capas para samsung galaxy +j5 2017
Pingback: capas sony xperia t3
Pingback: +capa +Galaxy +J3 2017
Pingback: capas sony e4
Pingback: [capas samsung9]
Pingback: florida-credit-repair-companies
Pingback: bolsas LG C70
Pingback: +capas +samsung +j5 2017
Pingback: [capas samsung s4]
Pingback: +capa +Galaxy +J3 2017
Pingback: broward-county-credit-repair-companies
Pingback: capa samsung galaxy +s4
Pingback: capas sony e4
Pingback: capa Samsung Galaxy +A5
Pingback: capa lg l fino
Pingback: dade-county-credit-repair-companies
Pingback: palm-beach-county-credit-repair-companies
Pingback: +capas para samsung +j3 2017
Pingback: capas huawei ascend g630
Pingback: Watch on YouTube
Pingback: +capas +samsung +j5 2017
Pingback: Pel?cula para +meizu
Pingback: [capas iphone 5 se]
Pingback: peliculas htc
Pingback: peliculas htc
Pingback: +pelicula +huawei +y6 pro 2017
Pingback: [capas de iphone 8]
Pingback: +capas +redmi +note 5a +prime
Pingback: peliculas htc
Pingback: capas vodafone smart 4 turbo
Pingback: capas lg zero
Pingback: [pelicula vidro temperado huawei p8 lite]
Pingback: capas para vodafone smart 4
Pingback: +capas +redmi +note 5a +prime
Pingback: +capas +redmi +note 5a
Pingback: capas lg zero
Pingback: +capas +redmi +note 5a
Pingback: +xiaomi +redmi +note 5a +prime +capas
Pingback: +redmi +note 5a +capa
Pingback: [capa iphone 8 plus]
Pingback: capa lg g2 mini
Pingback: capas lg zero
Pingback: [pelicula vidro temperado huawei p8 lite]
Pingback: +xiaomi +redmi +note 5a +prime +capas
Pingback: [capas de iphone 8]
Pingback: [capas de iphone 8]
Pingback: +Huawei +Mate 10 Lite +peliculas
Pingback: capa lg g2 mini
Pingback: best pocket pussy
Pingback: +pelicula +huawei +y6 pro 2017
Pingback: +samsung j5 2017 +peliculas
Pingback: peliculas htc
Pingback: capas para vodafone smart 4
Pingback: +galaxy j7 2016 +bateria
Pingback: capa lg g2
Pingback: capa para huawei p9
Pingback: [capas lg g4]
Pingback: [capa samsung j5 2017]
Pingback: bateria samsung s2
Pingback: pelicula para nokia lumia
Pingback: +capas +samsung 9]
Pingback: bumper case iphone 4
Pingback: Dagadam watch
Pingback: +bateria +samsung j7 2016
Pingback: Dagadam watch
Pingback: +capas +samsung 9]
Pingback: peliculas sony xperia j
Pingback: capa lg l65
Pingback: peliculas sony xperia j
Pingback: capa lg l65
Pingback: capa para huawei p9
Pingback: capa lg g2
Pingback: capas huawei g750
Pingback: bateria samsung galaxy Note
Pingback: [capas para huawei p9]
Pingback: [pelicula de vidro lumia 535]
Pingback: [pelicula de vidro lumia 535]
Pingback: top sex toys
Pingback: +bateria +j7 2016
Pingback: Smartwatch
Pingback: [pelicula de vidro lumia 535]
Pingback: Smartwatch
Pingback: [capas de telemoveis huawei p8 lite]
Pingback: [capas de telemoveis huawei p8 lite]
Pingback: [huawei y3 capas]
Pingback: [capas telemoveis motorola]
Pingback: [capas de telemovel]
Pingback: [capas telemoveis motorola]
Pingback: capa alcatel one touch
Pingback: +nokia 3 +peliculas
Pingback: [capas iphone 5]
Pingback: capa alcatel 4 plus
Pingback: [capa samsung j5]
Pingback: capas samsung galaxy s4
Pingback: iphone 4s capas
Pingback: capas vodafone smart 4
Pingback: capas vodafone smart 4
Pingback: comprar capas de telemovel
Pingback: iphone 4s capas
Pingback: best prostate massage
Pingback: thrusting jack rabbit
Pingback: Naija
Pingback: staffordshire bull terrier weight male 1117 kg
Pingback: capas blackberry z30
Pingback: [acessorios para telemoveis]
Pingback: [capas de telemoveis huawei p8 lite]
Pingback: capas para samsung s4 mini
Pingback: pictures of australian shepherds
Pingback: Smartest Dog Breeds
Pingback: afghan dogs pictures
Pingback: capa alcatel 4 plus
Pingback: images of french bulldogs
Pingback: [capas para huawei p8 lite]
Pingback: capas para samsung
Pingback: boxer images
Pingback: capas blackberry
Pingback: images of afghan hound
Pingback: labrador dog brown colour images
Pingback: rottweiler description
Pingback: [capas telemoveis motorola]
Pingback: capas para samsung s4 mini
Pingback: pics of french bulldogs
Pingback: capas samsung galaxy s4
Pingback: [capas para huawei p8 lite]
Pingback: pictures of pug
Pingback: doberman description
Pingback: image rottweiler
Pingback: ardell terrier
Pingback: rottweiler temperament fearless
Pingback: [capas para huawei p8 lite]
Pingback: brussels griffon history
Pingback: capas para samsung fresh
Pingback: A new puppy became a house nightmare: Puppy Training
Pingback: capas blackberry
Pingback: pics of corgi dogs
Pingback: [capas de telemoveis huawei p8 lite]
Pingback: capa huawei gr3
Pingback: Estate Agents Welwyn Garden City
Pingback: [capas samsung j5]
Pingback: in?aat sonras? temizli?i
Pingback: capa power bank iphone 6s
Pingback: [capa huawei p smart]
Pingback: in?aat sonras? temizlikci
Pingback: g?ndelik?i temizlikci
Pingback: dual sim
Pingback: +capa +mate 10
Pingback: yang?n temizli?i
Pingback: +capas +huawei mate 10
Pingback: +peliculas +samsung +j3 2017
Pingback: g?ndelik?i temizlik
Pingback: Alpha
Pingback: +capa +huawei mate 10
Pingback: capa Samsung Galaxy Tab
Pingback: +capas +huawei mate 10
Pingback: capa Samsung Galaxy Trend 2 Lite
Pingback: yang?n temizlikci
Pingback: +huawei mate 10 +capa
Pingback: +capa power bank +iphone 7 plus
Pingback: su bask?n? temizlik
Pingback: Vodafone
Pingback: melamine dinnerware
Pingback: in?aat sonras? temizlik
Pingback: melamine dinnerware
Pingback: melamine dinnerware
Pingback: ofis temizli?i
Pingback: melamine dinnerware
Pingback: in?aat sonras? temizlikci
Pingback: +pelicula +Galaxy +J3 2017
Pingback: in?aat sonras? temizlik
Pingback: [capa huawei p smart]
Pingback: in?aat sonras? temizlik
Pingback: in?aat sonras? temizlik
Pingback: thrusting sex toys for women
Pingback: capa samsung galaxy note 3
Pingback: capas htc one
Pingback: malamine tableware
Pingback: in?aat sonras? temizlik
Pingback: melamine picnic plates
Pingback: HTC
Pingback: +pelicula +Galaxy +J3 2017
Pingback: samsung galaxy 5 pre?o
Pingback: melamine dinnerware
Pingback: melamine picnic plates
Pingback: samsunga galaxy s 3
Pingback: capas telem?veis
Pingback: in?aat sonras? temizlik
Pingback: Samsung Galaxy Trend
Pingback: Letting Agents Welwyn Garden City
Pingback: ?irketi temizlik
Pingback: Fuel Software Done Right
Pingback: Fuel Safety for the 21st century
Pingback: in?aat sonras? temizlik
Pingback: Letting Agents Welwyn
Pingback: Fuel Software for Anyone
Pingback: Bateria Original Samsung
Pingback: Huawei Ascend Y300
Pingback: firmas? temizlik
Pingback: Estate Agents Welwyn Garden City
Pingback: Letting Agents Welwyn Garden City
Pingback: Estate Agents Hertfordshire
Pingback: 515 dual sim
Pingback: Letting Agents Welwyn Garden City
Pingback: Letting Agents Welwyn
Pingback: telemovel dual sim
Pingback: Letting Agents Welwyn
Pingback: samsung galaxy s2 pre?o
Pingback: samsung galaxy s2 pre?o
Pingback: telemovel dual sim
Pingback: Capa Galaxy Ace
Pingback: yang?n temizlik
Pingback: Estate Agents Welwyn
Pingback: Letting Agents Welwyn
Pingback: Estate Agents Hertfordshire
Pingback: Estate Agents Welwyn
Pingback: Fuel Software Done Right
Pingback: Estate Agents AL8
Pingback: Bateria Original Samsung
Pingback: BlackBerry Z10
Pingback: Estate Agents Hertfordshire
Pingback: Nokia Lumia 610
Pingback: samsung galaxy 5 pre?o
Pingback: Letting Agents Welwyn
Pingback: Fuel Software Done Right
Pingback: Letting Agents Welwyn
Pingback: alcatel ot pop c7
Pingback: Estate Agents AL8
Pingback: Onde comprar capas para telem?veis
Pingback: Fuel Safety for the 21st century
Pingback: Estate Agents AL8
Pingback: asha 500 dual sim
Pingback: Estate Agents AL8
Pingback: in?aat sonras? temizlik
Pingback: Alcatel One Touch Idol 2
Pingback: app games
Pingback: Loja de Acess?rios para telem?veis
Pingback: mobile games
Pingback: mobile games
Pingback: Galaxy Grand 2
Pingback: Estate Agents Hertfordshire
Pingback: Capa em Gel para Samsung Galaxy Core Plus
Pingback: app marketing
Pingback: Estate Agents Hertfordshire
Pingback: Estate Agents Welwyn Garden City
Pingback: Vodafone Smart 4
Pingback: gaming
Pingback: Loja de Acess?rios para telem?veis
Pingback: Estate Agents Welwyn
Pingback: Estate Agents Welwyn Garden City
Pingback: gamers
Pingback: Huawei Ascend G6
Pingback: Estate Agents Hertfordshire
Pingback: Letting Agents Welwyn Garden City
Pingback: Bolsa para Samsung Galaxy Star
Pingback: Alcatel One Touch Idol 2
Pingback: Estate Agents Welwyn Garden City
Pingback: Nokia Lumia 735
Pingback: Bolsa para Samsung Galaxy Star
Pingback: Letting Agents Welwyn
Pingback: Capa em pele para Samsung Galaxy S3 Mini
Pingback: Estate Agents Welwyn Garden City
Pingback: Estate Agents AL8
Pingback: wall stickers
Pingback: Peliculas de prote?ao de ecr? para Samsung Galaxy Core Plus
Pingback: Letting Agents Welwyn
Pingback: wall decoration
Pingback: peliculas sony xperia miro
Pingback: wall decor
Pingback: Estate Agents Welwyn
Pingback: wall stickers
Pingback: wall stickers
Pingback: +capa +xiaomi +note 5a
Pingback: bateria samsung galaxy s2
Pingback: [capas para nokia lumia 625]
Pingback: [capa sony xperia m4 aqua]
Pingback: Letting Agents Welwyn
Pingback: Estate Agents Welwyn
Pingback: Estate Agents Hertfordshire
Pingback: +xiaomi +redmi +note 5a +capas
Pingback: [capa para nokia lumia 625]
Pingback: +note 4 mediatek +capa
Pingback: Letting Agents Welwyn Garden City
Pingback: wall stickers
Pingback: +capa +xiaomi +note 5a
Pingback: super head honcho
Pingback: capas nokia lumia +925
Pingback: wall stickers
Pingback: [capas para lumia 640]
Pingback: wall decoration
Pingback: Estate Agents Welwyn
Pingback: wall stickers
Pingback: bateria samsung galaxy s2
Pingback: Tech Support Leads Vendor In Noida
Pingback: capas nokia lumia +925
Pingback: Estate Agents Hertfordshire
Pingback: Estate Agents Welwyn
Pingback: Estate Agents AL8
Pingback: Estate Agents Welwyn
Pingback: Estate Agents Welwyn
Pingback: Letting Agents Welwyn Garden City
Pingback: +capa +xiaomi +note 5a +prime
Pingback: Hookah delivery
Pingback: +xiaomi redmi note 4 mediatek +capas
Pingback: Letting Agents Welwyn
Pingback: Estate Agents AL8
Pingback: Hookah delivery
Pingback: capas para telemoveis huawei ascend y530
Pingback: +xiaomi redmi note 4 mediatek +capa
Pingback: peliculas sony xperia u
Pingback: Satta King
Pingback: small vibrating anal plug
Pingback: Estate Agents Hertfordshire
Pingback: how to sell my home
Pingback: inюaat sonrasэ temizlikci
Pingback: temizlik kadэn
Pingback: protective clothing
Pingback: how to sell my home
Pingback: pink platinum girls wool blend hooded plaid lined winter dress pea coat jacket
Pingback: austin ink apparel unisex mens city of new orleans louisiana 3 4 sleeve white baseball t shirt
Pingback: members only mens original iconic racer jacket
Pingback: roxy big girls backyard snow pant
Pingback: columbia boys tree time puffer jacket
Pingback: Fuel Safety
Pingback: sunday rose sundayrose womens lightweight quilted jacket full zip padded coat with zipper pockets
Pingback: Fuel Software
Pingback: sweet kids girls faux fur cape with satin tie
Pingback: lilax little girls faux fur vest
Pingback: su baskэnэ temizliрi
Pingback: columbia girls katelyn crest jacket
Pingback: gьndelikзi temizlik
Pingback: inюaat sonrasэ temizlikci
Pingback: joules boys cosy snowsuit
Pingback: nautica boys helm bubble with storm cuffs
Pingback: inюaat sonrasэ temizliрi
Pingback: oscar boys sherba lined buffalo fleece jacket
Pingback: ev temizlik
Pingback: kenneth cole new york mens modern fit 2 button side vent solid suit
Pingback: isobella chloe big girls fuchsia front zipper ruffles hood coat 7 12
Pingback: kasper womens petite size short sleeve two button seamed dress
Pingback: nautica boys water resistant expedition parka with faux fur
Pingback: 32 degrees girls outerwear jacket more styles available
Pingback: london fog girls lightweight polka dot trench coat
Pingback: tahari asl plus size herringbone skirt suit malibu pink
Pingback: kingsize mens tall pique polo shirt
Pingback: hotouch men casual round neck tropical print sleeveless tank tops
Pingback: doubleal girls buffalo cotton plaid quilted vest cute puff lined gilet
Pingback: milwaukee leather big mens distressed brown motorcycle jacket vents
Pingback: amazon essentials girls full zip polar fleece jacket
Pingback: lp facon mens vintage biker style motorcycle cafe racer distressed leather jacket
Pingback: adidas boys athletics jacket
Pingback: leg avenue womens plus size stretch lace open crotch thong
Pingback: fruit of the loom mens pocket crew neck t shirt pack of 4
Pingback: columbia womens kruser ridgetm softshell jacket
Pingback: mens vintage stand collar faux leather jacket
Pingback: diesel mens l mackson jacket jackets
Pingback: coolhides mens motorcycle super hero s logo red leather jacket
Pingback: port authority ladies value fleece vest
Pingback: sumtory womens solid deep v neck bandage hollow out sexy long sleeve bodysuits catsuit
Pingback: haggar mens premium no iron classic fit expandable waist pleat front pant
Pingback: ellie hebe womens round neck zipper long sleeve bodysuit stretchy leotard top
Pingback: tobeinstyle womens zip up sleeveless polar fleece vest
Pingback: lee mens big tall custom fit carpenter jean
Pingback: enlishop womens winter warm plus size waistcoat long faux fur vest jacket
Pingback: dickies mens multi pack dri tech moisture control crew socks
Pingback: weatherproof womens courtney burnout hooded pullover blend fleece w1162
Pingback: jinidu mens holiday slim fit solid blazer jackets suit separate jacket
Pingback: lamarque mens tate bomber jacket
Pingback: am clothes womens plus size padded wirefree sleep bra multi pack
Pingback: coofandy mens leather bomber jacket stripe varsity baseball jacket
Pingback: caing women large plus size baggy linen overalls casual wide leg pants sleeveless rompers jump suit vintage haren pants
Pingback: eberjey womens colette chemise
Pingback: cloudstyle mens plaid modern fit 3 piece suit blazer jacket tux vest trousers
Pingback: zexxxy women print nightshirt boyfriend pajama top long sleeve sleep dress
Pingback: black out boys zip front vegan leather updated moto with quilted design sleeve details
Pingback: sportides mens waistcoat gilet business gentleman vest suits blazer jza005
Pingback: carhartt womens stockbridge sherpa lined vest
Pingback: luyan womens wedding bridal faux fur fluffy edge shrug
Pingback: womens lace jacket casual floral lace patchwork lightweight short bomber jacket slim fit zipper coat
Pingback: beyove women lightweight hooded raincoat slim fit casual waterproof jacket w pocket
Pingback: kirkland signature ladies active jacket
Pingback: anne klein womens quilted jacket with belt
Pingback: hudson jeans womens riley crop easy slim boyfriend 5 pocket jeans
Pingback: bgsd womens alexa classic hooded long trench coat
Pingback: new balance womens hombre windcheater jacket
Pingback: exofficio flyq jacket
Pingback: http:/www.every-cloud.co.uk/
Pingback: levis womens ex boyfriend trucker
Pingback: bifast womens solid long sleeve open front slim fit casual blazer jacket
Pingback: ililily woman cotton slim fit sweatshirt oblique zipper hoodie rider jacket coat
Pingback: gьndelikзi temizliрi
Pingback: zeagoo women long sleeve baggy loose fit pockets casual maxi long dress
Pingback: Fuel Software Support
Pingback: Microsoft recruitment
Pingback: Every cloud recruitment
Pingback: shape activewear womens fashion glamper wind jacket
Pingback: Every cloud dynamics
Pingback: columbia womens tested tough in pink rain jacket ii
Pingback: london fog womens zip front quilt with hood
Pingback: columbia womens evaporation trench
Pingback: vince camuto womens lightweight quilted jacket with belt
Pingback: zero restriction womens hooded olivia rain jacket
Pingback: Microsoft dynamics jobs
Pingback: zennessa womens zip up military anorak drawstring jacket w pockets
Pingback: columbia womens plus size arcadia ii jacket
Pingback: Every Cloud
Pingback: acevog womens zip up military anorak jacket coat with pockets
Pingback: celebrity pink juniors skirted coat
Pingback: Microsoft dynamics jobs
Pingback: vfemage womens elegant vintage wear to work business bodycon sheath dress
Pingback: sakkas womens shiny metallic liquid high waist pencil skirt
Pingback: codefit yoga gym power flex dry fit high compression pants workout womens leggings
Pingback: Fuel Software
Pingback: Microsoft dynamics jobs
Pingback: maaji womens dazzling mid rise long legging
Pingback: spiewak womens wool blend fishtail hooded parka with detachable fur trim
Pingback: eddie bauer womens microtherm stormdown jacket
Pingback: tahari by arthur s levine womens crepe pant suit with contrast piping
Pingback: Microsoft dynamics developers
Pingback: cloud recruitment
Pingback: su baskэnэ temizliрi
Pingback: littleforbig short overalls shortalls babydoll overalls
Pingback: patagonia down sweater
Pingback: tahari asl womens petite faille skirt suit with beading
Pingback: yangэn temizlik
Pingback: calvin klein womens lux solid pencil skirt
Pingback: coorun womens waterproof outdoor windbreaker jacket super quick dry sports coat black
Pingback: UST Inspection
Pingback: beautytalk womens winter outdoor classic wool blended trench coat jacket
Pingback: lark ro womens sleeveless fit and flare dress 2
Pingback: gold toe
Pingback: romwe womens classic collar long sleeve curved hem pullover sweatshirt
Pingback: biadani women classic open front lightweight soft drape cardigan s 3x
Pingback: floria women button down crew neck long sleeve soft knit cardigan sweater s 3x
Pingback: Microsoft dynamics professionals
Pingback: charles river apparel womens front pocket classic pullover
Pingback: erosebridal new sleeveless lace chiffon wedding dress bridal gown
Pingback: pebble
Pingback: beachcoco womens sweetheart maxi dress
Pingback: jeans amazon mens fashion dresses
Pingback: cherry cat womens v neck cut loose bathing suit swimsuit cover ups beach dress us 6 14
Pingback: kut from the kloth
Pingback: assasins creed iii
Pingback: rekucci womens ease into comfort stretchable pull on 5 slimming tab short
Pingback: Fuel Inspections
Pingback: hot leathers
Pingback: travel
Pingback: longming womens fashion big v neck pullover loose sexy batwing sleeve wool cashmere sweater winter tops
Pingback: ixtreme
Pingback: miyang womens tankini striped vintage swim dress
Pingback: management
Pingback: lspace womens swimwear
Pingback: niczoe
Pingback: volcom
Pingback: gold toe moretz mens
Pingback: william rast mens outerwear
Pingback: wigwam mens socks
Pingback: Polos amazon fashion dresses mens clothing
Pingback: guess mens apparel
Pingback: pink platinum
Pingback: Fuel Software
Pingback: child rearing
Pingback: ibsen
Pingback: training
Pingback: UST Inspection
Pingback: slots
Pingback: teach your children well
Pingback: Fuel Dispenser Inspection
Pingback: slot
Pingback: vampire
Pingback: travel
Pingback: Housecleaning Dallas
Pingback: non-fiction
Pingback: amazing selling machine
Pingback: psychology
Pingback: gynt
Pingback: inspiration
Pingback: Hair Transplant Blog
Pingback: Turkey Hair Transplant
Pingback: Hair Transplant in Istanbul
Pingback: Trasplante Capilar Turquía
Pingback: Hair Transplant Blog
Pingback: Turkey Hair Transplant Cost
Pingback: Hair Transplant Clinic
Pingback: religion
Pingback: slot
Pingback: science
Pingback: Hair Transplant in Istanbul
Pingback: buy android installs
Pingback: How to Receive Pocket WiFi / Data SIM Card at Hakata Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Arakawa Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Kyoto Central Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Shinagawa Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Hongo Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Osaka North Post Office
Pingback: Pocket WiFi SIM Card Rental Service Japan LightPocket
Pingback: Japan Pocket Wifi and SIM Card Rental Service
Pingback: How to Receive Pocket WiFi / Data SIM Card at Fukuoka Central Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Sapporo Central Post Office
Pingback: Useful Japanese Post Office List - To Receive Your Packages at The Japan Post Office Nearest to Your Accommodation
Pingback: Japan Unlimited Data SIM Card Rental
Pingback: How to Receive Pocket WiFi / Data SIM Card at Chiba Central Post Office
Pingback: How to Receive Pocket WiFi / Data SIM Card at Meguro Post Office
Pingback: Are Free WiFi Spots in Japan Really Useful? Part 2: Security Problem
Pingback: Useful Knowledge to Use Internet in Japan: 5 Networks of Pocket WiFi / Prepaid SIM Card
Pingback: Narita Airport Pocket WiFi Rental Comparing
Pingback: All Japan Travelers Must Check: Sending & Receiving Packages Will Dramatically Be Easy
Pingback: How to Receive Pocket WiFi / Data SIM Card at Haneda Airport Post Office
Pingback: Japan Travel Tips: Luggage Transfer Storage Service List
Pingback: Can I Still Get Connected with Japan Prepaid SIM/Pocket WiFi? / Case 3: Itsukushima (Miyajima)
Pingback: Useful Websites to Get Around Japan: Guide Websites Part.2 LightPocket Blog
Pingback: One Major Problem at Airbnb in Japan: Failure to Receive Your Luggage: Part 1
Pingback: Prepaid SIM or Pocket WiFi? Try Easy Checker for Your Best Internet Connection in Your Japan Travel
Pingback: The Best Internet Contract for Staying in Japan for More Than 30 Days But Less Than 2 Years
Pingback: How to Receive Pocket WiFi / Data SIM Card at New Chitose Airport Post Office
Pingback: sell my house fast
Pingback: sell house fast
Pingback: sell my house fast
Pingback: sell house as is for cash
Pingback: sell my house fast
Pingback: sell house as is for cash
Pingback: sell my house fast
Pingback: sell house fast san antonio
Pingback: sell house as is for cash
Pingback: sell house as is for cash
Pingback: sell my house fast
Pingback: sell house fast
Pingback: sell house fast
Pingback: sell house as is for cash
Pingback: arcade tycoon
Pingback: sell house fast
Pingback: sell my house fast
Pingback: sell house fast
Pingback: sell house fast
Pingback: buen orador
Pingback: sell house fast
Pingback: bilingue orador publico mexicanos
Pingback: best Career Coaching
Pingback: public speaker espanol
Pingback: keynote presenter
Pingback: mexican motivational speakers
Pingback: diamond jewellery online
Pingback: online diamond jewellery in india
Pingback: ftec
Pingback: sell house as is for cash
Pingback: sell my house fast
Pingback: bilingual Public Speaker
Pingback: sciencetelling
Pingback: best Spanish keynote speaker
Pingback: latino public speaker
Pingback: sell house fast san antonio
Pingback: orador principal latina
Pingback: bilingue orador publico famoso
Pingback: orador publico famoso
Pingback: sell house fast san antonio
Pingback: Spanish public speaker
Pingback: best public speaker
Pingback: sell my house fast
Pingback: sell house fast
Pingback: bilingue orador publico dominicana
Pingback: buy online diamond jewellery
Pingback: sell my house fast
Pingback: sell house as is for cash
Pingback: orador motivacional dominicana
Pingback: online diamond jewellery in india
Pingback: tanishq diamond jewellery online
Pingback: sell house as is for cash
Pingback: Homepage
Pingback: Video porno
Pingback: best Spanish keynote speaker
Pingback: nakshatra diamond jewellery online shopping
Pingback: Click Here
Pingback: buy diamond jewellery online
Pingback: steel drum for sale
Pingback: tank drum for sale
Pingback: orador principal latino
Pingback: orador profesionales
Pingback: diamond jewellery online
Pingback: steel tongue drum sale
Pingback: diamond jewellery online
Pingback: Read More
Pingback: boost confidence
Pingback: latina motivational speakers
Pingback: bilingue orador motivacional significo
Pingback: tongue drum
Pingback: orador principal famoso
Pingback: corporate presenter
Pingback: orador principal ny
Pingback: Redtube
Pingback: orador publico latina
Pingback: steel tongue drum sale
Pingback: argentinian motivational speakers
Pingback: best spanish speaking public speaker
Pingback: orador motivacional famoso
Pingback: handpan
Pingback: Redtube
Pingback: bilingue orador motivacional latino
Pingback: Free porn
Pingback: Success Coach
Pingback: double function scaler
Pingback: Fishing Books
Pingback: Fishing Books
Pingback: handpan
Pingback: apex locator with gyroscope
Pingback: Fishing Camping Cups
Pingback: big dick
Pingback: biggest dildo in the world
Pingback: steel tongue drum
Pingback: Fly Fishing Flies
Pingback: steel drums for sale
Pingback: dental induction micromotor
Pingback: what vibrator to buy
Pingback: dental loupe
Pingback: tank drum
Pingback: scaling tips satelec
Pingback: dental loupe
Pingback: Fly Fishing Line
Pingback: steel drum for sale
Pingback: Fishing Clothing
Pingback: curing light aladyn
Pingback: steel drums for sale
Pingback: Study MBBS in Georgia
Pingback: Condoms
Pingback: Buy adult sex toys
Pingback: steel drum for sale
Pingback: Dynatech Industrial
Pingback: Buy adult sex toys
Pingback: handpan
Pingback: Fishing Charts and Maps
Pingback: steel drum for sale
Pingback: scaling tips ems
Pingback: tongue drum
Pingback: original gift
Pingback: led wireless scaler
Pingback: Fishing Bait Storage
Pingback: prophylaxys unit
Pingback: Fishing Knives
Pingback: Fishing Line Spooling Accessories
Pingback: KPI's of ERP Software Small Business
Pingback: Fishing Bait Bands
Pingback: Fishing Glasses
Pingback: erp comparison
Pingback: Fishing Chair Bags
Pingback: Fishing Line
Pingback: apex locator with gyroscope
Pingback: Leather Jackets
Pingback: Leather Jackets
Pingback: wireless intraoral camera
Pingback: Leather Jackets
Pingback: Leather Jackets
Pingback: Benefits of ERP Software
Pingback: ps3 skins
Pingback: Fishing Nets
Pingback: Leather Jackets
Pingback: Fishing Marker Buoys
Pingback: jackets for men amazon
Pingback: wmi provider host
Pingback: 3ds emulators
Pingback: wmi provider host
Pingback: tutuapp vip
Pingback: tutuapp vip
Pingback: tutuapp apk
Pingback: wmi provider host
Pingback: wmi provider host
Pingback: wmi provider host
Pingback: tutuapp vip
Pingback: Fishing Tent Accessories
Pingback: Fishing Rucksacks
Pingback: tutuapp apk
Pingback: Fishing Tents
Pingback: Quality Fishing Downriggers
Pingback: Quality Coarse Fishing Books
Pingback: Quality Fishing Clothing General
Pingback: Quality Fishing Jackets
Pingback: Quality Fishing Mugs
Pingback: Quality Fishing Camping Cups
Pingback: Quality Fishing Waders
Pingback: Quality Fishing Tackle
Pingback: Quality Fly Fishing Books
Pingback: Quality Fly Fishing Reels
Pingback: Quality Fishing Accessories
Pingback: Quality Sea Fishing Books
Pingback: Quality Fishing Bedchairs
Pingback: Quality Fishing Umbrellas
Pingback: medical marijuana certification ann arbor
Pingback: wmi provider host
Pingback: tutuapp vip
Pingback: tutuapp apk
Pingback: Quality Fishing Gaffs
Pingback: Quality Fishing Accessories
Pingback: Quality Fishing Tackle Boxes
Pingback: wmi provider host
Pingback: tutuapp vip
Pingback: tutuapp apk
Pingback: tutuapp apk
Pingback: 3ds emulators
Pingback: tutuapp vip
Pingback: More hints
Pingback: tutuapp vip
Pingback: this review
Pingback: Custom Lexus Dash Panels
Pingback: BMW steering wheel repair
Pingback: Quality Fishing Hook Sharpeners
Pingback: found this site
Pingback: Steering Wheel Repair
Pingback: article source
Pingback: check out this site
Pingback: 3ds emulators
Pingback: 3ds emulators
Pingback: Quality Fishing Reel Care Accessories
Pingback: this review
Pingback: medical marijuana certification ann arbor
Pingback: medical marijuana certification ann arbor
Pingback: medical marijuana certification ann arbor
Pingback: Visit This Link
Pingback: Quality Fishing Rod Racks
Pingback: click here
Pingback: terrarium tv app
Pingback: iTube Pro
Pingback: terrarium tv apK
Pingback: Discover More
Pingback: Continue Reading
Pingback: iTube Pro
Pingback: Additional Info
Pingback: Mercedes Steering Wheel repair
Pingback: terrarium tv apK
Pingback: Discover More
Pingback: terrarium tv apK
Pingback: iTube Pro APK
Pingback: in this site
Pingback: terrarium tv apK
Pingback: Discover More
Pingback: iTube Pro APK
Pingback: Going Here
Pingback: Custom Steering Wheel
Pingback: Asian Beauty Oldham
Pingback: Framaroot
Pingback: how to remove your steering wheel
Pingback: Framaroot
Pingback: Custom Steering Wheel
Pingback: site
Pingback: see more
Pingback: iTube Pro
Pingback: Related Site
Pingback: Web Design company columbus ohio
Pingback: Read Full Article
Pingback: Related Site
Pingback: custom solutions llc design
Pingback: next page
Pingback: Quality Fishing Tackle Wraps
Pingback: Quality Fishing Storage Trays
Pingback: Wedding Car Hire Nottingham
Pingback: UK Fly Fishing
Pingback: this site
Pingback: Clicking Here
Pingback: Go Here
Pingback: Visit Website
Pingback: Discover More Here
Pingback: Recommended Reading
Pingback: video chat per incontri
Pingback: video chat libera
Pingback: Clicking Here
Pingback: UK Fishing Travel Guide Books
Pingback: Our site
Pingback: More hints
Pingback: Our site
Pingback: Limo Hire Leicester
Pingback: get vpn
Pingback: UK Fishing Books
Pingback: Find Doctor jobs in UK
Pingback: fitnet vpn
Pingback: chat online senza registrazione
Pingback: webchat freee
Pingback: vpn
Pingback: vpn
Pingback: top 3 qualities successful of sales professionals
Pingback: design columbus
Pingback: UK Fly Fishing Rods
Pingback: 5 search marketing tips for bing ads
Pingback: the science of productivity
Pingback: leverage creates wealth
Pingback: how to get more search traffic
Pingback: whats the difference difference consultative selling normal selling
Pingback: how to think and grow rich
Pingback: website development services
Pingback: UK Fishing Gloves
Pingback: using the law of reciprocation and other persuasion techniques correctly
Pingback: videochat
Pingback: get vpn
Pingback: webcam chat
Pingback: chat per ragazzi
Pingback: fitnet vpn
Pingback: seo
Pingback: seo services
Pingback: cash
Pingback: vpn
Pingback: search engine optimization
Pingback: UK Fishing Safety Gear
Pingback: UK Fishing Bait Making Equipment
Pingback: website redesign columbus ohio
Pingback: 3 sales strategies to increase cashflow
Pingback: fitnet
Pingback: web maintenance columbus
Pingback: iran vpn
Pingback: best seo service
Pingback: fitnet
Pingback: get vpn
Pingback: bulletproof tactic to dominate google search rankings
Pingback: get vpn
Pingback: 5 lessons learnt late
Pingback: get vpn
Pingback: 5 needs that shape consumer behavior
Pingback: the 100 startup chris guillebeau book review
Pingback: 5 tips for increasing your google adwords quality score
Pingback: seo sites
Pingback: vpn
Pingback: how to become a millionaire
Pingback: buy vpn
Pingback: buy vpn
Pingback: get vpn
Pingback: inexpensive seo
Pingback: Fishing Hooks
Pingback: Quality Fly Fishing Rod and Reel Combos
Pingback: ecommerce web design and development columbus
Pingback: how to influence your friends and people around you
Pingback: graphic design services
Pingback: hack your mind and how to avoid procrastination
Pingback: epos system
Pingback: POS printer
Pingback: types of intelligence needed to make money
Pingback: best career advice guidance sundar pichai
Pingback: no mr nice guy
Pingback: POS printer
Pingback: learn anything in half time
Pingback: the 7 bold moves by entrepreneurs of all time
Pingback: 1 simple trick to rank high on google fast
Pingback: digital branding
Pingback: will never wake late reading
Pingback: logo design
Pingback: mobile pos printer
Pingback: epos system
Pingback: Quality Fish Books
Pingback: Samsung enclosure
Pingback: Samsung enclosure
Pingback: mpos tablet enclosure
Pingback: Fishing Waistcoats
Pingback: Fishing Pliers and Tools
Pingback: the power of positive and negative thinking
Pingback: Fishing Rods
Pingback: 5 tools that will help you drive traffic to your website
Pingback: 10 signs you wont be rich
Pingback: the effective ranking factor that google doesnt want you to know about
Pingback: how to be charismatic and attract success
Pingback: UK Fishing Reels
Pingback: search engine
Pingback: pay per click marketing columbus
Pingback: Using Ben Wa Balls
Pingback: UK Humourous Fishing Books
Pingback: marketing columbus ohio
Pingback: columbus website design company
Pingback: Quality Fish and Depth Finders
Pingback: UK Fishing Rod and Reel Combos
Pingback: rabbit wand attachment
Pingback: Realistic Penis Extender
Pingback: Chocolate Fudge
Pingback: trulia
Pingback: Morehouse
Pingback: Cookies & Cream
Pingback: Cookies & Cream
Pingback: suction dong
Pingback: double dildo
Pingback: thuê chung cÆ° celadon
Pingback: Denna Plumber
Pingback: Kristal Kennan
Pingback: Phyliss Brody
Pingback: Shauna Gieseke
Pingback: Teddy Coolbaugh
Pingback: Derrick Amin
Pingback: Simone Ponder
Pingback: Kit Mcnealy
Pingback: Bryant Madruga
Pingback: Iris Eversole
Pingback: Sharlene Gerardo
Pingback: Tommy Hoeppner
Pingback: thuê chung cÆ° celadon
Pingback: Gaylord Paules
Pingback: Sheilah Vanwingerden
Pingback: architectural visualization company
Pingback: Chi Fines
Pingback: Reggie Borgeson
Pingback: Tonita Pajak
Pingback: Donita Arrowsmith
Pingback: Loura Friedrichs
Pingback: Shizue Zeng
Pingback: architectural rendering service
Pingback: Mend The Marriage
Pingback: video production service
Pingback: Vesta Royals
Pingback: Wynona Tindle
Pingback: Shan Midkiff
Pingback: Vera Sheeler
Pingback: Bell Hiatt
Pingback: Kendal Pettengill
Pingback: Kristal Kennan
Pingback: Brook Mccafferty
Pingback: Cecily Shiflett
Pingback: Rosanna Sword
Pingback: Porsche Chica
Pingback: Billy Nylander
Pingback: Nanette Wakefield
Pingback: Pain Relief For Arthritis
Pingback: cheap custom t shirts online
Pingback: t shirt printing business
Pingback: personalized gift items
Pingback: custom t shirt design
Pingback: t shirt screening
Pingback: personalized shirts
Pingback: t shirt design near me
Pingback: tees
Pingback: Boat Show
Pingback: wedding gifts
Pingback: printed shirt design
Pingback: customized shirts
Pingback: customized womens t-shirt
Pingback: tee shirt printing near me
Pingback: custom items
Pingback: t shirt printing website
Pingback: mugs
Pingback: customize your shirt
Pingback: customized tees
Pingback: design my shirt
Pingback: t shirt design website
Pingback: engraved gift ideas
Pingback: personalized keepsakes
Pingback: Trisha Paytas Wikipedia
Pingback: Trisha Paytas Wikia
Pingback: cheap trips to the poconos
Pingback: poconos activities in the summer
Pingback: poconos rental properties
Pingback: poconos timeshare
Pingback: cabins Philadelphia
Pingback: poconos fall vacation
Pingback: pocono mountains what to do
Pingback: things to do in the poconos in january
Pingback: hotels in poconos
Pingback: cabin rentals Philly
Pingback: lodge poconos
Pingback: visit poconos pa summer
Pingback: pocono getaways
Pingback: kid friendly things to do in the poconos
Pingback: poconos stay
Pingback: kid friendly things to do in the poconos
Pingback: Erectile Dysfunction Painless Treatment
Pingback: things to do near mount pocono
Pingback: pocono lodges
Pingback: things to do in bushkill poconos
Pingback: poconos fun resorts
Pingback: rental aspen
Pingback: rental pocono
Pingback: los poconos pa
Pingback: root canal
Pingback: veneers
Pingback: Erectile Dysfunction Causes and Cures
Pingback: Erectile Dysfunction Causes and Cures
Pingback: Erectile Dysfunction Painless Treatment
Pingback: hong kong entertainment news
Pingback: Discover More Here
Pingback: Learn More Here
Pingback: Project
Pingback: algarve properties
Pingback: Discover More
Pingback: drama news
Pingback: china news
Pingback: Read This
Pingback: Discover More
Pingback: Going Here
Pingback: pocono summer weekend getaways
Pingback: Click This Link
Pingback: Learn More Here
Pingback: Read More Here
Pingback: Go Here
Pingback: Read More
Pingback: asian entertainment news
Pingback: movie news
Pingback: Learn More
Pingback: Learn More
Pingback: Discover More
Pingback: Read More Here
Pingback: asian entertainment
Pingback: Click Here
Pingback: Click This Link
Pingback: Discover More Here
Pingback: Learn More Here
Pingback: Project
Pingback: Go Here
Pingback: Learn More
Pingback: Click This Link
Pingback: Read More
Pingback: Learn More Here
Pingback: Discover More
Pingback: mt pocono things to do
Pingback: Read More
Pingback: Go Here
Pingback: Discover More Here
Pingback: Going Here
Pingback: Click This Link
Pingback: Discover More
Pingback: Click This Link
Pingback: things to do in poconos in july
Pingback: poconos museums
Pingback: Read This
Pingback: poconos pa winter activities
Pingback: Click Here
Pingback: vacation spots in poconos pa
Pingback: Clicking Here
Pingback: Read This
Pingback: Discover More
Pingback: Read More Here
Pingback: Opportunity
Pingback: interneta marketings
Pingback: zoo near poconos
Pingback: interneta marketings
Pingback: Unit
Pingback: top things to do in poconos
Pingback: pocono falls
Pingback: things to do in poconos in october
Pingback: things to do in poconos in the fall
Pingback: kid friendly things to do in the poconos
Pingback: poconos activities in june
Pingback: bags
Pingback: Jobs In Hazaribag
Pingback: Management
Pingback: project finance
Pingback: Jobs In Cheruvannur
Pingback: Jobs In Bijnor
Pingback: Jobs In Thoothukudi
Pingback: Jobs In Baramati
Pingback: Jobs In Phulwari
Pingback: Jobs In Ponnur
Pingback: Jobs In Ramanathapuram
Pingback: escrow agent fees
Pingback: Jobs In Kothagudem
Pingback: Jobs In Pondicherry
Pingback: toys
Pingback: fashion
Pingback: Jobs In Ranaghat
Pingback: toys
Pingback: dogs
Pingback: beauty
Pingback: womens
Pingback: Jobs In Gola Range
Pingback: fashion
Pingback: sports
Pingback: clothing
Pingback: Jobs In Baj Baj
Pingback: Jobs In Srikalahasti
Pingback: Metropolitan
Pingback: cheap poconos weekend getaway packages
Pingback: mens
Pingback: consumer
Pingback: womens
Pingback: toys
Pingback: toys
Pingback: womens
Pingback: Jobs In Wani
Pingback: drones
Pingback: romantic pocono getaways
Pingback: sports
Pingback: consumer
Pingback: home
Pingback: drones
Pingback: Jobs In Dallo Pura
Pingback: home
Pingback: fashion
Pingback: Jobs In Kharagpur
Pingback: Jobs In Ozhukarai
Pingback: dogs
Pingback: extensions
Pingback: poconos cottage
Pingback: places to stay near poconos
Pingback: hair
Pingback: drones
Pingback: Jobs In Ongole
Pingback: Jobs In Kandla
Pingback: sports
Pingback: mens
Pingback: Jobs In Manipur
Pingback: toys
Pingback: electronics
Pingback: bags
Pingback: drones
Pingback: clothing
Pingback: fashion
Pingback: Jobs In Shillong
Pingback: dogs
Pingback: pocono getaway packages
Pingback: Jobs In Uttarakhand
Pingback: pa poconos resort
Pingback: Jobs In Sikkim
Pingback: best poconos
Pingback: Jobs In Kairana
Pingback: poconos resort and spa retreat
Pingback: Jobs In Mau
Pingback: poconos skiing cabins
Pingback: Jobs In Ankleshwar
Pingback: Jobs In Silvassa
Pingback: Jobs In Kota
Pingback: poconos with family
Pingback: Jobs In Dod Ballapur
Pingback: Jobs In Katihar
Pingback: best places to go in the poconos
Pingback: Jobs In Kayankulam
Pingback: Jobs In Kollegal
Pingback: Jobs In Alappuzha
Pingback: Jobs In Lonavale
Pingback: Jobs In Dabgram
Pingback: Jobs In Hastsal
Pingback: Jobs In Koch Bihar
Pingback: Jobs In Khopoli
Pingback: Jobs In Gopichettipalaiyam
Pingback: Jobs In Bargarh
Pingback: Jobs In Narasaraopet
Pingback: Jobs In Mamandur
Pingback: Jobs In Dharmasala
Pingback: Jobs In Salem
Pingback: Jobs In Punamalli
Pingback: Jobs In Kannur
Pingback: Jobs In Narwana
Pingback: Jobs In Rampur
Pingback: cabin rentals Philly Pennsylvania
Pingback: Jobs In Sholapur
Pingback: Jobs In Chennai
Pingback: poconos house rental
Pingback: Jobs In Gir
Pingback: Jobs In Shantipur
Pingback: Jobs In Yadgir
Pingback: Jobs In Memari
Pingback: poconos cottage
Pingback: Jobs In Mira Bhayandar
Pingback: map of pocono mountains
Pingback: cottage rentals in pa
Pingback: Jobs In Daosa
Pingback: Jobs In Thiruvananthapuram
Pingback: Jobs In Palasa
Pingback: Jobs In Didwana
Pingback: Jobs In Robertsonpet
Pingback: Jobs In Bhopal
Pingback: Jobs In Karauli
Pingback: Jobs In Wokha
Pingback: pocono cottages
Pingback: pocono vacation home rentals
Pingback: pocono vacation rental
Pingback: Jobs In Pune Cantonment
Pingback: Jobs In Bareilly
Pingback: tarjeta sanitaria europea
Pingback: china deals
Pingback: transmission Repair
Pingback: Amsecrets.net
Pingback: china coupons
Pingback: Fossil watches
Pingback: Jobs In Hosakote
Pingback: tarjeta sanitaria europea
Pingback: Jobs In Guna
Pingback: tarjeta sanitaria europea
Pingback: hot china dealz
Pingback: Jobs In Ulhasnagar
Pingback: Jobs In Markapur
Pingback: china dealz
Pingback: china deals
Pingback: tarjeta sanitaria europea
Pingback: tarjeta sanitaria europea
Pingback: tarjeta sanitaria europea
Pingback: china mydealz
Pingback: best deals
Pingback: tarjeta sanitaria europea
Pingback: Matt Behdjou
Pingback: Fossil watches for men
Pingback: behdjou
Pingback: Luxury watches
Pingback: Matthew Behdjou
Pingback: Gold chain
Pingback: Men's jewelry
Pingback: Andrei Korottchenko
Pingback: next day id badges
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Online Secrets
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Activated charcoal teeth whitening powder
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Vegan friendly tooth polish natural organic
Pingback: Andrei Korottchenko
Pingback: Andrei Korottchenko
Pingback: Vegan friendly tooth polish natural organic
Pingback: recliner reviews
Pingback: Activated charcoal teeth whitening powder
Pingback: gaming recliners
Pingback: Activated charcoal teeth whitening powder
Pingback: recliner slipcovers
Pingback: best gaming recliners
Pingback: drones
Pingback: Uptown Ritz residences
Pingback: amazon training
Pingback: start an amazon business
Pingback: next day id badges
Pingback: premium iptv
Pingback: matthew behdjou
Pingback: boom beach pc
Pingback: mindfulness and stress
Pingback: respond skilfully to life’s ups and downs
Pingback: develop resilience with mindfulness
Pingback: how to meditate
Pingback: mindfulness Copenhagen
Pingback: a six week mindfulness course in Copenhagen
Pingback: stress management
Pingback: mindful coaching
Pingback: a six week mindfulness course in Copenhagen
Pingback: respond skilfully to life’s ups and downs
Pingback: mindfulness Copenhagen
Pingback: silent meditation retreat
Pingback: mindfulness and anxiety
Pingback: how to learn to meditate
Pingback: Porn Star
Pingback: boom beach pc
Pingback: personal training leicester
Pingback: netter cuaderno de anatomia para colorear pdf descargar gratis
Pingback: cirugia schwartz 10 edicion pdf descargar gratis
Pingback: libros de medicina gratis
Pingback: libros de medicina gratis
Pingback: bioquimica de laguna pdf
Pingback: libros de medicina en pdf
Pingback: boron fisiologia pdf
Pingback: netter para colorear español pdf
Pingback: descargar libros de medicina gratis
Pingback: libros de medicina pdf gratis
Pingback: netter cuaderno de anatomia para colorear pdf descargar
Pingback: libros de medicina pdf
Pingback: saladin anatomia y fisiologia pdf
Pingback: farmacos para el corazon opie pdf
Pingback: kvarts
Pingback: kivitasot virosta
Pingback: graniidist tooted
Pingback: nls diagnostik
Pingback: töötasapinna paigaldus
Pingback: kvartsist köögitasapinnad
Pingback: microbiologia y parasitologia humana 3ra edicion pdf
Pingback: Metavital
Pingback: OBERON 4021
Pingback: Nagpuri Song
Pingback: Reittherapie
Pingback: laser hair removal near mckinney
Pingback: laser hair removal near plano
Pingback: tierheilpraktiker
Pingback: bikini line laser hair removal
Pingback: Reitturniere
Pingback: töötasapinnad
Pingback: alt paigaldatavad valamud
Pingback: köögimööbel
Pingback: Naturheilkunde
Pingback: Metavital
Pingback: NLS-Methode
Pingback: kivitasapind
Pingback: Bioresonanz
Pingback: Reittherapie
Pingback: kivist töötasapind hind
Pingback: frisco laser hair removal
Pingback: analyse oberon
Pingback: diagnostik nls
Pingback: vmware quote
Pingback: Metavital Horse
Pingback: best laser hair removal in dallas
Pingback: best laser hair removal in mckinney
Pingback: tierarzt
Pingback: pferd diagnose
Pingback: hp wireless keyboard
Pingback: lenovo b sharp
Pingback: managed services 360
Pingback: cowgirl boots for kids
Pingback: girls western boots
Pingback: mens slip on work boots
Pingback: microsoft 365
Pingback: red cowgirl boots
Pingback: ariat boots women
Pingback: Termite eradicating
Pingback: hunter short rain boots
Pingback: cowgirl boots for kids
Pingback: mens work boots on sale
Pingback: girls western boots
Pingback: infant cowboy boots
Pingback: girls western boots
Pingback: justin boots for men
Pingback: Carte Verde
Pingback: Asigurari Moldova
Pingback: Cartea Verde
Pingback: cowgirl boots for kids
Pingback: Asigruari Chisinau
Pingback: redwing work boots
Pingback: cheap cowgirl boots for women
Pingback: Asigurare RCA
Pingback: Nurse practitioner
Pingback: iComfort Mitcham stocks a wide range of Swan mattresses at lowest prices
Pingback: A and H Brokerage Services Inc
Pingback: Cheapest king size mattresses at iComfort Mitcham
Pingback: Oil Change Dallas
Pingback: Cheapest mattresses and beds in Donvale VIC
Pingback: Honda Repair Dallas
Pingback: Carte Verde
Pingback: Asigurare Online
Pingback: Asigruari Chisinau
Pingback: iComfort Mitcham stocks a wide range of BedMaster mattresses at lowest prices
Pingback: Auto Repair Dallas
Pingback: Automobile Service
Pingback: Car Alignment Dallas
Pingback: Asigurare Online
Pingback: Calculator Asigurare Online
Pingback: Repair shop Dallas
Pingback: Cheapest mattresses and beds in Glen Waverley VIC
Pingback: Scam report
Pingback: SleepMaker Kingfisher pocket spring mattress available at iComfort Mitcham
Pingback: Repair shops for cars
Pingback: Best kids ergonomic adjustable desks and chairs available at iComfort Mitcham
Pingback: Quality and Affordable Mattresses in Wantirna Melbourne
Pingback: Car Alignment
Pingback: Oil Change
Pingback: Repair shop Dallas
Pingback: VMS Logistics Corp Broker
Pingback: Auto Repair Dallas
Pingback: Toyota repair
Pingback: Cheapest mattresses and beds in Glen Waverley VIC
Pingback: Alignment
Pingback: iComfort Mitcham stocks a wide range of Slumberest mattresses at lowest prices
Pingback: Pocket spring mattress start as low as $159 at iComfort Mitcham
Pingback: Honda Repair
Pingback: iComfort Mitcham stocks a wide range of SleepMaker mattresses at lowest prices
Pingback: Automobile Service
Pingback: Oil Change Dallas
Pingback: AC Repair Dallas
Pingback: Brake Repair Dallas
Pingback: Toyota repair Dallas
Pingback: K3S Motorsports
Pingback: iComfort Mitcham stocks a wide range of SleepMaker mattresses at lowest prices
Pingback: Best Value of Mattresses and Beds at iComfort Doncaster VIC
Pingback: Cheapest king size mattresses at iComfort Mitcham
Pingback: Nissan Brake repair
Pingback: Cheapest mattresses and beds in Donvale VIC
Pingback: Read more here
Pingback: Honda Repair
Pingback: Car repair
Pingback: Cheapest mattresses and beds in Donvale VIC
Pingback: Cheapest mattresses and beds in Templestowe VIC
Pingback: AC Repair Dallas
Pingback: Quality and Affordable Mattresses and Beds at iComfort Box Hill VIC
Pingback: Auto repair on
Pingback: Honda Repair
Pingback: Nissan Brake repair
Pingback: Ertugrul 116-117
Pingback: Cheapest queen size mattresses at iComfort Mitcham
Pingback: Nissan Repair
Pingback: SleepMaker mattress start as low as $159 at iComfort Mitcham
Pingback: Cheapest mattresses and beds in Nunawading VIC
Pingback: Clothes
Pingback: Cheapest single size mattresses at iComfort Mitcham
Pingback: K3S Motorsports
Pingback: AC repair
Pingback: Cheapest mattresses and beds in Mitcham VIC
Pingback: Brake repair
Pingback: ISG Syndrome
Pingback: VascuWave
Pingback: ulnar nerve entrapment
Pingback: Facettengelenkssyndrom
Pingback: Dallas Auto Repair
Pingback: Carpaltunnelsyndrom
Pingback: VascuWave
Pingback: Bandscheibenvorfall
Pingback: Car repair Dallas
Pingback: SleepMaker mattress start as low as $159 at iComfort Mitcham
Pingback: Ulnar tunnel syndrome
Pingback: Wirbelkanalverengung
Pingback: VascuWave
Pingback: VascuWave
Pingback: Repair shop Dallas
Pingback: Ulnarisrinnensyndrom
Pingback: Car Alignment
Pingback: Supinatorlogensyndrom
Pingback: Supinatorlogensyndrom
Pingback: Spondylolisthesis
Pingback: Honda Repair
Pingback: VascuWave
Pingback: Ulnar tunnel syndrome
Pingback: Repair shop Dallas
Pingback: Brake repair Dallas
Pingback: neurochirurg wiesbaden
Pingback: VascuWave
Pingback: Auto repair on
Pingback: Auto repair shop
Pingback: Auto Repair
Pingback: Saleh Farag
Pingback: Car Alignment Dallas
Pingback: Saleh Farag
Pingback: tarsal tunnel syndrome
Pingback: Repair shops for cars
Pingback: Ulnarisrinnensyndrom
Pingback: Ulnarisrinnensyndrom
Pingback: neurochirurgische
Pingback: Carpaltunnelsyndrom
Pingback: Automobile Service
Pingback: zero space technology massage chair
Pingback: Honda Repair Dallas
Pingback: Car Power window repair
Pingback: Car Power window repair
Pingback: Car repair
Pingback: Toyota repair Dallas
Pingback: see
Pingback: Free Sample
Pingback: Sublimated Jersey
Pingback: now
Pingback: wvisit
Pingback: url
Pingback: now
Pingback: this website
Pingback: url
Pingback: financial freedom
Pingback: this website
Pingback: this website
Pingback: link
Pingback: clicke here
Pingback: url
Pingback: url
Pingback: url
Pingback: click
Pingback: see
Pingback: link
Pingback: now
Pingback: link
Pingback: wvisit
Pingback: url
Pingback: see
Pingback: Think Transport LLC Seattle
Pingback: toddler convertible seat
Pingback: taxi numbers coventry
Pingback: coventry taxi to gatwick airport
Pingback: mini bus hire coventry
Pingback: coventry taxi numbers
Pingback: minibus hire coventry
Pingback: taxi coventry to birmingham airport
Pingback: 6 seater taxi
Pingback: taxi number coventry
Pingback: taxis coventry
Pingback: coventry taxi fares
Pingback: coventry taxi to stratford upon avon
Pingback: taxi parcel delivery coventry
Pingback: 7 seater taxi
Pingback: taxis coventry
Pingback: taxi coventry
Pingback: taxi firms in coventry
Pingback: taxi from coventry to birmingham airport
Pingback: taxi numbers coventry
Pingback: coventry taxi to stratford upon avon
Pingback: coventry taxi number
Pingback: taxi courier service
Pingback: taxi from coventry to birmingham airport
Pingback: forward facing car seat graco
Pingback: Corporate Wear
Pingback: fertility clinics in dc
Pingback: Custom Made Apparel
Pingback: minibus hire coventry
Pingback: Hockey
Pingback: coventry taxi firms
Pingback: minibus hire coventry
Pingback: coventry taxi number
Pingback: coventry taxis
Pingback: Corporate Wear
Pingback: coventry taxi numbers
Pingback: taxi firms in coventry
Pingback: Sublimated Apparel
Pingback: Jerseys
Pingback: 6 seater taxis Coventry
Pingback: Polo Shirt
Pingback: 6 seater taxi
Pingback: coventry taxi to london
Pingback: 6 seater taxi
Pingback: cheap car seats for sale
Pingback: taxi coventry to birmingham airport
Pingback: minibus hire coventry
Pingback: Jersey
Pingback: Team Outfit
Pingback: taxi number coventry
Pingback: Hockey Sock
Pingback: coventry cabs
Pingback: Hockey Sock
Pingback: minibus hire coventry
Pingback: taxi numbers coventry
Pingback: mini bus hire coventry
Pingback: coventry taxi to gatwick airport
Pingback: coventry taxis
Pingback: Polo Shirt
Pingback: coventry taxi to stratford upon avon
Pingback: Tennis Gear
Pingback: airport transfers coventry
Pingback: taxi coventry to birmingham airport
Pingback: taxi number coventry
Pingback: minibus hire coventry
Pingback: airport transfers coventry
Pingback: 6 seater taxi Coventry
Pingback: trasplante capilar turquia
Pingback: coventry taxi to stansted airport
Pingback: coventry taxi numbers
Pingback: taxi coventry to birmingham airport
Pingback: taxi from coventry to heathrow airport
Pingback: coventry taxi to stratford upon avon
Pingback: 4 ever all in one car seat
Pingback: taxi numbers in coventry
Pingback: coventry taxi to manchester airport
Pingback: taxi numbers in coventry
Pingback: 7 seater taxi Coventry
Pingback: high back booster car seat latch system
Pingback: coventry taxi to stratford upon avon
Pingback: Herunterladen The Boss Baby Full Movie Deutsch Ganzer Film Deutsch
Pingback: coventry taxi to stratford upon avon
Pingback: taxi coventry to birmingham airport
Pingback: mini bus hire coventry
Pingback: 7 seater taxis Coventry
Pingback: coventry taxi to stansted airport
Pingback: taxi coventry to birmingham airport
Pingback: taxis coventry
Pingback: 7 seater taxis Coventry
Pingback: mini bus hire coventry
Pingback: airport transfers coventry
Pingback: mini bus hire coventry
Pingback: coventry taxi to gatwick airport
Pingback: taxi numbers coventry
Pingback: taxi coventry to birmingham airport
Pingback: taxi coventry to birmingham airport
Pingback: acupuncture dc
Pingback: coventry taxi to manchester airport
Pingback: coventry taxi to gatwick airport
Pingback: coventry taxi to gatwick airport
Pingback: coventry taxi to gatwick airport
Pingback: coventry taxi to stratford upon avon
Pingback: taxi numbers coventry
Pingback: 7 seater taxi
Pingback: socks5
Pingback: coventry taxi to stansted airport
Pingback: nautilus car seat
Pingback: a baby car seat
Pingback: Fibre 500 Service
Pingback: music class in richmond hill
Pingback: Party Coordinator
Pingback: restaurants that cater in san diego
Pingback: best music school in richmond hill
Pingback: top music lesson markham
Pingback: top music school markham
Pingback: flute lesson in richmond hill
Pingback: guitar lesson in toronto
Pingback: drum lesson in toronto
Pingback: cheap baby car seats for sale
Pingback: music teacher in richmond hill
Pingback: Fibre 400/400 mbps
Pingback: viola lesson in toronto
Pingback: best music school in richmond hill
Pingback: vocal lesson in richmond hill
Pingback: vocal lesson in markham
Pingback: bass lesson in richmond hill
Pingback: car seat convertible booster
Pingback: violin lesson in richmond hill
Pingback: top music lesson markham
Pingback: music lesson in richmond hill
Pingback: viola lesson in richmond hill
Pingback: top music teacher in richmond hill
Pingback: music lesson in toronto
Pingback: violin lesson in markham
Pingback: cheap kids car seats
Pingback: top music teacher in richmond hill
Pingback: flute lesson in markham
Pingback: guitar lesson in markham
Pingback: vocal lesson in markham
Pingback: drum lesson in toronto
Pingback: saxophone lesson in markham
Pingback: harp lesson in markham
Pingback: cello lesson in toronto
Pingback: cello lesson in richmond hill
Pingback: bay and bow
Pingback: clarinet lesson in markham
Pingback: about us
Pingback: top music teacher in richmond hill
Pingback: saxophone lesson in toronto
Pingback: gallery
Pingback: best music school in richmond hill
Pingback: music lesson in markham
Pingback: top music teacher in richmond hill
Pingback: cello lesson in markham
Pingback: hung
Pingback: piano lesson in markham
Pingback: guitar lesson in richmond hill
Pingback: baby car seat convertible
Pingback: top music lesson markham
Pingback: music class in toronto
Pingback: services
Pingback: saxophone lesson in toronto
Pingback: drum lesson in toronto
Pingback: bass lesson in markham
Pingback: cello lesson in markham
Pingback: windows
Pingback: click here to learn more
Pingback: top music teacher in richmond hill
Pingback: music teacher in markham
Pingback: guitar lesson in markham
Pingback: windows
Pingback: viola lesson in toronto
Pingback: music lesson in markham
Pingback: gallery
Pingback: click here to learn more
Pingback: turn and tilt
Pingback: advice
Pingback: hung
Pingback: home
Pingback: Kendo classes Ravenswood
Pingback: services
Pingback: Kendo practice classes Ravenswood
Pingback: patio doors
Pingback: gallery
Pingback: Swordsmanship training classes Chicago
Pingback: about us
Pingback: Sword training classes Chicago
Pingback: Japanese Martial arts practice Ravenswood
Pingback: Expert Kendo classes in Chicago
Pingback: Kendo classes Chicago
Pingback: The Choyokan Kendo Dojo
Pingback: click here to learn more
Pingback: turn and tilt
Pingback: windows
Pingback: Japanese martial arts Chicago
Pingback: Japanese martial art classes Chicago
Pingback: Edmonton Concrete Cutting Inc.
Pingback: Expert Kendo classes in Chicago
Pingback: The Choyokan Kendo Dojo
Pingback: Kendo classes Ravenswood
Pingback: The Choyokan Kendo Dojo
Pingback: Kendo classes Chicago
Pingback: Japanese martial art classes Chicago
Pingback: Expert Kendo classes in Chicago
Pingback: Kendo training Chicago
Pingback: Kendo classes Ravenswood
Pingback: Sword training classes Ravenswood
Pingback: Kendo classes for beginners Chicago
Pingback: Japanese martial art classes Chicago
Pingback: Kendo classes Ravenswood
Pingback: Sword training classes Ravenswood
Pingback: The Choyokan Kendo Dojo
Pingback: Martial art classes Chicago
Pingback: Kendo classes for beginners Chicago
Pingback: Sword training classes Chicago
Pingback: Sword training classes Chicago
Pingback: attorney
Pingback: attorneys near me
Pingback: civil law
Pingback: attorney directory
Pingback: 3d printer
Pingback: family law
Pingback: lawyer directory
Pingback: kosteuttava kasvohoito
Pingback: lawyer
Pingback: lawyer consultation
Pingback: attorneys near me
Pingback: lawyer consultation
Pingback: family law
Pingback: Content Strategy
Pingback: klassiset ripsipidennykset
Pingback: legal aid lawyers
Pingback: immigration lawyer
Pingback: semi-permanent ink
Pingback: alexandria
Pingback: lawyers near me
Pingback: indiegame
Pingback: kestokulmat
Pingback: attorney search
Pingback: Kendo classes Chicago
Pingback: Kendo classes for beginners Chicago
Pingback: lawyer directory
Pingback: attorney at law
Pingback: business law
Pingback: civil attorney
Pingback: Content Strategy
Pingback: lawyer directory
Pingback: attorneys near me
Pingback: hellävarainen karvojen poisto
Pingback: attorney search
Pingback: Japanese martial arts practice Chicago
Pingback: law firms
Pingback: täydellinen jalkahoito
Pingback: alexandria sokerointi
Pingback: legal aid lawyers
Pingback: sokerointi
Pingback: local lawyers
Pingback: business law
Pingback: sothys
Pingback: Kendo practice classes Ravenswood
Pingback: find an attorney
Pingback: lawyers near me
Pingback: law finder
Pingback: ripsipidennykset
Pingback: attorney search
Pingback: local lawyers
Pingback: civil law
Pingback: law firm
Pingback: the fragrance shop
Pingback: body fat calculator
Pingback: kestolakkaus
Pingback: super scientific calculator
Pingback: android calculator
Pingback: body mass index female
Pingback: what is bmi index
Pingback: kestokulmat
Pingback: The Choyokan Kendo Dojo
Pingback: graphing linear equations calculator
Pingback: healthy body calculator
Pingback: qqpoker live chat
Pingback: obesity calculator
Pingback: maxbrows kestokulmat
Pingback: volyymiripset
Pingback: scientific calculator target
Pingback: 3D Printing Pen
Pingback: klassiset ripsipidennykset
Pingback: CHOYOKAN KENDO DOJO Chicago
Pingback: low gi foods
Pingback: Kendo practice classes Ravenswood
Pingback: kestokulmat
Pingback: digital calculator online
Pingback: body and bmi calculator
Pingback: Kendo beginner classes Chicago
Pingback: happipainehoito
Pingback: scientific calculator with fraction button
Pingback: solstice
Pingback: Professional martial arts classes Chicago
Pingback: Domino Kiu Kiu
Pingback: Domino Kiu Kiu
Pingback: Bandar QQ Domino
Pingback: Sword training classes Chicago
Pingback: indoor outdoor clothes dryer
Pingback: mil tactical assault gear
Pingback: Agen Judi Bola Online
Pingback: Bandar QQ Domino
Pingback: Domino Kiu Kiu
Pingback: outdoor equipment clothing
Pingback: clothing allowance 2009 military
Pingback: spec-ops tactical gear
Pingback: Agen Poker Online
Pingback: outdoor clothes
Pingback: Business Growth
Pingback: outdoor clothing and gear
Pingback: go outdoor clothing store
Pingback: contoh lamaran kerja sma
Pingback: fort jackson military clothing and sales
Pingback: outdoor rotary clothes dryer
Pingback: apps download for pc
Pingback: Online consumer Behavior
Pingback: outdoor clothing stores chicago
Pingback: usaf military clothing allowance
Pingback: used outdoor clothing
Pingback: outdoor clothing shopping
Pingback: clothing outerwear outdoor gear and
Pingback: aafes military clothing sales
Pingback: Performance Marketing
Pingback: tactical military gear reviews
Pingback: editorial photography
Pingback: concert images
Pingback: outdoor clothing on line
Pingback: military clothing sales fort hood
Pingback: us military 1960 clothing
Pingback: outdoor clothes drying
Pingback: womens outdoor clothing catalogs
Pingback: Digital Neuromarketing Strategy
Pingback: rockstar photographs
Pingback: sunline outdoor clothes dryer
Pingback: entertainment photography
Pingback: outdoor clothes
Pingback: military surplus clothing used
Pingback: outdoor wear clothing stores
Pingback: la police gear the operator tactical pants
Pingback: Neuromarketing Buy Button
Pingback: address tactical response gear
Pingback: military surplus clothes
Pingback: outdoors clothing designer stores
Pingback: clothing allowance 2009 military
Pingback: jobs in dhaka
Pingback: jobs in bekaa
Pingback: jobs in dammam
Pingback: start an amazon business
Pingback: RapidCrush
Pingback: Rapid Crush
Pingback: jobs in doha
Pingback: onlinesecrets
Pingback: Online Secrets
Pingback: what to sell on amazon
Pingback: sell on amazon
Pingback: how amazon fba works
Pingback: Onlinesecrets.com
Pingback: amazon podcasts
Pingback: Rapid Crush
Pingback: RapidCrush
Pingback: Rapid Crush
Pingback: Amz training
Pingback: Amz Insiders
Pingback: how to sell on amazon
Pingback: Onlinesecrets.com
Pingback: Rapid Crush
Pingback: Amz Insiders
Pingback: learn to sell on amazon
Pingback: Amz training
Pingback: jobs in zarqa
Pingback: Amz training
Pingback: matthew behdjou
Pingback: Amz training
Pingback: AmzInsiders
Pingback: RapidCrush
Pingback: Amz training
Pingback: learn to sell on amazon
Pingback: Onlinesecrets.com
Pingback: how amazon fba works
Pingback: what to sell on amazon
Pingback: matthew behdjou
Pingback: Amz training
Pingback: RapidCrush
Pingback: onlinesecrets.net
Pingback: jobs in saudi arabia
Pingback: onlinesecrets.net
Pingback: learn to sell on amazon
Pingback: AmzInsiders
Pingback: Amz Insiders
Pingback: jobs in amman
Pingback: how amazon fba works
Pingback: Amz training
Pingback: Rapid Crush
Pingback: start an amazon business
Pingback: matthew behdjou
Pingback: Amz training
Pingback: Amz Insiders
Pingback: Onlinesecrets.com
Pingback: selling on amazon
Pingback: onlinesecrets.net
Pingback: Amz Insiders
Pingback: learn to sell on amazon
Pingback: start an amazon business
Pingback: what to sell on amazon
Pingback: jobs in sharjah
Pingback: RapidCrush
Pingback: amazon podcasts
Pingback: amazon podcasts
Pingback: Onlinesecrets.com
Pingback: start an amazon business
Pingback: jobs in zufar
Pingback: sell on amazon
Pingback: Amz Insiders
Pingback: jobs in iraq
Pingback: what to sell on amazon
Pingback: start an amazon business
Pingback: Onlinesecrets.com
Pingback: jobs in jordan
Pingback: Rapid Crush
Pingback: Online Secrets
Pingback: Online Secrets
Pingback: RapidCrush
Pingback: amazon podcasts
Pingback: how amazon fba works
Pingback: matthew behdjou
Pingback: Rapid Crush
Pingback: how amazon fba works
Pingback: Rapid Crush
Pingback: learn to sell on amazon
Pingback: Online Secrets
Pingback: Online Secrets
Pingback: how amazon fba works
Pingback: onlinesecrets.net
Pingback: Amazing Selling Machine
Pingback: selling on amazon
Pingback: Rapid Crush
Pingback: AmzInsiders
Pingback: AmzInsiders
Pingback: onlinesecrets
Pingback: Online Secrets
Pingback: onlinesecrets.net
Pingback: Online Secrets
Pingback: sell on amazon
Pingback: Amz Insiders
Pingback: Amz training
Pingback: how to sell on amazon
Pingback: sell on amazon
Pingback: amazon podcasts
Pingback: matthew behdjou
Pingback: how amazon fba works
Pingback: matthew behdjou
Pingback: sell on amazon
Pingback: Onlinesecrets.com
Pingback: Physician Jobs
Pingback: amazon training
Pingback: learn to sell on amazon
Pingback: Amz training
Pingback: Onlinesecrets.com
Pingback: amazon podcasts
Pingback: Physician Recruiters
Pingback: Amz Insiders
Pingback: Online Secrets
Pingback: Online Secrets
Pingback: Onlinesecrets.com
Pingback: Online Secrets
Pingback: Physician Recruitment Firm
Pingback: Physician Recruiters
Pingback: Amz Insiders
Pingback: selling on amazon
Pingback: Physician Recruiters
Pingback: Online Secrets
Pingback: selling on amazon
Pingback: boom beach
Pingback: Onlinesecrets.com
Pingback: Amz Insiders
Pingback: how to sell on amazon
Pingback: what to sell on amazon
Pingback: boom beach
Pingback: sell on amazon
Pingback: boom beach
Pingback: boom beach pc
Pingback: boom beach download
Pingback: start an amazon business
Pingback: matthew behdjou
Pingback: start an amazon business
Pingback: what to sell on amazon
Pingback: start an amazon business
Pingback: learn to sell on amazon
Pingback: how to sell on amazon
Pingback: amazon training
Pingback: RapidCrush
Pingback: how to sell on amazon
Pingback: start an amazon business
Pingback: how to sell on amazon
Pingback: how to sell on amazon
Pingback: Amazing Selling Machine
Pingback: Amazing Selling Machine
Pingback: how amazon fba works
Pingback: RapidCrush
Pingback: onlinesecrets.net
Pingback: Onlinesecrets.com
Pingback: onlinesecrets
Pingback: amazon training
Pingback: AmzInsiders
Pingback: matthew behdjou
Pingback: onlinesecrets
Pingback: Amz training
Pingback: Onlinesecrets.com
Pingback: amazon podcasts
Pingback: Amz Insiders
Pingback: onlinesecrets
Pingback: start an amazon business
Pingback: Rapid Crush
Pingback: Amz Insiders
Pingback: Online Secrets
Pingback: selling on amazon
Pingback: Rapid Crush
Pingback: Online Secrets
Pingback: Amz Insiders
Pingback: website laten maken
Pingback: how amazon fba works
Pingback: Online Secrets
Pingback: how amazon fba works
Pingback: amazon podcasts
Pingback: how to sell on amazon
Pingback: Online Secrets
Pingback: how amazon fba works
Pingback: matthew behdjou
Pingback: matthew behdjou
Pingback: amazon training
Pingback: selling on amazon
Pingback: Online Secrets
Pingback: start an amazon business
Pingback: Amazing Selling Machine
Pingback: Rapid Crush
Pingback: start an amazon business
Pingback: Amz Insiders
Pingback: learn to sell on amazon
Pingback: Rapid Crush
Pingback: how to sell on amazon
Pingback: Amz training
Pingback: Online Secrets
Pingback: sell on amazon
Pingback: Amazing Selling Machine
Pingback: AmzInsiders
Pingback: AmzInsiders
Pingback: Amazing Selling Machine
Pingback: how to sell on amazon
Pingback: hook up sites
Pingback: RapidCrush
Pingback: Amz training
Pingback: dating
Pingback: Rapid Crush
Pingback: learn to sell on amazon
Pingback: how to sell on amazon
Pingback: matthew behdjou
Pingback: how to sell on amazon
Pingback: onlinesecrets.net
Pingback: matthew behdjou
Pingback: amazon podcasts
Pingback: matthew behdjou
Pingback: selling on amazon
Pingback: sell on amazon
Pingback: Amz Insiders
Pingback: Amz training
Pingback: how to sell on amazon
Pingback: start an amazon business
Pingback: onlinesecrets
Pingback: how to sell on amazon
Pingback: onlinesecrets
Pingback: Amz Insiders
Pingback: best free dating sites
Pingback: sell on amazon
Pingback: Onlinesecrets.com
Pingback: Amz Insiders
Pingback: onlinesecrets
Pingback: how to sell on amazon
Pingback: Rapid Crush
Pingback: how amazon fba works
Pingback: amazon podcasts
Pingback: Onlinesecrets.com
Pingback: learn to sell on amazon
Pingback: Dating Websites
Pingback: onlinesecrets
Pingback: Onlinesecrets.com
Pingback: amazon training
Pingback: amazon podcasts
Pingback: Amazing Selling Machine
Pingback: Onlinesecrets.com
Pingback: Http://suckhoenamkhoa.com/
Pingback: RapidCrush
Pingback: AmzInsiders
Pingback: Amz training
Pingback: how amazon fba works
Pingback: amazon podcasts
Pingback: RapidCrush
Pingback: RapidCrush
Pingback: onlinesecrets
Pingback: Amz training
Pingback: learn to sell on amazon
Pingback: Onlinesecrets.com
Pingback: Online Secrets
Pingback: selling on amazon
Pingback: Online Secrets
Pingback: best free dating sites
Pingback: Amz training
Pingback: Free Dating Online
Pingback: woman seeking men
Pingback: woman seeking men
Pingback: polyvore outfits
Pingback: amazon product research
Pingback: Daredevil Vs. She-Hulk – Marvel Super Heroes: What The–?! Ep. 33
Pingback: "FX’s Legion, Marvel’s Spider-Man, & Zach Braff Gets A Surprise on Earth’s Mightiest Show"
Pingback: how to make money with dropshipping
Pingback: Announcing: Marvel Powers United Oculus Rift + Touch VR trailer
Pingback: Actor Michael K. Williams stops by This Week in Marvel Podcast
Pingback: amazon fba for beginners
Pingback: Bitten by a Radioactive Spider – Spider Man – MARVEL 101
Pingback: womens high waisted bikini
Pingback: Cosplayer Miss Mad Love Becomes Captain Marvel – Marvel Becoming
Pingback: ship from china to amazon
Pingback: womens bikini sets
Pingback: Arab Escorts
Pingback: Kitchen storage and organization
Pingback: "Bobbi’s Back in Action – Marvel’s Agents of S.H.I.E.L.D. Season 3, Ep. 6"
Pingback: v-camo camo
Pingback: Cosplayer Cap Santiago Becomes Ares – Marvel Becoming
Pingback: British Escorts
Pingback: Tropical home decor
Pingback: LEGO Dimensions – All 8 DC Comics Characters + Free Roam Gameplay (DC Comics Adventure World)
Pingback: LEGO Marvel Super Heroes 2 – Thor Trailer
Pingback: Follow us on Instagram
Pingback: heathrow escort
Pingback: best product research tool
Pingback: how to make money with shopify
Pingback: Reusable Non-stick Oven BBQ Oil Paper Baking Mat
Pingback: Marvel NOW! Titles for July 26th
Pingback: webpage
Pingback: official
Pingback: Home textiles
Pingback: Outcall Escorts
Pingback: Carnage — Marvel 101
Pingback: Marvel LIVE! at New York Comic-Con 2017 – Day 4
Pingback: email
Pingback: womens bikini sets
Pingback: ship from china to amazon
Pingback: portal
Pingback: portal
Pingback: Lego Marvel Superheroes 2 – Animation Reel
Pingback: Gag Reel 2 – Marvel’s Avengers: Age of Ultron
Pingback: Marvel’s Doctor Strange Teaser Trailer
Pingback: 4-In-1 Separate Cooking Aluminum Alloy Frying Pan
Pingback: escorts in london
Pingback: contact
Pingback: apply
Pingback: MARVEL Powers United VR – Inhumans Trailer
Pingback: viral launch coupon code
Pingback: Laurenralphuk
Pingback: Portable Bent Toilet Cleaning Brush
Pingback: Unique Stainless Steel Pineapple Eye & Seed Remover
Pingback: The Stars of MTV’s Teen Wolf Prowl on Marvel LIVE! at San Diego Comic-Con 2015
Pingback: Marvel Top 10 Martial Artists
Pingback: "Secret Warriors Assemble – Marvel’s Agents of S.H.I.E.L.D. Season 3, Ep. 17"
Pingback: British Escorts
Pingback: DC Comics
Pingback: Marvel’s Captain America: The Winter Soldier – Featurette 2
Pingback: Private Investigation Bangalore
Pingback: Soul Stone – Marvel 101
Pingback: security guard agency in Bangalore
Pingback: Orrgo – Marvel 101 – Monsters Unleashed
Pingback: Welcome to Earth’s Mightiest Show!
Pingback: Agency Escorts
Pingback: Thor: The Dark World Official Trailer HD
Pingback: "These Are Volunteers? – Marvel’s Agents of S.H.I.E.L.D. Season 3, Ep. 20"
Pingback: security agency in Bangalore
Pingback: Ward! Casting Marvel’s Inhumans! – Marvel Minute 2017
Pingback: Marvel Super Heroes: What The–?! The Age Of ULTRON
Pingback: login
Pingback: Compressed High Air Pressure Kitchen Sink and Toilet Bowl Cleaning Drain Blaster
Pingback: Take Home Marvel’s “Captain America: The Winter Soldier”
Pingback: USA Commercial Cleaning Services
Pingback: On the Road to Doomsday Clock Trailer Reaction by Matt with Super Hero Nexus
Pingback: USA Commercial Cleaning Services - Services
Pingback: Marvel Studios’ Avengers: Infinity War — “Legacy” TV Spot
Pingback: Marvel Studios’ Black Panther – Don’t Miss TV Spot
Pingback: British Escorts
Pingback: Marvel Top 10 Most Powerful Magicians
Pingback: The stars of Marvel Studios’ Avengers: Infinity War talk with Earth’s Mightiest Show
Pingback: inspire ft2 workout machine
Pingback: Funny Interactive Rotating Butterfly Pet Toy For Cats
Pingback: Background Check Bangalore
Pingback: best home gym equipment
Pingback: Basketball Player Michael Jordan Vintage Wall Sticker
Pingback: home fitness equipment
Pingback: Security Auditing
Pingback: escort girls london
Pingback: Transit Trends
Pingback: inspire ft2 workout equipment
Pingback: Home storage and organization
Pingback: USA Commercial Cleaning Services - Contact Us
Pingback: adventure games
Pingback: Manned Security Agency Bangalore
Pingback: Follow us on Pinterest
Pingback: best home gym machine
Pingback: home gym equipment
Pingback: inspire ft2
Pingback: Background Investigation Bangalore
Pingback: Mini Keyboard Vacuum Cleaner & Household Dust Collector
Pingback: weight lighting equipment
Pingback: game development
Pingback: video games
Pingback: USA Commercial Cleaning Services - Picture Gallery
Pingback: metroidvania
Pingback: computer games
Pingback: Shop for home goods at Pichichome
Pingback: best home workout machine
Pingback: games
Pingback: Madden coins Xbox
Pingback: games
Pingback: home gym machine
Pingback: fitness equipment
Pingback: video game designer
Pingback: verniz para assoalho de madeira
Pingback: home gym
Pingback: verniz a base de agua
Pingback: Madden coins ps4
Pingback: wedding gifts
Pingback: verniz para piso de madeira
Pingback: exercise equipment
Pingback: exercise equipment
Pingback: inspire ft2
Pingback: home workout equipment
Pingback: inspire ft2 workout machine
Pingback: fitness equipment
Pingback: gym equipment
Pingback: best home gym machine
Pingback: Fut coins
Pingback: workout equipment
Pingback: curso de hambúrguer gourmet
Pingback: best home gym machine
Pingback: verniz para taco de madeira
Pingback: verniz para piso de madeira
Pingback: Blonde Escorts
Pingback: Buy Mut coins
Pingback: Buy cheap madden coins
Pingback: mystery action book
Pingback: Famous irvine comedians
Pingback: Chihuahua children's animal book
Pingback: midwest authors
Pingback: mystery action book
Pingback: Successful Weight Loss
Pingback: verniz piso madeira
Pingback: escort agency birmingham
Pingback: clairvoyant readings
Pingback: mindfulness for teachers
Pingback: Famous irvine comedians
Pingback: amateur comedy
Pingback: cute animal book
Pingback: cute animal book
Pingback: mindfulness for pupils
Pingback: kansas authors
Pingback: Boxing book
Pingback: escort uk
Pingback: curso de reparo de celular
Pingback: bad-dad joke book
Pingback: mindfulness courses
Pingback: mystery action book
Pingback: counselling and psychotherapy for adults
Pingback: couples counselling
Pingback: Chat Neuchatel
Pingback: diving in hurghada
Pingback: counselling and psychotherapy for children
Pingback: safari in hurghada
Pingback: digital piano and midi keyboard
Pingback: snorkelling in hurghada
Pingback: hurghada excursions
Pingback: best digital piano keyboard
Pingback: digital piano app
Pingback: hurghada to luxor excursions
Pingback: best digital piano india
Pingback: digital piano yamaha
Pingback: digital piano adelaide
Pingback: digital piano yamaha
Pingback: digital piano yamaha price
Pingback: digital piano action
Pingback: roland piano reviews
Pingback: digital piano australia
Pingback: digital piano assembly
Pingback: digital piano
Pingback: yamaha piano reviews baby grand
Pingback: digital piano amazon
Pingback: digital piano kawai
Pingback: digital piano vs acoustic piano
Pingback: piano accordion reviews
Pingback: digital piano lowest price
Pingback: digital piano adelaide
Pingback: web design agency
Pingback: digital piano action
Pingback: logo design
Pingback: piano keyboard brand reviews
Pingback: best digital pianos with weighted keys
Pingback: hijama birmingham
Pingback: Find high quality fishing rods and tools
Pingback: wedding events uae
Pingback: High-Tech Design Electronic Spice Mill with LED Lighting
Pingback: Unique Egglettes Egg Cooker
Pingback: web design agency
Pingback: Pet products
Pingback: Decorative 3D Acrylic Mirror Wall Stickers For Living Room & Bedroom
Pingback: Cookware just for you
Pingback: Kitchen utensils
Pingback: Vegetable Spiral Cutter Spiralizer Digging Device Corer For Stuffed Vegetables
Pingback: digital piano kawai
Pingback: georgetown piano bar reviews
Pingback: digital piano kawai
Pingback: acoustic piano reviews
Pingback: digital piano lowest price
Pingback: judi togel barcelona
Pingback: digital piano vs acoustic piano
Pingback: piano reviews australia
Pingback: piano adventures reviews
Pingback: digital piano 88 keys
Pingback: Milwaukee M18 Combo Kit
Pingback: digital piano lowest price
Pingback: piano app reviews
Pingback: Milwaukee M18 Drill
Pingback: Milwaukee 18-Volt Combo
Pingback: best digital piano under 500
Pingback: Best Milwaukee 2691-22 Drill
Pingback: acoustic piano reviews
Pingback: iota coin price
Pingback: best digital piano 2017
Pingback: best digital piano 2018
Pingback: piano reviews uk
Pingback: digital piano roland
Pingback: reviews piano keyboards
Pingback: Milwaukee M18 Drill
Pingback: Milwaukee Drill
Pingback: Milwaukee M18 Impact Driver
Pingback: humidifier
Pingback: Milwaukee M18 Drill
Pingback: Milwaukee 18-Volt Combo
Pingback: Milwaukee M18 Impact Driver
Pingback: Milwaukee Powerful Cordless Drill
Pingback: Milwaukee Powerful Cordless Drill
Pingback: Milwaukee Cordless Combo Kit
Pingback: Milwaukee Cordless Drill
Pingback: rap videos
Pingback: day trading cryptocurrency cryptocurrency trading
Pingback: Bare knuckle fighting
Pingback: Humidifier
Pingback: iost coin
Pingback: Humidifier
Pingback: virtual business
Pingback: website
Pingback: smart negosyo
Pingback: ofw investment
Pingback: work at home
Pingback: website directory
Pingback: Jinx Adc Doublelift season 8 runes and builds
Pingback: sign up now
Pingback: day trading cryptocurrency cryptocurrency trading
Pingback: trash containers
Pingback: furniture disposal
Pingback: roofing dumpster
Pingback: dumpster rental prices
Pingback: waste management rent a dumpster
Pingback: junk dumpster
Pingback: dumpster rental utah
Pingback: roll off container rental prices
Pingback: waste management portable dumpster
Pingback: open dumpster
Pingback: dumpster rental atlanta
Pingback: cost of a dumpster rental
Pingback: disposal bins rental
Pingback: construction dumpster
Pingback: dumpster delivery and pick up
Pingback: yard dumpster
Pingback: demolition container rental
Pingback: junk hauling services
Pingback: ten yard dumpster
Pingback: rent a small dumpster
Pingback: construction dumpster rental prices
Pingback: roll off trailers
Pingback: roll off bin rental
Pingback: dumpster waste management
Pingback: trash container rentals
Pingback: construction dumpster rental prices
Pingback: yard waste removal
Pingback: roll off trash containers
Pingback: rent a bin
Pingback: Advanced guitar bending techniques
Pingback: container dumpster rental
Pingback: rent trash container
Pingback: 40 yard roll off dumpster
Pingback: waste management company
Pingback: 40 yard dumpster rental
Pingback: cost for dumpster rental
Pingback: waste removal companies
Pingback: garbage bins for rent
Pingback: roll off companies
Pingback: how to buy instagram views
Pingback: roll off dumpster waste management
Pingback: dumpster site
Pingback: roll off trailer
Pingback: dumpster bin rental
Pingback: buy instagram views
Pingback: waste containers rental
Pingback: rolloff dumpster
Pingback: roll off dumpster service
Pingback: find your love
Pingback: how to buy instagram views
Pingback: bin rental
Pingback: dumpsters for rent
Pingback: how to buy instagram views
Pingback: roll off dumpster rental cost
Pingback: container garbage rental
Pingback: cost of renting dumpster
Pingback: dumpster container rental
Pingback: dumpster bin rentals
Pingback: rent small dumpster
Pingback: dumpster rental cost
Pingback: lets buy instagram video views
Pingback: lets buy instagram views
Pingback: buy instagram views
Pingback: buy instagram video views
Pingback: garbage bins for rent
Pingback: yard dumpster
Pingback: waste management dumpster bag
Pingback: 15 yard dumpster rental
Pingback: how to buy instagram video views
Pingback: how to buy instagram views
Pingback: waste container
Pingback: rental of dumpster
Pingback: garbage dumpster rental prices
Pingback: dumpster roll off rental
Pingback: dumpster rental services
Pingback: disposal services
Pingback: SEO Elizabethtown, KY
Pingback: roll off dumpster cost
Pingback: cost of 20 yard dumpster
Pingback: dumpster bin rental
Pingback: dumpster rental utah
Pingback: small dumpster rental
Pingback: sign up now
Pingback: rubbish bin rental
Pingback: rental bins
Pingback: waste disposal
Pingback: dumpster pick up
Pingback: 10 yard container
Pingback: construction roll off dumpsters
Pingback: construction waste containers
Pingback: gotjunk
Pingback: dumpster rental las vegas
Pingback: construction debris removal
Pingback: dumpster central
Pingback: 10 yard dumpster rental
Pingback: waste disposal bins
Pingback: dumpster roll off rental
Pingback: rolloff container
Pingback: refuse dumpster
Pingback: pick up garbage
Pingback: dumpster rental nashville
Pingback: rolloff dumpsters
Pingback: roll up dumpster
Pingback: garbage dump
Pingback: roll off
Pingback: yard waste dumpster
Pingback: Download Free PC Game
Pingback: trash hauling
Pingback: residential waste removal
Pingback: junk hauling services
Pingback: laptop game
Pingback: price of dumpster
Pingback: computer game download
Pingback: 4 yard dumpster
Pingback: free download games
Pingback: free pc games
Pingback: 40 yard trash container
Pingback: dump containers rental
Pingback: recycling roll off containers
Pingback: garbage bin
Pingback: pc games download for windows 7
Pingback: waste bins rental
Pingback: computer games download
Pingback: car racing game download
Pingback: couple
Pingback: size of dumpsters
Pingback: car racing games download
Pingback: free pc games
Pingback: cheap dumpsters
Pingback: refuse container rental
Pingback: how much to rent a dumpster
Pingback: metal dumpster
Pingback: where to rent dumpsters
Pingback: rolloff container
Pingback: trash removal
Pingback: city dumpster
Pingback: dumpster rental phoenix
Pingback: online pc games
Pingback: pc games free download full version for windows 8
Pingback: free pc games
Pingback: dirt dumpster rental
Pingback: 2 yard dumpster
Pingback: dumpsters to rent
Pingback: online pc games
Pingback: online games for pc
Pingback: online games for pc
Pingback: games free download
Pingback: dumpster rental san jose
Pingback: garbage waste disposal
Pingback: trash collection
Pingback: 40 yard dumpster cost
Pingback: small dumpsters for rent
Pingback: action games free download for windows
Pingback: junk removal
Pingback: pc games free download full version
Pingback: residential waste removal
Pingback: pc games free download full version for windows 8
Pingback: small games free download for windows
Pingback: small games free download for windows
Pingback: waste bin rental
Pingback: discount dumpsters
Pingback: dumpster trash
Pingback: dji phantom drones
Pingback: waste management dumpster sizes
Pingback: waste bin rental
Pingback: dating
Pingback: Best deal splashdrone
Pingback: garbage removal
Pingback: construction site dumpster
Pingback: dumpster rental ma
Pingback: dumpster rental minneapolis
Pingback: rent a garbage bin
Pingback: trash dumpsters
Pingback: best deal mavic platinum in australia
Pingback: container dumpster
Pingback: waste management company
Pingback: roll off waste containers
Pingback: dumpster garbage
Pingback: debris container rental
Pingback: yard waste
Pingback: garbage bin rental
Pingback: discount price dji mavic
Pingback: trash haulers
Pingback: roll off container dimensions
Pingback: order a dumpster
Pingback: 20 yard dumpster
Pingback: dumpster for a day
Pingback: 10 yard roll off dumpster
Pingback: buy dji drones
Pingback: roll away dumpster
Pingback: trash removal services
Pingback: Best deal splashdrone Australia
Pingback: roll off dumpster waste management
Pingback: rent dumpster prices
Pingback: demolition dumpster rental
Pingback: bfi dumpster rental
Pingback: dumpster rental winston fl
Pingback: dumpster bin rentals
Pingback: roll off bin rental
Pingback: waste management dumpster rates
Pingback: average cost of dumpster rental
Pingback: home trash removal
Pingback: 40 yard dumpster rental price
Pingback: dumpster rental near me
Pingback: roll off service
Pingback: dumpster pickup
Pingback: garbage recycling
Pingback: smallest dumpster size
Pingback: affordable dumpster rental
Pingback: waste management rent dumpster
Pingback: 10 yard dumpster dimensions
Pingback: couple
Pingback: dumpster pricing
Pingback: roll off dumpsters rental
Pingback: roll away dumpster cost
Pingback: waste pickup
Pingback: dumpster rental Winter Park
Pingback: waste management roll off containers
Pingback: dumpster rental Davenport
Pingback: construction debris dumpster
Pingback: roll off bin rental
Pingback: 20 yard dumpster prices
Pingback: dumpster rental Ocoee
Pingback: 1 yard dumpster
Pingback: 40 yard dumpster rental
Pingback: city dumpster
Pingback: dumpster rental prices
Pingback: disposable dumpster
Pingback: trash pickup
Pingback: price for dumpster rental
Pingback: 30 yard dumpster prices
Pingback: garbage companies
Pingback: garbage container rentals
Pingback: haul away junk
Pingback: trash hauling services
Pingback: junk container rental
Pingback: dumpster rental denver
Pingback: dumpster rental winston fl
Pingback: dirt dumpster
Pingback: i need a website
Pingback: Driving Instructor Jobs
Pingback: need a website
Pingback: bin rental toronto
Pingback: 800 junk
Pingback: roll off container dimensions
Pingback: local dumpster rental companies
Pingback: dumpster rental business
Pingback: junk removal nj
Pingback: bulk trash pickup
Pingback: waste disposal containers
Pingback: forex trade alerts
Pingback: seo services
Pingback: Photo booth near bloomfield nj
Pingback: ea coding
Pingback: Wedding nj
Pingback: The Accountant Plus
Pingback: www.boostgal.com/instagram.php
Pingback: fx robot
Pingback: www.boostgal.com/linkedin.php
Pingback: Your Accounting Service Partner
Pingback: The Accountant Plus
Pingback: www.boostgal.com/twitter.php
Pingback: www.boostgal.com
Pingback: www.boostgal.com/sites.php
Pingback: www.boostgal.com/website.php
Pingback: Your Accounting Service Partner
Pingback: The Accountant Plus
Pingback: Your Book keeping partner
Pingback: Laminated Loading Dock Bumpers
Pingback: www.boostgal.com/musically.php
Pingback: www.boostgal.com/google.php
Pingback: www.boostgal.com/tumblr.php
Pingback: Extra-Length Laminated Dock Bumpers
Pingback: The Accountant Plus
Pingback: The Accountant Plus
Pingback: stock screener tool
Pingback: The Accountant Plus
Pingback: www.boostgal.com/spotify.php
Pingback: Gym stringers
Pingback: Mens muscle shirt
Pingback: www.boostgal.com/periscope.php
Pingback: www.boostgal.com/youtube.php
Pingback: alpha wear
Pingback: Muscle shirt
Pingback: Steel-Face Dock Bumpers
Pingback: Molded Loading Dock Bumpers
Pingback: Dura-Soft Heavy-Duty Steel-Face Bumpers
Pingback: Womens fitness apparel
Pingback: capital smart city plots
Pingback: Fitness apparel
Pingback: Muscle club apparel
Pingback: Gym clothes
Pingback: how to learn a trade
Pingback: Lifting clothes
Pingback: Korea Online Shopping Site
Pingback: real estate capital smart city
Pingback: Gym hoodies
Pingback: cryptocurrency calculator
Pingback: Fitted hoodie
Pingback: capital smart city
Pingback: Gym apparel
Pingback: islamabad capital smart city
Pingback: capital smart city islamabad
Pingback: Read more here
Pingback: islamabad capital smart city
Pingback: Iceland Online Shopping Site
Pingback: top 10 cryptocurrency
Pingback: forex bonus
Pingback: Cryptocurrency
Pingback: AV
Pingback: ANGELIUM
Pingback: Blockchian
Pingback: Best Pest Market
Pingback: Sexy
Pingback: Buy pets Supplies
Pingback: Sexy
Pingback: link coin
Pingback: ICO
Pingback: Animal market
Pingback: Cyber sex
Pingback: Cryptocurrency
Pingback: Low price bluetooth heapdhones
Pingback: ark cryptocurrency
Pingback: AI platform
Pingback: estate agents Dublin
Pingback: FB messenger chatbot
Pingback: estate agents Dublin
Pingback: More about the author
Pingback: AI chatbot Management
Pingback: Dublin real estate agent
Pingback: Extra resources
Pingback: Visit Your URL
Pingback: Dublin letting agency
Pingback: Resources
Pingback: Our site
Pingback: HR chatbot
Pingback: Mental Health Advocate Justin Peck
Pingback: Chatbot How to
Pingback: click for source
Pingback: Dublin real estate agency
Pingback: Dublin real estate agencies
Pingback: FB messenger AI
Pingback: Ai chatbot
Pingback: AI chatbot Management
Pingback: Intelligence
Pingback: Dublin properties for sale
Pingback: Dublin letting agency
Pingback: Dublin properties for sale
Pingback: Dublin estate agents
Pingback: Dublin estate agent
Pingback: Messenger Chatbot
Pingback: estate agents Dublin
Pingback: Chatbots
Pingback: Dublin letting agency
Pingback: Artificial Intelligence
Pingback: AI Howto
Pingback: Dublin properties for sale
Pingback: Swing trading
Pingback: Intelligence
Pingback: seo meaning
Pingback: Bitcoin Price
Pingback: what is seo
Pingback: website search engine optimisation
Pingback: Mississauga Escorts
Pingback: seo meaning
Pingback: Huvafenfushi Maldives Resort
Pingback: One and Only Reethi Rah Maldives
Pingback: Montreal Escort
Pingback: trx price
Pingback: Learn About Stock Market Investing
Pingback: seo company uk
Pingback: seo company rankings
Pingback: Maldives Gili Lankanfushi
Pingback: website search engine optimization
Pingback: seo web design
Pingback: search engines
Pingback: Daytrading
Pingback: search engines list
Pingback: Dow Jones Today
Pingback: Soneva jani resort
Pingback: Soneva Fushi Maldives
Pingback: ethereum news
Pingback: Vancouver Escort
Pingback: Escort in Ottawa
Pingback: hair restoration
Pingback: stock market News
Pingback: hair restoration ireland
Pingback: hair restoration
Pingback: Milaidhoo island resort
Pingback: Web Development Packages
Pingback: hair restoration
Pingback: Web Development Packages
Pingback: Wall Street Forum
Pingback: hair restoration
Pingback: Dow Jones Today
Pingback: Web Development News
Pingback: Click Here for a Free Consultation
Pingback: Web Development Services
Pingback: New York Stock Exchange
Pingback: We Fight For The Injured
Pingback: harestoration Dublin
Pingback: Web Development Packages
Pingback: Web Development News
Pingback: hair restoration ireland
Pingback: London Escorts
Pingback: Atlanta Escorts
Pingback: Club flyers
Pingback: Photoshop flyers templates
Pingback: Unique flyer
Pingback: Night club flyer
Pingback: Psd flyer templates
Pingback: Photoshop Flyers
Pingback: Check Out Your URL
Pingback: click for source
Pingback: Microdermabrasion Miami
Pingback: We Fight For The Injured
Pingback: Resources
Pingback: Night club flyer
Pingback: next page
Pingback: next page
Pingback: More Help
Pingback: Unique flyer
Pingback: link
Pingback: Check Out Your URL
Pingback: Photoshop flyers templates
Pingback: Don't Pay Unless We Win Case
Pingback: Extra resources
Pingback: Psd templates
Pingback: Our site
Pingback: Free psd flyer
Pingback: helpful resources
Pingback: helpful hints
Pingback: Flyers Templates Psd
Pingback: Photoshop Flyers
Pingback: Night club flyer
Pingback: Free psd flyer
Pingback: More Help
Pingback: more helpful hints
Pingback: more helpful hints
Pingback: Flyer templates
Pingback: helpful resources
Pingback: next page
Pingback: More Bonuses
Pingback: Photoshop flyers templates
Pingback: Flyers Templates Psd
Pingback: We Fight For The Injured
Pingback: Chicago Escorts
Pingback: Photoshop flyers templates
Pingback: more helpful hints
Pingback: more helpful hints
Pingback: htthttps://www.minds.com/blog/view/835398603731398656
Pingback: Boston Escorts
Pingback: helpful hints
Pingback: Night club flyer
Pingback: Club flyers
Pingback: additional reading
Pingback: Gotpsd Templates
Pingback: Resources
Pingback: Source
Pingback: CR10 coupons
Pingback: Psd templates
Pingback: Extra resources
Pingback: More about the author
Pingback: more
Pingback: next page
Pingback: helpful resources
Pingback: additional reading
Pingback: More Bonuses
Pingback: Vacation Homes Mexico
Pingback: Continue Reading
Pingback: Resources
Pingback: CR10 discount coupons
Pingback: More hints
Pingback: Resources
Pingback: Don't Pay Unless We Win Case
Pingback: More Help
Pingback: We Fight For The Injured
Pingback: evo
Pingback: evo issues
Pingback: tuning
Pingback: evo 9 review
Pingback: Creality CR10 codes
Pingback: CR10 coupon codes
Pingback: mitsubishi
Pingback: evo 8 recalls
Pingback: Creality CR10 codes
Pingback: Houston Escorts
Pingback: evo recalls
Pingback: 1000hp evo
Pingback: Escort in Las Vegas
Pingback: 1000hp evo
Pingback: evo recalls
Pingback: evo 9 turbo
Pingback: LA Personal Injury Lawyers
Pingback: evo 8 review
Pingback: terrarium tv apK
Pingback: terrarium tv apK
Pingback: Don't Pay Unless We Win Case
Pingback: evo x
Pingback: terrarium tv apK
Pingback: wmi provider host
Pingback: wmi provider host
Pingback: terrarium tv apK
Pingback: evo 9 turbo
Pingback: tutuapp apk
Pingback: 1000hp evo
Pingback: Framaroot APK
Pingback: evo 8 recalls
Pingback: Escort in Miami
Pingback: evo 8 review
Pingback: czeromedia
Pingback: evo review
Pingback: evo 9
Pingback: star tattoos for men
Pingback: bull skull tattoos
Pingback: evolution
Pingback: czeromedia evo
Pingback: evo 9 launch
Pingback: half sun tattoos
Pingback: evo x
Pingback: czeromedia
Pingback: evo 8 build
Pingback: buddha tattoo designs
Pingback: evo review
Pingback: evo recalls
Pingback: music tattoo designs
Pingback: iTube Pro
Pingback: evo 8 review
Pingback: iTube Pro
Pingback: butterfly tattoos
Pingback: wrist tattoos for men
Pingback: star tattoo designs
Pingback: evo
Pingback: lancer evo
Pingback: losing weight while breastfeeding
Pingback: simple neck tattoos
Pingback: evo 8 turbo
Pingback: czeromedia evo
Pingback: how many calories to lose weight calculator
Pingback: evo 8 recalls
Pingback: buddha tattoo designs
Pingback: neck tattoos
Pingback: Los Angeles Escorts
Pingback: how to lose weight overnight
Pingback: MCA
Pingback: how to lose weight while pregnant
Pingback: Car
Pingback: does drinking water help lose weight
Pingback: how does apple cider vinegar help you lose weight
Pingback: evolution
Pingback: Moving violations
Pingback: best way to lose weight fast
Pingback: evo recalls
Pingback: evo 8 build
Pingback: evo
Pingback: Legal fees
Pingback: ants control service
Pingback: San Diego Escorts
Pingback: Assistance
Pingback: evo x
Pingback: evo 8 build
Pingback: cheap end of tenancy cleaning
Pingback: cheap end of tenancy cleaning
Pingback: cheap end of tenancy cleaning
Pingback: evo 8 recalls
Pingback: Medical consultant
Pingback: mitsubishi lancer
Pingback: Worldwide
Pingback: evo x
Pingback: evo review
Pingback: Hospitalized
Pingback: Car
Pingback: mitsubishi
Pingback: Help
Pingback: Escort in New York City
Pingback: mitsubishi
Pingback: mitsubishi lancer
Pingback: what to eat to lose weight
Pingback: Tack
Pingback: emergency
Pingback: end of tenancy cleaners
Pingback: Stolen vehicle
Pingback: Service
Pingback: lancer evo
Pingback: cleaning tenancy london
Pingback: evo x recalls
Pingback: evo review
Pingback: evo
Pingback: how to lose weight in one day
Pingback: evo x recalls
Pingback: how to lose weight fast naturally
Pingback: evo issues
Pingback: how to lose weight naturally
Pingback: mitsubishi lancer
Pingback: evo 9 launch
Pingback: Escort in San Francisco
Pingback: Seattle Escorts
Pingback: mitsubishi evo recalls
Pingback: i want to lose weight
Pingback: evo 9 review
Pingback: evo 8 recalls
Pingback: not losing weight on keto
Pingback: how to lose weight running
Pingback: evolution
Pingback: evolution
Pingback: evo 8 review
Pingback: evo x
Pingback: how much water to drink a day to lose weight
Pingback: czeromedia
Pingback: car body repair
Pingback: evo x
Pingback: evo review
Pingback: tuning
Pingback: diet meal plan to lose weight
Pingback: evo 8 jdm
Pingback: mitsubishi evo
Pingback: 1000hp evo
Pingback: ants exterminators
Pingback: evo review
Pingback: not losing weight
Pingback: evo 9 launch
Pingback: evo review
Pingback: pest control for ants
Pingback: tuning
Pingback: evo 9
Pingback: cheap end of tenancy cleaning
Pingback: mitsubishi
Pingback: best way to lose weight for women
Pingback: body shop near me
Pingback: dance to lose weight
Pingback: czeromedia
Pingback: not eating to lose weight
Pingback: evo 9
Pingback: evo review
Pingback: evo issues
Pingback: best way to lose weight for men
Pingback: little black ants exterminators
Pingback: evo 9 turbo
Pingback: best end of tenancy cleaning
Pingback: how do you lose weight
Pingback: evolution
Pingback: czeromedia evo
Pingback: ants exterminators
Pingback: czeromedia evo
Pingback: little black ants
Pingback: como posso emagrecer rapido e facil
Pingback: czeromedia
Pingback: evo x
Pingback: evolution
Pingback: how to lose weight in 3 days
Pingback: lancer evo
Pingback: suco emagrecedor
Pingback: halter neck
Pingback: evo 8 build
Pingback: does water help you lose weight
Pingback: czeromedia
Pingback: czeromedia
Pingback: fashion
Pingback: czeromedia
Pingback: evo recalls
Pingback: ajuda emagrecer
Pingback: cute bathing suit
Pingback: what's the best way to lose weight
Pingback: evo 9
Pingback: how to lose weight in your legs
Pingback: dicas para emagrecer rapido e com saude
Pingback: evo issues
Pingback: evo 9 turbo
Pingback: fastest way to lose weight in a month
Pingback: does yoga help lose weight
Pingback: blog
Pingback: evo 8 build
Pingback: evo 9 review
Pingback: evo x
Pingback: evo recalls
Pingback: dietas alimentares
Pingback: does adderall make you lose weight
Pingback: Women
Pingback: Beachwear
Pingback: teen
Pingback: mitsubishi evo
Pingback: losing weight after menopause
Pingback: lancer evo
Pingback: how fast can you lose weight
Pingback: emagrecer 8 kg em 4 meses
Pingback: mitsubishi
Pingback: how fast do you lose weight on wellbutrin
Pingback: evo 8 recalls
Pingback: czeromedia evo
Pingback: evo 9 review
Pingback: evo recalls
Pingback: Women
Pingback: tea to help lose weight
Pingback: dieta para emagrecer muito
Pingback: emagrecer 8 kg
Pingback: quit drinking lose weight
Pingback: evo
Pingback: Redmond exterminators
Pingback: evo review
Pingback: evo 9
Pingback: evo recalls
Pingback: how much weight can you lose in 3 months
Pingback: how much water should you drink to lose weight
Pingback: mitsubishi evo recalls
Pingback: tron cryptocurrency
Pingback: lancer evo
Pingback: emagrecer os braços
Pingback: evo 8 recalls
Pingback: sugar ants
Pingback: Noor system with ID number
Pingback: czeromedia
Pingback: evo review
Pingback: czeromedia
Pingback: how much walking to lose weight
Pingback: how to lose weight in 2 days
Pingback: evolution
Pingback: how to lose weight for men
Pingback: 1000hp evo
Pingback: losing weight for men
Pingback: how to lose weight in 2 days
Pingback: evo 8 recalls
Pingback: mitsubishi lancer
Pingback: evo 8 jdm
Pingback: lancer evo
Pingback: czeromedia evo
Pingback: evo 9 launch
Pingback: losing inches but not weight
Pingback: evo
Pingback: evo 9
Pingback: czeromedia evo
Pingback: mitsubishi evo recalls
Pingback: how to lose weight for men
Pingback: lose weight in 10 days
Pingback: evo 8 recalls
Pingback: evo 8 recalls
Pingback: evo review
Pingback: evo 9
Pingback: how to lose weight in two weeks
Pingback: evo 8 recalls
Pingback: evo 8 jdm
Pingback: evo 8 recalls
Pingback: how to lose weight during pregnancy
Pingback: lancer evo
Pingback: evo 9 review
Pingback: mitsubishi evo
Pingback: Sammamish exterminators
Pingback: evo 8 build
Pingback: how to lose weight in two weeks
Pingback: how to lose weight healthy
Pingback: best exercise to lose weight from stomach
Pingback: xp coin
Pingback: professional maids
Pingback: evo recalls
Pingback: mitsubishi evo recalls
Pingback: healthy diet plan to lose weight
Pingback: tuning
Pingback: how to lose weight in two weeks
Pingback: evo 8 turbo
Pingback: evo 9
Pingback: evo 9
Pingback: tuning
Pingback: evo 9
Pingback: mitsubishi lancer
Pingback: evo 8 jdm
Pingback: lose weight without dieting
Pingback: evo 9 launch
Pingback: mitsubishi evo
Pingback: evo 8 turbo
Pingback: how to lose baby weight
Pingback: czeromedia evo
Pingback: evo 8 recalls
Pingback: does lemon water help lose weight
Pingback: evo 9 review
Pingback: czeromedia
Pingback: evo issues
Pingback: evo
Pingback: mitsubishi
Pingback: evo 8 build
Pingback: tuning
Pingback: can i lose weight by walking
Pingback: losing weight in college
Pingback: what to eat before workout to lose weight
Pingback: czeromedia evo
Pingback: evo 8 review
Pingback: how much vitamin d should i take to lose weight
Pingback: does lemon water help you lose weight
Pingback: diet foods to lose weight fast
Pingback: evo x recalls
Pingback: evo 8 review
Pingback: affiliate marketing beginner training
Pingback: evo 8 turbo
Pingback: tuning
Pingback: how much weight do you lose overnight
Pingback: how to lose weight very fast
Pingback: evo 8 review
Pingback: ants control service
Pingback: evo review
Pingback: how much exercise to lose weight
Pingback: 1000hp evo
Pingback: disney park bag
Pingback: healthy lunch ideas for work to lose weight
Pingback: evo review
Pingback: evo issues
Pingback: how to lose weight in 4 easy steps
Pingback: evo x
Pingback: how to lose weight in 4 easy steps
Pingback: evo x recalls
Pingback: lancer evo
Pingback: evo review
Pingback: evo x recalls
Pingback: teens poncho
Pingback: evo 8 review
Pingback: lancer evo
Pingback: theme park accessories
Pingback: junior encyclopedia of animated characters
Pingback: evo 9 launch
Pingback: evo issues
Pingback: bitbelt for magic bands
Pingback: drawstring band backpack
Pingback: EXERCISE 101
Pingback: Best Diets
Pingback: plastic drawstring backpack
Pingback: kid poncho
Pingback: emergency rain poncho kids
Pingback: amusement park pack
Pingback: Dieting
Pingback: Dieting Does Not Equal Boring Food
Pingback: unisex rain poncho
Pingback: Fat to Fit
Pingback: family rain poncho
Pingback: Weight Loss Grants Scam
Pingback: Green Tea
Pingback: HEALTHY EATING
Pingback: How do you take Apple Cider Vinegar to lose weight
Pingback: Best Appetite Control Supplements
Pingback: Weight Loss Ideas
Pingback: Jasmine Tea
Pingback: Weight Loss Coaching
Pingback: How Fat is Created
Pingback: poncho backpack
Pingback: rain poncho
Pingback: chat gay
Pingback: plastic ponchos
Pingback: poncho hiking
Pingback: How to contact us
Pingback: chat gay
Pingback: The best way to publish your book
Pingback: adult ponchos
Pingback: How to become a successful writer
Pingback: How to contact us
Pingback: disney rain
Pingback: technology news
Pingback: rain kids poncho
Pingback: kids travel tray
Pingback: disposable poncho
Pingback: car tray for kids
Pingback: How to publish with us
Pingback: ponchos family pack disposable
Pingback: kids lap tray
Pingback: Latest news
Pingback: car toy organizer
Pingback: car activity tray
Pingback: car organizer for kids
Pingback: need chennai call boy agency
Pingback: ponchos family
Pingback: sleeves to cover arms for kids
Pingback: car organizer for kids
Pingback: car seat trays for toddlers
Pingback: How to contact us
Pingback: back seat organizer with tray
Pingback: cervical spondylosis
Pingback: mypillow
Pingback: car organizer for kids
Pingback: hunchback posture
Pingback: kids car travel tray
Pingback: car seat table
Pingback: rain poncho family pack
Pingback: dr recommended pillow
Pingback: kids travel tray
Pingback: Latest books
Pingback: car organizer for kids
Pingback: kids travel tray
Pingback: car toy organizer
Pingback: kids lap tray for car
Pingback: car travel bag organizer
Pingback: back seat pocket organizer
Pingback: back seat pocket organizer
Pingback: car seat tray
Pingback: car seat table
Pingback: back seat car tray
Pingback: hunchback posture
Pingback: arc4life pillow
Pingback: car back seat organzier
Pingback: car back seat organzier
Pingback: car activity tray
Pingback: chiropractic pillow
Pingback: neck pain
Pingback: back seat pocket organizer
Pingback: childs rain poncho
Pingback: car seat organizer tray
Pingback: kid rain poncho
Pingback: car organizer for kids
Pingback: car seat travel tray
Pingback: car seat tray for traveling
Pingback: kids travel tray back pack
Pingback: kids car travel tray
Pingback: Latest news
Pingback: car seat tray for traveling
Pingback: live premium channels
Pingback: back seat organizer with tray
Pingback: drawstring backpack for cheer
Pingback: back seat car tray
Pingback: kids car travel tray
Pingback: car seat travel bag
Pingback: kid ponchos
Pingback: How to design a book cover
Pingback: car toy organizer
Pingback: kids lap tray for car
Pingback: The best way to publish your book
Pingback: car organizer for kids
Pingback: back seat organizer with tray
Pingback: car seat table
Pingback: car seat tray
Pingback: kids lap tray for car
Pingback: Ristoranti bologna
Pingback: playlist promotion spotify
Pingback: car tray for kids
Pingback: car seat organizer tray
Pingback: car seat travel tray
Pingback: sluurpy
Pingback: live channels
Pingback: kids lap tray for car
Pingback: car seat tray
Pingback: back seat pocket organizer
Pingback: kids poncho disposable
Pingback: car seat trays for toddlers
Pingback: kids rain cover
Pingback: hong kong commercial register
Pingback: car back seat organzier
Pingback: car travel bag organizer
Pingback: kids rain ponchos
Pingback: back seat pocket organizer
Pingback: car seat travel bag
Pingback: rain panchos disposable
Pingback: kids car travel tray
Pingback: car seat trays for toddlers
Pingback: online newspaper
Pingback: car seat tray
Pingback: car seat organizer tray
Pingback: car seat tray
Pingback: disney rain poncho for kids
Pingback: new things
Pingback: kids lap tray for car
Pingback: car seat organizer tray
Pingback: kids car travel tray
Pingback: Ristoranti milano
Pingback: vsezame.si
Pingback: car toy organizer
Pingback: kids travel tray back pack
Pingback: car seat organizer tray
Pingback: car activity tray
Pingback: car toy organizer
Pingback: car seat travel bag
Pingback: car seat tray for traveling
Pingback: rain poncho for kids
Pingback: car seat trays for toddlers
Pingback: car seat tray
Pingback: car seat trays for toddlers
Pingback: car seat tray
Pingback: world news
Pingback: toners
Pingback: beauty blog
Pingback: emergency rain poncho with hood
Pingback: poncho backpack
Pingback: preppy beach lifestyle
Pingback: back seat car tray
Pingback: kids travel tray bag
Pingback: beach clothing
Pingback: back seat pocket organizer
Pingback: Ristoranti torino
Pingback: kids travel tray back pack
Pingback: car seat trays for toddlers
Pingback: kids travel tray back pack
Pingback: car seat travel bag
Pingback: car seat tray for traveling
Pingback: car activity tray
Pingback: kids car travel tray
Pingback: back seat pocket organizer
Pingback: kids lap tray for car
Pingback: cryptocurrency predictions
Pingback: inspire ft2
Pingback: exercise equipment
Pingback: car seat tray
Pingback: car seat tray for traveling
Pingback: car travel bag organizer
Pingback: back seat car tray
Pingback: car seat tray
Pingback: car seat organizer tray
Pingback: inspire ft2
Pingback: car seat trays for toddlers
Pingback: back seat pocket organizer
Pingback: Ristoranti napoli
Pingback: inspire ft2 home gym
Pingback: car seat travel tray
Pingback: kids lap tray
Pingback: back seat organizer with tray
Pingback: back seat organizer with tray
Pingback: Ristoranti parma
Pingback: no shortage of good days
Pingback: car seat tray
Pingback: kids car travel tray
Pingback: car seat travel bag
Pingback: mariner west
Pingback: kids travel tray back pack
Pingback: travel visa services
Pingback: car toy organizer
Pingback: inspire ft2
Pingback: Ristoranti palermo
Pingback: best home gym equipment
Pingback: best home workout equipment
Pingback: car seat trays for toddlers
Pingback: workout equipment
Pingback: car seat tray
Pingback: car seat tray
Pingback: Ristoranti roma
Pingback: home fitness equipment
Pingback: car seat travel bag
Pingback: car seat tray for traveling
Pingback: car toy organizer
Pingback: car seat organizer tray
Pingback: kids car travel tray
Pingback: back seat car tray
Pingback: best home gym equipment
Pingback: kids travel tray bag
Pingback: car seat travel tray
Pingback: car seat travel tray
Pingback: most comfortable clothes
Pingback: kids travel tray bag
Pingback: SunsetScreen
Pingback: the nautical
Pingback: car activity tray
Pingback: car seat trays for toddlers
Pingback: car travel bag organizer
Pingback: SunsetScreen
Pingback: car activity tray
Pingback: car seat trays for toddlers
Pingback: kids car travel tray
Pingback: car seat tray for traveling
Pingback: car seat travel tray
Pingback: link coin
Pingback: car seat travel tray
Pingback: back seat car tray
Pingback: car seat travel tray
Pingback: car toy organizer
Pingback: kids car travel tray
Pingback: redshift
Pingback: Painting Manawatu
Pingback: f.lux
Pingback: car seat travel bag
Pingback: car back seat organzier
Pingback: car seat organizer tray
Pingback: car seat tray
Pingback: kids travel tray bag
Pingback: kids car travel tray
Pingback: preppy fashion
Pingback: car seat organizer tray
Pingback: car seat tray for traveling
Pingback: back seat pocket organizer
Pingback: car seat travel tray
Pingback: Lancaster Kosmetik Erfahrungen
Pingback: back seat car tray
Pingback: car tray for kids
Pingback: kids lap tray for car
Pingback: car toy organizer
Pingback: kids lap tray
Pingback: car seat travel tray
Pingback: the nautical
Pingback: Parfum Bewertungen
Pingback: car activity tray
Pingback: Painting Manawatu
Pingback: car seat travel tray
Pingback: car tray for kids
Pingback: Molton Brown Pflege Test
Pingback: back seat pocket organizer
Pingback: car seat travel tray
Pingback: Missha Kosmetik Test
Pingback: Easycosmetic Bewertungen
Pingback: car organizer for kids
Pingback: car back seat organzier
Pingback: car seat table
Pingback: car seat tray
Pingback: car seat organizer tray
Pingback: web design
Pingback: car seat tray
Pingback: car seat table
Pingback: web design
Pingback: kids lap tray
Pingback: car seat tray
Pingback: kids travel tray
Pingback: PC
Pingback: car seat trays for toddlers
Pingback: car seat trays for toddlers
Pingback: kids car travel tray
Pingback: busty escorts London
Pingback: computer
Pingback: car seat tray for traveling
Pingback: kids travel tray back pack
Pingback: west coast prep
Pingback: car tray for kids
Pingback: car organizer for kids
Pingback: back seat car tray
Pingback: builder manawatu
Pingback: kids lap tray
Pingback: back seat organizer with tray
Pingback: car tray for kids
Pingback: back seat pocket organizer
Pingback: kids travel tray bag
Pingback: back seat pocket organizer
Pingback: kids travel tray back pack
Pingback: car seat table
Pingback: car seat organizer tray
Pingback: community newspaper
Pingback: back seat organizer with tray
Pingback: car seat travel bag
Pingback: arts
Pingback: blue orange pelican
Pingback: affordable hosting
Pingback: orange blue pelican
Pingback: international escorts
Pingback: sailing clothes
Pingback: website hosting
Pingback: sound machine
Pingback: south wales
Pingback: mp3 player with speaker
Pingback: baby shower gift
Pingback: touch lamp
Pingback: baby gifts
Pingback: personalized wall decals
Pingback: butterfly wall decals
Pingback: portable night light speaker
Pingback: decals?
Pingback: Plumbing manawatu
Pingback: touch lamp
Pingback: hurricane-shutter-tracks-and-headers
Pingback: portable night light
Pingback: wall quotes?
Pingback: desk light
Pingback: girls wall decals
Pingback: superhero wall decals
Pingback: custom wall stickers
Pingback: 2-25-bertha-h-header-4-build-out-sizes/
Pingback: sound machine
Pingback: bluetooth night light
Pingback: night light for kids
Pingback: touch lamp
Pingback: desk lamp
Pingback: panelmate-pro-screw-anchors-bag-of-100/
Pingback: girls wall decals
Pingback: child night light
Pingback: wall stickers for bedrooms?
Pingback: touch night light
Pingback: hurricane-shutter-tracks-and-headers
Pingback: kitchen wall decals
Pingback: safari Kenya
Pingback: sound machine
Pingback: desk light
Pingback: personalized wall decals
Pingback: dinner date escorts london
Pingback: baby gifts
Pingback: portable bluetooth night light
Pingback: portable night light
Pingback: studded-angle-with-studs-every-6-on-center/
Pingback: disney wall decals
Pingback: desk lamp
Pingback: portable night light
Pingback: washered-wingnuts
Pingback: sound machine
Pingback: wireless night light
Pingback: bluetooth night light
Pingback: Summary
Pingback: desk light
Pingback: portable night light speaker
Pingback: sound machine
Pingback: Summary
Pingback: desk lamp
Pingback: ebook download sites
Pingback: Summary
Pingback: night light speaker
Pingback: custom wall decals
Pingback: studded-angle-with-studs-every-6-on-center/
Pingback: Summary
Pingback: combination-sidewalk-bolts-bag-of-100/
Pingback: Kenya Safari
Pingback: Anchor: wall decoration
Pingback: desk lamp
Pingback: Summary
Pingback: washered-wingnuts
Pingback: desk light
Pingback: Anchor: wall decoration
Pingback: Anchor: wall decoration
Pingback: Anchor: wall decoration
Pingback: Summary
Pingback: Anchor: wall decoration
Pingback: Anchor: wall decoration
Pingback: Bandar Bola Piala Dunia Judi LiveCasino Sbobet 338a Online CGOAsia
Pingback: overnight escorts london
Pingback: Anchor: wall decoration
Pingback: 10906
Pingback: wall dcor
Pingback: 10906
Pingback: 10906
Pingback: wall stickers
Pingback: horse wall decals
Pingback: wall graphics
Pingback: science fiction movies
Pingback: romance movies
Pingback: wildlife safari
Pingback: 10906
Pingback: 10906
Pingback: wall mural decal
Pingback: western movies
Pingback: 10906
Pingback: Infinity War movie release
Pingback: Rampage movie release
Pingback: 10906
Pingback: wall stickers for bedrooms?
Pingback: wall mural decal
Pingback: London escorts
Pingback: decal stickers?
Pingback: Alien Covenant movie release
Pingback: fantasy
Pingback: wall stickers for bedrooms?
Pingback: mistery movies
Pingback: 10906
Pingback: Bandar Bola Piala Dunia Judi LiveCasino Sbobet 338a Online CGOAsia
Pingback: dumpster rental Portage
Pingback: upcoming movies
Pingback: animation movies
Pingback: current movie releases
Pingback: dumpster rental westmont
Pingback: dumpster rental Merrionette Park
Pingback: kenya tours
Pingback: roll off dumpster
Pingback: dumpster rental plano
Pingback: dumpster rental norridge
Pingback: dumpster rental plainfield
Pingback: dumpster rental bedford park
Pingback: something whisky mejor compra en bogota
Pingback: compra whisky en colombia
Pingback: La mejor tienda de whisky en colombia
Pingback: compra whisky en bogota
Pingback: horror movies
Pingback: trash disposal
Pingback: residential dumpster rental
Pingback: mat bang La Cosmo
Pingback: dumpsters rental
Pingback: compra whisky en colombia
Pingback: 2 yard dumpster
Pingback: garbage removal
Pingback: mejor tienda de whisky en bogota
Pingback: drama movies
Pingback: compra whisky en la mejor tienda colombia
Pingback: courses
Pingback: medical
Pingback: macallan de los mejores whiskies en colombia
Pingback: whisky de malta para regalo bogota
Pingback: macallan whisky fino en bogota
Pingback: compra jack daniels colombia
Pingback: chivas 25 el mejor whisky en whisky lord
Pingback: scholarships
Pingback: dumpsters rental
Pingback: whisky royal salute colombia compra
Pingback: rent a roll off dumpster
Pingback: compra whisky precio bogota
Pingback: best safari in Africa
Pingback: 20 yard dumpster cost
Pingback: compra old parr whisky precio bogota
Pingback: rent a trash dumpster
Pingback: construction dumpster rental cost
Pingback: whisky royal salute colombia compra
Pingback: dumpster roll off
Pingback: dumpster dimensions
Pingback: du an La Cosmo
Pingback: concrete dumpster
Pingback: historia del whisky en el mundo
Pingback: whisky premim regalo en colombia
Pingback: compra el mejor buchanans precio bogota
Pingback: glenfiddich 15 single malt whisky
Pingback: university
Pingback: trash dumpsters for rent
Pingback: johnnie walker compra en colombia
Pingback: whisky en colombia
Pingback: dumpsters near me
Pingback: compra whisky precio bogota
Pingback: Whisky para el dia del padre
Pingback: buy junk cars
Pingback: compra whisky en colombia
Pingback: compra el mejor buchanans precio bogota
Pingback: cash for cars Pittsburgh
Pingback: scrap your car for cash
Pingback: top dollar for junk cars
Pingback: whisky premim regalo en colombia
Pingback: Popsocket phone mount
Pingback: engineering
Pingback: tree wall decal
Pingback: 60
Pingback: wall quotes
Pingback: wall decor
Pingback: wall stickers
Pingback: african safari tours
Pingback: wall letters stickers
Pingback: local scrap car buyers
Pingback: Link: https://www.instagram.com/primedecals/
Pingback: buy old junk cars
Pingback: wall sticker quotes
Pingback: cash for scrap
Pingback: wall decoration
Pingback: need to sell my junk car
Pingback: decal stickers
Pingback: Worldinvest ICO
Pingback: tree wall decal
Pingback: 61
Pingback: sell my junk truck
Pingback: who pays for junk cars
Pingback: wall letter decals
Pingback: wall sticker quotes
Pingback: tree wall decal
Pingback: 60
Pingback: wall stencils?
Pingback: chat gratuita senza registrazione
Pingback: videochat per donne
Pingback: cam chat
Pingback: Five Things Dogs Like and Love You to Do
Pingback: 60
Pingback: Doctor
Pingback: Anyone Can Become Knowledgeable About rottweilers With These Easy Tips - Rottweiler Life
Pingback: The Red Rottweiler & Other Rare Rottweilers - Rottweiler Life
Pingback: Wolfgang Halbig
Pingback: Bite Archives - Rottweiler Life
Pingback: Rottweiler – Rottweiler Life
Pingback: where can i sell my car for scrap
Pingback: Rottweiler Life - rottweiler, rottweiler book, rottweiler puppy
Pingback: wall decor
Pingback: tree wall decal
Pingback: Kennel Submit - Rottweiler Life
Pingback: Found at:
Pingback: Rottweiler Saves Boy From Severe Pit Bull Attack Near Orlando - Rottweiler Life
Pingback: 10 Things Dogs Hate about Their Owners
Pingback: decals
Pingback: 61
Pingback: Three Ways Rottweilers Say "I love you"
Pingback: 60
Pingback: chatto
Pingback: History Facts Your Rottweiler Wants You to Know Rottweiler Life - rottweiler, rottweiler facts, rottweiler puppy
Pingback: the Dog Breed That Can’t Bark!
Pingback: 10 Things Dogs Hate about Their Owners
Pingback: Rottweiler Organization Donate
Pingback: rottweiler diseases Archives - Rottweiler Life
Pingback: 57
Pingback: sauna heater
Pingback: Rottweiler Archives - Page 12 of 19 - Rottweiler Life
Pingback: electric sauna heater
Pingback: 60
Pingback: webchat
Pingback: chat free
Pingback: chattare gratis
Pingback: Family of Rottweilers save life of lost 80 year-old woman - Rottweiler Life
Pingback: Fleas and Ticks Archives - Rottweiler Life
Pingback: 60
Pingback: live Archives - Rottweiler Life
Pingback: video chat per incontri
Pingback: Free E-Books - Rottweiler Life
Pingback: sticker wallpaper
Pingback: Rottweiler Archives - Rottweiler Life
Pingback: infrared sauna safety
Pingback: disney wall decals
Pingback: All Breed Archives - Page 16 of 17 - Rottweiler Life
Pingback: ¿è©±ï½/dsc_1586/
Pingback: digging Archives - Rottweiler Life
Pingback: sticker wallpaper
Pingback: portable dry sauna
Pingback: self adhesive wallpaper https://www.youtube.com/watch?v=MCJw5YENsFA
Pingback: home sauna units
Pingback: 60
Pingback: sauna room benefits
Pingback: Rottweiler Found With Nose and Ears Severed Has Been Adopted! UPDATE
Pingback: buy a sauna for your home
Pingback: video chat
Pingback: wall quotes
Pingback: videochat per incontri
Pingback: far infrared benefits
Pingback: decals
Pingback: wall stencils?
Pingback: 60
Pingback: mistakes Archives - Rottweiler Life
Pingback: сhаrасtеrіѕtісѕ оf rоttwеіlеrѕ
Pingback: ihealth sauna for sale
Pingback: sticker wallpaper
Pingback: decals?
Pingback: Dog Pregnancy Tips
Pingback: indoor dry sauna
Pingback: 4 - Rottweiler Life
Pingback: steam sauna home
Pingback: best women multivitamin
Pingback: Fitness watches for women
Pingback: best whey protein brand
Pingback: 60
Pingback: wallpaper for walls
Pingback: sticker wallpaper
Pingback: 60
Pingback: decals
Pingback: 60
Pingback: Best sports watches for men
Pingback: vinyl decals
Pingback: Rottweiler Life - Secrets You Don`t Know About Rottweiler - Page 20
Pingback: 65 wall quotes https://www.youtube.com/channel/UC-pipeloS9dmghPKK623M6Q
Pingback: Treadmill for sale near me
Pingback: cerita bokep
Pingback: best treadmill for running
Pingback: 1 person sauna kits
Pingback: 65 sticker wallpaper https://www.youtube.com/watch?v=p-Bdks2IVFg
Pingback: infrared sauna brands
Pingback: cerita dewasa
Pingback: cerita dewasa
Pingback: 65 self adhesive wallpaper https://www.youtube.com/watch?v=EFF1mULODps
Pingback: indoor dry sauna
Pingback: cerita sex
Pingback: 65 wall decor https://www.youtube.com/channel/UC-pipeloS9dmghPKK623M6Q
Pingback: cerita panas
Pingback: --------
Pingback: Anchor: removalble wallpaper
Pingback: 60 wall decor https://www.youtube.com/watch?v=p-Bdks2IVFg
Pingback: near infrared sauna for sale
Pingback: world map wall decals
Pingback: best treadmill for home use
Pingback: cerita sex
Pingback: 65 decals https://www.youtube.com/watch?v=98Sp8ZJxpFg
Pingback: wall letters stickers
Pingback: cerita dewasa
Pingback: wall quotes?
Pingback: Treadmill for sale near me
Pingback: sauna
Pingback: best infrared sauna
Pingback: 65 decal stickers https://www.youtube.com/watch?v=wny7j2vN9x4
Pingback: Anchor: wall paper decal
Pingback: cerita hot
Pingback: best treadmill for home use
Pingback: fir sauna
Pingback: 65 decals https://www.youtube.com/watch?v=98Sp8ZJxpFg
Pingback: 66 sticker wallpaper https://rainriverponcho.com/products/rain-river-poncho-disposable-rain-poncho-emergency-family-8-pack-extra-thick-1
Pingback: cerita mesum
Pingback: near infrared sauna for sale
Pingback: 65 wallpaper for walls https://www.youtube.com/watch?v=EFF1mULODps
Pingback: cerita hot
Pingback: 65 walls need love https://www.youtube.com/channel/UC-pipeloS9dmghPKK623M6Q
Pingback: best treadmill for home use
Pingback: life fitness treadmill
Pingback: cerita mesum
Pingback: how to live a healthy lifestyle
Pingback: 65 sticker wallpaper https://www.youtube.com/watch?v=-kkMhxFUS8k
Pingback: 65 vinyl decals https://www.youtube.com/watch?v=ShBFX6Zk9uM
Pingback: cerita mesum
Pingback: head lamp
Pingback: detik sport
Pingback: camping gear
Pingback: hardhat headlamp
Pingback: 65 temporary wall paper https://www.youtube.com/watch?v=-kkMhxFUS8k
Pingback: hiking headlamp
Pingback: carbon fiber sauna
Pingback: sauna design
Pingback: 65 wall decor https://www.youtube.com/watch?v=oqNrBg9_Qno
Pingback: cataracts in dogs
Pingback: home sauna units
Pingback: Symptoms and Effective Treatment for Dog Cataracts
Pingback: waterproof headlamp
Pingback: 62 decals https://www.youtube.com/watch?v=wny7j2vN9x4
Pingback: Various types of Cataracts in Dohs and their treatment
Pingback: lamparas recargables
Pingback: indoor home sauna
Pingback: spa infrared sauna
Pingback: led lenser headlamp
Pingback: 65 sticker wallpaper https://www.youtube.com/watch?v=jr8Vc50MRBU
Pingback: 65 vinyl decals https://www.youtube.com/watch?v=-EETC4bX-UM
Pingback: led lenser headlamp
Pingback: head torch
Pingback: 65 vinyl decals https://www.youtube.com/watch?v=-EETC4bX-UM
Pingback: headlamp flashlight
Pingback: Anchor: sticker wallpaper
Pingback: 65 wallpaper for walls https://rainriverponcho.com
Pingback: led headlamps
Pingback: camping headlamp
Pingback: sticker wallpaper?
Pingback: hemlock infrared sauna
Pingback: led headlamps
Pingback: infrared sauna to buy
Pingback: 65 sticker wallpaper https://www.youtube.com/watch?v=oqNrBg9_Qno
Pingback: wall sayings
Pingback: led headlight
Pingback: cerita sex
Pingback: head flashlights led
Pingback: hardhat headlamp
Pingback: wall sayings
Pingback: hard hat headlamp
Pingback: 66 vinyl decals https://rainriverponcho.com/products/rain-river-poncho-disposable-rain-poncho-emergency-family-8-pack-extra-thick-1
Pingback: butterfly wall decals
Pingback: 65 wall paper decal https://www.youtube.com/watch?v=XZyEE0XCIP8
Pingback: lamparas recargables
Pingback: 65 wall quotes https://www.etsy.com/shop/TrendyWallDesigns?ref=search_shop_redirect
Pingback: headlamps xtreme bright
Pingback: 62 wall decor https://rainriverponcho.com
Pingback: 100% original brand
Pingback: Womens Vintage
Pingback: camping light
Pingback: hiking gear
Pingback: led headlamps
Pingback: head lamp 10000lumen
Pingback: Used Item
Pingback: vinyl wall quotes
Pingback: head flashlights led
Pingback: cerita bokep
Pingback: girls wall decals
Pingback: 100% original brand
Pingback: headlamp led
Pingback: camping headlamp
Pingback: 65 walls need love https://rainriverponcho.com/products/rain-river-poncho-disposable-rain-poncho-emergency-family-8-pack-extra-thick-1
Pingback: camping equipment
Pingback: hiking headlamp
Pingback: wall letters stickers
Pingback: 63 wall quotes https://www.youtube.com/watch?v=3saCSKYfEbE
Pingback: head flashlights led
Pingback: rechargeable flashlights high lumens
Pingback: hiking gear
Pingback: head lights
Pingback: head lamps for adults
Pingback: 10906
Pingback: tactical headlamp
Pingback: womens tshirt fashion
Pingback: mens tshirt fashion
Pingback: Summary
Pingback: 10906
Pingback: head flashlights led
Pingback: camping light
Pingback: Second Hand Clothes
Pingback: camping lights
Pingback: Summary
Pingback: 10906
Pingback: 100% original brand
Pingback: used clothing
Pingback: 10906
Pingback: 10906
Pingback: led headlamp
Pingback: decals?
Pingback: Anchor: wall decoration
Pingback: head lights
Pingback: Summary
Pingback: rechargeable headlamp led
Pingback: helmet light
Pingback: wall sayings
Pingback: tree wall decal?
Pingback: hard hat headlamp
Pingback: 10906
Pingback: camping gear
Pingback: helmet flashlight
Pingback: Deck Department
Pingback: Spa Attendant
Pingback: led headlamp
Pingback: world map wall decals
Pingback: Shore Excursions
Pingback: helmet light
Pingback: Anchor: wall decoration
Pingback: Musician
Pingback: Summary
Pingback: led head lamp
Pingback: camping supplies
Pingback: wall stencils?
Pingback: wall letter decals
Pingback: camping supplies
Pingback: led head lamp
Pingback: hiking headlamp
Pingback: california rottweiler rescue
Pingback: Manicurist
Pingback: puppy cries all night
Pingback: rechargeable headlamp led
Pingback: hard hat headlamp
Pingback: headlights led
Pingback: Food & Beverage
Pingback: led head lamp
Pingback: head flashlights led
Pingback: extra large dog toys
Pingback: Photographer
Pingback: HR Manager
Pingback: dog is wheezing and shaking
Pingback: Hotel Utility
Pingback: stop puppy biting
Pingback: Malisa Shrum
Pingback: Leora Adkisson
Pingback: Lakeisha Riney
Pingback: puppy dew claws
Pingback: Chief Electrician
Pingback: Executive Chef
Pingback: Inocencia Blaker
Pingback: bike trainer
Pingback: Bunny Benard
Pingback: Idell Rodrigues
Pingback: Sylvester Alvord
Pingback: best buy bike
Pingback: Hostess
Pingback: rottweiler puppies mn
Pingback: Maria Mattioli
Pingback: Jessenia Beede
Pingback: puppy injections
Pingback: Sidney Veit
Pingback: Assistant Shop Manager
Pingback: Sherrill Zabel
Pingback: Deck Cadet
Pingback: german commands for dogs
Pingback: bike trainer
Pingback: Leila Sandor
Pingback: how do you stop a puppy from biting
Pingback: Teofila Yetman
Pingback: rottweiler fights pitbull
Pingback: american rottweiler puppies
Pingback: Alyce Lemus
Pingback: Deckhand
Pingback: tough chew dog toys
Pingback: german shepherd training commands
Pingback: Aletha Lish
Pingback: brothers complete advanced allergy care
Pingback: Tracie Brinkley
Pingback: Katelin Vanzile
Pingback: Assistant Casino Manager
Pingback: height weight photo chart
Pingback: Nery Gail
Pingback: Katelin Vanzile
Pingback: All natural pads
Pingback: indiana rottweiler rescue
Pingback: female puppy bumps on private area
Pingback: Katelin Vanzile
Pingback: Organic tampon
Pingback: Anastacia Griest
Pingback: Zack Voris
Pingback: bike trainer
Pingback: Keeley Frederic
Pingback: Trinity Wilderman
Pingback: Felisha Laduke
Pingback: Gillian Pintor
Pingback: Jenise Pero
Pingback: hot deal bike
Pingback: Aletha Lish
Pingback: Lawanda Billick
Pingback: canine heart attack
Pingback: Toxic shock syndrome
Pingback: AED MACHINE
Pingback: rottweiler puppies rescue
Pingback: puppy play biting and growling
Pingback: Chrissy Bowlby
Pingback: puppy spayed recovery
Pingback: Marcella Cogburn
Pingback: puppy limping but not in pain
Pingback: rottweiler puppy growth chart
Pingback: parvovirus symptoms in puppies
Pingback: Trinity Wilderman
Pingback: rottweiler mating
Pingback: puppy shot schedule
Pingback: Kaila Brockman
Pingback: big dog chew toys
Pingback: Brigitte Opp
Pingback: how to potty train a girl puppy
Pingback: panty liners always
Pingback: Tiny Dahle
Pingback: photos of a dew claw on dogs
Pingback: bottle feeding newborn puppies
Pingback: common dog diseases and symptoms
Pingback: rottweiler facts
Pingback: Toxic shock syndrome
Pingback: rottweiler ears
Pingback: CPR
Pingback: Vi Mcspadden
Pingback: Latoya Kollar
Pingback: panty liners always
Pingback: panty liners always
Pingback: Raphael Pease
Pingback: AED MACHINE
Pingback: panty liners always
Pingback: bright led
Pingback: lamparas recargables
Pingback: rechargeable headlamp
Pingback: buy supplements
Pingback: buy protein powder
Pingback: head flashlights led
Pingback: best value protein powder
Pingback: hiking gear
Pingback: head lights led
Pingback: super bright led
Pingback: b12 shots
Pingback: herbal supplements
Pingback: camping equipment
Pingback: head flashlight
Pingback: camping light
Pingback: waterproof headlamp
Pingback: head lamps
Pingback: head lights
Pingback: camping supplies
Pingback: head light
Pingback: hard hat light
Pingback: hiking gear
Pingback: tactical headlamp
Pingback: hiking headlamp
Pingback: hiking gear
Pingback: hiking gear
Pingback: led headlamp
Pingback: headlamp led
Pingback: waterproof headlamp
Pingback: driving ranges near me
Pingback: titanium sunglasses
Pingback: rechargeable headlamp led
Pingback: hard hat light
Pingback: Engine Department
Pingback: best lean protein
Pingback: health supplements capsules
Pingback: Amazon Web Service Blog
Pingback: cree headlamp
Pingback: cheap vitamins
Pingback: led headlamps
Pingback: turbo exhaust clamp
Pingback: front mount turbo
Pingback: lean muscle protein powder
Pingback: Plumber
Pingback: Pool Attendant
Pingback: best protein supplement in india
Pingback: led headlight
Pingback: head torch
Pingback: radiator with engine oil cooler
Pingback: corvette intercooler
Pingback: HONR Network
Pingback: Fitness Instructor
Pingback: camping supplies
Pingback: Chief Communication
Pingback: headlights led
Pingback: waterproof headlamp
Pingback: Cruise Ship Jobs
Pingback: head lights led
Pingback: helmet light
Pingback: headlamps for camping
Pingback: HONR Network
Pingback: Move In Cleaning Frisco TX
Pingback: led head lamp
Pingback: Land Based
Pingback: led head light
Pingback: Assistant Hotel Manager
Pingback: Maid Services Near Me
Pingback: headlight flashlight
Pingback: hard hat light
Pingback: Cleaning Company Frisco
Pingback: IT Department
Pingback: Amazon Web Services Forum
Pingback: led head lamp
Pingback: what is an intercooler
Pingback: HONR Network
Pingback: free robux
Pingback: tactical headlamp
Pingback: free robux
Pingback: 2.5 exhaust band clamp
Pingback: helmet flashlight
Pingback: HONR Network
Pingback: free robux for roblox
Pingback: led lenser headlamp
Pingback: free robux
Pingback: HONR Network
Pingback: led headlamps
Pingback: air to air vs air to water intercooler
Pingback: head lamps for adults
Pingback: headlamp flashlight
Pingback: hiking gear
Pingback: headlamp rechargeable
Pingback: free robux
Pingback: HONR Network
Pingback: headlamp rechargeable
Pingback: headlamp rechargeable
Pingback: HONR Network
Pingback: Cleaning Contractors Near Me
Pingback: led headlamps
Pingback: Cleaning Contractors Frisco TX
Pingback: wheels and tyres uk
Pingback: go to the link
Pingback: lenso wheels south africa
Pingback: headlamp led
Pingback: headlights led
Pingback: lamparas recargables
Pingback: madmotors co uk
Pingback: headband light
Pingback: sites like 123movies
Pingback: axe alloys uk
Pingback: mucus plug
Pingback: alternatives for solarmovie
Pingback: Amazon Web Services Business Directory
Pingback: sites like 123movies
Pingback: Check More Here
Pingback: Move In Cleaning Frisco TX
Pingback: alloy wheels online
Pingback: purpose of intercooler in turbocharger
Pingback: rechargeable flashlights high lumens
Pingback: tyres online uk
Pingback: cheap tyres for sale uk
Pingback: headlights led
Pingback: HONR Network
Pingback: how can i make money online 2018
Pingback: head lamp
Pingback: buy car mods
Pingback: rechargeable flashlights high lumens
Pingback: vehicle tyre
Pingback: headlamp flashlight
Pingback: Get Complete Info
Pingback: head lights
Pingback: head flashlight
Pingback: led head lamp
Pingback: HONR Network
Pingback: cheap car tyre deals
Pingback: Centerpiece
Pingback: bright led
Pingback: rechargeable headlamp
Pingback: led head lamp light
Pingback: head lights led
Pingback: uk tyres direct
Pingback: waterproof headlamp
Pingback: head flashlight
Pingback: tyre search by vehicle
Pingback: best way to make money online 2018
Pingback: headlamps for camping
Pingback: head lamp led rechargeable
Pingback: HONR Network
Pingback: head lamp led rechargeable
Pingback: head lamp led rechargeable
Pingback: super bright led
Pingback: hard hat light
Pingback: head flashlight
Pingback: cxracing intercooler piping
Pingback: alloy wheels direct
Pingback: head lamps
Pingback: alloy wheels direct
Pingback: cree headlamp
Pingback: Amazon Web Services Certification Groups
Pingback: alloy wheel manufacturers uk
Pingback: car engine cooling system pdf
Pingback: headlamp led
Pingback: Managerial Economics Tutorial
Pingback: headlight flashlight
Pingback: helmet flashlight
Pingback: rechargeable headlamp led
Pingback: ETL Testing Tutorial
Pingback: hard hat headlamp
Pingback: Web Service Testing Tutorial
Pingback: led headlamp rechargeable
Pingback: Pharmacology Tutorial
Pingback: cree headlamp
Pingback: Advertising Management Tutorial
Pingback: golf training
Pingback: hiking headlamp
Pingback: Data Warehouse ETL Toolkit Tutorial
Pingback: head lamps for adults
Pingback: free robux
Pingback: free robux
Pingback: ITIL Concepts Tutorial
Pingback: dodge neon srt 4 intercooler piping
Pingback: led head light
Pingback: Management Hotel Tutorial
Pingback: camping lights
Pingback: head lights
Pingback: white sex dolls
Pingback: HONR Network
Pingback: quality sex dolls
Pingback: HONR Network
Pingback: head lamp
Pingback: VBA For Excel Tutorial
Pingback: Sales Management Tutorial
Pingback: head lamp
Pingback: best sex dolls
Pingback: headlamps xtreme bright
Pingback: how to get free robux
Pingback: HONR Network
Pingback: JVM Tutorial
Pingback: alternatives to piratebay
Pingback: camping lights
Pingback: HONR Network
Pingback: head lamps
Pingback: lamparas recargables
Pingback: head light
Pingback: IBM-JCL Tutorial
Pingback: helmet flashlight
Pingback: HONR Network
Pingback: free robux for roblox
Pingback: Get Complete Info
Pingback: GSM Tutorial
Pingback: Local SEO Agency Toronto
Pingback: Research Methodology Tutorial
Pingback: headlamps for camping
Pingback: terminierung
Pingback: Javascript Objects Tutorial
Pingback: Hibernate Tutorial
Pingback: contentpflege
Pingback: bolero slx price
Pingback: Working Capital Management Tutorial
Pingback: Strategic Management Tutorial
Pingback: HONR Network
Pingback: led headlamps
Pingback: led head lamp
Pingback: camping supplies
Pingback: Django Tutorial
Pingback: head lamp 10000lumen
Pingback: zen spin
Pingback: leadgenerierung
Pingback: luxury sex dolls
Pingback: rechargeable headlamp led
Pingback: rechargeable flashlights high lumens
Pingback: head lamps for adults
Pingback: HONR Network
Pingback: hiking gear
Pingback: Angular 2 Tutorial
Pingback: lemforder ball joint
Pingback: Statistics Tutorial
Pingback: HONR Network
Pingback: waterproof headlamp
Pingback: datenbankaufbau
Pingback: mahindra tourister price
Pingback: bright led
Pingback: leadgenerierung
Pingback: how does a water to air intercooler work
Pingback: headlamps for camping
Pingback: head flashlights led
Pingback: bmw730i
Pingback: Wi-Fi Tutorial
Pingback: Local SEO Agency Toronto
Pingback: Java XML Tutorial
Pingback: maruti alto k10 accessories price list
Pingback: head lamp 10000lumen
Pingback: headlamp flashlight
Pingback: Backbone.js Tutorial
Pingback: HONR Network
Pingback: Apache Storm Tutorial
Pingback: contentpflege
Pingback: R Programming language Tutorial
Pingback: hard hat light
Pingback: kundenhotline
Pingback: Unittest Framework Tutorial
Pingback: SAP Webi Tutorial
Pingback: telefonservices
Pingback: head lamp
Pingback: Apache Kafka Tutorial
Pingback: HONR Network
Pingback: info autoradio gps
Pingback: terminierung
Pingback: autoradio-gps
Pingback: site autoradio gps
Pingback: autoradio gps direct
Pingback: WebGL Tutorial
Pingback: hardhat headlamp
Pingback: led head lamp light
Pingback: daten-contentservice
Pingback: super bright led
Pingback: camping headlamp
Pingback: autoradio 2018
Pingback: HONR Network
Pingback: Local SEO Scarborough
Pingback: Microwave Engineering Tutorial
Pingback: led headlamps
Pingback: Twitter Marketing Tutorial
Pingback: led lenser headlamp
Pingback: Computer Logical Organization Tutorial
Pingback: Din Rail Switched Mode PS
Pingback: i-Mode Tutorial
Pingback: Biometrics Tutorial
Pingback: headlamps for camping
Pingback: WAP Tutorial
Pingback: OpenNLP Tutorial
Pingback: head headlight
Pingback: autoradio 2018
Pingback: HONR Network
Pingback: direct autoradio gps
Pingback: camping lights
Pingback: hiking headlamp
Pingback: WML Tutorial
Pingback: A/B Testing Tutorial
Pingback: Human Computer Interface Tutorial
Pingback: Accounting Basics Tutorial
Pingback: headlights led
Pingback: suzuki swift suspension
Pingback: XML DOM Tutorial
Pingback: led head light
Pingback: Unix/Linux Tutorial
Pingback: skoda octavia front grill
Pingback: led headlamp
Pingback: autoradio gps info
Pingback: maruthi swift petrol
Pingback: Formula One Tutorial
Pingback: head headlight
Pingback: camping headlamp
Pingback: Workplace Stress Tutorial
Pingback: led headlamp
Pingback: led headlamp rechargeable
Pingback: waterproof headlamp
Pingback: HONR Network
Pingback: Job Search Skills Tutorial
Pingback: led head lamp
Pingback: head lamps
Pingback: camping headlamp
Pingback: HONR Network
Pingback: cree headlamp
Pingback: Jesey City Exterminator
Pingback: led head light
Pingback: Karate Tutorial
Pingback: Impromptu Speaking Tutorial
Pingback: hiking gear
Pingback: Web Services Tutorial For Beginners
Pingback: Jahanpanah Fort, Delhi Tutorial
Pingback: bitcoin sverige
Pingback: head torch
Pingback: rechargeable flashlights high lumens
Pingback: headlights led
Pingback: headlamp led
Pingback: E-Commerce Concepts Tutorial For Beginners
Pingback: Professional Ethics Tutorial
Pingback: helmet flashlight
Pingback: hardhat headlamp
Pingback: Internet Technologies Tutorial
Pingback: Organizational Design Tutorial
Pingback: led head lamp
Pingback: earn bitcoin
Pingback: Attention Management Tutorial
Pingback: Gwalior Fort, Gwalior Tutorial
Pingback: led head lamp
Pingback: head headlight
Pingback: helmet flashlight
Pingback: maruti eeco van diesel
Pingback: bright led
Pingback: Global Money Markets Tutorial For Beginners
Pingback: rechargeable headlamp
Pingback: camping light
Pingback: head lights
Pingback: General Knowledge Tutorial For Beginners
Pingback: opel astra engine parts
Pingback: HONR Network
Pingback: head torch
Pingback: Corporate Governance and Business Ethics Tutorial For Beginners
Pingback: kryptogenex sweden
Pingback: Computer Fundamentals Tutorial For Beginners
Pingback: Toko Online Palsu
Pingback: SAP ABAP Web Dynpro Tutorial For Beginners
Pingback: HONR Network
Pingback: poker online
Pingback: judi togel terpercaya
Pingback: head flashlight
Pingback: HONR Network
Pingback: head headlight
Pingback: HONR Network
Pingback: File Maker Tutorial For Beginners
Pingback: Principles of Management Tutorial For Beginners
Pingback: Best Poker Website in Town
Pingback: helmet flashlight
Pingback: agen taruhan judi bola
Pingback: sports betting tips
Pingback: Network Security Tutorial For Beginners
Pingback: hard hat headlamp
Pingback: second hand honda city in mumbai
Pingback: sports betting tips
Pingback: Marketing Management Tutorial For Beginners
Pingback: HONR Network
Pingback: rechargeable headlamp
Pingback: SAP HR Tutorial For Beginners
Pingback: Poker Online Uang Asli
Pingback: headlamps xtreme bright
Pingback: IBM DB2 Tutorial For Beginners
Pingback: Share Point 2010 Tutorial For Beginners
Pingback: waterproof headlamp
Pingback: chevrolet optra elite
Pingback: F Sharp (programming language) Tutorial For Beginners
Pingback: VascuWave
Pingback: VascuWave
Pingback: camping light
Pingback: TurboGears Tutorial For Beginners
Pingback: Agen SBOBET Resmi
Pingback: hard hat light
Pingback: Document Type Definition (DTD) Tutorial For Beginners
Pingback: rechargeable headlamp
Pingback: poker online tips
Pingback: helmet light
Pingback: Pay Per Click (PPC) Tutorial For Beginners
Pingback: alto 800 price in chennai
Pingback: headlight flashlight
Pingback: head flashlights led
Pingback: Mobile Security Tutorial For Beginners
Pingback: Situs Poker Online Penipu
Pingback: HONR Network
Pingback: head flashlight
Pingback: MATLAB Tutorial For Beginners
Pingback: CakePHP Tutorial For Beginners
Pingback: camping lights
Pingback: head lamp 10000lumen
Pingback: Java Bean Utils Tutorial For Beginners
Pingback: rechargeable flashlights high lumens
Pingback: Ionic Tutorial For Beginners
Pingback: Java 8 Tutorial For Beginners
Pingback: cPanel Tutorial For Beginners
Pingback: Apache Tapestry Tutorial For Beginners
Pingback: helmet light
Pingback: rechargeable headlamp led
Pingback: HONR Network
Pingback: VascuWave
Pingback: situs Judi Poker online
Pingback: Wireless Security Tutorial For Beginners
Pingback: VascuWave
Pingback: headlights led
Pingback: head light
Pingback: Microsoft Azure Tutorial For Beginners
Pingback: rechargeable headlamp led
Pingback: hiking gear
Pingback: led head light
Pingback: Cricket Tutorial For Beginners
Pingback: head headlight
Pingback: VascuWave
Pingback: Polo Tutorial For Beginners
Pingback: headband light
Pingback: Excel Dashboards Tutorial For Beginners
Pingback: Google Plus Tutorial For Beginners
Pingback: rechargeable headlamp led
Pingback: head light
Pingback: camping gear
Pingback: Functional Programming Tutorial For Beginners
Pingback: headlamps xtreme bright
Pingback: Individual and Group Behavior Tutorial For Beginners
Pingback: Public Library Management Tutorial For Beginners
Pingback: HONR Network
Pingback: deportation lawyer
Pingback: SAP Scripts Tutorial For Beginners
Pingback: rechargeable flashlights high lumens
Pingback: immigration lawyer in fort worth
Pingback: Sales Forecasting Tutorial For Beginners
Pingback: led head lamp light
Pingback: Svn Subversion Tutorial For Beginners
Pingback: helmet light
Pingback: immigration lawyer irving
Pingback: head lights
Pingback: deportation lawyer
Pingback: Sed (Stream Editor) Tutorial For Beginners
Pingback: Classroom Management Tutorial For Beginners
Pingback: helmet flashlight
Pingback: deportation defense lawyer
Pingback: COBOL Tutorial
Pingback: head flashlights led
Pingback: abogados de inmigracion en dallas tx
Pingback: head flashlights led
Pingback: lamparas recargables
Pingback: rechargeable headlamp
Pingback: immigration law firms in dallas
Pingback: helmet flashlight
Pingback: head torch
Pingback: immigration lawyer dallas
Pingback: camping headlamp
Pingback: deportation lawyer
Pingback: headlights led
Pingback: cree headlamp
Pingback: headlamps for camping
Pingback: visa lawyer
Pingback: HR Management Tutorial
Pingback: deportation defense attorney
Pingback: HTML Tutorial
Pingback: Networking Tutorial
Pingback: WinRunner Tutorial
Pingback: Perl Scripting Tutorial
Pingback: best immigration lawyer in dallas
Pingback: deportation defense attorney
Pingback: Business Communications Tutorial
Pingback: abogados de inmigracion en dallas
Pingback: immigration law firms in dallas
Pingback: deportation defense lawyer
Pingback: SAP MM Tutorial
Pingback: Data Warehousing Tutorial
Pingback: SAP WM Tutorial
Pingback: Change Management Tutorial
Pingback: visa lawyer
Pingback: Data Mining Tutorial
Pingback: deportation defense attorney
Pingback: CSS3 Tutorial
Pingback: SAP BW Tutorial
Pingback: Supply Chain Management Tutorial
Pingback: Computer Graphics Tutorial
Pingback: Six Sigma Tutorial
Pingback: Automata Theory Tutorial
Pingback: Security Analysis and Investment Management Tutorial
Pingback: System Analysis and Design Tutorial
Pingback: book adviser
Pingback: vista tube
Pingback: SAS Programming Tutorial
Pingback: pet bottle supplier malaysia
Pingback: Financial Services Marketing Tutorial
Pingback: Social Video
Pingback: Microsoft Excel Tutorial
Pingback: Perrysburg Ohio
Pingback: plastic product boxes
Pingback: amac
Pingback: Cconsultation
Pingback: hammer of thor forex
Pingback: Social Video
Pingback: Social Media
Pingback: Marketing Research Tutorial
Pingback: fold pak distributors
Pingback: archival envelopes
Pingback: Adobe Photoshop Tutorial
Pingback: wholesale product packaging
Pingback: Hadoop Tutorial
Pingback: Quantitative Techniques for management Tutorial
Pingback: Payroll Management Tutorial
Pingback: transparent cylinder container
Pingback: square acrylic containers
Pingback: plastic packaging for clothes
Pingback: Industrial Relations Management Tutorial
Pingback: plasticboxes com
Pingback: Drupal Tutorial
Pingback: Real Estate Photography
Pingback: Bootstrap Tutorial
Pingback: SAP Lumira Tutorial
Pingback: custom plastic sleeves
Pingback: crystal clear storage boxes
Pingback: Professional Video
Pingback: SAP Payroll Tutorial
Pingback: clear boxes packaging
Pingback: Java Swing Tutorial
Pingback: Materialize Tutorial
Pingback: Retail Management Tutorial
Pingback: amac containers
Pingback: Drools Tutorial
Pingback: Database system concepts Tutorial
Pingback: Quality Center (QC) Tutorial
Pingback: CSS Tutorial
Pingback: square plastic containers wholesale
Pingback: Adobe Flex Tutorial
Pingback: visi company
Pingback: MVC Framework Tutorial
Pingback: clear plastic cube boxes
Pingback: Microsoft Project Tutorial
Pingback: XHTML Tutorial
Pingback: amac1960
Pingback: 2x2 clear boxes
Pingback: Strongest sleeping tablets
Pingback: Node.js Tutorial
Pingback: clear pvc packaging boxes
Pingback: shirt boxes bulk
Pingback: acrylic tube australia
Pingback: Computer Security Tutorial
Pingback: packaging products corp
Pingback: archival envelopes clear
Pingback: Flask Tutorial
Pingback: clear plastic storage bins
Pingback: HighCharts Tutorial
Pingback: Cordova Tutorial
Pingback: Apache Ant Tutorial
Pingback: MariaDB Tutorial
Pingback: Service Oriented Architecture (SOA) Tutorial
Pingback: plastic box store
Pingback: React Native Tutorial
Pingback: JOGL Tutorial
Pingback: SAP IDT Tutorial
Pingback: mylar photo sleeves
Pingback: wholesale packaging containers
Pingback: Mahout Tutorial
Pingback: Security Testing Tutorial
Pingback: clear product packaging
Pingback: cello bags uk
Pingback: General Packet Radio Service (GPRS) Tutorial
Pingback: JavaFX Tutorial
Pingback: small clear plastic cases
Pingback: plastic box shop
Pingback: escorts in karachi
Pingback: plastic products company
Pingback: Eclipse Tutorial
Pingback: Parallel Algorithm Tutorial
Pingback: cellophane envelopes uk
Pingback: crystal bag image
Pingback: plastic retail packaging boxes
Pingback: Digital Signal Processing Tutorial
Pingback: NGN Tutorial
Pingback: Extreme Programming Tutorial
Pingback: small lucite boxes
Pingback: custom clear plastic boxes
Pingback: SAP PP Tutorial
Pingback: Lucene Tutorial
Pingback: PyQt Tutorial
Pingback: XML-RPC Tutorial
Pingback: Mobile Marketing Tutorial
Pingback: Batch Script Tutorial
Pingback: Apache Struts 2 Tutorial
Pingback: Facebook Marketing Tutorial
Pingback: Estimation Techniques Tutorial
Pingback: pak plastics
Pingback: Microsoft Expression Web Tutorial
Pingback: cellophane display bags
Pingback: AWT (Abstract Window Toolkit) Tutorial
Pingback: Spring MVC Framework Tutorial
Pingback: The Java Debugger (JDB) Tutorial
Pingback: Unix socket Tutorial
Pingback: Digital Communication Tutorial
Pingback: XSD Tutorial
Pingback: Lua (programming language) Tutorial
Pingback: plastic box packaging
Pingback: Genetic Algorithms Tutorial
Pingback: clear vinyl michaels
Pingback: Workplace Civility Tutorial
Pingback: Software Architecture and Design Tutorial
Pingback: Diu Fort, Diu Tutorial
Pingback: plastic boxes wholesale in india
Pingback: The Art of Happiness Tutorial
Pingback: Freestyle Skiing Tutorial
Pingback: packaging art
Pingback: Training and Development Tutorial For Beginners
Pingback: Tourism Management Tutorial
Pingback: plastic office storage
Pingback: clamshell box wholesale
Pingback: Business sales training Tutorial
Pingback: square plastic box
Pingback: Control Systems Tutorial
Pingback: glass jar suppliers ireland
Pingback: lip balm packaging uk
Pingback: escorts in islamabad
Pingback: plastic shipping boxes
Pingback: plastic tube packaging uk
Pingback: small packaging boxes
Pingback: plastic display boxes wholesale
Pingback: ITIL Configuration Management Tutorial For Beginners
Pingback: Billiards Tutorial
Pingback: amac uk
Pingback: Financial Management Tutorial For Beginners
Pingback: cylinder tube packaging
Pingback: amac australia
Pingback: SAP BI Tutorial For Beginners
Pingback: SQL Database Tutorial For Beginners
Pingback: Play pets
Pingback: SQL Server 2008 Tutorial For Beginners
Pingback: XML Tutorial For Beginners
Pingback: Oracle 9i Tutorial For Beginners
Pingback: votive display and packaging
Pingback: hdpe plastic bottle manufacturers
Pingback: Core Java Tutorial For Beginners
Pingback: small clear boxes with lids
Pingback: Java-Springs Tutorial For Beginners
Pingback: hanging retail boxes
Pingback: michaels organza bags price
Pingback: DB2 Using SQL Tutorial For Beginners
Pingback: IBM - RPG Tutorial For Beginners
Pingback: Siebel - CRM Tutorial For Beginners
Pingback: OBIEE Tutorial For Beginners
Pingback: Software Engineering Tutorial For Beginners
Pingback: plastic wholesale
Pingback: craft packaging supplies
Pingback: plastic containers wholesale
Pingback: clear plastic trays food packaging
Pingback: Strategic Brand Management Tutorial For Beginners
Pingback: IBM Cognos Tutorial For Beginners
Pingback: Agile Testing Tutorial For Beginners
Pingback: escorts in islamabad
Pingback: Web Designing Tutorial For Beginners
Pingback: clear clamshell food containers
Pingback: Programmable Logic controllers Tutorial For Beginners
Pingback: SAP GRC Tutorial For Beginners
Pingback: Modern Banking Tutorial For Beginners
Pingback: plastic sleeves for art
Pingback: Javascript Advanced Tutorial For Beginners
Pingback: J Query Tutorial For Beginners
Pingback: plastic containers wholesale
Pingback: pressure washing
Pingback: Yii Tutorial For Beginners
Pingback: JasmineJS Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: cccam server test line
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: cccam server test
Pingback: What is E-2 Investor Visa?
Pingback: H-2A visa application process
Pingback: clear archival bags
Pingback: L-1B nonimmigrant visa
Pingback: wholesale plastic products
Pingback: L-1A Company Transfer Work Visa
Pingback: clear box packaging
Pingback: Flasks for Liquor
Pingback: large plastic box
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: clearly discount code
Pingback: Flasks for Liquor
Pingback: cardboard powder shakers wholesale
Pingback: Grav Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: E-1 visa process
Pingback: Visa for Australians
Pingback: Sap Successfactors Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Google Charts Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: JUnit Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: B-2 Visa
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: IR-1 Visa application
Pingback: lucite boxes with lids
Pingback: F-4 Visa
Pingback: Flasks for Liquor
Pingback: products of plastic
Pingback: TN Visa
Pingback: Flasks for Liquor
Pingback: Cucumber Tutorial For Beginners
Pingback: iBATIS Tutorial For Beginners
Pingback: MooTools Tutorial For Beginners
Pingback: SAP Testing Tutorial For Beginners
Pingback: cccam server cheap
Pingback: cccam server f line
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: XPath Tutorial For Beginners
Pingback: K-1 fiancé visa
Pingback: plastic products company inc
Pingback: HBase Tutorial For Beginners
Pingback: XStream Tutorial For Beginners
Pingback: art plastic bags
Pingback: script.aculo.us Tutorial For Beginners
Pingback: Log4j Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Mobile computing Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Pinterest Marketing Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: michaels small gift bags
Pingback: plastic packing cases
Pingback: bangkok matching
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Unix makefile Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: small plastic products
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: crystal clear phone number
Pingback: clear can container
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: thin plastic box
Pingback: YouTube Marketing Tutorial For Beginners
Pingback: Cline server
Pingback: Flasks for Liquor
Pingback: server cccam to oscam
Pingback: Apache POI PPT Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Windows 10 Development Tutorial For Beginners
Pingback: Apache Xerces Tutorial For Beginners
Pingback: Parrot Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Telecom Billing Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Easy Mock Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Critical Thinking Tutorial For Beginners
Pingback: Workplace Politics Tutorial For Beginners
Pingback: Performance Management Tutorial For Beginners
Pingback: Anger Management Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Self-Confidence Tutorial For Beginners
Pingback: latest government jobs in pakistan
Pingback: Surveyor Jobs In Pakistan
Pingback: job vacancies in karachi
Pingback: online jobs in karachi
Pingback: Electrician Jobs In Pakistan
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: government jobs in pakistan
Pingback: Health Jobs In Pakistan
Pingback: Behavior Driven Development Tutorial For Beginners
Pingback: Flasks for Liquor
Pingback: Positive Body Language Tutorial For Beginners
Pingback: Design thinking Tutorial For Beginners
Pingback: Professor Jobs In Pakistan
Pingback: job opportunities in pakistan
Pingback: Professor Jobs In Pakistan
Pingback: patio tv covers
Pingback: review outdoor tv cover
Pingback: Sales Planning Tutorial For Beginners
Pingback: Technician Jobs In Pakistan
Pingback: Cccam test 24h
Pingback: 55 inch tv cover
Pingback: outdoor patio tv cover
Pingback: Assertiveness Tutorial For Beginners
Pingback: Antenna Theory Tutorial For Beginners
Pingback: Coordinator Jobs In Pakistan
Pingback: c line server cccam
Pingback: all jobs in pakistan 2016
Pingback: outdoor tv covers 55 inch lcd
Pingback: lcd tv cover
Pingback: tv covers for outdoor tvs
Pingback: Incentive planning Tutorial For Beginners
Pingback: outdoor tv covers 55 inch lcd
Pingback: Thematic Apperception Test Tutorial For Beginners
Pingback: Management Jobs In Pakistan
Pingback: vizio outdoor tv
Pingback: Accountant Jobs In Pakistan
Pingback: samsung outdoor tv covers
Pingback: Tennis Tutorial For Beginners
Pingback: ngo jobs in pakistan
Pingback: 55 inch outdoor tv cover
Pingback: Coaching and Mentoring Tutorial For Beginners
Pingback: samsung outdoor tv covers
Pingback: Kanban Tutorial For Beginners
Pingback: Interpersonal Skills Tutorial For Beginners
Pingback: Outcome Measurement Tutorial For Beginners
Pingback: tv covers for outdoor tvs
Pingback: Indian Polity Tutorial For Beginners
Pingback: Carpenter Jobs In Pakistan
Pingback: Security Jobs In Pakistan
Pingback: tv cover for outdoor tv
Pingback: review outdoor tv cover
Pingback: all jobs in pakistan 2016
Pingback: review outdoor tv cover
Pingback: Sony outdoor TV cover
Pingback: tv covers for outdoor use
Pingback: outdoor patio tv cover
Pingback: outdoor patio tv cover
Pingback: quality outdoor tv cover
Pingback: patio tv covers
Pingback: tv cover for outdoor tv
Pingback: Driver Jobs In Pakistan
Pingback: outdoor tv box cover
Pingback: Doctor Jobs In Pakistan
Pingback: insulated outdoor tv cover
Pingback: govt jobs in pakistan 2016
Pingback: outdoor tv cover amazon
Pingback: serveur cccam server
Pingback: flat screen covers outdoor
Pingback: television covers for outside
Pingback: promote my music on spotify
Pingback: tv covers for outdoor use
Pingback: outdoor tv cover amazon
Pingback: Valises & sacs
Pingback: Autres Chaussures
Pingback: best weatherproof outdoor tv cover
Pingback: tv covers for outside use
Pingback: Sous V̻tements
Pingback: outdoor patio tv cover
Pingback: lcd tv cover
Pingback: weatherproof outdoor tv cover
Pingback: led tv outdoor cover
Pingback: D̩coration
Pingback: best weatherproof outdoor tv cover
Pingback: rain outdoor tv cover
Pingback: LG waterproof tv cover
Pingback: led tv outdoor cover
Pingback: patio tv covers
Pingback: outdoor patio tv cover
Pingback: Sony outdoor TV cover
Pingback: Voir d'autres
Pingback: outdoor tv cover amazon Canada
Pingback: outdoor patio tv cover
Pingback: Toyota
Pingback: LG waterproof tv cover
Pingback: tv covers for outside use
Pingback: tv cover for outdoor tv
Pingback: outdoor tv covers 55 inch lcd
Pingback: Aspirateurs
Pingback: Canada outdoor tv cover
Pingback: Ordinateurs fixes
Pingback: lcd tv plastic cover
Pingback: best outdoor tv covers
Pingback: outdoor patio tv cover
Pingback: where to buy outdoor tv covers
Pingback: outdoor tv covers 55
Pingback: cheap outdoor tv covers
Pingback: vizio outdoor tv
Pingback: Disques Durs
Pingback: winter tv cover
Pingback: Mobilier
Pingback: Voitures
Pingback: Bijoux/Montres
Pingback: best outdoor tv covers
Pingback: vizio outdoor tv
Pingback: Foulards/Chapeaux
Pingback: television covers
Pingback: Sac ordinateur Portable
Pingback: Guttering repairs
Pingback: custom outdoor tv covers
Pingback: tv cover price
Pingback: tv covers for outdoor tvs
Pingback: cccam server buy
Pingback: rain outdoor tv cover
Pingback: waterproof tv cover
Pingback: rain outdoor tv cover
Pingback: cheap outdoor tv covers
Pingback: Tablettes
Pingback: custom outdoor tv covers
Pingback: Cccam
Pingback: Bureautiques, Cartouches & papiers
Pingback: Chaussures de villes
Pingback: Appareils photo
Pingback: Voir d'autres
Pingback: Polos & Chemises homme
Pingback: vizio outdoor tv covers
Pingback: Summer dress
Pingback: winter tv cover
Pingback: Aspirateurs
Pingback: best outdoor tv cover
Pingback: outdoor tv protective covers
Pingback: outdoor television covers
Pingback: cheap outdoor tv covers
Pingback: UML Tutorial
Pingback: SAP FICO Tutorial
Pingback: MS Access Tutorial
Pingback: winter outdoor tv cover
Pingback: child care tax credit
Pingback: C++ Tutorial
Pingback: which charity should i donate to
Pingback: custom outdoor tv covers
Pingback: plasma tv cover
Pingback: how to donate a house
Pingback: riser stand
Pingback: Financial Reporting and Analysis Tutorial
Pingback: samsung outdoor tv covers
Pingback: outdoor television covers
Pingback: donate my car
Pingback: rain outdoor tv cover
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: donald trump charity donations
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: charity property
Pingback: laptop computer stand
Pingback: Flasks for Liquor
Pingback: Informatica Tutorial
Pingback: the donated house
Pingback: donations to church tax deductible
Pingback: Flasks for Liquor
Pingback: QTP Tutorial
Pingback: Flasks for Liquor
Pingback: donate my car to charity
Pingback: Flasks for Liquor
Pingback: stop snoring
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: donating real estate to a non profit
Pingback: ASP.NET Tutorial
Pingback: cccam fline server
Pingback: Flasks for Liquor
Pingback: fair market value of charitable donations
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: donating real estate to charity
Pingback: irs bargain sale to charity
Pingback: Flasks for Liquor
Pingback: Flasks for Liquor
Pingback: SAP SOLMAN Tutorial
Pingback: home donations
Pingback: Flasks for Liquor
Pingback: can you donate a house
Pingback: Microsoft Powerpoint Tutorial
Pingback: Flasks for Liquor
Pingback: Online Marketing Tutorial
Pingback: which charity should i donate to
Pingback: Flasks for Liquor
Pingback: real estate donations to nonprofits
Pingback: why you should donate to charity
Pingback: LG waterproof tv cover
Pingback: charitable contributions
Pingback: mac stand
Pingback: 55 inch outdoor tv cover
Pingback: best weatherproof outdoor tv cover
Pingback: samsung outdoor tv covers
Pingback: national charities
Pingback: weatherproof rain outdoor tv cover
Pingback: Food Resources Manual Tutorial
Pingback: charitable contribution deduction
Pingback: Database Testing Tutorial
Pingback: best waterproof outdoor tv cover
Pingback: outdoor led tv covers
Pingback: chat per uomini
Pingback: Linux Embedded systems Tutorial
Pingback: chat gratis per single
Pingback: weatherproof tv cover
Pingback: folding laptop stand
Pingback: Microsoft Entity Framework Tutorial
Pingback: best charities to donate clothes
Pingback: chattare gratis
Pingback: samsung outdoor tv covers
Pingback: videochatta
Pingback: SASS (Syntactically Awesome Style sheets) Tutorial
Pingback: rain outdoor tv cover
Pingback: webchat freee
Pingback: business dumpster rental
Pingback: outdoor tv covers 55 inch lcd
Pingback: winter tv cover
Pingback: LG waterproof tv cover
Pingback: lcd tv plastic cover
Pingback: vizio outdoor tv
Pingback: cover for flat screen tv outside
Pingback: videochat senza registrazione
Pingback: plasma tv cover
Pingback: Web analytics Tutorial
Pingback: outdoor lcd tv covers
Pingback: winter outdoor tv cover
Pingback: JSON (JavaScript Object Notation) Tutorial
Pingback: cheap outdoor tv covers
Pingback: garbage dumpster sizes
Pingback: MVVM Tutorial
Pingback: weatherproof tv cover
Pingback: riser stand
Pingback: video chat per incontri
Pingback: insulated outdoor tv cover
Pingback: tv covers for outdoor use
Pingback: cheap outdoor tv covers
Pingback: 40 yard dumpster rental price
Pingback: LG waterproof tv cover
Pingback: vizio outdoor tv
Pingback: patio tv covers
Pingback: outdoor tv covers 55
Pingback: videochat per tutti
Pingback: large trash removal
Pingback: outside tv covers
Pingback: insulated outdoor tv cover
Pingback: Principles of Communication Tutorial
Pingback: Signals and Systems Tutorial
Pingback: winter tv cover
Pingback: toshiba outdoor tv gover
Pingback: television covers
Pingback: computer risers for desk
Pingback: video webchat
Pingback: video chat per ragazzi
Pingback: chat free
Pingback: toshiba outdoor tv gover
Pingback: WSDL Tutorial
Pingback: clipping path service
Pingback: Drop shadow service
Pingback: Information Security Cyber Law Tutorial
Pingback: MIRROR EFFECT SERVICE
Pingback: Distributed DBMS Tutorial
Pingback: OrientDB Tutorial
Pingback: best weatherproof outdoor tv cover
Pingback: samsung outdoor tv covers
Pingback: vizio outdoor tv covers
Pingback: tv cover for outdoor tv
Pingback: patio tv covers
Pingback: outdoor tv cover amazon Canada
Pingback: dumpster service
Pingback: Agile Methodology Tutorial
Pingback: photoshop masking
Pingback: winter outdoor tv cover
Pingback: Sony outdoor TV cover
Pingback: 10 yard dumpster rental
Pingback: cool tv covers
Pingback: outdoor tv protective covers
Pingback: Graph Theory Tutorial
Pingback: plasma tv cover
Pingback: outdoor lcd tv covers
Pingback: weatherproof tv cover
Pingback: quality outdoor tv cover
Pingback: cool tv covers
Pingback: outdoor waterproof tv covers
Pingback: outdoor tv cover amazon Canada
Pingback: cover for flat screen tv outside
Pingback: outdoor tv cover amazon Canada
Pingback: outdoor tv cover amazon Canada
Pingback: VECTOR CONVERSION
Pingback: dumpster rental Cook county
Pingback: Photo retouching
Pingback: outdoor tv covers 55
Pingback: plastic outdoor tv cover
Pingback: insulated outdoor tv cover
Pingback: rent a dumpster
Pingback: International Finance Tutorial
Pingback: Archery Tutorial
Pingback: cheap outdoor tv covers
Pingback: lcd tv cover
Pingback: outdoor tv dust cover
Pingback: Taj Mahal,Agra Tutorial
Pingback: Project Management Tutorial For Beginners
Pingback: cost of a dumpster
Pingback: Photo editing Help
Pingback: roll off container sizes
Pingback: waste bins rental
Pingback: vizio outdoor tv covers
Pingback: Clipping path career
Pingback: Workplace Wellness Tutorial
Pingback: waste pickup
Pingback: rain outdoor tv cover
Pingback: Work-Life Balance Tutorial
Pingback: outdoor patio tv cover
Pingback: get a dumpster
Pingback: laptop riser
Pingback: Plasma TV cover
Pingback: review outdoor tv cover
Pingback: how to improve guitar playing speed
Pingback: household dumpster rental
Pingback: junk disposal
Pingback: 30 cubic yard dumpster
Pingback: Plasma TV cover
Pingback: Running Tutorial
Pingback: Plasma TV cover
Pingback: outside tv covers
Pingback: weatherproof tv cover
Pingback: construction waste containers
Pingback: lcd tv cover
Pingback: custom outdoor tv covers
Pingback: Sony outdoor TV cover
Pingback: outdoor lcd tv covers
Pingback: patio tv covers
Pingback: quality outdoor tv cover
Pingback: dumpster rental ri
Pingback: rent roll off dumpster
Pingback: winter cold tv cover
Pingback: best waterproof outdoor tv cover
Pingback: quality outdoor tv cover
Pingback: outdoor patio tv cover
Pingback: winter tv cover
Pingback: dumpster for sale
Pingback: hunks hauling junk
Pingback: samsung outdoor tv covers
Pingback: lcd tv cover
Pingback: outdoor tv covers
Pingback: outdoor tv cover amazon Canada
Pingback: television covers for outside
Pingback: how to increase your guitar playing speed
Pingback: Plasma TV cover
Pingback: construction containers for rent
Pingback: tv covers for outdoor use
Pingback: outdoor waterproof tv covers
Pingback: 55 inch outdoor tv cover
Pingback: appliance parts pro
Pingback: a and e appliance repair
Pingback: appliance sales
Pingback: lcd tv cover screen
Pingback: outdoor tv covers 55 inch lcd
Pingback: appliance repair temecula
Pingback: outside tv covers
Pingback: best weatherproof outdoor tv cover
Pingback: Plasma TV cover
Pingback: quality outdoor tv cover
Pingback: frigidaire
Pingback: outdoor tv cover amazon Canada
Pingback: weatherproof outdoor tv cover
Pingback: lg refrigerator repair
Pingback: outdoor lcd tv covers
Pingback: tv covers for outdoor tvs
Pingback: westside appliance repair
Pingback: led tv outdoor cover
Pingback: insulated outdoor tv cover
Pingback: maytag washer parts
Pingback: review outdoor tv cover
Pingback: outdoor tv cover amazon
Pingback: tv covers for outdoor tvs
Pingback: outdoor flat screen tv covers
Pingback: patio tv covers
Pingback: outdoor lcd tv covers
Pingback: tv covers for outdoor use
Pingback: laptop riser
Pingback: plasma tv cover
Pingback: dj appliance service
Pingback: consumer energy appliance service plan
Pingback: appliance repair fairfax
Pingback: insulated outdoor tv cover
Pingback: hart appliance service
Pingback: tv covers for outdoor use
Pingback: outdoor tv cover amazon
Pingback: Canada outdoor tv cover
Pingback: vizio outdoor tv
Pingback: lcd tv plastic cover
Pingback: in home appliance repair service
Pingback: laptop riser
Pingback: outdoor tv covers 55 inch lcd
Pingback: appliance replacement parts
Pingback: appliances madison
Pingback: outdoor tv covers 55 inch lcd
Pingback: winter tv cover
Pingback: tv cover for outdoor tv
Pingback: dacor parts
Pingback: samsung outdoor tv covers
Pingback: plastic outdoor tv cover
Pingback: lcd tv plastic cover
Pingback: led tv outdoor cover
Pingback: best stove
Pingback: outdoor tv cover amazon
Pingback: toshiba outdoor tv gover
Pingback: LG outdoor tv cover
Pingback: quality outdoor tv cover
Pingback: kitchen stove
Pingback: plastic outdoor tv cover
Pingback: stove ranges
Pingback: cheap outdoor tv covers
Pingback: frigidaire oven repair
Pingback: kitchenaid refrigerator repair manual
Pingback: phoenix refrigerator repair
Pingback: maytag dishwasher
Pingback: a refrigerator
Pingback: refrigerator repair shop
Pingback: Cameras
Pingback: Feroz Shah Kotla Fort, Delhi Tutorial
Pingback: Fer ÌÊ repasser
Pingback: Talons/Ballerines
Pingback: Franbizz Solutions
Pingback: Employee Supervision Tutorial
Pingback: Business opportunity
Pingback: Franchise opportunities
Pingback: Sac ordinateur Portable
Pingback: Polos & Chemises homme
Pingback: Sac ordinateur Portable
Pingback: Portefeuilles
Pingback: International Business Management Tutorial
Pingback: Abbreviations Tutorial
Pingback: Preshool Franchise
Pingback: Recruitment and Selection Tutorial
Pingback: LoadRunner Tutorial For Beginners
Pingback: Congelateurs
Pingback: Sac ordinateur Portable
Pingback: Water Polo Tutorial
Pingback: Imprimantes et Scanners
Pingback: Cam̩ra
Pingback: IMMOBLIERS
Pingback: Franchise
Pingback: Golf Tutorial
Pingback: health franchise
Pingback: video chat per uomini
Pingback: video chat
Pingback: chat per donne
Pingback: chat per tutti
Pingback: video webchat
Pingback: Bar Franchise
Pingback: Cracking Interviews Tutorial
Pingback: webchat over 40
Pingback: Volleyball Tutorial
Pingback: chat senza registrazione
Pingback: Bar Franchise
Pingback: Teradata Tutorial For Beginners
Pingback: Choose Top 20 Food Franchise
Pingback: restaurant franchise
Pingback: Preshool Franchise
Pingback: Android Tutorial For Beginners
Pingback: chat italia
Pingback: Business Environment Tutorial For Beginners
Pingback: webcam chat
Pingback: webchat freee
Pingback: video webchat gratis
Pingback: chat incontri gratis
Pingback: IBM-REXX Tutorial For Beginners
Pingback: MySQL Tutorial For Beginners
Pingback: Fast Forward MBA in Business communication Tutorial For Beginners
Pingback: BLACKBERRY Tutorial For Beginners
Pingback: Data Structures Tutorial For Beginners
Pingback: IBM - AS/400 Tutorial For Beginners
Pingback: buy instagram followers
Pingback: SAP BASIS Tutorial For Beginners
Pingback: multiple listing service
Pingback: Microstrategy Tutorial For Beginners
Pingback: Wedding Cars Leicester
Pingback: $30 bubbler
Pingback: buy a marijuana pipe
Pingback: dab rig deals
Pingback: mp3 songs
Pingback: Back posture corrector for women
Pingback: SAP CRM Tutorial For Beginners
Pingback: vaporblunt-2.0-vaporizer-review
Pingback: 4 mm glass bong
Pingback: SAP SD Tutorial For Beginners
Pingback: g lab water pipe
Pingback: Posture corrector for men
Pingback: CoffeeScript Tutorial For Beginners
Pingback: real estate taxes
Pingback: UMTS Tutorial For Beginners
Pingback: coeur d'alene head shops
Pingback: dab rig and torch
Pingback: Back posture corrector for women
Pingback: Posture corrector
Pingback: vaporizer unhealthy
Pingback: head shop sioux falls
Pingback: Posture corrector for men
Pingback: HCatalog Tutorial For Beginners
Pingback: water pipe under driveway
Pingback: Microsoft Silverlight Tutorial For Beginners
Pingback: weed pipe bowl
Pingback: k-line water system
Pingback: Posture brace
Pingback: dab rig reviews
Pingback: vs.05 vaporizer
Pingback: Posture corrector
Pingback: Posture corrector
Pingback: head shop 82nd
Pingback: glass bowl lids
Pingback: Back posture corrector
Pingback: Back posture corrector for women
Pingback: weed pipe storage
Pingback: CSS Advanced Tutorial For Beginners
Pingback: Posture corrector for men
Pingback: Posture corrector
Pingback: Back posture corrector
Pingback: ProntoWash
Pingback: new glass bongs 2015
Pingback: Posture brace
Pingback: Back brace for posture women
Pingback: Posture brace
Pingback: ergonomia stanowiska pracy na produkcji
Pingback: rwa kulszowa
Pingback: marijuana pipe with cover
Pingback: Back brace for posture women
Pingback: Apex Tutorial For Beginners
Pingback: kurt b bubbler
Pingback: Penetration Testing Tutorial For Beginners
Pingback: Posture corrector for men
Pingback: Posture corrector for men
Pingback: 1 quart glass bowl
Pingback: TestNG Tutorial For Beginners
Pingback: ból karku
Pingback: f scott fitzgerald cut glass bowl
Pingback: Mockito Tutorial For Beginners
Pingback: bubbler app
Pingback: dab rig repair
Pingback: Posture corrector for women
Pingback: 7 quart glass bowl
Pingback: rwa kulszowa
Pingback: 9 mm dab rig
Pingback: Design Patterns Tutorial For Beginners
Pingback: Posture corrector for women
Pingback: Material Design Lite Tutorial For Beginners
Pingback: glass bong companies
Pingback: water bong gravity
Pingback: XQuery Tutorial For Beginners
Pingback: Posture brace
Pingback: 3 quart glass bowl
Pingback: Posture brace
Pingback: 8 water pipe cost
Pingback: ergonomia pracy przy komputerze
Pingback: CouchDB Tutorial For Beginners
Pingback: JFreeChart Tutorial For Beginners
Pingback: portable enail dab rig
Pingback: Posture corrector
Pingback: JavaMail API Tutorial For Beginners
Pingback: head xrc shop
Pingback: Apache Tajo Tutorial For Beginners
Pingback: Swift Programming Tutorial For Beginners
Pingback: Neo4j Tutorial For Beginners
Pingback: Windows Communication Foundation (WCF) Tutorial For Beginners
Pingback: bubbleroom d'brand
Pingback: Call Now Best Facebook Agency Free Ads Voy Media Apply Online
Pingback: Back posture corrector
Pingback: Apache Hive Tutorial For Beginners
Pingback: prediksi skor bola
Pingback: 5 mm bubbler
Pingback: dab rig outlet
Pingback: Posture corrector for men
Pingback: Posture brace
Pingback: Back brace for posture women
Pingback: Back posture corrector for women
Pingback: glass bowl shade
Pingback: bubbler pot
Pingback: Posture brace
Pingback: Back brace for posture women
Pingback: vaporizer asthma
Pingback: Windows Server 2012 Tutorial For Beginners
Pingback: Posture brace
Pingback: Back posture corrector for women
Pingback: Excel Data Analysis Tutorial For Beginners
Pingback: Back posture corrector
Pingback: Advanced Excel Functions Tutorial For Beginners
Pingback: Conversion Rate Optimisation Tutorial For Beginners
Pingback: Posture brace
Pingback: zurn bubbler
Pingback: Back posture corrector
Pingback: Back posture corrector
Pingback: Posture corrector
Pingback: pulsar 7 vaporizer how to use
Pingback: 2K18 PLAYMAKING SHOT CREATOR SF
Pingback: marijuana pipe pen
Pingback: water pipe 30mm
Pingback: Posture brace
Pingback: Posture corrector for women
Pingback: head shop zephyrhills
Pingback: Back posture corrector for women
Pingback: water quality pipe
Pingback: Adaptive software development Tutorial For Beginners
Pingback: Back posture corrector
Pingback: marijuana pipe for sale
Pingback: Avro Tutorial For Beginners
Pingback: Amazon Market Place Tutorial For Beginners
Pingback: Back posture corrector
Pingback: Apache Tika Tutorial For Beginners
Pingback: Posture corrector for women
Pingback: Posture corrector for men
Pingback: mens stainless bracelets
Pingback: Back posture corrector for women
Pingback: f-line water tank
Pingback: weed pipe malaysia
Pingback: dab rig dabber
Pingback: Fatehpur Sikri Fort Tutorial For Beginners
Pingback: stainless steel jewelry canada
Pingback: unique steel jewellery
Pingback: Aguada Fort, Goa Tutorial For Beginners
Pingback: Social Intelligence Tutorial For Beginners
Pingback: men's jewellery bracelets
Pingback: Posture corrector
Pingback: Posture corrector for men
Pingback: Back brace for posture women
Pingback: Improving Personal Productivity Tutorial For Beginners
Pingback: Posture corrector for women
Pingback: Collaborative Writing Tutorial For Beginners
Pingback: geno eaves
Pingback: Posture corrector for women
Pingback: 7's smoke shop brentwood ca
Pingback: d&k water pipe
Pingback: Posture brace
Pingback: glass bowl mushrooms
Pingback: geno eaves durham
Pingback: Back posture corrector
Pingback: vaporizer 40w
Pingback: vaporizer o
Pingback: Knowledge Management Tutorial For Beginners
Pingback: Workplace Diversity Tutorial For Beginners
Pingback: vaporizer case
Pingback: Geno eaves chickfila
Pingback: Posture corrector
Pingback: Back posture corrector for women
Pingback: Team Building Tutorial For Beginners
Pingback: yoda bubbler
Pingback: geno eaves chapel hill
Pingback: Microprocessor Tutorial For Beginners
Pingback: Posture brace
Pingback: Posture corrector for women
Pingback: kurt b bubbler
Pingback: Back posture corrector for women
Pingback: Back brace for posture women
Pingback: geno eaves chapel hill
Pingback: Posture corrector for women
Pingback: Posture corrector
Pingback: Back posture corrector for women
Pingback: C Tutorial
Pingback: build a dab rig
Pingback: HTML 4 Tutorial
Pingback: Cloud Computing Tutorial
Pingback: Back posture corrector
Pingback: Back posture corrector for women
Pingback: Posture brace
Pingback: geno eaves durham
Pingback: Posture corrector for men
Pingback: weed pipe with built in lighter
Pingback: Back posture corrector for women
Pingback: Posture corrector for men
Pingback: Back posture corrector
Pingback: Posture corrector for men
Pingback: watch movies online
Pingback: AJAX Tutorial
Pingback: metafores lymaton mykonos
Pingback: water bong 2 liter
Pingback: Oracle 11g Tutorial
Pingback: bubbler trackid=sp-006
Pingback: metafores lymaton santorinaios
Pingback: Back posture corrector for women
Pingback: Posture corrector
Pingback: Back posture corrector
Pingback: Posture brace
Pingback: Posture corrector for men
Pingback: weed pipe lighter
Pingback: v-9902 pro bubbler
Pingback: T-SQL Tutorial
Pingback: Back brace for posture women
Pingback: Posture brace
Pingback: weed pipe definition
Pingback: Mobile Testing Tutorial
Pingback: Back posture corrector for women
Pingback: water pipe repair
Pingback: Posture brace
Pingback: Back posture corrector
Pingback: Posture corrector for men
Pingback: Back posture corrector
Pingback: Back posture corrector
Pingback: metafores lymaton
Pingback: metafores lymaton santorinaios
Pingback: Pure.CSS Tutorial
Pingback: Posture corrector
Pingback: Back posture corrector
Pingback: Search Engine Optimization (SEO) Tutorial
Pingback: long island medium schedule
Pingback: stainless steel pendants wholesale
Pingback: Posture corrector for men
Pingback: Git (software) Tutorial
Pingback: clique aqui
Pingback: Posture brace
Pingback: Posture corrector
Pingback: veja mais
Pingback: men's stainless steel and gold bracelets
Pingback: Back posture corrector for women
Pingback: Posture corrector
Pingback: Angular Material Tutorial
Pingback: party
Pingback: Posture corrector for women
Pingback: Posture brace
Pingback: Tattoo shop
Pingback: zirconia
Pingback: bauble
Pingback: bezel
Pingback: conheça
Pingback: Elektro recycling
Pingback: Best tattoo shop
Pingback: Posture corrector
Pingback: Posture corrector
Pingback: surgical steel rings
Pingback: tassels
Pingback: Back brace for posture women
Pingback: conheça
Pingback: Back posture corrector
Pingback: infinity
Pingback: pearl
Pingback: Posture corrector for men
Pingback: Back posture corrector
Pingback: Posture corrector
Pingback: statement
Pingback: Posture corrector
Pingback: free past life reading
Pingback: Back posture corrector
Pingback: Back posture corrector
Pingback: Posture brace
Pingback: Back brace for posture women
Pingback: emprendimientos ecuador
Pingback: Back posture corrector
Pingback: cubic
Pingback: Posture corrector for men
Pingback: Back posture corrector for women
Pingback: clique aqui
Pingback: saiba mais
Pingback: bijoux
Pingback: birthstone
Pingback: Posture corrector
Pingback: clique aqui
Pingback: mens designer jewelry
Pingback: saiba mais
Pingback: clique aqui
Pingback: sapphire
Pingback: stones
Pingback: earrings
Pingback: Posture corrector for women
Pingback: stainless steel earring set
Pingback: conheça
Pingback: sapphire
Pingback: veja mais
Pingback: saiba mais
Pingback: clique aqui
Pingback: conheça
Pingback: San Diego
Pingback: halo
Pingback: saiba mais
Pingback: Back posture corrector
Pingback: stackable
Pingback: cubic
Pingback: Posture corrector for women
Pingback: Back brace for posture women
Pingback: metal bracelets for women
Pingback: wedding blog
Pingback: Solarmodule
Pingback: jewelry
Pingback: where can i buy stainless steel jewelry
Pingback: cool mens jewelry
Pingback: Tattoo shop
Pingback: band
Pingback: etsy
Pingback: wedding planner
Pingback: cape town wedding organizer
Pingback: free physic reading
Pingback: Posture corrector
Pingback: Posture corrector for women
Pingback: Posture corrector
Pingback: birthday
Pingback: flower ideas
Pingback: Posture brace
Pingback: stainless steel mens jewelry
Pingback: gold
Pingback: earrings
Pingback: mens steel necklace chain
Pingback: black stainless steel wedding bands
Pingback: custom stainless steel rings
Pingback: Back brace for posture women
Pingback: Back posture corrector
Pingback: Posture corrector
Pingback: Posture corrector for men
Pingback: wedding planner
Pingback: Back brace for posture women
Pingback: stainless steel jewellry
Pingback: layer
Pingback: Posture brace
Pingback: topaz
Pingback: Posture corrector for men
Pingback: engagement
Pingback: stainless steel mens diamond rings
Pingback: cape town wedding florist
Pingback: Tattoo San Diego
Pingback: Posture corrector for women
Pingback: stainless steel bracelets
Pingback: buy stainless steel jewelry
Pingback: Posture corrector for men
Pingback: new york
Pingback: royal wedding
Pingback: pearl
Pingback: Best tattoo artist
Pingback: Schoonmaakbedrijf Zaandam
Pingback: stainless steel jewelry bulk
Pingback: boys stainless steel necklace
Pingback: stones
Pingback: stainless steel ring price
Pingback: bloggers
Pingback: Back posture corrector for women
Pingback: Posture corrector for men
Pingback: diamond and steel jewelry
Pingback: Posture corrector for men
Pingback: timeless
Pingback: infinity
Pingback: stainless steel jewelry polish
Pingback: steel rings for sale
Pingback: stainless steel necklace and bracelet set
Pingback: Back brace for posture women
Pingback: free psychic consultation
Pingback: Back posture corrector
Pingback: Back posture corrector for women
Pingback: Posture corrector for women
Pingback: hearts
Pingback: hearts
Pingback: Back posture corrector
Pingback: stainless steel diamond engagement rings
Pingback: Back brace for posture women
Pingback: Best Visitor Counter Services
Pingback: hearts
Pingback: San Diego
Pingback: Tattoo San Diego
Pingback: Back posture corrector for women
Pingback: gemstone
Pingback: Back posture corrector
Pingback: free blog counter
Pingback: free visitor counter
Pingback: wide stainless steel rings
Pingback: wedding
Pingback: hit counter
Pingback: best hit counter
Pingback: best hit counter
Pingback: dangle
Pingback: Back posture corrector
Pingback: bride
Pingback: stainless jewelry wholesale
Pingback: Buy high quality CBD concentrates
Pingback: necklace
Pingback: Buy lab-tested cannabidiol products
Pingback: bloggers
Pingback: Back brace for posture women
Pingback: Posture corrector
Pingback: radiant
Pingback: Back posture corrector for women
Pingback: Posture corrector for men
Pingback: Posture corrector for men
Pingback: comment investir dans une ICO
Pingback: videochat libera
Pingback: videochat over 40
Pingback: Back posture corrector for women
Pingback: new york
Pingback: leigh
Pingback: fashion bloggers
Pingback: chattare gratis
Pingback: Back posture corrector for women
Pingback: videochat per donne
Pingback: bride
Pingback: Posture brace
Pingback: wholesale steel rings
Pingback: drop
Pingback: stainless steel jewelry wire
Pingback: sterling steel necklace
Pingback: timeless
Pingback: buy stainless steel jewelry
Pingback: stainless steel bangle bracelet wholesale
Pingback: stainless steel cz wedding rings
Pingback: mens stainless wedding bands
Pingback: Posture corrector
Pingback: stones
Pingback: long stainless steel necklace
Pingback: earrings
Pingback: 316l stainless steel ring
Pingback: stackable
Pingback: tassels
Pingback: necklaces for men stainless steel
Pingback: steeltime men's jewelry
Pingback: stainless steel diamond bracelet
Pingback: videochat senza registrazione
Pingback: Posture corrector
Pingback: plain stainless steel rings
Pingback: online shopping
Pingback: Back posture corrector
Pingback: Buy high quality CBD concentrates
Pingback: Posture corrector
Pingback: Back brace for posture women
Pingback: bauble bar
Pingback: stanley steel jewelry
Pingback: Posture corrector for women
Pingback: Back posture corrector
Pingback: Buy legal cannabis oil online
Pingback: women's stainless steel bracelets
Pingback: Back posture corrector
Pingback: duchess
Pingback: videochat
Pingback: tea room bridal shower los angeles
Pingback: bracelet
Pingback: statement
Pingback: Back posture corrector
Pingback: Posture corrector for women
Pingback: Back posture corrector
Pingback: Back brace for posture women
Pingback: Posture corrector for men
Pingback: Posture corrector
Pingback: Back posture corrector
Pingback: Back posture corrector for women
Pingback: stainless steel engagement rings
Pingback: affordable bridal shower location los angeles
Pingback: Back brace for posture women
Pingback: custom engraved stainless steel rings
Pingback: Back posture corrector for men
Pingback: Back brace posture corrector
Pingback: Posture brace for women
Pingback: Your trusted CBD source
Pingback: Buy high quality legal cannabis products
Pingback: leather camera strap
Pingback: gopalast
Pingback: Back posture corrector for men
Pingback: Best posture corrector
Pingback: Mongole Leipzig
Pingback: online scientific paraphrasing tool
Pingback: Posture corrector for women under clothes
Pingback: accounting project topics
Pingback: ACCOUNTING
Pingback: mens stainless steel cz rings
Pingback: project topics
Pingback: Best posture corrector
Pingback: PHYSICS
Pingback: Best posture corrector
Pingback: Back brace posture corrector
Pingback: Back posture corrector for men
Pingback: Back brace posture corrector
Pingback: PURCHASING
Pingback: PUBLIC HEALTH
Pingback: public administration projects
Pingback: Posture brace for women
Pingback: MASTERS DISSERTATION
Pingback: Back brace posture corrector
Pingback: Abendessen Leipzig
Pingback: Back posture corrector for men
Pingback: MASS COMMUNICATION
Pingback: Posture corrector for women under clothes
Pingback: MASTERS DISSERTATION
Pingback: PSYCHOLOGY
Pingback: MATHEMATICS
Pingback: free paraphrasing tool
Pingback: AGRICULTURAL SCIENCE
Pingback: Weihnachtsfeier in Leipzig
Pingback: Posture brace for women
Pingback: marketing project topics
Pingback: Legal weed worldwide delivery
Pingback: LITERATURE
Pingback: Mongolisch BBQ Leipzig
Pingback: medical paraphrasing tool
Pingback: The best of what cannabis has to offer
Pingback: Asiatisches Restaurnat Leipzig
Pingback: curcumin with bioperine
Pingback: Posture brace for women
Pingback: Back brace posture corrector
Pingback: Back brace posture corrector
Pingback: Posture corrector for women under clothes
Pingback: Home Cleaning
Pingback: Back posture corrector for men
Pingback: Posture corrector for women under clothes
Pingback: Best posture corrector
Pingback: DIY Cleaning Tips
Pingback: Top Cleaning Company in
Pingback: Back brace posture corrector
Pingback: Best Cleaning Company in
Pingback: Best posture corrector
Pingback: Perfect posture
Pingback: Posture brace for women
Pingback: Back posture corrector for men
Pingback: Home Cleaning
Pingback: Back posture corrector for men
Pingback: Best posture corrector
Pingback: Memphis
Pingback: Posture brace for women
Pingback: Posture corrector for women under clothes
Pingback: Back brace posture corrector
Pingback: Posture brace for women
Pingback: Best posture corrector
Pingback: Posture corrector for women under clothes
Pingback: Perfect posture
Pingback: and junk
Pingback: Posture corrector for women under clothes
Pingback: Best posture corrector
Pingback: Posture corrector for women under clothes
Pingback: Back posture corrector for men
Pingback: einen Blick hier werfen
Pingback: navigiere hier
Pingback: ursprüngliche Seite
Pingback: Lesen Sie die vollständigen Informationen hier
Pingback: Back posture corrector for men
Pingback: Back posture corrector for men
Pingback: nützliche Quelle
Pingback: großartige Seite
Pingback: Erfahren Sie mehr
Pingback: finde mehr
Pingback: Seite
Pingback: Weiterlesen
Pingback: Perfect posture
Pingback: offizielle Seite
Pingback: zu diesen Jungs hüpfen
Pingback: Best posture corrector
Pingback: Posture brace for women
Pingback: Weiterlesen
Pingback: Webseite hier
Pingback: Posture brace for women
Pingback: nützliche Referenz
Pingback: Anker
Pingback: meine Verbindung
Pingback: Klicken Sie hier, um mehr zu erfahren
Pingback: Klick für mehr
Pingback: Back brace posture corrector
Pingback: nützliche Referenz
Pingback: lesen Sie dies
Pingback: prüfe das
Pingback: Web site
Pingback: Back brace posture corrector
Pingback: probiere das aus
Pingback: schau auf diese Webseite
Pingback: meine Firma
Pingback: dieser Link
Pingback: großartige Seite
Pingback: Back posture corrector for men
Pingback: Best posture corrector
Pingback: explain yanny or laurel
Pingback: Back posture corrector for men
Pingback: Back posture corrector for men
Pingback: Back brace posture corrector
Pingback: Perfect posture
Pingback: Posture corrector for women under clothes
Pingback: Back posture corrector for men
Pingback: Back posture corrector for men
Pingback: Online Shops in Ecuador
Pingback: Best posture corrector
Pingback: Hong Kong Online
Pingback: Best posture corrector
Pingback: Go Here
Pingback: Visit Website
Pingback: Discover More
Pingback: Read This
Pingback: palm leaf plates wedding
Pingback: eco friendly wedding tableware
Pingback: jaytsujimura
Pingback: Find Out More
Pingback: eco friendly wedding tableware
Pingback: compostable wine glasses
Pingback: Discover More Here
Pingback: gold rimmed plastic plates
Pingback: Discover More Here
Pingback: Home Page
Pingback: Going Here
Pingback: Going Here
Pingback: Find Out More
Pingback: Click This Link
Pingback: Discover More Here
Pingback: Find Out More
Pingback: ofw entrepreneur
Pingback: smart negosyo
Pingback: internet page
Pingback: website
Pingback: Discover More Here
Pingback: Home Page
Pingback: website seo
Pingback: Read More Here
Pingback: vapormax off white
Pingback: Posture brace for women
Pingback: Best posture corrector
Pingback: Back brace posture corrector
Pingback: Perfect posture
Pingback: Posture brace for women
Pingback: Back posture corrector for men
Pingback: Transfert Aéroport Marrakech
Pingback: Back posture corrector for men
Pingback: Perfect posture
Pingback: Posture corrector for women under clothes
Pingback: Perfect posture
Pingback: Perfect posture
Pingback: Posture corrector for women under clothes
Pingback: Posture corrector for women under clothes
Pingback: Back brace posture corrector
Pingback: Back posture corrector for men
Pingback: Best posture corrector
Pingback: Posture brace for women
Pingback: Posture corrector for women under clothes
Pingback: Posture brace for women
Pingback: Back posture corrector for men
Pingback: Back brace posture corrector
Pingback: Back brace posture corrector
Pingback: Posture corrector for women under clothes
Pingback: Back brace posture corrector
Pingback: Back brace posture corrector
Pingback: Posture brace for women
Pingback: Best posture corrector
Pingback: Back posture corrector for men
Pingback: Back brace posture corrector
Pingback: Perfect posture
Pingback: Back brace posture corrector
Pingback: paneles solares para piscinas
Pingback: Back posture corrector for men
Pingback: Posture corrector for women under clothes
Pingback: Back posture corrector for men
Pingback: Perfect posture
Pingback: Back brace posture corrector
Pingback: Back brace posture corrector
Pingback: Posture corrector for women under clothes
Pingback: firmware
Pingback: Posture brace for women
Pingback: hardware
Pingback: Back brace posture corrector
Pingback: Posture corrector for women under clothes
Pingback: Back brace posture corrector
Pingback: Perfect posture
Pingback: Back posture corrector for men
Pingback: Back posture corrector for men
Pingback: Best posture corrector
Pingback: software
Pingback: update
Pingback: atualizar
Pingback: Back brace posture corrector
Pingback: Best posture corrector
Pingback: Posture brace for women
Pingback: Perfect posture
Pingback: Inspirational community
Pingback: Back posture corrector for men
Pingback: Back posture corrector for men
Pingback: where to buy clones
Pingback: female escort directory
Pingback: junk cars in queens
Pingback: where can i buy marijuana clones
Pingback: growing clones
Pingback: plant cloning gel
Pingback: pot clones
Pingback: Wolfgang Halbig
Pingback: dangers of marijuana
Pingback: Wolfgang Halbig
Pingback: medical marijuana doctors
Pingback: hublot big bang carbon
Pingback: buy weed clones online
Pingback: servidor de cs net criciuma
Pingback: medical marijuana for sale
Pingback: best rooting hormone for clones
Pingback: Wolfgang Halbig
Pingback: marijuana pictures
Pingback: best way to clone plants
Pingback: truth about marijuana
Pingback: curing marijuana
Pingback: servidor cs net santos
Pingback: mail order clones
Pingback: Http://toyotahaiduong.info
Pingback: cloning in soil made easy
Pingback: growing marijuana from clones
Pingback: Steve Engravalle Imagine
Pingback: Steven Engravalle Twitter
Pingback: california marijuana legalization
Pingback: Wolfgang Halbig
Pingback: Wolfgang Halbig
Pingback: home cleaning services
Pingback: air duct cleaning companies
Pingback: central air duct cleaning
Pingback: dryer vent cleaning service
Pingback: Steve Engravalle Education
Pingback: how to clean your air ducts
Pingback: dryer vent cleaning brighton
Pingback: cleaning air ducts yourself
Pingback: Terracotta Wall Cladding
Pingback: Wolfgang Halbig
Pingback: house vent cleaning
Pingback: the carpet cleaning company
Pingback: air care duct cleaning
Pingback: duct cleaning company
Pingback: clean out air ducts
Pingback: roseville cal
Pingback: home cleaning company
Pingback: cost for air duct cleaning
Pingback: Terracotta Panel
Pingback: carpet shampooing service
Pingback: ducts cleaner home services
Pingback: sacramento ca hvac
Pingback: cleaning services home
Pingback: home air vent
Pingback: duct cleaning twin cities
Pingback: carpet cleaning repair
Pingback: Wolfgang Halbig
Pingback: cleaning services carpet
Pingback: carpet cleaning service reviews
Pingback: provedor do cs net belem
Pingback: free charity cars
Pingback: Terracotta Tile
Pingback: cars for charity
Pingback: text to donate
Pingback: npr car donation program
Pingback: donate a car to me
Pingback: tax value of my car
Pingback: car donation md
Pingback: Steven Engravalle Technology
Pingback: 1800 donate cars
Pingback: donate the car
Pingback: cars for cancer donation
Pingback: where to donate your car
Pingback: how can i get a free car donated to me
Pingback: pbs donate car
Pingback: donate car to goodwill
Pingback: places to donate a car
Pingback: npr donate
Pingback: Privacy Policy
Pingback: car boat vehicle
Pingback: car donation utah
Pingback: donate a car canada
Pingback: Ambika Ahuja Jaipur Escorts
Pingback: if i donate a car is it tax deductible
Pingback: bath roofer
Pingback: NEHA TYAGI MODEL JAIPUR ESCORTS
Pingback: JAIPUR ESCORTS ALIYA SINHA
Pingback: BANGALORE COMPANION ESCORTS
Pingback: Dhruvi Jaipur Escorts
Pingback: JAIPUR ESCORTS MODEL DRISHYA
Pingback: Heena Khan Bangalore Escorts
Pingback: Godrej Meridien Gurgaon
Pingback: next page
Pingback: Jiya Malik High Profile Jaipur Escorts Model
Pingback: FUN WITH JAIPUR ESCORTS PUJA KAUR
Pingback: More hints
Pingback: XXX BANGALORE ESCORTS
Pingback: XXX PORN SAPNA CHAUDHARY ESCORTS
Pingback: bath roofer
Pingback: Selly Arora Independent Bangalore Escorts
Pingback: cannabis legale
Pingback: Enjoy With Jaipur Escorts Tanisha Walia
Pingback: RUBEENA RUSSIAN BANGALORE ESCORTS
Pingback: Resources
Pingback: Bristy Roy Independent Bangalore Escorts
Pingback: XXX PORN SRUTHI PATHAK MODEL ESCORTS
Pingback: Bangalore Escorts Sneha Despandey
Pingback: More hints
Pingback: XXX PORN Radhika Apte Model Escort
Pingback: bath roofer
Pingback: Resources
Pingback: More Help
Pingback: Extra resources
Pingback: additional reading
Pingback: Continue Reading
Pingback: helpful resources
Pingback: Our site
Pingback: Continued
Pingback: next page
Pingback: bath builder
Pingback: bath builder
Pingback: More Bonuses
Pingback: Extra resources
Pingback: Bonuses
Pingback: Continue
Pingback: More hints
Pingback: next page
Pingback: Our site
Pingback: american alsatians
Pingback: chihuahua poodle mix
Pingback: blackmouth cur
Pingback: how much do puppies sleep
Pingback: estrela mountain dog
Pingback: northern inuit dog
Pingback: shikoku inu puppy
Pingback: kerry blue terrier
Pingback: shih tzu maltese
Pingback: cannabis legale shop online
Pingback: More hints
Pingback: koolie
Pingback: hokkaido dog
Pingback: mudi
Pingback: frenchton
Pingback: native american indian dog
Pingback: cavapoo
Pingback: shikoku dog
Pingback: zuchon
Pingback: helpful hints
Pingback: maltipoo
Pingback: More Bonuses
Pingback: Continue Reading
Pingback: bearded dragon temperament
Pingback: aussie doodle
Pingback: cur dog
Pingback: labrador husky
Pingback: german spitz midget
Pingback: shikoku ken
Pingback: tamaskan dog
Pingback: squirrel dog breeds
Pingback: Border Collie Mix
Pingback: husky poodle mix
Pingback: pitbull puppies for sale
Pingback: dogs under 30 pounds
Pingback: blue lacy dog
Pingback: shichon
Pingback: rottweiler german shepherd mix
Pingback: american bully dog
Pingback: zuchon
Pingback: lurcher
Pingback: Lagotto Romagnolo
Pingback: boston bulldog
Pingback: shikoku dog
Pingback: australian labradoodle
Pingback: japanese spitz
Pingback: qualified company secretary
Pingback: puggle
Pingback: parson russell terrier
Pingback: australian labradoodle
Pingback: cheagle
Pingback: shikoku inu puppy
Pingback: ovcharka
Pingback: accountant fees for small business
Pingback: australian labradoodles
Pingback: bullboxer
Pingback: chihuahua corgi mix
Pingback: zuchon
Pingback: Pocket Pitbull
Pingback: goberian
Pingback: corgi chihuahua mix
Pingback: Pocket Pitbull
Pingback: pitbull puppies for sale
Pingback: carolina dog breed
Pingback: presa canarios pictures
Pingback: australian shepherd golden retriever mix
Pingback: how to register a company name
Pingback: blue lacy dog
Pingback: mountain feist dogs
Pingback: northern inuit dog
Pingback: cur representative species
Pingback: beagle mix
Pingback: sarplaninac
Pingback: american bully vs pitbull
Pingback: labrabull
Pingback: Chorkie
Pingback: whelping puppies
Pingback: czech wolfdog
Pingback: american white shepherd
Pingback: cheap rubber stamps
Pingback: silver labrador
Pingback: lab pit mix
Pingback: invoice book printing
Pingback: Peekapoo
Pingback: custom receipt book printing
Pingback: victorian bulldog
Pingback: anatolian shepherd mix
Pingback: german shepherd collie mix
Pingback: american foxhound puppies
Pingback: bullboxer
Pingback: teacup poodles
Pingback: dorgi
Pingback: company registered office address service
Pingback: company registration address
Pingback: white shepherd puppies
Pingback: poogle
Pingback: moyen poodle
Pingback: german shepherd puppies for sale
Pingback: victorian bulldog
Pingback: chihuahua dachshund mix
Pingback: mini english bulldog
Pingback: presa canarios pictures
Pingback: shikoku dog
Pingback: sheprador
Pingback: boxador
Pingback: bandog
Pingback: dorkie
Pingback: poogle
Pingback: chihuahua pomeranian mix
Pingback: Top 10 WhatsApp Tricks That You Should Know 2018
Pingback: white swiss shepherd
Pingback: caucasian mountain shepherd
Pingback: white doberman
Pingback: kangal
Pingback: types of shepherds
Pingback: malamute wolf hybrids
Pingback: corporate secretarial services
Pingback: 30 pound dog breeds
Pingback: landseer
Pingback: great dane pitbull mix
Pingback: mini golden doodle
Pingback: leonbergers pictures
Pingback: codejatt
Pingback: beagle mix
Pingback: cur dog breed
Pingback: landseer newfoundland
Pingback: corgi australian shepherd mix
Pingback: blue lacy dog
Pingback: caucasian mountain shepherd
Pingback: Native American Indian Dog
Pingback: pomsky puppies for sale
Pingback: german pinscher
Pingback: registered business address
Pingback: dorkie
Pingback: mini golden doodle
Pingback: chihuahua puppies for sale
Pingback: lab pit mix
Pingback: dingo dog
Pingback: blue lacy dog
Pingback: berger blanc suisse
Pingback: american bully vs pitbull
Pingback: bernedoodle
Pingback: corporate secretarial services singapore
Pingback: miki dog
Pingback: landseer newfoundland
Pingback: appenzeller sennenhund
Pingback: shepadoodle
Pingback: yorkie puppies for sale
Pingback: treeing feist
Pingback: Saarloos Wolfdog
Pingback: puppies for sale in pa
Pingback: maltese yorkie mix
Pingback: english mastiff puppies
Pingback: register a company
Pingback: firm registration
Pingback: types of bulldogs
Pingback: puppies for sale
Pingback: bookkeeping services singapore
Pingback: designer saree
Pingback: pug husky mix
Pingback: blue lacy dog
Pingback: types of shepherd dogs
Pingback: beagle mix
Pingback: presa canarios pictures
Pingback: czech wolfdog
Pingback: Gerberian Shepsky
Pingback: pitsky
Pingback: corgipoo
Pingback: american bullies
Pingback: corgipoo
Pingback: company secretary services singapore
Pingback: hhttps://disqus.com/by/disqus_BE5dbslalc/
Pingback: hhttps://disqus.com/by/disqus_BE5dbslalc/
Pingback: dalmatian puppies
Pingback: register my business name
Pingback: Learn More
Pingback: Find Out More
Pingback: shiloh shepherd dog
Pingback: shih tzu poodle mix
Pingback: bandogge mastiff
Pingback: sugar glider pet
Pingback: corgi pitbull mix
Pingback: golden retriever lab mix
Pingback: native american indian dog
Pingback: puppies for sale in pa
Pingback: lhasa poo
Pingback: Find Out More
Pingback: king german shepherd
Pingback: shih poo
Pingback: Go Here
Pingback: whelping puppies
Pingback: king german shepherd
Pingback: lurcher
Pingback: mudi
Pingback: Click Here
Pingback: the formations company
Pingback: Kolkata Escorts
Pingback: mini labradoodle
Pingback: chinese crested powder puff
Pingback: 30 lb dog breeds
Pingback: Click Here
Pingback: Learn More
Pingback: Learn More
Pingback: appenzeller sennenhund
Pingback: Read More
Pingback: company secretary services singapore
Pingback: personalized rubber stamps
Pingback: Go Here
Pingback: pomeranian puppies for sale
Pingback: Clicking Here
Pingback: pariah dog
Pingback: shiloh shepherds
Pingback: Going Here
Pingback: feist dog breed
Pingback: Read This
Pingback: Beagle Mix
Pingback: incorporated business
Pingback: Read This
Pingback: Go Here
Pingback: russian bear hunting dog
Pingback: pomeranian puppies for sale
Pingback: anerican bully
Pingback: dingo dog
Pingback: Go Here
Pingback: eurasier
Pingback: tamaskan dog
Pingback: Discover More
Pingback: maltipoo
Pingback: do hounds shed
Pingback: Find Out More
Pingback: Clicking Here
Pingback: Saarloos Wolfdog
Pingback: dachshund puppies for sale
Pingback: incorporation of companies
Pingback: german shepherd doberman mix
Pingback: Read More
Pingback: Discover More
Pingback: great dane pitbull mix
Pingback: dich vu seo gia re
Pingback: teacup poodles
Pingback: Going Here
Pingback: drahthaar
Pingback: hokkaido dog
Pingback: dich vu seo la gi
Pingback: Discover More
Pingback: cavachon
Pingback: husky puppies for sale
Pingback: Learn More
Pingback: moyen poodle
Pingback: Learn More
Pingback: Clicking Here
Pingback: pitbull chihuahua mix
Pingback: cur dog
Pingback: Clicking Here
Pingback: pomeranian chihuahua
Pingback: pomsky
Pingback: Go Here
Pingback: american alsation
Pingback: golden shepherd
Pingback: Read This
Pingback: Clicking Here
Pingback: cavapoo
Pingback: dich vu seo tu khoa
Pingback: chipoo
Pingback: mi-ki
Pingback: hokkaido dog
Pingback: leonbergers pictures
Pingback: 30 lb dog breeds
Pingback: how much do puppies sleep
Pingback: husky pug mix
Pingback: colorado bulldog
Pingback: berger blanc suisse
Pingback: german shepherd collie mix
Pingback: self inking rubber stamps
Pingback: english shepherd
Pingback: bernedoodle
Pingback: shikoku dog
Pingback: set up of company
Pingback: Sylvester Alvord
Pingback: german shepherd australian shepherd mix
Pingback: bandog
Pingback: yorkie chihuahua mix
Pingback: shikoku ken
Pingback: shikoku inu puppy
Pingback: Golden Cocker Retriever
Pingback: squirrel dog breeds
Pingback: Saarloos Wolfdog
Pingback: cheap custom rubber stamps
Pingback: american bully
Pingback: american bandogge mastiff
Pingback: irish water spaniel
Pingback: wolf hybrid puppies
Pingback: alabai dog
Pingback: Border Collie Mix
Pingback: mudi dog
Pingback: dog breeds under 30 pounds
Pingback: malshi
Pingback: victorian bulldog
Pingback: american bandogge
Pingback: great pyrenees lab mix
Pingback: russian mountain dog
Pingback: Gerberian Shepsky
Pingback: mini golden doodle
Pingback: japanese tosa
Pingback: how much do puppies sleep
Pingback: corporation registration
Pingback: biewer terrier
Pingback: toy aussie size
Pingback: shikoku inu
Pingback: business incorporation services
Pingback: american indian dog
Pingback: king german shepherd
Pingback: maltese yorkie mix
Pingback: custom name stamp
Pingback: Maxie Wingham
Pingback: german shepherd australian shepherd mix
Pingback: chinese imperials
Pingback: presser canary dogs
Pingback: company secretary requirements
Pingback: chihuahua poodle mix
Pingback: jack russell chihuahua mix
Pingback: corgi puppies for sale
Pingback: register my business name
Pingback: company secretarial services package
Pingback: teacup poodles
Pingback: miki dog
Pingback: yorkie chihuahua mix
Pingback: shikoku inu
Pingback: biewer terrier
Pingback: american indian dog
Pingback: mini labradoodle
Pingback: american bully puppies
Pingback: shikoku inu
Pingback: rat terrier chihuahua mix
Pingback: kerry blue terrier
Pingback: husky poodle mix
Pingback: russian mountain dog
Pingback: do hounds shed
Pingback: teacup poodles
Pingback: caucasian mountain shepherd
Pingback: berger blanc suisse
Pingback: labrabull
Pingback: anatolian shepherd mix
Pingback: chihuahua pomeranian mix
Pingback: mastador
Pingback: pitbull german shepherd mix
Pingback: dog temperament
Pingback: german shepherd puppies for sale
Pingback: american bully dog
Pingback: shiloh shepherd
Pingback: yorkie puppies for sale
Pingback: llewellin setters
Pingback: native american dog
Pingback: corgi pug mix
Pingback: caucasian mountain shepherd
Pingback: german shepherd mix
Pingback: rottweiler puppies for sale
Pingback: canary islands mastiff
Pingback: boxer puppies for sale
Pingback: japanese spitz
Pingback: northern inuit dog
Pingback: beagle mix
Pingback: corporate secretarial services
Pingback: Brindle Pitbull
Pingback: chinese crested powder puff
Pingback: poogle
Pingback: russian bear hunting dog
Pingback: how to register a business
Pingback: cheap company secretary singapore
Pingback: Cloud Drive
Pingback: registered address service singapore
Pingback: business formation
Pingback: cost of incorporating a company
Pingback: registered business address
Pingback: bookkeeping services singapore
Pingback: d?ch v? seo t?i Äà n?ng
Pingback: company registered office address
Pingback: company registered office address service
Pingback: Discover More
Pingback: Clicking Here
Pingback: Read This
Pingback: Discover More
Pingback: Learn Chinese
Pingback: d?ch v? seo top
Pingback: black mold
Pingback: d?ch v? seo uy tín tphcm
Pingback: Singapore company registration
Pingback: cryptocurrency
Pingback: change registered office address
Pingback: pvt ltd company registration
Pingback: Alpha9
Pingback: incorporation of private limited company
Pingback: change company registered address
Pingback: duties of a company secretary
Pingback: Supra TK Society
Pingback: invoice book printing
Pingback: how to register a company name
Pingback: company registration services
Pingback: role of company secretary
Pingback: receipt book printing
Pingback: clickfunnels free trial
Pingback: what is clickfunnels
Pingback: 4K Cinema HDR
Pingback: accounting service provider
Pingback: company registration singapore
Pingback: what is clickfunnels
Pingback: what is clickfunnels
Pingback: accounting companies
Pingback: BinBase review
Pingback: bookkeeping services
Pingback: Glass Design
Pingback: outsourced bookkeeping services
Pingback: custom made stamps
Pingback: newly setup company
Pingback: clickfunnels free trial
Pingback: clickfunnels review
Pingback: best accounting services
Pingback: cost of incorporating a company
Pingback: custom receipt book printing
Pingback: company registration address
Pingback: corporate secretarial services singapore
Pingback: Cinema Screen
Pingback: clickfunnels
Pingback: custom stamp maker
Pingback: clickfunnels
Pingback: OLED 55 C8
Pingback: cheap team soccer jerseys
Pingback: cheap company secretary singapore
Pingback: clickfunnels
Pingback: clickfunnels free trial
Pingback: custom stamps
Pingback: cpa firm
Pingback: accountant fees for small business
Pingback: business registration address
Pingback: Dolby Atmos
Pingback: Virtual office Singapore
Pingback: how to check company registration
Pingback: myob accounting
Pingback: TruMotion 240
Pingback: outsourced bookkeeping services
Pingback: company registration
Pingback: chartered accountant
Pingback: cheap secretarial services singapore
Pingback: natural hair conditioner coconut
Pingback: how to incorporate a company
Pingback: styling cream men
Pingback: company set up
Pingback: cheap address stamps
Pingback: name card design
Pingback: myob accounting
Pingback: hair curl products
Pingback: Pinyin Helper
Pingback: registered company
Pingback: incorporation of companies
Pingback: sme accounting services
Pingback: Fifa world cup 2018 prize money
Pingback: Best app for learning Chinese
Pingback: pre inked rubber stamps
Pingback: set up of company
Pingback: receipt book printing
Pingback: cheap secretarial services singapore
Pingback: sme accounting services
Pingback: top email marketing tools
Pingback: company name registration
Pingback: Learn Chinese easily
Pingback: registered office address service
Pingback: custom logo stamp
Pingback: Termite Control Imperial Beach
Pingback: company registration services
Pingback: Pest Control Goldenrod
Pingback: The thao tin nhanh, bong da
Pingback: World cup 2018 opening ceremony
Pingback: Free Online Movies
Pingback: Watch asian Series
Pingback: Comedy Movies
Pingback: Crime movies online
Pingback: Movies
Pingback: Watch Movies 2017 Online
Pingback: style
Pingback: Thrilling Movies
Pingback: retiree
Pingback: Musical Movies
Pingback: get a new job
Pingback: Western movies
Pingback: Photo Liker
Pingback: Watch free wrestling online
Pingback: Sports Movies
Pingback: English movies online
Pingback: Free Online Movies
Pingback: video chat
Pingback: tv show host
Pingback: Myers-Brigg Type Indicator (MBTI)
Pingback: AutoCommenter
Pingback: Aygıtlar
Pingback: job is making me sick
Pingback: board certified coach
Pingback: Facebook
Pingback: ECO-PGC
Pingback: job is making me sick
Pingback: Auto Liker
Pingback: soft skills training
Pingback: twitter
Pingback: Prince Georges County
Pingback: about Dr. Charles
Pingback: Real Price Silver
Pingback: financial aid
Pingback: soft skills training
Pingback: career satisfaction
Pingback: China Link
Pingback: voiceover talent
Pingback: mt57387tcyn43mtyd7td
Pingback: Simplified Software Solutions India
Pingback: Mobile app development company
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: qqpoker
Pingback: car rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental Orlando
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: activewear
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Custom ERP Software Development Company
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: online shipping in UAE
Pingback: car rental in Amsterdam
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: car rental Turkey
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Lauderdale Carngo
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Palermo Car Rental
Pingback: pug crossed with boston terrier
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental Langkawi
Pingback: car rental in Orlando
Pingback: Car rental in Marrakech
Pingback: Car Rental
Pingback: pictures of terriers dog types
Pingback: activewear
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental
Pingback: Car Rental
Pingback: Car Rental
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: AutoCommenter
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Car Rental Langkawi
Pingback: Car Rental
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Palermo Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental Palermo
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Hot & Spicy Chicken and Poultry Recipes
Pingback: Best 500 Hot & Spicy Recipes
Pingback: Car Rental
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: travel around the world
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: rent a car in Frankfurt
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Mietwagen
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: Car Rental
Pingback: Web Design
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Car Rental
Pingback: Aves exoticas
Pingback: Car Rental
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Mietwagen
Pingback: Car Rental
Pingback: Offerte noleggio auto in Italia
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Hot & Spicy Soups Recipes
Pingback: Hot & Spicy Appetizers and Light Meals Recipes
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: travel around the world
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Website Design
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Hot & Spicy Fish and Shellfish Recipes
Pingback: Aves exoticas
Pingback: Hot & Spicy Desserts and Drinks Recipes
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Spicy Meat and Beef Recipes
Pingback: Aves exoticas
Pingback: Spicy Rice and Noodles Recipes
Pingback: Aves exoticas
Pingback: world travel
Pingback: www.ventaavesexoticas.com
Pingback: www.ventaavesexoticas.com
Pingback: Aves exoticas
Pingback: Website Design
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: free quote foundation repair san antonio texas
Pingback: Aves exoticas
Pingback: Spicy Side Dishes and Accompaniments Recipes
Pingback: Aves exoticas
Pingback: Spicy Vegetarian Main Dishes Recipes
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: free quote foundation repair companies san antonio tx
Pingback: best slab repair contractor in san antonio texas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Top sunken driveway slabs repair companies in san antonio texas
Pingback: Aves exoticas
Pingback: travel around the world
Pingback: Cheap foundation companies san antonio
Pingback: Aves exoticas
Pingback: top foundation repair contractors in san antonio near me
Pingback: Aves exoticas
Pingback: PolyLevel Injection Foam to Raise Settled Concrete in san antonio
Pingback: Foundation Repair for concrete slab san antonio tx
Pingback: best pier and beam foundation repair contractors san antonio tx
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: top slab repair contractor in san antonio tx
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: foundation repair companies in san antonio tx
Pingback: best pier and beam foundation repair companies san antonio
Pingback: low cost foundation companies san antonio
Pingback: Web Design
Pingback: Aves exoticas
Pingback: Lift settled slab san antonio
Pingback: Aves exoticas
Pingback: raised slab foundation repair san antonio near me
Pingback: Aves exoticas
Pingback: Top sunken driveway slabs repair companies in san antonio tx
Pingback: Aves exoticas
Pingback: under-slab plumbing leak repair san antonio tx
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Foundation Repair for concrete slabs in San antonio tx
Pingback: Aves exoticas
Pingback: under-slab plumbing leaks repair san antonio tx
Pingback: concrete slab repair contractors san antonio
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Hoaxer
Pingback: games for pc download
Pingback: free download for windows pc
Pingback: apps download for windows 7
Pingback: apps download for windows 10
Pingback: games for pc download
Pingback: download games for windows 7
Pingback: free apps download for windows 10
Pingback: free download for pc windows
Pingback: apps download for windows 7
Pingback: free pc games download full version for windows 7
Pingback: free download for laptop
Pingback: download games for pc
Pingback: free download for windows 8
Pingback: free download for windows 7
Pingback: app download for windows 7
Pingback: pc app free download
Pingback: pc games free download for mac
Pingback: pc games free download for windows 8
Pingback: pc games apps for laptop
Pingback: Hoaxer
Pingback: app download for pc
Pingback: app download for windows 8
Pingback: free laptop games download
Pingback: pc apps for windows xp
Pingback: free games download for windows 8
Pingback: software download for windows 8
Pingback: games for windows pc download
Pingback: apps download for windows 7
Pingback: app download for windows 8
Pingback: free windows app download
Pingback: apps for pc download
Pingback: software download for windows 10
Pingback: apps download for pc
Pingback: app pc download for windows
Pingback: apps download for pc
Pingback: free app for laptop
Pingback: free app download
Pingback: free download for windows 10
Pingback: free download for windows 8
Pingback: pc games for windows 8
Pingback: free download for windows 8
Pingback: free download for windows 7
Pingback: pc games free download for windows 10
Pingback: free software download for windows 7
Pingback: free app for laptop
Pingback: free download for pc windows
Pingback: software download for pc
Pingback: app download for windows 8
Pingback: app for pc download
Pingback: free download for windows pc
Pingback: apps for pc download
Pingback: free download for pc windows
Pingback: app download for windows 10
Pingback: free full download for windows
Pingback: app for laptop
Pingback: free apps for pc download
Pingback: free download for windows 8
Pingback: apps download for pc
Pingback: app download for windows
Pingback: free download for windows 7
Pingback: download games for pc
Pingback: pc games apps for laptop
Pingback: pc games free download full version for windows 10
Pingback: pc app free download
Pingback: free download for windows 10
Pingback: apps for pc free download
Pingback: app for pc download
Pingback: app download for pc
Pingback: apps for pc
Pingback: pc apps for windows 10
Pingback: games for pc download
Pingback: free games download for windows 8
Pingback: apps for pc download
Pingback: apps download for pc
Pingback: free download for laptop
Pingback: games for windows pc download
Pingback: pc games free download full version for windows 8
Pingback: free download for pc
Pingback: free app for pclaptop app free download
Pingback: pc games free download for windows xp
Pingback: pc games free download for windows 8
Pingback: games pc download
Pingback: apps download for windows 7
Pingback: pc app free download
Pingback: pc games apps free download
Pingback: Aves exoticas
Pingback: pc app free download
Pingback: games for pc download
Pingback: free software download for windows 10
Pingback: pc games free download for windows 10
Pingback: Aves exoticas
Pingback: apps download for windows 10
Pingback: free apps download for windows 10
Pingback: Marijuana
Pingback: pc games for windows 10
Pingback: free download for windows pc
Pingback: apps download for windows 7
Pingback: apps for pc free download
Pingback: Aves exoticas
Pingback: pc app for windows 10
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: download games for windows 8
Pingback: free download for pc
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: software download for windows 8
Pingback: cmwy54tygvnegmicwv53ec
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Aves exoticas
Pingback: Judi Togel
Pingback: Men's Sports Compression Wear
Pingback: Sports Compression shirts
Pingback: Click Here
Pingback: cheap soccer jerseys wholesale
Pingback: Home Page
Pingback: Executive Sponsorship
Pingback: Executive Sponsorship
Pingback: Performance Management
Pingback: Executive Development
Pingback: Resources Planning
Pingback: pc games for windows 8
Pingback: Discover More Here
Pingback: Employer Value Proposition
Pingback: Human Resource Systems
Pingback: Merger and Acquisition
Pingback: HR Policy Development and Execution
Pingback: Human Resource Systems
Pingback: Training and Development
Pingback: Payroll Administration
Pingback: Talent Development
Pingback: Industrial Relations
Pingback: Click This Link
Pingback: Training and Development
Pingback: Benefits and Compensation
Pingback: Resources Planning
Pingback: Click This Link
Pingback: Visit This Link
Pingback: Lawsuit Settlement Assistance
Pingback: Employee Assistance and Wellness
Pingback: Recruitment and Selection
Pingback: Occupational Health and Safety
Pingback: pc games apps free download
Pingback: Merger and Acquisition
Pingback: Contract Negotiation
Pingback: Learn More
Pingback: Read This
Pingback: Employer Value Proposition
Pingback: Discover More Here
Pingback: Occupational Health and Safety
Pingback: Read More
Pingback: Benefits and Compensation
Pingback: Learn More
Pingback: play games no download
Pingback: Occupational Health and Safety
Pingback: Human Resource Systems
Pingback: Human Resource Systems
Pingback: Collective Agreement
Pingback: Settlement Negotiations
Pingback: hhttp://9club.co/forum/profile.php?id=364773
Pingback: Read More
Pingback: Discover More
Pingback: Read This
Pingback: Employer Value Proposition
Pingback: Talent Development
Pingback: Grievance and Arbitration
Pingback: Job Analysis
Pingback: HR Policy Development and Execution
Pingback: Executive Sponsorship
Pingback: Industrial Relations
Pingback: Occupational Health and Safety
Pingback: Human Resource Administration
Pingback: Collective Agreement
Pingback: Payroll Administration
Pingback: Read More
Pingback: Executive Development
Pingback: Collective Agreement
Pingback: we buy any house falls church va
Pingback: sell my house in virginia
Pingback: urbanx development falls church va
Pingback: urbanx development falls church va
Pingback: sell my house in virginia
Pingback: sell my house in virginia
Pingback: urbanx development falls church va
Pingback: cash home buyers falls church
Pingback: cash home buyers falls church
Pingback: cash home buyers falls church
Pingback: we buy any house falls church va
Pingback: we buy any house falls church va
Pingback: play online games
Pingback: sell my house in maryland
Pingback: sell my house in virginia
Pingback: sell my house in maryland
Pingback: sell my house in maryland
Pingback: we buy any house falls church va
Pingback: urbanx development falls church va
Pingback: sell my house in virginia
Pingback: pc app free download
Pingback: urbanx development falls church va
Pingback: games for pc download
Pingback: cash home buyers falls church
Pingback: sell my house in washington dc
Pingback: free download for windows pc
Pingback: sell my house in virginia
Pingback: sell my house in virginia
Pingback: pc games for windows 10
Pingback: we buy any house falls church va
Pingback: cash home buyers falls church
Pingback: cash home buyers falls church
Pingback: sell my house in virginia
Pingback: sell my house in virginia
Pingback: sell my house in washington dc
Pingback: urbanx development falls church va
Pingback: sell my house in virginia
Pingback: sell my house in virginia
Pingback: sell my house in maryland
Pingback: sell my house in virginia
Pingback: urbanx development falls church va
Pingback: we buy any house falls church va
Pingback: sell my house in maryland
Pingback: sell my house in washington dc
Pingback: sell my house in virginia
Pingback: urbanx development falls church va
Pingback: sell my house in maryland
Pingback: sell my house in virginia
Pingback: we buy any house falls church va
Pingback: urbanx development falls church va
Pingback: sell my house in maryland
Pingback: we buy any house falls church va
Pingback: we buy any house falls church va
Pingback: we buy any house falls church va
Pingback: sell my house in washington dc
Pingback: cash home buyers falls church
Pingback: urbanx development falls church va
Pingback: sell my house in virginia
Pingback: sell my house in washington dc
Pingback: pc games for windows 8
Pingback: free download for pc windows
Pingback: urbanx development falls church va
Pingback: cash home buyers falls church
Pingback: sell my house in washington dc
Pingback: we buy any house falls church va
Pingback: urbanx development falls church va
Pingback: pc games for windows 7
Pingback: pc games for windows 7
Pingback: games for pc download
Pingback: apps download for windows 10
Pingback: hotmail login
Pingback: apps download for windows 7
Pingback: free download for windows 10
Pingback: pc games for windows 7
Pingback: free download for windows 8
Pingback: games for pc download
Pingback: apps download for windows 8
Pingback: free download for windows 7
Pingback: free app for pc
Pingback: free windows app download
Pingback: free app for pc
Pingback: free laptop games download
Pingback: laptop app free download
Pingback: free app for pc
Pingback: free pc games download
Pingback: app for laptop
Pingback: free download for pc windows
Pingback: free app for pc
Pingback: free pc games download
Pingback: free download for windows 8
Pingback: keywords:free download for windows 7
Pingback: free download for pc
Pingback: app for laptop
Pingback: games for pc download
Pingback: pc app free download
Pingback: Discover More Here
Pingback: Find Out More
Pingback: laptop app
Pingback: free app for pc
Pingback: Discover More Here
Pingback: Click Here
Pingback: This Site
Pingback: Discover More Here
Pingback: This Site
Pingback: free download for windows 8
Pingback: free download for pc
Pingback: Homepage
Pingback: Discover More Here
Pingback: Home Page
Pingback: free app for laptop
Pingback: laptop app
Pingback: Website
Pingback: Discover More Here
Pingback: pc games free download
Pingback: Read This
Pingback: Click Here
Pingback: Clicking Here
Pingback: Click This Link
Pingback: play online games
Pingback: Get More Information
Pingback: This Site
Pingback: Read This
Pingback: Get More Information
Pingback: Web Site
Pingback: Discover More Here
Pingback: play games on pc
Pingback: Visit This Link
Pingback: Click Here
Pingback: Get More Info
Pingback: play free pc games
Pingback: Going Here
Pingback: Click This Link
Pingback: pc games for windows 8
Pingback: Get More Info
Pingback: Visit Website
Pingback: Going Here
Pingback: Learn More Here
Pingback: Click Here
Pingback: Discover More
Pingback: Discover More
Pingback: Clicking Here
Pingback: pubg mobile
Pingback: pc games for windows 8
Pingback: Discover More Here
Pingback: pc games for windows 8
Pingback: Discover More Here
Pingback: Click Here
Pingback: clash of clans
Pingback: Forex Ads
Pingback: candy crush soda saga
Pingback: Forex Ads
Pingback: Forex Ads
Pingback: Advertising Forex
Pingback: Advertising Forex
Pingback: Forex Directory
Pingback: Advertising Forex
Pingback: Forex Ads
Pingback: Forex Directory
Pingback: apps for pc download
Pingback: Advertising Forex
Pingback: candy crush soda saga
Pingback: Advertising Forex
Pingback: Forex Directory
Pingback: Advertising Forex
Pingback: Forex Directory
Pingback: Forex Directory
Pingback: Forex Directory
Pingback: the sims freeplay
Pingback: Forex Directory
Pingback: board kings
Pingback: Forex Ads
Pingback: Advertising Forex
Pingback: sonic dash
Pingback: pokemon go
Pingback: Advertising Forex
Pingback: Advertising Forex
Pingback: asphalt 8: airborne
Pingback: Advertising Forex
Pingback: Advertising Forex
Pingback: Forex Ads
Pingback: iron blade
Pingback: Legit Reviews
Pingback: Real Reviews
Pingback: Legit Reviews
Pingback: Real Reviews
Pingback: Real Reviews
Pingback: Trusted Reviews
Pingback: Legit Reviews
Pingback: Real Reviews
Pingback: Trusted Reviews
Pingback: Legit Reviews
Pingback: Real Reviews
Pingback: Legit Reviews
Pingback: ea sports ufc
Pingback: Trusted Reviews
Pingback: futurama: worlds of tomorrow
Pingback: forge empires
Pingback: game of thrones conquest
Pingback: hill climb racing 2
Pingback: sniper 3d
Pingback: king of avalon
Pingback: march of empires
Pingback: guild of heroes
Pingback: kritika the white knights
Pingback: rise of the kings
Pingback: olympus rising
Pingback: instagram followers and like
Pingback: wsop
Pingback: the sims mobile
Pingback: 카지노사이트추천
Pingback: School bus rental Sharjah
Pingback: Home Page
Pingback: Look At This
Pingback: Home Page
Pingback: Going Here
Pingback: Discover More Here
Pingback: Visit Website
Pingback: Click This Link
Pingback: Full Report
Pingback: Discover More
Pingback: Get More Information
Pingback: dumpster rental Carefree
Pingback: dumpster rental Gilbert
Pingback: trash bins for rent
Pingback: waste removal
Pingback: Waterproof televisions
Pingback: waste management rentals
Pingback: temporary dumpster
Pingback: 1800 junk
Pingback: 30 yard dumpster rental
Pingback: home dumpster service
Pingback: waste management dumpster rental cost
Pingback: 1800junk
Pingback: garbage hauling
Pingback: dumpster rental las vegas
Pingback: residential garbage removal
Pingback: night light speaker
Pingback: best price dumpster rental
Pingback: container rentals
Pingback: find a dump near me
Pingback: 7 yard dumpster
Pingback: bfi trash removal
Pingback: wastemanagement
Pingback: portable night light
Pingback: sauna accessories
Pingback: sauna accessories
Pingback: steam sauna kits
Pingback: diy sauna
Pingback: portable home sauna
Pingback: benefits of infrared sauna
Pingback: hot sauna
Pingback: outdoor saunas
Pingback: infrared saunas
Pingback: bluetooth lamp
Pingback: infrared sauna detoxification
Pingback: infrared sauna 2 person
Pingback: steam sauna bath
Pingback: sauna treatment
Pingback: sauna home
Pingback: small infrared sauna
Pingback: custom sauna
Pingback: gift for kids
Pingback: infrared sauna accessories
Pingback: health benefits of infrared sauna
Pingback: sauna sauna
Pingback: 2 car tent garage
Pingback: infrared outdoor sauna
Pingback: infrared sauna sale
Pingback: home saunas for sale
Pingback: relax infrared sauna
Pingback: red heat sauna
Pingback: sauna steam generator
Pingback: the best infrared sauna
Pingback: ir sauna benefits
Pingback: infrared sauna buy
Pingback: home saunas for sale
Pingback: 10 yard dumpster cost
Pingback: dumpster rental Powder Springs
Pingback: rent dumpster
Pingback: car shelter reviews
Pingback: waste management dumpster sizes
Pingback: trash dumpster rental
Pingback: dumpster cost
Pingback: construction dumpster
Pingback: dumpster rental canton
Pingback: rent a dumpster
Pingback: dumpster container
Pingback: dumpster removal
Pingback: concrete dumpster rental
Pingback: on site dumpster rental
Pingback: roll off trash containers
Pingback: garbage removal services
Pingback: dump containers for rent
Pingback: rubbish removal
Pingback: roll away trash containers
Pingback: dumpster bins for rent
Pingback: household dumpster rental
Pingback: dumpster rental canton
Pingback: roll off
Pingback: cheap dumpster rental
Pingback: dumpster rental Mableton
Pingback: waste removal
Pingback: junk removal companies
Pingback: rent a dump
Pingback: i need a dumpster rental
Pingback: trash haulers
Pingback: small dumpster rental prices
Pingback: big dumpster rental
Pingback: waste management 10 yard dumpster
Pingback: residential garbage removal
Pingback: trash removal companies
Pingback: find a dump near me
Pingback: Mariann Mcdavis
Pingback: Margeret Almond
Pingback: Susanne Seawright
Pingback: Raphael Pease
Pingback: Darline Kunst
Pingback: Roselle Prost
Pingback: Elmira Alcantara
Pingback: Danny Willis
Pingback: Venessa Smidt
Pingback: Vi Mcspadden
Pingback: Sheree Alaimo
Pingback: Fred Block
Pingback: Susanne Seawright
Pingback: Aletha Lish
Pingback: Carlyn Nicastro
Pingback: Kourtney Blay
Pingback: Armand Nordberg
Pingback: Cleora Pilling
Pingback: Becki Hammers
Pingback: Shemika Lipsett
Pingback: Latoya Kollar
Pingback: professeur
Pingback: teacher meet student
Pingback: Student
Pingback: education
Pingback: enseignant
Pingback: enseignant
Pingback: education
Pingback: education
Pingback: Teaching
Pingback: platform for teachers and students
Pingback: remedial teaching
Pingback: platform for teachers and students
Pingback: nightlight
Pingback: Green Star juicers parts
Pingback: online destination green
Pingback: Ultimate Green power juicer
Pingback: online destination buy juicers
Pingback: Green Star Juice
Pingback: ultimate online buy juicers
Pingback: greenstar juicers
Pingback: Ultimate green star 5000
Pingback: Green Star extractor
Pingback: digital marketing agency
Pingback: Mini classic water distiller
Pingback: destination green juicers
Pingback: destination green star juicers
Pingback: ultimate online green star
Pingback: ultimate Solo star juicers
Pingback: loft conversion architect plans
Pingback: adult rain cover
Pingback: adult ponchos for rain disney
Pingback: panchos rain
Pingback: rain poncho men
Pingback: rain poncho for kids
Pingback: disney accessories for the parks
Pingback: poncho rain pack
Pingback: plastic rain ponchos disposable
Pingback: childrens poncho
Pingback: disposable teen
Pingback: panchos rain
Pingback: family travel backpack
Pingback: child pack
Pingback: disposable ponchos family
Pingback: id bracelet for kids
Pingback: toddler poncho
Pingback: family travel backpack
Pingback: rain ponch
Pingback: kids poncho
Pingback: kids poncho
Pingback: kids emergency
Pingback: kids survival pack
Pingback: rain poncho for kids
Pingback: emergency rain poncho with hood
Pingback: ponchos family
Pingback: family travel backpack
Pingback: rain plastic poncho
Pingback: loft conversions london
Pingback: childrens emergency poncho
Pingback: rain ponchos for disney
Pingback: good poncho
Pingback: magic band bitbelts
Pingback: teen ponchos for rain
Pingback: ponchos child
Pingback: kids disposable ponchos
Pingback: reusable poncho
Pingback: rain ponchos for disney
Pingback: ponchos rain adult
Pingback: disposable poncho drawstring
Pingback: matador blanket pocket
Pingback: rain pncho
Pingback: Miele fridge repairs
Pingback: survival package for men
Pingback: ponchos disposable
Pingback: good poncho
Pingback: long sleeve arm covers for men
Pingback: their post
Pingback: this page
Pingback: this handy article
Pingback: great section on their site
Pingback: read the full post here.
Pingback: click here to read the entire article
Pingback: click here to read the entire article
Pingback: original link
Pingback: looking for vacuum cleaner automatic reviews
Pingback: cleaning robot
Pingback: great section on their site
Pingback: article they wrote
Pingback: click here to read
Pingback: original link
Pingback: in a blog post
Pingback: their post
Pingback: visit website
Pingback: automatic vacuum cleaner reviews ideas
Pingback: visit website
Pingback: a great blog article
Pingback: get more info
Pingback: check out this blog
Pingback: click here to read
Pingback: Click This Link
Pingback: Website
Pingback: Home Page
Pingback: This Site
Pingback: Read More
Pingback: Ethereum
Pingback: Homepage
Pingback: Home Page
Pingback: Visit This Link
Pingback: Home Page
Pingback: Learn More
Pingback: Learn More
Pingback: Visit Website
Pingback: Going Here
Pingback: Learn More
Pingback: Click This Link
Pingback: Find Out More
Pingback: Read More Here
Pingback: Read More
Pingback: Read More Here
Pingback: Discover More Here
Pingback: Learn More
Pingback: Visit This Link
Pingback: Homepage
Pingback: Visit Website
Pingback: Discover More
Pingback: Click Here
Pingback: Visit Website
Pingback: Discover More
Pingback: Discover More
Pingback: Homepage
Pingback: dumpster rental Aguila
Pingback: 10 cubic yard dumpster
Pingback: 40 yard dumpster
Pingback: Web Site
Pingback: waste management dumpster rental
Pingback: disposal bin rental
Pingback: residential dumpster rental
Pingback: dumpster rental Desert Hills
Pingback: 10 cubic yard dumpster
Pingback: dumpster rental Mesa
Pingback: roll off dumpster
Pingback: yard waste removal
Pingback: waste management company
Pingback: roll off container sizes
Pingback: Continue
Pingback: More hints
Pingback: waste disposal containers
Pingback: article source
Pingback: beauty
Pingback: Continued
Pingback: link
Pingback: local dumpster
Pingback: next page
Pingback: helpful hints
Pingback: namaste gesture
Pingback: helpful hints
Pingback: Our site
Pingback: buy unlocked phones online
Pingback: dumpster containers for rent
Pingback: trash removal companies
Pingback: Buy cell phones online
Pingback: cell phones deals
Pingback: buy unlocked phone
Pingback: buy unlocked phones online
Pingback: cell phones deals
Pingback: cell phones deals
Pingback: Buy cell phones online
Pingback: cell phones deals
Pingback: buy unlocked phone
Pingback: cell phones deals
Pingback: cell phones deals
Pingback: Buy cell phones online
Pingback: buy unlocked phones online
Pingback: buy unlocked phones online
Pingback: buy unlocked phone
Pingback: dumpster rental Albany
Pingback: 10 yard dumpster
Pingback: dumpster rental canton
Pingback: dumpster rental Woodstock
Pingback: residential dumpster rental
Pingback: dumoster rental Hiram
Pingback: dumpster rental prices
Pingback: construction dumpster
Pingback: dumpster rental Woodstock
Pingback: dumpster rental Brunswick
Pingback: dumpster rental Hinesville
Pingback: debris box
Pingback: disposal bin rental
Pingback: dumpster bin
Pingback: 15 yard dumpster
Pingback: rent a trash bin
Pingback: dumpster delivery
Pingback: 8 yard dumpster
Pingback: yard dumpster
Pingback: pick up junk
Pingback: commercial dumpster service
Pingback: 30 yard dumpster rental prices
Pingback: container rental
Pingback: on site dumpster rental
Pingback: astaxanthin
Pingback: service company
Pingback: towing company in taylor mi
Pingback: Eureka Telegraph Towing near US-24
Pingback: Eureka Telegraph Towing near WCCCD Downriver
Pingback: pennsylvania rd towing
Pingback: best towing company in midway sports taylor
Pingback: Eureka Telegraph Towing
Pingback: cryptocurrency exchange
Pingback: crytocurrency coin swap
Pingback: Siacoin price in india
Pingback: ZCash ZEC
Pingback: Ripple to INR
Pingback: crytocurrency coin swap
Pingback: PIVX price in inr
Pingback: Ark
Pingback: Enigma ENG
Pingback: Dogecoin price in india
Pingback: cryptocurrency exchange
Pingback: tow truck in i-75
Pingback: Augur
Pingback: cryptocurrency exchange
Pingback: Eureka Telegraph Towing near Lincoln Park
Pingback: crytocurrency coin swap
Pingback: cryptocurrency exchange
Pingback: crytocurrency coin swap
Pingback: BitShares
Pingback: the most reliable tow truck company near northline rd
Pingback: cryptocurrency exchange
Pingback: crytocurrency coin swap
Pingback: crytocurrency coin swap
Pingback: crytocurrency coin swap
Pingback: Stratis STRAT
Pingback: Zilliqa price in india
Pingback: Eureka Telegraph Towing near I-94
Pingback: cryptocurrency exchange
Pingback: tow truck company near mortenview dr
Pingback: crytocurrency coin swap
Pingback: crytocurrency coin swap
Pingback: crytocurrency coin swap
Pingback: Eureka Telegraph Towing near I-94
Pingback: crytocurrency coin swap
Pingback: Eureka Telegraph Towing near Pelham Rd
Pingback: Bitcoin cash india
Pingback: Golem price in inr
Pingback: cryptocurrency exchange
Pingback: tow truck service provider near heritage park
Pingback: Litecoin rates
Pingback: DigixDAO price in inr
Pingback: Zilliqa ZIL
Pingback: Monero
Pingback: gta 5 how to make money online xbox one
Pingback: TRON
Pingback: Augur price in inr
Pingback: Ethereum
Pingback: Dentacoin price in inr
Pingback: tow truck company in wcccd
Pingback: Eureka Telegraph Towing serving Allen Park
Pingback: emergency roadside service in southgate
Pingback: Electroneum price in inr
Pingback: Ark
Pingback: Polymath price in inr
Pingback: NXT
Pingback: Ethereum price in india
Pingback: Litecoin
Pingback: NEO price in india
Pingback: Verge XVG
Pingback: Ontology ONT
Pingback: Factom price in inr
Pingback: Monero
Pingback: Augur REP
Pingback: Indian bitcoin exchanges price
Pingback: Qtum price in inr
Pingback: Basic Attention Token price in inr
Pingback: Ethereum price in inr
Pingback: Ontology ONT
Pingback: Stratis price in inr
Pingback: DigixDAO price in india
Pingback: chat incontri gratis
Pingback: Sandy Hook Shooting
Pingback: best book for net exam paper 1
Pingback: dbt bet exam 2012
Pingback: bangalore internships
Pingback: indian horticulture research institute
Pingback: grade 12 courses
Pingback: private school summer school
Pingback: tifr exam syllabus
Pingback: icar jrf agronomy question paper
Pingback: calicut university msc entrance exam 2017
Pingback: summer school in august
Pingback: Freestanding Baths
Pingback: all india medical entrance 2017
Pingback: iit biology courses
Pingback: scope of microbiology after msc
Pingback: sai life sciences
Pingback: asrb net 2017 exam date
Pingback: thapar institute of engineering & technology
Pingback: summer in kolkata
Pingback: schinken
Pingback: Loom Network price in inr
Pingback: NXT price in inr
Pingback: schinken
Pingback: Phoenix Recording
Pingback: Qtum
Pingback: schinken
Pingback: Loom Network
Pingback: VeChain VEN
Pingback: Dash price in india
Pingback: schinken
Pingback: Substratum price in india
Pingback: Kyber network
Pingback: Ethereum price in india
Pingback: ICON price in inr
Pingback: Substratum
Pingback: Electroneum
Pingback: 15 minute manifestation reviews
Pingback: funda españa
Pingback: Fisioterapia Motora
Pingback: Fisioterapia Domiciliar
Pingback: Fisioterapia Respiratoria
Pingback: Cuidadores de Idosos
Pingback: AVC Hemorragico
Pingback: AVC Isquemico
Pingback: Fisioterapia Domiciliar
Pingback: Fisioterapia Respiratoria
Pingback: Fisioterapia Neurológica
Pingback: Derrame cerebral
Pingback: AVC Isquemico
Pingback: Fisioterapia Respiratoria
Pingback: Doenca de Alzheimer
Pingback: Derrame cerebral
Pingback: Fisioterapia Respiratoria
Pingback: Cuidadores de Idosos
Pingback: Mal de Parkinson
Pingback: Home Care
Pingback: Cuidadores de Idosos para atendimento em tempo integral
Pingback: Cuidadores de Idosos para administracao de alimentacao
Pingback: Cuidadores de Idosos para atendimento em tempo integral
Pingback: Cuidadores de Idosos para administracao de medicacao
Pingback: Cuidadores de Idosos para atendimento em tempo integral
Pingback: Cuidadores de Idosos para Mudanca de Decubito
Pingback: Derrame cerebral
Pingback: AVC Isquemico
Pingback: Derrame cerebral
Pingback: AVC Isquemico
Pingback: Cuidadores de Idosos para remocoes e deslocamentos
Pingback: Cuidadores de Idosos para atendimento em tempo integral
Pingback: Fisioterapia Geriatrica
Pingback: Fisioterapia Ortopedica
Pingback: Cuidadores de Idosos para curativos e feridas
Pingback: Fisioterapia Ortopedica
Pingback: Fisioterapia Uroginecologica
Pingback: Cuidadores de Idosos para banhos diversos
Pingback: Cuidadores de Idosos
Pingback: Cuidadores de Idosos para atendimento em tempo parcial
Pingback: Fisioterapia Motora
Pingback: Fisioterapia Geriatrica
Pingback: Cuidadores de Idosos para manuseio de sondas
Pingback: Derrame cerebral
Pingback: Cuidadores de Idosos para atendimento em tempo integral
Pingback: Fisioterapia Uroginecologica
Pingback: Doenca de Alzheimer
Pingback: Fisioterapia Domiciliar
Pingback: Cuidadores de Idosos
Pingback: Fisioterapia Domiciliar
Pingback: Cuidadores de Idosos para manuseio de sondas
Pingback: Cuidadores de Idosos para remocoes e deslocamentos
Pingback: Fisioterapia Domiciliar
Pingback: Fisioterapia Motora
Pingback: Fisioterapia Respiratoria
Pingback: Cuidadores de Idosos para atendimento em tempo parcial
Pingback: Fisioterapia Geriatrica
Pingback: AVC Hemorragico
Pingback: 4m5ntwcmo5tnexc54t
Pingback: kaskus bola
Pingback: Damp Proofing Portsmouth
Pingback: Wood rot Southampton
Pingback: Your Domain Name
Pingback: Going Here
Pingback: link
Pingback: Urbane (Home Page)
Pingback: Urbanical Poet
Pingback: mp3 download google search
Pingback: Reduce the incidence of asthma in 6 very easy ways
Pingback: Know why the popularity of the Indian Bengali serial in the country
Pingback: To get rid of the problem of dental problems, do the job in the morning
Pingback: Stay healthy, beauty advice
Pingback: Diabetes patient snacks and diet rules
Pingback: Tomato reduces male infertility
Pingback: At the age of 26, women's sexual excitement reached the peak.
Pingback: Find out the witch way to crack the skin.
Pingback: The logical response to women
Pingback: See what's in Barbecue Foods of different countries. (Video)
Pingback: These severe problems arise when hemoglobin in the blood decreases
Pingback: Teenager is encouraged by sex, from the addiction to porn movies!
Pingback: The way people know the nose at the nose
Pingback: Watch a funny video about "Coca-Banana" (Video)
Pingback: Know 'no' to say something very good to learn
Pingback: The world's most secret recipe
Pingback: Doing to whiten the teeth perfectly
Pingback: Drink these 4 drinks everyday to reduce fat fatty acids
Pingback: The island has been named Snake Island.
Pingback: Bill Gates plays toilet water!
Pingback: Find out the solution of stomach legs
Pingback: A different recipe of garlic and some unknown benefits
Pingback: The second Titanic floats in 2016
Pingback: A woman dead in front of television.
Pingback: Rosicruous for diabetic patients
Pingback: Life abroad
Pingback: gambling strategy new jersey
Pingback: Tefl course
Pingback: online gambling new jersey
Pingback: online sports betting new jersey
Pingback: Teach English in China
Pingback: China Jobs
Pingback: teaching english in china reddit
Pingback: TESOL
Pingback: Certified
Pingback: Jobs Teachin English
Pingback: teaching english in china reviews
Pingback: Chinese Visa
Pingback: TESOL
Pingback: Tefl course
Pingback: gambling strategy new jersey
Pingback: top online casino games new jersey
Pingback: China Link Facebook
Pingback: online casino games new jersey
Pingback: online slot games new jersey
Pingback: Brian Acton China Link ESL
Pingback: China Link Website
Pingback: Read More
Pingback: Certified
Pingback: teaching english in china jobs
Pingback: English Teacher
Pingback: China Link ESL
Pingback: English Teacher
Pingback: British Teacher
Pingback: galaxy s9
Pingback: Baum garten
Pingback: Cherokee Logistics GA
Pingback: Agence marketing Digitale
Pingback: kratom capsules philippines
Pingback: Fertilizations
Pingback: vulnerabilty
Pingback: Home Page
Pingback: Going Here
Pingback: Find Out More
Pingback: Click Here
Pingback: Go Here
Pingback: Going Here
Pingback: Discover More
Pingback: house
Pingback: Click This Link
Pingback: Go Here
Pingback: Homepage
Pingback: Home Page
Pingback: Going Here
Pingback: Clicking Here
Pingback: Go Here
Pingback: gift shop bd
Pingback: roof
Pingback: fire door inspection cost
Pingback: car window repair
Pingback: car window fix
Pingback: glass repair near me
Pingback: glass repair houston tx
Pingback: katy glass companies
Pingback: Wedding Music Philadelphia
Pingback: katy auto glass
Pingback: windshield repair
Pingback: priceless auto glass
Pingback: safetech houston
Pingback: houston window repair
Pingback: car side window
Pingback: window repair houston
Pingback: team ryan automotive
Pingback: glass restoration
Pingback: local auto glass repair shop near me
Pingback: cracked windshield
Pingback: car glass repair
Pingback: car glass shop
Pingback: chat over 40
Pingback: car side window repair
Pingback: glass repair auto
Pingback: replace rear window
Pingback: broken car window
Pingback: local auto glass
Pingback: glass repairs for cars
Pingback: glass store houston
Pingback: autoglass near me
Pingback: glass repair car
Pingback: affordable windshield repair
Pingback: glass auto body
Pingback: Best windshield material for repair and replacement of auto glass
Pingback: car window repairs
Pingback: D?ch v? seo web Äà n?ng
Pingback: windshield repair katy
Pingback: glass repair houston
Pingback: affordable windshield
Pingback: vehicle window repair
Pingback: auto glass houston texas
Pingback: mobile auto glass inc
Pingback: katy windshield repair
Pingback: auto glass center
Pingback: glass company near me
Pingback: auto car window replacement
Pingback: glass repair shops
Pingback: auto glass company
Pingback: auto glass near me
Pingback: drive car riccione
Pingback: glass and auto repair
Pingback: auto glass spring tx
Pingback: side glass car
Pingback: Affordable Auto Glass Houston
Pingback: New Homes lehigh valley pa
Pingback: auto car window repair
Pingback: auto glass repair service conroe, tx
Pingback: glass automotive
Pingback: car glass houston
Pingback: auto glass repair shop
Pingback: auto body shop midtown houston
Pingback: glass auto repair
Pingback: ryans automotive
Pingback: mey54cyyetvnbev54et
Pingback: auto glass chip repair
Pingback: windshield material
Pingback: car window replacement
Pingback: auto glass replacement
Pingback: who fix car windows
Pingback: automotive glass
Pingback: mobile home windows
Pingback: side car window
Pingback: window repair shop
Pingback: Auto Glass Repair and Collision Center in Houston
Pingback: BIGG BOSS TELUGU VOTE
Pingback: car glass repairs
Pingback: autoglass houston
Pingback: houston tx auto glass
Pingback: auto glass shop
Pingback: polishing auto glass
Pingback: windshields in houston
Pingback: windshield houston
Pingback: auto glass cypress tx
Pingback: vehicle glass repair
Pingback: affordable windshield replacement
Pingback: windshields houston
Pingback: car glass repair shops
Pingback: american auto glass houston
Pingback: Mobile Auto Glass Repair
Pingback: automotive shop
Pingback: ryan auto service
Pingback: star maa bigg boss vote
Pingback: auto glass houston, tx
Pingback: auto glass repair
Pingback: Best Divorce Advocate
Pingback: rapid auto glass
Pingback: side window glass
Pingback: Divorce Lawyer in Mumbai
Pingback: Thi?t k? web Äà n?ng
Pingback: d?ch v? seo web t?i Äà n?ng
Pingback: Top Divorce Attorney
Pingback: streaming bokep indo
Pingback: jilbab bugil
Pingback: bokep indo
Pingback: download bokep malaysia
Pingback: film bokep streaming
Pingback: donate car tax write off
Pingback: garage storage
Pingback: nonton bokep
Pingback: vibokep streaming
Pingback: video bokep indo dan malay mp4 3gp
Pingback: bokep crot
Pingback: vehicle donation program
Pingback: bokep nyepong
Pingback: car donation tax write off
Pingback: car tax write off
Pingback: donate my old car
Pingback: best charity for car donation
Pingback: how to donate old car
Pingback: donate car tax
Pingback: smash the con
Pingback: san diego
Pingback: video ngentot
Pingback: bokep indo
Pingback: Satriani Style
Pingback: download bokep malaysia
Pingback: streaming bokep indo
Pingback: video sex indo mp4
Pingback: donation pick up
Pingback: bokep semprot
Pingback: best place to donate your car
Pingback: donating a car without a title
Pingback: how to donate vehicle
Pingback: where can i donate my old car
Pingback: Guitar Backing Track
Pingback: film bokep streaming
Pingback: bokepindo
Pingback: nonton bokep
Pingback: abg ngentot
Pingback: donate your car kidney foundation
Pingback: car donation california
Pingback: nonton bokep indonesia
Pingback: Read More
Pingback: text donations
Pingback: car give away charity
Pingback: donation of car to charity tax deductible
Pingback: video crot
Pingback: download ikibokep
Pingback: nonton bokep indonesia
Pingback: streamingbokepindo
Pingback: Streaming Bokep Indo
Pingback: fair market value of car for tax purposes
Pingback: car donation for tax deduction
Pingback: kqed donate car
Pingback: Huron Towing serving Detroit
Pingback: junkyard cars for sale
Pingback: bokep hijab
Pingback: streaming bokep indo
Pingback: bokep crot
Pingback: video crot
Pingback: video sex malay mp4
Pingback: tow truck dearborn
Pingback: warrendale detroit towing service
Pingback: san diego
Pingback: Streaming Bokep Indo
Pingback: End of Tenancy Cleaners
Pingback: Huron Towing serving Detroit
Pingback: tow truck company near detroit mi
Pingback: Huron Towing
Pingback: iheart gaming
Pingback: Huron Towing near Detroit MI
Pingback: Huron Towing
Pingback: compare roadside assistance
Pingback: towing service near warrendale detroit
Pingback: shop for trucks
Pingback: lift and tow
Pingback: towing service provider in southfield
Pingback: End of Tenancy Cleaning Prices
Pingback: asurion roadside assistance
Pingback: Detroit Metro Towing
Pingback: iheart gaming
Pingback: auto wrecker service in midtown
Pingback: learn about towing here
Pingback: pasco auto wrecking
Pingback: comprehensive car insurance coverage
Pingback: towing service in harper woods
Pingback: emergency roadside assistance in farmington hills
Pingback: tow truck beds
Pingback: emergency towing hazel park
Pingback: buying auto insurance
Pingback: where to go for urban exploration in berlin
Pingback: iheart gaming
Pingback: best towing company in detroit mi
Pingback: price of a tow truck
Pingback: emergency roadside service in downtown detroit
Pingback: tow truck near me now
Pingback: a towing company
Pingback: where did david bowie live in berlin
Pingback: super smash bros
Pingback: car trailer truck
Pingback: Tanjev Grimm
Pingback: Tanjev Grimm Wilhelmshaven
Pingback: Sebastian Baar Wilhelmshaven
Pingback: where to buy sex toys
Pingback: Gadgets
Pingback: gear
Pingback: geek
Pingback: Technology
Pingback: Accessories
Pingback: homegoods
Pingback: watches
Pingback: tool
Pingback: bags
Pingback: Cameras
Pingback: Electronics
Pingback: Accessories
Pingback: geek
Pingback: Gadgets
Pingback: Technology
Pingback: Gadgets
Pingback: Gadgets
Pingback: Accessories
Pingback: watches
Pingback: homegoods
Pingback: faster hair growth
Pingback: Gadgets
Pingback: homegoods
Pingback: gear
Pingback: Electronics
Pingback: geek
Pingback: gifts
Pingback: tool
Pingback: geek
Pingback: faster hair growth
Pingback: watches
Pingback: geek
Pingback: Tech
Pingback: Tech
Pingback: Forros de PVC instalacao
Pingback: Accessories
Pingback: homegoods
Pingback: gear
Pingback: bags
Pingback: Kitchen
Pingback: Tech
Pingback: san diego
Pingback: tool
Pingback: Gadgets
Pingback: Gadgets
Pingback: geek
Pingback: tool
Pingback: Kitchen
Pingback: gear
Pingback: tool
Pingback: Tech
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: homegoods
Pingback: Technology
Pingback: geek
Pingback: gifts
Pingback: Kitchen
Pingback: tool
Pingback: Technology
Pingback: gifts
Pingback: Kitchen
Pingback: homegoods
Pingback: Tech
Pingback: geek
Pingback: faster hair growth
Pingback: tool
Pingback: Accessories
Pingback: Cameras
Pingback: homegoods
Pingback: watches
Pingback: faster hair growth
Pingback: Technology
Pingback: gifts
Pingback: Technology
Pingback: Cameras
Pingback: gear
Pingback: best supplement for hair growth
Pingback: tool
Pingback: best supplement for hair growth
Pingback: Technology
Pingback: homegoods
Pingback: Tech
Pingback: geek
Pingback: tool
Pingback: construir un sitio web
Pingback: best supplement for hair growth
Pingback: best supplement for hair growth
Pingback: best supplement for hair growth
Pingback: apartments for rent in hanoi
Pingback: best supplement for hair growth
Pingback: best supplement for hair growth
Pingback: best supplement for hair growth
Pingback: best supplement for hair growth
Pingback: apartment for rent in hoan kiem
Pingback: best thing for joint pain
Pingback: finance courses in dubai
Pingback: Get More Info
Pingback: living room decor ideas
Pingback: living room decor ideas
Pingback: living room decor ideas
Pingback: Discover More
Pingback: This Site
Pingback: wall decor
Pingback: vinyl stickers
Pingback: decals
Pingback: wall art
Pingback: flower wall decals
Pingback: home furnishings
Pingback: wall stencils
Pingback: Visit This Link
Pingback: living room decor ideas
Pingback: phone holder
Pingback: home decor
Pingback: pop mount
Pingback: living room decor ideas
Pingback: disney wall decals
Pingback: disney wall decals
Pingback: vinyl stickers
Pingback: superhero wall decals
Pingback: vinyl stickers
Pingback: home decor
Pingback: wall decor
Pingback: living room decor ideas
Pingback: phone mount for car
Pingback: Look At This
Pingback: Check This Out
Pingback: car phone holder
Pingback: home decor
Pingback: flower wall decals
Pingback: home decor
Pingback: disney wall decals
Pingback: Find Out More
Pingback: home decor
Pingback: phone holder
Pingback: phone holder
Pingback: phone mount for car
Pingback: cell phone holder
Pingback: car phone holder
Pingback: car phone holder
Pingback: phone mount for car
Pingback: superhero wall decals
Pingback: phone mount for car
Pingback: Visit Website
Pingback: disney wall decals
Pingback: cell phone holder
Pingback: home decor
Pingback: wall decor ideas
Pingback: phone mount for car
Pingback: phone holder
Pingback: pop mount
Pingback: wall decor ideas
Pingback: More Info
Pingback: home decor
Pingback: home decor
Pingback: pop mount
Pingback: Discover More Here
Pingback: cell phone holder
Pingback: phone holder
Pingback: wall decor
Pingback: wall decor
Pingback: wall stickers
Pingback: shopify-section-header
Pingback: wall decor
Pingback: pop mount
Pingback: wall stickers
Pingback: wall decor
Pingback: home decor
Pingback: Clicking Here
Pingback: AddToCartText
Pingback: Visit Website
Pingback: This Site
Pingback: Home Page
Pingback: Learn More
Pingback: flexslider--slider
Pingback: Click This Link
Pingback: Find Out More
Pingback: Discover More
Pingback: webchat freee
Pingback: Go Here
Pingback: Home Page
Pingback: best hair growth products
Pingback: hair growth supplements
Pingback: hair growth
Pingback: hair regrowth
Pingback: wall art
Pingback: wall stencils
Pingback: hair skin and nails vitamins
Pingback: flower wall decals
Pingback: disney wall decals
Pingback: vinyl stickers
Pingback: star wars decals
Pingback: flower wall decals
Pingback: living room decor ideas
Pingback: thinning hair
Pingback: home decor
Pingback: home decor
Pingback: star wars decals
Pingback: home decor
Pingback: wall stencils
Pingback: superhero wall decals
Pingback: wall decor
Pingback: haircut for women
Pingback: hair growth products
Pingback: hair growth
Pingback: hair growth vitamins
Pingback: hair growth supplements
Pingback: hair growth vitamins
Pingback: haircut for women
Pingback: haircut for women
Pingback: thinning hair
Pingback: thinning hair women
Pingback: vitamins for skin
Pingback: thinning hair
Pingback: hair growth supplements
Pingback: haircut for women
Pingback: hair vitamins
Pingback: best hair vitamins
Pingback: hair growth products
Pingback: hair and nail vitamins
Pingback: hair products for thin hair
Pingback: haircut for women
Pingback: biotin for hair growth
Pingback: hair growth products
Pingback: best hair vitamins
Pingback: natural hair growth
Pingback: hair growth
Pingback: hair loss treatment
Pingback: vitamins for hair loss
Pingback: hair vitamins
Pingback: biotin for hair growth
Pingback: best shampoo for thinning hair
Pingback: hair regrowth
Pingback: biotin for hair growth
Pingback: CABLES
Pingback: thinning hair
Pingback: best vitamins for hair growth
Pingback: hair growth
Pingback: best hair growth products
Pingback: hair loss
Pingback: bald women
Pingback: hair and nail vitamins
Pingback: hair growth supplements
Pingback: natural hair growth
Pingback: haircut for women
Pingback: hair growth products
Pingback: best shampoo for thinning hair
Pingback: hair growth products
Pingback: best vitamins for hair growth
Pingback: best medical mariujuana doctor michigan
Pingback: mens wear
Pingback: natural hair growth
Pingback: thinning hair
Pingback: natural hair growth
Pingback: haircut for women
Pingback: hair re-growth
Pingback: thinning hair women
Pingback: hair growth
Pingback: hair growth pill
Pingback: bald women
Pingback: thinning hair
Pingback: faster hair growth
Pingback: thinning hair women
Pingback: hair and nail vitamins
Pingback: hair growth pill
Pingback: hair growth supplements
Pingback: hair growth
Pingback: best hair growth products
Pingback: Soapland Tokyo
Pingback: hair growth pill
Pingback: natural hair growth
Pingback: hair re-growth
Pingback: hair products for thin hair
Pingback: hair products for thin hair
Pingback: hair and nail vitamins
Pingback: hair growth pill
Pingback: faster hair growth
Pingback: hair re-growth
Pingback: hair growth
Pingback: best shampoo for thinning hair
Pingback: vitamins for skin
Pingback: vitamins for skin
Pingback: faster hair growth
Pingback: High class escorts Sydney
Pingback: Maegan Mcevoy
Pingback: fastest hair growth
Pingback: fastest hair growth
Pingback: Maxie Wingham
Pingback: biotin hair
Pingback: Gregoria Rosner
Pingback: fastest hair growth
Pingback: hair growing fast
Pingback: Chrissy Bowlby
Pingback: hair growing fast
Pingback: biotin hair
Pingback: biotin hair
Pingback: men tie
Pingback: grow hair vitamin
Pingback: fastest hair growth
Pingback: grow hair vitamin
Pingback: fastest hair growth
Pingback: biotin hair
Pingback: hair nails and skin vitamin
Pingback: vitamin for hair
Pingback: hair growth vitamins
Pingback: vitamin for hair growth
Pingback: vitamin for hair
Pingback: hair nails and skin vitamin
Pingback: hair growth vitamins
Pingback: menù originali
Pingback: namo tv
Pingback: grow hair pills
Pingback: Tokyo people
Pingback: vitamin for hair
Pingback: vitamin for hair
Pingback: Escorts in Tokyo
Pingback: vitamin for hair growth
Pingback: vitamin for hair
Pingback: menù dei ristoranti
Pingback: sfoglia menù
Pingback: sfoglia menù
Pingback: vitamin for hair
Pingback: sfoglia menù
Pingback: menù dei ristoranti
Pingback: menù dei ristoranti
Pingback: vitamin a for hair growth
Pingback: menù originali
Pingback: hair vitamins
Pingback: menù dei ristoranti
Pingback: menù originali
Pingback: menù dei ristoranti
Pingback: sluurpy
Pingback: hair growing vitamin
Pingback: hair vitamin
Pingback: Ticks
Pingback: Zika Virus
Pingback: hair growing vitamin
Pingback: vitamin a for hair growth
Pingback: Lyme Disease
Pingback: hair skin and nails vitamin
Pingback: hair growing vitamin
Pingback: hair vitamin
Pingback: hair vitamin
Pingback: hair vitamins
Pingback: hair growing vitamin
Pingback: hair vitamin
Pingback: hair growing vitamin
Pingback: Phâ~u Thuâ?t Ha`m Hô
Pingback: hair growing vitamin
Pingback: South African Music
Pingback: Home Page
Pingback: African hair braiding styles
Pingback: African Wall Art
Pingback: African Jewelry
Pingback: South African Music
Pingback: 3xm84n5ctgwxtci5gwv4tct
Pingback: African Print Dresses
Pingback: hair growing vitamin
Pingback: hair growing vitamin
Pingback: hair growing vitamin
Pingback: Get More Info
Pingback: Lyme Disease
Pingback: hair growing vitamin
Pingback: hair growing vitamin
Pingback: Ticks
Pingback: Ticks
Pingback: African Dresses
Pingback: African Fashion
Pingback: African Art
Pingback: Traditional African music
Pingback: hair growing vitamin
Pingback: How to Get Rid of Acid Reflux in Throat
Pingback: hair growth
Pingback: hair growing vitamin
Pingback: fastest hair growth
Pingback: African skirts
Pingback: fastest hair growth
Pingback: fastest hair growth
Pingback: hair vitamins
Pingback: fastest hair growth
Pingback: Coconut oil for african american hair
Pingback: African Shirt
Pingback: African Wedding Dresses
Pingback: African Culture
Pingback: African Clothing
Pingback: hair vitamins
Pingback: fastest hair growth
Pingback: hair vitamins
Pingback: Bug Repellent
Pingback: hair vitamins
Pingback: fastest hair growth
Pingback: Ticks
Pingback: hair vitamins
Pingback: More Info
Pingback: Ticks
Pingback: super vpn
Pingback: turbo vpn
Pingback: vpn
Pingback: vpn private
Pingback: vpn
Pingback: vpn private
Pingback: hair re-growth
Pingback: hair re-growth
Pingback: hair re-growth
Pingback: vpn
Pingback: hair re-growth
Pingback: hair re-growth
Pingback: hair re-growth
Pingback: hair re-growth
Pingback: biotin hair
Pingback: biotin hair
Pingback: vpn
Pingback: free vpn
Pingback: vpn master
Pingback: vpn
Pingback: biotin hair
Pingback: Zika Virus
Pingback: vpn private
Pingback: vpn master
Pingback: vpn
Pingback: Mosquitoes
Pingback: Ticks
Pingback: biotin hair
Pingback: hair growing fast
Pingback: biotin hair
Pingback: biotin hair
Pingback: biotin hair
Pingback: Visit This Link
Pingback: biotin hair
Pingback: vpn hotspot
Pingback: vpn
Pingback: vpn private
Pingback: vpn
Pingback: Clicking Here
Pingback: free vpn
Pingback: Web Site
Pingback: free vpn
Pingback: free vpn
Pingback: Ticks
Pingback: Zika Virus
Pingback: Home Page
Pingback: Lyme Disease
Pingback: bitcoin office
Pingback: bitcoin 100
Pingback: vpn
Pingback: vpn hotspot
Pingback: vpn
Pingback: vpn
Pingback: bitcoin 6 months ago
Pingback: Bug Repellent
Pingback: Mosquitoes
Pingback: maquinas technogym
Pingback: small coffee machine
Pingback: coffee machine price
Pingback: manual grinder
Pingback: coffee review
Pingback: monin
Pingback: iced coffee
Pingback: coffee beans
Pingback: business coffee machine
Pingback: coffee machine maintenance
Pingback: Rugby News
Pingback: Pallini syrups
Pingback: latte
Pingback: Ticks
Pingback: Best Chocolate Powder
Pingback: Mosquitoes
Pingback: coffee machine dubai
Pingback: Vending Milk Powder
Pingback: coffee pods
Pingback: commercial coffee machines
Pingback: coffee shop supplies
Pingback: Vanilla tea
Pingback: profesional coffee machines
Pingback: Spice Tea Latte
Pingback: coffee beans suppliers
Pingback: office coffee machine
Pingback: coffee machine maintenance
Pingback: office coffee machine
Pingback: coffee grinder
Pingback: cappuccino
Pingback: drip coffee
Pingback: Muebles pinto
Pingback: coffee maker
Pingback: diseño web de pagina web
Pingback: Rugby News
Pingback: Italian coffee machines
Pingback: coffee machine uae
Pingback: cafe supplies
Pingback: business coffee machine
Pingback: dog arthritis natural remedy
Pingback: grinder on demand
Pingback: Cookies and Creme Frappe
Pingback: Gourmet Chocolate Powder
Pingback: coffee shop supplier
Pingback: coffee grinder
Pingback: Arkadia
Pingback: good coffee machine
Pingback: Italian Coffee Dubai
Pingback: coffee beans price
Pingback: coffee shop supplier
Pingback: Chocolate Frappe
Pingback: office coffee machine
Pingback: coffee syrups
Pingback: vitamin b for dogs
Pingback: glucosamine for dogs
Pingback: homemade dog food for arthritis
Pingback: Pallini syrups
Pingback: filter coffee machine
Pingback: dog arthritis supplements
Pingback: What kind of pain reliever can you give your dog?
Pingback: manual grinder
Pingback: Turmeric Latte
Pingback: espresso coffee machine
Pingback: Matcha Latte
Pingback: joint medicine for dogs
Pingback: dog arthritis medication
Pingback: lipton
Pingback: probiotic supplements
Pingback: coffee beans price
Pingback: barista training
Pingback: Best Chocolate Powder
Pingback: Caramel Frappe
Pingback: Green Gunpowder
Pingback: Vending Chocolate Powder
Pingback: manual grinder
Pingback: hajj tours
Pingback: Italian Coffee
Pingback: which coffee machine
Pingback: organic coffee
Pingback: gps tracking tags
Pingback: grinder
Pingback: www.schoolbanners.co.nz/faqs
Pingback: puppia dog harness
Pingback: cafe equipment
Pingback: Italian Coffee Dubai
Pingback: coffee shop equipment
Pingback: coffee machine service
Pingback: organic coffee
Pingback: jura coffee machines
Pingback: Spice Tea Latte
Pingback: organic coffee
Pingback: coffee pods
Pingback: Turmeric Frappe
Pingback: Vending Milk Powder
Pingback: Fully automatic machines
Pingback: espresso machine reviews
Pingback: www.schoolbanners.co.nz/tablecloths
Pingback: Rugby Live Scores
Pingback: emergency car locksmith service
Pingback: filter coffee machine
Pingback: coffee machine uae
Pingback: ice tea
Pingback: managed wordpress hosting
Pingback: siam square
Pingback: Learn More Here
Pingback: Get More Info
Pingback: Discover More Here
Pingback: Get More Info
Pingback: Clicking Here
Pingback: soppong
Pingback: Click This Link
Pingback: Website
Pingback: Web Site
Pingback: Look At This
Pingback: Visit This Link
Pingback: More Info
Pingback: astaxanthin
Pingback: Homepage
Pingback: Look At This
Pingback: astaxanthin
Pingback: Web Site
Pingback: Look At This
Pingback: Get More Info
Pingback: Go Here
Pingback: Click Here
Pingback: disposable rain poncho with hood
Pingback: disposable poncho
Pingback: rain poncho family pack
Pingback: toddler poncho
Pingback: rain poncho
Pingback: kids rain poncho
Pingback: rain poncho
Pingback: rain poncho
Pingback: ponchos for kids
Pingback: Hormone replacement compounding pharmacy arizona
Pingback: disney poncho
Pingback: disposable ponchos
Pingback: Veterinary compounding pharmacy
Pingback: kids rain poncho
Pingback: ponchos for kids
Pingback: rain pancho
Pingback: Veterinary compounding pharmacy Arizona
Pingback: id bracelet for kids
Pingback: magic band bitbelts
Pingback: rain pancho
Pingback: disposable rain poncho
Pingback: disney rain poncho
Pingback: emergency poncho
Pingback: panchos rain
Pingback: disposable ponchos
Pingback: disposable rain poncho with hood
Pingback: id bracelet for kids
Pingback: disposable ponchos
Pingback: rain ponchos for kids
Pingback: rain poncho kids
Pingback: rain pancho
Pingback: id bracelet for kids
Pingback: real estate Marbella
Pingback: rain pancho
Pingback: toddler poncho
Pingback: panchos rain
Pingback: rain poncho for kids
Pingback: magic band bitbelts
Pingback: toddler poncho
Pingback: disposable rain poncho
Pingback: rain pancho
Pingback: disposable poncho
Pingback: disposable rain poncho with hood
Pingback: rain poncho
Pingback: magic band bitbelts
Pingback: rain ponchos
Pingback: toddler rain poncho
Pingback: magic band bitbelts
Pingback: ponchos family pack
Pingback: disposable ponchos
Pingback: rain poncho kids
Pingback: Flower Studio Pakistan
Pingback: www.theflowerstudio.pk/
Pingback: where to buy flowers online
Pingback: where to buy flowers
Pingback: Flower Studio
Pingback: Flower Studio Pk
Pingback: The Flower Studio
Pingback: disney poncho
Pingback: id bracelet for kids
Pingback: toddler rain poncho
Pingback: where to buy flowers online
Pingback: Flower Studio Pakistan
Pingback: FlowerStudio
Pingback: Flower Studio Pakistan
Pingback: disposable ponchos
Pingback: disposable rain poncho
Pingback: The Flower Studio
Pingback: www.theflowerstudio.pk/
Pingback: the flower delivery company
Pingback: disney rain poncho
Pingback: kids poncho
Pingback: konami digital entertainment
Pingback: most entertaining apps
Pingback: the entertainer piano
Pingback: instagram ghost followers
Pingback: Flower Studio Pakistan
Pingback: www.theflowerstudio.pk/
Pingback: Check This
Pingback: TheFlowerStudioPakistan
Pingback: eagle rock entertainment
Pingback: www.theflowerstudio.pk/
Pingback: wedding photographer Canaseraga
Pingback: wedding photographer Colton
Pingback: same day flower delivery
Pingback: The Flower Studio
Pingback: TheFlowerStudioPakistan
Pingback: influencers
Pingback: TheFlowerStudioPakistan
Pingback: wedding photographer Andover
Pingback: wedding photographer Antwerp
Pingback: TheFlowerStudioPk
Pingback: the flower delivery company
Pingback: alternative to instagram bots
Pingback: productivity
Pingback: merlin entertainment
Pingback: expert advisor
Pingback: Flower Studio Pk
Pingback: same day flower delivery
Pingback: sony entertainment television
Pingback: entertainment news gossip
Pingback: las vegas entertainment
Pingback: 3cmt54wvtvwc5vtwc54tx
Pingback: fifa
Pingback: bbc entertainment news
Pingback: multiple instagram accounts
Pingback: entertainment phoenix
Pingback: ashley entertainment center
Pingback: korean entertainment
Pingback: wedding photographer Ogdensburg
Pingback: shamrock entertainment
Pingback: wedding photographer Islandia
Pingback: wedding photographer Melrose Park
Pingback: wedding photographer in Stillwater
Pingback: types of entertainment
Pingback: wedding photographer Round Lake
Pingback: tv entertainment center
Pingback: iq home entertainment
Pingback: post
Pingback: wedding photographer Elba
Pingback: side hustle
Pingback: clothing line
Pingback: wedding photographer in Lincoln Park
Pingback: rain ponchos
Pingback: who unfollowed me
Pingback: ponchos for kids
Pingback: emergency poncho
Pingback: rain ponchos for adults disposable
Pingback: kids rain poncho
Pingback: rain ponchos
Pingback: panchos rain
Pingback: kids rain poncho
Pingback: rain ponchos for adults disposable
Pingback: rain ponchos for kids
Pingback: wedding photographers in North Gates
Pingback: toddler poncho
Pingback: disposable rain poncho
Pingback: wedding photographers in Franklinville
Pingback: emergency poncho
Pingback: kids rain poncho
Pingback: wedding photographer in Brasher Falls
Pingback: rain poncho kids
Pingback: wedding photographer in East Quogue
Pingback: wedding photographer South Floral Park
Pingback: wedding photographer University at Buffalo
Pingback: rain poncho for kids
Pingback: panchos rain
Pingback: matador blanket pocket
Pingback: importance of customer loyalty
Pingback: toddler rain poncho
Pingback: id bracelet for kids
Pingback: social media experiment
Pingback: disposable poncho
Pingback: wedding photographer in Fillmore
Pingback: instagram followers
Pingback: rain ponchos
Pingback: rain poncho family pack
Pingback: rain ponchos for kids
Pingback: rain ponchos for kids
Pingback: customer service quality
Pingback: toddler poncho
Pingback: rain pancho
Pingback: kids poncho
Pingback: id bracelet for kids
Pingback: panchos rain
Pingback: toddler poncho
Pingback: disney poncho
Pingback: magic band bitbelts
Pingback: get what you want
Pingback: South Nyack wedding photographer
Pingback: influencer campaigns
Pingback: Hortonville wedding photographer
Pingback: rain poncho for kids
Pingback: disposable rain poncho with hood
Pingback: guerilla marketing ideas
Pingback: disposable ponchos
Pingback: reposting
Pingback: ponchos family pack
Pingback: disposable rain poncho with hood
Pingback: disney poncho
Pingback: matador blanket pocket
Pingback: business greatness
Pingback: xrp money
Pingback: what is social media
Pingback: matador blanket pocket
Pingback: rain ponchos for kids
Pingback: ponchos for kids
Pingback: ponchos family pack
Pingback: stand out online
Pingback: content marketing tips
Pingback: rain poncho family pack
Pingback: matador blanket pocket
Pingback: rain pancho
Pingback: rain poncho for kids
Pingback: Wood Floor Sanding Sheffield
Pingback: instagram new account
Pingback: Engineering Consultant United Kingdom
Pingback: disposable rain poncho
Pingback: panchos rain
Pingback: rain poncho kids
Pingback: Floor Restoration Sheffield
Pingback: first media campaign
Pingback: toddler poncho
Pingback: rain poncho kids
Pingback: disney rain poncho
Pingback: disposable poncho
Pingback: toddler poncho
Pingback: disposable ponchos
Pingback: rain ponchos for adults disposable
Pingback: disposable rain poncho
Pingback: rain poncho for kids
Pingback: matador blanket pocket
Pingback: panchos rain
Pingback: kids poncho
Pingback: stretch and fit insta lids cover
Pingback: stretch and fit lids
Pingback: silicon stretch food lids cover
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: instalids
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: silicone bowl covers
Pingback: silicone bowl lids cover
Pingback: Felix Pantaleon
Pingback: stretch and seal lids cover
Pingback: silicone lids
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: stretch seal lids cover
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: stretch and seal covers
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: instalids lids cover
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: stretch and fit insta covers
Pingback: Felix Pantaleon
Pingback: Felix Pantaleon
Pingback: womens
Pingback: designer
Pingback: free printable coupon websites
Pingback: Ristoranti Padova
Pingback: free promotional codes
Pingback: coupon cut out
Pingback: Ristoranti Firenze
Pingback: Ristoranti Brescia
Pingback: wooden
Pingback: round
Pingback: voucher deals
Pingback: silicon stretch covers
Pingback: Ristoranti Catania
Pingback: Ristoranti Cagliari
Pingback: click funnels italiano
Pingback: Get the facts
Pingback: funnel marketing formula
Pingback: social media marketing aziendale
Pingback: Ristoranti Trieste
Pingback: Ristoranti Messina
Pingback: Ristoranti Perugia
Pingback: Ristoranti Pisa
Pingback: facebook ads
Pingback: affilizioni di amazon
Pingback: Ristoranti Reggio Emilia
Pingback: clickfunnels
Pingback: pixel di facebook
Pingback: More Info
Pingback: funnel marketing
Pingback: Ristoranti Siracusa
Pingback: Visit This Link
Pingback: vendere online
Pingback: Learn More
Pingback: tecniche di copywriting
Pingback: funnel marketing
Pingback: marketing formula
Pingback: Read Full Article
Pingback: affilizioni di amazon
Pingback: Ristoranti Udine
Pingback: marketing formula
Pingback: Ristoranti Como
Pingback: social media marketing aziendale
Pingback: vendere online
Pingback: guadagnare online
Pingback: retargeting
Pingback: More hints
Pingback: clickfunnels
Pingback: andrea sansonna
Pingback: Ristoranti Arezzo
Pingback: corso di marketing
Pingback: Ristoranti Treviso
Pingback: funnel marketing formula
Pingback: Ristoranti Pavia
Pingback: Ristoranti Bolzano
Pingback: Ristoranti Monza
Pingback: Source
Pingback: Ristoranti Massa
Pingback: Ristoranti Pozzuoli
Pingback: Ristoranti Fiumicino
Pingback: andrea sansonna
Pingback: Ristoranti Caserta
Pingback: affilizioni di amazon
Pingback: Ristoranti Trapani
Pingback: Extra resources
Pingback: Our site
Pingback: Ristoranti Carbonia
Pingback: Ristoranti Cesenatico
Pingback: vendere online
Pingback: facebook ads
Pingback: Ristoranti Sanremo
Pingback: Ristoranti Riccione
Pingback: Ristoranti Sassari
Pingback: guadagnare online
Pingback: hypnosis for
Pingback: strategie di Funnel Marketing
Pingback: Ristoranti Piacenza
Pingback: corso di marketing
Pingback: funnel marketing formula
Pingback: funnel marketing strategia
Pingback: lake worth
Pingback: vendere online
Pingback: Ristoranti Cremona
Pingback: Ristoranti Savona
Pingback: out of body
Pingback: Ristoranti Alghero
Pingback: Ristoranti Sorrento
Pingback: Ristoranti Fano
Pingback: Ristoranti Cesena
Pingback: Ristoranti Grosseto
Pingback: Ristoranti Ancona
Pingback: Ristoranti Lido di Ostia
Pingback: Ristoranti Viterbo
Pingback: Ä?t bi?n Äà n?ng
Pingback: Ristoranti Aosta
Pingback: gift for men
Pingback: Ristoranti Taormina
Pingback: for wedding
Pingback: daddy and son
Pingback: groomsmen gift
Pingback: Ristoranti Novara
Pingback: wedding bow tie
Pingback: Ristoranti Ragusa
Pingback: groomsmen bow tie
Pingback: boys bow tie
Pingback: pocket square
Pingback: toddler bow tie
Pingback: Ristoranti Lecco
Pingback: Ristoranti Civitanova M.
Pingback: linen necktie
Pingback: Ristoranti Cuneo
Pingback: Ristoranti Gallipoli
Pingback: Ristoranti Varese
Pingback: Ristoranti Matera
Pingback: baixa autoestima
Pingback: teste depressão
Pingback: Going Here
Pingback: Ristoranti Anzio
Pingback: Ristoranti Cervia
Pingback: Ristoranti Cosenza
Pingback: Visit This Link
Pingback: Discover More Here
Pingback: Go Here
Pingback: Visit Website
Pingback: Click This Link
Pingback: Home Page
Pingback: Get More Information
Pingback: Click Here
Pingback: hiperatividade
Pingback: Visit Website
Pingback: Find Out More
Pingback: Web Site
Pingback: Discover More Here
Pingback: Read More
Pingback: Get More Information
Pingback: Website
Pingback: Get More Information
Pingback: Go Here
Pingback: Read More
Pingback: Read More Here
Pingback: Read This
Pingback: Click Here
Pingback: Clicking Here
Pingback: Learn More
Pingback: Ruby Sen Kolkata Independent Escorts
Pingback: Diana Diaz Goa Independent Escorts Services
Pingback: al azhar karawang
Pingback: Pontoon Boat Anchors Merritt Island, FL
Pingback: Pontoon Boat Anchors Bonita Springs, FL
Pingback: Diksha Arya Independent Escorts Services in Kolkata
Pingback: Pontoon Boat Anchors Tampa, FL
Pingback: al azhar memorial
Pingback: Swan
Pingback: al azhar karawang
Pingback: Sripatum University Thailand
Pingback: al azhar memorial
Pingback: designer perfume oil
Pingback: Devika Kakkar Goa Escorts Services
Pingback: quartz worktops manchester
Pingback: Rebecca Desuza Goa Independent Escorts Services
Pingback: Yamini Mittal Independent Escorts Services in Goa
Pingback: Simmi Mittal Kolkata Escorts Services
Pingback: Read This
Pingback: Click Here
Pingback: Read More Here
Pingback: Website
Pingback: Discover More
Pingback: 91stspecialforcesgroup
Pingback: milsim application
Pingback: 91st sfg clan
Pingback: Emotion
Pingback: escort agency coventry
Pingback: Relationship
Pingback: 91st
Pingback: husband
Pingback: coventry escort agency
Pingback: Laugh
Pingback: arma 2
Pingback: milsim
Pingback: milsim application
Pingback: 91stspecialforcesgroup
Pingback: New age
Pingback: Attack
Pingback: web design portfolio
Pingback: Boyfriend
Pingback: informatica
Pingback: woman
Pingback: Things
Pingback: informatica
Pingback: Wife
Pingback: Boyfriend
Pingback: People
Pingback: programas
Pingback: husband
Pingback: adobe-premiere-cc-2017
Pingback: softwares
Pingback: husband
Pingback: Dating
Pingback: Attack
Pingback: Love
Pingback: Dating
Pingback: Find Out More
Pingback: Find Out More
Pingback: Learn More Here
Pingback: Website
Pingback: Girlfriend
Pingback: Homepage
Pingback: Clicking Here
Pingback: Things
Pingback: Dating
Pingback: Wife
Pingback: woman
Pingback: woman
Pingback: produtos personalizados
Pingback: Dating
Pingback: Laugh
Pingback: Emotion
Pingback: Things
Pingback: husband
Pingback: produtos personalizados
Pingback: Kolkata Escorts Services Ragini Mehta
Pingback: Girlfriend
Pingback: adr games online
Pingback: games oniles
Pingback: jogos onlines
Pingback: Thought
Pingback: kogama
Pingback: biochemist average salary
Pingback: Navya Sharma Independent Kolkata Escorts Services
Pingback: apps download for windows 7
Pingback: pc apps for windows 7
Pingback: apps download for windows 7
Pingback: best education schools in texas
Pingback: free download for pc windows
Pingback: download games for windows 7
Pingback: easy chemistry lessons
Pingback: download games for windows 10
Pingback: pharmaceutical manufacturing companies in germany
Pingback: astaxanthin
Pingback: pharmaceutical companies in austria
Pingback: Woman issue
Pingback: biosimilars companies in india
Pingback: biotechnology companies belgium
Pingback: pop socket
Pingback: pop socket
Pingback: Dating
Pingback: phone mount
Pingback: phone holder for car
Pingback: cell phone holder
Pingback: car phone holder
Pingback: popsocket
Pingback: pop socket
Pingback: phone mount
Pingback: husband
Pingback: post jobs
Pingback: phone mount
Pingback: sbobetcasino
Pingback: pop socket
Pingback: phone holder for car
Pingback: pop mount
Pingback: phone holder for car
Pingback: pop mount
Pingback: popsocket
Pingback: phone holder for car
Pingback: Attack
Pingback: pop socket
Pingback: phone holder for car
Pingback: chronic pain management
Pingback: sore lower back
Pingback: sciatic nerve treatment
Pingback: cheap men jewelry online
Pingback: cheap men watches
Pingback: ankle pain
Pingback: sciatic nerve treatment
Pingback: men watches buy online
Pingback: chronic pain treatment
Pingback: quell pain relief
Pingback: luxury men watches
Pingback: Click Here
Pingback: next page
Pingback: men watches buy online
Pingback: luxury men watches
Pingback: Our site
Pingback: our website
Pingback: Image to PDF convert
Pingback: JPG to PDF converter
Pingback: Elisha Roy Goa Independent Escorts Services
Pingback: Read This
Pingback: Get More Info
Pingback: Home Page
Pingback: Visit This Link
Pingback: The 4 Hour Work Week
Pingback: Extreme Ownership
Pingback: Alisha Oberoi Kolkata Escorts Services
Pingback: biotechnology careers list and salaries
Pingback: job opportunities for biotechnology graduates
Pingback: biotechnology careers in india
Pingback: biotechnology careers list and salaries
Pingback: what jobs can you get with a biotechnology degree
Pingback: biotechnology careers list and salaries
Pingback: biotechnology degree salary
Pingback: Benjamin Franklin: The Way to Wealth
Pingback: Moonwalking with Einstein
Pingback: Work the System
Pingback: biotechnology degree salary
Pingback: Born a Crime: Stories from a South African Childhood
Pingback: what jobs are in the biotechnology field?
Pingback: The 4 Hour Body: An Uncommon Guide to Rapid Fat Loss, Incredible Sex and Becoming Superhuman
Pingback: Mans Search for Meaning
Pingback: biotechnology careers list and salaries
Pingback: The Untethered Soul
Pingback: The 10X Rule
Pingback: biotechnology career opportunities
Pingback: job opportunities for biotechnology graduates
Pingback: biotechnology career opportunities
Pingback: job opportunities for biotechnology graduates
Pingback: biotechnology careers in india
Pingback: palestine sunglasses
Pingback: kufiya
Pingback: palestine sunglasses
Pingback: The War of Art
Pingback: palestine sunglasses
Pingback: palestine sunglasses
Pingback: keffiyeh
Pingback: kufiya
Pingback: A Short Guide to a Long-Life
Pingback: keffiyeh
Pingback: kufiya
Pingback: keffiyeh
Pingback: The Everything Store
Pingback: palestine sunglasses
Pingback: Total Recall
Pingback: keffiyeh
Pingback: Keep Any Promise
Pingback: palestine sunglasses
Pingback: palestine sunglasses
Pingback: kufiya
Pingback: palestine sunglasses
Pingback: kufiya
Pingback: keffiyeh
Pingback: keffiyeh
Pingback: palestine sunglasses
Pingback: ag13 battery
Pingback: button cell battery
Pingback: ag13 battery
Pingback: ag13 battery
Pingback: button cell battery
Pingback: button cell battery
Pingback: ag13 button battery
Pingback: ag13 button battery
Pingback: Going Here
Pingback: Going Here
Pingback: Click This Link
Pingback: Learn More
Pingback: Read This
Pingback: Get More Info
Pingback: Visit This Link
Pingback: Homepage
Pingback: Visit This Link
Pingback: Home Page
Pingback: Get More Info
Pingback: Click Here
Pingback: Read More
Pingback: Find Out More
Pingback: Web Site
Pingback: Discover More
Pingback: Read This
Pingback: Read More Here
Pingback: Home Page
Pingback: Learn More
Pingback: Visit This Link
Pingback: Learn More Here
Pingback: Decubal face vital cream
Pingback: sas
Pingback: hortonworks
Pingback: sas
Pingback: Divya Arora Goa Independent Escorts Services
Pingback: afp
Pingback: mysql
Pingback: sdi
Pingback: seebeyond
Pingback: cpa
Pingback: ahip
Pingback: cpa
Pingback: apc
Pingback: Certification Dump
Pingback: apics
Pingback: IBM Certifications
Pingback: polycom
Pingback: workkeys
Pingback: nokia
Pingback: garp
Pingback: Simran Batra Independent Escorts in Kolkata
Pingback: peoplecert
Pingback: axis
Pingback: android
Pingback: fortinet
Pingback: liferay
Pingback: res
Pingback: redhat
Pingback: eccouncil
Pingback: Ashna Ahuja Escorts Services in Kolkata
Pingback: beac
Pingback: infosys
Pingback: haad
Pingback: afp
Pingback: acsm
Pingback: symantec
Pingback: Pitch Perfect
Pingback: appsense
Pingback: mcdata
Pingback: Wholesale green fabric
Pingback: Sofia Desai Escorts Services in Goa
Pingback: rsa
Pingback: infosys
Pingback: Latest braindumps
Pingback: Latest Exam VCE
Pingback: IT Certifications
Pingback: ged
Pingback: ism
Pingback: juniper
Pingback: isc
Pingback: eccouncil
Pingback: best way to invest
Pingback: Mayra Khan Escorts Services in Kolkata
Pingback: organic cotton fabric wholesale
Pingback: iisfa
Pingback: isilon
Pingback: extreme-networks
Pingback: afp
Pingback: ahima
Pingback: Super Better
Pingback: juniper
Pingback: cisco
Pingback: mile2
Pingback: Onward
Pingback: Crushing It
Pingback: Clash Royale cheats mobile
Pingback: iassc
Pingback: guidance-software
Pingback: Dot Com Secrets
Pingback: recycled cotton fabric
Pingback: sybase
Pingback: network-general
Pingback: amazon
Pingback: CCNA
Pingback: spss
Pingback: Candlestick Charting Explained Workbook
Pingback: Elon Musk Book
Pingback: The First 20 Hours
Pingback: cips
Pingback: informatica
Pingback: recycled polyester fabric wholesale
Pingback: salesforce
Pingback: hp
Pingback: cybertech back brace
Pingback: Deep Work
Pingback: cips
Pingback: Shopping search
Pingback: master class
Pingback: Good to Great
Pingback: unsecured loans
Pingback: athlectic greens
Pingback: equipment financing
Pingback: toe nail fungus
Pingback: audible
Pingback: metamucil
Pingback: probiotics
Pingback: foam roller
Pingback: new mood
Pingback: toenail fungus infections
Pingback: Bad Credit Loans
Pingback: toenail fungus treat
Pingback: Benjamin Franklins Book of Virtues
Pingback: Tools of Titans
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Managing Oneself
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Spider MMO - The Best Online Browser Games 2018
Pingback: Best Baby Walkers and Jumpers
Pingback: Honey Preet Bangalore Escorts Services
Pingback: Best Baby Walkers and Jumpers
Pingback: coupons for online shopping
Pingback: best online discount shopping
Pingback: ici
Pingback: body shop online coupons
Pingback: conseilme.com
Pingback: lien
Pingback: www.conseilme.com
Pingback: discount online shopping sites
Pingback: shopping coupons online
Pingback: discount online shopping websites
Pingback: conseilme.com
Pingback: Eva J Law Independent Goa Escorts Services
Pingback: ici
Pingback: source
Pingback: best online discount shopping
Pingback: discount online shopping sites
Pingback: Trunk Injections
Pingback: le magazine
Pingback: conseilme.com
Pingback: le magazine
Pingback: conseilme.com
Pingback: cursos online portal educa
Pingback: conseilme
Pingback: conseilme.com
Pingback: conseilme.com
Pingback: voir
Pingback: voir
Pingback: voir
Pingback: le magazine
Pingback: ici
Pingback: Spark Training Bangalore
Pingback: lien
Pingback: Spark Training In Bangalore
Pingback: Apache Spark Training Bangalore
Pingback: Apache Spark Training In Bangalore
Pingback: conseilme
Pingback: lien
Pingback: conseilme.com
Pingback: voir
Pingback: HOTELS IN LONAVALA
Pingback: source
Pingback: phantom orion bb118
Pingback: takara tomy phantom orion beyblade
Pingback: manjaro comandos
Pingback: bokep japan terbaru
Pingback: takara tomy
Pingback: here
Pingback: indo video
Pingback: video bolep
Pingback: bokep jepanese
Pingback: download bokeb jepang
Pingback: bokep xnxx
Pingback: bokep streaming jepang
Pingback: video bokeb
Pingback: download bokep video
Pingback: download bokep video
Pingback: download bokeb indo
Pingback: bokep indonesia
Pingback: DC Fawcett Virtual Wholesaling
Pingback: video bf jepang
Pingback: takara tomy bb118
Pingback: bokep porno
Pingback: toys
Pingback: www.amazon.com/Beyblades-JAPANESE-Fusion-Starter-Phantom/dp/B0054XOMX4/ref=sr_1_2?m=AZPT26WLSX32I&s=merchant-items&ie=UTF8&qid=1525922470&sr=1-2
Pingback: comandos apt
Pingback: gan69
Pingback: takara tomy phantom orion beyblade
Pingback: jilbab bugil
Pingback: video sex indo mp4
Pingback: here
Pingback: phantom orion b:d 4d beyblade
Pingback: download bokeb jepang
Pingback: china fucking
Pingback: beyblades
Pingback: download bokep china
Pingback: abg bokep
Pingback: china video sex
Pingback: debian apt
Pingback: Travel
Pingback: video abg xxx
Pingback: china movie porn
Pingback: bokep china hot
Pingback: download video bokep 2018
Pingback: hot sex china
Pingback: see more
Pingback: film hot china terbaru
Pingback: skandal abg terbaru
Pingback: abg indo 3gp
Pingback: pepek abg
Pingback: bokep abg sange
Pingback: abg bugil bandung
Pingback: Casino
Pingback: tocil abg
Pingback: Cheap
Pingback: abg goyang bugil
Pingback: abg bugil ngentot
Pingback: implante dental fortaleza
Pingback: quanto tempo demora para fazer um implante dentario
Pingback: tobrut abg
Pingback: fotos de lente de contato dental
Pingback: clareamento dental em fortaleza
Pingback: colmek abg
Pingback: ngentot abg sma
Pingback: Virtual Rehabbing
Pingback: bokep streaming abg cantik
Pingback: video abg streaming
Pingback: abg toge cantik
Pingback: abg tobrut bugil
Pingback: abg ngentot bareng
Pingback: video mesum abg cantik
Pingback: sex indonesia abg
Pingback: video bokep abg india
Pingback: abg diperkosa rame rame
Pingback: abg cantik streaming
Pingback: sex abg bugil
Pingback: bokep abg indo ngentot
Pingback: abg pentil
Pingback: abg kalimantan bugil
Pingback: abg imut hot
Pingback: abg manado bugil
Pingback: abg sma nungging
Pingback: bugil abg terbaru
Pingback: abg bugil di kelas
Pingback: abg nakal ngentot
Pingback: find a salon
Pingback: hairdressers near me
Pingback: abg cantik bugil sange
Pingback: diamond dremel cutting wheel
Pingback: cewek abg indonesia ngentot
Pingback: book beautician appointment
Pingback: abg toge twitter
Pingback: find a beautician
Pingback: tante arab ngesex
Pingback: local beauty salon
Pingback: abg buka rok
Pingback: arab sex 3gp
Pingback: hd porn arab
Pingback: arab porn.com
Pingback: video tante arab
Pingback: bokep abg 2015
Pingback: twitter abg mesum
Pingback: Virtual Rehabbing
Pingback: abg jaman now
Pingback: flim porno arab
Pingback: penari arab hot
Pingback: arab bugi
Pingback: arab saudi bokep
Pingback: find a salon
Pingback: vidio ngewe arab
Pingback: book makeup appointment online
Pingback: local beauty salon
Pingback: video prno arab
Pingback: film sek arab
Pingback: meki arab hot
Pingback: www kontol arab com
Pingback: hijab xxx
Pingback: Satoshi
Pingback: video arab sek
Pingback: phantom orion b:d 4d beyblade
Pingback: phantom orion b:d 4d beyblade
Pingback: website laten maken
Pingback: Bitcoin News
Pingback: phantom orion beyblade
Pingback: jablay cikarang barat
Pingback: indonesian hijab porn
Pingback: takara tomy bb118
Pingback: video bokep hijab indo
Pingback: www.amazon.com/Beyblades-JAPANESE-Fusion-Starter-Phantom/dp/B0054XOMX4/ref=sr_1_2?m=AZPT26WLSX32I&s=merchant-items&ie=UTF8&qid=1525922470&sr=1-2
Pingback: streaming hijab
Pingback: hijab smp
Pingback: website laten maken
Pingback: hijab porn free
Pingback: jilbab horny
Pingback: tn660 toner cartridge refill
Pingback: funny news
Pingback: funny
Pingback: www.goledelraganello.com
Pingback: Torrentismo gole del raganello
Pingback: DC Fawcett Virtual Rehabbing
Pingback: COACHING CAMPO GRANDE
Pingback: CURSO DE PSICOLOGIA POSITIVA
Pingback: CURSO DE PSICOLOGIA POSITIVA MS
Pingback: CURSO DE PSICOLOGIA POSITIVA
Pingback: free app for pc download
Pingback: free games download for pc
Pingback: games for windows pc download
Pingback: DC Fawcett Virtual Rehabbing
Pingback: full apps download
Pingback: Cursos pela internet
Pingback: clinica de implante dentario em fortaleza
Pingback: Cursos pela internet
Pingback: Cursos online
Pingback: quanto custa um implante de dente
Pingback: implante preço fortaleza
Pingback: dentista implante dental fortaleza
Pingback: Cursos online
Pingback: games for pc download
Pingback: dentista implante dental fortaleza
Pingback: Rc cursos online
Pingback: Rc cursos online
Pingback: Rc cursos online
Pingback: dentista implante dental fortaleza
Pingback: dentista implante fortaleza
Pingback: implante dental em fortaleza
Pingback: tipos de implantes dentais
Pingback: implante dental em fortaleza
Pingback: dentista implante fortaleza
Pingback: implante dentário em fortaleza
Pingback: clinica de implante dentario em fortaleza
Pingback: implante dental fortaleza
Pingback: implante dental fortaleza
Pingback: pc app free download
Pingback: clinica implante em fortaleza
Pingback: dentista implante fortaleza
Pingback: implante dental fortaleza
Pingback: implante dental fortaleza
Pingback: implante dental fortaleza
Pingback: app download for windows
Pingback: Cursos pela internet
Pingback: Cursos online
Pingback: Cursos online
Pingback: Rc cursos online
Pingback: Cursos online
Pingback: Cursos pela internet
Pingback: James Tracy
Pingback: free app for pclaptop app free download
Pingback: Cursos pela internet
Pingback: Cursos pela internet
Pingback: pc games free download full version for windows 7
Pingback: scripts for plays
Pingback: pc games free download for windows 8
Pingback: app download for windows 7
Pingback: free games download for pc
Pingback: software download for windows 10
Pingback: free download for windows 8
Pingback: Best personal injury attorney Chicago
Pingback: pc games free download full version for windows 7
Pingback: affordable business attire
Pingback: office attire for work
Pingback: app download for windows
Pingback: maxi dresses
Pingback: trendy blouses
Pingback: pc apps free download
Pingback: app download for windows
Pingback: white bathing suit top
Pingback: summer pocketbooks
Pingback: jeans sale
Pingback: apps download for windows 10
Pingback: pc games for windows 7
Pingback: free download for pc windows
Pingback: free laptop games download
Pingback: Gatwick airport taxi
Pingback: Gatwick airport taxi
Pingback: London airport taxis
Pingback: Gatwick pickups
Pingback: Heathrow pickups
Pingback: Gatwick pickups
Pingback: gym equipment
Pingback: London airport taxis
Pingback: Heathrow pickups
Pingback: pilates reformer
Pingback: download games for windows 7
Pingback: Air Rower
Pingback: app pc download for windows
Pingback: Gatwick taxi
Pingback: Gatwick pickups
Pingback: app for pc download
Pingback: Heathrow taxi
Pingback: Squat Rack
Pingback: car service from heathrow to london
Pingback: pilates training equipmen packages
Pingback: Gatwick pickups
Pingback: airport pickups
Pingback: games for windows pc download
Pingback: upright bike for sale
Pingback: free download for pc
Pingback: pc app free download
Pingback: Studio projektowe
Pingback: pilates reformer for sale
Pingback: water rowing machines
Pingback: app download for windows
Pingback: spinning bike
Pingback: free full download for windows pc
Pingback: Virtual Rehabbing
Pingback: Brand design
Pingback: Evree design
Pingback: skillmill treadmill for sale
Pingback: thermal carafe
Pingback: thermos flask
Pingback: pc games free download for windows 10
Pingback: large thermos
Pingback: coffee carafe
Pingback: apps for pc download
Pingback: how to learn mandarin Chinese for beginners
Pingback: best app to learn Chinese
Pingback: apps for pc download
Pingback: how to learn mandarin
Pingback: apps for learning Chinese
Pingback: best way to learn mandarin
Pingback: apps for learning Chinese
Pingback: best way to learn Chinese
Pingback: tea thermos
Pingback: apps for learning Chinese
Pingback: how to learn Chinese
Pingback: free games download for windows 8
Pingback: how to learn Chinese characters
Pingback: learn to speak Chinese
Pingback: best way to learn Chinese
Pingback: how to learn pinyin
Pingback: apps for learning Chinese
Pingback: learn to speak Chinese
Pingback: how to learn Chinese language
Pingback: how to learn Chinese
Pingback: how to learn Chinese
Pingback: learn to speak Chinese
Pingback: best way to learn mandarin
Pingback: best way to learn Chinese
Pingback: how to learn pinyin
Pingback: how to learn Chinese writing
Pingback: the Easiest way to learn mandarin Chinese
Pingback: how to learn pinyin
Pingback: apps for learning Chinese
Pingback: pc games for windows 7
Pingback: how to learn Chinese
Pingback: learn to speak Chinese
Pingback: how to learn Chinese pinyin
Pingback: learn Chinese fast
Pingback: the Easiest way to learn mandarin Chinese
Pingback: how to learn Chinese pinyin
Pingback: learn Chinese app
Pingback: coffee dispenser
Pingback: best way to learn Chinese
Pingback: how to learn Chinese language
Pingback: learn to speak mandarin
Pingback: best way to learn Chinese
Pingback: how to learn Chinese pinyin
Pingback: best way to learn Chinese
Pingback: best way to learn Chinese
Pingback: coffee carafe
Pingback: the Easiest way to learn mandarin Chinese
Pingback: how to learn Chinese
Pingback: apps for learning Chinese
Pingback: how to learn pinyin
Pingback: insulated carafe
Pingback: app in Chinese
Pingback: how to learn Chinese pinyin
Pingback: thermal carafe
Pingback: how to learn pinyin
Pingback: best way to learn mandarin
Pingback: DC Fawcett Virtual Wholesaling
Pingback: learn to speak Chinese
Pingback: thermos flask
Pingback: how to learn Chinese characters
Pingback: learn to speak Chinese
Pingback: how to learn Chinese writing
Pingback: best way to learn mandarin
Pingback: carafe with lid
Pingback: best way to learn mandarin
Pingback: best way to learn Chinese
Pingback: learn to speak mandarin
Pingback: carafe with lid
Pingback: best way to learn Chinese
Pingback: how to learn mandarin Chinese for beginners
Pingback: best way to learn Chinese
Pingback: how to learn pinyin
Pingback: thermal carafe
Pingback: coffee thermos
Pingback: carafe with lid
Pingback: coffee carafe
Pingback: carafe with lid
Pingback: coffee carafe
Pingback: best thermal coffee carafe
Pingback: stainless steel vacuum carafe
Pingback: thermal carafe
Pingback: situs judi online
Pingback: tea thermos
Pingback: best thermal coffee carafe
Pingback: thermos flask
Pingback: carafe with lid
Pingback: 안전놀이터
Pingback: coffee carafe
Pingback: large thermos
Pingback: tea thermos
Pingback: large thermos
Pingback: large thermos
Pingback: carafe with lid
Pingback: large thermos
Pingback: carafe with lid
Pingback: DC Fawcett Virtual Wholesaling
Pingback: lanyard personalizzati
Pingback: porta badge personalizzati online
Pingback: 8 Ball Pool Unlimited Coins
Pingback: stock trading&page=1
Pingback: 8 Ball Pool Free Coins Links
Pingback: Technologies Pvt Ltd~8888
Pingback: 8 Ball Pool Coins Tricks
Pingback: market Training in hyderabad.html
Pingback: Software/
Pingback: 1998 world cup
Pingback: Estate Sale Jewelry
Pingback: Estate Sale Jewelry
Pingback: bc football
Pingback: richmond football
Pingback: lowes lumber cedar
Pingback: lacci portabadge
Pingback: texas uil football
Pingback: Estate Sales 30 years experience
Pingback: Estate Liquidation Orange County California
Pingback: red cedar ceiling
Pingback: 4 x 6 x 8
Pingback: aashirvaad sugar release control atta
Pingback: 6 inch cedar lap siding
Pingback: siding that looks like a log cabin
Pingback: Business Liquidation Orange County California
Pingback: Estate Liquidation Orange County California
Pingback: siding instalation
Pingback: ravens football schedule
Pingback: Virtual Rehabbing
Pingback: hip flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Vizio TV Sale
Pingback: Hip Flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: Smart Android TV
Pingback: hip flask
Pingback: Fire TV Sale
Pingback: gadget portachiavi personalizzati
Pingback: hip flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Samsung TV Sale
Pingback: hip flask
Pingback: Hip Flask
Pingback: Leslie
Pingback: Hip Flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: hip flask
Pingback: hip flask
Pingback: coinnewscenter
Pingback: hip flask
Pingback: Hip Flask
Pingback: online furniture purchase bangalore
Pingback: sofa set online shopping in chennai
Pingback: hip flask
Pingback: hip flask
Pingback: pinch harmonics guitar
Pingback: Hip Flask
Pingback: hip flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: bitcoin
Pingback: Porn
Pingback: hip flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: Skyline University College
Pingback: hip flask
Pingback: Philadelphia University
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: Hip Flask
Pingback: hip flask
Pingback: cryptocurrencynews
Pingback: hip flask
Pingback: flower garden decor
Pingback: solar garden
Pingback: garden lighting solar
Pingback: flower garden decor
Pingback: Al-Zaytoonah University
Pingback: solar garden lights outdoor stakes
Pingback: in the light of the garden
Pingback: Buy Office 2013 Professional Plus
Pingback: decorative solar lights
Pingback: solar garden
Pingback: Buy Windows 10
Pingback: outdoor yard lights
Pingback: outdoor yard lights
Pingback: flower garden decor
Pingback: flower garden decor
Pingback: ethereum
Pingback: Buy Windows 10 Home
Pingback: garden and outdoor
Pingback: solar flowers
Pingback: solar flowers
Pingback: spécialiste chauffage photovoltaïque neuchâtel
Pingback: solar powered garden lights
Pingback: decorative garden stakes
Pingback: garden and outdoor
Pingback: solar flowers
Pingback: decorative garden stakes
Pingback: solar powered garden lights
Pingback: lily flowers
Pingback: garden and outdoor
Pingback: chauffage neuchâtel
Pingback: garden and outdoor
Pingback: monero
Pingback: chauffage neuchâtel
Pingback: garden stakes decorative
Pingback: solar stake lights outdoor
Pingback: grave decorations
Pingback: garden solar lights outdoor decorative
Pingback: garden solar lights outdoor decorative
Pingback: solar yard decorations
Pingback: flower garden
Pingback: garden stake
Pingback: blockchain
Pingback: solar yard decorations
Pingback: garden solar lights outdoor decorative
Pingback: outdoor garden lights
Pingback: outdoor solar lights decorative
Pingback: solar lights outdoor decorative
Pingback: outdoor solar lights decorative
Pingback: solar lights outdoor decorative
Pingback: solar lights outdoor garden
Pingback: solar garden light
Pingback: solar garden decorations
Pingback: outdoor garden lights
Pingback: garden figurines
Pingback: flower lights
Pingback: outdoor garden lights
Pingback: it paslaugos
Pingback: it ukio prieziura
Pingback: led garden lights
Pingback: led garden lights
Pingback: it paslaugos
Pingback: coinbase
Pingback: vpn
Pingback: cheap car leasing
Pingback: led garden lights
Pingback: solar lights garden
Pingback: yard art
Pingback: solar garden lights outdoor
Pingback: garden decor
Pingback: garden decor
Pingback: garden lights solar powered
Pingback: garden lights
Pingback: solar yard lights
Pingback: administrador de condominio
Pingback: solar garden lights
Pingback: garden lights
Pingback: solar garden lights
Pingback: garden decorations outdoor
Pingback: litecoin
Pingback: software para condominios
Pingback: garden decor
Pingback: yard art
Pingback: solar yard lights
Pingback: software para gestão de condominios
Pingback: garden lights solar powered
Pingback: backyard lighting
Pingback: solar lights garden
Pingback: calla lily bulbs
Pingback: garden and outdoor
Pingback: solar garden lights
Pingback: outdoor yard lights
Pingback: brain enhancement pills
Pingback: flower garden
Pingback: garden lighting
Pingback: nootropic stack
Pingback: solar flower
Pingback: solar garden lights outdoor stakes
Pingback: lily flowers
Pingback: roughsex everyday !
Pingback: my asia sluts !
Pingback: brain supplements
Pingback: nootropic
Pingback: garden lighting solar
Pingback: flower garden decor
Pingback: ripple
Pingback: memory supplement for the brain
Pingback: in the light of the garden
Pingback: nootropic brain supplement
Pingback: garden decor
Pingback: solar flower
Pingback: flower garden decor
Pingback: led garden lights
Pingback: decorative solar lights
Pingback: solar garden decorations
Pingback: decorative solar lights
Pingback: outdoor garden lights
Pingback: backyard lighting
Pingback: solar yard decorations
Pingback: Takarítás
Pingback: flower garden
Pingback: in the light of the garden
Pingback: liverates
Pingback: Takaritas Budapest
Pingback: Takarítás Budapest
Pingback: garden art
Pingback: solar stake lights outdoor
Pingback: solar garden lights outdoor
Pingback: garden decorations outdoor
Pingback: yard art
Pingback: in the light of the garden
Pingback: garden figurines
Pingback: garden decor
Pingback: solar garden stakes
Pingback: decorative garden stakes
Pingback: free printables
Pingback: flower lights
Pingback: outdoor solar lights decorative
Pingback: solar lights outdoor garden
Pingback: solar garden light
Pingback: shop
Pingback: garden stake
Pingback: garden figurines
Pingback: newest army gear for soldiers
Pingback: garden flowers
Pingback: outdoor solar lights decorative
Pingback: in the light of the garden
Pingback: flower garden decor
Pingback: flower lights
Pingback: in the light of the garden
Pingback: backyard lighting
Pingback: solar garden stakes
Pingback: solar garden decorations
Pingback: Hemstädning Solna
Pingback: Hemstädning Solna
Pingback: Hemstädning Nacka
Pingback: Flyttstädning Sollentuna
Pingback: privacypolicy
Pingback: AR670 boots for military operations
Pingback: check out this site
Pingback: Continue
Pingback: Continue Reading
Pingback: found this site
Pingback: Discover More Here
Pingback: Continue Reading
Pingback: termsofservice
Pingback: Homepage
Pingback: Christian Investing
Pingback: Terry Sacka AAMS
Pingback: wireless car charger mount
Pingback: best way to lose weight
Pingback: Syrian Refugee Immigration
Pingback: Precious Metals IRA
Pingback: Wealth Preservation
Pingback: Asset Preservation
Pingback: Link
Pingback: Christian Gold
Pingback: The Jubilee Year
Pingback: vlog travel
Pingback: silver investment
Pingback: forum
Pingback: outfits
Pingback: Christian Investing
Pingback: Interesting Read
Pingback: Video Link
Pingback: Wealth Transfer
Pingback: IMF currencies
Pingback: Investing in Silver
Pingback: HB224
Pingback: Chinese Yuan
Pingback: 2015 prophecies
Pingback: Secure IRA
Pingback: Interesting Read
Pingback: Click Here
Pingback: where to find bee pollen in grocery store
Pingback: Teach Abroad
Pingback: Damoka
Pingback: truth about teaching english in china
Pingback: China Jobs
Pingback: Live abroad
Pingback: teaching english in china jobs
Pingback: Visa for China
Pingback: Visa for China
Pingback: Chinese Visa
Pingback: how long does honey syrup last
Pingback: Teach English
Pingback: Neptune Medical Devices
Pingback: Neptune Medical Devices
Pingback: Neptune Medical Devices
Pingback: Z Visa USA
Pingback: @China_Link_ESL
Pingback: golf clash hack 2018
Pingback: Chinese Visa
Pingback: Teach Abroad
Pingback: Z Visas China UK
Pingback: China Teacher
Pingback: where to buy local bee pollen
Pingback: Neptune Medical Devices
Pingback: Neptune Medical Devices
Pingback: Neptune Medical Devices
Pingback: Neptune Medical Devices
Pingback: ESL
Pingback: Z Visa Requirements 2020
Pingback: Home Page
Pingback: banana teether
Pingback: baby toothpaste
Pingback: how do you get bee pollen
Pingback: baby toothbrush 6 to 12 months
Pingback: baby toothpaste
Pingback: baby teeth
Pingback: Get the facts
Pingback: baby toothpaste
Pingback: baby teeth
Pingback: toddler toothbrush
Pingback: banana teether
Pingback: baby toothbrush
Pingback: baby toothpaste
Pingback: baby banana toothbrush
Pingback: baby toothbrush
Pingback: baby teeth
Pingback: infant toothbrush
Pingback: toddler toothpaste
Pingback: baby toothbrush
Pingback: baby banana toothbrush
Pingback: toddler toothpaste
Pingback: banana teether
Pingback: infant toothbrush
Pingback: toddler toothpaste
Pingback: Web Site
Pingback: how to make honey simple syrup
Pingback: Click This Link
Pingback: toddler toothpaste
Pingback: finger toothbrush for baby
Pingback: toothbrushes kids
Pingback: finger toothbrush for baby
Pingback: baby toothbrush 12 months and up
Pingback: toddler toothbrush
Pingback: infant toothbrush
Pingback: advogados comendador soares
Pingback: toothbrushes kids
Pingback: baby banana toothbrush
Pingback: infant toothbrush
Pingback: the alarm
Pingback: the alarm
Pingback: safesound personal alarm
Pingback: scream safe alarm keychain
Pingback: baby toothbrush 12 months and up
Pingback: scream safe alarm
Pingback: personal safe
Pingback: jack and jill toothpaste
Pingback: pocket guardian
Pingback: personal alarm
Pingback: safe sound personal alarm
Pingback: too much bee pollen
Pingback: safe sound personal alarm
Pingback: the alarm
Pingback: scream safe alarm keychain
Pingback: personal protection
Pingback: scream safe alarm
Pingback: personal protection
Pingback: personal alarm
Pingback: ring alarm
Pingback: safesound personal alarm
Pingback: baby toothbrush
Pingback: baby toothpaste
Pingback: safe and sound
Pingback: cupom desconto comendador soares
Pingback: personal safe
Pingback: personal alarm
Pingback: ring alarm
Pingback: safe and sound
Pingback: safe sound personal alarm
Pingback: personal safe
Pingback: personal alarms for women
Pingback: baby banana toothbrush
Pingback: personal protection
Pingback: damsel in defense products
Pingback: damsel in defense products
Pingback: safe and sound
Pingback: the alarm
Pingback: safesound personal alarm
Pingback: baby toothbrush
Pingback: ring alarm
Pingback: personal alarm
Pingback: safe sound personal alarm
Pingback: safesound personal alarm
Pingback: safesound personal alarm keychain
Pingback: scream safe alarm keychain
Pingback: scream safe alarm keychain
Pingback: personal alarm
Pingback: damsel in defense products
Pingback: finger toothbrush for baby
Pingback: jack and jill toothpaste
Pingback: safesound personal alarm keychain
Pingback: bee pollen health benefits
Pingback: the alarm
Pingback: personal protection
Pingback: scream safe alarm
Pingback: scream safe alarm keychain
Pingback: pocket guardian
Pingback: personal alarm
Pingback: personal alarms for women
Pingback: baby banana toothbrush
Pingback: damsel in defense products
Pingback: the alarm
Pingback: baby toothbrush 6 to 12 months
Pingback: ring alarm
Pingback: pocket guardian
Pingback: pocket guardian
Pingback: personal alarm
Pingback: safe and sound
Pingback: baby banana toothbrush
Pingback: safe and sound
Pingback: personal safe
Pingback: toothbrushes kids
Pingback: personal protection
Pingback: scream safe alarm keychain
Pingback: personal alarms for women
Pingback: safesound personal alarm keychain
Pingback: toddler toothpaste
Pingback: personal protection
Pingback: safe and sound
Pingback: safe and sound
Pingback: baby toothbrush
Pingback: safesound personal alarm keychain
Pingback: jack and jill toothpaste
Pingback: personal alarm
Pingback: damsel in defense
Pingback: safe and sound
Pingback: baby toothpaste
Pingback: damsel in defense products
Pingback: baby toothpaste
Pingback: pocket guardian
Pingback: pocket guardian
Pingback: banana teether
Pingback: safesound personal alarm
Pingback: baby teeth
Pingback: baby toothbrush
Pingback: ring alarm
Pingback: jack and jill toothpaste
Pingback: personal safe
Pingback: damsel in defense
Pingback: baby toothpaste
Pingback: organic bee pollen capsules
Pingback: personal alarms for women
Pingback: safe sound personal alarm
Pingback: the alarm
Pingback: personal alarms for women
Pingback: safe sound personal alarm
Pingback: scream safe alarm
Pingback: personal alarms for women
Pingback: safe sound personal alarm
Pingback: scream safe alarm keychain
Pingback: damsel in defense products
Pingback: baby toothbrush 6 to 12 months
Pingback: ring alarm
Pingback: damsel in defense products
Pingback: baby teeth
Pingback: safe and sound
Pingback: safesound personal alarm keychain
Pingback: damsel in defense
Pingback: personal safe
Pingback: finger toothbrush for baby
Pingback: personal alarms for women
Pingback: personal alarms for women
Pingback: toddler toothpaste
Pingback: damsel in defense
Pingback: baby toothbrush 6 to 12 months
Pingback: ring alarm
Pingback: safe sound personal alarm
Pingback: safe sound personal alarm
Pingback: personal protection
Pingback: personal safe
Pingback: scream safe alarm keychain
Pingback: Food Safety
Pingback: safe and sound
Pingback: personal alarm
Pingback: scream safe alarm keychain
Pingback: safesound personal alarm keychain
Pingback: safesound personal alarm
Pingback: damsel in defense
Pingback: damsel in defense
Pingback: safe and sound
Pingback: personal protection
Pingback: scream safe alarm keychain
Pingback: safesound personal alarm
Pingback: safe sound personal alarm
Pingback: safe sound personal alarm
Pingback: personal protection
Pingback: safe and sound
Pingback: baby toothbrush 12 months and up
Pingback: scream safe alarm
Pingback: safesound personal alarm keychain
Pingback: damsel in defense products
Pingback: safesound personal alarm
Pingback: personal alarms for women
Pingback: safesound personal alarm
Pingback: damsel in defense
Pingback: personal alarms for women
Pingback: ring alarm
Pingback: banana teether
Pingback: personal protection
Pingback: safe sound personal alarm
Pingback: safesound personal alarm
Pingback: pocket guardian
Pingback: scream safe alarm keychain
Pingback: ring alarm
Pingback: safe and sound
Pingback: baby banana toothbrush
Pingback: personal alarms for women
Pingback: personal safe
Pingback: buy 10 instagram followers
Pingback: scream safe alarm
Pingback: damsel in defense products
Pingback: personal alarm
Pingback: safesound personal alarm
Pingback: toddler toothpaste
Pingback: damsel in defense
Pingback: personal alarm
Pingback: toddler toothbrush
Pingback: the alarm
Pingback: finger toothbrush for baby
Pingback: personal safe
Pingback: jack and jill toothpaste
Pingback: safe and sound
Pingback: safesound personal alarm keychain
Pingback: banana teether
Pingback: scream safe alarm
Pingback: damsel in defense
Pingback: the alarm
Pingback: the alarm
Pingback: safe and sound
Pingback: safesound personal alarm keychain
Pingback: agen judi
Pingback: safe and sound
Pingback: personal protection
Pingback: ring alarm
Pingback: personal protection
Pingback: personal protection
Pingback: the alarm
Pingback: safesound personal alarm keychain
Pingback: damsel in defense products
Pingback: damsel in defense
Pingback: safesound personal alarm
Pingback: safesound personal alarm keychain
Pingback: damsel in defense products
Pingback: baby toothbrush
Pingback: personal alarms for women
Pingback: scream safe alarm
Pingback: damsel in defense
Pingback: personal alarm
Pingback: safe sound personal alarm
Pingback: infant toothbrush
Pingback: baby banana toothbrush
Pingback: safe and sound
Pingback: baby teeth
Pingback: baby toothbrush 6 to 12 months
Pingback: toddler toothbrush
Pingback: safe sound personal alarm
Pingback: damsel in defense
Pingback: personal protection
Pingback: damsel in defense products
Pingback: baby banana toothbrush
Pingback: ring alarm
Pingback: personal alarm
Pingback: ring alarm
Pingback: personal alarms for women
Pingback: damsel in defense products
Pingback: scream safe alarm
Pingback: baby teeth
Pingback: personal alarm
Pingback: safesound personal alarm
Pingback: safesound personal alarm
Pingback: damsel in defense products
Pingback: scream safe alarm keychain
Pingback: personal protection
Pingback: baby banana toothbrush
Pingback: personal alarms for women
Pingback: damsel in defense
Pingback: safe sound personal alarm
Pingback: the alarm
Pingback: safesound personal alarm
Pingback: buy 100 real youtube subscribers
Pingback: pocket guardian
Pingback: safe sound personal alarm
Pingback: safe and sound
Pingback: safe sound personal alarm
Pingback: personal alarms for women
Pingback: pocket guardian
Pingback: toothbrushes kids
Pingback: infant toothbrush
Pingback: baby toothbrush 6 to 12 months
Pingback: toddler toothpaste
Pingback: damsel in defense
Pingback: damsel in defense
Pingback: scream safe alarm
Pingback: safe and sound
Pingback: the alarm
Pingback: personal protection
Pingback: scream safe alarm
Pingback: safe and sound
Pingback: buy 100 facebook likes cheap
Pingback: personal alarms for women
Pingback: scream safe alarm keychain
Pingback: infant toothbrush
Pingback: safesound personal alarm
Pingback: personal alarms for women
Pingback: safesound personal alarm keychain
Pingback: safe and sound
Pingback: the alarm
Pingback: personal alarms for women
Pingback: scream safe alarm keychain
Pingback: finger toothbrush for baby
Pingback: personal protection
Pingback: safesound personal alarm keychain
Pingback: personal protection
Pingback: damsel in defense
Pingback: damsel in defense products
Pingback: damsel in defense
Pingback: safe sound personal alarm
Pingback: personal safe
Pingback: safe and sound
Pingback: the alarm
Pingback: baby toothbrush
Pingback: pocket guardian
Pingback: damsel in defense
Pingback: personal safe
Pingback: pocket guardian
Pingback: finger toothbrush for baby
Pingback: safe sound personal alarm
Pingback: personal protection
Pingback: baby toothbrush 6 to 12 months
Pingback: safe sound personal alarm
Pingback: safe sound personal alarm
Pingback: toothbrushes kids
Pingback: ring alarm
Pingback: ring alarm
Pingback: damsel in defense products
Pingback: safesound personal alarm keychain
Pingback: baby toothpaste
Pingback: scream safe alarm
Pingback: baby toothbrush 12 months and up
Pingback: the alarm
Pingback: buy real active youtube subscribers
Pingback: safesound personal alarm keychain
Pingback: pocket guardian
Pingback: ring alarm
Pingback: safe sound personal alarm
Pingback: damsel in defense
Pingback: scream safe alarm keychain
Pingback: damsel in defense
Pingback: safesound personal alarm keychain
Pingback: finger toothbrush for baby
Pingback: safesound personal alarm keychain
Pingback: safe and sound
Pingback: damsel in defense products
Pingback: personal alarm
Pingback: personal protection
Pingback: scream safe alarm keychain
Pingback: damsel in defense products
Pingback: scream safe alarm keychain
Pingback: scream safe alarm
Pingback: buy facebook business page likes
Pingback: personal protection
Pingback: personal alarm
Pingback: damsel in defense
Pingback: safesound personal alarm
Pingback: ring alarm
Pingback: ring alarm
Pingback: personal safe
Pingback: toothbrushes kids
Pingback: damsel in defense products
Pingback: the alarm
Pingback: personal protection
Pingback: baby toothbrush 6 to 12 months
Pingback: damsel in defense
Pingback: damsel in defense products
Pingback: damsel in defense
Pingback: baby toothbrush
Pingback: jack and jill toothpaste
Pingback: scream safe alarm
Pingback: safe and sound
Pingback: personal alarms for women
Pingback: scream safe alarm
Pingback: safe and sound
Pingback: toddler toothpaste
Pingback: pocket guardian
Pingback: ring alarm
Pingback: safe and sound
Pingback: safe sound personal alarm
Pingback: pocket guardian
Pingback: safesound personal alarm
Pingback: damsel in defense
Pingback: banana teether
Pingback: personal alarms for women
Pingback: damsel in defense products
Pingback: ring alarm
Pingback: personal alarm
Pingback: personal protection
Pingback: pocket guardian
Pingback: safesound personal alarm keychain
Pingback: safesound personal alarm
Pingback: safe sound personal alarm
Pingback: personal protection
Pingback: baby toothbrush 6 to 12 months
Pingback: personal alarms for women
Pingback: baby toothpaste
Pingback: personal safe
Pingback: buy 5000 instagram followers
Pingback: baby banana toothbrush
Pingback: pocket guardian
Pingback: safe and sound
Pingback: scream safe alarm keychain
Pingback: personal safe
Pingback: safe sound personal alarm
Pingback: pocket guardian
Pingback: safesound personal alarm keychain
Pingback: baby toothpaste
Pingback: damsel in defense
Pingback: baby banana toothbrush
Pingback: pocket guardian
Pingback: banana teether
Pingback: scream safe alarm keychain
Pingback: personal alarm
Pingback: baby teeth
Pingback: safe and sound
Pingback: safesound personal alarm
Pingback: the alarm
Pingback: personal alarms for women
Pingback: baby toothpaste
Pingback: pocket guardian
Pingback: baby teeth
Pingback: the alarm
Pingback: safe sound personal alarm
Pingback: safe sound personal alarm
Pingback: scream safe alarm keychain
Pingback: baby toothbrush
Pingback: safesound personal alarm keychain
Pingback: personal protection
Pingback: personal alarms for women
Pingback: personal safe
Pingback: scream safe alarm keychain
Pingback: baby toothpaste
Pingback: safesound personal alarm keychain
Pingback: safe sound personal alarm
Pingback: baby toothbrush
Pingback: personal protection
Pingback: safe and sound
Pingback: personal alarms for women
Pingback: scream safe alarm
Pingback: pocket guardian
Pingback: scream safe alarm
Pingback: personal safe
Pingback: the alarm
Pingback: personal alarm
Pingback: scream safe alarm
Pingback: the alarm
Pingback: safesound personal alarm keychain
Pingback: personal safe
Pingback: safesound personal alarm keychain
Pingback: scream safe alarm
Pingback: personal alarms for women
Pingback: personal safe
Pingback: safe and sound
Pingback: toddler toothbrush
Pingback: safesound personal alarm
Pingback: personal safe
Pingback: safe sound personal alarm
Pingback: Damien Hayward
Pingback: Maria Mattioli
Pingback: Hye Carle
Pingback: toddler toothpaste
Pingback: damsel in defense
Pingback: Emmie Robitaille
Pingback: scream safe alarm
Pingback: pocket guardian
Pingback: personal protection
Pingback: baby toothbrush
Pingback: Almeta Hoefler
Pingback: personal protection
Pingback: Teofila Yetman
Pingback: Agueda Heidecker
Pingback: Trinity Wilderman
Pingback: Isa Soni
Pingback: safe sound personal alarm
Pingback: safesound personal alarm
Pingback: personal alarm
Pingback: buy youtube views
Pingback: finger toothbrush for baby
Pingback: Serina Mealy
Pingback: safe sound personal alarm
Pingback: jack and jill toothpaste
Pingback: pocket guardian
Pingback: Marlyn Deveaux
Pingback: the alarm
Pingback: personal alarms for women
Pingback: Mariann Mcdavis
Pingback: scream safe alarm keychain
Pingback: Delma Christiansen
Pingback: Maxie Wingham
Pingback: pocket guardian
Pingback: Nevada Goold
Pingback: safe sound personal alarm
Pingback: Dwain Bibb
Pingback: Rosina Howser
Pingback: pocket guardian
Pingback: Denna Seeger
Pingback: safesound personal alarm
Pingback: Merrie Patrick
Pingback: scream safe alarm keychain
Pingback: Julio Ramos
Pingback: Kourtney Blay
Pingback: personal alarm
Pingback: Trinity Wilderman
Pingback: Carly Landrum
Pingback: personal alarms for women
Pingback: safe sound personal alarm
Pingback: safe sound personal alarm
Pingback: seller central
Pingback: Arletha Alldredge
Pingback: scream safe alarm
Pingback: Johnna Nunnally
Pingback: amazon in sale
Pingback: pocket guardian
Pingback: Ping Geyer
Pingback: sell on amazon
Pingback: amazon seller
Pingback: pocket guardian
Pingback: personal protection
Pingback: damsel in defense products
Pingback: junlgescout
Pingback: personal protection
Pingback: amazon marketplace
Pingback: seller amazon
Pingback: personal protection
Pingback: Serina Mealy
Pingback: Mariann Mcdavis
Pingback: seller central amazon
Pingback: Markus Guinan
Pingback: Abe Pietrowski
Pingback: Jed Istre
Pingback: personal alarms for women
Pingback: damsel in defense products
Pingback: safesound personal alarm
Pingback: Dwayne Olander
Pingback: Meri Weigand
Pingback: amazon in sale
Pingback: Cornell Rumph
Pingback: scream safe alarm
Pingback: how to sell things on amazon
Pingback: safesound personal alarm keychain
Pingback: Leena Yale
Pingback: safesound personal alarm keychain
Pingback: seller amazon
Pingback: Latoya Kollar
Pingback: damsel in defense
Pingback: Vincent Lesane
Pingback: personal protection
Pingback: the alarm
Pingback: the alarm
Pingback: safesound personal alarm
Pingback: safesound personal alarm keychain
Pingback: Markus Guinan
Pingback: Dusty Sitzes
Pingback: Tangela Allman
Pingback: safesound personal alarm
Pingback: Adelaida Pillot
Pingback: Branda Mariscal
Pingback: personal safe
Pingback: Georgette Loiacono
Pingback: Leighann Deines
Pingback: Thuy Wiseley
Pingback: Sylvester Alvord
Pingback: Ping Geyer
Pingback: junlgescout
Pingback: personal safe
Pingback: personal protection
Pingback: ring alarm
Pingback: Sebrina Weiss
Pingback: damsel in defense
Pingback: Cornell Rumph
Pingback: Ultimas notícias da Paraíba
Pingback: personal safe
Pingback: damsel in defense products
Pingback: Tiny Dahle
Pingback: Johnna Nunnally
Pingback: damsel in defense products
Pingback: Wanda Kuehn
Pingback: scream safe alarm keychain
Pingback: damsel in defense
Pingback: what to sell on amazon
Pingback: seller amazon
Pingback: personal alarm
Pingback: Tattoos
Pingback: amazon seller
Pingback: scream safe alarm
Pingback: personal alarm
Pingback: personal protection
Pingback: pocket guardian
Pingback: safesound personal alarm
Pingback: damsel in defense
Pingback: safesound personal alarm
Pingback: personal alarm
Pingback: damsel in defense products
Pingback: Notícias do Cariri
Pingback: scream safe alarm
Pingback: personal safe
Pingback: scream safe alarm keychain
Pingback: personal safe
Pingback: seller central
Pingback: scream safe alarm
Pingback: damsel in defense
Pingback: Notícias
Pingback: amazon sell
Pingback: safesound personal alarm
Pingback: damsel in defense products
Pingback: ring alarm
Pingback: damsel in defense products
Pingback: personal safe
Pingback: amazon marketplace
Pingback: damsel in defense
Pingback: damsel in defense
Pingback: the alarm
Pingback: pocket guardian
Pingback: safe sound personal alarm
Pingback: safesound personal alarm
Pingback: pocket guardian
Pingback: the alarm
Pingback: safesound personal alarm keychain
Pingback: damsel in defense
Pingback: pocket guardian
Pingback: personal safe
Pingback: ring alarm
Pingback: scream safe alarm keychain
Pingback: ring alarm
Pingback: ring alarm
Pingback: pocket guardian
Pingback: pocket guardian
Pingback: work from home
Pingback: damsel in defense
Pingback: personal protection
Pingback: how to sell things on amazon
Pingback: amazon fba
Pingback: personal protection
Pingback: damsel in defense products
Pingback: personal safe
Pingback: safe and sound
Pingback: safesound personal alarm
Pingback: the alarm
Pingback: damsel in defense
Pingback: safesound personal alarm keychain
Pingback: personal protection
Pingback: personal safe
Pingback: ring alarm
Pingback: safesound personal alarm keychain
Pingback: safe sound personal alarm
Pingback: scream safe alarm
Pingback: pocket guardian
Pingback: safesound personal alarm
Pingback: seller amazon
Pingback: damsel in defense
Pingback: seller amazon
Pingback: personal protection
Pingback: personal safe
Pingback: personal alarms for women
Pingback: selling on amazon
Pingback: pocket guardian
Pingback: scream safe alarm
Pingback: damsel in defense products
Pingback: ring alarm
Pingback: sell on amazon
Pingback: pocket guardian
Pingback: safe sound personal alarm
Pingback: amazon fba
Pingback: personal safe
Pingback: scream safe alarm keychain
Pingback: safesound personal alarm keychain
Pingback: safe and sound
Pingback: make money easy
Pingback: how to sell things on amazon
Pingback: amazon fba
Pingback: seller central amazon
Pingback: seller central
Pingback: junlgescout
Pingback: seller amazon
Pingback: amazon fba
Pingback: seller central amazon
Pingback: amazon sell
Pingback: Helium 10
Pingback: sell on amazon
Pingback: make money easy
Pingback: seller central
Pingback: amazon seller
Pingback: St-Eugene EXIT Realty Listings
Pingback: amazon fba
Pingback: make money easy
Pingback: selling on amazon
Pingback: seller central amazon
Pingback: amazon in sale
Pingback: amazon in sale
Pingback: how to sell things on amazon
Pingback: amazon fba
Pingback: seller central
Pingback: sell on amazon
Pingback: junlgescout
Pingback: how to sell on amazon
Pingback: sell on amazon
Pingback: how to sell stuff on amazon
Pingback: how to sell on amazon
Pingback: junlgescout
Pingback: how to sell on amazon
Pingback: how to sell things on amazon
Pingback: sell on amazon
Pingback: seller amazon
Pingback: make money easy
Pingback: seller central amazon
Pingback: amazon sell
Pingback: what to sell on amazon
Pingback: stanstead airport taxi
Pingback: how to sell stuff on amazon
Pingback: seller central amazon
Pingback: amazon marketplace
Pingback: luton airport transfers
Pingback: amazon fba
Pingback: how to sell on amazon
Pingback: seller central
Pingback: amazon marketplace
Pingback: seller central amazon
Pingback: seller amazon
Pingback: free money
Pingback: seller central
Pingback: seller central
Pingback: junlgescout
Pingback: Helium 10
Pingback: make money easy
Pingback: how to sell on amazon
Pingback: amazon sell
Pingback: junlgescout
Pingback: how to start selling on amazon
Pingback: seller amazon
Pingback: amazon marketplace
Pingback: how to sell stuff on amazon
Pingback: seller central
Pingback: seller amazon
Pingback: amazon marketplace
Pingback: amazon sell
Pingback: seller central
Pingback: how to start selling on amazon
Pingback: sell on amazon
Pingback: free money
Pingback: amazon marketplace
Pingback: amazon seller
Pingback: sell on amazon
Pingback: seller amazon
Pingback: baby organizer
Pingback: baby organizer
Pingback: baby storage organizer
Pingback: nanny Jakarta
Pingback: baby shower registry
Pingback: storage caddy
Pingback: baby organizer
Pingback: baby storage organizer
Pingback: baby diaper caddy organizer
Pingback: gift registry baby shower
Pingback: storage caddy
Pingback: baby shower registry
Pingback: baby diaper caddy
Pingback: changing table organizer
Pingback: diaper organizer
Pingback: diaper caddy organizer
Pingback: diaper caddy
Pingback: baby basket
Pingback: baby shower registry
Pingback: baby organizer
Pingback: nursery organizer
Pingback: diaper organizer
Pingback: gift registry
Pingback: nursery organizer
Pingback: baby registry must haves
Pingback: gift registry baby shower
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: baby diaper caddy
Pingback: gift registry baby shower
Pingback: hair growth vitamin
Pingback: changing table organizer
Pingback: nursery organizer
Pingback: changing table organizer
Pingback: changing table organizer
Pingback: Instagram Takipçi Satýn Al 9.99 TL'den Baþlayan Fiyatlarla Hýzlý Teslimat
Pingback: 5000 Türk Takipçi Asistagram.com
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: 2000 Türk Takipçi Asistagram.com
Pingback: faster hair growth
Pingback: 1000 Türk Takipçi Asistagram.com
Pingback: changing table organizer
Pingback: baby diaper caddy organizer
Pingback: faster hair growth
Pingback: diaper caddy
Pingback: 3000 Türk Takipçi Asistagram.com
Pingback: faster hair growth
Pingback: storage caddy
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: baby shower registry
Pingback: diaper organizer
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: gift registry
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: nursery organizer
Pingback: baby basket
Pingback: nursery organizer
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: baby registry must haves
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: gift registry
Pingback: hair growth vitamin
Pingback: baby diaper caddy
Pingback: gift registry
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: baby shower registry
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: baby basket
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: diaper caddy organizer
Pingback: hair growth vitamin
Pingback: baby registry must haves
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: diaper caddy organizer
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: baby diaper caddy
Pingback: diaper caddy organizer
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: storage caddy
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: Türk Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: Instagram Aktif Türk Takipçi Asistagram.com
Pingback: hair growth vitamin
Pingback: baby diaper caddy organizer
Pingback: Türk Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: Türk Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: Instagram Aktif Türk Takipçi Asistagram.com
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: gift registry
Pingback: changing table organizer
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: diaper caddy organizer
Pingback: Instagram Aktif Türk Takipçi Asistagram.com
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: gift registry
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: baby registry must haves
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: baby organizer
Pingback: baby diaper caddy organizer
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: baby basket
Pingback: baby registry must haves
Pingback: faster hair growth
Pingback: baby basket
Pingback: hair growth supplement
Pingback: diaper caddy organizer
Pingback: changing table organizer
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: hair growth vitamin
Pingback: gift registry baby shower
Pingback: faster hair growth
Pingback: Instagram Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: Instagram Kombo Paketi Asistagram.com Hemen Satýn Al
Pingback: Instagram Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: Türk Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: Instagram Otomatik Beðeni Asistagram.com Hemen Satýn Al
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: diaper caddy organizer
Pingback: baby basket
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: gift registry
Pingback: changing table organizer
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: diaper organizer
Pingback: faster hair growth
Pingback: diaper caddy organizer
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: baby diaper caddy organizer
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: changing table organizer
Pingback: hair growth supplement
Pingback: gift registry
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: Palm Muting
Pingback: nursery organizer
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: changing table organizer
Pingback: hair growth supplement
Pingback: nursery organizer
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: baby organizer
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: diaper caddy
Pingback: baby organizer
Pingback: hair growth vitamin
Pingback: storage caddy
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: baby registry must haves
Pingback: hair growth vitamin
Pingback: diaper caddy
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: changing table organizer
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: roulette uang asli
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: baby basket
Pingback: gift registry
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: baby diaper caddy organizer
Pingback: diaper caddy organizer
Pingback: hair growth vitamin
Pingback: gift registry baby shower
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: baby basket
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: web development jobs utah
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: baby basket
Pingback: faster hair growth
Pingback: web development interview questions
Pingback: baby diaper caddy
Pingback: nursery organizer
Pingback: hair growth vitamin
Pingback: r programming language web development
Pingback: online shop yang trusted
Pingback: web development in assembly
Pingback: diaper caddy organizer
Pingback: hair growth supplement
Pingback: online shop kaise khole
Pingback: hair growth supplement
Pingback: c&a online shopping
Pingback: web development quote example
Pingback: diaper organizer
Pingback: online shop coming soon
Pingback: faster hair growth
Pingback: online shop ph
Pingback: web development environment mac
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: hair growth vitamin
Pingback: diaper caddy organizer
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: online shop gratis ongkir
Pingback: hair growth supplement
Pingback: baby shower registry
Pingback: baby diaper caddy organizer
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: online shop kenya
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: nursery organizer
Pingback: baby diaper caddy organizer
Pingback: changing table organizer
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: diaper organizer
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: baby diaper caddy organizer
Pingback: changing table organizer
Pingback: online shop yang lagi booming
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: baby diaper caddy organizer
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: d mart online shopping
Pingback: storage caddy
Pingback: baby organizer
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: baby storage organizer
Pingback: web development history
Pingback: faster hair growth
Pingback: iphone 6 online shopping in saudi arabia
Pingback: faster hair growth
Pingback: gift registry baby shower
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: diaper organizer
Pingback: hair growth vitamin
Pingback: computer services youngstown ohio
Pingback: hair growth vitamin
Pingback: network installation materials
Pingback: computer services 77095
Pingback: hair growth vitamin
Pingback: solar solutions mentor
Pingback: hair growth supplement
Pingback: solar solutions oü
Pingback: hair growth supplement
Pingback: network installation failed hp printer
Pingback: baby organizer
Pingback: u.s computer services company
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: solar solutions scotland
Pingback: network installation of centos 7
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: surface pro 4 web development
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: network installation bradenton
Pingback: hair growth vitamin
Pingback: situs judi slot online
Pingback: faster hair growth
Pingback: computer services corp
Pingback: faster hair growth
Pingback: web development on windows 7
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: unsuccessful network installation hp 8610
Pingback: 530 solar solutions
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: austin computer services 100 congress ave
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: kenny p computer services
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: computer services charlottesville va
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: air conditioning and heating Payson Az
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: trockener alkoholiker
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: air conditioners Payson AZ
Pingback: hair growth supplement
Pingback: air conditioning and heating Payson Az
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: alkoholiker
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: reviews
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: news
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: games
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: news
Pingback: reviews
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: decal
Pingback: faster hair growth
Pingback: decals
Pingback: wall decor
Pingback: home decor ideas
Pingback: faster hair growth
Pingback: wall murals
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: decals
Pingback: wall stencils
Pingback: hair growth vitamin
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: Ninja
Pingback: hair growth vitamin
Pingback: kitchen decor
Pingback: home decor
Pingback: decals
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: home decor ideas
Pingback: faster hair growth
Pingback: wall decoration
Pingback: hair growth supplement
Pingback: decals
Pingback: wall decor
Pingback: wall decoration
Pingback: wall decor
Pingback: hair growth supplement
Pingback: wall decor
Pingback: home decor ideas
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: hair growth supplement
Pingback: home decor ideas
Pingback: wall decor
Pingback: faster hair growth
Pingback: wall stickers
Pingback: wall decoration
Pingback: faster hair growth
Pingback: decal
Pingback: home decor ideas
Pingback: wall stickers
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: custom wall stickers
Pingback: hair growth supplement
Pingback: wall stickers
Pingback: faster hair growth
Pingback: wall stencils
Pingback: home decor
Pingback: wall decoration
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: wall stickers
Pingback: wall murals
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: decals
Pingback: faster hair growth
Pingback: wall stickers
Pingback: hair growth vitamin
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: wall murals
Pingback: hair growth supplement
Pingback: home decor
Pingback: decal
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: custom wall stickers
Pingback: faster hair growth
Pingback: decal
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: home decor
Pingback: hair growth supplement
Pingback: wall decor
Pingback: hair growth vitamin
Pingback: decal
Pingback: hair growth supplement
Pingback: home decor ideas
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: wall decor
Pingback: hair growth supplement
Pingback: wall stencils
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: wall decoration
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: kitchen decor
Pingback: hair growth supplement
Pingback: home decor ideas
Pingback: kitchen decor
Pingback: wall decor
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: custom wall stickers
Pingback: faster hair growth
Pingback: home decor
Pingback: faster hair growth
Pingback: wall decor
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: kitchen decor
Pingback: faster hair growth
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: wall stickers
Pingback: hair growth supplement
Pingback: wall decor
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: decals
Pingback: decals
Pingback: faster hair growth
Pingback: custom wall stickers
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: decal
Pingback: hair growth vitamin
Pingback: wall stickers
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: wall stickers
Pingback: hair growth vitamin
Pingback: wall decoration
Pingback: hair growth supplement
Pingback: wall decoration
Pingback: wall decoration
Pingback: faster hair growth
Pingback: Thanh toan GemRiverside
Pingback: faster hair growth
Pingback: decals
Pingback: faster hair growth
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: wall stickers
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: Twitter Video Downloader
Pingback: custom wall stickers
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: faster hair growth
Pingback: wall stencils
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth supplement
Pingback: wall decor
Pingback: hair growth supplement
Pingback: kitchen decor
Pingback: decal
Pingback: faster hair growth
Pingback: custom wall stickers
Pingback: home decor ideas
Pingback: hair growth vitamin
Pingback: wall stickers
Pingback: kitchen decor
Pingback: home decor
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: faster hair growth
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: hair growth supplement
Pingback: hair growth vitamin
Pingback: kitchen decor
Pingback: faster hair growth
Pingback: Youtube Video Downloader
Pingback: wall decor
Pingback: kitchen decor
Pingback: home decor ideas
Pingback: home decor ideas
Pingback: home decor
Pingback: wall decor
Pingback: wall stencils
Pingback: decal
Pingback: wall decor
Pingback: home decor ideas
Pingback: wall decor
Pingback: custom wall stickers
Pingback: kitchen decor
Pingback: decal
Pingback: decals
Pingback: home decor
Pingback: home decor
Pingback: wall murals
Pingback: wall stencils
Pingback: decals
Pingback: kitchen decor
Pingback: wall decor
Pingback: wall decor
Pingback: wall stickers
Pingback: decals
Pingback: wall decoration
Pingback: wall murals
Pingback: wall stencils
Pingback: home decor ideas
Pingback: wall stencils
Pingback: decal
Pingback: custom wall stickers
Pingback: decal
Pingback: home decor
Pingback: custom wall stickers
Pingback: wall decoration
Pingback: wall murals
Pingback: wall stickers
Pingback: wall decoration
Pingback: wall decoration
Pingback: decals
Pingback: wall stickers
Pingback: home decor
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: decals
Pingback: decals
Pingback: home decor ideas
Pingback: wall decor
Pingback: decals
Pingback: wall decor
Pingback: home decor ideas
Pingback: home decor
Pingback: home decor ideas
Pingback: wall stencils
Pingback: kitchen decor
Pingback: home decor ideas
Pingback: wall murals
Pingback: wall stickers
Pingback: wall stickers
Pingback: home decor
Pingback: Fitness Supplements Online
Pingback: custom wall stickers
Pingback: UK Supplements Online
Pingback: wall stencils
Pingback: Supplement Shop
Pingback: wall murals
Pingback: Fitness Supplement Shop
Pingback: wall decor
Pingback: decals
Pingback: wall decoration
Pingback: decals
Pingback: decals
Pingback: home decor
Pingback: wall decoration
Pingback: wall stencils
Pingback: decals
Pingback: Supplements Online
Pingback: wall decor
Pingback: wall murals
Pingback: Bodybuilding Supplements
Pingback: decal
Pingback: wall decor
Pingback: wall stickers
Pingback: UK Supplements
Pingback: Bodybuilding Supplements
Pingback: Nobel price
Pingback: home decor
Pingback: wall murals
Pingback: decals
Pingback: decal
Pingback: wall murals
Pingback: Redruth Supplement Shop
Pingback: wall decoration
Pingback: Supplement Shop
Pingback: wall decor
Pingback: wall stencils
Pingback: wall murals
Pingback: custom wall stickers
Pingback: decal
Pingback: Gym Power Supplement Shop
Pingback: Gym Power
Pingback: home decor ideas
Pingback: decals
Pingback: wall decor
Pingback: Cornwall Protein Shop
Pingback: Bodybuilding Supplements Online
Pingback: wall stickers
Pingback: UK Supplements Online
Pingback: home decor ideas
Pingback: Gym Power
Pingback: custom wall stickers
Pingback: wall stencils
Pingback: Fitness Supplement Shop
Pingback: wall murals
Pingback: decal
Pingback: custom wall stickers
Pingback: kitchen decor
Pingback: wall decoration
Pingback: wall stickers
Pingback: home decor ideas
Pingback: wall decor
Pingback: decal
Pingback: home decor
Pingback: kitchen decor
Pingback: Sustainable decision making
Pingback: UK Supplements Online
Pingback: custom wall stickers
Pingback: Consumption habits
Pingback: Behavioral design classes
Pingback: wall stickers
Pingback: custom wall stickers
Pingback: wall stencils
Pingback: decal
Pingback: Gym Power UK
Pingback: decals
Pingback: wall decor
Pingback: decal
Pingback: Fitness Supplements Online
Pingback: wall stencils
Pingback: Gym Power Supplement Shop
Pingback: wall decoration
Pingback: wall decoration
Pingback: wall stencils
Pingback: home decor
Pingback: decals
Pingback: wall decoration
Pingback: wall decor
Pingback: decals
Pingback: wall stencils
Pingback: wall stencils
Pingback: wall decor
Pingback: decals
Pingback: Nudging Tokyo
Pingback: home decor
Pingback: wall decoration
Pingback: Cornwall Protein Shop
Pingback: decal
Pingback: wall stencils
Pingback: Redruth Protein Shop
Pingback: wall stencils
Pingback: wall decoration
Pingback: kitchen decor
Pingback: wall decoration
Pingback: wall decoration
Pingback: wall stickers
Pingback: home decor ideas
Pingback: wall decor
Pingback: UK Supplements Online
Pingback: wall stickers
Pingback: UK Supplements Online
Pingback: wall decoration
Pingback: wall stencils
Pingback: bse market
Pingback: Supplement Shop
Pingback: wall stickers
Pingback: home decor ideas
Pingback: wall decoration
Pingback: Behavior design Mumbai
Pingback: wall stickers
Pingback: wall decor
Pingback: share market today
Pingback: home decor
Pingback: Choice architecture Mumbai
Pingback: home decor ideas
Pingback: Supplements Online
Pingback: Nudging Europe
Pingback: Gym Power UK
Pingback: Gym Power Supplement Shop
Pingback: bse share price
Pingback: Redruth Fitness Supplement Shop
Pingback: Fitness Supplements Online
Pingback: Sharing beauty with all
Pingback: consumer decision making
Pingback: Gym Power Redruth
Pingback: Gym Power UK
Pingback: Gym Power Redruth
Pingback: Communication design
Pingback: Gym Power Protein Shop
Pingback: bse market
Pingback: traveling behavior
Pingback: UK Supplements Shop
Pingback: Visit This Link
Pingback: behavioral design experts
Pingback: Redruth Supplement Shop
Pingback: Our site
Pingback: Nudging Seto
Pingback: Bonuses
Pingback: Full Article
Pingback: Nudging Spain
Pingback: Behavior design London
Pingback: Nudge unit
Pingback: Nudge seattle
Pingback: Full Report
Pingback: Sustainable behavior
Pingback: Nudge udvikling
Pingback: Nudge agency
Pingback: click here
Pingback: OECD
Pingback: Behavior design South Africa
Pingback: Web Site
Pingback: Forbrugeradfærd
Pingback: Work behavior
Pingback: Fitness Supplement Shop
Pingback: Homepage
Pingback: This Site
Pingback: Learn More Here
Pingback: Nudging team
Pingback: this review
Pingback: Get More Info
Pingback: eating behavior
Pingback: Click Here
Pingback: Click This Link
Pingback: this site
Pingback: Fitness Supplements Online
Pingback: Redruth Fitness Supplement Shop
Pingback: Cornwall Protein Shop
Pingback: Redruth Fitness Supplement Shop
Pingback: article source
Pingback: Extra resources
Pingback: Fitness Supplement Shop
Pingback: best6x9speakersforbass.simplesite.com
Pingback: Bodybuilding Supplements
Pingback: Look At This
Pingback: Web Site
Pingback: Clicking Here
Pingback: see more
Pingback: Redruth Supplement Shop
Pingback: Read Full Report
Pingback: found this site
Pingback: Learn More
Pingback: Continue
Pingback: Check This Out
Pingback: Read More
Pingback: Bodybuilding Supplements
Pingback: Source
Pingback: Discover More
Pingback: Gym Power Protein Shop
Pingback: Discover More
Pingback: More Bonuses
Pingback: Our site
Pingback: Recommended Reading
Pingback: More Bonuses
Pingback: Learn More
Pingback: our website
Pingback: Clicking Here
Pingback: Click Here
Pingback: additional reading
Pingback: site
Pingback: Gym Power Redruth
Pingback: Read Full Article
Pingback: Get More Information
Pingback: pendik escort
Pingback: Click Here
Pingback: Redruth Fitness Supplement Shop
Pingback: Click This Link
Pingback: Redruth Supplement Shop
Pingback: luxury
Pingback: Gym Power Redruth
Pingback: Slim Couture
Pingback: Get More Information
Pingback: Bodybuilding Supplements
Pingback: our website
Pingback: Cornwall Fitness Supplement Shop
Pingback: Redruth Fitness Supplement Shop
Pingback: Public transportation and behavior
Pingback: Gym Power Redruth
Pingback: UK Supplements Online
Pingback: Fitness Supplement Shop
Pingback: UK Supplements Online
Pingback: UK Supplements Shop
Pingback: Bodybuilding Supplements
Pingback: Gym Power Supplement Shop
Pingback: Bodybuilding Supplements Shop
Pingback: Gym Power UK
Pingback: UK Supplements Shop
Pingback: Cornwall Supplement Shop
Pingback: Supplement Shop
Pingback: UK Supplements Shop
Pingback: Redruth Supplement Shop
Pingback: Redruth Protein Shop
Pingback: UK Supplements Shop
Pingback: Redruth Protein Shop
Pingback: UK Supplements Online
Pingback: Gym Power Protein Shop
Pingback: Supplement Shop
Pingback: Supplements Online
Pingback: Gym Power
Pingback: Cornwall Fitness Supplement Shop
Pingback: Click Here
Pingback: Slim Couture
Pingback: Gym Power UK
Pingback: UK Supplements Shop
Pingback: Bodybuilding Supplements Shop
Pingback: Supplement Shop
Pingback: Supplements Online
Pingback: Gym Power UK
Pingback: Home Page
Pingback: Discover More Here
Pingback: Full Article
Pingback: Find Out More
Pingback: Look At This
Pingback: Read This
Pingback: Homepage
Pingback: Click Here
Pingback: Going Here
Pingback: Discover More
Pingback: Click Here
Pingback: Click Here
Pingback: This Site
Pingback: This Site
Pingback: Read This
Pingback: Visit This Link
Pingback: Full Report
Pingback: Full Article
Pingback: Sruthi Pathak Escorts in Bangalore
Pingback: Find Out More
Pingback: Going Here
Pingback: Read This
Pingback: Slim Couture
Pingback: Read Full Article
Pingback: This Site
Pingback: Learn More Here
Pingback: Website
Pingback: Visit Website
Pingback: Going Here
Pingback: Read Full Article
Pingback: Web Site
Pingback: Look At This
Pingback: Clicking Here
Pingback: Web Site
Pingback: Recommended Reading
Pingback: Ambika Ahuja Jaipur Escorts Services
Pingback: Rent a Van
Pingback: Transfer Aeroport Otopeni
Pingback: Transfer Aeroport Otopeni
Pingback: Rent a Van
Pingback: Rent a Car Otopeni
Pingback: Read This
Pingback: computer run faster
Pingback: Roku.com/link
Pingback: Luxury Car Rental
Pingback: Inchirieri masini
Pingback: Masini cu sofer
Pingback: Fizyka
Pingback: web page
Pingback: Świetnyzestawienie szamb z betonu
Pingback: Postawic
Pingback: Zestawienie szamb z betonu
Pingback: Rent a Mercedes
Pingback: Najistotniejsza agencja od szamb zbiorników Obejżyj
Pingback: pozycjonowanie za granicą
Pingback: Wódka
Pingback: edgeworth a place that buys junk cars close by
Pingback: towing company
Pingback: Rent a Mercedes
Pingback: where to take junk cars for money in crescent township pa
Pingback: places to junk cars for money near south heights pa
Pingback: where to junk my car near me close by coraopolis pa
Pingback: coraopolis auto junk dealers nearby
Pingback: sale my car fast crescent township pa
Pingback: Warmwasser mit solarthermie
Pingback: prediksi pertandingan bola malam ini
Pingback: south hts auto junk dealers nearby
Pingback: Nigeria entertainment
Pingback: where to sale junk cars moon pa
Pingback: Cash for Junk Cars Caropolis serving Crescent Township
Pingback: auto salvage around south heights
Pingback: coraopolis a place that buys junk cars around
Pingback: sell broken car for cash close by coraopolis pa
Pingback: auto recyclers near moon
Pingback: chain clevis
Pingback: auto junk yard in moon
Pingback: Cash for Junk Cars Caropolis in Hayesville
Pingback: auto junk dealers nearby glen osborne
Pingback: we pay for junk cars around emsworth pa
Pingback: who buys junk cars in my area in ben avon heights pa
Pingback: auto junkers close by moon
Pingback: Shoes(Mens)
Pingback: SHOULDER BAGS
Pingback: scrap car removal for cash nearby coraopolis pa
Pingback: LAPTOP BAGS
Pingback: Watches
Pingback: get rid of my junk car near glen osborne pa
Pingback: Shoes(Mens)
Pingback: emsworth auto junk dealers close by
Pingback: a place that buys junk cars nearby sewickley
Pingback: Watches
Pingback: Watches
Pingback: Unisex Bags
Pingback: sewickley auto junk yard around
Pingback: we buy scrap cars near me around crescent twp pa
Pingback: ben avon a place that buys junk cars in
Pingback: Sunglasses
Pingback: Watches
Pingback: Belts & Wallets
Pingback: duct insulation
Pingback: energy saving dryer vent
Pingback: best dryer vent
Pingback: cleaning the dryer vent
Pingback: SLING BAGS
Pingback: dryer vent lint trap
Pingback: Belts & Wallets
Pingback: flat dryer vent
Pingback: dryer systems
Pingback: vodafone network issues
Pingback: three mobile coverage
Pingback: dryer vent caps
Pingback: how to clean out dryer
Pingback: Belts & Wallets
Pingback: three mobile coverage
Pingback: O2 coverage checker
Pingback: Watches
Pingback: clothes dryer venting options
Pingback: Shirts
Pingback: Vodafone mobile coverage
Pingback: dryer booster fan
Pingback: Get More Information
Pingback: Orlando West Dryer Vents
Pingback: vent for dryer
Pingback: ee network issues
Pingback: SIZE 6
Pingback: SIZE 6
Pingback: Shoes(Mens)
Pingback: rigid dryer vent
Pingback: SIZE 8
Pingback: gutter vent
Pingback: duct supplies
Pingback: air conditioning offers
Pingback: indoor clothes dryer vent
Pingback: clean dryer vent pipe
Pingback: Keep dryer from catching fire
Pingback: O2 network problems
Pingback: blow dryer brush
Pingback: outside dryer vent
Pingback: dryer lint remover
Pingback: deflecto dryer vent
Pingback: Going Here
Pingback: vent systems
Pingback: air conditioner technician
Pingback: Aura Scanning
Pingback: dryer booster fan
Pingback: as air conditioning
Pingback: dryer lint cleaner
Pingback: dryer roof vents
Pingback: Avoid a dryer fire
Pingback: outdoor dryer vent cover
Pingback: exterior dryer vent covers
Pingback: Reiki Emergency Healing
Pingback: hvac in
Pingback: Discover More Here
Pingback: furnace duct cleaning service
Pingback: dryer vent installation
Pingback: Samridhi Shaktipat
Pingback: dryer hose vent
Pingback: periscope dryer vents
Pingback: Reiki Distance Healing
Pingback: metal dryer duct
Pingback: Aura Scanning
Pingback: Reiki Emergency Healing
Pingback: dryer lint
Pingback: custom embroidery Houston
Pingback: Crystal Charging
Pingback: ventilation ducting
Pingback: air vent for dryer
Pingback: furnace duct cleaning
Pingback: Oviedo dryer vents
Pingback: gas dryer venting
Pingback: Aura Cleansing
Pingback: air duct cleaning
Pingback: metal ductwork
Pingback: low profile dryer duct
Pingback: Clothes dryer maintenance
Pingback: how to clean dryer vent
Pingback: vent home
Pingback: dryer vents cleaning
Pingback: slim dryer vent
Pingback: Dryer performance problems
Pingback: dryer vent hood
Pingback: o2 balance check number
Pingback: lebara balance check uk
Pingback: dryer hose vent
Pingback: clothes dryer vent cleaner
Pingback: three balance check
Pingback: tesco mobile check balance
Pingback: how do you clean out a dryer vent
Pingback: Aura Cleansing
Pingback: asda mobile check balance
Pingback: kitchen scissors
Pingback: dryer exhaust vent
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: indoor clothes dryer vent
Pingback: dryer vent lint catcher
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: ibadah haji dan umrah
Pingback: heavy duty scissors
Pingback: ee check balance call
Pingback: talk mobile balance check number
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: custom sports uniform Houston
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: umroh bintang 5
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: how to check virgin balance
Pingback: idea loan number
Pingback: truecaller online search
Pingback: lycamobile balance check uk
Pingback: truecaller number search online
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: prediksi bola info
Pingback: prediksi bola nanti malam
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: vodafone uk balance check
Pingback: heavy duty scissors
Pingback: sandalwood
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: lemon
Pingback: giffgaff balance check by text
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: prediksi bola nanti malam
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: massage oil
Pingback: kitchen scissors
Pingback: perfume
Pingback: heavy duty scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: heavy duty scissors
Pingback: kitchen scissors
Pingback: kitchen scissors
Pingback: odour
Pingback: wall decor
Pingback: decal
Pingback: custom wall stickers
Pingback: kids all decor
Pingback: bsnl loan
Pingback: wall decor
Pingback: wall decor
Pingback: uninor loan code
Pingback: aircel emergency loan code
Pingback: vodafone loan
Pingback: jio loan
Pingback: wallpaper decals
Pingback: wall decor
Pingback: custom wall stickers
Pingback: decal
Pingback: airtel loan number
Pingback: wall decor
Pingback: removable wall murals
Pingback: FOOD PHOTOGRAPHY
Pingback: decal
Pingback: removable wall murals
Pingback: wall decor
Pingback: home decor
Pingback: custom wall stickers
Pingback: decal
Pingback: tata docomo loan code
Pingback: home decor
Pingback: home decor
Pingback: custom wall stickers
Pingback: игровые автоматы
Pingback: removable wall murals
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: decal
Pingback: wall decor
Pingback: Ab
Pingback: home decor
Pingback: decal
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: wall decor
Pingback: wall decor
Pingback: kids all decor
Pingback: RESTAURANT PHOTOGRAPHY
Pingback: fund
Pingback: decal
Pingback: wallpaper decals
Pingback: home decor
Pingback: kids all decor
Pingback: removable wall murals
Pingback: SMS gateway provider
Pingback: linktelmedia
Pingback: Bulk SMS service provider in India
Pingback: removable wall murals
Pingback: linktelmedia
Pingback: linktel media
Pingback: home decor
Pingback: wallpaper decals
Pingback: bulk sms noida
Pingback: removable wall murals
Pingback: decal
Pingback: Crowns / Bridge
Pingback: home decor
Pingback: api for bulk sms
Pingback: decal
Pingback: wall decor
Pingback: custom wall stickers
Pingback: home decor
Pingback: decal
Pingback: RENT LUXURY CARS in Switzerland
Pingback: wallpaper decals
Pingback: home decor
Pingback: wall decor
Pingback: RENT LUXURY CARS in Switzerland
Pingback: removable wall murals
Pingback: Gum left / Gum Re-contouring
Pingback: decal
Pingback: wallpaper decals
Pingback: wallpaper decals
Pingback: kids all decor
Pingback: removable wall murals
Pingback: home decor
Pingback: decal
Pingback: custom wall stickers
Pingback: wallpaper decals
Pingback: Teeth whitening /bleaching
Pingback: removable wall murals
Pingback: removable wall murals
Pingback: Orthodontics
Pingback: CHAUFFEURED SERVICES Zurich
Pingback: Limousine Service Switzerland
Pingback: CHAUFFEURED SERVICES Zurich
Pingback: "Paket Biaya Harga Umrah Murah Arbain YouTube
Pingback: wall decor
Pingback: wall decor
Pingback: Anklets
Pingback: wall decor
Pingback: wallpaper decals
Pingback: wall decor
Pingback: wallpaper decals
Pingback: wall decor
Pingback: wall decor
Pingback: wallpaper decals
Pingback: decal
Pingback: home decor
Pingback: cancer support
Pingback: removable wall murals
Pingback: Chokers
Pingback: removable wall murals
Pingback: decal
Pingback: custom wall stickers
Pingback: removable wall murals
Pingback: CAGED System
Pingback: removable wall murals
Pingback: home decor
Pingback: decal
Pingback: removable wall murals
Pingback: Statement Necklaces
Pingback: Chokers
Pingback: wallpaper decals
Pingback: home decor
Pingback: kids all decor
Pingback: kids all decor
Pingback: Statement Necklaces
Pingback: home decor
Pingback: wall decor
Pingback: removable wall murals
Pingback: kids all decor
Pingback: custom wall stickers
Pingback: decal
Pingback: wallpaper decals
Pingback: kids all decor
Pingback: Breast Cancer Survival Rate
Pingback: Breast Cancer Definition
Pingback: Lungs cancer Definition
Pingback: Breast Cancer Screening
Pingback: wall decor
Pingback: removable wall murals
Pingback: resume services in uganda
Pingback: Lung Cancer Earliest Symptoms
Pingback: Lung Cancer Screening
Pingback: cv services in kenya
Pingback: custom wall stickers
Pingback: Lung Nodules
Pingback: resume services in uganda
Pingback: resume writers in nairobi
Pingback: home decor
Pingback: prediksi kedai bola
Pingback: Going Here
Pingback: Homepage
Pingback: More about the author
Pingback: Continued
Pingback: Going Here
Pingback: more helpful hints
Pingback: link
Pingback: kids all decor
Pingback: removable wall murals
Pingback: Visit This Link
Pingback: helpful resources
Pingback: Read More Here
Pingback: Resources
Pingback: Continued
Pingback: Check Out Your URL
Pingback: More about the author
Pingback: Web Site
Pingback: Check Out Your URL
Pingback: helpful hints
Pingback: More Help
Pingback: Click This Link
Pingback: Find Out More
Pingback: home decor
Pingback: wall decor
Pingback: Web Site
Pingback: Going Here
Pingback: home decor
Pingback: More hints
Pingback: Learn More
Pingback: removable wall murals
Pingback: our website
Pingback: Discover More
Pingback: Bonuses
Pingback: Triple Negative Breast Cancer
Pingback: What You Should Know About Breast Cancer
Pingback: Learn More Here
Pingback: Go Here
Pingback: home decor
Pingback: The Things You Need To Know About Stage 4 Lung Cancer
Pingback: What you should know about Melanoma?
Pingback: Discover More Here
Pingback: Mesothelioma Information
Pingback: Read More Here
Pingback: Continue Reading
Pingback: more helpful hints
Pingback: Find Out More
Pingback: Breast Cancer Surgery
Pingback: Extra resources
Pingback: decal
Pingback: decal
Pingback: Web Site
Pingback: custom wall stickers
Pingback: wall decor
Pingback: custom wall stickers
Pingback: Read More
Pingback: additional reading
Pingback: Student fashion
Pingback: Visit Website
Pingback: Continued
Pingback: Your Domain Name
Pingback: Bonuses
Pingback: Click Here
Pingback: More Bonuses
Pingback: Check Out Your URL
Pingback: Read This
Pingback: Visit Website
Pingback: kids all decor
Pingback: custom wall stickers
Pingback: Click This Link
Pingback: Website
Pingback: helpful resources
Pingback: helpful resources
Pingback: Continue Reading
Pingback: Website
Pingback: Squamous Cell Carcinoma
Pingback: Website
Pingback: Read More
Pingback: Clicking Here
Pingback: Find Out More
Pingback: our website
Pingback: Understanding Inflammatory Breast Cancer
Pingback: Website
Pingback: More about the author
Pingback: Rock Sauxy7even Crop Tee
Pingback: Extra resources
Pingback: Rock Sauxy7even Crop Tee
Pingback: What to do when diagnosed with mesothelioma
Pingback: New Horizons in Mesothelioma Treatment/Cure
Pingback: Entertainment
Pingback: Mesothelioma info: Treatments
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: How to Avoid Mesothelioma ?
Pingback: Mesothelioma: New Treatments Research
Pingback: Mesothelioma: Treatment Side Effects
Pingback: Cancer Immunotherapy
Pingback: Rock Sauxy7even Crop Tee
Pingback: Surgery in Mesothelioma
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: Rock Sauxy7even Crop Tee
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: Rock Sauxy7even Crop Tee
Pingback: Is Mesothelioma Curable ?
Pingback: Rock Sauxy7even Crop Tee
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: R.VONNI PREMIUM SHIRT MEN'S
Pingback: link
Pingback: Umroh semarang
Pingback: Discover More Here
Pingback: More Bonuses
Pingback: Source
Pingback: situs prediksi bola paling akurat
Pingback: Resources
Pingback: Custom wristbands
Pingback: Dallas Mesothelioma Attorneys
Pingback: Mesothelioma Symptoms
Pingback: Mesothelioma: Risk Factors
Pingback: Top US Mesothelioma Lawyers & Attorneys
Pingback: Cause
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: Boston Mesothelioma Lawyers
Pingback: R,VONNI GIRL SHORTS
Pingback: Best New York Mesothelioma Attorney
Pingback: R,VONNI GIRL SHORTS
Pingback: R.VONNI GIRL CAPRI LEGGINGS
Pingback: lie detector
Pingback: R.VONNI GIRL CAPRI LEGGINGS
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: R,VONNI GIRL SHORTS
Pingback: JWhiting999.blogspot.com
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: Visit Website
Pingback: Read More
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: Web Site
Pingback: Visit This Link
Pingback: Find Out More
Pingback: Homepage
Pingback: R.VONNI GIRL CAPRI LEGGINGS
Pingback: R.VONNI GIRL CAPRI LEGGINGS
Pingback: Top US Mesothelioma Lawyers & Attorneys
Pingback: lie detector test
Pingback: lie detector maidstone
Pingback: Find Out More
Pingback: R,VONNI GIRL SHORTS
Pingback: lie detectors uk
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: R,VONNI GIRL SHORTS
Pingback: Clicking Here
Pingback: steam iron for clothes
Pingback: R,VONNI GIRL SHORTS
Pingback: steam iron
Pingback: Read More
Pingback: Go Here
Pingback: Find Out More
Pingback: Get More Info
Pingback: R,VONNI GIRL SHORTS
Pingback: Learn More Here
Pingback: Learn More Here
Pingback: Web Site
Pingback: Click Here
Pingback: Learn More Here
Pingback: clothes steamer handheld
Pingback: THICK AND THIN SHIRT WOMEN
Pingback: travel iron
Pingback: ancer support resources
Pingback: Mesothelioma Settlements
Pingback: toilet seat covers california
Pingback: breast cancer
Pingback: baby registry must haves
Pingback: How to pass math final exam
Pingback: steam iron for clothes
Pingback: baby diaper caddy
Pingback: Costco cash cards online
Pingback: mesothelioma treatment
Pingback: get free amazon gift cards online
Pingback: Earn gift certificates online
Pingback: gift registry baby shower
Pingback: Mesothelioma Information: Organizations Offering Support For Patients
Pingback: baby diaper caddy organizer
Pingback: costco cash cards for sale
Pingback: gift registry baby shower
Pingback: baby diaper caddy
Pingback: diaper organizer
Pingback: baby shower registry
Pingback: baby diaper caddy
Pingback: baby diaper caddy
Pingback: changing table organizer
Pingback: Instant gift cards india
Pingback: resume writers in uganda
Pingback: Toilet bidet combo uk
Pingback: gift registry
Pingback: CV Writers in Nairobi
Pingback: diaper caddy
Pingback: CV services in nairobi
Pingback: changing table organizer
Pingback: prediksi bola info
Pingback: Mesothelioma Claims: Reasons Patients May Get Compensated
Pingback: Five Important Facts About Mesothelioma Claims
Pingback: cv services in kenya
Pingback: baby basket
Pingback: baby diaper caddy
Pingback: gift registry baby shower
Pingback: diaper caddy
Pingback: gift registry baby shower
Pingback: wrinkle release spray
Pingback: hand steamer
Pingback: baby registry must haves
Pingback: diaper caddy
Pingback: baby organizer
Pingback: prediksi sepak bola malam
Pingback: judi domino qq
Pingback: baby diaper caddy
Pingback: prediksi bola akurat
Pingback: storage caddy
Pingback: baby registry must haves
Pingback: dietas
Pingback: baby organizer
Pingback: Sanremo locali musica live
Pingback: gift registry baby shower
Pingback: nursery organizer
Pingback: baby shower registry
Pingback: steamer for clothes
Pingback: alimentação natural
Pingback: baby shower registry
Pingback: baby shower registry
Pingback: nursery organizer
Pingback: baby diaper caddy
Pingback: baby diaper caddy organizer
Pingback: baby registry must haves
Pingback: diaper caddy organizer
Pingback: baby diaper caddy organizer
Pingback: steamer for clothes
Pingback: diaper organizer
Pingback: baby shower registry
Pingback: diaper organizer
Pingback: situs prediksi bola terlengkap
Pingback: diaper caddy organizer
Pingback: travel iron
Pingback: baby basket
Pingback: alimentação natural
Pingback: Sanremo Wine Bar
Pingback: how to get better at math and science
Pingback: baby registry must haves
Pingback: diaper caddy
Pingback: baby storage organizer
Pingback: diaper organizer
Pingback: how to get better at english language arts
Pingback: clothing steamer
Pingback: Telegraph rewards app for android
Pingback: gift registry baby shower
Pingback: steam iron
Pingback: Get instant amazon gift cards
Pingback: Coke rewards app for android
Pingback: baby diaper caddy organizer
Pingback: gift registry baby shower
Pingback: storage caddy
Pingback: diaper caddy
Pingback: Sanremo locali musica live
Pingback: baby diaper caddy organizer
Pingback: storage caddy
Pingback: baby registry must haves
Pingback: changing table organizer
Pingback: storage caddy
Pingback: get instant amazon gift cards
Pingback: diaper caddy
Pingback: travel iron
Pingback: Biaya Umroh Murah Berangkat Dari Bandung – satuTours.co.id
Pingback: steam iron
Pingback: reverse phone lookup indiana
Pingback: gift registry baby shower
Pingback: baby diaper caddy
Pingback: nursery organizer
Pingback: storage caddy
Pingback: Online casino free roulette spins
Pingback: gift registry
Pingback: nursery organizer
Pingback: gift registry
Pingback: travel steamer
Pingback: Travel umroh terbesar di indonesia
Pingback: Tavernacolo Sanremo
Pingback: baby diaper caddy
Pingback: gift registry
Pingback: travel steamer for clothes
Pingback: baby shower registry
Pingback: portable steamer
Pingback: gift registry baby shower
Pingback: Cbd wholesale
Pingback: steam iron for clothes
Pingback: clothes steamer handheld
Pingback: gift registry
Pingback: portable steamer
Pingback: diaper organizer
Pingback: baby registry must haves
Pingback: handheld steamer
Pingback: nursery organizer
Pingback: Cbd manufacturing
Pingback: baby basket
Pingback: steam iron
Pingback: travel iron
Pingback: baby organizer
Pingback: baby registry must haves
Pingback: storage caddy
Pingback: diaper organizer
Pingback: changing table organizer
Pingback: paket umroh vip
Pingback: diaper caddy organizer
Pingback: baby organizer
Pingback: fabric steamer
Pingback: hand steamer
Pingback: clothes steamer handheld
Pingback: baby basket
Pingback: baby diaper caddy
Pingback: diaper organizer
Pingback: steamer for clothes
Pingback: Harmonic Scanner Strategy
Pingback: diaper organizer
Pingback: Free gift cards ps4 codes
Pingback: Umrah Murah Plus Promo 12 Hari Bintang 3 - Perjalanan
Pingback: situs agen yang terpercaya
Pingback: baby storage organizer
Pingback: gift registry baby shower
Pingback: agen judi casino online
Pingback: baby storage organizer
Pingback: travel iron
Pingback: clothing steamer
Pingback: jack and jill toothpaste
Pingback: vpn
Pingback: baby shower registry
Pingback: infant toothbrush
Pingback: vpn
Pingback: baby toothbrush 6 to 12 months
Pingback: free vpn
Pingback: vpn free
Pingback: hand steamer
Pingback: baby toothbrush
Pingback: vpn free
Pingback: vpn free
Pingback: free vpn
Pingback: changing table organizer
Pingback: baby banana toothbrush
Pingback: storage caddy
Pingback: baby toothbrush
Pingback: storage caddy
Pingback: gift registry
Pingback: "WA 081384597889 Umroh Murah Promo Umroh Murah Biaya Umroh Murah - YouTube
Pingback: toothbrushes kids
Pingback: storage caddy
Pingback: hand steamer
Pingback: handheld steamer
Pingback: baby registry must haves
Pingback: baby toothbrush 12 months and up
Pingback: baby organizer
Pingback: toothbrushes kids
Pingback: baby diaper caddy organizer
Pingback: diaper caddy
Pingback: baby banana toothbrush
Pingback: baby diaper caddy
Pingback: diaper caddy
Pingback: baby teeth
Pingback: baby storage organizer
Pingback: fabric steamer
Pingback: free vpn
Pingback: directtv deals
Pingback: free vpn
Pingback: Judi domino online indonesia
Pingback: baby toothbrush 12 months and up
Pingback: garment steamer
Pingback: garment steamer
Pingback: gift card
Pingback: free vpn
Pingback: travel steamer for clothes
Pingback: clothes steamer handheld
Pingback: steam iron for clothes
Pingback: vpn free
Pingback: toddler toothbrush
Pingback: baby banana toothbrush
Pingback: free vpn
Pingback: baby toothpaste
Pingback: finger toothbrush for baby
Pingback: portable steamer
Pingback: free vpn
Pingback: aerospace and defense sector stocks
Pingback: vpn free
Pingback: baby toothbrush 12 months and up
Pingback: disney rain poncho
Pingback: steam iron
Pingback: clothes steamer handheld
Pingback: clothes steamer
Pingback: infant toothbrush
Pingback: disney rain poncho
Pingback: ponchos
Pingback: kids ponchos
Pingback: rain poncho kids
Pingback: disney travel accessories
Pingback: kids ponchos for rain disney
Pingback: poncho
Pingback: disposable ponchos
Pingback: disposable rain poncho with hood
Pingback: ponchos
Pingback: disposable poncho
Pingback: adult rain poncho
Pingback: diaper caddy organizer
Pingback: Phrase
Pingback: travel poncho
Pingback: toddler poncho
Pingback: pancho
Pingback: rain poncho
Pingback: travel rain poncho
Pingback: plastic poncho
Pingback: disposable rain ponchos
Pingback: panchos rain kids
Pingback: reusable poncho
Pingback: panchos rain
Pingback: disposable ponchos
Pingback: baby shower registry
Pingback: plastic poncho
Pingback: reusable poncho
Pingback: disney poncho
Pingback: panchos rain
Pingback: rain ponchos
Pingback: poncho kids
Pingback: panchos
Pingback: rain pancho
Pingback: nursery organizer
Pingback: kids rain poncho with hood
Pingback: travel rain poncho
Pingback: emergency rain poncho
Pingback: rain poncho kids
Pingback: kids ponchos for rain
Pingback: baby organizer
Pingback: poncho plastic
Pingback: disposable rain ponchos
Pingback: toddler toothpaste
Pingback: baby toothbrush
Pingback: baby registry must haves
Pingback: baby toothbrush
Pingback: emergency poncho
Pingback: kids ponchos
Pingback: baby diaper caddy organizer
Pingback: rain ponchos for adults disposable
Pingback: gift registry
Pingback: rain poncho for kids
Pingback: theme park accessories
Pingback: baby toothbrush
Pingback: baby toothbrush 6 to 12 months
Pingback: banana teether
Pingback: disney travel accessories
Pingback: baby registry must haves
Pingback: poncho plastic
Pingback: panchos rain
Pingback: pancho
Pingback: finger toothbrush for baby
Pingback: emergency rain poncho
Pingback: emergency poncho
Pingback: baby toothbrush
Pingback: videochat per tutti
Pingback: baby basket
Pingback: baby basket
Pingback: kids rain poncho
Pingback: baby toothpaste
Pingback: diaper organizer
Pingback: baby organizer
Pingback: nursery organizer
Pingback: banana teether
Pingback: baby teeth
Pingback: baby toothbrush 6 to 12 months
Pingback: baby toothbrush 12 months and up
Pingback: ponchos family pack
Pingback: disposable poncho
Pingback: toddler toothpaste
Pingback: videochatta
Pingback: disney ponchos
Pingback: rain poncho kids
Pingback: kids rain ponchos
Pingback: jack and jill toothpaste
Pingback: youth rain gear
Pingback: kid poncho
Pingback: gift registry
Pingback: rain poncho
Pingback: toddler toothbrush
Pingback: youth rain gear
Pingback: kids ponchos
Pingback: infant toothbrush
Pingback: storage caddy
Pingback: rain ponchos for adults disposable
Pingback: baby toothbrush 12 months and up
Pingback: toddler toothpaste
Pingback: kids ponchos for rain
Pingback: baby teeth
Pingback: baby toothbrush 12 months and up
Pingback: gift registry baby shower
Pingback: infant toothbrush
Pingback: diaper caddy organizer
Pingback: baby banana toothbrush
Pingback: videochat gratis
Pingback: toddler toothbrush
Pingback: gift registry
Pingback: rain ponchos
Pingback: panchos rain
Pingback: Paket Umroh Murah 12 Hari Jadwal Kegiatan Umrah Murah 12 Hari Harga Paket Umroh Murah 12 Hari
Pingback: youth poncho
Pingback: toddler toothbrush
Pingback: baby teeth
Pingback: toothbrushes kids
Pingback: baby diaper caddy
Pingback: baby diaper caddy
Pingback: gift registry
Pingback: changing table organizer
Pingback: toddler toothpaste
Pingback: mens poncho
Pingback: jack and jill toothpaste
Pingback: reusable rain poncho
Pingback: reusable rain poncho
Pingback: kids rain poncho
Pingback: banana teether
Pingback: waterproof poncho
Pingback: poncho
Pingback: baby toothbrush
Pingback: gift registry
Pingback: poncho
Pingback: baby storage organizer
Pingback: rain gear
Pingback: baby basket
Pingback: baby toothbrush 12 months and up
Pingback: Promo umroh 2018
Pingback: nursery organizer
Pingback: waterproof poncho
Pingback: disposable rain ponchos
Pingback: Free Games
Pingback: baby toothbrush 12 months and up
Pingback: baby toothbrush 6 to 12 months
Pingback: baby toothbrush 6 to 12 months
Pingback: storage caddy
Pingback: nursery organizer
Pingback: nursery organizer
Pingback: banana teether
Pingback: baby basket
Pingback: baby diaper caddy
Pingback: toddler toothbrush
Pingback: baby toothpaste
Pingback: baby diaper caddy organizer
Pingback: finger toothbrush for baby
Pingback: diaper caddy organizer
Pingback: rain gear
Pingback: waterproof poncho
Pingback: baby diaper caddy organizer
Pingback: kids rain poncho
Pingback: gift registry baby shower
Pingback: toddler toothbrush
Pingback: poncho
Pingback: baby diaper caddy organizer
Pingback: diaper organizer
Pingback: travel iron
Pingback: raincoat
Pingback: clothes steamer
Pingback: toddler toothbrush
Pingback: hiking rain poncho
Pingback: baby toothbrush
Pingback: best poncho
Pingback: jack and jill toothpaste
Pingback: jack and jill toothpaste
Pingback: baby diaper caddy organizer
Pingback: mens poncho
Pingback: disposable rain ponchos
Pingback: raincoat
Pingback: hiking rain poncho
Pingback: best poncho
Pingback: baby toothbrush 6 to 12 months
Pingback: baby toothbrush
Pingback: rain gear
Pingback: 0818 0791 3639 (XL) Agen dan Umrah Murah di Jakarta Selatan - YouTube
Pingback: hiking rain poncho
Pingback: infant toothbrush
Pingback: 2-Way Radios & Accessories
Pingback: toothbrushes kids
Pingback: best poncho
Pingback: raincoat
Pingback: infant toothbrush
Pingback: mens poncho
Pingback: handheld steamer
Pingback: hiking rain poncho
Pingback: jack and jill toothpaste
Pingback: Cell Phones & Accessories
Pingback: poncho
Pingback: jack and jill toothpaste
Pingback: fabric steamer
Pingback: rain gear
Pingback: Computers & Accessories
Pingback: cách làm âm đao giả tại nhà
Pingback: Alarm Clocks
Pingback: MP3 & MP4 Players
Pingback: best poncho
Pingback: disposable rain ponchos
Pingback: waterproof poncho
Pingback: disposable rain ponchos
Pingback: baby toothbrush 12 months and up
Pingback: waterproof poncho
Pingback: hiking rain poncho
Pingback: golf rain suit
Pingback: raincoat
Pingback: infant toothbrush
Pingback: kids rain poncho
Pingback: travel steamer
Pingback: clothes steamer handheld
Pingback: golf rain suit
Pingback: waterproof poncho
Pingback: raincoat
Pingback: baby toothbrush
Pingback: banana teether
Pingback: hiking rain poncho
Pingback: baby teeth
Pingback: paket umroh jakarta 2018
Pingback: jack and jill toothpaste
Pingback: Telephones
Pingback: finger toothbrush for baby
Pingback: Radio Scanners
Pingback: banana teether
Pingback: infant toothbrush
Pingback: Umroh wajib adalah
Pingback: toothbrushes kids
Pingback: steam iron
Pingback: baby toothbrush 12 months and up
Pingback: fabric steamer
Pingback: toddler toothpaste
Pingback: baby toothpaste
Pingback: toddler toothbrush
Pingback: finger toothbrush for baby
Pingback: clothing steamer
Pingback: Highfields Sports Park
Pingback: Inpatient rehab centers
Pingback: hand steamer
Pingback: wrinkle release spray
Pingback: clothing steamer
Pingback: baby toothbrush 12 months and up
Pingback: access control allow origin chrome
Pingback: cystic blackhead extraction
Pingback: catch a cheater gps tracker
Pingback: clothes steamer handheld
Pingback: serwisk omputerowy
Pingback: BandarQ Online
Pingback: portable steamer
Pingback: travel iron
Pingback: clothing steamer
Pingback: hand steamer
Pingback: Rubber Bracelet
Pingback: kids rain poncho
Pingback: Microsoft online training Malaysia
Pingback: portable steamer
Pingback: raincoat
Pingback: poncho
Pingback: mens poncho
Pingback: best poncho
Pingback: toddler toothbrush
Pingback: rain poncho
Pingback: banana teether
Pingback: mens poncho
Pingback: hiking rain poncho
Pingback: poncho
Pingback: disposable rain ponchos
Pingback: poncho
Pingback: golf rain suit
Pingback: toothbrushes kids
Pingback: reusable rain poncho
Pingback: kids rain poncho
Pingback: rain poncho
Pingback: raincoat
Pingback: travel iron
Pingback: Haarverlängerung Ulm
Pingback: baby toothbrush
Pingback: sudesh.rocharam
Pingback: finger toothbrush for baby
Pingback: sudesh rocharam
Pingback: sudesh.rocharam
Pingback: sudesh.rocharam
Pingback: reusable rain poncho
Pingback: sudesh.rocharam
Pingback: baby toothbrush
Pingback: sudesh.rocharam
Pingback: rain poncho
Pingback: hiking rain poncho
Pingback: Astralreisen
Pingback: make wristbands usa
Pingback: golf rain suit
Pingback: hiking rain poncho
Pingback: best poncho
Pingback: golf rain suit
Pingback: poncho
Pingback: rain gear
Pingback: raincoat
Pingback: waterproof poncho
Pingback: baby toothbrush 12 months and up
Pingback: raincoat
Pingback: portable steamer
Pingback: hiking rain poncho
Pingback: golf rain suit
Pingback: finger toothbrush for baby
Pingback: Windelfrei
Pingback: Motor Club Company
Pingback: poncho
Pingback: reusable rain poncho
Pingback: rain gear
Pingback: disposable rain ponchos
Pingback: raincoat
Pingback: waterproof poncho
Pingback: best poncho
Pingback: rain gear
Pingback: mens poncho
Pingback: sudesh.rocharam
Pingback: sudesh rocharam
Pingback: sudesh.rocharam
Pingback: sudesh.rocharam
Pingback: oversized beach towel
Pingback: big beach towel
Pingback: beach towel
Pingback: pool towel
Pingback: sudesh.rocharam
Pingback: boys beach towel
Pingback: beach towel set
Pingback: sudesh.rocharam
Pingback: Estime de soi
Pingback: Formation confiance en soi
Pingback: sudesh.rocharam
Pingback: sand free beach towel
Pingback: sudesh.rocharam
Pingback: sudesh.rocharam
Pingback: Travailler la confiance en soi
Pingback: Paket Umrah Murah Akhir 2018 - Biaya Umroh Murah 18 Jt Promo Direct
Pingback: beach towel
Pingback: travel towel
Pingback: large towels
Pingback: boys beach towel
Pingback: sudesh.rocharam
Pingback: sand free beach towel
Pingback: oversized beach towel
Pingback: beach towels
Pingback: oversized beach towels
Pingback: beach towel set
Pingback: microfiber travel towel
Pingback: boys beach towel
Pingback: Confiance en soi
Pingback: beach towels for adults
Pingback: camping towel
Pingback: Formation confiance en soi
Pingback: kitchen decor
Pingback: toddler toothpaste
Pingback: camping towel
Pingback: big beach towel
Pingback: toddler toothpaste
Pingback: Web Design Mansfield
Pingback: wall decor
Pingback: jewelry software
Pingback: travel towel
Pingback: paket umroh tiket murah
Pingback: beach towel set
Pingback: beach towels oversized
Pingback: microfiber travel towel
Pingback: infant toothbrush
Pingback: wall decoration
Pingback: beach towels
Pingback: singing success mastering harmony download
Pingback: custom wall stickers
Pingback: beach towel set
Pingback: sand free beach towel
Pingback: large towels
Pingback: sand free beach blanket
Pingback: baby toothbrush
Pingback: large towels
Pingback: sand free beach blanket
Pingback: baby toothpaste
Pingback: backpacking towel
Pingback: large towels
Pingback: series online
Pingback: bath towels extra large
Pingback: beach accessories
Pingback: large beach towels
Pingback: beach towels for adults
Pingback: weight loss program
Pingback: baby teeth
Pingback: backpacking towel
Pingback: beach accessories for women
Pingback: backpacking towel
Pingback: bath towels extra large
Pingback: cv writing service
Pingback: beach towel
Pingback: boys beach towel
Pingback: Nexus androstenone pheromones
Pingback: large beach towel
Pingback: beach towel
Pingback: Silicone bracelets
Pingback: Paket umroh 6 orang
Pingback: beach towels oversized
Pingback: microfiber towel
Pingback: travel towels fast drying
Pingback: big beach towel
Pingback: beach towels for adults
Pingback: microfiber towel
Pingback: microfiber towel
Pingback: kitchen decor
Pingback: beach accessories for women
Pingback: extinguishing
Pingback: wall decoration
Pingback: microfiber beach towel
Pingback: wall stickers
Pingback: home decor ideas
Pingback: swim towel
Pingback: resume writer online
Pingback: resume writing services
Pingback: beach towels oversized
Pingback: sand free beach towel
Pingback: beach towel
Pingback: swim towel
Pingback: beach accessories for women
Pingback: pay your linux server with bitcoin
Pingback: Manasik haji dan umrah
Pingback: microfiber towel
Pingback: boys beach towel
Pingback: prediksi bola menang paling akurat
Pingback: sand free beach blanket
Pingback: beach towel set
Pingback: beach towel
Pingback: bath towels extra large
Pingback: Judi capsa online terpercaya
Pingback: backpacking towel
Pingback: travel towel
Pingback: cheap beach towels
Pingback: travel towel
Pingback: xl beach towel
Pingback: xl beach towel
Pingback: beach towel set
Pingback: boys beach towel
Pingback: sand free beach blanket
Pingback: beach towel oversized
Pingback: boys beach towel
Pingback: mouse click the up coming web site
Pingback: travel towel
Pingback: large beach towels
Pingback: extra large beach towels
Pingback: beach towel oversized
Pingback: Situs Domino99 online
Pingback: oversized beach towel
Pingback: big beach towel
Pingback: microfiber travel towel
Pingback: travel towels fast drying
Pingback: beach towel
Pingback: microfiber beach towel
Pingback: beach towel oversized
Pingback: extra large beach towels
Pingback: boys beach towel
Pingback: cheap beach towels
Pingback: sand free beach blanket
Pingback: oversized beach towel
Pingback: beach towel set
Pingback: beach towel set
Pingback: large beach towels
Pingback: microfiber beach towel
Pingback: pool towel
Pingback: oversized beach towel
Pingback: backpacking towel
Pingback: property buyers agent
Pingback: extra large beach towels
Pingback: property buyers agent
Pingback: large beach towel
Pingback: buyers agent
Pingback: property buyers agent
Pingback: smoothie straws
Pingback: real estate buyers agent
Pingback: property buyers agent
Pingback: real estate buyers agent
Pingback: property acquisition
Pingback: real estate buyers agent
Pingback: property buyers agent
Pingback: decals
Pingback: dublin buyers agent
Pingback: dublin buyers agent
Pingback: real estate buyers agent
Pingback: buyers agent
Pingback: dublin buyers agent
Pingback: wall decoration
Pingback: property buyers agent
Pingback: dublin buyers agent
Pingback: property buyers agent
Pingback: wall murals
Pingback: home decor
Pingback: buyers agent
Pingback: dublin buyers agent
Pingback: wall decoration
Pingback: guns
Pingback: property acquisition
Pingback: buyers agent
Pingback: property acquisition
Pingback: decal
Pingback: wall decoration
Pingback: custom wall stickers
Pingback: wall murals
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: wall decoration
Pingback: wall stencils
Pingback: custom wall stickers
Pingback: home decor
Pingback: home decor
Pingback: wall decor
Pingback: home decor
Pingback: wall murals
Pingback: home decor
Pingback: wall murals
Pingback: buyers agent
Pingback: wall murals
Pingback: custom wall stickers
Pingback: wall decor
Pingback: wall murals
Pingback: wall murals
Pingback: wall decor
Pingback: wall stencils
Pingback: Benjamin Mcnichols
Pingback: home decor
Pingback: wall decoration
Pingback: wall stencils
Pingback: home decor
Pingback: custom wall stickers
Pingback: Stephaine Chalfant
Pingback: Brigitte Opp
Pingback: Cristobal Sane
Pingback: wall decor
Pingback: custom wall stickers
Pingback: wall decor
Pingback: wall decor
Pingback: kitchen decor
Pingback: Beatriz Vandeusen
Pingback: wall decoration
Pingback: decals
Pingback: wall decor
Pingback: Codi Broaddus
Pingback: Darline Kunst
Pingback: Marlyn Deveaux
Pingback: kitchen decor
Pingback: custom wall stickers
Pingback: Email without Blacklist
Pingback: custom wall stickers
Pingback: Teodoro Marenco
Pingback: buyers agent
Pingback: home decor
Pingback: kitchen decor
Pingback: URL
Pingback: decals
Pingback: Janeth Zeman
Pingback: Mitch Comfort
Pingback: Buddy Kirst
Pingback: home decor ideas
Pingback: wall murals
Pingback: decals
Pingback: buyers agent
Pingback: wall stencils
Pingback: decal
Pingback: home decor
Pingback: home decor ideas
Pingback: wall murals
Pingback: wall murals
Pingback: kitchen decor
Pingback: wall decoration
Pingback: kitchen decor
Pingback: Teofila Yetman
Pingback: home decor ideas
Pingback: decal
Pingback: home decor ideas
Pingback: Leila Sandor
Pingback: wall murals
Pingback: Lawanda Billick
Pingback: wall decoration
Pingback: Youlanda Kahan
Pingback: decal
Pingback: decals
Pingback: wall decor
Pingback: decals
Pingback: home decor ideas
Pingback: kitchen decor
Pingback: wall murals
Pingback: wall murals
Pingback: home decor ideas
Pingback: home decor ideas
Pingback: wall stickers
Pingback: wall stickers
Pingback: decals
Pingback: wall stickers
Pingback: decals
Pingback: real estate buyers agent
Pingback: kitchen decor
Pingback: custom wall stickers
Pingback: kitchen scissors
Pingback: decal
Pingback: wall stencils
Pingback: Madlyn Spann
Pingback: wall decoration
Pingback: kitchen scissors dishwashersafe
Pingback: wall stencils
Pingback: kitchen decor
Pingback: Wanda Kuehn
Pingback: home decor
Pingback: Rosanne Peele
Pingback: wall decoration
Pingback: home decor ideas
Pingback: Kaila Brockman
Pingback: wall decor
Pingback: custom wall stickers
Pingback: home decor
Pingback: Raising kids
Pingback: vitalux vitamin
Pingback: Moises Schrage
Pingback: cooking scissors
Pingback: decals
Pingback: wall decoration
Pingback: kitchen scissors
Pingback: custom wall stickers
Pingback: kitchen scissors dishwashersafe
Pingback: URL
Pingback: wall decor
Pingback: wall decor
Pingback: decal
Pingback: URL
Pingback: URL
Pingback: cooking scissors
Pingback: kitchen decor
Pingback: wall stencils
Pingback: decal
Pingback: home decor
Pingback: pizza scissors
Pingback: decal
Pingback: decals
Pingback: wall decoration
Pingback: wall murals
Pingback: wall stencils
Pingback: cooking scissors
Pingback: home decor ideas
Pingback: wall decor
Pingback: wall murals
Pingback: decals
Pingback: decal
Pingback: kitchen scissors dishwashersafe
Pingback: wall stencils
Pingback: home decor ideas
Pingback: meat scissors
Pingback: wall decor
Pingback: home decor
Pingback: custom wall stickers
Pingback: kitchen decor
Pingback: wall stickers
Pingback: decals
Pingback: home decor
Pingback: cooking scissors
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: who calling me from this number
Pingback: decals
Pingback: decals
Pingback: home decor ideas
Pingback: wall decor
Pingback: wall murals
Pingback: wall decor
Pingback: kitchen decor
Pingback: decal
Pingback: wall decoration
Pingback: wall murals
Pingback: kitchen scissors dishwashersafe
Pingback: wall murals
Pingback: wall stickers
Pingback: home decor
Pingback: kitchen scissors
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: wall murals
Pingback: decals
Pingback: kitchen scissors
Pingback: custom wall stickers
Pingback: wall stencils
Pingback: wall decoration
Pingback: kitchen decor
Pingback: wall stickers
Pingback: wall stencils
Pingback: wall stencils
Pingback: wall stickers
Pingback: custom wall stickers
Pingback: decals
Pingback: wall murals
Pingback: home decor
Pingback: meat scissors
Pingback: kitchen decor
Pingback: wall decor
Pingback: wall stickers
Pingback: wall decoration
Pingback: wall stickers
Pingback: decal
Pingback: wall stencils
Pingback: custom wall stickers
Pingback: wall stencils
Pingback: URL
Pingback: wall murals
Pingback: wall decor
Pingback: wall stickers
Pingback: custom wall stickers
Pingback: URL
Pingback: home decor ideas
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: wall decor
Pingback: wall murals
Pingback: wall decoration
Pingback: wall stencils
Pingback: decal
Pingback: home decor
Pingback: formátování
Pingback: decal
Pingback: wall decor
Pingback: home decor ideas
Pingback: custom wall stickers
Pingback: home decor
Pingback: wall decor
Pingback: home decor ideas
Pingback: wall murals
Pingback: kitchen decor
Pingback: home decor
Pingback: URL
Pingback: URL
Pingback: wall stickers
Pingback: home decor ideas
Pingback: kitchen scissors dishwashersafe
Pingback: kitchen decor
Pingback: decals
Pingback: decal
Pingback: wall stencils
Pingback: home decor ideas
Pingback: wall stencils
Pingback: kitchen scissors
Pingback: home decor
Pingback: custom wall stickers
Pingback: decal
Pingback: decals
Pingback: wall decor
Pingback: wall decor
Pingback: home decor
Pingback: URL
Pingback: wall decor
Pingback: wall stencils
Pingback: decals
Pingback: home decor ideas
Pingback: Ferrari ecu repair
Pingback: kitchen decor
Pingback: wall stencils
Pingback: wall murals
Pingback: wall decoration
Pingback: decal
Pingback: wall murals
Pingback: home decor ideas
Pingback: home decor
Pingback: home decor
Pingback: decal
Pingback: home decor
Pingback: decals
Pingback: pizza scissors
Pingback: wall stickers
Pingback: decal
Pingback: wall stickers
Pingback: kitchen decor
Pingback: wall stencils
Pingback: custom wall stickers
Pingback: decal
Pingback: vpn free
Pingback: home decor ideas
Pingback: wall decoration
Pingback: wall stickers
Pingback: kitchen decor
Pingback: home decor
Pingback: wall decoration
Pingback: wall murals
Pingback: pizza scissors
Pingback: kitchen decor
Pingback: decals
Pingback: free vpn
Pingback: wall stickers
Pingback: wall stencils
Pingback: wall decor
Pingback: custom wall stickers
Pingback: wall decor
Pingback: custom wall stickers
Pingback: home decor ideas
Pingback: decal
Pingback: kitchen decor
Pingback: wall stickers
Pingback: home decor
Pingback: pizza scissors
Pingback: kitchen decor
Pingback: meat scissors
Pingback: decals
Pingback: wall stencils
Pingback: wall stickers
Pingback: kitchen scissors
Pingback: decals
Pingback: kitchen decor
Pingback: home decor
Pingback: home decor
Pingback: wall decoration
Pingback: decals
Pingback: decals
Pingback: wall decoration
Pingback: wall stencils
Pingback: decals
Pingback: home decor
Pingback: wall stencils
Pingback: wall stencils
Pingback: URL
Pingback: home decor ideas
Pingback: wall stencils
Pingback: kitchen scissors
Pingback: wall murals
Pingback: decals
Pingback: wall decor
Pingback: pizza scissors
Pingback: home decor
Pingback: wall decoration
Pingback: kitchen scissors dishwashersafe
Pingback: home decor ideas
Pingback: wall stickers
Pingback: wall murals
Pingback: decals
Pingback: home decor ideas
Pingback: wall decoration
Pingback: URL
Pingback: home decor ideas
Pingback: meat scissors
Pingback: decal
Pingback: home decor
Pingback: home decor
Pingback: kitchen decor
Pingback: meat scissors
Pingback: kitchen scissors
Pingback: kitchen scissors dishwashersafe
Pingback: cooking scissors
Pingback: wall decoration
Pingback: army ranger
Pingback: pizza scissors
Pingback: wall decoration
Pingback: wall stencils
Pingback: home decor ideas
Pingback: home decor ideas
Pingback: profit
Pingback: meat scissors
Pingback: kitchen scissors dishwashersafe
Pingback: generally
Pingback: meat scissors
Pingback: cooking scissors
Pingback: meat scissors
Pingback: phone number details with name
Pingback: kitchen scissors dishwashersafe
Pingback: whose number is this
Pingback: whose number is this calling me
Pingback: pizza scissors
Pingback: who calling me from this number
Pingback: seriously free reverse phone lookup
Pingback: phone number details with name
Pingback: whose number is this
Pingback: wall stickers
Pingback: kitchen decor
Pingback: wall stencils
Pingback: wall stickers
Pingback: wall stickers
Pingback: wall decor
Pingback: decals
Pingback: home decor ideas
Pingback: decals
Pingback: decal
Pingback: decals
Pingback: custom wall stickers
Pingback: wall murals
Pingback: kitchen decor
Pingback: home decor
Pingback: home decor ideas
Pingback: home decor
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: wall stencils
Pingback: wall decor
Pingback: custom wall stickers
Pingback: wall murals
Pingback: custom wall stickers
Pingback: home decor
Pingback: decal
Pingback: wall stencils
Pingback: wall murals
Pingback: decals
Pingback: decals
Pingback: wall decoration
Pingback: wall stencils
Pingback: home decor
Pingback: fortnite v bucks generator nintendo switch
Pingback: vigaplus price
Pingback: wall murals
Pingback: home decor
Pingback: home decor
Pingback: wall decoration
Pingback: wall murals
Pingback: wall decoration
Pingback: decal
Pingback: whose telephone number is this
Pingback: wall decor
Pingback: home decor
Pingback: wall stickers
Pingback: decals
Pingback: URL
Pingback: kitchen decor
Pingback: wall stickers
Pingback: kitchen decor
Pingback: decals
Pingback: Buy Windows 10 Pro from $17.95
Pingback: kitchen decor
Pingback: decal
Pingback: URL
Pingback: decal
Pingback: wall decor
Pingback: wall decoration
Pingback: decal
Pingback: custom wall stickers
Pingback: wall murals
Pingback: custom wall stickers
Pingback: decals
Pingback: home decor ideas
Pingback: custom wall stickers
Pingback: home decor
Pingback: Take my online class
Pingback: custom wall stickers
Pingback: home decor ideas
Pingback: decals
Pingback: decals
Pingback: decals
Pingback: wall decor
Pingback: decals
Pingback: wall decor
Pingback: BuyPlaya Advisors
Pingback: wall decor
Pingback: wall decor
Pingback: wall stickers
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: Buy Windows 10 Home from $16.95
Pingback: wall stickers
Pingback: home decor
Pingback: who is this number registered to
Pingback: home decor ideas
Pingback: home decor
Pingback: home decor
Pingback: home decor
Pingback: kitchen decor
Pingback: decals
Pingback: home decor ideas
Pingback: decals
Pingback: decals
Pingback: decals
Pingback: decals
Pingback: home decor
Pingback: home decor
Pingback: wall decor
Pingback: decals
Pingback: wall stickers
Pingback: wall decor
Pingback: whose mobile number is this
Pingback: wall decor
Pingback: decals
Pingback: wall decor
Pingback: home decor
Pingback: home decor
Pingback: decals
Pingback: home decor
Pingback: wall decor
Pingback: home decor ideas
Pingback: home decor
Pingback: Buy Microsoft Office 2013 Professional Plus from $16.95
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: home decor ideas
Pingback: whose number is this
Pingback: seriously free reverse phone lookup
Pingback: wall stickers
Pingback: decals
Pingback: 3 internet home based businesses anyone can start
Pingback: decals
Pingback: ecu devices
Pingback: Healthy eating for a healthy body
Pingback: whose number is this
Pingback: buyplaya.business.site/
Pingback: wall decor
Pingback: The benefits of whey protein
Pingback: Building ecommerce websites: where do i start?
Pingback: home decor
Pingback: Do you need accounting software for your small
Pingback: kitchen decor
Pingback: whose mobile number is this
Pingback: Dating online – the new way to meet people
Pingback: whose phone number is this for free
Pingback: играть слоты онлайн
Pingback: home decor ideas
Pingback: How to have a better relationship with men
Pingback: telford escort agency
Pingback: Managing your home based online business
Pingback: Online Dating For Dummies
Pingback: 10 reasons to use online dating sites
Pingback: URL
Pingback: URL
Pingback: Does online dating work?
Pingback: URL
Pingback: URL
Pingback: The truth about weight loss. The 6 biggest myths
Pingback: URL
Pingback: URL
Pingback: who is calling me from this number
Pingback: whose number is this
Pingback: A guide to dating
Pingback: whose number is this
Pingback: The Final Solution For Dating
Pingback: All about computer viruses
Pingback: hijama in birmingham
Pingback: who calling me from this number
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: homes for sale Whispering Pines NC
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: precision nutrition lean eating program
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: free live webcams
Pingback: Mizuno Golf School
Pingback: rfid parking system cost
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: vigaplus bad reviews
Pingback: wet cupping
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: birmingham escort agency
Pingback: Mizuno Golf
Pingback: Schwarzarbeit
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Defense intelligence agency hiring
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Ben White Whispering Pines referral agent
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: tropical vacation spots
Pingback: Mizuno Golf
Pingback: Mizuno Golf School
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: split ends
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: natural hair
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: Mizuno Golf
Pingback: bed pillows
Pingback: back sleeper pillow
Pingback: best pillow
Pingback: neck pillow for sleeping
Pingback: metabolic cooking reviews
Pingback: bed pillows
Pingback: extra firm pillow
Pingback: Benjamin White
Pingback: standard pillow
Pingback: orthopedic pillow
Pingback: best pillows for sleeping
Pingback: ergonomic pillow
Pingback: back sleeper pillow
Pingback: pillow for neck and shoulder pain
Pingback: king pillows
Pingback: pillow for neck and shoulder pain
Pingback: muscle relaxer
Pingback: bed pillow
Pingback: coconut oil teeth whitening
Pingback: back sleeper pillow
Pingback: extra firm pillow
Pingback: neck pain
Pingback: bed pillows
Pingback: neck brace for neck pain
Pingback: neck stretcher
Pingback: neck pain pillow
Pingback: standard pillow
Pingback: neck brace
Pingback: neck pain pillow
Pingback: ergonomic pillow
Pingback: standard pillow
Pingback: cervical pillow
Pingback: best pillows for sleeping
Pingback: king size pillow
Pingback: best pillows for sleeping
Pingback: king pillow
Pingback: spine alignment
Pingback: king pillow
Pingback: neck pain pillow
Pingback: neck pain pillow
Pingback: back sleeper pillow
Pingback: cervical pillow for neck pain
Pingback: cervical neck traction device
Pingback: king size pillow
Pingback: cervical traction device
Pingback: health and nutrition
Pingback: muscle relaxer
Pingback: side sleeper pillow for neck pain
Pingback: neck support pillow
Pingback: king size pillow
Pingback: chiropractic pillow
Pingback: muscle relaxer
Pingback: back sleeper pillow
Pingback: neck pain pillow
Pingback: queen pillow
Pingback: chiropractic pillow
Pingback: neck pillow for sleeping
Pingback: chiropractic pillow
Pingback: king pillows
Pingback: king size pillow
Pingback: queen pillow
Pingback: home goods
Pingback: eating well
Pingback: food pyramid
Pingback: muscle pain relief
Pingback: muscle pain relief
Pingback: cervical pillow for neck pain
Pingback: muscle pain relief
Pingback: orthopedic pillow
Pingback: side sleeper pillow
Pingback: neck travel pillow
Pingback: cervical traction device
Pingback: neck pillow for sleeping
Pingback: ergonomic pillow
Pingback: queen pillows
Pingback: queen pillow
Pingback: muscle pain relief
Pingback: amazon pillow
Pingback: long sleeve maxi dress
Pingback: standard pillow
Pingback: cervical neck traction device
Pingback: neck brace for neck pain
Pingback: cervical pillow for neck pain
Pingback: neck traction
Pingback: standard pillow
Pingback: orthopedic pillow
Pingback: neck support
Pingback: pillows for neck pain
Pingback: queen pillow
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: stomach ulcer diet
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: prediksi skor bola akurat
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: aplikasi prediksi bola
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: Flyttstädning Solna
Pingback: impede
Pingback: rfid parking system
Pingback: jewelry software
Pingback: Streaming Hentai Online Free
Pingback: osama
Pingback: R1hundred
Pingback: Flyttstädning Solna
Pingback: Submit your music
Pingback: travel solo
Pingback: pill reminder
Pingback: medicine dispenser
Pingback: medicine box
Pingback: 7 day pill box
Pingback: testimonials
Pingback: we buy houses north oaks mn
Pingback: Flyttstädning Solna
Pingback: Pill box
Pingback: Pill box
Pingback: we buy houses south saint paul mn
Pingback: we buy houses wayzata mn
Pingback: we buy houses spring lake park mn
Pingback: we buy houses orono mn
Pingback: we buy houses eden prairie mn
Pingback: we buy houses crystal mn
Pingback: medicine organizer
Pingback: contact us
Pingback: we buy houses lakeville mn
Pingback: Pill Holder
Pingback: we buy houses new hope mn
Pingback: we buy houses st louis park mn
Pingback: pill box organizer
Pingback: Pill Holder
Pingback: 7 day pill organizer
Pingback: medication organizer
Pingback: we buy houses maplewood mn
Pingback: Pill case organizer
Pingback: daily pill organizer
Pingback: we buy houses arden hills mn
Pingback: we buy houses burnsville mn
Pingback: compare
Pingback: how we buy houses
Pingback: medication organizer
Pingback: 7 day pill organizer
Pingback: daily pill box
Pingback: we buy houses eagan mn
Pingback: Pill dispenser
Pingback: Pill Holder
Pingback: daily pill organizer
Pingback: travel pill case
Pingback: we buy houses medina mn
Pingback: daily pill organizer
Pingback: travel pill case
Pingback: medicine box
Pingback: 7 day pill organizer
Pingback: Pill dispenser
Pingback: we buy houses excelsior mn
Pingback: Pill dispenser
Pingback: medicine dispenser
Pingback: Pill Organizer
Pingback: weekly pill box
Pingback: medicine dispenser
Pingback: Pill Case
Pingback: medication organizer
Pingback: pill box organizer
Pingback: Submit your music
Pingback: Love and hip hop
Pingback: bloghow to avoid foreclosure in minneapolis
Pingback: blogthe state of the market for buyers in minneapolis
Pingback: blogwhat is a pre foreclosure
Pingback: blogselling my house fast in minneapolis
Pingback: blogwhy wont my house sell in minneapolis
Pingback: our company
Pingback: blogcan i sell my minneapolis house in foreclosure
Pingback: bloginherited a house what to do in minneapolis
Pingback: we buy houses new brighton mn
Pingback: blogbehind in my mortgage payments in minneapolis
Pingback: blogwe buy houses for cash in minneapolis
Pingback: we buy houses champlin mn
Pingback: pill box organizer
Pingback: Pill dispenser
Pingback: blogwho are the cash house buyers in minneapolis mn
Pingback: 7 day pill box
Pingback: Pill Organizer
Pingback: we buy houses maple grove mn
Pingback: we buy houses brooklyn center mn
Pingback: we buy houses fridley mn
Pingback: blogcash house buyers in minneapolis
Pingback: we buy houses woodbury mn
Pingback: resource page
Pingback: blogwe buy houses in minneapolis companies
Pingback: blogbuy my house for cash in minneapolis
Pingback: blogcash for houses in minneapolis
Pingback: blogavoid trouble paying your mortgage
Pingback: Weekly pill organizer
Pingback: we buy houses stillwater mn
Pingback: daily pill box
Pingback: medication organizer
Pingback: Pill Holder
Pingback: 7 day pill box
Pingback: Pill Organizer
Pingback: medicine organizer
Pingback: medicine organizer
Pingback: blogsell a house for cash in minneapolis ryan buys houses 4 cash
Pingback: Pill Organizer
Pingback: blogforeclosure effects in minneapolis mn
Pingback: medicine dispenser
Pingback: travel pill case
Pingback: 7 day pill organizer
Pingback: medicine box
Pingback: medication organizer
Pingback: daily pill box
Pingback: daily pill organizer
Pingback: we buy houses mendota heights mn
Pingback: Pill dispenser
Pingback: we buy houses coon rapids mn
Pingback: Weekly Pill box organizer
Pingback: bloghow to stay in my home after foreclosure in minneapolis
Pingback: Weekly Pill box organizer
Pingback: Pill Holder
Pingback: Weekly pill organizer
Pingback: Pill box
Pingback: sell your house
Pingback: daily pill organizer
Pingback: medication organizer
Pingback: All on 4 dental implants cost in India
Pingback: medicine organizer
Pingback: Pill Case
Pingback: daily pill box
Pingback: Pill Case
Pingback: medicine organizer
Pingback: Pill dispenser
Pingback: Pill dispenser
Pingback: we buy houses richfield mn
Pingback: blogwho can buy my home with cash in minneapolis
Pingback: we buy houses minnetonka mn
Pingback: medicine dispenser
Pingback: medicine dispenser
Pingback: Pill Holder
Pingback: Pill Box 7 day
Pingback: daily pill box
Pingback: medicine organizer
Pingback: we buy houses plymouth mn
Pingback: 7 day pill organizer
Pingback: medicine dispenser
Pingback: we buy houses apple valley mn
Pingback: 7 day pill organizer
Pingback: we buy houses deephaven mn
Pingback: pill reminder
Pingback: pill reminder
Pingback: Pill case organizer
Pingback: Teeth Whitening Services in Vasant Kunj
Pingback: Pill Box 7 day
Pingback: Pill case organizer
Pingback: 7 day pill box
Pingback: travel pill case
Pingback: pill box organizer
Pingback: Cost of Dental treatment in New Delhi
Pingback: Pill dispenser
Pingback: dental services in vasant vihar
Pingback: Dentist in South Delhi
Pingback: Dental Treatment in South Delhi
Pingback: Dentist in vasant vihar
Pingback: professional seo consultant
Pingback: email marketing trends
Pingback: Usa attorney directory
Pingback: Landrover ecu repair
Pingback: cost of dental implants in vasant vihar
Pingback: website design, development, optimization polus media
Pingback: for publishers polus media
Pingback: Paratigratis.com
Pingback: pay per click management
Pingback: social
Pingback: Garment conveyor
Pingback: link building services
Pingback: Iron ThundeR
Pingback: locksmith services
Pingback: medicine dispenser
Pingback: 7 day pill box
Pingback: gluten free cacao
Pingback: Pill case organizer
Pingback: daily pill box
Pingback: medicine organizer
Pingback: medicine box
Pingback: medicine box
Pingback: 7 day pill organizer
Pingback: daily pill box
Pingback: medicine dispenser
Pingback: medicine organizer
Pingback: Pill Organizer
Pingback: locksmith near me
Pingback: car service msp airport
Pingback: weekly pill box
Pingback: medicine box
Pingback: Pill dispenser
Pingback: Pill case organizer
Pingback: weekly pill box
Pingback: weekly pill box
Pingback: Pill Case
Pingback: daily pill organizer
Pingback: medicine box
Pingback: Pill case organizer
Pingback: 7 day pill organizer
Pingback: daily pill box
Pingback: medicine box
Pingback: Weekly pill organizer
Pingback: daily pill organizer
Pingback: Pill box
Pingback: 7 day pill box
Pingback: weekly pill box
Pingback: 7 day pill organizer
Pingback: Weekly pill organizer
Pingback: 7 day pill box
Pingback: Weekly Pill box organizer
Pingback: 7 day pill box
Pingback: daily pill box
Pingback: Free roulette games online no download
Pingback: pill box organizer
Pingback: medicine dispenser
Pingback: Pill box
Pingback: daily pill organizer
Pingback: daily pill organizer
Pingback: pill reminder
Pingback: medication organizer
Pingback: Pill Holder
Pingback: situs prediksi bola terlengkap
Pingback: weekly pill box
Pingback: Pill case organizer
Pingback: medicine box
Pingback: 7 day pill organizer
Pingback: Weekly pill organizer
Pingback: Pill Box 7 day
Pingback: Pill dispenser
Pingback: travel pill case
Pingback: 7 day pill box
Pingback: Guitar
Pingback: pill reminder
Pingback: Weekly pill organizer
Pingback: daily pill organizer
Pingback: daily pill organizer
Pingback: Pill box
Pingback: medication organizer
Pingback: roasted cacao
Pingback: medicine dispenser
Pingback: Weekly Pill box organizer
Pingback: Pill dispenser
Pingback: medicine box
Pingback: Pill Box 7 day
Pingback: daily pill organizer
Pingback: medicine dispenser
Pingback: Weekly pill organizer
Pingback: medicine box
Pingback: Pill Holder
Pingback: Pill Holder
Pingback: Weekly pill organizer
Pingback: medication organizer
Pingback: Pill Box 7 day
Pingback: Pill Organizer
Pingback: Pill Holder
Pingback: Pill Holder
Pingback: medicine box
Pingback: travel pill case
Pingback: Pill case organizer
Pingback: daily pill organizer
Pingback: Pill dispenser
Pingback: medicine organizer
Pingback: daily pill box
Pingback: Weekly Pill box organizer
Pingback: Pill Box 7 day
Pingback: Pill Box 7 day
Pingback: medicine dispenser
Pingback: 7 day pill organizer
Pingback: pill box organizer
Pingback: medication organizer
Pingback: pill box organizer
Pingback: pill reminder
Pingback: Pill case organizer
Pingback: daily pill organizer
Pingback: Pill box
Pingback: weekly pill box
Pingback: Pill case organizer
Pingback: Pill dispenser
Pingback: Weekly pill organizer
Pingback: Weekly Pill box organizer
Pingback: pill box organizer
Pingback: argued
Pingback: medicine organizer
Pingback: Weekly pill organizer
Pingback: 7 day pill organizer
Pingback: Pill case organizer
Pingback: medication organizer
Pingback: Weekly pill organizer
Pingback: pill reminder
Pingback: travel pill case
Pingback: Pill case organizer
Pingback: Pill Organizer
Pingback: daily pill box
Pingback: Weekly pill organizer
Pingback: Pill Holder
Pingback: pill reminder
Pingback: pill reminder
Pingback: c3wm54no7tebcomvvnwecttv54t
Pingback: Tablice
Pingback: paket umroh berapa hari
Pingback: prediksi bola jitu
Pingback: women silicone wedding ring
Pingback: prediksi sepak bola nanti malam
Pingback: silicone wedding ring for women
Pingback: silicone wedding ring women
Pingback: womens silicone ring
Pingback: silicone rings
Pingback: silicon rings women
Pingback: silicone wedding ring for women
Pingback: silicone rings for women
Pingback: silicone wedding ring women
Pingback: silicone rings
Pingback: stackable silicone rings for women
Pingback: silicone ring women
Pingback: silicon rings
Pingback: silicon rings women
Pingback: rubber wedding ring for women
Pingback: silicone wedding ring women
Pingback: silicon rings
Pingback: silicon rings
Pingback: rubber wedding ring for women
Pingback: womens silicone ring
Pingback: Travel umroh wajib
Pingback: silicone rings
Pingback: silicone wedding ring women
Pingback: rubber wedding ring for women
Pingback: silicone rings for women
Pingback: silicone rings
Pingback: silicone wedding ring for women
Pingback: silicon rings
Pingback: silicon rings women
Pingback: silicon ring
Pingback: stackable silicone rings for women
Pingback: silicon ring
Pingback: stackable silicone rings for women
Pingback: stackable silicone rings for women
Pingback: silicone rings for women
Pingback: rubber wedding ring for women
Pingback: women wedding bands
Pingback: silicone wedding ring women
Pingback: silicone rings
Pingback: silicon ring
Pingback: Healthy chocolate
Pingback: silicone rings
Pingback: silicone ring women
Pingback: women wedding bands
Pingback: silicon rings women
Pingback: women silicone wedding ring
Pingback: silicon rings women
Pingback: silicone rings
Pingback: womens silicone wedding ring
Pingback: silicon rings women
Pingback: silicon rings women
Pingback: rubber rings for women
Pingback: silicon rings
Pingback: silicon ring
Pingback: silicon rings women
Pingback: silicone wedding ring women
Pingback: silicone rings for women
Pingback: silicon ring
Pingback: rubber wedding ring for women
Pingback: rubber rings for women
Pingback: silicon rings
Pingback: stackable silicone rings for women
Pingback: silicone ring women
Pingback: rubber rings for women
Pingback: silicone rings for women
Pingback: women wedding bands
Pingback: silicon ring
Pingback: silicone rings for women
Pingback: women silicone wedding ring
Pingback: silicon ring
Pingback: silicone wedding ring women
Pingback: maca capsules
Pingback: womens silicone ring
Pingback: silicon ring
Pingback: rubber rings for women
Pingback: women wedding bands
Pingback: silicon rings women
Pingback: silicone rings
Pingback: silicone ring women
Pingback: rubber rings for women
Pingback: silicone wedding ring for women
Pingback: women wedding bands
Pingback: rubber wedding ring for women
Pingback: silicon rings women
Pingback: silicone rings for women
Pingback: women silicone wedding ring
Pingback: women silicone wedding ring
Pingback: HEALTH INSURANCE A NECESSITY OF LIFE
Pingback: women silicone wedding ring
Pingback: rubber wedding ring for women
Pingback: silicone wedding ring women
Pingback: silicone wedding ring for women
Pingback: silicon rings women
Pingback: womens silicone wedding ring
Pingback: silicon rings women
Pingback: umroh indonesia
Pingback: silicon rings
Pingback: silicone wedding ring for women
Pingback: silicone rings
Pingback: women wedding bands
Pingback: women silicone wedding ring
Pingback: silicone rings for women
Pingback: womens silicone wedding ring
Pingback: rubber rings for women
Pingback: silicone wedding ring women
Pingback: silicone rings
Pingback: silicon rings women
Pingback: Weight Loss And Natural Weight Loss Supplements
Pingback: stackable silicone rings for women
Pingback: rubber wedding ring for women
Pingback: Safe Travel Usa App
Pingback: Defence Engineering
Pingback: women silicone wedding ring
Pingback: Safe Travel Alone
Pingback: rubber rings for women
Pingback: Safe Travel To Morocco
Pingback: silicone rings
Pingback: silicone rings
Pingback: women wedding bands
Pingback: silicone rings for women
Pingback: Organic Quinoa
Pingback: Safe Travel Sd
Pingback: Safe Travel Rome
Pingback: women silicone wedding ring
Pingback: silicon rings women
Pingback: Safe Places To Travel
Pingback: rubber rings for women
Pingback: Safe Travel Wishes Quotes
Pingback: Safe Travel Organization Crossword
Pingback: silicon rings
Pingback: rubber wedding ring for women
Pingback: Safe Travel Stones
Pingback: stackable silicone rings for women
Pingback: silicone rings for women
Pingback: silicon rings women
Pingback: Are You Having Heart Attack And How To Prevent It
Pingback: silicone rings
Pingback: Safe To Travel In Groups
Pingback: women wedding bands
Pingback: Safe Travel Ratings
Pingback: Safe Travel Usa South Dakota
Pingback: stackable silicone rings for women
Pingback: Lemon Nutrition: Health Benefits and Complete Nutrition Facts About The Lemons
Pingback: travel haji dan umroh terbaik
Pingback: Safe Travel Outside Us
Pingback: Safe Travel Rune
Pingback: Safe Travel Rugby
Pingback: Safe Travel Thailand
Pingback: Safe Travel Tips
Pingback: Safe Travel Org Nz
Pingback: Renewable Energy Technologies
Pingback: Medications Before and After Weight-loss Surgery
Pingback: TEN MISTAKES TO AVOID WHEN BUYING YOUR MORTGAGE
Pingback: Safe Travel Symbols
Pingback: Researchers Say Kitchen Towels Could Be The Reason For The Food Poisoning
Pingback: 9H tempered glass For
Pingback: Travel Safe Listening Answers
Pingback: Safe Travel Cutty Ranks
Pingback: Handmade Dream Catcher Keychain
Pingback: Safe Travel Wallet
Pingback: Safe Travel Ratings
Pingback: New Summer Style Funny Promoted to
Pingback: Travel Safe
Pingback: KISS WIFE Women Necklaces & Pendants multi
Pingback: gluten free maca
Pingback: silicone ring women
Pingback: womens silicone ring
Pingback: stackable silicone rings for women
Pingback: women silicone wedding ring
Pingback: stackable silicone rings for women
Pingback: rubber wedding ring for women
Pingback: silicone ring women
Pingback: silicon ring
Pingback: silicon ring
Pingback: womens silicone ring
Pingback: womens silicone wedding ring
Pingback: silicone wedding ring women
Pingback: womens silicone ring
Pingback: stackable silicone rings for women
Pingback: silicon ring
Pingback: silicone ring women
Pingback: women wedding bands
Pingback: silicone rings for women
Pingback: losing weight quickly
Pingback: stackable silicone rings for women
Pingback: womens silicone ring
Pingback: women wedding bands
Pingback: Google
Pingback: silicone wedding ring women
Pingback: womens silicone wedding ring
Pingback: silicone ring women
Pingback: silicone rings
Pingback: Consuming Of Nuts Reduces The Risk Of Developing Heart Rhythm Irregularity
Pingback: silicone rings for women
Pingback: silicone ring women
Pingback: silicon ring
Pingback: silicone ring women
Pingback: women silicone wedding ring
Pingback: preparing food
Pingback: rubber rings for women
Pingback: rubber rings for women
Pingback: rubber rings for women
Pingback: home business internet income
Pingback: rubber wedding ring for women
Pingback: Luxury Silk Leather Wallet
Pingback: silicon rings
Pingback: silicone wedding ring women
Pingback: silicon rings women
Pingback: silicon ring
Pingback: silicon rings women
Pingback: silicone wedding ring women
Pingback: silicon rings
Pingback: silicone ring women
Pingback: stackable silicone rings for women
Pingback: silicone ring women
Pingback: silicone rings
Pingback: silicone ring women
Pingback: "085781458110 promo Umroh Murah Harga Plus Al YouTube
Pingback: stackable silicone rings for women
Pingback: womens silicone wedding ring
Pingback: womens silicone ring
Pingback: rubber wedding ring for women
Pingback: maca peruana
Pingback: Super Hot Summer Fashion
Pingback: rubber wedding ring for women
Pingback: silicone ring women
Pingback: rubber wedding ring for women
Pingback: silicone rings for women
Pingback: women wedding bands
Pingback: rubber wedding ring for women
Pingback: silicone rings for women
Pingback: women wedding bands
Pingback: silicone wedding ring for women
Pingback: womens silicone ring
Pingback: silicone rings for women
Pingback: safety belt
Pingback: stackable silicone rings for women
Pingback: womens silicone ring
Pingback: silicon rings women
Pingback: auto comment site
Pingback: auto followers facebook 2018
Pingback: autobiz in
Pingback: umroh 17 juta
Pingback: travel umroh bintang 5 2018
Pingback: auto like
Pingback: fb liker for iphone
Pingback: Paket Umroh Murah Reguler 9 hari Dian Cahaya Travel - YouTube
Pingback: auto comment facebook
Pingback: autolikeviet
Pingback: auto followers fb
Pingback: auto biz liker
Pingback: Plus Size XS-4XL Fashion Summer T Women
Pingback: Free shipping infant walking
Pingback: 2018 VOGUE Summer Women T Shirt
Pingback: Canvas Wall Art Pictures
Pingback: 2Pcs Auto Car Window
Pingback: 1080P Universal 7020G Car DVD Video
Pingback: Daddy And Daughter Best Friends For Fathers
Pingback: Podofo 2 din Car Multimedia Player Audio
Pingback: Funko pop Official Movies: The Godfather
Pingback: Baby Pillow Car Safety
Pingback: 1080P Universal 7020G Car DVD Video
Pingback: Custom Wallpaper 3D Stereoscopic Embossed Gray Oil
Pingback: 9H Hardness 4D Curved Edge Full
Pingback: Zen Art Brass Feng
Pingback: For iphone X case
Pingback: Leather Back Cover Luxury Protection Flip
Pingback: Women Casual Solid Long
Pingback: Business Bluetooth Headphones stereo
Pingback: Hot Sale Fitness MMA
Pingback: 4D Round Curved Edge Tempered Glass iPhone
Pingback: 9H Hardness 4D Curved Edge Full
Pingback: Trendy Culture Galaxy flower
Pingback: Wireless charger For
Pingback: Rhinestone Necklace Bowknot Collars
Pingback: Plant Hanger Handmade Hemp Rope Plant
Pingback: 360° Tangle-Free, Heavy Duty Retractable Dog
Pingback: real mink lash extensions
Pingback: Personal trainer with reviews Altamonte Springs FL
Pingback: Safe Travel Wallet
Pingback: Best rated trainers Altamonte Springs
Pingback: Hire a Personal Trainer Altamonte Springs FL
Pingback: Hire a Personal Trainer Altamonte Springs FL
Pingback: Hire a personal trainer Altamonte Springs FL
Pingback: Altamonte Springs personal trainer
Pingback: Best rated trainers Altamonte Springs
Pingback: Hire a Personal Trainer Altamonte Springs FL
Pingback: Bongkar Rincian biaya Umroh Murah - Info Biaya Umroh Murah AfiPerjalanan
Pingback: Find a fitness trainer in Altamonte Springs FL
Pingback: improve your golf fitness Altamonte Springs FL
Pingback: Find a fitness trainer in Altamonte Springs FL
Pingback: Full Report
Pingback: Altamonte Springs best trainers
Pingback: find the best trainers Altamonte Springs FL
Pingback: Propulsion Engineering
Pingback: Altamonte Springs personal trainer
Pingback: Altamonte Springs weight loss personal trainer
Pingback: find the best trainers Altamonte Springs FL
Pingback: Altamonte Springs weight loss coach
Pingback: personal training Altamonte Springs FL
Pingback: Altamonte Personal Trainer
Pingback: Personal trainer with reviews Altamonte Springs FL
Pingback: Find a fitness trainer in Altamonte Springs FL
Pingback: Best rated trainers Altamonte Springs
Pingback: multi-platform publisher of cryptocurrency
Pingback: fastcryptotrade
Pingback: Go Here
Pingback: cryptox blockchain technology
Pingback: cryptocurrency news
Pingback: Discover More
Pingback: cryptoportal
Pingback: cryptomarket analysis
Pingback: Coinbase fastcrypto
Pingback: Coinbase fastcrypto
Pingback: visa mastercard withdraw bitcoin
Pingback: cryptocurrency news portal analysis
Pingback: Click Here
Pingback: cryptonews
Pingback: Cryptolinenews
Pingback: visa mastercard withdraw bitcoin
Pingback: fastcrypto blockchain technology
Pingback: fastcryptotrade
Pingback: multi-platform cryptocurrency
Pingback: fastcrypto
Pingback: fastcrypto
Pingback: Fast Crypto
Pingback: Solar Energy Consultant Africa
Pingback: CryptoX
Pingback: fastcrypto blockchain technology
Pingback: cryptomarket analysis
Pingback: Fast Crypto
Pingback: Cryptolinenews
Pingback: cryptoportal
Pingback: fastcryptotrade
Pingback: cryptocurrency analysis portal
Pingback: multi-platform publisher of cryptocurrency
Pingback: cryptonews
Pingback: finance and investments cryptocurrency
Pingback: Carros Hibridos
Pingback: catererglobal hospitality jobs
Pingback: cryptocurrency news portal analysis
Pingback: fastcrypto
Pingback: cryptocurrency news portal analysis
Pingback: Coinbase cryptox
Pingback: fastcrypto
Pingback: Fast Crypto
Pingback: Coinbase fastcrypto
Pingback: Tabela Fipe
Pingback: bitcoin payments paypal visa
Pingback: cryptoportal
Pingback: CryptoX
Pingback: bitcoin payments paypal visa
Pingback: Coinbase fastcrypto
Pingback: cryptocurrency analysis portal
Pingback: cryptoportal
Pingback: Coinbase cryptox
Pingback: bitcoin payments paypal visa
Pingback: fastcryptotrade
Pingback: cryptonews
Pingback: Fast Crypto
Pingback: fastcrypto
Pingback: Coinbase cryptox
Pingback: multi-platform publisher of cryptocurrency
Pingback: CryptoX
Pingback: cryptocurrency finance and investments
Pingback: cryptocurrency finance and investments
Pingback: visa mastercard withdraw bitcoin
Pingback: cryptocurrency news
Pingback: fastcryptotrade
Pingback: visa mastercard withdraw bitcoin
Pingback: Cryptolinenews
Pingback: Coinbase cryptox
Pingback: cryptocurrency finance
Pingback: Lançamento de Carros
Pingback: fastcryptotrade
Pingback: Asia travel blog
Pingback: visa mastercard withdraw bitcoin
Pingback: Coinbase cryptox
Pingback: bitcoin payments paypal visa
Pingback: cryptomarket analysis
Pingback: bitcoin payments paypal visa
Pingback: cryptocurrency news portal analysis
Pingback: cryptonews
Pingback: IPVA
Pingback: cryptocurrency news portal analysis
Pingback: berita terkini
Pingback: Catering plates bulk
Pingback: tellybuzz
Pingback: youtube banner maker
Pingback: ECU Hardware repair
Pingback: Mundonoticias247.com
Pingback: "Paket Umrah Murah 2018 Umrah Murah Umrah Murah 2018
Pingback: instagram marketing
Pingback: buy bitcoin
Pingback: kaabil full movie
Pingback: lift system
Pingback: uniforms near me
Pingback: Plumbeous forest falcon
Pingback: Limo Hire Chesterfield
Pingback: market research
Pingback: platinum elevators companies
Pingback: bmw update egypt
Pingback: BMW NAVIGATION EGYPT
Pingback: Youtube.com
Pingback: bandarq terbaik
Pingback: 조치원출장안마
Pingback: umroh lounge
Pingback: butaigui
Pingback: safesound personal alarm
Pingback: damsel in defense products
Pingback: the alarm
Pingback: safesound personal alarm
Pingback: personal safe
Pingback: safesound personal alarm keychain
Pingback: Manasik haji dan umroh
Pingback: personal safe
Pingback: personal safe
Pingback: scream safe alarm keychain
Pingback: personal safe
Pingback: scream safe alarm
Pingback: safe and sound
Pingback: safe sound personal alarm
Pingback: damsel in defense products
Pingback: personal alarm
Pingback: ring alarm
Pingback: personal alarm
Pingback: arms industries careers
Pingback: transfer belt conveyor
Pingback: ring alarm
Pingback: scream safe alarm keychain
Pingback: scream safe alarm keychain
Pingback: pocket guardian
Pingback: damsel in defense products
Pingback: personal safe
Pingback: personal protection
Pingback: personal protection
Pingback: personal alarms for women
Pingback: personal safe
Pingback: personal alarm
Pingback: scream safe alarm
Pingback: pocket guardian
Pingback: safesound personal alarm
Pingback: damsel in defense products
Pingback: safe and sound
Pingback: personal alarms for women
Pingback: damsel in defense
Pingback: personal safe
Pingback: scream safe alarm
Pingback: damsel in defense products
Pingback: dresses designs
Pingback: ring alarm
Pingback: personal safe
Pingback: safe sound personal alarm
Pingback: scream safe alarm
Pingback: personal alarm
Pingback: pocket guardian
Pingback: scream safe alarm
Pingback: personal safe
Pingback: safe and sound
Pingback: ring alarm
Pingback: pocket guardian
Pingback: damsel in defense
Pingback: damsel in defense
Pingback: pakistani wedding dresses
Pingback: ring alarm
Pingback: personal alarm
Pingback: pakistani wedding dresses
Pingback: ring alarm
Pingback: scream safe alarm keychain
Pingback: damsel in defense
Pingback: Pakistan Independence Day Quotes
Pingback: dresses designs
Pingback: 예스카지노 사이트
Pingback: democracy definition
Pingback: prediksi bola akurat malam ini
Pingback: prediksi bola menang paling akurat
Pingback: puretime replica
Pingback: prediksi bola jitu
Pingback: Buy bitcoins
Pingback: agustawestland
Pingback: Dream song lyrics
Pingback: Corporate tax accountant job description
Pingback: Anchortext
Pingback: decal
Pingback: Cohérence cardiaque
Pingback: Bioénergie
Pingback: home decor
Pingback: wall murals
Pingback: best poncho
Pingback: wall decoration
Pingback: waterproof poncho
Pingback: custom wall stickers
Pingback: rain poncho
Pingback: best poncho
Pingback: wall stencils
Pingback: mens poncho
Pingback: decal
Pingback: golf rain suit
Pingback: disposable rain ponchos
Pingback: hiking rain poncho
Pingback: hiking rain poncho
Pingback: poncho
Pingback: home decor ideas
Pingback: wall stencils
Pingback: reusable rain poncho
Pingback: custom wall stickers
Pingback: raincoat
Pingback: waterproof poncho
Pingback: golf rain suit
Pingback: rain gear
Pingback: hiking rain poncho
Pingback: wall decoration
Pingback: home decor ideas
Pingback: wall decor
Pingback: kitchen decor
Pingback: poncho
Pingback: decal
Pingback: wall decor
Pingback: raincoat
Pingback: poncho
Pingback: raincoat
Pingback: rain poncho
Pingback: wall decor
Pingback: mens poncho
Pingback: rain gear
Pingback: rain gear
Pingback: rain gear
Pingback: decal
Pingback: decals
Pingback: home decor
Pingback: wall stickers
Pingback: wall decoration
Pingback: decal
Pingback: poncho
Pingback: raincoat
Pingback: raincoat
Pingback: waterproof poncho
Pingback: kitchen decor
Pingback: mens poncho
Pingback: reusable rain poncho
Pingback: home decor ideas
Pingback: wall decoration
Pingback: home decor
Pingback: wall stencils
Pingback: wall murals
Pingback: reusable rain poncho
Pingback: home decor ideas
Pingback: rain poncho
Pingback: home decor
Pingback: mens poncho
Pingback: kitchen decor
Pingback: disposable rain ponchos
Pingback: kitchen decor
Pingback: hiking rain poncho
Pingback: home decor
Pingback: custom wall stickers
Pingback: disposable rain ponchos
Pingback: Herboristerie
Pingback: Meditation
Pingback: disposable rain ponchos
Pingback: disposable rain ponchos
Pingback: decals
Pingback: disposable rain ponchos
Pingback: rain poncho
Pingback: reusable rain poncho
Pingback: home decor
Pingback: home decor
Pingback: Cofre para Armas
Pingback: home decor ideas
Pingback: Cofres Mecanicos
Pingback: poncho
Pingback: kitchen decor
Pingback: reusable rain poncho
Pingback: poncho
Pingback: disposable rain ponchos
Pingback: waterproof poncho
Pingback: kitchen decor
Pingback: poncho
Pingback: decals
Pingback: home decor ideas
Pingback: raincoat
Pingback: home decor
Pingback: decals
Pingback: wall decor
Pingback: Cofres Digitais
Pingback: rain poncho
Pingback: kitchen decor
Pingback: wall decoration
Pingback: best poncho
Pingback: hiking rain poncho
Pingback: rain poncho
Pingback: kitchen decor
Pingback: decals
Pingback: kitchen decor
Pingback: best poncho
Pingback: mens poncho
Pingback: disposable rain ponchos
Pingback: mens poncho
Pingback: wall decor
Pingback: hiking rain poncho
Pingback: rain poncho
Pingback: custom wall stickers
Pingback: wall murals
Pingback: wall decoration
Pingback: best poncho
Pingback: reusable rain poncho
Pingback: wall stickers
Pingback: decals
Pingback: home decor ideas
Pingback: rain poncho
Pingback: rain poncho
Pingback: hiking rain poncho
Pingback: Cofre Boca de Lobo
Pingback: rain poncho
Pingback: wall decor
Pingback: custom wall stickers
Pingback: progrès
Pingback: kitchen decor
Pingback: poncho
Pingback: Massage Amma-assis
Pingback: poncho
Pingback: reusable rain poncho
Pingback: waterproof poncho
Pingback: home decor ideas
Pingback: golf rain suit
Pingback: hiking rain poncho
Pingback: home decor
Pingback: kids rain poncho
Pingback: rain poncho
Pingback: home decor ideas
Pingback: mens poncho
Pingback: home decor ideas
Pingback: decal
Pingback: best poncho
Pingback: poncho
Pingback: home decor
Pingback: home decor
Pingback: hiking rain poncho
Pingback: kids rain poncho
Pingback: kids rain poncho
Pingback: rain poncho
Pingback: kids rain poncho
Pingback: rain poncho
Pingback: mens poncho
Pingback: best poncho
Pingback: home decor ideas
Pingback: kids rain poncho
Pingback: mens poncho
Pingback: reusable rain poncho
Pingback: wall stickers
Pingback: Tarzana boiler repair
Pingback: kids rain poncho
Pingback: rain gear
Pingback: Woodland Hills septic tank plumbing
Pingback: poncho
Pingback: Woodland Hills water heaters
Pingback: reusable rain poncho
Pingback: home decor
Pingback: wall decoration
Pingback: best poncho
Pingback: reusable rain poncho
Pingback: wall decor
Pingback: waterproof poncho
Pingback: Tarzana plumbing contractor
Pingback: hiking rain poncho
Pingback: home decor ideas
Pingback: home decor ideas
Pingback: raincoat
Pingback: raincoat
Pingback: disposable rain ponchos
Pingback: wall murals
Pingback: disposable rain ponchos
Pingback: kids rain poncho
Pingback: golf rain suit
Pingback: reusable rain poncho
Pingback: raincoat
Pingback: waterproof poncho
Pingback: mens poncho
Pingback: Burbank gas line repair
Pingback: kids rain poncho
Pingback: kitchen decor
Pingback: disposable rain ponchos
Pingback: herbalism
Pingback: decals
Pingback: home decor
Pingback: wall decor
Pingback: wall murals
Pingback: wall decoration
Pingback: golf rain suit
Pingback: kids rain poncho
Pingback: kids rain poncho
Pingback: reusable rain poncho
Pingback: raincoat
Pingback: Ayurveda
Pingback: golf rain suit
Pingback: hiking rain poncho
Pingback: golf rain suit
Pingback: raincoat
Pingback: wall decoration
Pingback: raincoat
Pingback: rain gear
Pingback: disposable rain ponchos
Pingback: hiking rain poncho
Pingback: poncho
Pingback: wall decor
Pingback: decals
Pingback: decals
Pingback: waterproof poncho
Pingback: waterproof poncho
Pingback: acheter base email
Pingback: poncho
Pingback: decals
Pingback: base de donnee email
Pingback: rain poncho
Pingback: home decor ideas
Pingback: wall decoration
Pingback: raincoat
Pingback: hiking rain poncho
Pingback: raincoat
Pingback: hiking rain poncho
Pingback: base de donnee email
Pingback: best poncho
Pingback: wall murals
Pingback: wall decor
Pingback: hiking rain poncho
Pingback: hiking rain poncho
Pingback: disposable rain ponchos
Pingback: home decor ideas
Pingback: reusable rain poncho
Pingback: base de donnee email
Pingback: custom wall stickers
Pingback: decals
Pingback: wall decor
Pingback: wall stickers
Pingback: waterproof poncho
Pingback: custom wall stickers
Pingback: golf rain suit
Pingback: hiking rain poncho
Pingback: custom wall stickers
Pingback: poncho
Pingback: acheter base de donnee email
Pingback: raincoat
Pingback: golf rain suit
Pingback: wall murals
Pingback: mens poncho
Pingback: custom wall stickers
Pingback: waterproof poncho
Pingback: wall decoration
Pingback: psychologue
Pingback: acheter base email
Pingback: coach
Pingback: mens poncho
Pingback: wall stencils
Pingback: rain gear
Pingback: wall murals
Pingback: acheter base email
Pingback: decal
Pingback: raincoat
Pingback: best poncho
Pingback: best poncho
Pingback: bursa dan prediksi bola
Pingback: wall murals
Pingback: poncho
Pingback: home decor ideas
Pingback: decal
Pingback: rain poncho
Pingback: wall stencils
Pingback: wall decor
Pingback: rain poncho
Pingback: poncho
Pingback: best poncho
Pingback: best poncho
Pingback: reusable rain poncho
Pingback: hiking rain poncho
Pingback: decal
Pingback: wall decor
Pingback: best poncho
Pingback: kids rain poncho
Pingback: decal
Pingback: home decor ideas
Pingback: decal
Pingback: home decor ideas
Pingback: hiking rain poncho
Pingback: rain gear
Pingback: mens poncho
Pingback: decal
Pingback: decals
Pingback: raincoat
Pingback: home decor
Pingback: disposable rain ponchos
Pingback: mens poncho
Pingback: waterproof poncho
Pingback: poncho
Pingback: mens poncho
Pingback: reusable rain poncho
Pingback: disposable rain ponchos
Pingback: rain poncho
Pingback: mens poncho
Pingback: mens poncho
Pingback: home decor ideas
Pingback: Hypnose
Pingback: wall stickers
Pingback: waterproof poncho
Pingback: aplikasi prediksi bola
Pingback: Magnetism
Pingback: situs prediksi bola terlengkap
Pingback: prediksi bola hari ini semua liga
Pingback: prediksi pasar taruhan bola
Pingback: prediksi jitu bola malam ini
Pingback: umroh murah vs haji
Pingback: bioenergy
Pingback: Aromatology
Pingback: prediksi bola parlay
Pingback: черепица
Pingback: California contractors home study courses
Pingback: prediksi sepak bola malam
Pingback: reverse phone lookup kansas city mo
Pingback: prediksi score bola malam ini
Pingback: legal
Pingback: Free roulette online no download
Pingback: Synergologie
Pingback: Gesret method
Pingback: sex chat
Pingback: prediksi bola paling akurat
Pingback: prediksi jitu bola malam ini
Pingback: prediksi sepak bola info
Pingback: Technical Acupressure Tapas
Pingback: Reboutologie
Pingback: prediksi bola nanti malam
Pingback: bursa
Pingback: loveisland, love island, love island tv show, loveisland tv show, loveisland tv, love island tv
Pingback: decals
Pingback: Cofre Eletronico
Pingback: kitchen decor
Pingback: prediksi pertandingan bola malam ini
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: wall murals
Pingback: decals
Pingback: home decor ideas
Pingback: Detachment of trauma
Pingback: prediksi bola malam ini
Pingback: Ayurvedic medicine
Pingback: decals
Pingback: Cofre para lotéricas
Pingback: home decor ideas
Pingback: wall stencils
Pingback: Cofre Boca de Lobo
Pingback: software
Pingback: decal
Pingback: wall stickers
Pingback: lankaemarketing
Pingback: wood working tools and accessories
Pingback: best cheap fitness tracker
Pingback: wall decoration
Pingback: custom wall stickers
Pingback: personal fitness monitors
Pingback: wall stencils
Pingback: Stanley Shao
Pingback: wall stencils
Pingback: smart activity tracker
Pingback: tracking bracelet
Pingback: wall decoration
Pingback: home decor ideas
Pingback: exercise tracker watch
Pingback: custom wall stickers
Pingback: Stephaine Chalfant
Pingback: exercise wrist monitors
Pingback: wall decoration
Pingback: face 360
Pingback: wall decor
Pingback: wall stencils
Pingback: home decor
Pingback: home decor
Pingback: decals
Pingback: android digital watch
Pingback: wall stickers
Pingback: wall decoration
Pingback: home decor ideas
Pingback: decals
Pingback: motorola moto 360 watch
Pingback: 3plus activity tracker
Pingback: smart watch video
Pingback: wall decor
Pingback: wristband tracker
Pingback: kitchen decor
Pingback: u8 smart watch
Pingback: wall decoration
Pingback: kitchen decor
Pingback: airport handlers dubai
Pingback: ground handling dnata
Pingback: custom wall stickers
Pingback: show me smart watches
Pingback: best smartwatch review
Pingback: wall decor
Pingback: best smartwatch brands
Pingback: pebble smart watch
Pingback: prediksi skor bola
Pingback: i smartwatch
Pingback: android watch
Pingback: wall stickers
Pingback: home decor ideas
Pingback: decals
Pingback: wall murals
Pingback: home decor
Pingback: wall decoration
Pingback: wall stencils
Pingback: Adelaida Pillot
Pingback: wall decoration
Pingback: wall murals
Pingback: decals
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: watch get smart
Pingback: wall murals
Pingback: wall decor
Pingback: decal
Pingback: smart calling watch
Pingback: custom wall stickers
Pingback: decal
Pingback: best smartwatch for teenager
Pingback: wall murals
Pingback: wall stencils
Pingback: kitchen decor
Pingback: wall stickers
Pingback: home decor ideas
Pingback: Kourtney Blay
Pingback: smart watch phone
Pingback: Adelaida Pillot
Pingback: wall murals
Pingback: decals
Pingback: smartwatch with heart rate monitor
Pingback: decal
Pingback: Why is my hair falling out female
Pingback: emarketing
Pingback: wall decor
Pingback: fitness tracker watch
Pingback: wall stencils
Pingback: decals
Pingback: aviations services dubai
Pingback: hr activity tracker
Pingback: home decor
Pingback: wall stickers
Pingback: aviation services united arab emirates
Pingback: wall stickers
Pingback: kitchen decor
Pingback: best 2017 smart watch
Pingback: Heavy rain walkthrough
Pingback: decals
Pingback: custom wall stickers
Pingback: home decor ideas
Pingback: decals
Pingback: custom wall stickers
Pingback: decals
Pingback: gear s2 watch
Pingback: wall stencils
Pingback: wall murals
Pingback: the best smartwatch for android
Pingback: wall stencils
Pingback: best activity tracker for women
Pingback: home decor ideas
Pingback: step tracking devices
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: decals
Pingback: decals
Pingback: home decor ideas
Pingback: decals
Pingback: ios compatible smart watches
Pingback: custom wall stickers
Pingback: lg smart watch app
Pingback: wall stickers
Pingback: home decor ideas
Pingback: wall murals
Pingback: home decor
Pingback: home decor ideas
Pingback: home decor ideas
Pingback: wall stickers
Pingback: wall murals
Pingback: best smartwatch for apple
Pingback: wall stencils
Pingback: home decor ideas
Pingback: wall stickers
Pingback: home decor ideas
Pingback: 2017 smart watches
Pingback: wall decor
Pingback: top women's smart watches
Pingback: wall murals
Pingback: activity monitors watch
Pingback: kitchen decor
Pingback: android watch reviews
Pingback: home decor ideas
Pingback: fitness activity watch
Pingback: hasil liga inggris
Pingback: kitchen decor
Pingback: charter flights
Pingback: wall stickers
Pingback: best fitness tracker with heart rate
Pingback: wearable fitness devices
Pingback: wall murals
Pingback: smart watch android woman
Pingback: free smart watch
Pingback: gear 2 watch
Pingback: decal
Pingback: wall stickers
Pingback: wearable fitness devices
Pingback: essure implant lawsuit
Pingback: hr activity tracker
Pingback: decals
Pingback: custom wall stickers
Pingback: decals
Pingback: best smartwatch for teenager
Pingback: custom wall stickers
Pingback: home decor
Pingback: home decor
Pingback: wall decor
Pingback: custom wall stickers
Pingback: health tracker bracelet
Pingback: smart watches for iphone 6
Pingback: home insurance
Pingback: home decor
Pingback: wall decor
Pingback: kitchen decor
Pingback: best sleep tracker wristband
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: marketing
Pingback: wall decor
Pingback: Chicken coop plans manual
Pingback: Chicken Coop Tour The Garden Coop
Pingback: Chicken Coop Plans That Work
Pingback: custom wall stickers
Pingback: custom wall stickers
Pingback: decal
Pingback: home decor
Pingback: decal
Pingback: custom wall stickers
Pingback: wall murals
Pingback: home decor ideas
Pingback: wall murals
Pingback: home decor
Pingback: latestvideo sirius577 abdu23na3430 abdu23na34
Pingback: home decor
Pingback: wall decoration
Pingback: kitchen decor
Pingback: wall stickers
Pingback: home decor
Pingback: decals
Pingback: wall decor
Pingback: wall murals
Pingback: kitchen decor
Pingback: wall decor
Pingback: How to Raise Chickens Some Questions and Answers
Pingback: decal
Pingback: custom wall stickers
Pingback: wall stickers
Pingback: wall decoration
Pingback: wall decor
Pingback: Mistakes To Avoid When Building A Chicken Coop
Pingback: wall stickers
Pingback: wall murals
Pingback: Free DIY Chicken Coop Designs
Pingback: kitchen decor
Pingback: wall murals
Pingback: decals
Pingback: home decor
Pingback: National Chicken Council News
Pingback: wall decor
Pingback: wall decoration
Pingback: decals
Pingback: wall decoration
Pingback: home decor ideas
Pingback: kitchen decor
Pingback: decals
Pingback: wall decor
Pingback: kitchen decor
Pingback: wall decor
Pingback: decals
Pingback: decals
Pingback: wall decoration
Pingback: custom wall stickers
Pingback: wall decor
Pingback: decals
Pingback: kitchen decor
Pingback: visit sri lanka
Pingback: sri lanka honeymoon
Pingback: sri lanka vacation
Pingback: wall stickers
Pingback: wall stencils
Pingback: Build A Chicken Coop Quickly And Easily
Pingback: sri lanka holiday packages
Pingback: Simple Chicken Coop Plans Learn How To Easily Build A Chicken Coop Yourself
Pingback: srilanka tour package
Pingback: visit sri lanka
Pingback: wall decor
Pingback: home decor
Pingback: Video Easy DIY Chicken Coop Plans
Pingback: wall murals
Pingback: prediksi bola info
Pingback: sri lanka travel
Pingback: sri lanka honeymoon
Pingback: cheap subscriptions
Pingback: sri lanka honeymoon packages
Pingback: srilanka tour package
Pingback: sri lanka honeymoon
Pingback: sri lanka holidays
Pingback: visit sri lanka
Pingback: sri lanka honeymoon
Pingback: sri lanka travel
Pingback: schindler elevators careers
Pingback: sri lanka vacation
Pingback: prediksi bola paling akurat
Pingback: srilanka tour package
Pingback: visit sri lanka
Pingback: sri lanka travel
Pingback: sri lanka holidays
Pingback: sri lanka honeymoon packages
Pingback: sri lanka vacation
Pingback: srilanka tour package
Pingback: sri lanka vacation
Pingback: sri lanka vacation
Pingback: sri lanka tour packages price
Pingback: visit sri lanka
Pingback: sri lanka honeymoon
Pingback: srilanka tour package
Pingback: sri lanka holidays
Pingback: Best deal on penomet
Pingback: Alquiler de auto en Cordoba
Pingback: latestvideo sirius375 abdu23na909 abdu23na66
Pingback: Car rentals
Pingback: new siriustube809 abdu23na6790 abdu23na70
Pingback: buy bitcoins with credit card no id
Pingback: best magazine subscriptions
Pingback: make money online
Pingback: Renta Car
Pingback: Kotfraktur behandling
Pingback: cheap magazine subscription
Pingback: wristband custom silicone bracelets
Pingback: prediksi sepak bola malam
Pingback: SEO Doha
Pingback: SEO Bradford
Pingback: SEO Bradford
Pingback: SEO Nottingham
Pingback: SEO Nottingham
Pingback: SEO Doha
Pingback: SEO Doha
Pingback: SEO Doha
Pingback: SEO Bradford
Pingback: SEO Bradford
Pingback: SEO Bradford
Pingback: SEO Nottingham
Pingback: sports betting
Pingback: SEO Bradford
Pingback: SEO Bradford
Pingback: SEO Nottingham
Pingback: SEO Bradford
Pingback: bola
Pingback: review of pushup magic panties
Pingback: SEO Doha
Pingback: SEO Nottingham
Pingback: SEO Doha
Pingback: SEO Doha
Pingback: SEO Bradford
Pingback: SEO Bradford
Pingback: active burn bra to tighten the breasts 2018
Pingback: active burn best of breast lifting bra active burn
Pingback: SEO Bradford
Pingback: SEO Doha
Pingback: SEO Doha
Pingback: SEO Nottingham
Pingback: activburn push up magic bra female
Pingback: SEO Bradford
Pingback: prediksi bola biru
Pingback: jouer 1xbet
Pingback: jadwal liga inggris
Pingback: prediksi sepak bola info
Pingback: prediksi bola terbaik
Pingback: beautiful extreme breast lifting bra probe
Pingback: prediksi jitu bola
Pingback: prediksi score bola malam ini
Pingback: aplikasi prediksi bola
Pingback: omni cryptocurrency
Pingback: where to get pushup bra instagram trends
Pingback: prediksi bola nanti malam
Pingback: 슬롯머신
Pingback: prediksi jitu bola
Pingback: prediksi bola akurat gratis
Pingback: prediksi bola hongkong
Pingback: prediksi score bola malam ini
Pingback: como conquistar uma vida plena com foco e disciplina
Pingback: qual o sintoma de ansiedade
Pingback: prediksi sepak bola malam
Pingback: prediksi bola menang pasti
Pingback: prediksi bola fb
Pingback: situs prediksi bola paling akurat
Pingback: aplikasi prediksi bola
Pingback: crise de ansiedade sintomas
Pingback: qual o sintoma de ansiedade
Pingback: prediksi bola hari ini semua liga
Pingback: situs prediksi bola
Pingback: the complete remote influencing training system by gerald o'donnell
Pingback: psicologia
Pingback: prediksi bola liga champion
Pingback: como diminuir a ansiedade
Pingback: 3d optical lamp night light dinosau
Pingback: lofts for rent in detroit
Pingback: michigan lake house rentals
Pingback: michigan housing
Pingback: prediksi bola parlay
Pingback: apartments in michigan
Pingback: prediksi score bola
Pingback: detroit rentals
Pingback: complete remote viewing reviews
Pingback: apartments for rent in maryland
Pingback: detroit apartments
Pingback: apartments for rent in vermont
Pingback: houses for rent metro detroit
Pingback: townhouses for rent in michigan
Pingback: best apartments in michigan
Pingback: apartments for rent in vermont
Pingback: best sex dolls
Pingback: conneticut school shooting
Pingback: homes for rent in ann arbor mi
Pingback: 5 bedroom homes for rent in michigan
Pingback: english tutor
Pingback: detroit homes for rent by owner
Pingback: private landlords in michigan
Pingback: cheap townhomes for rent in michigan
Pingback: 4 bedroom townhomes for rent in michigan
Pingback: best condos in michigan
Pingback: 5 bedroom homes for rent in michigan
Pingback: lofts for rent in metro detroit
Pingback: cheap 1 bedroom apartments in michigan
Pingback: apartments for rent in southeast michigan
Pingback: houses for rent southwest detroit mi
Pingback: apartments for rent lansing mi
Pingback: rentals
Pingback: apartments in metro detroit area
Pingback: cheap 3 bedroom apartments in michigan
Pingback: prediksi taruhan bola
Pingback: find a pt
Pingback: efficiency apartment
Pingback: flats for rent in bangalore
Pingback: to rent an apartment
Pingback: prediksi jitu bola
Pingback: apt list
Pingback: garage apartment
Pingback: search apartments for rent
Pingback: apt
Pingback: apartment complexes
Pingback: one bedroom apartments for rent near me
Pingback: available apartments
Pingback: prediksi bola terbaik
Pingback: complete remote influencing training download
Pingback: prediksi bola liga champion
Pingback: prediksi bola hongkong
Pingback: cost to rent a dumpster
Pingback: dumpster container
Pingback: residential dumpster service
Pingback: B.G. dumpster rental
Pingback: portable dumpster rental
Pingback: dumpster bin
Pingback: prediksi bola akurat 100
Pingback: debris box
Pingback: dumpster waste management
Pingback: prediksi bola gratis
Pingback: cost for dumpster rental
Pingback: rental of dumpster
Pingback: dirt dumpster
Pingback: dumpster sizes waste management
Pingback: garbage containers rental
Pingback: trash container rental prices
Pingback: 40 yard container
Pingback: 10 yard dumpster rental cost
Pingback: aplikasi prediksi bola
Pingback: mobile phone
Pingback: music teacher in markham
Pingback: garbage skip
Pingback: prediksi bola fb
Pingback: yard waste container rental
Pingback: price of dumpster
Pingback: rental bins for garbage
Pingback: bfi bin rental
Pingback: prediksi score bola
Pingback: junk hauling business
Pingback: dumpster dimensions waste management
Pingback: dumpster rental minneapolis
Pingback: average price for dumpster rental
Pingback: roll off trash dumpster
Pingback: dumpster rental business
Pingback: trash container service
Pingback: prediksi skor bola
Pingback: inside dryer vents
Pingback: clothes dryer vent booster
Pingback: air ducting
Pingback: congressional country club bethesda
Pingback: dryer exhaust vents
Pingback: how to clean dryer vent duct
Pingback: "Paket Umrah Murah 2018 Khusus Pesawat Saudia Al
Pingback: clean a dryer vent
Pingback: prediksi bola jitu malam ini
Pingback: Dryer vent cleaning how to
Pingback: flexible air duct
Pingback: dryer duct vent
Pingback: ductwork parts
Pingback: dryer tube
Pingback: cleaning dryer lint
Pingback: Longer drying cycles
Pingback: indoor dryer vent
Pingback: dryer venting kits
Pingback: Garten Bewässerungssystem
Pingback: dryer wizard
Pingback: install dryer vent
Pingback: rooftop dryer vent
Pingback: how do you clean dryer vents
Pingback: dryer vent hoses
Pingback: bursa dan prediksi bola
Pingback: new rich lazy trader review
Pingback: prediksi bola akurat 100
Pingback: bursa dan prediksi bola
Pingback: best music school in richmond hill
Pingback: best sex dolls
Pingback: best sex dolls
Pingback: 3d optical lamp night light dinosau
Pingback: bail bonds fulton county
Pingback: trusted gun store
Pingback: Kent State
Pingback: golf trophy cup
Pingback: bursa dan prediksi bola
Pingback: prediksi sepak bola nanti malam
Pingback: Clicking Here
Pingback: houses for sale
Pingback: Clicking Here
Pingback: Check This Out
Pingback: More Info
Pingback: Marietta Homes for Sale
Pingback: Get More Info
Pingback: Read More Here
Pingback: Click This Link
Pingback: Clicking Here
Pingback: Web Site
Pingback: Home Page
Pingback: Read This
Pingback: Click Here
Pingback: Homepage
Pingback: Read This
Pingback: Look At This
Pingback: Visit Website
Pingback: 3d optical lamp night light star wa
Pingback: Discover More
Pingback: Visit Website
Pingback: Find Out More
Pingback: Visit Website
Pingback: Discover More
Pingback: Website
Pingback: Check This Out
Pingback: download slot
Pingback: Home Page
Pingback: Check This Out
Pingback: Website
Pingback: Home Page
Pingback: Web Site
Pingback: Visit This Link
Pingback: Read This
Pingback: Click Here
Pingback: Click This Link
Pingback: Read More
Pingback: Going Here
Pingback: Look At This
Pingback: Homepage
Pingback: Clicking Here
Pingback: Read More Here
Pingback: Visit This Link
Pingback: Read This
Pingback: Read More Here
Pingback: Clicking Here
Pingback: Find Out More
Pingback: Look At This
Pingback: Discover More Here
Pingback: Discover More
Pingback: Posture corrector brace
Pingback: Posture support brace
Pingback: How to correct posture
Pingback: Posture
Pingback: Posture Brace
Pingback: Posture corrector device
Pingback: Posture corrector device
Pingback: prediksi bola jitu
Pingback: How to correct posture
Pingback: Posture Corrector
Pingback: How to correct posture
Pingback: Posture correction brace
Pingback: Posture support brace
Pingback: Improve Posture
Pingback: Posture Corrector
Pingback: Web App
Pingback: Fix posture
Pingback: Back Brace for Posture
Pingback: Posture support brace
Pingback: prediksi bola gratis
Pingback: Perfect posture
Pingback: Posture support brace
Pingback: Posture corrector device
Pingback: Best Posture Corrector
Pingback: Posture support brace
Pingback: Posture corrector device
Pingback: Best Posture Corrector
Pingback: Posture
Pingback: Do posture braces work
Pingback: Posture corrector brace
Pingback: download film semi korea
Pingback: semi movie
Pingback: prediksi sepak bola malam
Pingback: Posture support brace
Pingback: Posture correction brace
Pingback: Posture Brace
Pingback: Do posture braces work
Pingback: prediksi score bola
Pingback: Fix posture
Pingback: Posture corrector device
Pingback: Back Brace for Posture
Pingback: How to fix posture
Pingback: Posture corrector device
Pingback: Posture support
Pingback: Fix Posture
Pingback: Fix posture
Pingback: Cloud Storage
Pingback: videos
Pingback: Posture correction brace
Pingback: Posture support
Pingback: Fix posture
Pingback: How to correct posture
Pingback: Posture support
Pingback: How to Fix your Posture
Pingback: next player immediately
Pingback: Improve Posture
Pingback: Posture corrector brace
Pingback: Improve Posture
Pingback: Perfect posture
Pingback: Posture corrector brace
Pingback: How to Fix your Posture
Pingback: Posture corrector brace
Pingback: prediksi bola malam ini
Pingback: Perfect posture
Pingback: Do posture braces work
Pingback: Posture correction brace
Pingback: Posture corrector brace
Pingback: Fix Posture
Pingback: Posture corrector brace
Pingback: Perfect posture
Pingback: Best Posture Corrector
Pingback: Posture Corrector
Pingback: Back Brace for Posture
Pingback: Cloud OS
Pingback: Posture
Pingback: How to correct posture
Pingback: Do posture braces work
Pingback: How to correct posture
Pingback: streaming film semi
Pingback: streaming film semi
Pingback: How to Fix your Posture
Pingback: Best Posture Corrector
Pingback: Do posture braces work
Pingback: Perfect posture
Pingback: How to Fix your Posture
Pingback: How to Fix your Posture
Pingback: Improve Posture
Pingback: Perfect posture
Pingback: Posture support brace
Pingback: How to Fix your Posture
Pingback: Posture Corrector
Pingback: download film semi sub indo
Pingback: Posture correction brace
Pingback: Fix Posture
Pingback: How to Fix your Posture
Pingback: Posture support
Pingback: Posture support brace
Pingback: Fix posture
Pingback: 24 hour locksmith
Pingback: Posture support
Pingback: Posture Corrector
Pingback: How to Improve posture
Pingback: Posture support brace
Pingback: How to Improve posture
Pingback: Do posture braces work
Pingback: Do posture braces work
Pingback: How to correct posture
Pingback: How to correct posture
Pingback: Posture corrector brace
Pingback: read without glasses method dvd download
Pingback: How to fix posture
Pingback: prediksi bola liga inggris
Pingback: Best posture brace
Pingback: Posture
Pingback: Posture Brace
Pingback: How to correct posture
Pingback: How to Fix your Posture
Pingback: How to Improve posture
Pingback: Improve Posture
Pingback: Back Brace for Posture
Pingback: Clarins hand and nail treatment cream 50ml
Pingback: Fix posture
Pingback: Posture corrector device
Pingback: Posture support
Pingback: Posture corrector brace
Pingback: Posture corrector device
Pingback: Posture
Pingback: Fix Posture
Pingback: Back Brace for Posture
Pingback: Free images
Pingback: Back Brace for Posture
Pingback: Posture correction brace
Pingback: How to fix posture
Pingback: Perfect posture
Pingback: Posture support brace
Pingback: Improve Posture
Pingback: Posture corrector brace
Pingback: How to Fix your Posture
Pingback: Posture correction brace
Pingback: Best Posture Corrector
Pingback: Fix posture
Pingback: Do posture braces work
Pingback: Posture correction brace
Pingback: Posture Corrector
Pingback: Posture Corrector
Pingback: Improve Posture
Pingback: home visit cupping
Pingback: Posture Corrector
Pingback: How to fix posture
Pingback: Perfect posture
Pingback: Posture support brace
Pingback: Perfect posture
Pingback: Do posture braces work
Pingback: Posture corrector brace
Pingback: Fix posture
Pingback: How to fix posture
Pingback: How to fix posture
Pingback: Improve Posture
Pingback: Fix posture
Pingback: Posture correction brace
Pingback: Best posture brace
Pingback: Fix posture
Pingback: Posture support
Pingback: Best Posture Corrector
Pingback: Posture Brace
Pingback: How to fix posture
Pingback: Posture Brace
Pingback: Posture
Pingback: Posture corrector brace
Pingback: Best Posture Corrector
Pingback: Perfect posture
Pingback: How to fix posture
Pingback: Fix posture
Pingback: Posture
Pingback: Posture corrector brace
Pingback: Posture Corrector
Pingback: Posture Brace
Pingback: Posture support brace
Pingback: How to Improve posture
Pingback: Posture corrector brace
Pingback: Posture support
Pingback: Do posture braces work
Pingback: Posture
Pingback: Posture correction brace
Pingback: Posture Corrector
Pingback: Perfect posture
Pingback: Posture corrector device
Pingback: How to Improve posture
Pingback: Posture Corrector
Pingback: How to correct posture
Pingback: Posture Corrector
Pingback: How to Improve posture
Pingback: How to Fix your Posture
Pingback: Posture Corrector
Pingback: Posture support brace
Pingback: Improve Posture
Pingback: Best posture brace
Pingback: How to correct posture
Pingback: Posture correction brace
Pingback: Do posture braces work
Pingback: Best posture brace
Pingback: Posture support
Pingback: Back Brace for Posture
Pingback: Posture correction brace
Pingback: Posture corrector brace
Pingback: Posture
Pingback: Posture correction brace
Pingback: How to correct posture
Pingback: Improve Posture
Pingback: Posture support brace
Pingback: Do posture braces work
Pingback: Improve Posture
Pingback: Posture
Pingback: Do posture braces work
Pingback: Posture corrector brace
Pingback: Posture support brace
Pingback: Posture Corrector
Pingback: Best posture brace
Pingback: Posture correction brace
Pingback: Perfect posture
Pingback: Posture
Pingback: Posture corrector device
Pingback: Fix Posture
Pingback: How to fix posture
Pingback: Posture support
Pingback: How to fix posture
Pingback: Posture corrector device
Pingback: Posture correction brace
Pingback: Improve Posture
Pingback: Fix posture
Pingback: Posture correction brace
Pingback: Back Brace for Posture
Pingback: Fix posture
Pingback: Best posture brace
Pingback: Posture corrector device
Pingback: How to Improve posture
Pingback: Posture
Pingback: Best Posture Corrector
Pingback: Perfect posture
Pingback: Do posture braces work
Pingback: How to correct posture
Pingback: Fix posture
Pingback: Posture corrector brace
Pingback: Posture support
Pingback: Posture support brace
Pingback: Posture support brace
Pingback: Back Brace for Posture
Pingback: Best Posture Corrector
Pingback: Posture corrector brace
Pingback: Improve Posture
Pingback: URL
Pingback: URL
Pingback: Improve Posture
Pingback: Fix posture
Pingback: URL
Pingback: URL
Pingback: Posture Corrector
Pingback: Fix posture
Pingback: Posture Brace
Pingback: Back Brace for Posture
Pingback: Do posture braces work
Pingback: Posture Brace
Pingback: URL
Pingback: How to correct posture
Pingback: Best Posture Corrector
Pingback: Posture support
Pingback: Posture corrector brace
Pingback: Posture corrector device
Pingback: How to Fix your Posture
Pingback: How to Fix your Posture
Pingback: Best posture brace
Pingback: Posture support brace
Pingback: How to fix posture
Pingback: Posture corrector device
Pingback: Perfect posture
Pingback: Do posture braces work
Pingback: Posture corrector brace
Pingback: Posture corrector brace
Pingback: Posture corrector brace
Pingback: Posture correction brace
Pingback: Posture Brace
Pingback: Posture corrector device
Pingback: How to correct posture
Pingback: Posture correction brace
Pingback: Best posture brace
Pingback: Best posture brace
Pingback: Posture Brace
Pingback: Posture support brace
Pingback: Posture Corrector
Pingback: Perfect posture
Pingback: Improve Posture
Pingback: Fix posture
Pingback: Best posture brace
Pingback: Posture correction brace
Pingback: improvement projects
Pingback: acheter-fichier-email.com
Pingback: acheter fichier email
Pingback: acheter-fichier-email.com
Pingback: acheter-fichier-email.com
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: epoxy floor paint indianapolis 2
Pingback: acheter-fichier-email.com
Pingback: acheter-fichier-email.com
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: harvoni price in india
Pingback: Lotus tree necklace
Pingback: Butterfly pendant
Pingback: Owl and moon phone case
Pingback: Butterfly lover's necklace
Pingback: epoxy floor paint indianapolis 2
Pingback: Hindu elephant phone cover
Pingback: the Jolly Cat home page
Pingback: Owl lover necklace
Pingback: Cat and moon pendant
Pingback: Elephant iPhone X cover
Pingback: Nature necklace
Pingback: Hindu elephant phone cover
Pingback: Yoga pendant necklace
Pingback: Elephant iPhone X cover
Pingback: Owl phone cover
Pingback: Nature phone case
Pingback: Nature necklace
Pingback: garage floor coating indianapolis
Pingback: garage flooring indianapolis
Pingback: agenqq
Pingback: garage floor epoxy indianapolis
Pingback: agen qq 365
Pingback: agenqq
Pingback: agenqq
Pingback: agenqq365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agen qq 365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agen qq 365
Pingback: agenqq365
Pingback: agenqq365
Pingback: agen qq 365
Pingback: agen qq 365
Pingback: agen qq 365
Pingback: agenqq365
Pingback: agenqq365
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur 365
Pingback: terrazzo flooring indianapolis
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur 365
Pingback: epoxy flooring indianapolis 2
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur 365
Pingback: garage floor paint indianapolis
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur 365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: makmur365
Pingback: terrazzo flooring indianapolis
Pingback: acheter base de donnee email
Pingback: www.acheter-base-de-donnee-email.com/
Pingback: acheter base de donnee email
Pingback: www.acheter-base-de-donnee-email.com/
Pingback: www.acheter-base-de-donnee-email.com/
Pingback: www.acheter-base-de-donnee-email.com/
Pingback: acheter base de donnee e-mail
Pingback: www.acheter-base-de-donnee-email.com/
Pingback: acheter base de donnee email
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: vpn
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: bandar 855
Pingback: Affiliate program
Pingback: bandar855
Pingback: bandar855
Pingback: bandar855
Pingback: download on mobile935 afeu23na767 abdu23na39
Pingback: bandar855
Pingback: bandar855
Pingback: tubepla.net download601 afeu23na7413 abdu23na16
Pingback: bandar855
Pingback: bandar855
Pingback: bandar855
Pingback: bandar855
Pingback: acheter base email
Pingback: acheter base email
Pingback: www.acheter-base-de-donnees-emails.fr/
Pingback: acheter base de donnee email
Pingback: Get More Information
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: Get the facts
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: acheter fichier email
Pingback: waikato dial a driver
Pingback: sober driver hamilton
Pingback: Clicking Here
Pingback: dic driver hamilton
Pingback: sober driver waikato
Pingback: how much does dial a driver cost
Pingback: dial a driver hamilton
Pingback: dial a driver
Pingback: Website
Pingback: dial a driver cambridge
Pingback: Read More
Pingback: dial a driver cambridge
Pingback: dial a driver raglan
Pingback: Get More Information
Pingback: dic hamilton
Pingback: Full Report
Pingback: how much does dial a driver cost
Pingback: http://hayastannews.com/news/168773.html
Pingback: control de plagas granada
Pingback: fknjn544a646 afeu23na3273 abdu23na86
Pingback: super vpn
Pingback: free vpn
Pingback: vpn
Pingback: super vpn
Pingback: vpn
Pingback: decal
Pingback: Buy Michigan CBD
Pingback: wall decoration
Pingback: wall stencils
Pingback: kitchen decor
Pingback: decal
Pingback: wall decoration
Pingback: wall murals
Pingback: wall murals
Pingback: wall decor
Pingback: wall decoration
Pingback: wall decoration
Pingback: kitchen decor
Pingback: wall decor
Pingback: home decor ideas
Pingback: wall murals
Pingback: decals
Pingback: wall murals
Pingback: home decor
Pingback: kitchen decor
Pingback: kitchen decor
Pingback: home decor
Pingback: home decor
Pingback: home decor ideas
Pingback: decal
Pingback: home decor ideas
Pingback: wall stickers
Pingback: wall stencils
Pingback: wall murals
Pingback: home decor
Pingback: wall stickers
Pingback: wall murals
Pingback: wall stickers
Pingback: www.primedecals.com
Pingback: EcoPlanet Bamboo Investment Kenya
Pingback: EcoPlanet Nicaragua
Pingback: Sruthi Pathak Bangalore Escorts Services
Pingback: SDR
Pingback: Silver Investing
Pingback: www.terrysacka.com
Pingback: EcoPlanet Bamboo South Africa
Pingback: Secure IRA
Pingback: EcoPlanet South Africa
Pingback: 2016 US Market Crash
Pingback: Camille Rebelo Kenya
Pingback: Barack Obama 2016
Pingback: International Monetary Fund
Pingback: Buy Silver
Pingback: Troy Wiseman Eco Planet Bamboo
Pingback: EcoPlanet Bamboo South Africa
Pingback: EcoPlanet Nicaragua
Pingback: Troy Wiseman EcoPlanet Bamboo
Pingback: 7 Cycles of Empire
Pingback: lose fat
Pingback: More About
Pingback: free information online
Pingback: Investment Advice
Pingback: emploi togo
Pingback: lomé city
Pingback: free vpn
Pingback: vpn
Pingback: free vpn
Pingback: wall decor
Pingback: arcade games discussions
Pingback: wall decor
Pingback: supreme fanny pack
Pingback: Vinyl Plank Flooring
Pingback: solotravel
Pingback: db bahn
Pingback: lisbon
Pingback: know thy traveler
Pingback: wall decals quotes
Pingback: decal stickers
Pingback: onesimcard
Pingback: london
Pingback: Wish Promo Codes
Pingback: stickers decor
Pingback: england
Pingback: beer
Pingback: czech
Pingback: vienna
Pingback: where to buy wall tattoos
Pingback: safety
Pingback: google maps
Pingback: tiny wall stickers
Pingback: Kaila Brockman
Pingback: tree wall stickers online
Pingback: Nevada Goold
Pingback: vlog
Pingback: hostel
Pingback: large wall stickers
Pingback: porto
Pingback: learning
Pingback: cdg
Pingback: full wall stickers online
Pingback: western europe
Pingback: peel and stick wall art
Pingback: visit berlin
Pingback: backpacking
Pingback: language
Pingback: Erminia Deer
Pingback: europe travel
Pingback: safety
Pingback: travel planning
Pingback: Serina Mealy
Pingback: Olin Flink
Pingback: make money blogging
Pingback: make money amazon
Pingback: ground improvement contractors
Pingback: foundation solutions
Pingback: Receipt Maker
Pingback: scheduling app
Pingback: Maldives resorts
Pingback: best sheets to buy
Pingback: bed sheets online
Pingback: best sheets
Pingback: best sheets
Pingback: best bed sheets
Pingback: Discover More Here
Pingback: bamboo sheets amazon
Pingback: bamboo sheets review
Pingback: best sheets
Pingback: how to choose bed sheets
Pingback: how to sell herbalife
Pingback: how to sign up for herbalife
Pingback: photography sites
Pingback: how to sign up for herbalife
Pingback: dirt bike riding tips for beginners
Pingback: long black dress cheap
Pingback: photography sites
Pingback: how to freshen up your old dirt bike
Pingback: common causes of engine failure and how to prevent it
Pingback: photography sites
Pingback: dirt bike chain and sprocket maintenance
Pingback: parts that will give your dirt bike more power
Pingback: camera reviews
Pingback: cameras for beginners
Pingback: mypsychicadvice.com
Pingback: www.mypsychicadvice.com/
Pingback: www.mypsychicadvice.com/
Pingback: photographers near me
Pingback: robert
Pingback: home page
Pingback: buy women shoes in india
Pingback: souris gamer avec et sans fil
Pingback: topelek souris gamer sans fil 2000 dpi
Pingback: souris pc gamer fnac
Pingback: souris gamer gost ms50
Pingback: fast affordable iPhone repair
Pingback: souris gamer razer entrée de gamme
Pingback: fast affordable software restoration
Pingback: water damage phone, save my pictures
Pingback: Snap backs
Pingback: Segurança Digital
Pingback: babysitter
Pingback: best pediatrics doctor in amman
Pingback: Segurança da Informação
Pingback: Tecnologia da Informação
Pingback: Segurança na Internet
Pingback: Segurança Cibernética
Pingback: wcm549w4xjc5nvtc5tvewcr
Pingback: Trully Independent Bangalore Escorts
Pingback: pest control
Pingback: seattle pest control
Pingback: seattle exterminators
Pingback: seattle exterminators
Pingback: pest control
Pingback: serial online seriya smotret
Pingback: Äîìàøíèé àðåñò âñå ñåðèè
Pingback: domashnij-arest
Pingback: Venom 2018
Pingback: 2018
Pingback: hdseriionline.ru
Pingback: hdseriionline.ru/bg/
Pingback: c3t5w4jjjjno4otwctrwc49n5
Pingback: 3wc70vt5c7tv54c7wd54vwt4
Pingback: seattle commercial exterminators
Pingback: seattle commercial exterminators
Pingback: seattle commercial exterminators
Pingback: seattle exterminators
Pingback: seattle commercial exterminators
Pingback: commercial exterminators
Pingback: seattle pest control
Pingback: seattle pest control
Pingback: Goa Escorts Services Drishti Goyal
Pingback: Trully Independent Bangalore Escorts Services
Pingback: → 10 Revestimentos Para Bancadas Desde Cozinha | Pro-tekst
Pingback: 2r34cyrn64tc24t2xw3w3
Pingback: Art Tribal Graphics
Pingback: nt54wcm85nvw4t4covtw
Pingback: Fiza Khan Kolkata Independent Call Girls Services
Pingback: 2cn48527tbx34cwtv425d
Pingback: anal dildo|anal extreme
Pingback: Ruchika Roy Kolkata Escorts Call Girls Services
Pingback: slotsjoker123.net
Pingback: free mp3 download
Pingback: bad credit loans online
Pingback: pay day loan
Pingback: Brazzers Hqporner
Pingback: casinos usa
Pingback: http://paydayadvance.us.org/
Pingback: casino gambling online
Pingback: farming simulator 19 mods
Pingback: farming simulator 19 mods
Pingback: Free Brazzers Video
Pingback: http://derekframpton.com/
Pingback: pocket sluicebox
Pingback: Haroon ur Rasheed columns
Pingback: cash loans
Pingback: https://cashloans.us.org/
Pingback: https://www.carinsurancequote.us.org
Pingback: Exie Strobl
Pingback: Dakota Lynch
Pingback: credits.us.org
Pingback: shophousevincitygrandparkquan9
Pingback: nhaphovincityquan9az
Pingback: waterproof document holder
Pingback: Manifestation Magic
Pingback: http://homeinsurancequotes.us.org/
Pingback: http://homeinsurancequotes.us.org/
Pingback: best ivf centre in delhi ncr
Pingback: badminton socks
Pingback: news2
Pingback: Demeter Fertility
Pingback: Layarkaca21
Pingback: poker online
Pingback: poker online
Pingback: Demeter Fertility
Pingback: https://allthingscrypto.tech/anguk-law-offices/feed/
Pingback: http://www.islamiccall.info/?option=com_k2&view=itemlist&task=user&id=343664
Pingback: http://libsindustry.com/index.php/component/k2/itemlist/user/6779
Pingback: https://www.palmettowebsolutions.com/2884/waffle-house-menu-its-worthwhile-to-check-out-this/
Pingback: 123Movies
Pingback: https://allthingscrypto.tech/news/page/5/
Pingback: Power Efficiency Guide
Pingback: jasa view youtube
Pingback: Cheap Jordans
Pingback: Cheap Air Jordans
Pingback: tobacco online australia
Pingback: SAT
Pingback: TECNICO
Pingback: wildlife removal
Pingback: https://casinoclb.de/book-of-moorhuhn/
Pingback: Nonton Film
Pingback: Nonton Film Bioskop
Pingback: animal control solutions
Pingback: bat removal
Pingback: seo byrå oslo
Pingback: wildlife removal
Pingback: 123Movies
Pingback: plot functions/index
Pingback: area perimeter calculator
Pingback: Latest Urdu Columns
Pingback: Latest Pakistani Talkshows
Pingback: Wedoitforthenextgirl.wordpress.com
Pingback: sosyal medya yönetimi"
Pingback: positivewordsresearch
Pingback: positive
Pingback: Acompanhantes Caxias do Sul
Pingback: dijital ajans
Pingback: How to Make Money with CPA
Pingback: 123Movies
Pingback: Roxanne Hurlock
Pingback: Roxanne Hurlock
Pingback: SEO
Pingback: Cheap Escort London
Pingback: Cheap Escort London
Pingback: Ben Marks
Pingback: Ben Marks
Pingback: gold and white 11s
Pingback: white retro jordans
Pingback: Viral Video
Pingback: Artist
Pingback: download terbiasa bahagia
Pingback: terbiasa bahagia mp3
Pingback: Jasa Youtube
Pingback: Jasa Youtube
Pingback: website design new york
Pingback: radiostation
Pingback: teavana
Pingback: https://foxtailmarketing.com/ico-marketing-agency/
Pingback: Gavin
Pingback: sex tube
Pingback: wao tube
Pingback: Merrie Patrick
Pingback: dragkrokskungen
Pingback: new hunters assistant
Pingback: starting items of bill
Pingback: UrbanFiction
Pingback: Javed Chaudhry Columns
Pingback: Krissy Lehmkuhl
Pingback: plumbing jobs riverside ca
Pingback: tipobet365 giris
Pingback: rivalo giris
Pingback: teen porn
Pingback: lucky patcher
Pingback: lucky patcher
Pingback: plumbing jobs riverside ca
Pingback: learn this here now
Pingback: buy houses in lekki
Pingback: https://khadubds.blogspot.com
Pingback: shophouse Phu Quoc
Pingback: click on
Pingback: new year template
Pingback: when time does the store close
Pingback: store closing hours
Pingback: https://rajakhan694663976.wordpress.com/2018/10/28/prime-factors-why-music-posters-will-change-your-home/
Pingback: lmfao
Pingback: Escorts in Kolkata
Pingback: Kolkata Independent Escorts
Pingback: Parallel Profits Review
Pingback: Parallel Profits
Pingback: jual subscriber
Pingback: jual subscriber
Pingback: Fiza Khan Kolkata Independent Escorts Call Girls Services
Pingback: best smm panel
Pingback: Fiza Khan Kolkata Call Girls Escorts Services
Pingback: over the door hanger
Pingback: door valet
Pingback: Diksha Arya Kolkata Escorts Call Girls Services
Pingback: Visit this page for more mspy reviews
Pingback: Diksha Arya Kolkata Independent Escorts Call Girls Services
Pingback: Visit this page for more
Pingback: Ben Marks
Pingback: viagra
Pingback: cialis
Pingback: Roxanne Hurlock
Pingback: coat hanger door
Pingback: over door coat rack
Pingback: dubai
Pingback: dubaiescorts.com
Pingback: 바카라
Pingback: jasa like instagram
Pingback: jual followers instagram
Pingback: Hosting Website Bokep
Pingback: Bokep Online
Pingback: Large Abstract Art For Sale
Pingback: Black And White Abstract Canvas Art
Pingback: Free sex videos
Pingback: kratom locally
Pingback: sbobet casino
Pingback: poker terpercaya indonesia
Pingback: lagu terpopuler
Pingback: lagu terpopuler
Pingback: gozoaccommodations
Pingback: malta properties
Pingback: best kratom strain
Pingback: 30th birthday invitations
Pingback: Best Free Credit Repair
Pingback: is credit repair legal in Florida?
Pingback: Tradestation Indicators
Pingback: you can try this out
Pingback: click here
Pingback: click for more info
Pingback: jual view
Pingback: jasa view youtube
Pingback: Amy Edmunds
Pingback: Diana Ball
Pingback: ATTACHMENTS
Pingback: ATTACHMENTS
Pingback: do you agree
Pingback: she said
Pingback: rscrevolution
Pingback: rscrevolution
Pingback: Layar Kaca 21
Pingback: posture corrector for teens
Pingback: digitad
Pingback: sewingnuts.blogspot.com
Pingback: http://thewholemommything.blogspot.com
Pingback: metaal techniek
Pingback: review surveys
Pingback: CG CASINO APP
Pingback: http://www.portaspotter.com.br/
Pingback: you could check here
Pingback: check it out
Pingback: 8 May 2014
Pingback: Best wart remover
Pingback: Pandora Charms
Pingback: Premier League Store
Pingback: Free scan to see if your PC is part of a bot
Pingback: yahoo mail login
Pingback: hotmail fr
Pingback: deals store
Pingback: beroepsadvies breda
Pingback: bemiddeling tilburg
Pingback: correo hotmail iniciar session
Pingback: outlook iniciar sesion
Pingback: новости игр ps4
Pingback: Find Out More
Pingback: click over here
Pingback: walmartone login
Pingback: Pet Quarantine Sri Lanka
Pingback: xero accounting
Pingback: Pet Move
Pingback: 123Movies
Pingback: 123Movies
Pingback: Dining Room Canvas Art
Pingback: Large Canvas Wall Art Online
Pingback: 2019
Pingback: Christian T-Shirts With Scripture
Pingback: send bulk email
Pingback: gmail password
Pingback: Crisis prevention training online
Pingback: matilde menendez
Pingback: matilde menendez presa
Pingback: Ladakh Honeymoon Packages For Couple
Pingback: Kashmir Holiday Tour Packages
Pingback: China Soccer Uniforms
Pingback: debt relief
Pingback: debt relief
Pingback: Manifestation Magic
Pingback: waalwijk
Pingback: 사다리사이트
Pingback: pinched nerve
Pingback: manicure
Pingback: نقل اثاث ابوظبي
Pingback: mua win bản quyền
Pingback: ایمپلنت
Pingback: roofer in South Dakota
Pingback: online art mall
Pingback: therapie
Pingback: inmobiliaria pereira e hijos quilmes
Pingback: fuck movie
Pingback: la collina toscana coffee syrup set 6 ounces
Pingback: oregon 37 601 sprayer backpack 4 gallon
Pingback: sollicitatie
Pingback: Power Efficiency Guide
Pingback: virgin hair
Pingback: 사다리사이트
Pingback: 토토사이트 검증
Pingback: Nonton Movie
Pingback: bath bombs
Pingback: 123Movies
Pingback: ekg certification class
Pingback: gotporn.me
Pingback: ekg tech classes near me
Pingback: bản quyền game giá rẻ
Pingback: Immigration law
Pingback: 안전공원
Pingback: 사다리사이트
Pingback: movers in Sharjah
Pingback: ایمپلنت
Pingback: revenge postings
Pingback: Grow taller 4 idiots
Pingback: Black And White Canvas Art Online
Pingback: massageauflage24.de
Pingback: Guitar Backing Track
Pingback: leather front pocket wallet
Pingback: sergey
Pingback: JASE CHRISTOPHER
Pingback: raleigh nc bat control
Pingback: 메이저공원
Pingback: 사설토토
Pingback: https://cincin4d.blogspot.com/2019/01/pengalaman-pribadi-yang-tak-terlupakan.html
Pingback: https://agenpoker2019.tumblr.com/
Pingback: http://situspokeronline15678.isblog.net/top-latest-five-togel-sydney-urban-news-9417564
Pingback: http://messiahigcwt.diowebhost.com/16106256/about-togel-sydney
Pingback: Hand assembly
Pingback: 로투스홀짝
Pingback: 안전공원사이트
Pingback: 먹튀검증
Pingback: auto chat profits demo
Pingback: 로투스카지노
Pingback: 네임드사다리
Pingback: degree for sale
Pingback: 3D modeling
Pingback: Earn $2000+ Monthly Autopilot Systems
Pingback: logiciel pour faire des affiches
Pingback: Ewen Chia's Autopilot Income
Pingback: usps lite blue
Pingback: lite blue
Pingback: Unique Weight Loss Method
Pingback: GET Facebook Bot
Pingback: Get Slim in 7 Days
Pingback: 먹튀검증
Pingback: 먹튀검증
Pingback: Autopilot Money Machine
Pingback: mompreneur philippines
Pingback: agen resmi Maxbet
Pingback: judi bola indonesia
Pingback: How To Make Money On Twitter
Pingback: entrepreneur philippines
Pingback: real casino games
Pingback: Burn Belly Fat in 21Days or Money Back
Pingback: legal fat burning steroids
Pingback: are anabloic steroids legal
Pingback: Istanbul escorts
Pingback: donate now
Pingback: Escorts
Pingback: کادو تولد
Pingback: ios app reviews
Pingback: tempo traveller chandigarh to amritsar
Pingback: glitter bomb
Pingback: metropolitan group home exteriors
Pingback: metropolitan group home exteriors
Pingback: troy king denver colorado
Pingback: metropolitan group home exteriors
Pingback: metropolitan group home exteriors review
Pingback: Virginia furniture store
Pingback: kadikoy escort
Pingback: drone-works.com
Pingback: Gold Coast The Risks of Guaranteed Accepted Life Insurance
Pingback: Women Club Dresses
Pingback: 22mm silk sheets
Pingback: Gold Coast Life InsuranceOverweight
Pingback: My Service Canada Account – Review and Usage in 2019
Pingback: 2 Week Diet
Pingback: solarglow garden lights
Pingback: Owning a Car With The Ontario G2 License – Pros and Cons
Pingback: try these out
Pingback: atakoy escort
Pingback: thai massage albany ny
Pingback: findikzade escort bayan
Pingback: psychologically pharmacy
Pingback: child porn
Pingback: torture porn
Pingback: Moskov Top Global
Pingback: HIV
Pingback: daftar domino
Pingback: buy seeds
Pingback: biodegradablestraw1
Pingback: tungsten ring
Pingback: http://19216811ips.com/
Pingback: https://www.abccarpetcleaning-bronx-ny.com
Pingback: Top Test Companies in India
Pingback: Furniture assembly experts
Pingback: Discover More Here
Pingback: health insurance
Pingback: 안전놀이터
Pingback: life insurance
Pingback: singapore proposal photograhy
Pingback: object manipulation
Pingback: trippy toys
Pingback: web link
Pingback: how to make money online
Pingback: concorde group review
Pingback: life insurance
Pingback: travel insurance
Pingback: John Goslow
Pingback: car insurance
Pingback: Diet pills 2019
Pingback: content
Pingback: get car towed for money
Pingback: American Music Download
Pingback: how to print cd labels
Pingback: how to make a dvd cover
Pingback: paxful wallet
Pingback: cbd products near me
Pingback: belajar wordpress
Pingback: sportsbook online
Pingback: nail salon near me
Pingback: jurusan kuliah
Pingback: 안전놀이터
Pingback: free games
Pingback: 스포츠토토사이트
Pingback: porn
Pingback: online casino usa
Pingback: paxful login
Pingback: polish mi nail salon
Pingback: https://www.signinsupport.net
Pingback: 먹튀검증
Pingback: arabian casino
Pingback: Medical Cannabis Seed
Pingback: traslados heathrow londres
Pingback: buy facebook accounts
Pingback: how to attract girls
Pingback: free
Pingback: sports
Pingback: Best restaurant cleaning services
Pingback: instagram takipçi satın al
Pingback: vietnam visa cost
Pingback: download free
Pingback: Bathroom Cleaning
Pingback: GTA San Andreas Android
Pingback: bot
Pingback: free
Pingback: Opera Mini App Download for Android
Pingback: catering menu
Pingback: storeholidayhours.org
Pingback: tourist destinations in spain
Pingback: Cheap
Pingback: Nidika Offer Call Girls in Bangalore
Pingback: free download
Pingback: http://www.k9andcompany.com/
Pingback: business
Pingback: marketing
Pingback: home windows
Pingback: beeg sex
Pingback: xlxx com beeg
Pingback: Agence web et site internet Jura Bernois
Pingback: beeg sex
Pingback: windows replacement
Pingback: createemailaccounts.net
Pingback: create email accounts
Pingback: Karakuri
Pingback: Hair salon in Silver spring MD
Pingback: Cryptocurrency
Pingback: Free Download
Pingback: windows 10 password recovery
Pingback: How To Register A Business In Singapore
Pingback: rhythm guitar
Pingback: Online Company Registration Form
Pingback: Layarkaca21 Korea
Pingback: health
Pingback: small sex doll
Pingback: free
Pingback: gambling
Pingback: forskolin extract
Pingback: aadhar card urn status
Pingback: https://agenbenardanterpercaya.blogspot.com/p/bagisiapa-saja-taruhan-judi-merupakan.html
Pingback: Payday
Pingback: https://8thclassresult.wixsite.com/8thclassresult2019/home/why-is-school-education-an-important-part-of-life
Pingback: loans
Pingback: https://permainseru.blogspot.com/2019/03/bibit-kemunculan-situs-togel-online.html
Pingback: my rant
Pingback: hot-milf
Pingback: Product Rapid Dot Com
Pingback: jenny jerkygirls
Pingback: прививка, вакцинация, пентаксим
Pingback: остеопороз, остеопорозе у ребёнка
Pingback: hot-women-fucking
Pingback: upskirt no panties spy
Pingback: Gas Grills
Pingback: https://www.bloglovin.com/@rainasethi/alcohol-industry-under-risk-from-cannabis
Pingback: https://drohiorenuan.com/
Pingback: magnetmotor kaufen
Pingback: https://www.nairaland.com/5106601/us-tax-cuts-really-helping
Pingback: Product Rapid
Pingback: Money Exchange
Pingback: gas grills review
Pingback: real estate marketing
Pingback: happy background music
Pingback: free background music
Pingback: binnance
Pingback: Cryptocurrency hardware wallet
Pingback: list of companies using cloud computing
Pingback: Layarkaca21
Pingback: sàn forex uy tín
Pingback: Layar Kaca 21
Pingback: China
Pingback: junk my car for cash near me
Pingback: Free Classified Ads
Pingback: forex trading
Pingback: free download
Pingback: poker online
Pingback: forex trading
Pingback: hệ thống tưới diện tích lớn
Pingback: công ty thiết kế website tại đà nẵng
Pingback: built in grills review
Pingback: lyric prank on girlfriend songs
Pingback: Hellomaphie
Pingback: finger exercises for guitar players
Pingback: subscription monthly boxes
Pingback: https://www.123moviesl.com
Pingback: SSNI-472
Pingback: mezuzah on door in breaking bad tv show
Pingback: 먹튀 폴리스
Pingback: free background music
Pingback: http://ighodalo.com/
Pingback: 먹튀검증 업체
Pingback: 먹튀 폴리스
Pingback: anti-aging
Pingback: 안전놀이터
Pingback: 안전 놀이터
Pingback: how much does botox cost in nyc
Pingback: passin grass
Pingback: passingrass
Pingback: https://sicboonlineterpercaya.blogspot.com/p/asyiknya-bermain-judi-sicbo-online.html
Pingback: passin grass
Pingback: passingrass
Pingback: 메이저 사이트
Pingback: http://bandartogelterpercaya.blogolink.com/billet/sejarah-singkat-poker-dan-6-pemain-poker-terkaya-di-dunia-121998.html
Pingback: 베트맨 토토
Pingback: 43ytr.icu
Pingback: smilforalifetime
Pingback: passingrass.com
Pingback: passin grass
Pingback: porn online
Pingback: Raw Food Certification Bali
Pingback: 먹튀검증
Pingback: Kadetskaya Law Firm
Pingback: 그래프 메이저사이트
Pingback: 大阪 地下鉄 路線図 梅田
Pingback: buy forskolin online
Pingback: Robert Smith Newcastle
Pingback: Unlimited Internet & Data @ 50 Mbps starting at Rs 599 onwards
Pingback: 京浜東北線 赤羽駅
Pingback: ssni 473
Pingback: Magento 2 Gift Voucher
Pingback: visit us
Pingback: 먹튀사이트
Pingback: all Gator sports
Pingback: 먹튀폴리스 가족방
Pingback: 바다이야기 하는법
Pingback: 바다이야기 무료게임 다운로드
Pingback: medical practice management software
Pingback: free classifieds
Pingback: 야마토 릴게임
Pingback: Commercial Solar Power
Pingback: sofa and loveseat
Pingback: animoporn
Pingback: Commercial Roofer Aberdeen
Pingback: telugu aunty boobs photos
Pingback: viagra
Pingback: Dr Robert Smith Newcastle
Pingback: Ida Wong Taylor
Pingback: Robert Smith Newcastle
Pingback: Jamie Nemtsas
Pingback: Josh Dinnerman
Pingback: learn black magic
Pingback: Jamie Nemtsas
Pingback: Joshua DInnerman
Pingback: funny gift
Pingback: software
Pingback: Joshua Dinnerman
Pingback: cialis
Pingback: JAV
Pingback: Hamilton Lindley
Pingback: 토토사이트
Pingback: freedom lifestyles academy
Pingback: online poker terpercaya
Pingback: 오션파라다이스
Pingback: https://youtu.be/w54FJv7exrI
Pingback: ufa
Pingback: 릴게임 바다이야기
Pingback: 다자바
Pingback: https://youtu.be/w54FJv7exrI
Pingback: Buy Shatter Online
Pingback: hotel paris
Pingback: Liteblue
Pingback: indiatimes
Pingback: mobileporn
Pingback: Sage Naumann Brighton
Pingback: https://mmablogexperts.com/2019/05/05/what-is-sambo/
Pingback: Book cheap hotel
Pingback: Haircare line upgrade
Pingback: listings
Pingback: Construction Debris Removal
Pingback: green card organization
Pingback: shipping calculator
Pingback: 무료스포츠중계
Pingback: usb air humidifier essential oil aromatherapy diffuser
Pingback: Anime store online
Pingback: Layarkaca21
Pingback: Layarkaca21
Pingback: Superior Singing Method
Pingback: The Lost Ways
Pingback: inmotion
Pingback: Employer Tools
Pingback: Training Brisbane
Pingback: 먹튀 폴리스
Pingback: end of lease cleaning australia
Pingback: Cheap Domain Registration
Pingback: 야마토게임
Pingback: best way to clean scuff marks off walls
Pingback: 안전사이트
Pingback: bandarq online
Pingback: More about the author
Pingback: pop over to these guys
Pingback: estate agent tenerife
Pingback: travel blog
Pingback: this page
Pingback: 릴게임 오션파라다이스
Pingback: Where to buy Total Curve
Pingback: 우리 카지노
Pingback: 토토사이트
Pingback: form
Pingback: His Secret Obsession
Pingback: 토토사이트 추천
Pingback: Mobile Mechanic Henderson Nv
Pingback: round wedding arch
Pingback: confinement meals delivery kl
Pingback: Situs Judi Online
Pingback: căn hộ sala
Pingback: walmartone login
Pingback: walmartone login
Pingback: walmartone login
Pingback: https://www.signinsupport.net
Pingback: cruise
Pingback: Dream
Pingback: bohemian jewelry
Pingback: beginner tuts courses
Pingback: ABP 866
Pingback: mobile app giving
Pingback: marketing
Pingback: 먹튀폴리스 검증
Pingback: AIM GLOBAL United Kingdom
Pingback: super elastic anti-slip tights
Pingback: how to illustrate children's books tips
Pingback: Oliver isaacs blockchain
Pingback: https://www.filedune.tk
Pingback: Oliver Isaacs Forbes
Pingback: sustainability
Pingback: Eago
Pingback: EZ Battery Reconditioning
Pingback: free steam game keys
Pingback: forex signals
Pingback: mở tài khoản forex
Pingback: oliverzok instagram
Pingback: hundekurv tilbud
Pingback: satta king
Pingback: how to play a guitar for beginners
Pingback: gucci women
Pingback: 먹튀폴리스 가족방
Pingback: Mobile car wash Swindon
Pingback: poker online
Pingback: dog training with collars
Pingback: smm instagram
Pingback: smm google
Pingback: botulism botox
Pingback: liteblue login
Pingback: mylifeline
Pingback: stars 090
Pingback: Shriram Earth Whitefield
Pingback: Free YouTube to MP3 Converter
Pingback: 안전토토사이트
Pingback: Home
Pingback: second hand clothes
Pingback: frontend portfolio
Pingback: cheap wedding rings
Pingback: Layarkaca21
Pingback: https://www.lastingsafe.com/vault-door
Pingback: strong room door
Pingback: YouTube Downloader
Pingback: liteblue login
Pingback: MIAA-105
Pingback: MIDE-662
Pingback: wanz 871
Pingback: safe deposit boxes
Pingback: 조건만남사이트
Pingback: Shriram Earth Marathahalli
Pingback: ksd301
Pingback: Shriram Earth Devanahalli
Pingback: is it down right now
Pingback: website down
Pingback: Machines
Pingback: hire someone to catch a cheater
Pingback: il baise ma femme
Pingback: digital marketing agency in delhi
Pingback: philly
Pingback: fabulousaaa replica
Pingback: Living Room Large Abstract Art
Pingback: chanel replica handbags review
Pingback: art deco bronze figures
Pingback: tech blog
Pingback: scooter
Pingback: trump news
Pingback: seo
Pingback: Ida Wong Taylor
Pingback: Ida Wong Taylor
Pingback: medium
Pingback: cash
Pingback: free steam cards
Pingback: kraftig dildo
Pingback: Christine Reidhead, Author
Pingback: maple ridge appliance repair
Pingback: Halki Diabetes Remedy
Pingback: cal poly financial technology
Pingback: site
Pingback: singapore corporate gift distributor
Pingback: Replica Oakleys
Pingback: Fake Oakley Sunglasses
Pingback: Layarkaca21
Pingback: Transport de personnes à mobilité réduite (PMR) et organisation de mariage de prestige. CHAUFFEUR PRIVÉ POUR VOS TRAJETS SUR-MESURE
Pingback: Yoga Burn
Pingback: safe deposit locker
Pingback: Self-service safe deposit
Pingback: журнал Зарплата
Pingback: free charm bracelet
Pingback: Cincinnati fashion boutique
Pingback: wedding live band
Pingback: Ishq Subhan Allah
Pingback: Flat Belly Fix
Pingback: Majeda Awawdeh
Pingback: gmail messagerie
Pingback: 약판매사이트
Pingback: aws training and placement in pune
Pingback: Hispanic Director
Pingback: Cannabis
Pingback: Dallas Video Production
Pingback: Director Portfolio
Pingback: environmentally safe car wash soap
Pingback: Salem Music Group
Pingback: pirater un compte facebook
Pingback: Buchanan, Williams & O'Brien
Pingback: Bulk Image Editing For eCommerce
Pingback: free fundraising sites for schools
Pingback: theflyer.com
Pingback: Donating profits to charity
Pingback: tuugo.us
Pingback: Manji Law, P.C.
Pingback: thenumbers.marketplace.org
Pingback: Tadeo & Silva
Pingback: Top Forex Brokers
Pingback: Janitorial Services
Pingback: Healthy breakfast ideas
Pingback: forum
Pingback: what hairstyle suits me quiz
Pingback: Hundeseng på ben
Pingback: difference between plc and rtu
Pingback: cyberlink
Pingback: porn
Pingback: 먹튀검증커뮤니티
Pingback: mega vars
Pingback: รับแก้เพจถูกแฮก
Pingback: 우리카지노
Pingback: https://taxiindenbosch.nl
Pingback: Most effective posture corrector
Pingback: ยุโรป
Pingback: online dating
Pingback: Continue Reading
Pingback: telegraph
Pingback: Unusual and inspiring travel ideas
Pingback: feder fiskeolie
Pingback: desi school sex
Pingback: intensedebate
Pingback: lung health institute tampa
Pingback: tegn på orm hos hund
Pingback: ô quảng cáo
Pingback: no deposit bonus forex 2019
Pingback: bloglovin
Pingback: https://www.emailconnexion.org/
Pingback: iDisplay
Pingback: Instagram template PSD download 2019
Pingback: 1Pro Vancouver moving company 604 721-4555
Pingback: ormekur hvalpe
Pingback: full body massage
Pingback: Leading MSO in North India
Pingback: Ormekur til kat
Pingback: timelines templates for powerpoint
Pingback: lọc nước công nghiệp
Pingback: nuru massage london
Pingback: body to body massage
Pingback: PlanB sydney airport transfers
Pingback: body massage london
Pingback: Ormekur til kat
Pingback: family values
Pingback: 우리카지노 계열
Pingback: kids furniture outlet. Office furniture outlet
Pingback: appliance repair coquitlam (604) 404-1677
Pingback: cabinets bellevue
Pingback: pharma cheap
Pingback: video bokep indonesia
Pingback: xóc đĩa bịp mới nhất
Pingback: MIAA-127
Pingback: HQD
Pingback: WANZ-882
Pingback: http://cleaningtips99.angelfire.com/
Pingback: TCLM appliance repair (604) 404-1677
Pingback: topcleaners99
Pingback: GVG 916
Pingback: WANZ 878
Pingback: Dallas hosting
Pingback: click here
Pingback: Brigitte Opp
Pingback: MIAA 129
Pingback: nonton video bokep
Pingback: đồ xóc đĩa bịp
Pingback: Ikov Bot for Unlimited Votes
Pingback: đồ xóc đĩa bịp
Pingback: MIDE-671
Pingback: http://cleanersinfo.nation2.com/
Pingback: full spectrum led
Pingback: Message Board
Pingback: bandmix.com
Pingback: Faulkner Law
Pingback: lawyerlegion.com
Pingback: cannabinoids
Pingback: ikea assembly
Pingback: quitting
Pingback: satta king
Pingback: cedar homes for sale
Pingback: Hirschen Amriswili
Pingback: famous abstract artists
Pingback: Trinken Amriswil
Pingback: https://flakeads.co.uk/
Pingback: 토토 사이트
Pingback: مكتب تمريض
Pingback: magazine for women
Pingback: uttaratoday
Pingback: pure pashmina
Pingback: 먹튀 폴리스
Pingback: 베트맨
Pingback: strip club taxi
Pingback: groomsmen
Pingback: crafty vaporizer
Pingback: courier to Romania
Pingback: boostscores
Pingback: how to tell if mice are gone
Pingback: rnetwork discount card
Pingback: black decker 40v battery
Pingback: health
Pingback: pirater un compte facebook
Pingback: gvg 918
Pingback: ô dù chính tâm
Pingback: Daraz BD
Pingback: post free ads in nigeria
Pingback: www.NorthRustic.com
Pingback: lung institute
Pingback: 10th Class Result 2019 Multan Board
Pingback: แทงบอลออนไลน์
Pingback: dù sân vườn
Pingback: 파워볼
Pingback: TOYS
Pingback: 10th Class Result 2019 Bahawalpur Board
Pingback: Epilators
Pingback: 슈어맨2
Pingback: Red Tea
Pingback: 파워볼예측
Pingback: 에그벳카지노
Pingback: cheap lacoste shirts
Pingback: top 10 binary options brokers
Pingback: free keynote templates
Pingback: findlocationsnearme.net
Pingback: 바카라사이트
Pingback: Samsung NE58K9560 Induction
Pingback: ormekur hund
Pingback: Zip Up Hoodies
Pingback: Dragon Ball T-Shirts
Pingback: anti terror course
Pingback: h8d3k
Pingback: Hd porn
Pingback: Ormekur kat tyskland
Pingback: Sports
Pingback: Ormekur kat
Pingback: risk analysis ireland
Pingback: dse assessor course
Pingback: fire warden training
Pingback: interior design art
Pingback: fire manager
Pingback: online stress training
Pingback: islamic abstract arabic art
Pingback: mwt0g
Pingback: game hay cho android
Pingback: Kilberry motionscykel
Pingback: Schwinn motionscykel
Pingback: ez battery reconditioning secret
Pingback: Great Clips Coupons
Pingback: taxi taxi taxi taxi taxi taxi
Pingback: greyhound wagering
Pingback: Gifts for dad
Pingback: ez battery reconditioning program review
Pingback: capread
Pingback: chronic panic attacks
Pingback: Find den perfekte dildo
Pingback: tips to help with anxiety
Pingback: ban can ho sarimi
Pingback: spolorm hund
Pingback: ormekur kat apotek
Pingback: LuLaRoe Size Chart
Pingback: watchxxxfree
Pingback: fake money online
Pingback: Hidden Asset Searches Baldwin County
Pingback: Hundemad i pølser
Pingback: Missing Person Invesigations in Baldwin County
Pingback: thuoc kich duc sg
Pingback: 메이저놀이터
Pingback: order adipex online legally
Pingback: walmart call in number
Pingback: figma wireframing meaning in dccn
Pingback: BIGPOND EMAIL SUPPORT
Pingback: penis extender
Pingback: world oldest wood watch
Pingback: create a wikipedia biography
Pingback: Shopping WebSites
Pingback: bitcoin code review
Pingback: make a wikipedia article about yourself
Pingback: Wikipedia editors for hire
Pingback: turmeric curcumin capsules
Pingback: how to create a wikipedia page for a school
Pingback: Video Animation Company
Pingback: hemp oil UK
Pingback: forum
Pingback: 먹튀 검증
Pingback: SW 650
Pingback: It is racist to deny Whites & Arabs are a mix of blond haired blue eyed white skinned Nordics and the Indian race, do you agree?
Pingback: 360 wigs
Pingback: lace front wig
Pingback: 우리카지노계열
Pingback: It is racist to deny Whites & Arabs are a mix of blond haired blue eyed white skinned Nordics and the Indian race, do you agree?
Pingback: 13x6 bob wig
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: no wig cap needed wig
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: elva hair
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: http://pixieenvy.tumblr.com
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: booking
Pingback: Best church giving apps
Pingback: booking
Pingback: booking
Pingback: Donation forms for nonprofits
Pingback: demir leather
Pingback: Saudi Shia News
Pingback: diyarbakir escort
Pingback: Fine
Pingback: Bewafa Shayari
Pingback: one punch man sticker
Pingback: ted.com
Pingback: 릴게임오션파라다이스
Pingback: paginas web puebla
Pingback: 메이저놀이터
Pingback: how to guitar solo
Pingback: patent registration
Pingback: smm reseller panel
Pingback: 릴게임다운로드
Pingback: Situs Judi Online
Pingback: 메이저놀이터
Pingback: telegram forex signals
Pingback: MIAA-146
Pingback: loft conversions Eastleigh
Pingback: MIAA 143
Pingback: Sonos
Pingback: gai goi da nang
Pingback: Blog Designer Pro
Pingback: empty nail oil pen
Pingback: visit
Pingback: yeezy shoes wholesale
Pingback: Eweka
Pingback: Click Here
Pingback: minyak kelapa VCO
Pingback: קניית צפיות ישראלים
Pingback: linktaimod
Pingback: Locksmith North York
Pingback: Ormekur kat håndkøb
Pingback: linktaimod
Pingback: korean contact lenses amazon
Pingback: 오션파라다이스 다운로드
Pingback: cashmere scarf
Pingback: Online donation forms
Pingback: Online donation forms
Pingback: are korean contact lenses safe
Pingback: 먹튀 검증
Pingback: beach wear
Pingback: 베트맨
Pingback: spolorm hund
Pingback: official statement
Pingback: ormekur hund
Pingback: Data back-up and recovery
Pingback: Russian foo store
Pingback: 123 Movies
Pingback: huge store discounts
Pingback: shoes
Pingback: Sleepwear Manufacturers
Pingback: glycemic index management books
Pingback: parc komo balance units
Pingback: florence residences
Pingback: haus on handy balance units
Pingback: gifts for men
Pingback: JUFE 096
Pingback: parc esta
Pingback: treasure at tampines showflat
Pingback: anxiety and panic attack books
Pingback: female urination device disposable
Pingback: 사설토토사이트
Pingback: organic tea
Pingback: 해외토토사이트
Pingback: read more
Pingback: Locksmith near me
Pingback: Homemade Generator
Pingback: 먹튀업체
Pingback: Locksmith near me
Pingback: 토토
Pingback: 토토사이트
Pingback: Instagram promotion
Pingback: how to generate free internet traffic
Pingback: https://officialgojicream.com/pt
Pingback: hp
Pingback: site here
Pingback: new user aliexpress coupons
Pingback: read more
Pingback: cbd
Pingback: Places to eat
Pingback: SSNI-575
Pingback: ghế lười
Pingback: places to eat near me now
Pingback: http://betting-sports.info
Pingback: Car lockout Richmond Hill
Pingback: Indian Office Wear
Pingback: teds woodworking reviews
Pingback: teds mind guide
Pingback: support
Pingback: 아동미술학원
Pingback: pomeranian puppies for sale
Pingback: Trixie hundeseng
Pingback: beagle puppies for sale in ny
Pingback: cotonpoo puppies for sale
Pingback: best penis enlargement methods
Pingback: malshi puppies
Pingback: papillon puppies for sale near me
Pingback: casareparacoes24h.pt
Pingback: cavachon puppies for sale
Pingback: cavalier king charles spaniel puppies for sale
Pingback: puggle puppies for sale near me
Pingback: labrador retriever puppies for sale
Pingback: pekingese puppies for sale
Pingback: frenchton puppies for sale
Pingback: teddy bear puppies for sale near me
Pingback: chihuahua puppies for sale near me
Pingback: shiba inu puppies for sale
Pingback: pembroke welsh corgi puppies for sale
Pingback: yorkiepoo puppies for sale
Pingback: porsche
Pingback: site here
Pingback: best garment steamer
Pingback: thung giay
Pingback: buy stocks
Pingback: bulk sms abu dhabi
Pingback: eggless cakes flowers delivery by Phoolwala
Pingback: bulk sms marketing dubai
Pingback: nhà hàng ở vinh
Pingback: homemade generator
Pingback: citytowtruck.com
Pingback: homemade generator
Pingback: tecmo koei
Pingback: weight loss 40 pounds
Pingback: we-b-tv.com
Pingback: career development blog
Pingback: توشيبا العربي
Pingback: ormekur kat håndkøb
Pingback: ormekur kat apotek
Pingback: 蜂駆除
Pingback: ssa gujarat online hajri
Pingback: gotukola hair mask
Pingback: http://upholsterycleaningsydney.jigsy.com/
Pingback: Porn website that shows what you want to see
Pingback: Insurance Telesales Training
Pingback: Funny T Shirts For Woman
Pingback: Shirts For Woman
Pingback: Knitwear manufacturers
Pingback: Stream Complet
Pingback: 예스카지노
Pingback: cruises from Sydney
Pingback: Flower Tulle Dress
Pingback: Text Chemistry
Pingback: Merrie Patrick
Pingback: Fred Block
Pingback: clash of lights s2
Pingback: Neck Pain Relief Hammock
Pingback: Best Drone 2019
Pingback: Girls Bikini Set
Pingback: peppymode islamic wear
Pingback: Christmas nutcrackers for sale
Pingback: Ver PelÃculas Online Gratis
Pingback: link
Pingback: proton-pack.com
Pingback: anturamuotti
Pingback: e commerce website name generator
Pingback: Read More
Pingback: How to Use Medicare PlanFinder
Pingback: 188bet link
Pingback: orm hos hunde
Pingback: rolex toronto
Pingback: autotallin nosto ovi
Pingback: palete de ruj
Pingback: 안전놀이터
Pingback: temp mail
Pingback: bændelorm kat
Pingback: Tours to Istanbul
Pingback: escorts in kanpur
Pingback: fenugreek seeds ayurveda and its uses
Pingback: lightning protection
Pingback: Chris Westfall Medicare Agent
Pingback: buy CBD oil
Pingback: israelnightclub.com/girls-cat/דירות-דיסקרטיות-בבאר-שבע/
Pingback: CBD gummies
Pingback: Gifts to Loharu India
Pingback: cbd gummies
Pingback: Gifts to Kadambur India
Pingback: healthy weight loss
Pingback: buy viagra
Pingback: buy viagra
Pingback: best CBD gummies
Pingback: 온라인으로 즐기는 카지노게임
Pingback: 웨이하이 골프투어
Pingback: negative effects of keto diet
Pingback: #jeffrenfroe
Pingback: #AlPacino
Pingback: #AmazonPrime
Pingback: phishing website
Pingback: Situs Bola Online
Pingback: hack game clash of clans
Pingback: Interactive Thriller Adventure
Pingback: agencasino
Pingback: học makeup cá nhân
Pingback: Visit Site
Pingback: wordpress virus removal
Pingback: Stream Complet HD
Pingback: Hyderabad Escorts Call Girls Services
Pingback: viagra
Pingback: esta sexo
Pingback: esta usa
Pingback: viagra
Pingback: viagra
Pingback: visto sesso
Pingback: private detective
Pingback: Tech A Look
Pingback: web agency
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: private detective
Pingback: viagra
Pingback: visto burkina
Pingback: viagra
Pingback: Viagra online
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: viagra
Pingback: Rothgen Capital Ltd
Pingback: viagra
Pingback: viagra
Pingback: orm hos hunde
Pingback: upholstery cleaning fayetteville nc
Pingback: Carpet Cleaning Hope Mills NC
Pingback: CISCO 300-560 Dumps
Pingback: http://www.drugfreeworkplace.org/
Pingback: 메이저사이트 추천
Pingback: Steampunk
Pingback: MontrealFilm
Pingback: Google Play Developer Promoter
Pingback: Houston Breast Lift
Pingback: Casting
Pingback: Google Adwords PPC Services Singapore
Pingback: digitale transformation beratung
Pingback: IP CCTV systems
Pingback: how to lose face fat
Pingback: kids clothes
Pingback: pizza near me
Pingback: dominos coupons
Pingback: best Italian Orlando
Pingback: fine dining Orlando
Pingback: Discount Code
Pingback: bitcoin cash out machine
Pingback: gear oils
Pingback: how many rings does curry have
Pingback: gai goi
Pingback: Sphuket tours
Pingback: Amircani Law
Pingback: free download for pc windows
Pingback: free apk latest version download
Pingback: Manji Law
Pingback: 500px.com
Pingback: 稼ぐ
Pingback: cbd oil for sale
Pingback: laweekly.com
Pingback: Bangalore Cheap Escorts Sevices
Pingback: Curtains in Pakistan
Pingback: biden
Pingback: Ukrayna
Pingback: progentra reviews
Pingback: Discount Code
Pingback: read virtual
Pingback: "Click here for more information"
Pingback: my address
Pingback: my location
Pingback: fake driver license
Pingback: best home radon test Pueblo
Pingback: 토토사이트
Pingback: acoustic treatment for ed Lynchburg
Pingback: Majeda Awawdeh
Pingback: 릴게임사이트
Pingback: free IPTV
Pingback: ananizi sikeyim
Pingback: james amato visionweb
Pingback: internet marketing
Pingback: BTS shop
Pingback: Kajaani
Pingback: limmit kopi
Pingback: Watch TV Shows
Pingback: dentist thailand
Pingback: amarjit jhaj
Pingback: jhaj amarjit
Pingback: NNPJ 367
Pingback: movers north vancouver
Pingback: proair hfa
Pingback: optrimax ezy
Pingback: القيادة والإدارة
Pingback: free underground hip hop instrumentals
Pingback: Dr Majeda Awawdeh
Pingback: Gorgeous girl by Danny Berryhill on Fee Free Music Store #Rock
Pingback: koroush pour
Pingback: nicotine e-liquids Australia
Pingback: Legacy Of Discord Apk Mod
Pingback: Legacy Of Discord Apk Download
Pingback: salon
Pingback: Pune Escorts Services Call Girls
Pingback: canadianpharmacystorm.com
Pingback: gencialiscoupon.com
Pingback: genericvgrmax.com
Pingback: viagrawithoutdoctorspres.com
Pingback: https://www.gartenmoebelsets2020-kaufen.com/finehome-campingmoebel-set-5tlg-alu-120x60x58-70cm-4-campingstuehle-beige-stoff-oxfort-1x-xxl-campingtisch-mit-tragegriff-online-kaufen/
Pingback: SEEU Damen Laufshirt mit 1/2 Reißverschluss Fitness Sweatshirt Laufjacke Sport Langarm Shirt günstig
Pingback: 메이저놀이터
Pingback: canpharmb3.com
Pingback: best cbd oil for sleep
Pingback: best cbd oil for anxiety
Pingback: best cbd oil for pain
Pingback: 婚約指輪
Pingback: how to get more instagram followers
Pingback: gain financial freedom
Pingback: buzzlly.com
Pingback: Bet
Pingback: kostenlose v bucks bekommen
Pingback: Garrett
Pingback: custream
Pingback: quickmeme click here to view
Pingback: продвижение сайта нижний новгород
Pingback: please go through the following link
Pingback: here-in meaning
Pingback: digital advertising agency
Pingback: discourage concrete nouns
Pingback: click here for more information button
Pingback: why not find out more
Pingback: https://kemistroy.ru/communication/forum/messages/forum4/message3180/3138-lean-system-7-diet-pills?result=new
Pingback: Http://receptom.Ru
Pingback: BioGen Keto Reviews
Pingback: cheap car insurance
Pingback: Elite Male Gummies
Pingback: price
Pingback: item533101692
Pingback: seo services
Pingback: quote
Pingback: Auto insurance
Pingback: item539051147
Pingback: property damage
Pingback: item514047884
Pingback: Commercial daycare insurance
Pingback: Insurance Las Vegas NV
Pingback: http://freetto.net
Pingback: click here please
Pingback: read briefly yours online
Pingback: go to my site
Pingback: clicking here will get you there
Pingback: Http://vtik.net
Pingback: Http://Gimnazia-lanchkhuti.ge/
Pingback: zhabbo.free.fr
Pingback: Auto insurance agents Chicago
Pingback: Cheap sr22 insurance Chicago
Pingback: Https://Dain-Rmc.Co.Kr/Bbs/Board.Php?Bo_Table=Free&Wr_Id=941125
Pingback: Gpbpatriot.Ru
Pingback: tatra114.ru
Pingback: http://www.clrobur.com/bbs/board.php?bo_table=free&wr_id=622679
Pingback: please see the link below for more information
Pingback: 80Aaa2Bbjbajhsi0Bu.рф